Evaluation of Behavior of Castable versus Machined Solid Abutments for Morse Tapper Implant Connection: A Clinical Retrospective Study
Abstract
:1. Introduction
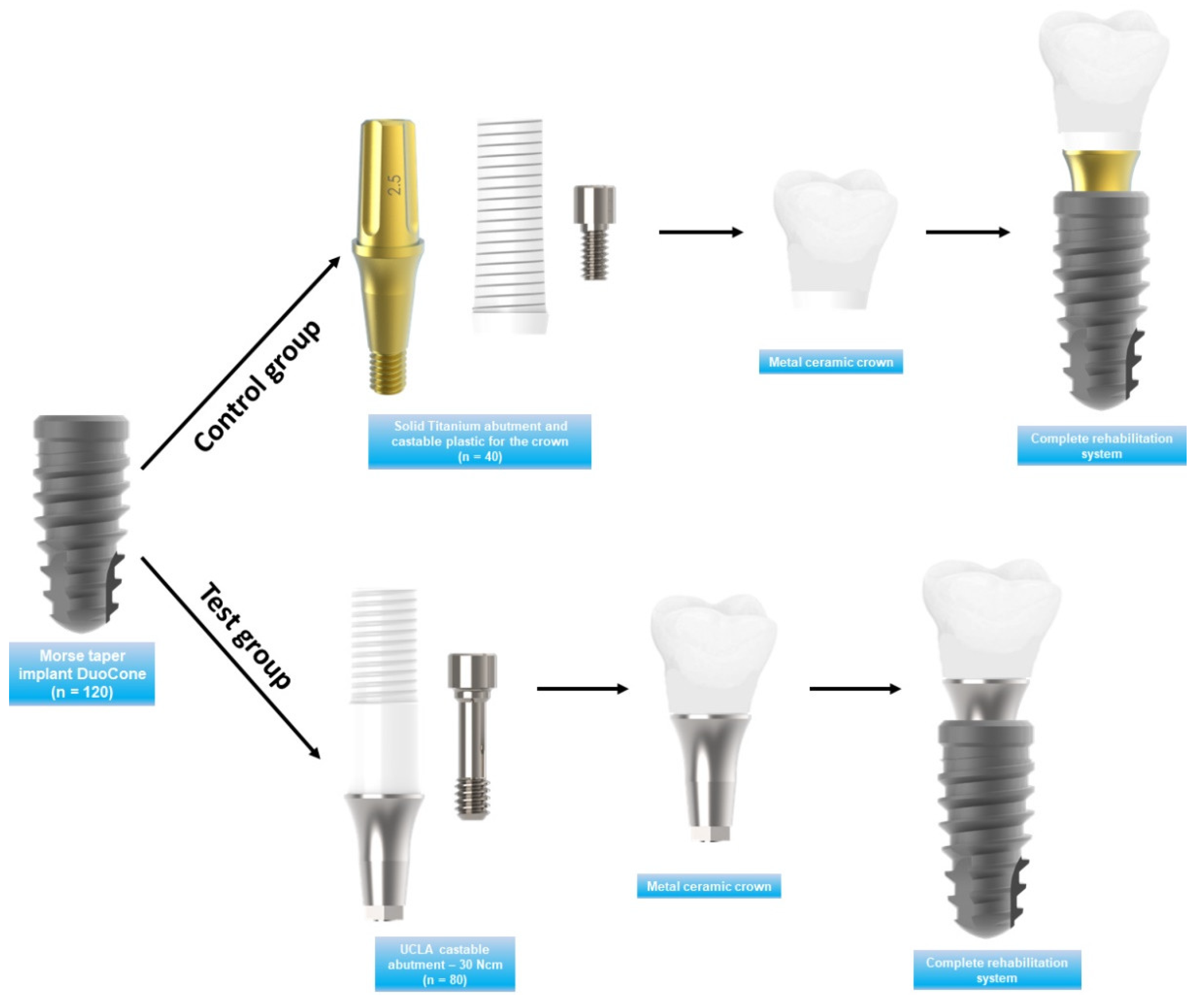
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Clinical Assessment
2.3. Radiographic Evaluation
2.4. Statistical Analysis and Sample Size Calculations
3. Results
4. Discussion
Study Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Buser, D.; Sennerby, L.; De Bruyn, H. Modern implant dentistry based on osseointegration: 50 years of progress, current trends and open questions. Periodontology 2000 2017, 73, 7–21. [Google Scholar] [CrossRef]
- Clark, D.; Levin, L. In the dental implant era, why do we still bother saving teeth? Dent. Traumatol. 2019, 35, 368–375. [Google Scholar] [CrossRef] [Green Version]
- Bianchini, M.A.; Junior, N.B.; Dedavid, B.A.; De Aza, P.N.; Gehrke, S.A. Comparative analysis of the mechanical limits of resistance in implant/abutment set of a new implant design: An in vitro study. PLoS ONE 2023, 18, e0280684. [Google Scholar] [CrossRef] [PubMed]
- Gehrke, S.A.; Júnior, J.A.; Treichel, T.L.E.; do Prado, T.D.; Dedavid, B.A.; de Aza, P.N. Effects of insertion torque values on the marginal bone loss of dental implants installed in sheep mandibles. Sci. Rep. 2022, 12, 538. [Google Scholar] [CrossRef] [PubMed]
- Francisco, H.; Finelle, G.; Bornert, F.; Sandgren, R.; Herber, V.; Warfving, N.; Pippenger, B.E. Peri-implant bone preservation of a novel, self-cutting, and fully tapered implant in the healed crestal ridge of minipigs: Submerged vs. transgingival healing. Clin. Oral. Investig. 2021, 25, 6821–6832. [Google Scholar] [CrossRef] [PubMed]
- Canullo, L.; Dehner, J.F.; Penarrocha, D.; Checchi, V.; Mazzoni, A.; Breschi, L. Soft Tissue Response to Titanium Abutments with Different Surface Treatment: Preliminary Histologic Report of a Randomized Controlled Trial. Biomed Res. Int. 2016, 2016, 2952530. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, F.; Messias, A.; Sanz-Sánchez, I.; Carrillo de Albornoz, A.; Nicolau, P.; Taylor, T.; Beuer, F.; Schär, A.; Sader, R.; Guerra, F.; et al. Influence of implant neck and abutment characteristics on peri-implant tissue health and stability. Oral Reconstr. Found. Consens. Rep. Clin. Oral Implant. Res. 2019, 30, 588–593. [Google Scholar] [CrossRef] [Green Version]
- Caricasulo, R.; Malchiodi, L.; Ghensi, P.; Fantozzi, G.; Cucchi, A. The influence of implant-abutment connection to peri-implant bone loss: A systematic review and meta-analysis. Clin. Implant. Dent. Relat. Res. 2018, 20, 653–664. [Google Scholar] [CrossRef]
- Zhang, C.; Zeng, C.; Wang, Z.; Zeng, T.; Wang, Y. Optimization of stress distribution of bone-implant interface (BII). Biomater. Adv. 2023, 147, 213342. [Google Scholar] [CrossRef]
- Vinhas, A.S.; Aroso, C.; Salazar, F.; López-Jarana, P.; Ríos-Santos, J.V.; Herrero-Climent, M. Review of the Mechanical Behavior of Different Implant-Abutment Connections. Int. J. Environ. Res. Public Health 2020, 17, 8685. [Google Scholar] [CrossRef]
- Atieh, M.A.; Almutairi, Z.; Amir-Rad, F.; Koleilat, M.; Tawse-Smith, A.; Ma, S.; Lin, L.; Alsabeeha, N.H.M. A Retrospective Analysis of Biological Complications of Dental Implants. Int. J. Dent. 2022, 2022, 1545748. [Google Scholar] [CrossRef] [PubMed]
- Gehrke, S.A.; Scarano, A.; Cortellari, G.C.; Fernandes, G.V.O.; Mesquita, A.M.M.; Bianchini, M.A. Marginal Bone Level and Biomechanical Behavior of Titanium-Indexed Abutment Base of Conical Connection Used for Single Ceramic Crowns on Morse-Taper Implant: A Clinical Retrospective Study. J. Funct. Biomater. 2023, 14, 128. [Google Scholar] [CrossRef] [PubMed]
- Ramalho, I.S.; Bergamo, E.T.P.; Witek, L.; Coelho, P.G.; Lopes, A.C.O.; Bonfante, E.A. Implant-abutment fit influences the mechanical performance of single-crown prostheses. J. Mech. Behav. Biomed. Mater. 2020, 102, 103506. [Google Scholar] [CrossRef] [PubMed]
- Lewis, S.; Beumer, J., 3rd; Hornburg, W.; Moy, P. The “UCLA” abutment. Int. J. Oral Maxillofac. Implants. 1988, 3, 37–58. [Google Scholar] [CrossRef]
- Schmitt, C.M.; Nogueira-Filho, G.; Tenenbaum, H.C.; Lai, J.Y.; Brito, C.; Döring, H.; Nonhoff, J. Performance of conical abutment (Morse Taper) connection implants: A systematic review. J. Biomed. Mater. Res. A 2014, 102, 552–574. [Google Scholar] [CrossRef]
- Pessoa, R.S.; Sousa, R.M.; Pereira, L.M.; Neves, F.D.; Bezerra, F.J.; Jaecques, S.V.; Sloten, J.V.; Quirynen, M.; Teughels, W.; Spin-Neto, R. Bone Remodeling Around Implants with External Hexagon and Morse-Taper Connections: A Randomized, Controlled, Split-Mouth, Clinical Trial. Clin. Implant Dent. Relat. Res. 2017, 19, 97–110. [Google Scholar] [CrossRef] [Green Version]
- Peruzetto, W.M.; Martinez, E.F.; Peruzzo, D.C.; Joly, J.C.; Napimoga, M.H. Microbiological Seal of Two Types of Tapered Implant Connections. Braz. Dent. J. 2016, 27, 273–277. [Google Scholar] [CrossRef] [Green Version]
- Kungsadalpipob, K.; Supanimitkul, K.; Manopattanasoontorn, S.; Sophon, N.; Tangsathian, T.; Arunyanak, S.P. The lack of keratinized mucosa is associated with poor peri-implant tissue health: A cross-sectional study. Int. J. Implant Dent. 2020, 6, 28. [Google Scholar] [CrossRef]
- Renvert, S.; Persson, G.R.; Pirih, F.Q.; Camargo, P.M. Peri-implant health, periimplant mucositis, and peri-implantitis: Case definitions and diagnostic considerations. J. Clin. Periodontol. 2018, 45 (Suppl. S20), S278–S285. [Google Scholar] [CrossRef] [Green Version]
- Gehrke, S.A.; Dedavid, B.A.; Marín, J.M.G.; Canullo, L. Behavior of implant and abutment sets of three different connections during the non-axial load application: An in vitro experimental study using a radiographic method. Biomed. Mater. Eng. 2022, 33, 101–112. [Google Scholar] [CrossRef]
- Pozzi, A.; Tallarico, M.; Moy, P.K. Three-year post-loading results of a randomised, controlled, split-mouth trial comparing implants with different prosthetic interfaces and design in partially posterior edentulous mandibles. Eur. J. Oral Implantol. 2014, 7, 47–61. [Google Scholar] [PubMed]
- Lin, M.I.; Shen, Y.W.; Huang, H.L.; Hsu, J.T.; Fuh, L.J. A retrospective study of implant-abutment connections on crestal bone level. J. Dent. Res. 2013, 92, 202S–207S. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pieri, F.; Aldini, N.N.; Marchetti, C.; Corinaldesi, G. Influence of implant-abutment interface design on bone and soft tissue levels around immediately placed and restored single-tooth implants: A randomized controlled clinical trial. Int. J. Oral Maxillofac. Implants 2011, 26, 169–178. [Google Scholar] [PubMed]
- Esposito, M.; Aparicio, C.; Xhanari, E.; Meloni, S.M.; Bolle, C.; Buti, J.; Boda, S.K.; Tallarico, M. Machined versus cast abutments for dental implants: A 1-year within-patient multicentre randomized controlled trial assessing marginal seal capacity and outcomes. Clin. Trials Dent. 2021, 3, 19–31. [Google Scholar] [CrossRef]
- Kano, S.C.; Binon, P.P.; Curtis, D.A. A classification system to measure the implant-abut- ment microgap. Int. J. Oral Maxillofac. Impl. 2007, 22, 879–885. [Google Scholar]
- Do Nascimento, C.; Barbosa, R.E.; Issa, J.P.; Watanabe, E.; Ito, I.Y.; Albuquerque, R.F., Jr. Bacterial leakage along the implant-abutment interface of pre-machined or cast components. Int. J. Oral Maxillofac. Surg. 2008, 37, 177–180. [Google Scholar] [CrossRef] [PubMed]
- Do Nascimento, C.; Barbosa, R.E.; Issa, J.P.; Watanabe, E.; Ito, I.Y.; de Albuquerque Junior, R.F. Use of checkerboard DNA-DNA hybridization to evaluate the internal contamination of dental implants and comparison of bacterial leakage with cast or pre-machined abutments. Clin. Oral Implant. Res. 2009, 20, 571–577. [Google Scholar] [CrossRef]
- Malaguti, G.; Denti, L.; Bassoli, E.; Franchi, I.; Bortolini, S.; Gatto, A. Dimensional tolerances and assembly accuracy of dental implants and machined ver- sus cast-on abutments. Clin. Impl. Dent. Relat. Res. 2011, 13, 134–140. [Google Scholar] [CrossRef] [PubMed]
- Atzenia, E.; Bassolib, E.; Dentib, L.; Gattob, A.; Iulianoa, L.; Minetolaa, P.; Salmi, A. Tolerance analysis for cast vs machined dental implants. Procedia. CIRP 2015, 33, 263–268. [Google Scholar] [CrossRef] [Green Version]
- Borges, H.; Correia, A.R.M.; Castilho, R.M.; Fernandes, G.V.O. Zirconia Implants and Marginal Bone Loss: A Systematic Review and Meta-Analysis of Clinical Studies. Int. J. Oral Maxillofac. Implants 2020, 35, 707–720. [Google Scholar] [CrossRef]
- Teigen, K.; Jokstad, A. Dental implant suprastructures using cobalt-chromium alloy compared with gold alloy framework veneered with ceramic or acrylic resin: A retrospective cohort study up to 18 years. Clin. Oral Implant. Res. 2012, 23, 853–860. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, G.V.O.; Costa, B.M.G.N.; Trindade, H.F.; Castilho, R.M.; Fernandes, J.C.H. Comparative analysis between extra-short implants (≤6 mm) and 6 mm-longer implants: A meta-analysis of randomized controlled trial. Aust. Dent. J. 2022, 67, 194–211. [Google Scholar] [CrossRef]
- Ravidà, A.; Arena, C.; Tattan, M.; Caponio, V.C.A.; Saleh, M.H.A.; Wang, H.L.; Troiano, G. The role of keratinized mucosa width as a risk factor for peri-implant disease: A systematic review, meta-analysis, and trial sequential analysis. Clin. Implant Dent. Relat Res. 2022, 24, 287–300. [Google Scholar] [CrossRef]
- Kikuchi, T.; Wada, M.; Mameno, T.; Hasegawa, D.; Serino, G.; Ikebe, K. Longitudinal study on the effect of keratinized mucosal augmentation surrounding dental implants in preventing peri-implant bone loss. Peer. J. 2022, 10, e13598. [Google Scholar] [CrossRef] [PubMed]
- Mahardawi, B.; Jiaranuchart, S.; Damrongsirirat, N.; Arunjaroensuk, S.; Mattheos, N.; Somboonsavatdee, A.; Pimkhaokham, A. The lack of keratinized mucosa as a risk factor for peri-implantitis: A systematic review and meta-analysis. Sci. Rep. 2023, 13, 3778. [Google Scholar] [CrossRef] [PubMed]
- Soares, F.M.S.; Elias, C.N.; Monteiro, E.S.; Coimbra, M.E.R.; Santana, A.I.C. Galvanic Corrosion of Ti Dental Implants Coupled to CoCrMo Prosthetic Component. Int. J. Biomater. 2021, 2021, 1313343. [Google Scholar] [CrossRef]







| Source of Variation | DF | SS | MS | p-Value |
|---|---|---|---|---|
| Abutment type | 1 | 3.549 | 3.549 | 0.001 |
| Collar height | 1 | 3.999 | 3.999 | <0.001 |
| Interaction | 1 | 0.00825 | 0.00825 | 0.873 |
| Residual | 116 | 37.541 | 0.324 | |
| Total | 119 | 45.776 | 0.385 |
| Source of Variation | DF | SS | MS | p-Value |
|---|---|---|---|---|
| Abutment type | 1 | 6.474 | 6.474 | <0.001 |
| Collar height | 1 | 3.816 | 3.816 | <0.001 |
| Interaction | 1 | 0.178 | 0.178 | 0.434 |
| Residual | 116 | 33.647 | 0.290 | |
| Total | 119 | 45.219 | 0.380 |
| Abutment Type | ||||
|---|---|---|---|---|
| Solid (n = 40) | UCLA (n = 80) | |||
| Collar Height | Mesial | Distal | Mesial | Distal |
| 1.5 (n = 49) | 1.02 ± 0.46 a,c,e | 0.88 ± 0.47 g,i | 1.37 ± 0.51 a,b,e | 1.46 ± 0.48 f,i |
| 2.5 (n = 71) | 0.61 ± 0.33 c,d | 0.57 ± 0.34 g,h | 1.00 ± 0.71 b,d | 0.99 ± 0.66 f,h |
| Comparison | Control Group (p) | Test Group (p) |
|---|---|---|
| m-MBL 7 mm × 9 mm | 0.4546 | 0.6504 |
| d-MBL 7 mm × 9 mm | 0.2423 | 0.3020 |
| m-MBL 7 mm × 11 mm | 0.5805 | 0.0351 * |
| d-MBL 7 mm × 11 mm | 0.5137 | 0.0115 * |
| m-MBL 9 mm × 11 mm | 0.8422 | 0.0005 * |
| d-MBL 9 mm × 11 mm | 0.2135 | 0.0005 * |
| Comparison (Control × Test) | p-Value |
|---|---|
| m-MBL 7 mm vs. 7 mm | 0.3484 |
| d-MBL 7 mm vs. 7 mm | 0.7773 |
| m-MBL 9 mm vs. 9 mm | 0.0003 * (lower in control) |
| d-MBL 9 mm vs. 9 mm | <0.0001 * (lower in control) |
| m-MBL 11 mm vs. 11 mm | 0.8182 |
| d-MBL 11 mm vs. 11 mm | 0.9755 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gehrke, S.A.; Scarano, A.; Cortellari, G.C.; Fernandes, G.V.O.; Watinaga, S.E.; Bianchini, M.A. Evaluation of Behavior of Castable versus Machined Solid Abutments for Morse Tapper Implant Connection: A Clinical Retrospective Study. Medicina 2023, 59, 1250. https://doi.org/10.3390/medicina59071250
Gehrke SA, Scarano A, Cortellari GC, Fernandes GVO, Watinaga SE, Bianchini MA. Evaluation of Behavior of Castable versus Machined Solid Abutments for Morse Tapper Implant Connection: A Clinical Retrospective Study. Medicina. 2023; 59(7):1250. https://doi.org/10.3390/medicina59071250
Chicago/Turabian StyleGehrke, Sergio Alexandre, Antonio Scarano, Guillermo Castro Cortellari, Gustavo Vicentis Oliveira Fernandes, Sidney Eiji Watinaga, and Marco Aurélio Bianchini. 2023. "Evaluation of Behavior of Castable versus Machined Solid Abutments for Morse Tapper Implant Connection: A Clinical Retrospective Study" Medicina 59, no. 7: 1250. https://doi.org/10.3390/medicina59071250









