Journal Description
Clinical and Translational Neuroscience
Clinical and Translational Neuroscience
is an international, peer-reviewed, open access journal on neuroscience. The journal is owned by the Swiss Federation of Clinical Neuro-Societies and is published quarterly online by MDPI (from Volume 5 Issue 2-2021).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), EBSCO, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 20.6 days after submission; acceptance to publication is undertaken in 3.5 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Latest Articles
The International Master of Advanced Studies (MAS) in Sleep Medicine of the Universities of Bern and Svizzera Italiana
Clin. Transl. Neurosci. 2024, 8(2), 19; https://doi.org/10.3390/ctn8020019 - 10 Apr 2024
Abstract
Introduction: Sleep–wake circadian disorders (SWCDs) are very frequent and linked to major negative effects on the body, mental health, the brain, and on occupational and societal health. The prevention, diagnosis, and treatment of SWCDs and the promotion of sleep health require the sufficient
[...] Read more.
Introduction: Sleep–wake circadian disorders (SWCDs) are very frequent and linked to major negative effects on the body, mental health, the brain, and on occupational and societal health. The prevention, diagnosis, and treatment of SWCDs and the promotion of sleep health require the sufficient education of general practitioners, specialists, and other health professionals. Unfortunately, education at pre- and postgraduate level is insufficient in most countries across the world. Aims and methods: This article describes the historical context, basic considerations, and methodological approach for the creation of the International Postgraduate Sleep Master by the University of Bern and Svizzera Italiana. Results: The postgraduate Master, which was launched in 2017, is a part-time, flexible course, taken over 2 ½ years, which targets health professionals, scientists, and technicians. After an initial introduction, which is the same for everybody (“common trunk”), the course can be individualized. The 12 modules of the Master include online lectures, schools, internships in a sleep center (in one of our 15 partner universities), case discussions and interactive sessions with students and internationally recognized experts from over 20 countries across the world, and culminates with a Master thesis. The program covers sleep–wake circadian biology; the management of SWCDs; disturbances of consciousness and sleep-related epilepsies; novel approaches in sleep medicine (e.g., clinical trials, telemedicine, data science, artificial intelligence); and topics of increasing relevance (e.g., neurodegenerative disorders, gender and diversity, sleep health, new technologies, artificial intelligence, professional and societal implications). Students are encouraged to also take “crash courses” in preparation for the national, European, and World sleep examinations. Conclusion: The Postgraduate University Sleep Master of the Universities of Bern and Svizzera Italiana offers a unique part-time, (mainly) virtual opportunity to acquire state-of the art knowledge, skills, and professional experiences to prepare for a clinical or scientific career in sleep medicine for physicians, scientists, and other health professionals.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►
Show Figures
Open AccessArticle
Comparison of Aneurysmal and Non-Aneurysmal Spontaneous Cervical Artery Dissections in a Large Multicenter Cohort
by
Valentin K. Steinsiepe, Hakan Sarikaya, Pasquale R. Mordasini, Susanne Wegener, Corinne Inauen, Philipp Baumgartner, Simon Jung, Kateryna Antonenko, Urs Fischer, Jan Gralla, Roza M. Umarova, Barbara Goeggel Simonetti, Constance J. H. C. M. van Laarhoven, Gert J. de Borst, Hugues Chabriat, Mirjam R. Heldner and Marcel Arnold
Clin. Transl. Neurosci. 2024, 8(2), 18; https://doi.org/10.3390/ctn8020018 - 6 Apr 2024
Abstract
►▼
Show Figures
Dissecting aneurysms in patients with spontaneous cervical artery dissections have, so far, been reported as “benign”, but more specific information is scarce. We aimed to elucidate (1) vascular risk factors, (2) local and ischemic symptoms, and (3) long-term prognosis compared to non-aneurysmal dissections.
[...] Read more.
Dissecting aneurysms in patients with spontaneous cervical artery dissections have, so far, been reported as “benign”, but more specific information is scarce. We aimed to elucidate (1) vascular risk factors, (2) local and ischemic symptoms, and (3) long-term prognosis compared to non-aneurysmal dissections. This case–control study included consecutive patients with spontaneous cervical artery dissection from three university hospitals in Switzerland and France, evaluated at baseline and at 3 months. In addition, further follow-ups were performed at the discretion of the treating physician. Dissecting aneurysms were diagnosed with duplex sonography, magnetic resonance angiography, and/or digital subtraction angiography. Of 1012 patients, 151 (14.9%) presented with 167 dissecting aneurysms at baseline (n = 103) or follow-up (n = 64). The median follow-up was 24.9 months (IQR: 6.8–60.8). Compared to patients without a dissecting aneurysm there were no significant differences in the vascular risk factors or local symptoms (91.4 vs. 89.8%). Ischemic strokes at baseline were less common (29.1% vs. 54.4%; OR: 0.41; 95% CI: 0.28–0.60) in patients with a dissecting aneurysm, even after correction for the degree of stenosis of the dissected arteries (OR: 0.53; 95% CI: 0.34–0.81). Patients with a dissecting aneurysm more often had a favorable clinical outcome (modified Rankin Scale Score of 0–1) at 3 months (80.6% vs. 54.5%). There was no significant difference in recurrent cerebrovascular events at 3 months or overall. The lower rate of ischemic strokes at baseline may reflect a different pathogenic mechanism, such as a smaller initial tear in the vessel wall or an increased vessel caliber from an early or primary intramural hematoma with a different shape.
Full article

Figure 1
Open AccessArticle
Foam Cells Analysis from Retrieved Stroke Clot for the Identification of Atherothrombotic Etiology
by
Fabrizio Giammello, Antonio Ciacciarelli, Domenico Cosenza, Santi Galletta, Valeria Barresi, Paolino La Spina, Maria Carolina Fazio, Jolanda De Caro, Masina Cotroneo, Cristina Dell’Aera, Francesco Grillo, Serena Ammendola, Agostino Tessitore, Sergio Lucio Vinci, Rosa Fortunata Musolino, Carmela Casella and Antonio Toscano
Clin. Transl. Neurosci. 2024, 8(2), 17; https://doi.org/10.3390/ctn8020017 - 5 Apr 2024
Abstract
►▼
Show Figures
Background: In atherothrombotic acute ischemic stroke (AIS), when the atheroma breaks down, the clot can incorporate foam cells (FCs). The identification of the correct etiology is paramount for secondary stroke prevention. This study aims to evaluate the presence of the FC in
[...] Read more.
Background: In atherothrombotic acute ischemic stroke (AIS), when the atheroma breaks down, the clot can incorporate foam cells (FCs). The identification of the correct etiology is paramount for secondary stroke prevention. This study aims to evaluate the presence of the FC in the arterial clot, and to determine whether patients with FCs and patients without FCs (NFCs) had different cerebrovascular risk factors, haemato-chemical parameters, and atherosclerotic disease incidence, in order to predict the etiological diagnosis. Methods: We collected 100 clots retrieved by mechanical thrombectomy from 495 consecutive AIS patients with large vessel occlusion. An expert pathologist evaluated the FC presence by histological examination stained with hematoxylin and eosin. Results: We observed FCs in 29/100 (29%) of retrieved clots and divided the patients into two groups, with/without FCs. The two groups had similar clinical and laboratory features, with a discrepancy between the FC presence in the clot and the clinical etiological diagnosis, even if not statistically significant. Conclusions: Our study showed the presence of FCs in approximately one-third of the retrieved clots, but the identification of the clot that presumably comes from the atheromatous plaque rupture tended to disagree with the clinical diagnosis. Future studies may reveal their potential to disclose clot origin or specific patient characteristics, guiding treatment options.
Full article
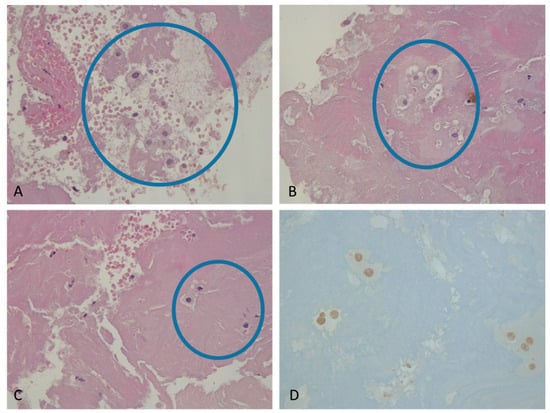
Figure 1
Open AccessCase Report
Creutzfeldt–Jakob Disease Associated with E200K Mutation and SARS-CoV-2 Infection: Pure Coincidence or Neurodegenerative Acceleration?
by
Elisa Colaizzo, Luca Prosperini, Antonio Petrucci and Alessia Perna
Clin. Transl. Neurosci. 2024, 8(2), 16; https://doi.org/10.3390/ctn8020016 - 26 Mar 2024
Abstract
►▼
Show Figures
Several recent studies reported on some patients developing Creutzfeldt–Jakob disease (CJD) following coronavirus disease 2019, but, to the best of our knowledge, this case is the first reported in Italy on an onset of a CJD genetic form (gCJD) immediately after COVID-19 infection.
[...] Read more.
Several recent studies reported on some patients developing Creutzfeldt–Jakob disease (CJD) following coronavirus disease 2019, but, to the best of our knowledge, this case is the first reported in Italy on an onset of a CJD genetic form (gCJD) immediately after COVID-19 infection. We present a 51-year-old woman with a positive family history for CJD, who, two months after a mild SARS-CoV-2 infection, presented a rapidly progressing dementia diagnosed as CJD through clinical features, imaging, electroencephalography, and cerebrospinal fluid analysis. Genetic testing revealed the E200K mutation (p.Glu200Lys) c.598G>A, with homozygosity for methionine (MET) at codon 129, thus confirming the diagnosis of Creutzfeldt–Jakob disease. She passed away two months later. Interestingly, our case confirms that homozygous E200K gCJD patients are characterized by a relatively younger age of onset; moreover, it also sheds light on the neurodegeneration underlying both prion diseases and COVID-19 infection. In our opinion, the rising global prevalence of neurodegenerative complications following COVID-19 disease adds urgency to the study of this potential relationship, mostly in elderly patients who may experience worse long-lasting outcomes systemically and within the nervous system.
Full article
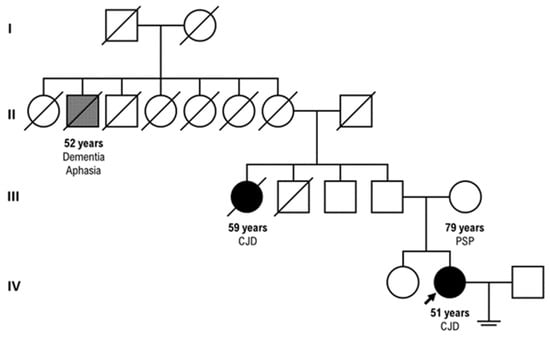
Figure 1
Open AccessCommunication
What Cluster Headache Patients Would Like Their Relatives to Know: Results from a Qualitative Study
by
Papitha Saravanamuthu, Susanne Wegener and Heiko Pohl
Clin. Transl. Neurosci. 2024, 8(1), 15; https://doi.org/10.3390/ctn8010015 - 21 Mar 2024
Abstract
Many patients with cluster headaches report that their relatives do not understand what they are going through. This qualitative study aimed to collect patients’ recommendations and wishes on how others should respond to those suffering from cluster headaches. We recruited 22 patients with
[...] Read more.
Many patients with cluster headaches report that their relatives do not understand what they are going through. This qualitative study aimed to collect patients’ recommendations and wishes on how others should respond to those suffering from cluster headaches. We recruited 22 patients with episodic or chronic cluster headaches for this cross-sectional study. They responded to seven questions that assessed the disease’s impact on their relationships with relatives and their wishes for others’ behaviour towards them. Seven recommendations for relatives emerged: (i) withdraw during attacks, (ii) respect post-ictal exhaustion, (iii) do not insist on discussing the disorder, (iv) help the patient to lead a “normal” life, (v) support preserving social contacts, (vi) show being aware of the disease severity, and (vii) expect the disease to take up space in patients’ lives and minds. Two recommendations for the interictal period indicate avoidance, which is considered a negative coping strategy. Conversely, the suggestion to support preserving social contacts might mean confronting the disease, which is likely associated with more favourable outcomes. Still, adhering to all patients’ requests might increase suffering instead of reducing it. Thus, further research is needed to develop strategies suited to improve well-being.
Full article
Open AccessPerspective
The Swiss Sleep House Bern—A New Approach to Sleep Medicine
by
Simone B. Duss, Albrecht P. A. Vorster, Antoine Urech, Wolfgang J. Schmitt, Jonas Beck, Daniella Hilt, Oriella Gnarra, Julia van der Meer, Marina Tüzün, Thomas Berger, Carolin Schäfer, Anne-Kathrin Brill, Markus H. Schmidt, Kaspar A. Schindler and Claudio L. A. Bassetti
Clin. Transl. Neurosci. 2024, 8(1), 14; https://doi.org/10.3390/ctn8010014 - 19 Mar 2024
Abstract
►▼
Show Figures
Sleep is essential for health, well-being, creativity, and productivity. Sleep loss and sleep–wake circadian disorders (SWCDs) affect at least one in three individuals but are underdiagnosed and undertreated for different reasons: First, the importance of sleep health and, second, the burden of sleep
[...] Read more.
Sleep is essential for health, well-being, creativity, and productivity. Sleep loss and sleep–wake circadian disorders (SWCDs) affect at least one in three individuals but are underdiagnosed and undertreated for different reasons: First, the importance of sleep health and, second, the burden of sleep loss and SWCDs are underestimated. Third, education in sleep medicine is insufficient and health care-related sleep research is underdeveloped. Fourth, the validation and implementation of tele-sleep medicine approaches and novel devices to monitor SWCDs are still insufficient. Fifth, the reimbursement of sleep medicine in most countries is inadequate and the availability of specialized care is limited to a few centers. The Swiss Sleep House Bern (SSHB) was founded in 2022 to address these challenges and eventually promote better care for patients with SWCDs and improve sleep health for the broader population. The interdisciplinary and interprofessional team of the SSHB, which is integrated in the Bernese Interdisciplinary Sleep-Wake-Epilepsy Center, links sleep specialists with primary care providers to offer a rapid and accessible triage and first-level management of sleep complaints and SWCDs. The SSHB also promotes awareness and offers educational programs on sleep health and SWCDs, performs health care research, and fosters the implementation of new technologies, data science, and telemedicine into clinical routine.
Full article

Figure 1
Open AccessOpinion
Sleep Research in the Era of AI
by
Pinar Göktepe-Kavis, Florence M. Aellen, Sigurd L. Alnes and Athina Tzovara
Clin. Transl. Neurosci. 2024, 8(1), 13; https://doi.org/10.3390/ctn8010013 - 26 Feb 2024
Cited by 1
Abstract
The field of sleep research is both broad and rapidly evolving. It spans from the diagnosis of sleep-related disorders to investigations of how sleep supports memory consolidation. The study of sleep includes a variety of approaches, starting with the sole focus on the
[...] Read more.
The field of sleep research is both broad and rapidly evolving. It spans from the diagnosis of sleep-related disorders to investigations of how sleep supports memory consolidation. The study of sleep includes a variety of approaches, starting with the sole focus on the visual interpretation of polysomnography characteristics and extending to the emergent use of advanced signal processing tools. Insights gained using artificial intelligence (AI) are rapidly reshaping the understanding of sleep-related disorders, enabling new approaches to basic neuroscientific studies. In this opinion article, we explore the emergent role of AI in sleep research, along two different axes: one clinical and one fundamental. In clinical research, we emphasize the use of AI for automated sleep scoring, diagnosing sleep-wake disorders and assessing measurements from wearable devices. In fundamental research, we highlight the use of AI to better understand the functional role of sleep in consolidating memories. While AI is likely to facilitate new advances in the field of sleep research, we also address challenges, such as bridging the gap between AI innovation and the clinic and mitigating inherent biases in AI models. AI has already contributed to major advances in the field of sleep research, and mindful deployment has the potential to enable further progress in the understanding of the neuropsychological benefits and functions of sleep.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessEditorial
The Awakening of Sleep Medicine: A Global Quest for Quality Rest and Health
by
Raffaele Ferri
Clin. Transl. Neurosci. 2024, 8(1), 12; https://doi.org/10.3390/ctn8010012 - 19 Feb 2024
Abstract
The burden of sleep disorders is a global health concern that affects millions of people worldwide [...]
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessReview
The Bidirectional Relationship between Sleep and Neurodegeneration: Actionability to Improve Brain Health
by
Abubaker Ibrahim, Birgit Högl and Ambra Stefani
Clin. Transl. Neurosci. 2024, 8(1), 11; https://doi.org/10.3390/ctn8010011 - 2 Feb 2024
Abstract
Recently, it has become increasingly clear that there is a bidirectional relationship between sleep/circadian rhythms and neurodegeneration. Knowledge about this topic further improved after the description of the glymphatic system, which is mainly active during sleep. Changes in sleep and circadian rhythms are
[...] Read more.
Recently, it has become increasingly clear that there is a bidirectional relationship between sleep/circadian rhythms and neurodegeneration. Knowledge about this topic further improved after the description of the glymphatic system, which is mainly active during sleep. Changes in sleep and circadian rhythms are present not only in overt neurodegenerative diseases but also in their early, prodromal, and preclinical phases, supporting that they precede (and contribute to) the development of neurodegeneration. This narrative review provides a brief overview of sleep and circadian rhythm disruption in neurodegeneration, highlights the bidirectional relationship between sleep changes and neurodegeneration, and addresses future perspectives, in particular, whether sleep changes are able to predict neurodegeneration and the potential sleep actionability to prevent or modulate the development of neurodegenerative diseases.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures
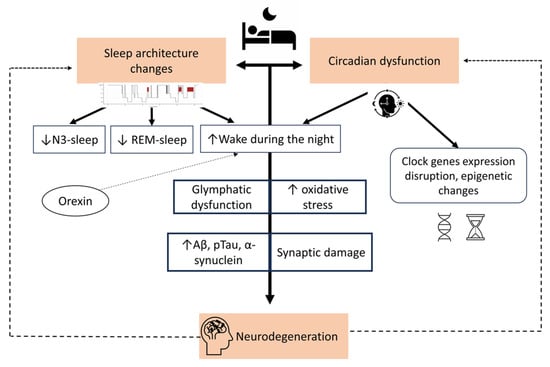
Figure 1
Open AccessCommentary
Insomnia Guidelines—The European Update 2023
by
Dieter Riemann, Raphael J. Dressle and Kai Spiegelhalder
Clin. Transl. Neurosci. 2024, 8(1), 10; https://doi.org/10.3390/ctn8010010 - 26 Jan 2024
Cited by 1
Abstract
The last ten years have seen the development and publication of numerous national and international guidelines devoted to the diagnosis and treatment of insomnia. These include guidelines by the American College of Physicians (ACP), the American Academy of Sleep Medicine (AASM), the British
[...] Read more.
The last ten years have seen the development and publication of numerous national and international guidelines devoted to the diagnosis and treatment of insomnia. These include guidelines by the American College of Physicians (ACP), the American Academy of Sleep Medicine (AASM), the British Sleep Society (BSS), the German Sleep Society (GSS), and the European Sleep Research Society (ESRS). Though coming from very diverse authors and backgrounds, these guidelines by and large agree concerning the therapeutic recommendations: cognitive behavioral treatment of insomnia (CBT-I), a multicomponent psychotherapeutic intervention, is unequivocally recommended as a first-line treatment. In this report, we will focus on the most recent guideline update from the ESRS, which was published in November 2023. After suggesting a careful diagnostic procedure, CBT-I, both applied face to face (F2F) or digitally (dCBT-I), is again recommended as a first-line treatment based on the available evidence. Hypnotic medications like benzodiazepines (BZ), benzodiazepine receptor agonists (BZRA), sedating antidepressants, and others are approved for short-term-treatment of up to four weeks. Orexin receptor antagonists (i.e., daridorexant) and prolonged release melatonin are considered as options for longer-term treatment when carefully considering the advantages and disadvantages. Both light therapy and exercise regimens were viewed as promising; however, they still lack convincing evidence for the time being. Given the fact that not every patient responds satisfactorily or even remits following CBT-I or other treatment options, the research agenda calls for the development and evaluation of new therapeutic avenues and combination therapies.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessFeature PaperReview
The Many Unknowns of Partial Sensory Disconnection during Sleep: A Review of the Literature
by
Chiara Cirelli and Giulio Tononi
Clin. Transl. Neurosci. 2024, 8(1), 9; https://doi.org/10.3390/ctn8010009 - 24 Jan 2024
Cited by 1
Abstract
When we are asleep, we lose the ability to promptly respond to external stimuli, and yet we spend many hours every day in this inherently risky behavioral state. This simple fact strongly suggests that sleep must serve essential functions that rely on the
[...] Read more.
When we are asleep, we lose the ability to promptly respond to external stimuli, and yet we spend many hours every day in this inherently risky behavioral state. This simple fact strongly suggests that sleep must serve essential functions that rely on the brain going offline, on a daily basis, and for long periods of time. If these functions did not require partial sensory disconnection, it would be difficult to explain why they are not performed during waking. Paradoxically, despite its central role in defining sleep and what sleep does, sensory disconnection during sleep remains a mystery. We have a limited understanding of how it is implemented along the sensory pathways; we do not know whether the same mechanisms apply to all sensory modalities, nor do we know to what extent these mechanisms are shared between non-rapid eye movement (NREM) sleep and REM sleep. The main goal of this contribution is to review some knowns and unknowns about sensory disconnection during sleep as a first step to fill this gap.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessReview
Sleep Health
by
Albrecht P. A. Vorster, Eus J. W. van Someren, Allan I. Pack, Reto Huber, Markus H. Schmidt and Claudio L. A. Bassetti
Clin. Transl. Neurosci. 2024, 8(1), 8; https://doi.org/10.3390/ctn8010008 - 24 Jan 2024
Cited by 2
Abstract
Together with (physical and mental) exercise, diet, and social activities, sleep is a key health behavior that occupies one third of our lives, yet remains neglected. In the first part of this review, we present the current knowledge on how sleep promotes body,
[...] Read more.
Together with (physical and mental) exercise, diet, and social activities, sleep is a key health behavior that occupies one third of our lives, yet remains neglected. In the first part of this review, we present the current knowledge on how sleep promotes body, brain, mental, occupational, and social health as well as creativity, productivity, and well-being. In the second part, we discuss how good sleep and screening for sleep–wake disorders may improve health and reduce the burden of brain, mental, cardiovascular, metabolic disorders and cancer. We also review the literature on measurements of sleep health and present the Bernese Sleep Health Questionnaire, a new and simple tool to assess sleep health and screen for sleep–wake circadian disorders in clinical practice.
Full article
(This article belongs to the Special Issue Brain Health)
►▼
Show Figures
Figure 1
Open AccessCorrection
Correction: Neumeier et al. The Loneliness of Migraine Scale: A Development and Validation Study. Clin. Transl. Neurosci. 2022, 6, 12
by
Clinical and Translational Neuroscience Editorial Office
Clin. Transl. Neurosci. 2024, 8(1), 7; https://doi.org/10.3390/ctn8010007 - 17 Jan 2024
Abstract
The Clinical and Translational Neuroscience Editorial Office would like to make the following correction to the Academic Editor listed on this published paper [...]
Full article
Open AccessHypothesis
Cellular Stress, Energy Constraints and the Energy Allocation Hypothesis of Sleep
by
Markus H. Schmidt and Kaspar A. Schindler
Clin. Transl. Neurosci. 2024, 8(1), 6; https://doi.org/10.3390/ctn8010006 - 10 Jan 2024
Abstract
A growing body of literature demonstrates a critical role for sleep in upregulating diverse biological processes related to protein synthesis, immune function, and cellular housekeeping such as intracellular transport and membrane repair. The energy allocation (EA) hypothesis places sleep in a broader context
[...] Read more.
A growing body of literature demonstrates a critical role for sleep in upregulating diverse biological processes related to protein synthesis, immune function, and cellular housekeeping such as intracellular transport and membrane repair. The energy allocation (EA) hypothesis places sleep in a broader context of resource optimization where sleep–wake partitioning of metabolic operations optimizes resource utilization. The EA hypothesis of sleep carries important implications in health, disease, and homeostatic mechanisms. Specifically, conditions that lead to cellular stress, energy constraints or depression of neuronal activity, such as epilepsy, ischemic stroke or cortical spreading depression, are here proposed to follow similar conserved processes that favor sleep. This review examines the role of local mechanisms, including cytokine release or the accumulation of adenosine, in downregulating wakefulness to favoring sleep, loss of functional connectivity and the upregulation sleep-coupled processes that promote survival.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessReview
The Two-Process Model: Origin of Its Concepts and Their Implications
by
Alexander Borbély and Irene Tobler
Clin. Transl. Neurosci. 2024, 8(1), 5; https://doi.org/10.3390/ctn8010005 - 30 Dec 2023
Abstract
The two-process model of sleep regulation has served as a conceptual framework in the last four decades for understanding sleep physiology. In the 1970s, long-term recordings of sleep in rats were obtained thanks to EEG telemetry. NonREM sleep and REM sleep were found
[...] Read more.
The two-process model of sleep regulation has served as a conceptual framework in the last four decades for understanding sleep physiology. In the 1970s, long-term recordings of sleep in rats were obtained thanks to EEG telemetry. NonREM sleep and REM sleep were found to differ in their time course and response to light-dark protocols. There were indications for their coupling to the circadian system, in particular the light-dark and the dark-light transitions. With the advent of quantitative EEG analysis, slow-wave activity in nonREM sleep was recognized as a sleep-wake-dependent variable. The term “sleep homeostasis” was coined to specify the regulated balance between sleep and waking. The regulatory homeostatic process was designated as “Process S”. In the two-process model, its interaction with the circadian pacemaker “Process C” can account for sleep duration under various experimental protocols. Local, use-dependent slow-wave activity changes were demonstrated in both humans and rats by the selective, unilateral activation of a cortical region prior to sleep. Finding that rest in invertebrates has sleep-like regulatory properties opened a new realm of animal studies. Comparative sleep studies in a broad variety of animal species confirmed the validity of the basic concepts of the two-process model. Recent studies have addressed sleep-related changes of brain temperature as an indicator of brain metabolism; the application of the model to Drosophila; the divergence of cortical and subcortical states; and sleep in an increasing number of species and taxa.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures

Figure 1
Open AccessCorrection
Correction: Schmid et al. SLEEPexpert+: Blending Internet-Based Cognitive Behavioral Therapy for Insomnia with In-Person Psychotherapy—A Feasibility Study in Routine Care. Clin. Transl. Neurosci. 2023, 7, 27
by
Clinical and Translational Neuroscience Editorial Office
Clin. Transl. Neurosci. 2024, 8(1), 4; https://doi.org/10.3390/ctn8010004 - 29 Dec 2023
Abstract
The Clinical and Translational Neuroscience Editorial Office would like to make the following correction regarding the academic editor listed in this published paper [...]
Full article
Open AccessReview
Sleep and Adolescent Depression
by
Chiara E. G. Castiglione-Fontanellaz and Leila Tarokh
Clin. Transl. Neurosci. 2024, 8(1), 3; https://doi.org/10.3390/ctn8010003 - 22 Dec 2023
Cited by 1
Abstract
Adolescence is a pivotal period of development marked by significant physiological and psychological changes, making youth particularly susceptible to mental health challenges, including depression. A growing body of research has highlighted the important role of sleep in the etiology and exacerbation of adolescent
[...] Read more.
Adolescence is a pivotal period of development marked by significant physiological and psychological changes, making youth particularly susceptible to mental health challenges, including depression. A growing body of research has highlighted the important role of sleep in the etiology and exacerbation of adolescent depression. Disruptions in sleep patterns, including insomnia and irregular sleep-wake cycles, are prevalent among depressed adolescents and can exacerbate depressive symptoms. In this review, we examine alterations to sleep behavior and physiology in adolescent depression. Furthermore, we introduce a theoretical model of hypersomnia in adolescent depression. This manuscript explores the intricate relationship between sleep and adolescent depression, with a focus on future directions for research and intervention.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures
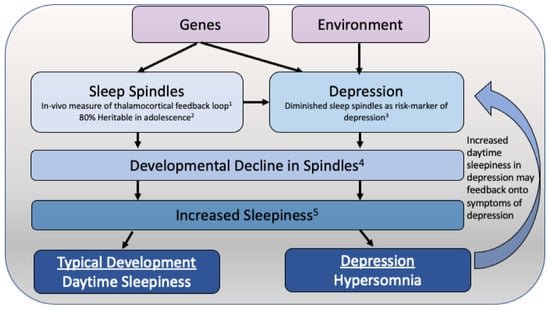
Figure 1
Open AccessFeature PaperArticle
SPHYNCS: The Use of the Swiss Narcolepsy Scale in a New Cohort of Patients with Narcolepsy and Its Borderland and Review of the Literature
by
Kseniia Zub, Jan D. Warncke, Julia van der Meer, Elena S. Wenz, Livia G. Fregolente, Panagiotis Bargiotas, Gülçin Benbir Şenel, Christian Sturzenegger, Gert Jan Lammers, Ulf Kallweit, Markus H. Schmidt, Ramin Khatami, Zhongxing Zhang, Sigrid von Manitius, Silvia Miano, Jens G. Acker, Matthias Strub and Claudio L. A. Bassetti
Clin. Transl. Neurosci. 2024, 8(1), 2; https://doi.org/10.3390/ctn8010002 - 20 Dec 2023
Abstract
Introduction and aims: Narcolepsy type 1 (NT1) is a central disorder of hypersomnolence (CDH) characterized by excessive daytime sleepiness and cataplexy. The Swiss Narcolepsy Scale (SNS), which includes the updated and short (sSNS) versions, has recently been introduced as a reliable diagnostic tool
[...] Read more.
Introduction and aims: Narcolepsy type 1 (NT1) is a central disorder of hypersomnolence (CDH) characterized by excessive daytime sleepiness and cataplexy. The Swiss Narcolepsy Scale (SNS), which includes the updated and short (sSNS) versions, has recently been introduced as a reliable diagnostic tool for identifying NT1. This study aims to assess the validity of the SNS scales in a new cohort of patients with CDH, while also introducing the French and Italian versions of the SNS and providing a summary of the existing literature on SNS. Materials and methods: The current study is based on the international Swiss Primary Hypersomnolence and Narcolepsy Cohort Study (iSPHYNCS) which aims to identify new biomarkers for CDH. Diagnostic accuracy of the SNS was assessed by calculating sensitivity, specificity, positive predictive value, and negative predictive value. Results: In our population, 108 participants with suspected CDH (including 28 NT1 patients) and 14 healthy controls completed the scale. Original SNS, updated SNS and sSNS scores showed a high sensitivity (86%, 89% and 79%, respectively) and high specificity (96%, 90% and 95%, respectively) for diagnosing NT1 compared to other CDH. The French version was completed by 5 participants, and the Italian version by 8 participants. Regarding previous studies, the SNS has now been assessed in six different populations, involving a total of 1247 subjects (including 326 with narcolepsy with cataplexy/NT1), suggesting high sensitivity (85–100%) and specificity (86–100%) of the SNS for the diagnosis of NT1. Conclusion: The SNS is a simple screening tool validated in seven languages (German, English, French, Italian, Dutch, Turkish and Japanese), demonstrating high sensitivity and specificity for the diagnosis of NT1.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
►▼
Show Figures
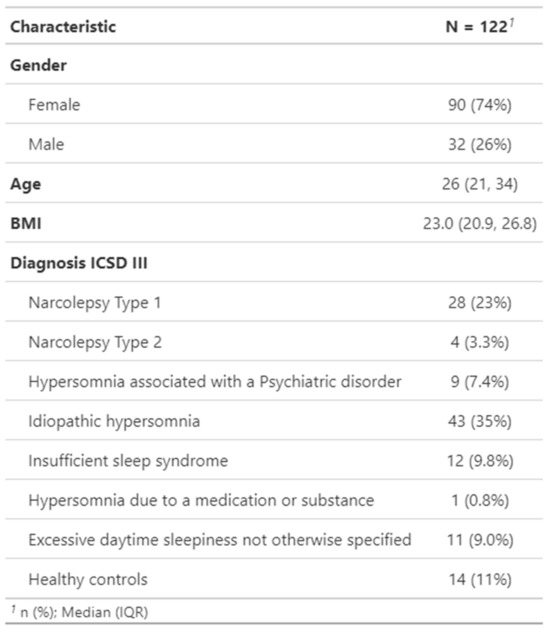
Figure 1
Open AccessFeature PaperReview
Is Sleep-Related Eating Disorder (SRED) a NREM Parasomnia or a Heterogenous Disease?
by
Nico Zobrist, Zhongxing Zhang and Ramin Khatami
Clin. Transl. Neurosci. 2024, 8(1), 1; https://doi.org/10.3390/ctn8010001 - 19 Dec 2023
Abstract
Sleep-related eating disorder (SRED) is a relatively rare but probably underestimated disorder, where affected patients exhibit nocturnal eating episodes with impaired consciousness and subsequent amnesia. SRED has originally been classified as NREM (non-rapid eye movement) parasomnia, with an obviously high number of concomitant
[...] Read more.
Sleep-related eating disorder (SRED) is a relatively rare but probably underestimated disorder, where affected patients exhibit nocturnal eating episodes with impaired consciousness and subsequent amnesia. SRED has originally been classified as NREM (non-rapid eye movement) parasomnia, with an obviously high number of concomitant sleep disorders. We suggest that SRED may represent a heterogenous disease, based on accumulating data in recent studies. Some SRED patients may be better classified as sleep-related movement disorders with an underlying dopaminergic dysfunction. Hypnotic drugs may play a crucial role in triggering amnestic SRED in both parasomnic and sleep-related movement-disordered SRED.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Open AccessReview
Pharmacological Treatments of Sleep–Wake Disorders: Update 2023
by
Marcel S. Kallweit, Nayeli P. Kallweit and Ulf Kallweit
Clin. Transl. Neurosci. 2023, 7(4), 42; https://doi.org/10.3390/ctn7040042 - 29 Nov 2023
Abstract
Biological, environmental, behavioral, and social factors can influence sleep and lead to sleep disorders or diseases. Sleep disorders are common, numerous, and heterogeneous in terms of their etiology, pathogenesis, and symptomatology. The management of sleep–wake circadian disorders (SWCDs) includes education on sleep hygiene,
[...] Read more.
Biological, environmental, behavioral, and social factors can influence sleep and lead to sleep disorders or diseases. Sleep disorders are common, numerous, and heterogeneous in terms of their etiology, pathogenesis, and symptomatology. The management of sleep–wake circadian disorders (SWCDs) includes education on sleep hygiene, behavioral strategies, psychotherapy (cognitive behavioral therapy (CBT), particularly), instrument-based treatments (i.e., positive airway pressure therapy, hypoglossal nerve stimulation), and pharmacotherapy. Depending on the disease, therapy varies and is executed sequentially or can be a combination of several forms of therapy. Drugs used for SWCDs include traditional sleep- or wake-promoting agents and chronotherapeutic agents. Recently, novel medications, which more precisely act on specific neurochemical systems (i.e., the orexin system) important for sleep and waking, are also increasingly being used. In this review, the pharmacotherapy of common sleep disorders (insomnia, sleep-related breathing disorder, central disorders of hypersomnolence, circadian rhythm sleep–wake disorders, parasomnias, and sleep-related movement disorders) embedded in the overall therapeutic concept of each disorder is presented. There is also an outlook on possible future pharmacotherapies.
Full article
(This article belongs to the Special Issue Sleep–Wake Medicine)
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
CTN
Brain Health
Guest Editors: Claudio Bassetti, Lukas Sveikata, Susanne Wegener, Indrit BègueDeadline: 31 December 2024