A Comparison of the Impact of Two Methods of Nutrition-Behavioral Intervention on Selected Auxological and Biochemical Parameters in Obese Prepubertal Children—Crossover Preliminary Study
Abstract
:1. Introduction
2. Material and Methods
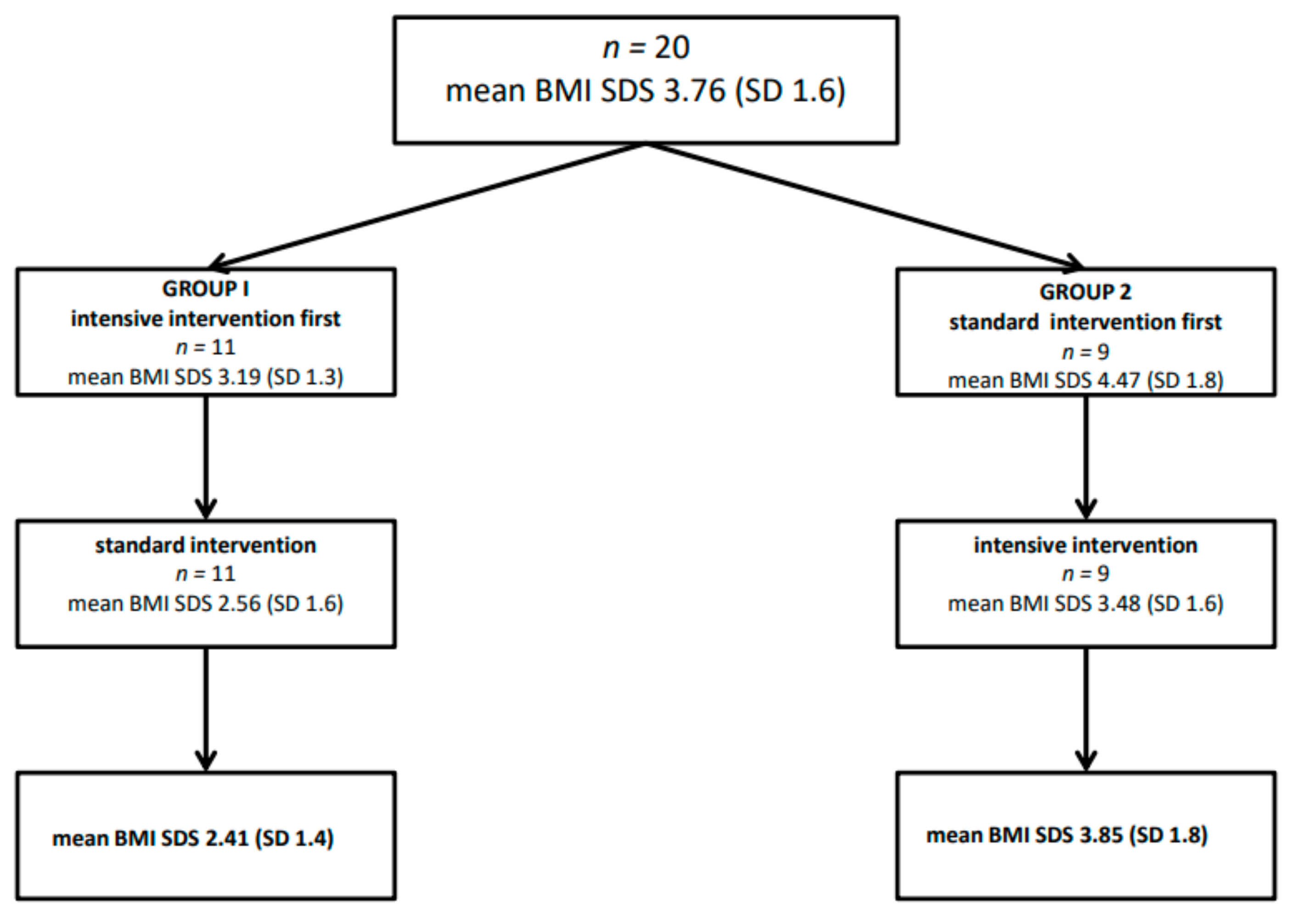
2.1. Study Group
2.2. Dietetic Intervention in the Intensive Intervention Phase
2.3. Dietetic Intervention in the Standard Intervention Phase
2.4. Physical Activity Recommendations in the Intensive Intervention Phase
2.5. Physical Activity Recommendations in the Standard Intervention Phase
2.6. Anthropometric Measurements
2.7. Biochemical Assays, Ultrasound and Blood Pressure Examinations
2.8. Statistics
2.9. Ethics
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Overweight and Obesity—BMI Statistics. Available online: http://ec.europa.eu/eurostat/statisticsexplained/index.php/Overweight_and_obesity_-_BMI_statistics (accessed on 2 April 2019).
- NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: A pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet 2017, 16, 2627–2642. [Google Scholar]
- World Health Organization. Report of the Commission on Ending Childhood Obesity; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- Weker, H.; Barańska, M.; Riahi, A.; Strucińska, M.; Więch, M.; Rowicka, G.; Dyląg, H.; Klemarczyk, W.; Bzikowska, A.; Socha, P. Dietary patterns in toddlers with excess weight. The 2016 PITNUTS study. Dev. Period Med. 2017, 21, 272–285. [Google Scholar] [PubMed]
- Manios, Y.; Androutsos, O.; Katsarou, C.; Vampouli, E.A.; Kulaga, Z.; Gurzkowska, B.; Iotova, V.; Usheva, N.; Cardon, G.; Koletzko, B.; et al. Prevalence and sociodemographic correlates of overweight and obesity in a large Pan-European cohort of preschool children and their families: The ToyBox study. Nutrition 2018, 55, 192–198. [Google Scholar] [CrossRef] [PubMed]
- Instytut Matki i Dziecka, Nadwaga i otyłość u polskich 8-latków w świetle uwarunkowań biologicznych, behawioralnych i społecznych. Raport z międzynarodowych badań WHO European Childhood Obesity SurveillanceInitiative (COSI), Warszawa, Poland. 2017. Available online: http://www.imid.med.pl/files/imid/Do%20pobrania/Raport%20COSI (accessed on 1 August 2019).
- Instytut Matki i Dziecka, Zdrowie uczniów w 2018 roku na tle nowego modelu badań HBSC, Warszawa, Poland. 2018. Available online: http://www.imid.med.pl/files/imid/Aktualnosci/Aktualnosci/raport%20HBSC%202018.pdf (accessed on 2 August 2019).
- Lissner, L.; Wijnhoven, T.M.A.; Mehlig, K.; Sjöberg, A.; Kunesova, M.; Yngve, A.; Breda, J.; Rito, A.I.; Petrauskiene, A.; Duleva, V. Socioeconomic inequalities in childhood overweight: Heterogeneity across five countries in the WHO European Childhood Obesity Surveillance Initiative (COSI-2008). Int. J. Obes. 2016, 40, 796–802. [Google Scholar] [CrossRef] [PubMed]
- Daniels, S.R.; Greer, F.R.; The AAP Committee on Nutrition. Lipid screening and cardiovascular health in childhood. Pediatrics 2008, 122, 198–208. [Google Scholar] [CrossRef] [PubMed]
- Suder, A.; Gomula, A.; Koziel, S. Central overweight and obesity in Polish schoolchildren aged 7–18 years: Secular changes of waist circumference between 1966 and 2012. Eur. J. Pediatr. 2017, 176, 909–916. [Google Scholar] [CrossRef] [PubMed]
- Giontella, A.; Bonafini, S.; Tagett, A.; Bresadola, I.; Minuz, P.; Gaudino, R.; Cavarzere, P.; Ramaroli, D.A.; Marcon, D.; Branz, L.; et al. Relation between Dietary Habits, Physical Activity, and Anthropometric and Vascular Parameters in Children Attending the Primary School in the Verona South District. Nutrients 2019, 11, 1070. [Google Scholar] [CrossRef]
- Jiménez-Aguilar, A.M.; Rodríguez-Oliveros, G.; Uribe-Carvajal, R.; González-Unzaga, M.A.; Escalante-Izeta, E.I.; Reyes-Morales, H. Design of an educational startegy based on Intervention Mapping for nutritional health promotion in Child Care Center. Eval. Program Plan. 2019, 76, 101672. [Google Scholar] [CrossRef]
- August, G.P.; Caprio, S.; Fennoy, I.; Freemark, M.; Kaufman, F.R.; Lustig, R.H.; Silverstein, J.H.; Speiser, P.W.; Styne, D.M.; Montori, V.M.; et al. Prevention and treatment of paediatric obesity: An endocrine society clinical practice guideline based on expert opinion. J. Clin. Endocrinol. Metab. 2008, 93, 4576–4599. [Google Scholar] [CrossRef]
- McGovern, L.; Johnson, J.N.; Paulo, R.; Hettinger, A.; Singhal, V.; Kamath, C.; Erwin, P.J.; Montori, V.M. Clinical review: Treatment of pediatric obesity: A systematic review and meta-analysis of randomizedtrials. J. Clin. Endocrinol. Metab. 2008, 93, 4600–4605. [Google Scholar] [CrossRef]
- Oude Luttikhuis, H.; Baur, L.; Jansen, H.; Shrewsbury, V.A.; O’Malley, C.; Stolk, R.P.; Summerbell, C.D. Summary of ‘Interventions for treating obesity in children. Evid. Based Child Health A Cochrane Rev. J. 2009, 4, 1730–1733. [Google Scholar] [CrossRef]
- Larson, T.A.; Normand, M.P.; Morley, A.J.; Hustyi, K.M. The Role of the Physical Environment in Promoting Physical Activity in Children across Different Group Compositions. Behav. Modif. 2014, 38, 837–851. [Google Scholar] [CrossRef] [PubMed]
- De Henauw, S.; Michels, N.; Vyncke, K.; Hebestreit, A.; Russo, P.; Intemann, T.; Peplies, J.; Fraterman, A.; Eiben, G.; de Lorgeril, M.; et al. On behalf of the IDEFICS consortium Blood lipids among young children in Europe: Results from the European IDEFICS study. Int. J. Obes. 2014, 38, S67–S75. [Google Scholar] [CrossRef] [PubMed]
- Mancin, M.C. Metabolic syndrome in children and adolescents-criteria for diagnosis. Diabetol. Metab. Syndr. 2009, 1, 20. [Google Scholar] [CrossRef] [PubMed]
- Szajewska, H.; Horvath, A. Żywienie i leczenie żywieniowe dzieci i młodzieży, Wyd; Medycyna Praktyczna: Kraków, Poland, 2017. (In Polish) [Google Scholar]
- Tokmakidis, S.P.; Kasambalis, A.; Christodoulos, A.D. Committee of Experts on Sports Research (1988) European test of physical fitness (EUROFIT). Fitness levels of Greek primary schoolchildren in relationship to overweight and obesity. Eur. J. Pediatr. 2006, 165, 867–874. [Google Scholar] [CrossRef] [PubMed]
- Kułaga, Z.; Litwin, M.; Tkaczyk, M. Polish 2010 growth references for school-aged children and adolescents. Eur. J. Pediatr. 2011, 170, 599–609. [Google Scholar] [CrossRef] [PubMed]
- Mccarthy, H.D.; Cole, T.J.; Fry, T.; Jebb, S.A.; Prentice, A.M. Body fat reference curves for children. Int. J. Obes. 2006, 30, 598–602. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- GFR Calculator for Children and Adolescents 1 to 17 Years Old. Bedside Schwartz and Counahan-Barratt Methods by Stephen, Z., Fadem, M.D. FASN. Available online: http://nephron.com/bedside_peds_nic.cgi (accessed on 1 June 2019).
- National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 2004, 114, 555–576. [Google Scholar] [CrossRef]
- National Institute for Health and Clinical Excellence. NICE clinical guideline. In Obesity: Identification, Assessment and Management of Overweight and Obesity in Children, Young People and Adults; NICE: London, UK, 2016. [Google Scholar]
- Wake, M.; Baur, L.A.; Gerner, B.; Gibbons, K.; Gold, L.; Gunn, J.; Levickis, P.; McCallum, Z.; Naughton, G.; Sanci, L.; et al. Outcomes and costs of primary care surveillance and intervention for overweight or obese children: The LEAP 2 randomised controlled trial. BMJ 2009, 339, b3308. [Google Scholar] [CrossRef]
- Reinehr, T.; Schaefer, A.; Winkel, K.; Finne, E.; Toschke, A.M.; Kolip, P. An effective lifestyle intervention in overweight children: Findings from a randomized controlled trial on “Obeldicks light”. Clin. Nutr. 2010, 29, 331–336. [Google Scholar] [CrossRef]
- Sandhu, J.; Ben-Shlomo, Y.; Cole, T.J.; Holly, J.; Smith, D.G. The impact of childhood body mass index on timing of puberty, adult stature and obesity: A follow-up study based on adolescent anthropometry recorded at Christ’s Hospital (1936–1964). Int. J. Obes. 2006, 30, 14–22. [Google Scholar] [CrossRef] [PubMed]
- Ho, M.; Garnett, S.P.; Baur, L.; Burrows, T.; Stewart, L.; Neve, M.; Collins, C. Effectiveness of Lifestyle Interventions in Child Obesity: Systematic Review With Meta-analysis. Pediatrics 2012, 130, e1647–e1671. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Stark, L.J.; Filigno, S.S.; Kichler, J.C.; Bolling, C.; Ratcliff, M.B.; Robson, S.M.; Simon, S.L.; BethMcCullough, M.; Clifford, L.M.; OdarStough, C.; et al. Maintenance Following a Randomized Trial of a Clinic and Home-based Behavioral Intervention of Obesity in Preschoolers. J. Pediatr. 2019, 20. [Google Scholar] [CrossRef] [PubMed]
- Cook, S.; Kavey, R.E. Dyslipidemia and pediatric obesity. Pediatr. Clin. North. Am. 2011, 58, 1363–1373. [Google Scholar] [CrossRef] [PubMed]
- Santiprabhob, J.; Leewanun, C.; Limprayoon, K.; Kiattisakthavee, P.; Wongarn, R.; Aanpreung, P.; Likitmaskul, S. Outcomes of group-based treatment program with parental involvement for the management of childhood and adolescent obesity. Patient Educ. Couns. 2014, 97, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Pedrosa, C.; Oliveira, B.M.; Albuquerque, I.; Simões-Pereira, C.; Vaz-de-Almeida, M.D.; Correia, F. Markers of metabolic syndrome in obese children before and after 1-year lifestyle intervention program. Eur. J. Nutr. 2011, 50, 391–400. [Google Scholar] [CrossRef] [PubMed]
- Levy-Marchal, C.; Arslanian, S.; Cutfield, W.; Sinaiko, A.; Druet, C. Insulin resistance in children: Consensus, perspective, and future directions. J. Clin. Endocrinol. Metab. 2010, 95, 5189–5198. [Google Scholar] [CrossRef] [PubMed]
- Pastucha, D.; Malinčíková, J.; Horák, S.; Povová, J.; Konečný, P. Effect of physical activity in treatment of paediatric obesity. Cent. Eur. J. Public Health 2015, 23, S57–S61. [Google Scholar]
- Nemet, D.; Barkan, S.; Epstein, Y.; Friedland, O.; Kowen, G.; Eliakim, A. Short-and long-term beneficial effects of a combined dietary-behavioral-physical activity intervention for the treatment of childhood obesity. Pediatrics 2005, 115, e443–e449. [Google Scholar] [CrossRef]
- Kang, H.S.; Gutin, B.; Barbeau, P.; Owens, S.; Lemmon, C.R.; Allison, J.; Litaker, M.S.; Le, N.A. Physical training improves insulin resistance syndrome markers in obese adolescents. Med. Sci. Sports Exerc. 2002, 34, 1920–1927. [Google Scholar] [CrossRef]
| Mean Change Value [SD] | Intensive Intervention | Standard Intervention | p |
|---|---|---|---|
| Δ% of weight-to-height excess | −9.8 [11.3] | −2.6 [6.5] | 0.02 * |
| ΔBMI SDS | −0.5 [0.5] | −0.2 [0.6] | 0.09 |
| Δ body fat (BF%) | −2.9 [2.4] | −1.4 [2.4] | 0.09 |
| Δ waist circumference (cm) | −2.2 [5.6] | −1.3 [5.0] | 0.9 |
| Δ hip circumference (cm) | −2.4 [2.9] | 0 [2.9] | 0.01 * |
| Δ jump length (cm) | 1 [17] | 12 [17] | 0.03 * |
| Δ time required for performing 30 crunches (s) | −4.3 [6.1] | −3.3 [6.7] | 0.9 |
| Δ systolic blood pressure (mmHg) | −3.8 [11.1] | −0.6 [9.5] | 0.3 |
| Δ diastolic blood pressure (mmHg) | −1.8 [5.0] | 1.1 [5.0] | 0.2 |
| Δ fasting blood glucose (mmol/L) | −0.02 [0.3] | 0.08 [0.5] | 0.2 |
| Δ fasting blood insulin (µIU/mL) | 1.3 [8.6] | 1.0 [12.0] | 0.5 |
| Δ HOMA IR | 0.36 [1.8] | 0.05 [3.5] | 0.7 |
| Δ fasting ALT activity (IU/L) | −7.2 [14.6] | −4.4 [15.2] | 0.7 |
| Δ fasting AST activity (IU/L) | −2.9 [9.7] | −1.4 [9.5] | 0.5 |
| Δ fasting GGT activity (IU/L) | −1.1 [2.6] | 0.6 [5.2] | 0.4 |
| Δ fasting creatinine level (µmol/L) | −0.26 [2.5] | 0.3 [3.6] | 0.7 |
| Δ eGFR | 2.3 [6.2] | 1.0 [9.2] | 0.8 |
| Δ fasting uric acid (µmol/L) | −3.1 [48.8] | 2.2 [40.5] | 0.8 |
| Δ fasting total cholesterol (mmol/L) | −0.1 [0.5] | 0.08 [0.6] | 0.5 |
| Δ fasting LDL (mmol/L) | −0.1 [0.4] | −0.1 [0.4] | 0.9 |
| Δ fasting HDL (mmol/L) | 0.07 [0.1] | 0.03 [0.1] | 0.2 |
| Δ fasting TG (mmol/L) | −0.2 [0.6] | 0.1 [0.4] | 0.07 |
| Group I | Group II | |||||||
|---|---|---|---|---|---|---|---|---|
| Baseline | After Intensive Intervention (1st Phase) | After Standard Intervention (2nd Phase) | p Value | Baseline | After Standard Intervention (1st Phase) | After Intensive Intervention (2nd Phase) | p Value | |
| mean % of weight-to-height excess [SD] | 46.3 [18.7] | 33 [22.7] (Δ = −13.3) | 29.4 [19.4] (Δ = −3.6) | p = 0.003 * p = 0.9 ** | 58.8 [13.3] | 51 [19] (Δ = −7.9) | 45.6 [16.2] (Δ = − 5.4) | p = 0.03 * p = 0.08 ** |
| mean BMI SDS | 3.1 [1.3] | 2.6 [1.6] (Δ = −0.5) | 2.4 [1.4] (Δ = −0.2) | p = 0.006 * p = 0.4 ** | 4.5 [1.8] | 3.8 [1.6] (Δ = −0.8) | 3.5 [1.6] (Δ = −0.3) | p = 0.02 * p = 0.007 ** |
| mean body fat (BF%)% | 35 [6.4] | 31.4 [5.9] (Δ = −3.6) | 30 [5.7] (Δ = −1.4) | p = 0.005 * p = 0.5 ** | 38.6 [3.9] | 36.2 [4.7] (Δ = −2,4) | 34 [5.2] (Δ = −2,2) | p = 0.02 * p = 0.007 * |
| mean waist circumference (cm) | 81 [12] | 77.2 [10.7] (Δ = −3.8) | 76 [10.4] (Δ = 1.2) | p = 0.1 * p = 0.5 ** | 84 [7.2] | 80.5 [0.4] (Δ = −3.5) | 81 [9.4] (Δ = +0,5) | p = 0.08 * p = 0.07 ** |
| mean hip circumference (cm) | 87.9 [11.4] | 85.2 [12] (Δ = −2.7) | 85.3 [11.1] (Δ = +0.1) | p = 0.04 * p = 0.06 | 89.2 [6.7] | 88 [8.4] (Δ = −1.2) | 85.9 [8.6] (Δ = −2.1) | p = 0.3 * p = 0.01 ** |
| mean jump length (cm) | 116.4 [18.2] | 113.4 [19.8] (Δ = −3) | 127.1 [15] (Δ = +13.7) | p = 0.2 * p = 0.02 ** | 101.2 [14.7] | 117 [24.8] (Δ = +16.2) | 124 [12.6] (Δ = +7) | p = 0.05 * p = 0.3 ** |
| mean time required for performing 30 crunches (s) | 37 [16.2] | 34 [12.5] (Δ = −3) | 31 [7.9] (Δ = −3) | p = 0.03 * p = 0.4 ** | 40 [4.1] | 35.2 [6.7] (Δ = −4.8) | 31 [3.2] (Δ = −4.2) | p = 0.04 * p = 0.06 ** |
| systolic blood pressure (mmHg) | 105.1 [10.2] | 101.8 [8.7] (Δ = −3.3) | 101.1 [3.3] (Δ = −0.7) | p = 0.3 * p = 0.9 ** | 106.6 [11.4] | 105.5 [8.8] (Δ = −1.1) | 102.2 [8.3] (Δ = −3.3) | p = 0.8 * p = 0.3 ** |
| diastolic blood pressure (mmHg) | 63.2 [4.6] | 60 [0.1] (Δ = −3.2) | 61.1 [3.3] (Δ = 1.1) | p = 0.06 * p = 0.9 ** | 62.2 [5.1] | 63.3 [5] (Δ = +1.1) | 63.3 [5] (Δ = 0) | p = 0.6 * p = 0.9 ** |
| fasting blood glucose (mmol/L) | 4.5 [0.4] | 4.4 [0.2] (Δ = −0.1) | 4.7 [0.3] (Δ = +0.3) | p = 0.8 * p = 0.1 ** | 4.6 [0.7] | 4.6 [0.3] (Δ = 0) | 4.6 [0.3] (Δ = 0) | p = 0.4 * p = 0.8 ** |
| fasting blood insulin (µIU/mL) | 13.5 [5.6] | 12.7 [7.1] (Δ = −0.8) | 16.9 [12.5] (Δ = −0.8) | p = 0.4 * p = 0.1 ** | 21.5 [14.6] | 13.6 [7.1] (Δ = −7.9) | 18.7 [15.7] (Δ = +5.1) | p = 0.3 * p = 0.6 ** |
| HOMA IR | 2.6 [0.9] | 3.6 [3.2] (Δ = +1) | 1.6 [2.9] (Δ = −2) | p = 0.6 * p = 0.2 ** | 4.6 [3.9] | 2.8 [1.6] (Δ = −1.8) | 3.9 [3.4] (Δ = +1.1) | p = 0.03 * p = 0.1 ** |
| fasting ALT activity (IU/L) | 32.3 [6.2] | 25.7 [5.9] (Δ = −6.6) | 25 [7.8] (Δ = −0.7) | p = 0.01 * p = 0.8 ** | 45.4 [10.9] | 38.6 [25.7] (Δ = −6.8) | 30.7 [7.7] (Δ = −7.9) | p = 0.1 * p = 0.4 ** |
| fasting AST activity (IU/L) | 29.1 [4.5] | 27.8 [2.8] (Δ = −1.3) | 27.7 [4.0] (Δ = −0.1) | p = 0.6 * p = 0.3 ** | 33.3 [8.2] | 33.3 [16.6] (Δ = 0) | 28.5 [4.3] (Δ = −4.8) | p = 0.2 * p = 0.4 ** |
| fasting GGT activity (IU/L) | 18 [6.4] | 16 [5.1] (Δ = −2) | 17.4 [10.6] (Δ = +1.4) | p = 0.2 * p = 0.32 ** | 18.8 [3.8] | 17.2 [3.8] (Δ = −1.6) | 16.9 [4.5] (Δ = −0.3) | p = 0.08 * p = 0.1 ** |
| fasting creatinine level (µmol/L) | 43.6 [4.8] | 42.9 [5.0] (Δ = −0.7) | 45.2 [6.4] (Δ = +2.3) | p = 0.4 * p = 0.8 ** | 41.7 [3.9] | 41.5 [3.4] (Δ = −0.2) | 42.4 [4.0] (Δ = +0.9) | p = 0.5 * p = 0.9 ** |
| eGFR | 118.5 [16.8] | 122.3 [19.7] (Δ = +3.8) | 117.8 [16.5] (Δ = −4.5) | p = 0.08 * p = 0.6 ** | 121.6 [12.5] | 123 [8.2] (Δ = +1.4) | 124 [9.9] (Δ = +1) | p = 0.6 * p = 0.9 ** |
| fasting uric acid (µmol/L) | 286.2 [76.2] | 266.3 [76] (Δ = −19.9) | 270.9 [89.1] (Δ = +4.6) | p = 0.5 * p = 0.8 ** | 322.5 [37.1] | 319.9 [51.6] (Δ = −2.6) | 325.2 [31.4] (Δ = +5.3) | p = 0.9 * p = 0.4 * |
| fasting total cholesterol (mmol/L) | 4.5 [0.9] | 4.3 [0.6] (Δ = −0.2) | 4.5 [0.6] (Δ = +0.2) | p = 0.1 * p = 0.3 ** | 4.4 [0.6] | 4.3 [0.6] (Δ = −0.1) | 4.4 [0.6] (Δ = +0.1) | p = 0.6 * p = 0.5 ** |
| fasting LDL (mmol/L) | 2.8 [0.7] | 2.6 [0.6] (Δ = −0.2) | 2.5 [0.5] (Δ = −0.1) | p = 0.1 * p = 0.7 ** | 2.8 [0.5] | 2.5 [0.6] (Δ = −0.3) | 2.5 [0.5] (Δ = 0) | p = 0.7 * p = 0.2 ** |
| fasting HDL (mmol/L) | 1.1 [0.2] | 1.2 [0.2] (Δ = +0.1) | 1.3 [0.3] (Δ = +0.1) | p = 0.04 * p = 0.2 ** | 1.1 [0.3] | 1.1 [0.4] (Δ = 0) | 1.2 [0.3] (Δ = +0.1) | p = 0.8 * p = 0.04 ** |
| fasting TG (mmol/L) | 1.4 [1.3] | 1.1 [0.9] (Δ = −0.3) | 1.4 [1.3] (Δ = +0.1) | p = 0.06 * p = 0.07 ** | 1.5 [0.5] | 1.4 [0.6] (Δ = −1) | 1.3 [0.5] (Δ = −1) | p = 0.5 * p = 0.7 ** |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kozioł-Kozakowska, A.; Wójcik, M.; Furtak, A.; Januś, D.; Starzyk, J.B. A Comparison of the Impact of Two Methods of Nutrition-Behavioral Intervention on Selected Auxological and Biochemical Parameters in Obese Prepubertal Children—Crossover Preliminary Study. Int. J. Environ. Res. Public Health 2019, 16, 2841. https://doi.org/10.3390/ijerph16162841
Kozioł-Kozakowska A, Wójcik M, Furtak A, Januś D, Starzyk JB. A Comparison of the Impact of Two Methods of Nutrition-Behavioral Intervention on Selected Auxological and Biochemical Parameters in Obese Prepubertal Children—Crossover Preliminary Study. International Journal of Environmental Research and Public Health. 2019; 16(16):2841. https://doi.org/10.3390/ijerph16162841
Chicago/Turabian StyleKozioł-Kozakowska, Agnieszka, Małgorzata Wójcik, Aleksandra Furtak, Dominika Januś, and Jerzy B. Starzyk. 2019. "A Comparison of the Impact of Two Methods of Nutrition-Behavioral Intervention on Selected Auxological and Biochemical Parameters in Obese Prepubertal Children—Crossover Preliminary Study" International Journal of Environmental Research and Public Health 16, no. 16: 2841. https://doi.org/10.3390/ijerph16162841







