Journal Description
Audiology Research
Audiology Research
is an international, scientific, peer-reviewed, open access journal on audiology and neurotology, published bimonthly online by MDPI (from Volume 10, Issue 2 - 2020). The Italian Society of Vestibology (VIS) is affiliated with Audiology Research and its members receive a discount on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 22.9 days after submission; acceptance to publication is undertaken in 3.7 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.7 (2022);
5-Year Impact Factor:
1.6 (2022)
Latest Articles
Reply to Hornibrook, J. Comment on “Tabet et al. Vestibular Migraine versus Méniere’s Disease: Diagnostic Utility of Electrocochleography. Audiol. Res. 2023, 13, 12–22”
Audiol. Res. 2024, 14(3), 505-506; https://doi.org/10.3390/audiolres14030042 (registering DOI) - 30 May 2024
Abstract
We appreciate the comments made by Hornibrook (2024) [...]
Full article
Open AccessArticle
Assessment of Outer and Middle Ear Pathologies in Lilongwe, Malawi
by
Ruth Mtamo, Jenna Vallario, Ambuj Kumar, Jesse Casanova and Julia Toman
Audiol. Res. 2024, 14(3), 493-504; https://doi.org/10.3390/audiolres14030041 (registering DOI) - 30 May 2024
Abstract
►▼
Show Figures
Outer and middle ear pathologies are known to disproportionately affect low-income countries but data is limited. We aim to quantify the prevalence rate of patients presenting with middle/outer ear pathologies at ABC Hearing Clinic and Training Centre in Lilongwe, Malawi. Audiological consultations (adult
[...] Read more.
Outer and middle ear pathologies are known to disproportionately affect low-income countries but data is limited. We aim to quantify the prevalence rate of patients presenting with middle/outer ear pathologies at ABC Hearing Clinic and Training Centre in Lilongwe, Malawi. Audiological consultations (adult and paediatric) from 2018–2020 were reviewed for outer and middle ear pathologies. Secondary outcomes included patient type (private vs. community) compared to otoscopy findings, tympanometry findings, need for follow up, and follow up compliance. Out of 1576 patients reviewed, the proportion of abnormal cases’ was 98.2%, with 41.4% being unilateral and 57.4% bilateral. Eighty-three percent presented with outer/middle ear pathologies. 68% of those presented with a pathology often associated with some degree of conductive hearing loss (occluding wax, perforation, discharge, Type B/Type C tympanogram). Average age was 29 + 0.527 years; 41.6% private and 58.2% community patients. Cerumen impaction was most common finding (51%). Higher rates of otoscopic abnormalities and type B tympanograms were noted in community vs. private patient (~40% vs. ~30%; ~70% vs. ~30%). Adherence to follow up was higher for community vs. private patients (29% vs. 17%); ~70% reported subjective improvement upon follow up. The majority required multiple interventions on follow up. Secondary follow up was recommended in 64.8%. A significant disease burden of outer and middle ear pathologies was identified. Further research is required to understand the disease burden and promote health policy.
Full article

Figure 1
Open AccessPerspective
Hearing Loss and Cognitive Decline in the Aging Population: Emerging Perspectives in Audiology
by
Naveen K. Nagaraj
Audiol. Res. 2024, 14(3), 479-492; https://doi.org/10.3390/audiolres14030040 - 23 May 2024
Abstract
In this perspective article, the author explores the connections between hearing loss, central auditory processing, and cognitive decline, offering insights into the complex dynamics at play. Drawing upon a range of studies, the relationship between age-related central auditory processing disorders and Alzheimer’s disease
[...] Read more.
In this perspective article, the author explores the connections between hearing loss, central auditory processing, and cognitive decline, offering insights into the complex dynamics at play. Drawing upon a range of studies, the relationship between age-related central auditory processing disorders and Alzheimer’s disease is discussed, with the aim of enhancing our understanding of these interconnected conditions. Highlighting the evolving significance of audiologists in the dual management of cognitive health and hearing impairments, the author focuses on their role in identifying early signs of cognitive impairment and evaluates various cognitive screening tools used in this context. The discussion extends to adaptations of hearing assessments for older adults, especially those diagnosed with dementia, and highlights the significance of objective auditory electrophysiological tests. These tests are presented as vital in assessing the influence of aging and Alzheimer’s disease on auditory processing capabilities and to signal cognitive dysfunction. The article underscores the critical role of audiologists in addressing the challenges faced by the aging population. The perspective calls for further research to improve diagnostic and therapeutic strategies in audiology, and emphasizes the need for a multidisciplinary approach in tackling the nexus of hearing loss, auditory processing, and cognitive decline.
Full article
(This article belongs to the Special Issue Cognitive Decline within the Audiology Scope of Practice)
Open AccessArticle
Comparison of Psychometric Functions Measured Using Remote Testing and Laboratory Testing
by
Nirmal Srinivasan, Chhayakanta Patro, Radhika Kansangra and Angelica Trotman
Audiol. Res. 2024, 14(3), 469-478; https://doi.org/10.3390/audiolres14030039 - 22 May 2024
Abstract
►▼
Show Figures
The use of remote testing to collect behavioral data has been on the rise, especially after the COVID-19 pandemic. Here we present psychometric functions for a commonly used speech corpus obtained in remote testing and laboratory testing conditions on young normal hearing listeners
[...] Read more.
The use of remote testing to collect behavioral data has been on the rise, especially after the COVID-19 pandemic. Here we present psychometric functions for a commonly used speech corpus obtained in remote testing and laboratory testing conditions on young normal hearing listeners in the presence of different types of maskers. Headphone use for the remote testing group was checked by supplementing procedures from prior literature using a Huggins pitch task. Results revealed no significant differences in the measured thresholds using the remote testing and laboratory testing conditions for all the three masker types. Also, the thresholds measured obtained in these two conditions were strongly correlated for a different group of young normal hearing listeners. Based on the results, excellent outcomes on auditory threshold measurements where the stimuli are presented both at levels lower than and above an individual’s speech-recognition threshold can be obtained by remotely testing the listeners.
Full article

Figure 1
Open AccessArticle
Hebrew Digits in Noise (DIN) Test in Cochlear Implant Users and Normal Hearing Listeners
by
Riki Taitelbaum-Swead and Leah Fostick
Audiol. Res. 2024, 14(3), 457-468; https://doi.org/10.3390/audiolres14030038 - 20 May 2024
Abstract
This study aimed to compare the Hebrew version of the digits-in-noise (DIN) thresholds among cochlear implant (CI) users and their normal-hearing (NH) counterparts, explore the influence of age on these thresholds, examine the effects of early auditory exposure versus its absence on DIN
[...] Read more.
This study aimed to compare the Hebrew version of the digits-in-noise (DIN) thresholds among cochlear implant (CI) users and their normal-hearing (NH) counterparts, explore the influence of age on these thresholds, examine the effects of early auditory exposure versus its absence on DIN threshold, and assess the correlation between DIN thresholds and other speech perception tests. A total of 13 children with CI (aged 5.5–11 years), 15 pre-lingual CI users (aged 14–30 years), and 15 post-lingual CI users (aged 22–77 years), and their age-matched NH controls (n = 45) participated in the study. Speech perception tasks, including the DIN test, one-syllable word test, and sentence identification tasks in various auditory conditions, served as the main outcome measures. The results indicated that CI users exhibited higher speech reception thresholds in noise across all age groups compared to NH peers, with no significant difference between pre-lingual and post-lingual CI users. Significant differences were also observed in monosyllabic word and sentence accuracy in both quiet and noise conditions between CI and NH groups. Furthermore, correlations were observed between the DIN and other speech perception tests. The study concludes that CI users require a notably higher signal-to-noise ratio to discern digits in noise, underscoring the DIN test’s utility in assessing speech recognition capabilities in CI users while emphasizing the need for a comprehensive test battery to fully gauge their speech perception abilities.
Full article
(This article belongs to the Special Issue Rehabilitation of Hearing Impairment: 2nd Edition)
►▼
Show Figures

Figure 1
Open AccessArticle
Evolution of Hyperventilation-Induced Nystagmus in Acute Unilateral Vestibulopathy—Interpretative Model and Etiopathogenetic Hypotheses
by
Francesco Frati, Alessandra D’Orazio, Valeria Gambacorta, Giacomo Ciacca, Giampietro Ricci and Mario Faralli
Audiol. Res. 2024, 14(3), 442-456; https://doi.org/10.3390/audiolres14030037 - 18 May 2024
Abstract
►▼
Show Figures
Hyperventilation induces metabolic changes that can elicit nystagmus (hyperventilation-induced nystagmus, HVIN) in various vestibular disorders, revealing vestibular imbalance and bringing out central or peripheral asymmetries. In acute unilateral vestibulopathy (AUVP, namely vestibular neuritis), hyperventilation can induce different patterns of nystagmus (excitatory, inhibitory, or
[...] Read more.
Hyperventilation induces metabolic changes that can elicit nystagmus (hyperventilation-induced nystagmus, HVIN) in various vestibular disorders, revealing vestibular imbalance and bringing out central or peripheral asymmetries. In acute unilateral vestibulopathy (AUVP, namely vestibular neuritis), hyperventilation can induce different patterns of nystagmus (excitatory, inhibitory, or negative), disclosing or modifying existing static vestibular asymmetries through its ability to invalidate compensation or increase peripheral excitability. In this context, we followed the evolutionary stages of HVIN in AUVP across 35 consecutive patients, with the goal of assessing alterations in the oculomotor pattern caused by hyperventilation over time. In the acute phase, the incidence of the excitatory pattern (and the strongly excitatory one, consisting of a reversal nystagmus evoked by hyperventilation) was significantly higher compared to the inhibitory pattern; then, a progressive reduction in the incidence of the excitatory pattern and a concomitant gradual increase in the incidence of the inhibitory one were observed in the follow-up period. Assuming the role of the ephaptic effect and the transient loss of vestibular compensation as opposing mechanisms, i.e., excitatory and inhibitory, respectively, the oculomotor pattern evoked by hyperventilation is the result of the interaction of these two factors. The data obtained allowed us to hypothesize an interpretative model regarding the pathogenetic aspects of responses evoked by hyperventilation and the etiologies of the disease: according to our hypotheses, the excitatory pattern implies a neuritic (viral) form of AUVP; instead, the inhibitory (and negative) one can be an expression of both the neuritic (viral) and vascular forms of the disease.
Full article

Figure 1
Open AccessArticle
Posterior Semicircular Canal Plugging Relieves Tumarkin’s Crisis in Ménière’s Disease Patients
by
Francesco Comacchio, Anna Bordin, Valerio Maria Di Pasquale Fiasca, Barbara Bellemo, Paola Magnavita, Elena Fasanaro and Elisabetta Poletto
Audiol. Res. 2024, 14(3), 432-441; https://doi.org/10.3390/audiolres14030036 - 9 May 2024
Abstract
►▼
Show Figures
(1) Background: Patients affected by Ménière’s disease can experience Tumarkin’s syndrome, which is characterized by postural instability, gait abnormalities, and, occasionally, an abrupt loss of balance known as vestibular drop attack or Tumarkin’s crisis. In this study, semicircular canal plugging is proposed as
[...] Read more.
(1) Background: Patients affected by Ménière’s disease can experience Tumarkin’s syndrome, which is characterized by postural instability, gait abnormalities, and, occasionally, an abrupt loss of balance known as vestibular drop attack or Tumarkin’s crisis. In this study, semicircular canal plugging is proposed as the definitive treatment for this condition. The outcomes of this type of surgery are discussed. (2) Methods: A total of 9 patients with a confirmed diagnosis of Ménière disease suffering from Tumarkin crisis underwent posterior semicircular canal plugging. These patients were assessed with Video Head Impulse Tests, vestibular evoked myogenic potentials, and Pure Tone Audiometry preoperatively and postoperatively. (3) Results: VHIT showed a postoperative decrease in PSC gain median (Preop. 0.86 and postop. 0.52; p < 0.009). No statistically significant differences were described for the anterior semicircular canal and the lateral semicircular canal. No patient experienced new Tumarkin crisis after the surgical treatment. (4) Conclusions: Our ten years of experience with posterior semicircular canal plugging in Ménière disease patients with Tumarkin’s syndrome has shown that this type of surgical procedure is successful in controlling Tumarkin’s crisis, with high patient satisfaction and little worsening in hearing level.
Full article

Figure 1
Open AccessReview
The Current State of Evidence Regarding Audiologist-Provided Cognitive Behavioural Therapy for the Management of Tinnitus: A Scoping Review
by
Louise A. Burke and Amr El Refaie
Audiol. Res. 2024, 14(3), 412-431; https://doi.org/10.3390/audiolres14030035 - 30 Apr 2024
Abstract
►▼
Show Figures
Background: Cognitive behavioural therapy (CBT) for tinnitus management is effective and widely recommended by national and international practice guidelines. However, all the evidence for CBT so far has come from Psychologist-led programs, and the potential role of Audiologists in providing CBT for tinnitus
[...] Read more.
Background: Cognitive behavioural therapy (CBT) for tinnitus management is effective and widely recommended by national and international practice guidelines. However, all the evidence for CBT so far has come from Psychologist-led programs, and the potential role of Audiologists in providing CBT for tinnitus remains an important consideration. Objectives: This study sets out to systematically map the body of literature relating to Audiologist-provided CBT for tinnitus, in order to summarise the current state of evidence and determine directions for future research. Eligibility criteria: Sources were eligible for inclusion if they addressed the concept of Audiologist-provided CBT. No restrictions were imposed on the date of publication. Only sources published in English were included. Sources of evidence: A wide range of primary and secondary literature sources were sought. Charting methods: Data from included sources were charted systematically using a pre-designed data charting form. Results: Of the 267 identified sources, 30 were included in this review. This included both primary and secondary literature sources. Primary sources were compared and showed variation across Audiologist-provided CBT programs both in terms of procedural details and from a research standpoint. Conclusions: A growing body of evidence has addressed the concept of Audiologist-provided CBT. Directions for future research include further primary research with an increased focus on face-to-face Audiologist-provided CBT, and a comparison of the outcomes of Audiologist-provided vs. Psychologist-provided CBT.
Full article
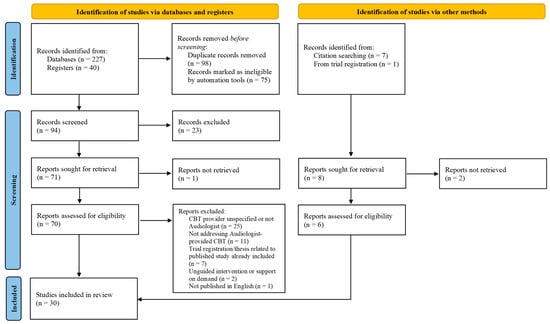
Figure 1
Open AccessArticle
Multi-Magnet Cochlear Implant Technology and Magnetic Resonance Imaging: The Safety Issue
by
Pietro Canzi, Elena Carlotto, Elisabetta Zanoletti, Johan H. M. Frijns, Daniele Borsetto, Antonio Caruso, Luisa Chiapparini, Andrea Ciorba, Giorgio Conte, Nathan Creber, Stefania Criscuolo, Filippo Di Lella, Sebastiano Franchella, Erik F. Hensen, Lorenzo Lauda, Stefano Malpede, Marco Mandalà, Liselotte J. C. Rotteveel, Anna Simoncelli, Anna Chiara Stellato, Diego Zanetti and Marco Benazzoadd
Show full author list
remove
Hide full author list
Audiol. Res. 2024, 14(3), 401-411; https://doi.org/10.3390/audiolres14030034 - 26 Apr 2024
Abstract
►▼
Show Figures
Despite the spread of novel-generation cochlear-implant (CI) magnetic systems, access to magnetic resonance imaging (MRI) for CI recipients is still limited due to safety concerns. The aim of this study is to assess and record the experiences of Hires Ultra 3D (Advanced Bionics)
[...] Read more.
Despite the spread of novel-generation cochlear-implant (CI) magnetic systems, access to magnetic resonance imaging (MRI) for CI recipients is still limited due to safety concerns. The aim of this study is to assess and record the experiences of Hires Ultra 3D (Advanced Bionics) recipients who underwent an MRI examination. A multicentric European survey about this topic was conducted focusing on safety issues, and the results were compared with the current literature. We collected a total of 65 MRI scans performed in 9 otologic referral centers for a total of 47 Hires Ultra 3D recipients, including, for the first time, 2 children and 3 teenagers. Preventive measures were represented by scanning time and sedation for children. Head wrapping was used in eight cases, and six of the eight cases received local anesthesia, even if both measures were not needed. Only three patients complained of pain (3/65 examinations, 4.6%) due to the tight head bandage, and one of the three cases required MRI scan interruption. No other adverse events were reported. We believe that these results should encourage MRI execution in accordance with manufacturer recommendations for Ultra 3D recipients.
Full article
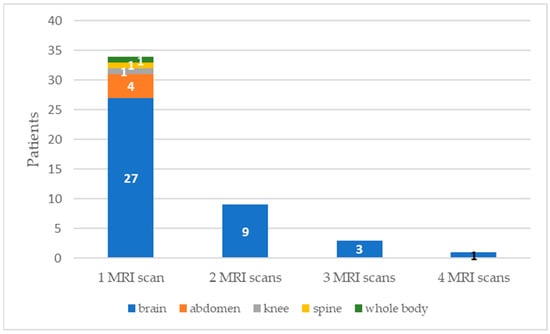
Figure 1
Open AccessArticle
Bone-Anchored Hearing Aid Effects on Vestibular Function: A Preliminary Report
by
Federica Pollastri, Beatrice Giannoni, Vincenzo Marcelli, Giulia Spadavecchia and Rudi Pecci
Audiol. Res. 2024, 14(2), 386-400; https://doi.org/10.3390/audiolres14020033 - 20 Apr 2024
Abstract
Objective: Cochlear receptors are sensitive to vibratory stimuli. Based on this sensibility, bone-anchored hearing aids have been introduced to correct unilateral or bilateral conductive or mixed hearing loss and unilateral deafness. The vestibular system is also sensitive to the vibratory stimulus and this
[...] Read more.
Objective: Cochlear receptors are sensitive to vibratory stimuli. Based on this sensibility, bone-anchored hearing aids have been introduced to correct unilateral or bilateral conductive or mixed hearing loss and unilateral deafness. The vestibular system is also sensitive to the vibratory stimulus and this type of response is used in clinics to test its functionality. Being aware of this double separated sensibility, we wondered whether bone vibration, which activates the acoustic receptors of patients with bone conduction aids, can also influence the functionality of the vestibular system. Methods: To this end, we recruited 12 patients with a bone-anchored hearing aid and evaluated their vestibular function with and without an activated vibratory acoustic device. Results: Our results show that the vibratory stimulus delivered by the bone conduction aid also reaches and stimulates the vestibular receptors; this stimulation is evidenced by the appearance or modification of some nystagmus findings during bedside vestibular testing. Despite this, none of these patients complained of dizziness or vertigo during prosthesis use. Nystagmus that appeared or changed during acoustic vibratory stimulation through the prosthesis was almost all predominantly horizontal, unidirectional with respect to gaze or body position, inhibited by fixation, and most often consistent with vestibular function tests indicating peripheral vestibular damage. Conclusions: The findings of sound-evoked nystagmus seem to indicate peripheral rather than central vestibular activation. The occurrence of some predominantly horizontal and high-frequency induced nystagmus seems to attribute the response mainly to the utricle and lateral semicircular canal.
Full article
Open AccessArticle
Otic Capsule Dehiscences Simulating Other Inner Ear Diseases: Characterization, Clinical Profile, and Follow-Up—Is Ménière’s Disease the Sole Cause of Vertigo and Fluctuating Hearing Loss?
by
Joan Lorente-Piera, Carlos Prieto-Matos, Raquel Manrique-Huarte, Octavio Garaycochea, Pablo Domínguez and Manuel Manrique
Audiol. Res. 2024, 14(2), 372-385; https://doi.org/10.3390/audiolres14020032 - 12 Apr 2024
Abstract
Introduction: We present a series of six cases whose clinical presentations exhibited audiovestibular manifestations of a third mobile window mechanism, bearing a reasonable resemblance to Ménière’s disease and otosclerosis. The occurrence of these cases in such a short period has prompted a review
[...] Read more.
Introduction: We present a series of six cases whose clinical presentations exhibited audiovestibular manifestations of a third mobile window mechanism, bearing a reasonable resemblance to Ménière’s disease and otosclerosis. The occurrence of these cases in such a short period has prompted a review of the underlying causes of its development. Understanding the pathophysiology of third mobile window syndrome and considering these entities in the differential diagnosis of conditions presenting with vertigo and hearing loss with slight air-bone gaps is essential for comprehending this group of pathologies. Materials and Methods: A descriptive retrospective cohort study of six cases diagnosed at a tertiary center. All of them went through auditive and vestibular examinations before and after a therapeutic strategy was performed. Results: Out of 84 cases of dehiscences described in our center during the period from 2014 to 2024, 78 belonged to superior semicircular canal dehiscence, while 6 were other otic capsule dehiscences. Among these six patients with a mean age of 47.17 years (range: 18–73), all had some form of otic capsule dehiscence with auditory and/or vestibular repercussions, measured through hearing and vestibular tests, with abnormalities in the results in five out of six patients. Two of them were diagnosed with Ménière’s disease (MD). Another two had cochleo-vestibular hydrops without meeting the diagnostic criteria for MD. In two cases, the otic capsule dehiscence diagnosis resulted from an intraoperative complication due to a gusher phenomenon, while in one case, it was an accidental radiological finding. All responded well to the proposed treatment, whether medical or surgical, if needed. Conclusions: Otic capsule dehiscences are relatively new and unfamiliar entities that should be considered when faced with cases clinically suggestive of Ménière’s disease, with discrepancies in complementary tests or a poor response to treatment. While high-sensitivity and specificity audiovestibular tests exist, completing the study with imaging, especially petrous bone CT scans, is necessary to locate and characterize the otic capsule defect responsible for the clinical presentation.
Full article
(This article belongs to the Special Issue Third Mobile Window Syndromes: New Insights in Pathomechanisms, Instrumental Diagnosis and Surgical Treatment)
►▼
Show Figures
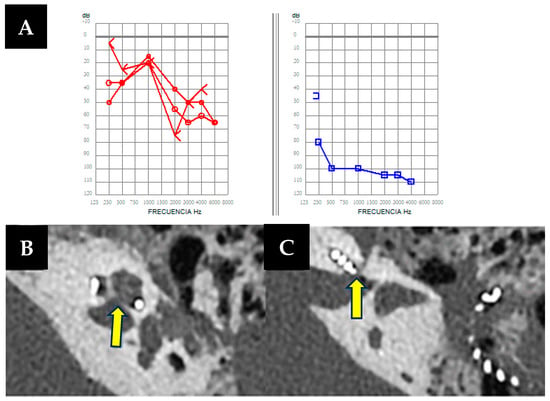
Figure 1
Open AccessArticle
AUDISTIM® Day/Night Alleviates Tinnitus-Related Handicap in Patients with Chronic Tinnitus: A Double-Blind Randomized Placebo-Controlled Trial
by
Didier Portmann, Marie José Esteve-Fraysse, Bruno Frachet, Florent Herpin, Florian Rigaudier and Christine Juhel
Audiol. Res. 2024, 14(2), 359-371; https://doi.org/10.3390/audiolres14020031 - 10 Apr 2024
Abstract
►▼
Show Figures
The aim of this study is to evaluate the efficacy of taking a daily supplement based on active compounds (AUDISTIM® Day Night: A D/N) in alleviating tinnitus-related disability, as suggested by previous real-life studies. This double-blind randomized placebo-controlled study was conducted in
[...] Read more.
The aim of this study is to evaluate the efficacy of taking a daily supplement based on active compounds (AUDISTIM® Day Night: A D/N) in alleviating tinnitus-related disability, as suggested by previous real-life studies. This double-blind randomized placebo-controlled study was conducted in adults with mild to severe tinnitus receiving a 3-month supplementation with A D/N (magnesium, vitamins, phytochemicals) or placebo (excipients without active ingredients). Tinnitus-related handicap (THI), psychological stress (MSP-9), and sleep quality (PSQI) were assessed at baseline and during intervention, perceived impression of tinnitus improvement at the end of the follow-up. The full set analysis included 114 patients (59 A D/N, 55 placebo) aged 53.8 ± 11.4 years, 58% women, with fluctuating (45%) or permanent (55%) tinnitus from 9.3 ± 9.4 years. A D/N supplementation led to greater changes in THI (−13.2 ± 16.0 vs. −6.2 ± 14.4, p = 0.0158, Cohen’s d = 0.44) at 3 months (primary outcome), especially with continuous tinnitus (−15.0 ± 16.3 vs. −4.6 ± 12.8, p = 0.0065), and, to a lesser extent, at 1 month (−9.8 ± 13.1 for A vs. −4.3 ± 12.1, p = 0.0213). PSQI significantly improved over time in both groups, but MSP-9 only with A D/N. In lines with previous observational studies, both clinical (THI score > 7 pts) and statistical (vs. placebo) improvement, more pronounced in permanent tinnitus, demonstrate the effectiveness of the combination of active compounds and support its use in the management of mild to severe tinnitus.
Full article
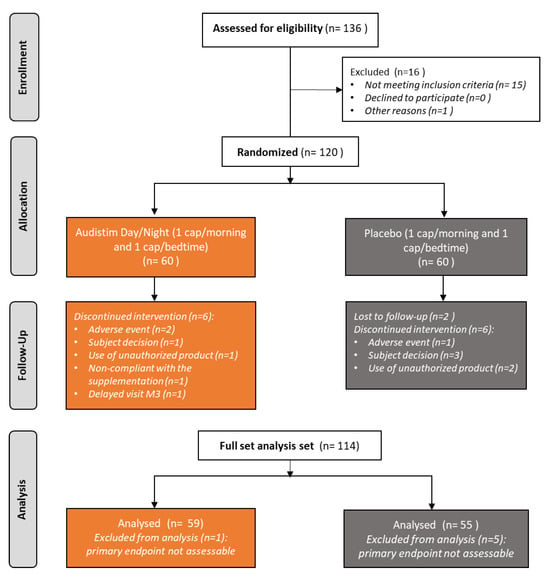
Figure 1
Open AccessArticle
Digits-in-Noise Test as an Assessment Tool for Hearing Loss and Hearing Aids
by
Carly Schimmel, Kayla Cormier, Vinaya Manchaiah, De Wet Swanepoel and Anu Sharma
Audiol. Res. 2024, 14(2), 342-358; https://doi.org/10.3390/audiolres14020030 - 8 Apr 2024
Abstract
►▼
Show Figures
The aim of this study was to examine the relationship between an American English Digits in Noise (DIN) test and commonly used audiological measures to evaluate the DIN test’s ability to detect hearing loss and validate hearing aid fitting. QuickSIN and DIN tests
[...] Read more.
The aim of this study was to examine the relationship between an American English Digits in Noise (DIN) test and commonly used audiological measures to evaluate the DIN test’s ability to detect hearing loss and validate hearing aid fitting. QuickSIN and DIN tests were completed by participants with untreated hearing loss (n = 46), prescription hearing aids (n = 15), and over-the-counter (OTC) hearing aids (n = 12). Performance on the QuickSIN showed moderate positive correlations with DIN for untreated hearing loss participants and prescription hearing aid users, but not for OTC hearing aid users. For untreated hearing loss participants, both QuickSIN and DIN tests showed positive moderate to strong correlations with high frequency puretone averages. In OTC users, DIN scores did not significantly change over a 6-month time period and were better when conducted remotely compared to in-person testing. Our results suggest that the DIN test may be a feasible monitoring option for individuals with hearing loss and those fitted with hearing aids. However, due to small sample size in this pilot study, future research is needed to examine DIN test’s utility for fitting and validating OTC hearing aids.
Full article
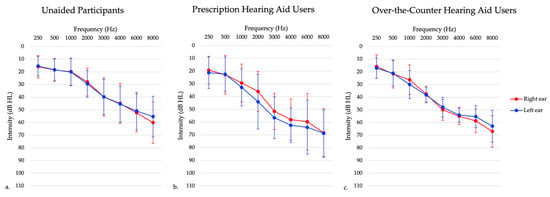
Figure 1
Open AccessArticle
Assessing the Effectiveness of Different Hyperbaric Oxygen Treatment Methods in Patients with Sudden Sensorineural Hearing Loss
by
Paweł Rozbicki, Jacek Usowski, Sandra Krzywdzińska, Dariusz Jurkiewicz and Jacek Siewiera
Audiol. Res. 2024, 14(2), 333-341; https://doi.org/10.3390/audiolres14020029 - 29 Mar 2024
Abstract
Introduction: Hyperbaric oxygen therapy (HBOT) is one of the treatment methods in patients with sudden sensorineural hearing loss (SSNHL). It is recommended as an elective treatment in patients undergoing steroid therapy. According to current scientific reports, HBOT should be implemented within two weeks
[...] Read more.
Introduction: Hyperbaric oxygen therapy (HBOT) is one of the treatment methods in patients with sudden sensorineural hearing loss (SSNHL). It is recommended as an elective treatment in patients undergoing steroid therapy. According to current scientific reports, HBOT should be implemented within two weeks after the first symptoms. However, as far as the profile of HBOT is concerned, there are no straightforward recommendations. Methods: The data obtained from the medical records of 218 patients undergoing HBOT for SSNHL at the Military Institute of Medicine—National Research Institute were analyzed statistically for the impact of the duration and the delay in implementing HBOT on the end results of pure-tone audiometry (PTA). Results: A statistically significant hearing improvement in patients undergoing more than 15 cycles of HBOT was detected at all frequencies except for 1500 Hz; in the group reporting for treatment with a delay of more than 10 days, hearing improvement was statistically unsignificant at frequencies of 1500, 3000, and 4000 Hz. Conclusions: The statistical analysis showed that the urgent onset of HBOT could be a significant factor in the therapy of SSNHL.
Full article
(This article belongs to the Special Issue Hearing Loss: Causes, Symptoms, Diagnosis, and Treatment)
Open AccessArticle
Posterior Semicircular Canal Dehiscence with Vestibulo-Ocular Reflex Reduction for the Affected Canal at the Video-Head Impulse Test: Considerations to Pathomechanisms
by
Andrea Castellucci, Georges Dumas, Sawsan M. Abuzaid, Enrico Armato, Salvatore Martellucci, Pasquale Malara, Mohamad Alfarghal, Rosanna Rita Ruberto, Pasquale Brizzi, Angelo Ghidini, Francesco Comacchio and Sébastien Schmerber
Audiol. Res. 2024, 14(2), 317-332; https://doi.org/10.3390/audiolres14020028 - 24 Mar 2024
Abstract
►▼
Show Figures
Posterior semicircular canal dehiscence (PSCD) has been demonstrated to result in a third mobile window mechanism (TMWM) in the inner ear similar to superior semicircular canal dehiscence (SSCD). Typical clinical and instrumental features of TMWM, including low-frequency conductive hearing loss (CHL), autophony, pulsatile
[...] Read more.
Posterior semicircular canal dehiscence (PSCD) has been demonstrated to result in a third mobile window mechanism (TMWM) in the inner ear similar to superior semicircular canal dehiscence (SSCD). Typical clinical and instrumental features of TMWM, including low-frequency conductive hearing loss (CHL), autophony, pulsatile tinnitus, sound/pressure-induced vertigo and enhanced vestibular-evoked myogenic potentials, have been widely described in cases with PSCD. Nevertheless, video-head impulse test (vHIT) results have been poorly investigated. Here, we present six patients with PSCD presenting with a clinical scenario consistent with a TMWM and an impaired vestibulo-ocular reflex (VOR) for the affected canal on vHIT. In two cases, an additional dehiscence between the facial nerve and the horizontal semicircular canal (HSC) was detected, leading to a concurrent VOR impairment for the HSC. While in SSCD, a VOR gain reduction could be ascribed to a spontaneous “auto-plugging” process due to a dural prolapse into the canal, the same pathomechanism is difficult to conceive in PSCD due to a different anatomical position, making a dural herniation less likely. Alternative putative pathomechanisms are discussed, including an endolymphatic flow dissipation during head impulses as already hypothesized in SSCD. The association of symptoms/signs consistent with TMWM and a reduced VOR gain for the posterior canal might address the diagnosis toward PSCD.
Full article
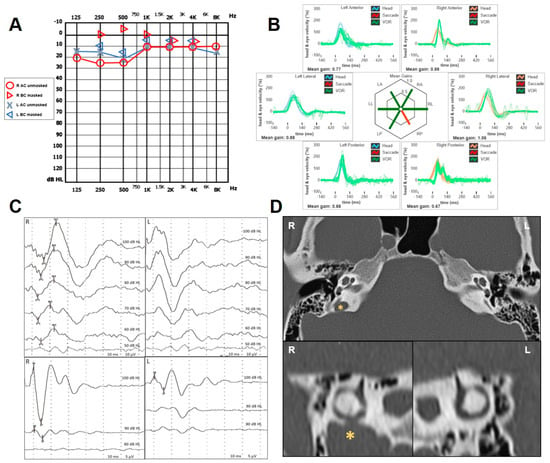
Figure 1
Open AccessArticle
Large Vestibular Aqueduct-Associated Symptoms: Endolymphatic Duct Blockage as a Surgical Treatment
by
Issam Saliba, Sarah Alshehri, Isabelle Fournier and Nasser Altamami
Audiol. Res. 2024, 14(2), 304-316; https://doi.org/10.3390/audiolres14020027 - 18 Mar 2024
Abstract
►▼
Show Figures
Objective: This study aimed to evaluate the effectiveness of endolymphatic duct blockage (EDB) on dizziness control in patients with a large vestibular aqueduct (LVA) and to evaluate its effect on hearing. Study design: This is a prospective nonrandomized study. Setting: Five adults and
[...] Read more.
Objective: This study aimed to evaluate the effectiveness of endolymphatic duct blockage (EDB) on dizziness control in patients with a large vestibular aqueduct (LVA) and to evaluate its effect on hearing. Study design: This is a prospective nonrandomized study. Setting: Five adults and one child with dizziness and five children with progressive hearing loss were referred to our tertiary centers. Methods: The dizziness handicap inventory (DHI) and DHI-PC (dizziness handicap inventory—patient caregiver) questionnaires were used before and after surgery. All patients underwent a preoperative temporal bone HRCT scan and pure tone audiometry one day before surgery, then four and twelve months after surgery and at the last follow-up. The mean follow-up time was 5.6 years. Student’s t-test was used to compare DHI/-PC results. Results: The DHI scores were 44, 24, 84, 59 and 56 before surgery, respectively, for Patients 1 to 5. The DHI scores at four months was significantly different, i.e., 4, 6, 0, 7 and 18 (p = 0.001). No differences were found between 4 and 12 months. Patient 6 (child) had Trisomy 21; their DHI-PC score dropped from 38 (preoperative score) to 8 (postoperative score), showing no activity limitations; clinical evaluation showed the complete resolution of symptoms. We found no significant differences between hearing loss before the surgery and at 1 and 12 months post operation for four adult patients. Our fifth adult patient’s hearing changed from severe to profound SNHL. For 5 out of 6 pediatric patients, preoperative PTA and mean ABG were 63 dB and 20 dB, respectively; postoperatively, they improved to 42 dB and 16 dB, respectively. The hearing loss level for the sixth pediatric patient dropped from moderate (PTA = 42 dB) to severe (PTA = 85 dB) due to an opening of the endolymphatic sac and a sudden leak of the endolymph. Conclusions: EDB, using two titanium clips, seems to be helpful for controlling vestibular symptoms and for stabilizing hearing or even to improve hearing in 82% of cases. Nevertheless, there is a risk of hearing worsening.
Full article

Figure 1
Open AccessArticle
Over-the-Counter (OTC) Hearing Aid Availability across the Spectrum of Human Skin Colors
by
Shade Avery Kirjava and Sam Jones Faulkner
Audiol. Res. 2024, 14(2), 293-303; https://doi.org/10.3390/audiolres14020026 - 12 Mar 2024
Abstract
Background: Over-the-counter (OTC) hearing aids were recently approved for sale in the United States. Research has shown that consumers prefer hearing devices that match their skin color because these devices are less noticeable. Colorism is discrimination against individuals with relatively darker skin that
[...] Read more.
Background: Over-the-counter (OTC) hearing aids were recently approved for sale in the United States. Research has shown that consumers prefer hearing devices that match their skin color because these devices are less noticeable. Colorism is discrimination against individuals with relatively darker skin that manifests in “skin-color” product offerings as products being offered primarily in relatively lighter colors. Methods: This study compared images of U.S. Food and Drug Administration (FDA)-registered over-the-counter hearing aids to a range of human skin colors. Results: Most over-the-counter hearing aids are only offered in relatively lighter beige colors. Few over-the-counter hearing aids are available in darker skin colors. Conclusions: These findings may represent structural bias, preventing equitable access to darker skin-color OTC hearing aids for individuals with darker skin.
Full article
(This article belongs to the Special Issue Hearing Loss: Causes, Symptoms, Diagnosis, and Treatment)
►▼
Show Figures
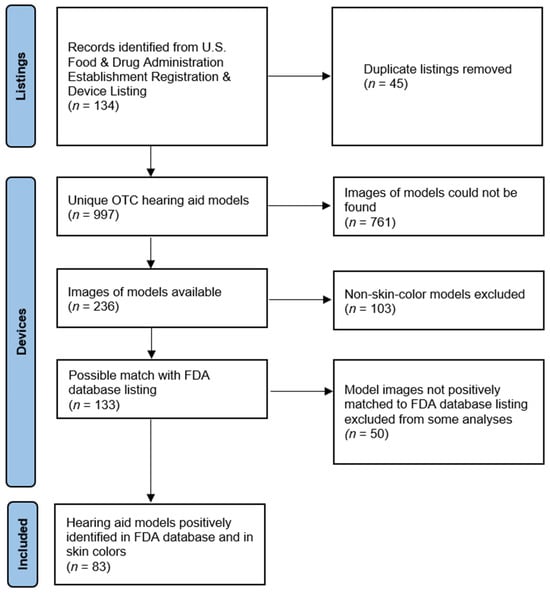
Figure 1
Open AccessArticle
Renewed Concept of Mastoid Cavity Obliteration with the Use of Temporoparietal Fascial Flap Injected by Injectable Platelet-Rich Fibrin after Subtotal Petrosectomy for Cochlear Implant Patients
by
Aleksander Zwierz, Krystyna Masna, Paweł Burduk, Stephan Hackenberg and Matthias Scheich
Audiol. Res. 2024, 14(2), 280-292; https://doi.org/10.3390/audiolres14020025 - 1 Mar 2024
Abstract
Background: The subtotal petrosectomy procedure may be useful for cochlear implantation in selected patient groups. Although it is highly effective, complications can arise, which may have economic implications for the patient due to the high cost of the device. Therefore, several authors have
[...] Read more.
Background: The subtotal petrosectomy procedure may be useful for cochlear implantation in selected patient groups. Although it is highly effective, complications can arise, which may have economic implications for the patient due to the high cost of the device. Therefore, several authors have attempted to identify the most effective concept for obliteration. Methods: We present a pilot descriptive study of application techniques for obliterating cavities after subtotal petrosectomy using a temporoparietal fascial flap (TPFF) modified with injectable platelet-rich fibrin (IPRF+) for three cochlear implant (CI) patients. Results: Our concept preserves important anatomical structures, such as the temporalis muscle, which covers the CI receiver–stimulator. Injection of IPRF+ also increases the available tissue volume for obliteration and enhances its anti-inflammatory and regenerative potential. Conclusions: To the best of our knowledge, the use of TPFF for filling the cavity has not been adopted for CI with SP and for blind sac closure. Our literature review and our experience with this small group of patients suggest that this procedure, when combined with IPRF+ injections, may reduce the risk of potential infection in the obliterated cavity, particularly when used with CI. This technique is applicable only in cases when the surgeons are convinced that the middle ear cavity is purged of cholesteatoma.
Full article
(This article belongs to the Special Issue Hearing Loss: Causes, Symptoms, Diagnosis, and Treatment)
►▼
Show Figures
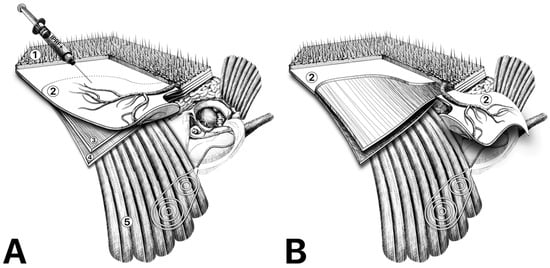
Figure 1
Open AccessArticle
Development of New Open-Set Speech Material for Use in Clinical Audiology with Speakers of British English
by
Mahmoud Keshavarzi, Marina Salorio-Corbetto, Tobias Reichenbach, Josephine Marriage and Brian C. J. Moore
Audiol. Res. 2024, 14(2), 264-279; https://doi.org/10.3390/audiolres14020024 - 26 Feb 2024
Abstract
Background: The Chear open-set performance test (COPT), which uses a carrier phrase followed by a monosyllabic test word, is intended for clinical assessment of speech recognition, evaluation of hearing-device performance, and the fine-tuning of hearing devices for speakers of British English. This paper
[...] Read more.
Background: The Chear open-set performance test (COPT), which uses a carrier phrase followed by a monosyllabic test word, is intended for clinical assessment of speech recognition, evaluation of hearing-device performance, and the fine-tuning of hearing devices for speakers of British English. This paper assesses practice effects, test–retest reliability, and the variability across lists of the COPT. Method: In experiment 1, 16 normal-hearing participants were tested using an initial version of the COPT, at three speech-to-noise ratios (SNRs). Experiment 2 used revised COPT lists, with items swapped between lists to reduce differences in difficulty across lists. In experiment 3, test–retest repeatability was assessed for stimuli presented in quiet, using 15 participants with sensorineural hearing loss. Results: After administration of a single practice list, no practice effects were evident. The critical difference between scores for two lists was about 2 words (out of 15) or 5 phonemes (out of 50). The mean estimated SNR required for 74% words correct was −0.56 dB, with a standard deviation across lists of 0.16 dB. For the participants with hearing loss tested in quiet, the critical difference between scores for two lists was about 3 words (out of 15) or 6 phonemes (out of 50).
Full article
(This article belongs to the Special Issue Rehabilitation of Hearing Impairment: 2nd Edition)
►▼
Show Figures
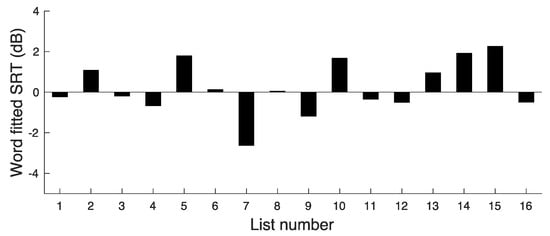
Figure 1
Open AccessReview
Navigating the Usher Syndrome Genetic Landscape: An Evaluation of the Associations between Specific Genes and Quality Categories of Cochlear Implant Outcomes
by
Micol Busi and Alessandro Castiglione
Audiol. Res. 2024, 14(2), 254-263; https://doi.org/10.3390/audiolres14020023 - 26 Feb 2024
Abstract
Usher syndrome (US) is a clinically and genetically heterogeneous disorder that involves three main features: sensorineural hearing loss, retinitis pigmentosa (RP), and vestibular impairment. With a prevalence of 4–17/100,000, it is the most common cause of deaf-blindness worldwide. Genetic research has provided crucial
[...] Read more.
Usher syndrome (US) is a clinically and genetically heterogeneous disorder that involves three main features: sensorineural hearing loss, retinitis pigmentosa (RP), and vestibular impairment. With a prevalence of 4–17/100,000, it is the most common cause of deaf-blindness worldwide. Genetic research has provided crucial insights into the complexity of US. Among nine confirmed causative genes, MYO7A and USH2A are major players in US types 1 and 2, respectively, whereas CRLN1 is the sole confirmed gene associated with type 3. Variants in these genes also contribute to isolated forms of hearing loss and RP, indicating intersecting molecular pathways. While hearing loss can be adequately managed with hearing aids or cochlear implants (CIs), approved RP treatment modalities are lacking. Gene replacement and editing, antisense oligonucleotides, and small-molecule drugs hold promise for halting RP progression and restoring vision, enhancing patients’ quality of life. Massively parallel sequencing has identified gene variants (e.g., in PCDH15) that influence CI results. Accordingly, preoperative genetic examination appears valuable for predicting CI success. To explore genetic mutations in CI recipients and establish correlations between implant outcomes and involved genes, we comprehensively reviewed the literature to gather data covering a broad spectrum of CI outcomes across all known US-causative genes. Implant outcomes were categorized as excellent or very good, good, poor or fair, and very poor. Our review of 95 cochlear-implant patients with US, along with their CI outcomes, revealed the importance of presurgical genetic testing to elucidate potential challenges and provide tailored counseling to improve auditory outcomes. The multifaceted nature of US demands a comprehensive understanding and innovative interventions. Genetic insights drive therapeutic advancements, offering potential remedies for the retinal component of US. The synergy between genetics and therapeutics holds promise for individuals with US and may enhance their sensory experiences through customized interventions.
Full article
(This article belongs to the Special Issue Genetics of Hearing Loss—Volume II)

Journal Menu
► ▼ Journal Menu-
- Audiology Research Home
- Aims & Scope
- Editorial Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Topical Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Audiology Research
The Vestibular System: Physiology and Testing Methods
Guest Editors: Giacinto Asprella Libonati, Herman Kingma, Vito Enrico PettorossiDeadline: 30 June 2024
Special Issue in
Audiology Research
Third Mobile Window Syndromes: New Insights in Pathomechanisms, Instrumental Diagnosis and Surgical Treatment
Guest Editors: Andrea Castellucci, Bryan Kevin Ward, Raymond Van De Berg, Leonardo ManzariDeadline: 31 July 2024
Special Issue in
Audiology Research
Inner Ear Conductive Hearing Loss: Current Studies and Controversies
Guest Editors: Andrea Castellucci, Eduardo Martin Sanz, Soumit Dasgupta, Issam SalibaDeadline: 31 August 2024
Special Issue in
Audiology Research
A Tribute to John M. Epley
Guest Editors: Giacinto Asprella Libonati, Gerard Gianoli, Meiho NakayamaDeadline: 31 December 2024
Topical Collections
Topical Collection in
Audiology Research
Cochlear Implants: Challenges and Opportunities in Hearing Rehabilitation
Collection Editors: Andrea Ciorba, Daniele Borsetto
Topical Collection in
Audiology Research
Translational Audiology
Collection Editor: Agnieszka Szczepek




