-
 Implementation of a Multicomponent Otago-Based Virtual Fall Reduction, Education, and Exercise Program (MOVing FREEly) in Older Veterans
Implementation of a Multicomponent Otago-Based Virtual Fall Reduction, Education, and Exercise Program (MOVing FREEly) in Older Veterans -
 The Influence of Physical, Mental, and Cognitive Factors on Health-Related Quality of Life among Community-Dwelling Older Adults: A Focus on Central Sensitization-Related Symptoms
The Influence of Physical, Mental, and Cognitive Factors on Health-Related Quality of Life among Community-Dwelling Older Adults: A Focus on Central Sensitization-Related Symptoms -
 Perceptions of Patients, Caregivers, and Healthcare Professionals toward Telemedicine Use for Cognitive and Movement Disorders in the Aegean Islands, Greece
Perceptions of Patients, Caregivers, and Healthcare Professionals toward Telemedicine Use for Cognitive and Movement Disorders in the Aegean Islands, Greece
Journal Description
Geriatrics
Geriatrics
is an international, peer-reviewed, scientific open access journal on geriatric medicine published bimonthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, and other databases.
- Journal Rank: CiteScore - Q2 (Health (social science))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 22.4 days after submission; acceptance to publication is undertaken in 2.9 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Testimonials: See what our editors and authors say about Geriatrics.
Impact Factor:
2.3 (2022);
5-Year Impact Factor:
2.5 (2022)
Latest Articles
Effectiveness of Non-Pharmacological Interventions for Dementia among the Elderly: A Randomized Controlled Trial
Geriatrics 2024, 9(2), 52; https://doi.org/10.3390/geriatrics9020052 - 18 Apr 2024
Abstract
(1) Background: Up until now, there is still no medicine that can cure dementia, but there are some that can only help slow down the progression of the disease and reduce some symptoms. Pharmacological interventions for dementia have many side effects and are
[...] Read more.
(1) Background: Up until now, there is still no medicine that can cure dementia, but there are some that can only help slow down the progression of the disease and reduce some symptoms. Pharmacological interventions for dementia have many side effects and are expensive, so non-pharmacological treatments for dementia become more urgent. This study aimed to evaluate the effectiveness of multifactorial non-pharmacological interventions in dementia patients; (2) Methods: This is a randomized controlled trial conducted in Hai Duong from July 2021 to December 2022. Selected subjects included 88 patients diagnosed with very mild, mild, and moderate dementia, of whom 44 patients were assigned to the intervention group and 44 patients to the control group; (3) Results: For the effectiveness of the non-pharmacological multifactorial intervention on depression severity: in the intervention group, the GDS 15 depression score decreased from 4.8 to 2.9, while, in the control group, the GDS 15 depression score increased by 1.3 points after six months of no intervention. For the effect of the non-pharmacological multifactorial intervention on the level of sleep disturbance, in the intervention group, the PSQI sleep disturbance score decreased by nearly half (from 10.2 to 5.6), while, in the control group, this trend was not clear. For the effect of the non-pharmacological multifactorial intervention on daily functioning: in the intervention group, the ADL and IADL scores improved (1.02 ± 1.32 and 1.23 ± 1.75), while, in the control group, the ADL and IADL scores decreased (0.93 ± 1.2 and 0.98 ± 2.19). For the effect of the non-pharmacological multifactorial intervention on quality of life: in the intervention group, the EQ-5D-5L scores improved (0.17 ± 0.19), while, in the control group, the EQ-5D-5L scores decreased (0.20 ± 0.30); (4) Conclusions: Non-pharmacological multifactorial interventions, including physical activity, cognitive training, listening to educational lectures, and organizing miniature social models, have been shown to improve mental health, self-control, and quality of life.
Full article
(This article belongs to the Section Geriatric Public Health)
Open AccessSystematic Review
Pharmacological Treatment for Terminal Agitation, Delirium and Anxiety in Frail Older Patients
by
Dine A. D. Jennes, Tim Biesbrouck, Maaike L. De Roo, Tinne Smets and Nele Van Den Noortgate
Geriatrics 2024, 9(2), 51; https://doi.org/10.3390/geriatrics9020051 - 18 Apr 2024
Abstract
Context: Psychological distress symptoms in the last days of life often contribute to the overall symptom burden in frail older patients. Good symptom management practices are crucial to ensure high-quality end-of-life care in an aging population, though the best pharmacological approach to treat
[...] Read more.
Context: Psychological distress symptoms in the last days of life often contribute to the overall symptom burden in frail older patients. Good symptom management practices are crucial to ensure high-quality end-of-life care in an aging population, though the best pharmacological approach to treat these psychological symptoms has yet to be established. Objectives: To identify current evidence-based and practice-based knowledge of pharmacological interventions for the treatment of agitation, delirium, and anxiety during the last days of life in frail older patients. Methods: A systematic, mixed methods review was performed through MEDLINE via PubMed and EMBASE from inception until February 2022 and updated through March 2023. National and international guideline databases and grey literature were searched for additional studies and guidelines. Results: Four quantitative studies, two non-randomized and two descriptive, were identified. No randomized controlled trials met inclusion criteria. No qualitative studies were withheld. The three consensus-based protocols that were found through citation searching and screening of grey literature did not meet the standards for inclusion. Haloperidol is recommended in consensus-based guidelines for delirium and is widely used, but high-quality evidence about its efficacy is missing. Better control of agitation or refractory delirium might be achieved with the addition of a benzodiazepine. There is no evidence available about the treatment of anxiety in the last days of life in frail older patients. Conclusions: This mixed methods review demonstrates the lack of good quality evidence that is needed to help clinicians with pharmacological treatment decisions when confronted with psychological symptoms in the last days of life in frail older patients. Population aging will only emphasize the need for further research in this specific population.
Full article
(This article belongs to the Special Issue Enriching Lives: Palliative Care in Geriatrics)
►▼
Show Figures
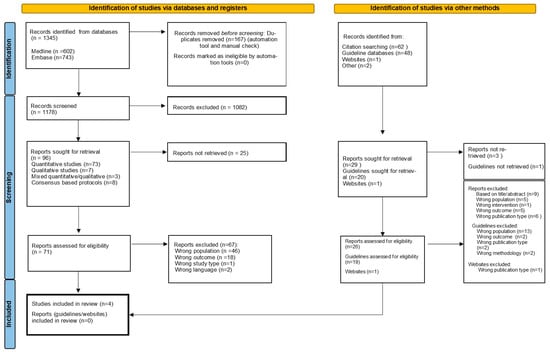
Figure 1
Open AccessReview
Assessment and Management of Atrial Fibrillation in Older Adults with Frailty
by
Andrea Nathalie Rosas Diaz, Aaron L. Troy, Vladimir Kaplinskiy, Abiah Pritchard, Rati Vani, Darae Ko and Ariela R. Orkaby
Geriatrics 2024, 9(2), 50; https://doi.org/10.3390/geriatrics9020050 - 15 Apr 2024
Abstract
Atrial fibrillation (AF) is a major driver of morbidity and mortality among older adults with frailty. Moreover, frailty is highly prevalent in older adults with AF. Understanding and addressing the needs of frail older adults with AF is imperative to guide clinicians caring
[...] Read more.
Atrial fibrillation (AF) is a major driver of morbidity and mortality among older adults with frailty. Moreover, frailty is highly prevalent in older adults with AF. Understanding and addressing the needs of frail older adults with AF is imperative to guide clinicians caring for older adults. In this review, we summarize current evidence to support the assessment and management of older adults with AF and frailty, incorporating numerous recent landmark trials and studies in the context of the 2023 US AF guideline.
Full article
(This article belongs to the Section Cardiogeriatrics)
►▼
Show Figures
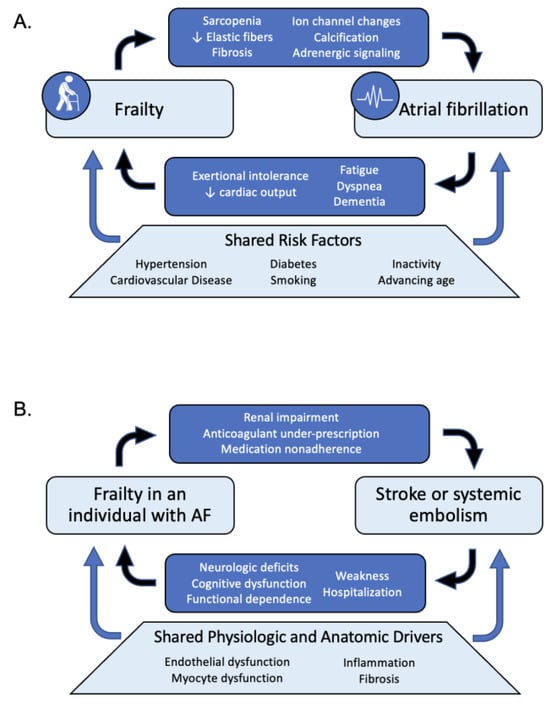
Figure 1
Open AccessArticle
Qualities of Older Adults’ Family and Friendship Relationships and Their Association with Life Satisfaction
by
Elias Mpofu, Rong-Fang Zhan, Cheng Yin and Kaye Brock
Geriatrics 2024, 9(2), 49; https://doi.org/10.3390/geriatrics9020049 - 10 Apr 2024
Abstract
While family and friendship relationship qualities are associated with life satisfaction, evidence on how these types of relationships interact to contribute to older adults’ life satisfaction is sparse. This study examined how family and friendship relationship qualities may be supportive of (compensatory) or
[...] Read more.
While family and friendship relationship qualities are associated with life satisfaction, evidence on how these types of relationships interact to contribute to older adults’ life satisfaction is sparse. This study examined how family and friendship relationship qualities may be supportive of (compensatory) or conflict with (competing) older adults’ life satisfaction. We adopted a cross-sectional design to analyze data from the Health and Retirement Study (n = 1178, females = 54.8%, mean age = 67.9 years, SD = 9.3 years) to examine compensatory (as in social support) and competing (as in social strain) qualities of family and friendship social relationships and their association with life satisfaction in older adults. For greater explanatory power, we also controlled for life satisfaction by sociodemographic variables of age, gender, education, self-reported general health, physical health and activity, depression, and personality traits. Our findings indicate that the spouse/partner support relationship contributes to older adults’ life satisfaction overall and is associated with greater social support and less social strain. Friendship support is associated with improved life satisfaction for older adults reporting spouse/partner strain. Relationship support for the life satisfaction of older adults should consider their need for social support from their social network while minimizing the risk of social strain from adversarial relationships in life situations.
Full article
(This article belongs to the Section Healthy Aging)
►▼
Show Figures
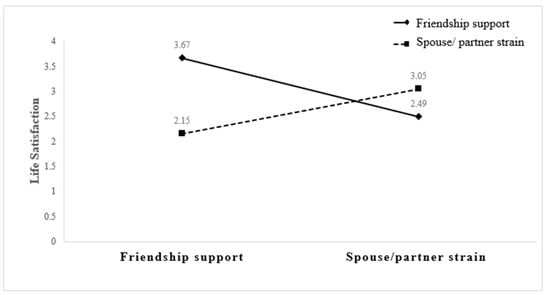
Figure 1
Open AccessArticle
Assessing Adhesiveness Levels in a Dysphagia Diet for Older Adults
by
Tae-Heon Lee and Jin-Woo Park
Geriatrics 2024, 9(2), 48; https://doi.org/10.3390/geriatrics9020048 - 09 Apr 2024
Abstract
Background: Viscosity is a common focus in the diet of patients with dysphagia. However, adhesiveness is an equally significant property that can affect swallowing function, even in semi-solid foods with similar levels of viscosity. The purpose of this study was to classify the
[...] Read more.
Background: Viscosity is a common focus in the diet of patients with dysphagia. However, adhesiveness is an equally significant property that can affect swallowing function, even in semi-solid foods with similar levels of viscosity. The purpose of this study was to classify the adhesiveness of food into stages and determine whether these classifications are relevant to swallowing function. Methods: This study included 30 healthy elderly adults aged 65 years. After categorizing adhesiveness into three levels based on the results of the sensory test, 30 participants were asked to swallow representative foods at each level. A videofluoroscopic swallowing study (VFSS) was performed to determine the presence or absence of pharyngeal residues based on the level of adhesiveness. The chi-square test was used to verify whether there was a difference in remnants according to the level of adhesiveness, and significance was judged with a p-value of less than 0.05. Results: Adhesiveness was categorized into three distinct levels: level 1 (0–4 mJ), level 2 (4–18 mJ), and level 3 (>18 mJ). Upon examining the subjects presenting with residual material, we observed three cases of level 1 adhesiveness, 16 cases of level 2, and 25 cases of level 3. The chi-square test was used to assess the statistical significance between the levels, revealing a significant difference with a p-value < 0.0001. Conclusions: We presented the level of adhesiveness by dividing it into three stages and proved that it is meaningful in relation to the swallowing function. Selecting and recommending foods with an appropriate level of adhesiveness will help enhance swallowing safety in older adults.
Full article
(This article belongs to the Section Dysphagia)
►▼
Show Figures
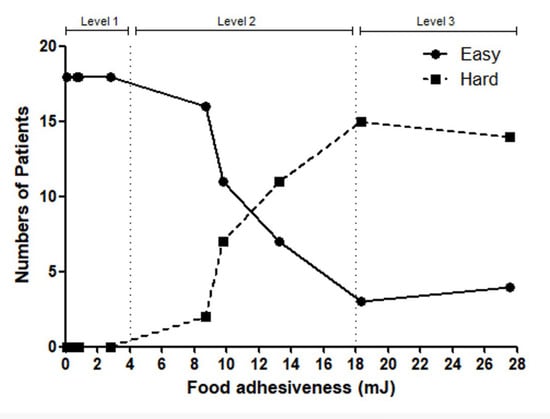
Figure 1
Open AccessArticle
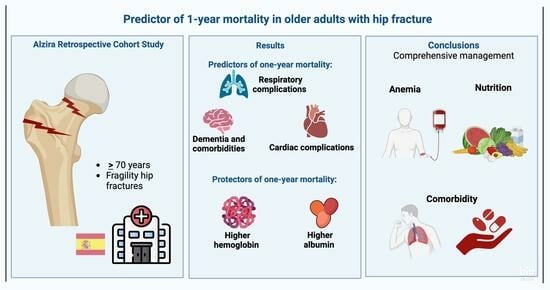
Respiratory Complications Are the Main Predictors of 1-Year Mortality in Patients with Hip Fractures: The Results from the Alzira Retrospective Cohort Study
by
Elisa García-Tercero, Ángel Belenguer-Varea, Daniela Villalon-Ruibio, Jesús López Gómez, Rodrigo Trigo-Suarez, Cristina Cunha-Pérez, Miguel Germán Borda and Francisco Jose Tarazona-Santabalbina
Geriatrics 2024, 9(2), 47; https://doi.org/10.3390/geriatrics9020047 - 09 Apr 2024
Abstract
Introduction: Hip fractures pose a significant challenge for older individuals given their high incidence and one-year mortality rate. The objective of this study was to identify the primary predictors of one-year mortality in older adults hospitalized for hip fractures. Methods: We conducted
[...] Read more.
Introduction: Hip fractures pose a significant challenge for older individuals given their high incidence and one-year mortality rate. The objective of this study was to identify the primary predictors of one-year mortality in older adults hospitalized for hip fractures. Methods: We conducted a retrospective cohort study involving adults aged 70 years or older who were admitted to the hospital for fragility hip fractures between 1 January 2014 and 31 December 2021. A total of 3229 patients were recruited, with 846 (26.2%) experiencing one-year mortality. Results: Respiratory complications (HR 2.42, 95%CI 1.42–4.14; p = 0.001) were the most significant predictors of one-year mortality, followed by hospital readmission (HR 1.96, 95%CI 1.66–2.32; p < 0.001), the male sex (HR 1.88, 95%CI 1.46–2.32; p < 0.001), cardiac complications (HR 1.88, 95%CI 1.46–2.32; p < 0.001), and a diagnosis of dementia at admission (HR 1.37, 95%CI 1.13–1.66; p = 0.001). The Charlson Index and the American Society of Anesthesiologists physical status classification system also significantly increased the mortality risk. Conversely, higher hemoglobin levels at admission and elevated albumin at discharge significantly reduced the mortality risk. Conclusions: The one-year mortality rate is substantial in older adults with hip fractures who are admitted to an orthogeriatric unit. The appropriate management of anemia, nutritional disorders, and comorbidity at admission and during the follow-up could potentially mitigate long-term mortality after hip fractures.
Full article
(This article belongs to the Section Geriatric Pulmonology)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Short-Term Opioid Treatment of Acute Locomotor Pain in Older Adults: Comparison of Effectiveness and Safety between Tramadol and Oxycodone: A Randomized Trial
by
Wim Henri Janssens, Pauwelijn Verhoestraete, Ruth D. Piers and Nele J. Van Den Noortgate
Geriatrics 2024, 9(2), 46; https://doi.org/10.3390/geriatrics9020046 - 05 Apr 2024
Abstract
Introduction: We conducted a head-to-head comparison of step 2 (tramadol) and step 3 (oxycodone) of the WHO pain ladder in older adults with moderate to severe acute locomotor pain. Materials and methods: Multi-center prospective randomized study. Patients were 70 years or older, admitted
[...] Read more.
Introduction: We conducted a head-to-head comparison of step 2 (tramadol) and step 3 (oxycodone) of the WHO pain ladder in older adults with moderate to severe acute locomotor pain. Materials and methods: Multi-center prospective randomized study. Patients were 70 years or older, admitted to the acute geriatric ward of three hospitals, suffering from acute moderate to severe locomotor pain, and opioid-naive. Patients were randomized into two treatment groups: tramadol versus oxycodone. The Consort reporting guidelines were used. Results: Forty-nine patients were included. Mean numeric rating scale (NRS) decreased significantly between day 0 and 2 of the inclusion in both groups. A sustained significant decrease in mean NRS was seen at day 7 in both groups. Nausea was significantly more prevalent in the tramadol group, with a trend towards a higher prevalence of delirium and falls and three serious adverse events in the same group. Conclusions: Opioid therapy may be considered as a short-term effective treatment for moderate to severe acute locomotor pain in older adults. Oxycodone may possibly be preferred for safety reasons. These results can have implications for geriatric practice, showing that opioids for treatment of acute moderate to severe locomotor pain in older patients are effective and safe if carefully monitored for side effects. Opioid therapy may be considered as a short-term treatment for moderate to severe acute locomotor pain in older adults, if carefully monitored for (side) effects, while oxycodone may possibly be preferred for safety reasons. These results can have implications for daily practice in geriatric, orthopedic, and orthogeriatric wards, as well as in terminal care, more precisely for the treatment of moderate to severe acute locomotor pain in older adults.
Full article
(This article belongs to the Special Issue Enriching Lives: Palliative Care in Geriatrics)
Open AccessReview
Inflammaging in Multidrug-Resistant Sepsis of Geriatric ICU Patients and Healthcare Challenges
by
Nishitha R. Kumar, Tejashree A. Balraj, Kusuma K. Shivashankar, Tejaswini C. Jayaram and Akila Prashant
Geriatrics 2024, 9(2), 45; https://doi.org/10.3390/geriatrics9020045 - 03 Apr 2024
Abstract
Multidrug-resistant sepsis (MDR) is a pressing concern in intensive care unit (ICU) settings, specifically among geriatric patients who experience age-related immune system changes and comorbidities. The aim of this review is to explore the clinical impact of MDR sepsis in geriatric ICU patients
[...] Read more.
Multidrug-resistant sepsis (MDR) is a pressing concern in intensive care unit (ICU) settings, specifically among geriatric patients who experience age-related immune system changes and comorbidities. The aim of this review is to explore the clinical impact of MDR sepsis in geriatric ICU patients and shed light on healthcare challenges associated with its management. We conducted a comprehensive literature search using the National Center for Biotechnology Information (NCBI) and Google Scholar search engines. Our search incorporated keywords such as “multidrug-resistant sepsis” OR “MDR sepsis”, “geriatric ICU patients” OR “elderly ICU patients”, and “complications”, “healthcare burdens”, “diagnostic challenges”, and “healthcare challenges” associated with MDR sepsis in “ICU patients” and “geriatric/elderly ICU patients”. This review explores the specific risk factors contributing to MDR sepsis, the complexities of diagnostic challenges, and the healthcare burden faced by elderly ICU patients. Notably, the elderly population bears a higher burden of MDR sepsis (57.5%), influenced by various factors, including comorbidities, immunosuppression, age-related immune changes, and resource-limited ICU settings. Furthermore, sepsis imposes a significant economic burden on healthcare systems, with annual costs exceeding $27 billion in the USA. These findings underscore the urgency of addressing MDR sepsis in geriatric ICU patients and the need for tailored interventions to improve outcomes and reduce healthcare costs.
Full article
(This article belongs to the Topic One Health Approach in Global Health and Clinical Medicine)
►▼
Show Figures
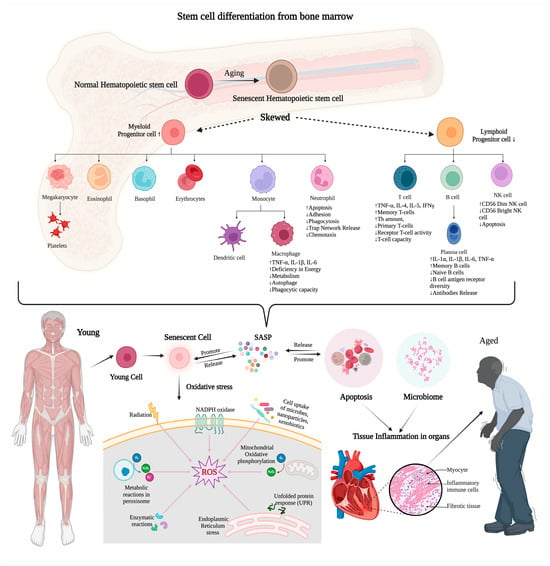
Figure 1
Open AccessArticle
Clinical Outcomes after Surgical Aortic Valve Replacement in 681 Octogenarians: A Single-Center Real-World Experience Comparing the Old Patients with the Very Old Patients
by
Wilhelm Mistiaen, Ivo Deblier, Karl Dossche and Anthony Vanermen
Geriatrics 2024, 9(2), 44; https://doi.org/10.3390/geriatrics9020044 - 01 Apr 2024
Abstract
Aortic valve disease is a lethal condition, once it becomes symptomatic. Surgical aortic valve replacement (SAVR) has, for a long time, been the only treatment option. In patients aged 85 and older, the consequences of SAVR have rarely been investigated. A total of
[...] Read more.
Aortic valve disease is a lethal condition, once it becomes symptomatic. Surgical aortic valve replacement (SAVR) has, for a long time, been the only treatment option. In patients aged 85 and older, the consequences of SAVR have rarely been investigated. A total of 681 octogenarian patients were subdivided into a group with patients between 80 and 84 years (n = 527) and a group with patients aged 85 or older (n = 154). For each group, the temporal referral pattern, preoperative comorbid profile, operative data, postoperative need for resources, and adverse postoperative events including 30-day mortality and long-term survival were determined using the chi-squared test, Student’s t-test, and log-rank test. For both age groups, the predictors for mortality were identified using a logistic regression analysis. In the oldest patient group, there were significantly more prior episodes of heart failure (75/154 vs. 148/527) and a greater need for urgent SAVR (45/150 vs. 109/515). The operative data and the need for postoperative resources were comparable, but the 30-day mortality was almost twice as high (24/154 vs. 45/527). The need for urgent SAVR was twice as high in the oldest group (odds ratio of 3.12 vs. 6.64). A logistic regression analysis for all 681 patients showed that age over 85 ranked fourth of six predictors for 30-day mortality. Five-year survival was favorable for both groups (67.8 ± 2.1% vs. 60.0 ± 4.3%). A Cox proportional hazard analysis failed to identify an age over 85 as a predictor for long-term mortality. Aortic valve disease and its effect on the left ventricle seemed to be more advanced in the highest age group. The mortality rate was almost double the need for urgent SAVR. This can be avoided by obtaining an earlier referral.
Full article
(This article belongs to the Section Cardiogeriatrics)
►▼
Show Figures
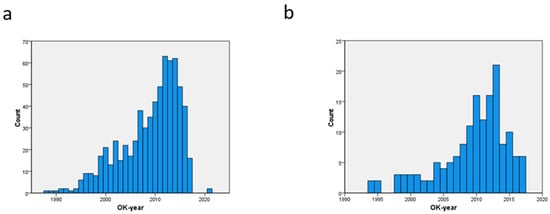
Figure 1
Open AccessBrief Report
The 2-Minutes Walking Test Is Not Correlated with Aerobic Fitness Indices but with the 5-Times Sit-to-Stand Test Performance in Apparently Healthy Older Adults
by
Marina Gil-Calvo, José Antonio de Paz, Alba Herrero-Molleda, Arthur Zecchin, María Teresa Gómez-Alonso, Beatriz Alonso-Cortés and Daniel Boullosa
Geriatrics 2024, 9(2), 43; https://doi.org/10.3390/geriatrics9020043 - 01 Apr 2024
Abstract
The 2-minutes walking test (2-MWT) is a valid and reliable test that has a high correlation with the distance walked in the 6-minutes walking test (6-MWT). However, to date, no study has determined the relationship between 2-MWT performance and the aerobic fitness indices
[...] Read more.
The 2-minutes walking test (2-MWT) is a valid and reliable test that has a high correlation with the distance walked in the 6-minutes walking test (6-MWT). However, to date, no study has determined the relationship between 2-MWT performance and the aerobic fitness indices obtained during a maximal incremental test to confirm if this test is a valid surrogate of aerobic fitness in apparently healthy older adults. The main objective of this work was to identify the factors associated to the performance in the 2-MWT, including aerobic fitness, functional and spatial-temporal gait parameters. Seventeen elderly adults performed a maximal incremental cycling test to determine maximum oxygen consumption (VO2max) and ventilatory thresholds (VT1 and VT2), two static standing balance tests with open and close eyes, a 5-times sit-to-stand test (5-TSTS), a handgrip test, and a 2-MWT on three different days over 2 weeks. No correlations were found between aerobic fitness indices and the distance covered in 2-MWT, but significant moderate correlations were found between the distance covered in 2-MWT and the time to perform the 5-TSTS (rho = −0.49) and with stride length (rho = 0.52) during the test. In conclusion, the 2-MWT does not seem a good test to assess aerobic capacity while it showed to be associated to the 5-TSTS performance of the elderly.
Full article
Open AccessBrief Report
Effects of Advance Care Planning on End-of-Life Indicators for Nursing Home Residents—An Experimental Study with a Retrospective Chart Review
by
Yu-Tai Lo, Jin-Jy Wang, Yi-Ching Yang, Chiu-Yen Yu, Chia-Ming Chang and Ya-Ping Yang
Geriatrics 2024, 9(2), 42; https://doi.org/10.3390/geriatrics9020042 - 27 Mar 2024
Abstract
Advance care planning (ACP) has the potential to improve the outcomes of end-of-life care for residents in nursing homes. The aim of this study was to determine whether an ACP program was beneficial for nursing home residents by assessing end-of-life indicators. An experimental
[...] Read more.
Advance care planning (ACP) has the potential to improve the outcomes of end-of-life care for residents in nursing homes. The aim of this study was to determine whether an ACP program was beneficial for nursing home residents by assessing end-of-life indicators. An experimental study with a retrospective chart review was conducted. In total, 37 residents in the intervention group participated in an institutional advance care planning program for 1 year, and their chart data over 1 year were collected following the completion of the program; 33 residents in the control group had died within 1 year before the start date of program, and their chart data were reviewed retrospectively. Chi-square and t tests were used to examine four indicators of the quality of end-of-life care. Compared with the control group, the intervention group had a higher proportion of do-not-resuscitate directives, hospice care before death, and deaths in the nursing home, and fewer hospitalizations and deaths in an emergency department. ACP programs may improve the quality of end-of-life care for nursing home residents in Taiwan. Further research across different long-term care facilities is warranted.
Full article
(This article belongs to the Special Issue Health and Disease in Frail Older Individuals: Assessment and Management in Clinical Practice)
Open AccessArticle
The Association between Functional Health Patterns and Frailty in Hospitalized Geriatric Patients
by
Elisabeta Ioana Hiriscau, Omar Cauli, Valer Donca, Luminita-Aurelia Marinescu, Antonia-Eugenia Macarie, Lucretia Avram, Oana-Gabriela Cancel, Steliana Donca, Elena-Cristina Buzdugan, Dana-Alina Crisan and Constantin Bodolea
Geriatrics 2024, 9(2), 41; https://doi.org/10.3390/geriatrics9020041 - 26 Mar 2024
Abstract
►▼
Show Figures
This study investigates the association between the Functional Health Pattern Assessment Screening Tool (FHPAST) and frailty in hospitalized geriatric patients. One hundred and forty patients (mean age 78.2 years, age range 65–90) were screened for frailty using the Frail Scale during hospitalization in
[...] Read more.
This study investigates the association between the Functional Health Pattern Assessment Screening Tool (FHPAST) and frailty in hospitalized geriatric patients. One hundred and forty patients (mean age 78.2 years, age range 65–90) were screened for frailty using the Frail Scale during hospitalization in the geriatric unit. Among them, 57 patients were identified as prefrail (40.7%), and 83 were identified as frail (59.3%). A comparative analysis between groups in terms of the FHPAST components covering health risk, general well-being, and health promotion was performed. Correlations between FHAPST components, socio-demographic data, frailty criteria, as well as logistic regression to identify variables that better predict frailty were also sought. Frailty was mainly associated with difficulty urinating, limitations in performing activities of daily living and walking, physical discomfort, less positive feelings in controlling one’s own life, lower compliance with recommendations from the healthcare provider, and engagement in seeking healthcare services. Patients with difficulty urinating and walking had a probability of 4.38 times (OR = 4.38, CI 95% [1.20–15.94]), p = 0.025) and 65.7 times (OR = 65.7, CI 95% [19.37–223.17], p < 0.001) higher of being frail rather than prefrail. The relationship between frailty and prefrailty in hospitalized geriatric patients and components of nursing Functional Health Patterns (FHP) has yet to be explored. This study provides evidence of the most prevalent needs of frail geriatric patients in hospital settings.
Full article
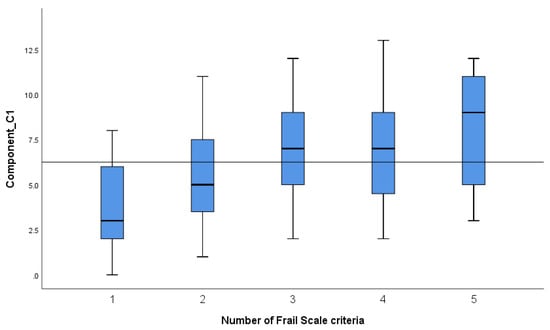
Figure 1
Open AccessArticle
Agreement in the Postural Assessment of Older Adults by Physical Therapists Using Clinical and Imaging Methods
by
Naoki Sugiyama, Yoshihiro Kai, Hitoshi Koda, Toru Morihara and Noriyuki Kida
Geriatrics 2024, 9(2), 40; https://doi.org/10.3390/geriatrics9020040 - 22 Mar 2024
Abstract
►▼
Show Figures
Postural assessment is one of the indicators of health status in older adults. Since the number of older adults is on the rise, it is essential to assess simpler methods and automated ones in the future. Therefore, we focused on a visual method
[...] Read more.
Postural assessment is one of the indicators of health status in older adults. Since the number of older adults is on the rise, it is essential to assess simpler methods and automated ones in the future. Therefore, we focused on a visual method (imaging method). The purpose of this study is to determine the degree of agreement between the imaging method and the palpation and visual methods (clinical method). In addition, the influence of differences in the information content of the sagittal plane images on the assessment was also investigated. In this experiment, 28 sagittal photographs of older adults whose posture had already been assessed using the clinical method were used. Furthermore, based on these photographs, 28 gray and silhouette images (G and S images) were generated, respectively. The G and S images were assessed by 28 physical therapists (PTs) using the imaging method. The assessment was based on the Kendall classification, with one of four categories selected for each image: ideal, kyphosis lordosis, sway back, and flat back. Cross-tabulation matrices of the assessments using the clinical method and imaging method were created. In this table, four categories and two categories of ideal and non-ideal (KL, SB, and FB) were created. The agreement was evaluated using the prevalence-adjusted bias-adjusted kappa (PABAK). In addition, sensitivity and specificity were calculated to confirm the reliability. When comparing the clinical and imaging methods in the four posture categories, the PABAK values were −0.14 and −0.29 for the S and G images, respectively. In the case of the two categories, the PABAK values were 0.57 and 0.5 for the S and G images, respectively. The sensitivity and specificity were 86% and 57% for the S images and 76% and 71% for the G images, respectively. The four categories show that the imaging method is difficult to assess regardless of the image processing. However, in the case of the two categories, the same assessment of the clinical method applied to the imaging method for both the S and G images. Therefore, no differences in image processing were observed, suggesting that PTs can identify posture using the visual method.
Full article
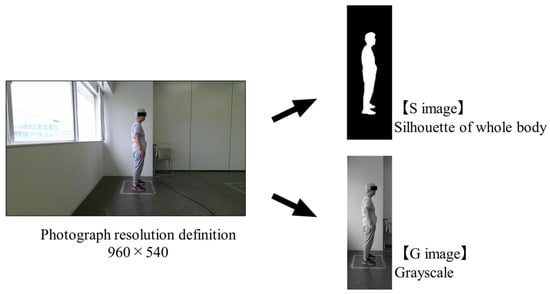
Figure 1
Open AccessOpinion
A Proposal for a Multidisciplinary Integrated Oral Health Network for Patients Undergoing Major Orthopaedic Surgery (IOHN-OS)
by
Matteo Briguglio, Thomas W. Wainwright, Marialetizia Latella, Aurora Ninfa, Claudio Cordani, Cecilia Colombo, Giuseppe Banfi, Luca Francetti and Stefano Corbella
Geriatrics 2024, 9(2), 39; https://doi.org/10.3390/geriatrics9020039 - 19 Mar 2024
Abstract
The passing of the years of life physiologically leads to the accumulation of changes in tissues in the oral cavity, influencing dentition, chewing and swallowing mechanisms, and the oral microbiota. Some diseases and medications can aggravate oral symptoms and negatively influence eating behaviours,
[...] Read more.
The passing of the years of life physiologically leads to the accumulation of changes in tissues in the oral cavity, influencing dentition, chewing and swallowing mechanisms, and the oral microbiota. Some diseases and medications can aggravate oral symptoms and negatively influence eating behaviours, increasing the likelihood of becoming malnourished. This could make older individuals more vulnerable to complications when undergoing major orthopaedic surgery. Hidden infection foci in the oral cavity are a recognised cause of post-operative periprosthetic joint infections. Dysfunctional oral problems might also compromise feeding after surgery when good nutrition represents a fundamental aspect of a proper recovery. To manage these shortcomings, in this article, the authors hypothesise a multidisciplinary path of care named the Integrated Oral Health Network applied to major Orthopaedic Surgery (IOHN-OS). This peri-operative initiative would include pre-operative oral health screening and risk management by a dental team, patient education programmes before and after surgery, and bedside gerodontology actions like oral care and meal and eating support for fragile individuals. The IOHN-OS has the potential to reshape the concept of suitability for major orthopaedic surgery and generate momentum for designing community-based surveillance programmes that can keep the mouths of older subjects healthy for a long time.
Full article
(This article belongs to the Special Issue Advancing Oral Health Care for the Ageing Population: Exploring Gerodontology and Geriatric Dentistry)
►▼
Show Figures
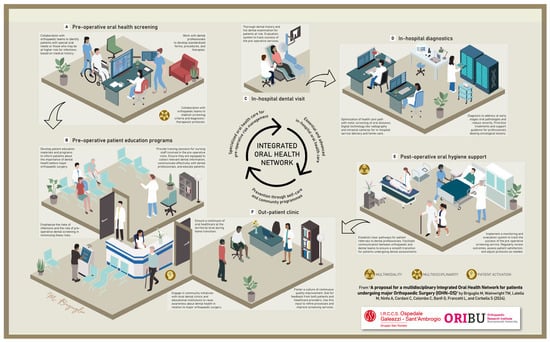
Figure 1
Open AccessArticle
Hope Mediates Stress to Reduce Burden in Family Caregivers of Persons with Alzheimer’s Disease
by
Jocelyn Shealy McGee, Edward C. Polson, Dennis R. Myers, Angela McClellan, Rebecca Meraz, Weiming Ke and Holly Carlson Zhao
Geriatrics 2024, 9(2), 38; https://doi.org/10.3390/geriatrics9020038 - 18 Mar 2024
Abstract
The experience of burden among family caregivers of persons with Alzheimer’s disease and other forms of dementia may be deleterious for their health and well-being. Little is known, however, about the degree to which internal positive psychological resources, such as hope, influence burden
[...] Read more.
The experience of burden among family caregivers of persons with Alzheimer’s disease and other forms of dementia may be deleterious for their health and well-being. Little is known, however, about the degree to which internal positive psychological resources, such as hope, influence burden perceptions in this population. The current study is novel in that it examined how multiple dimensions of hope, hope–agency and hope–pathway, influenced burden in a sample of one-hundred and fifty-five family caregivers of persons with Alzheimer’s disease. The stress process model was used as the theoretical framework for variable specification in this study. Hope was conceptualized using Snyder and colleagues’ hope theory. Supporting our first hypothesis, we found that burden was negatively associated with hope–agency, r = −0.33, p < 0.001 and hope–pathway, r = −0.24, p < 0.01. Multiple regression was used to determine if hope–agency and hope–pathway independently contributed to burden. Analysis revealed that hope–agency but not hope–pathway influenced burden when other key variables were taken into consideration. Findings from mediation analysis affirmed that hope–agency had a small but significant mediation effect between stress and burden in this sample. This study provides evidence for the relevance of assessing multiple dimensions of hope when working with caregivers of persons with Alzheimer’s. Although replication studies are warranted, the current study confirms a need for further development and refinement of hope-bolstering behavioral interventions which may mediate stress and burden in this population. These interventions should be systematically assessed for efficacy and effectiveness via implementation studies in real-world settings.
Full article
(This article belongs to the Section Geriatric Psychiatry and Psychology)
►▼
Show Figures
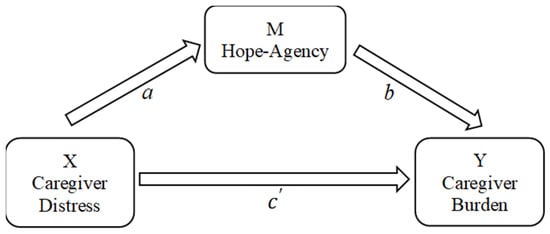
Figure 1
Open AccessArticle
Neurocognitive Effects of an Online Brain Health Program and Weekly Telehealth Support Group in Older Adults with Subjective Memory Loss: A Pilot Study
by
Ryan M. Glatt, Amylee Amos, David A. Merrill, John F. Hodes, Claudia L. Wong, Karen J. Miller and Prabha Siddarth
Geriatrics 2024, 9(2), 37; https://doi.org/10.3390/geriatrics9020037 - 14 Mar 2024
Abstract
Introduction: Adopting healthy lifestyle behaviors has the potential to slow cognitive decline in older adults by reducing risks associated with dementia. Curriculum-based group health coaching may aid in establishing behavior change centered for dementia risk factors. Methods: In this pilot clinical care patient
[...] Read more.
Introduction: Adopting healthy lifestyle behaviors has the potential to slow cognitive decline in older adults by reducing risks associated with dementia. Curriculum-based group health coaching may aid in establishing behavior change centered for dementia risk factors. Methods: In this pilot clinical care patient group study (n = 6), we examined the effects of a six-month online Cognitive Health Program combined with a weekly telehealth support group led by the course creator, and personalized health optimization by a collaborating physician, in older adults with subjective cognitive decline. Cognition was assessed at baseline and post-intervention using a computerized battery. Results: Cognitive changes were estimated with nonparametric tests and effect sizes (Cohen’s d). Results showed significant improvements in global cognition (p < 0.03, d = 1.6), spatial planning (p < 0.01, d = 2.3), and visuospatial processing (p < 0.05, d = 1.1) compared to baseline. Participants reported high levels of satisfaction with the virtual group format and online curriculum. Conclusions: This small pilot study suggests that a virtual six-month personalized health coaching group with self-paced online health education is feasible and potentially efficacious for improving cognition in participants with subjective cognitive complaints. This format may facilitate behavior change to slow cognitive decline. Future studies should include a control group, a larger, more diverse sample as well as assessing mood and other subjective measures.
Full article
(This article belongs to the Section Geriatric Psychiatry and Psychology)
►▼
Show Figures
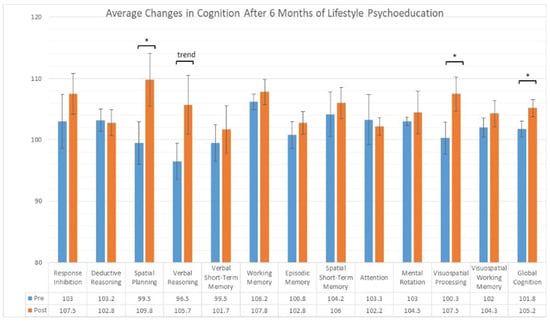
Figure 1
Open AccessArticle
Moderating Effect of Muscular Strength in the Association between Cardiovascular Events and Depressive Symptoms in Middle-Aged and Older Adults—A Cross Sectional Study
by
Diogo Veiga, Miguel Peralta, Élvio R. Gouveia, Marcelo de Maio Nascimento, Laura Carvalho, Jorge Encantado and Adilson Marques
Geriatrics 2024, 9(2), 36; https://doi.org/10.3390/geriatrics9020036 - 12 Mar 2024
Abstract
Background: Depression and cardiovascular diseases are two main health conditions contributing to the global disease burden. Several studies indicate a reciprocal association between them. It is still unclear how changes in overall muscle strength may impact this association. This study aimed to analyse
[...] Read more.
Background: Depression and cardiovascular diseases are two main health conditions contributing to the global disease burden. Several studies indicate a reciprocal association between them. It is still unclear how changes in overall muscle strength may impact this association. This study aimed to analyse how muscular strength moderates the relationship between cardiovascular events and depressive symptoms among middle-aged and older adults. Methods: Wave 8 of the population-based Survey of Health, Ageing, and Retirement in Europe (2019/2020) cross-sectional data, which included 41,666 participants (17,986 men) with a mean age of 70.65 (9.1) years old, was examined. Grip strength was measured twice on each hand using a dynamometer. The 12-item EURO-D scale was employed to gauge depressive symptoms. Results: Grip strength negatively moderates the link between cardiovascular events and depressive symptoms (male: B = −0.03, 95% CI = −0.04, −0.03; female: B = −0.06, 95% CI = −0.06, −0.05). Additionally, the grip strength moderation values in the significant zone for males and females were less than 63.2 kg and 48.3 kg, respectively. Conclusions: Muscular strength modifies depressive symptoms and lessens their correlation with cardiovascular diseases. Muscle-strengthening activities could be incorporated into primary and secondary preventive strategies to reduce the burden of depression in people with CVD.
Full article
(This article belongs to the Section Geriatric Public Health)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Ophiocephalus striatus Extract Supplementation Decreases Serum IL-6 Levels in Older People with Sarcopenia—A Single-Center Experience
by
Nur Riviati, Legiran Legiran, Irsan Saleh, Taufik Indrajaya, Zulkhair Ali, Irfannuddin and Probosuseno
Geriatrics 2024, 9(2), 35; https://doi.org/10.3390/geriatrics9020035 - 07 Mar 2024
Abstract
Sarcopenia, a condition characterized by muscle loss and decreased function in older adults, is a growing public health concern. This study aimed to investigate the effects of Ophiocephalus striatus extract on insulin-like growth factor-1 serum, interleukin-6 serum levels, and sarcopenia-related parameters in older
[...] Read more.
Sarcopenia, a condition characterized by muscle loss and decreased function in older adults, is a growing public health concern. This study aimed to investigate the effects of Ophiocephalus striatus extract on insulin-like growth factor-1 serum, interleukin-6 serum levels, and sarcopenia-related parameters in older adults with sarcopenia. This double-blind randomized controlled trial included 80 older adults with sarcopenia. Participants were randomly assigned to receive Ophiocephalus striatus extract or a placebo for two weeks. The IGF-1 serum and IL-6 serum levels were assessed as primary outcomes. The Ophiocephalus striatus extract intervention resulted in a significant reduction in serum IL-6 levels. Although the IGF-1 levels did not show significant changes, there was an increase for the intervention group. This study demonstrated that a 2-week intervention with Ophiocephalus striatus extract positively impacted the serum IL-6 levels in older adults with sarcopenia. While the IGF-1 levels did not change significantly in this short intervention period, the observed improvements in IGF-1, calf circumference, muscle mass, and muscle strength are promising. The findings suggest that Ophiocephalus striatus extract may offer a valuable intervention for managing sarcopenia, particularly in regions with abundant Ophiocephalus striatus production, such as South Sumatera. This study was registered with trial number NCT05869383.
Full article
(This article belongs to the Topic Preventing and Managing Sarcopenia in Older Adults through Physical Activity, Exercise and Nutrition Interventions and Approaches)
►▼
Show Figures
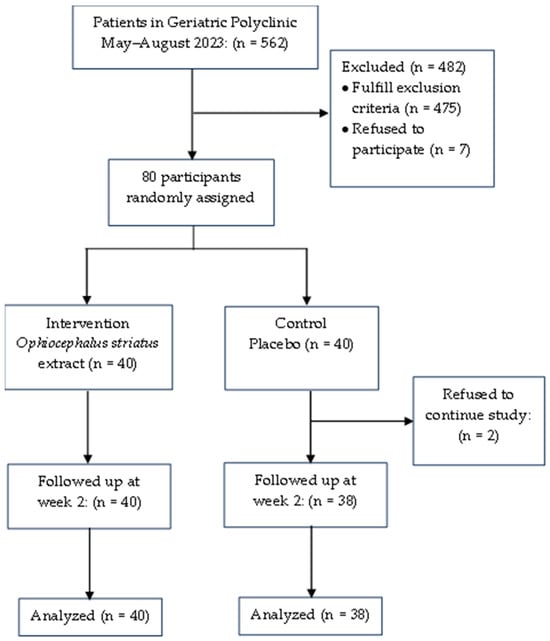
Figure 1
Open AccessPerspective
Pulmonary Diseases in Older Patients: Understanding and Addressing the Challenges
by
Pushpa Raj Joshi
Geriatrics 2024, 9(2), 34; https://doi.org/10.3390/geriatrics9020034 - 07 Mar 2024
Abstract
As the global population ages, pulmonary diseases among older people have emerged as a significant and growing public health concern. The increasing incidence of these conditions has led to higher rates of morbidity and mortality among older adults. This perspective study offers a
[...] Read more.
As the global population ages, pulmonary diseases among older people have emerged as a significant and growing public health concern. The increasing incidence of these conditions has led to higher rates of morbidity and mortality among older adults. This perspective study offers a thorough overview of the prevalent pulmonary diseases affecting the elderly demographic. It delves into the challenges encountered during the diagnosis and management of these conditions in older individuals, considering factors such as comorbidities, functional limitations, and medication complexities. Furthermore, innovative strategies and personalized interventions such as precision medicine, advanced therapies, telemedicine solutions, and patient-centered support systems aimed at enhancing the care provided to older individuals grappling with pulmonary disorders are thoroughly explored. By addressing the unique needs and complexities of this vulnerable population, healthcare systems can strive towards improving outcomes and enhancing the quality of life for elderly individuals affected by pulmonary diseases.
Full article
(This article belongs to the Section Geriatric Pulmonology)
Open AccessArticle
Informing Dementia Support Programs That Serve Low-Income, Multilingual Communities in a Safety Net Health System: Use of Focus Groups to Identify Specific Needs
by
Andrew Pak, Abriella Demanes, Shirley Wu, Katherine Ward and Mailee Hess
Geriatrics 2024, 9(2), 33; https://doi.org/10.3390/geriatrics9020033 - 06 Mar 2024
Abstract
The Centers of Medicare and Medicaid Services recently announced a new voluntary nationwide model. This model aims to provide comprehensive, standard care for people living with dementia and their unpaid caregivers and to enhance health equity in dementia care. However, little is known
[...] Read more.
The Centers of Medicare and Medicaid Services recently announced a new voluntary nationwide model. This model aims to provide comprehensive, standard care for people living with dementia and their unpaid caregivers and to enhance health equity in dementia care. However, little is known about the needs of older adults with dementia and their caregivers in a multiethnic and multicultural patient population of a safety net health system. The aim of this study is to include their voices. We conducted four focus groups in English and Spanish to investigate the common needs and barriers unique to the care of patients within the Los Angeles County healthcare system. Using qualitative, iterative analyses of the transcripts, we identified four domains of concern from the dyads (persons with dementia and their caregivers): need for education for dyad-centered care, barriers to resources, dyad safety, and caregiver burden and insight. These domains are interconnected, and the way this patient population experiences these domains may differ compared to those in well-resourced or predominantly English-speaking healthcare settings. Therefore, the identified domains serve as potential building blocks for dementia support programs inclusive of underserved, multicultural populations.
Full article
(This article belongs to the Section Geriatric Psychiatry and Psychology)
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cells, Geriatrics, Immuno, IJMS, JCM
Inflammaging: The Immunology of Aging
Topic Editors: Juan Pablo de Rivero Vaccari, Alejandro Martín-MontalvoDeadline: 30 June 2024
Topic in
Geriatrics, Healthcare, IJERPH, JCM, TropicalMed
One Health Approach in Global Health and Clinical Medicine
Topic Editors: Roy Rillera Marzo, Adnan Kisa, Atin Adhikari, Bijaya PadhiDeadline: 31 July 2024
Topic in
Biomedicines, Brain Sciences, Geriatrics, Life, Neurology International
Translational Advances in Neurodegenerative Dementias
Topic Editors: Francesco Di Lorenzo, Annibale AntonioniDeadline: 31 October 2024
Topic in
Behavioral Sciences, Brain Sciences, Children, Geriatrics, Healthcare
Personality, Health and Well-Being among Different Age Groups
Topic Editors: Hajime Iwasa, Yuko YoshidaDeadline: 31 December 2024

Conferences
Special Issues
Special Issue in
Geriatrics
Psycho-Bio-Social Factors to Drive Frailty: What’s New?
Guest Editors: Guilherme Furtado, André Luis Lacerda Bachi, Marcelo BarrosDeadline: 30 April 2024
Special Issue in
Geriatrics
Physical Activity and Exercise in Older Adults
Guest Editor: Nicola AdamsDeadline: 30 June 2024
Special Issue in
Geriatrics
Psychological Perspectives on Driving Behavior in Aging: Implications for Assessment Tools and Training Methods
Guest Editors: Luigi Tinella, Alessandro Oronzo Caffò, Andrea BoscoDeadline: 31 July 2024
Special Issue in
Geriatrics
Nutrition Care and Support in Geriatrics
Guest Editor: Olof Gudny GeirsdottirDeadline: 30 September 2024
Topical Collections
Topical Collection in
Geriatrics
Joint Arthroplasty in the Oldest People
Collection Editors: Juan F. Blanco, Carmen da Casa
Topical Collection in
Geriatrics
Ageism, the Black Sheep of the Decade of Healthy Ageing
Collection Editor: Lydia Gimenez Llort
Topical Collection in
Geriatrics
Responding to the Pandemic: Geriatric Care Models
Collection Editor: James Powers





