Risk Factors Associated with Nursing Home COVID-19 Outbreaks: A Retrospective Cohort Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Setting
2.3. Outcomes and Data Sources
2.4. Analyses
3. Results
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Variable | NH (N = 57) | Participation in the Survey | p | |
|---|---|---|---|---|
| Yes (N = 45) | No (N = 12) | |||
| Total residents #, n Mean ± SD | 5145 90.3 ± 42.9 | 4158 92.4 ± 45.1 | 987 82.3 ± 33.7 | 0.399 * |
| Total beds #, n Mean ± SD | 5263 92.3 ± 43.5 | 4273 94.9 ± 45.7 | 990 82.5 ± 33.7 | 0.305 * |
| At least 1 resident COVID-19 case, n | 37 (64.9%) | 28 (75.7%) | 9 (24.3%) | 0.410 |
| Incidence of COVID-19 (%), median [p25–p75] ° | 4.8 [0–40] | 2.9 [0–39] | 17 [1.2–46] | 0.605 |
| Facility size | 0.697 | |||
| Small–medium (≤70 beds), n | 21 (36.8%) | 16 (35.6%) | 5 (41.7%) | |
| Large (>70 beds), n | 36 (63.2%) | 29 (64.4%) | 7 (58.3%) | |
| General characteristics | ||||
| NH with special care units, n | 27 (47.4%) | 22 (48.9%) | 5 (41.7%) | 0.656 |
| NH with dementia care units, n | 14 (24.6%) | 13 (28.9%) | 1 (8.3%) | 0.142 |
| NH with care units for complex clinical problems, n | 13 (22.8%) | 9 (20%) | 4 (33.3%) | 0.328 |
| Conformity to structural quality standards (yes), n | 32 (56.1%) | 25 (55.6%) | 7 (58.3%) | 0.863 |
| Metropolitan status | 0.025 | |||
| Urban, n | 18 (31.6%) | 11 (24.4%) | 7 (58.3%) | |
| Rural, n | 39 (68.4%) | 34 (75.6%) | 5 (41.7%) | |
| Geographical region | 0.274 | |||
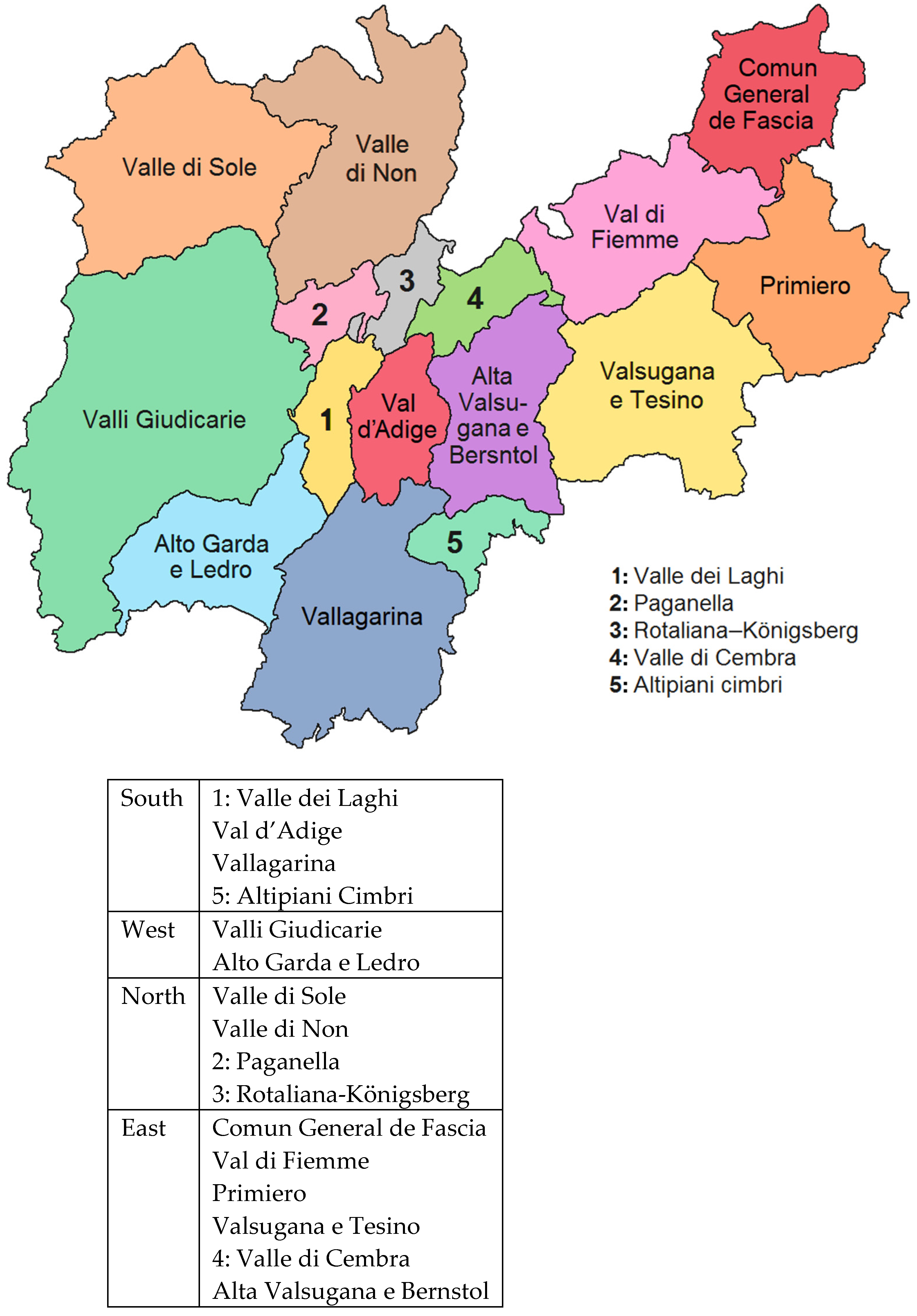
| North, n | 8 (14%) | 5 (11.1%) | 3 (25%) | |
| South, n | 21 (36.8%) | 15 (33.3%) | 6 (50%) | |
| East, n | 16 (28.1%) | 14 (31.1%) | 2 (16.7%) | |
| West, n | 12 (21.1%) | 11 (24.4%) | 1 (8.3%) | |
| Variables | |
|---|---|
| Total rooms, n (median) (IQR) | 2372 (44) (38–61) |
| Single occupancy | 581 (10) (4–19) |
| Double occupancy | 1541 (31) (22–38) |
| Triple occupancy | 125 (0) (0–3) |
| Quadruple and more occupancy | 125 (0) (0–0) |
| Staff (units), median [p25–p75] | |
| Full-time equivalent nurses | 9 [7–13] |
| Full-time equivalent physicians | 1 [0.77–1] |
| Full-time equivalent nurse aides | 38 [29–55] |
| OR (95% CI) | |
|---|---|
| Specific training on infection control and prevention | 1.9 (0.4; 10.4) |
| Presence of a committee for infection control and prevention | 17.4 (0.9; 307.2) |
| Procedure for management of residents with suspected communicable diseases | 0.8 (0.2; 4.0) |
| Policies for management of personnel at risk of infection | 0.7 (0.2; 2.8) |
| Staff is trained on the management of occupational exposures to biohazards | 0.6 (0.1; 3.2) |
| Established infection surveillance program | 0.7 (0.2; 2.9) |
| Personnel are instructed on the correct hand hygiene procedure | 0.1 (0.0; 4.0) |
| Procedure on standard and additional precautions | 0.7 (0.1; 4.1) |
| Personnel receive specific training on the correct use of PPE | 1.8 (0.3; 9.7) |
| Alcohol solution for hand hygiene is made thoroughly available | 0.7 (0.1; 3.7) |
| Staff are trained on how to prevent the spread of respiratory infections | 1.1 (0.3; 5.0) |
| Operations of routine and terminal cleaning/sanitation/disinfection are respected | 1.2 (0.2; 8.1) |
| Regular checks of the quality of the cleaning/sanitation/disinfection | 1.2 (0.2; 8.5) |
| Official documents on infection control and prevention measures | 1.8 (0.4; 8.3) |
| Official documents on outbreak management | 0.2 (0.0; 3.3) |
| Official documents on hand hygiene | 0.2 (0.0; 5.9) |
| Official documents on use of PPE | 5.7 (0.3; 100.9) |
| Official documents on isolation measures | 1.3 (0.3; 6.2) |
| Official documents on sanitation | 1.3 (0.2; 7.2) |
References
- Shi, S.M.; Bakaev, I.; Chen, H.; Travison, T.G.; Berry, S.D. Risk Factors, Presentation, and Course of Coronavirus Disease 2019 in a Large, Academic Long-Term Care Facility. J. Am. Med. Dir. Assoc. 2020, 2, 1378–1383. [Google Scholar] [CrossRef] [PubMed]
- Thompson, D.C.; Barbu, M.G.; Beiu, C.; Popa, L.G.; Mihai, M.M.; Berteanu, M.; Popescu, M.N. The Impact of COVID-19 Pandemic on Long-Term Care Facilities Worldwide: An Overview on International Issues. BioMed Res. Int. 2020, 2020, 8870249. [Google Scholar] [CrossRef] [PubMed]
- Hashan, M.R.; Smoll, N.; King, C.; Ockenden-Muldoon, A.; Walker, J.; Wattiaux, A.; Graham, J.; Booy, R.; Khandaker, G. Epidemiology and clinical features of COVID-19 outbreaks in aged care facilities: A systematic review and meta-analysis. E Clin. Med. 2021, 33, 100771. [Google Scholar]
- European Centre for Disease Prevention and Control (ECDC). Surveillance of COVID-19 in Long-Term Care Facilities in the EU/EEA; ECDC: Stockholm, Sweden, 19 May 2020; Available online: https://www.ecdc.europa.eu/en/publications-data/surveillance-COVID-19-long-term-care-facilities-EU-EEA (accessed on 20 May 2021).
- Cassone, M.; Mody, L. Measuring the outsized impact of COVID-19 in the evolving setting of aged care facilities. E Clin. Med. 2021, 34, 100825. [Google Scholar]
- Bolcato, M.; Trabucco Aurilio, M.; Di Mizio, G.; Piccioni, A.; Feola, A.; Bonsignore, A.; Tettamanti, C.; Ciliberti, R.; Rodriguez, D.; Aprile, A. The Difficult Balance between Ensuring the Right of Nursing Home Residents to Communication and Their Safety. Int. J. Environ. Res. Public Health 2021, 18, 2484. [Google Scholar] [CrossRef]
- McMichael, T.M.; Clark, S.; Pogosjans, S.; Kay, M.; Lewis, J.; Baer, A.; Kawakami, V.; Lukoff, M.D.; Ferro, J.; Brostrom-Smith, C.; et al. Public Health–Seattle & King County, Evergreen Health, and CDC COVID-19 Investigation Team. COVID-19 in a Long-Term Care Facility-King County, Washington, 27 February–9 March 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 339–342. [Google Scholar]
- Belmin, J.; Um-Din, N.; Donadio, C.; Magri, M.; Nghiem, Q.D.; Oquendo, B.; Pariel, S.; Lafuente-Lafuente, C. Coronavirus Disease 2019 Outcomes in French Nursing Homes That Implemented Staff Confinement With Residents. JAMA Netw. Open. 2020, 3, e2017533. [Google Scholar] [CrossRef] [PubMed]
- Bagchi, S.; Mak, J.; Li, Q.; Sheriff, E.; Mungai, E.; Anttila, A.; Soe, M.M.; Edwards, J.R.; Benin, A.L.; Pollock, D.A.; et al. Rates of COVID-19 Among Residents and Staff Members in Nursing Homes-United States, 25 May–22 November 2020. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 52–55. [Google Scholar] [CrossRef] [PubMed]
- van Hensbergen, M.; den Heijer, C.D.J.; Wolffs, P.; Hackert, V.; Ter Waarbeek, H.L.G.; Oude Munnink, B.B.; Sikkema, R.S.; Heddema, E.R.; Hoebe, C.J.P.A. COVID-19: First long-term care facility outbreak in the Netherlands following cross-border introduction from Germany, March 2020. BMC Infect. Dis. 2021, 21, 418. [Google Scholar] [CrossRef]
- Heudorf, U.; Müller, M.; Schmehl, C.; Gasteyer, S.; Steul, K. COVID-19 in long-term care facilities in Frankfurt am Main, Germany: Incidence, case reports, and lessons learned. GMS Hyg. Infect. Control 2020, 15, Doc26. [Google Scholar]
- Camerotto, A.; Sartorio, A.; Mazzetto, A.; Gusella, M.; Luppi, O.; Lucianò, D.; Sofritti, O.; Pelati, C.; Munno, E.; Tessari, A.; et al. Early Phase Management of the SARS-CoV-2 Pandemic in the Geographic Area of the Veneto Region, in One of the World’s Oldest Populations. Int. J. Environ. Res. Public Health 2020, 17, 9045. [Google Scholar] [CrossRef]
- Frazer, K.; Mitchell, L.; Stokes, D.; Lacey, E.; Crowley, E.; Kelleher, C. A rapid systematic review of measures to protect older people in long term care facilities from COVID-19. medRxiv 2020. [Google Scholar] [CrossRef]
- Ochieng, N.; Chidambaram, P.; Garfield, R.; Neuman, T. Factors Associated With COVID-19 Cases and Deaths in Long-Term Care Facilities: Findings from a Literature Review. Available online: https://www.kff.org/coronavirus-covid-19/issue-brief/factors-associated-with-covid-19-cases-and-deaths-in-long-term-care-facilities-findings-from-a-literature-review/view/footnotes/#footnote-508312-29 (accessed on 20 May 2021).
- Béland, D.; Marier, P. COVID-19 and Long-Term Care Policy for Older People in Canada. J. Aging Soc. Policy 2020, 32, 358–364. [Google Scholar] [CrossRef]
- Torri, E.; Sbrogiò, L.G.; Rosa, E.D.; Cinquetti, S.; Francia, F.; Ferro, A. Italian Public Health Response to the COVID-19 Pandemic: Case Report from the Field, Insights and Challenges for the Department of Prevention. Int. J. Environ. Res. Public Health 2020, 17, 3666. [Google Scholar] [CrossRef]
- Gabutti, G.; d’Anchera, E.; De Motoli, F.; Savio, M.; Stefanati, A. The Epidemiological Characteristics of the COVID-19 Pandemic in Europe: Focus on Italy. Int. J. Environ. Res. Public Health 2021, 18, 2942. [Google Scholar] [CrossRef]
- The Italian National Institute of Health (ISS). National Survey on COVID-19 Infection in Long-Stay Residential Care Homes. Final Report. 5 May 2020. (In Italian). Available online: https://www.epicentro.iss.it/coronavirus/pdf/sars-cov-2-survey-rsa-rapporto-finale.pdf (accessed on 20 May 2021).
- Eurostat. Health Statistics at Regional Level. Life Expectancy. March 2020. Available online: https://ec.europa.eu/eurostat/statiscs-explained (accessed on 20 May 2021).
- Italian Ministry of Health. Statistical Yearbook of the National Health Service, 2018. Healthcare Territorial Assistance to the Elderly [Assistenza territoriale agli anziani]. (In Italian). Available online: https://www.salute.gov.it/imgs/C_17_pubblicazioni_2980_allegato.pdf (accessed on 20 May 2021).
- Bruno Kessler Foundation (FBK). Health Situation Emergency COVID-19. Autonomous Province of Trento. (In Italian). Available online: https://covid19trentino.fbk.eu/ (accessed on 20 May 2021).
- Department of Civil Protection—Presidency of the Council of Ministers. COVID-19 Italia—Monitoring of the Situation. Daily Bulletins and Situation Maps. (In Italian). Available online: http://www.protezionecivile.gov.it/ (accessed on 20 May 2021).
- World Health Organization (WHO). COVID 19 Infection. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 20 May 2021).
- European Centre for Disease Prevention and Control (ECDC). Technical Document. Protocol for Point Prevalence Surveys of Healthcare-Associated Infections and Antimicrobial Use in European Long-Term Care Facilities—Version 2.1; ECDC: Solna Municipality, Sweden, 2016; Available online: https://www.ecdc.europa.eu/sites/default/files/media/en/publications/Publications/HALT-3-LTCF-PPS-Protocol-v2.1.pdf (accessed on 20 May 2021).
- Furmenti, M.F.; Rossello, P.; Bianco, S.; Olivero, E.; Thomas, R.; Emelurumonye, I.N.; Zotti, C.M.; HALT3 Italian Collaborating Group. Healthcare-associated infections and antimicrobial use in long-term care facilities (HALT3): An overview of the Italian situation. J. Hosp. Infect. 2019, 102, 425–430. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention (CDC). The Infection Prevention and Control Assessment Tool for Long-Term Care Facilities, Version 1.3.1, September 2016. Available online: https://www.cdc.gov/hai/pdfs/IC/CDC_IC_Assessment_Tool_LTCF.pdf (accessed on 21 May 2021).
- Montagna, M.T.; De Giglio, O.; Napoli, C.; Diella, G.; Rutigliano, S.; Agodi, A.; Auxilia, F.; Baldovin, T.; Bisetto, F.; Arnoldo, L.; et al. Control and prevention measures for legionellosis in hospitals: A cross-sectional survey in Italy. Environ. Res. 2018, 166, 55–60. [Google Scholar] [CrossRef] [PubMed]
- Institute of Statistics of the Autonomous Province of Trento (ISPAT). Statistical Yearbook 2018. (In Italian). Available online: http://www.statistica.provincia.tn.it/binary/pat_statistica_new/news/AnnStatEd2019Presentazione.1578495792.pdf (accessed on 20 May 2021).
- Backhaus, R.; Verbeek, H.; van Rossum, E.; Capezuti, E.; Hamers, J.P. Nurse staffing impact on quality of care in nursing homes: A systematic review of longitudinal studies. J. Am. Med. Dir. Assoc. 2014, 15, 383–393. [Google Scholar] [CrossRef] [PubMed]
- Ryskina, K.L.; Konetzka, R.T.; Werner, R.M. Association between 5-Star Nursing Home Report Card Ratings and Potentially Preventable Hospitalizations. Inquiry 2018, 55, 46958018787323. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine (US) Committee on Improving Quality in Long-Term Care. Improving the Quality of Long-Term Care; Wunderlich, G.S., Kohler, P.O., Eds.; National Academies Press (US): Washington, DC, USA, 2001. Available online: https://www.ncbi.nlm.nih.gov/books/NBK224500/ (accessed on 20 May 2021). [CrossRef] [Green Version]
- Sugg, M.M.; Spaulding, T.J.; Lane, S.J.; Runkle, J.D.; Harden, S.R.; Hege, A.; Iyer, L.S. Mapping community-level determinants of COVID-19 transmission in nursing homes: A multi-scale approach. Sci. Total Environ. 2021, 15, 141946. [Google Scholar] [CrossRef] [PubMed]
- White, E.M.; Kosar, C.M.; Feifer, R.A.; Blackman, C.; Gravenstein, S.; Ouslander, J.; Mor, V. Variation in SARS-CoV-2 Prevalence in U.S. Skilled Nursing Facilities. J. Am. Geriatr. Soc. 2020, 68, 2167–2173. [Google Scholar] [CrossRef]
- Gorges, R.J.; Konetzka, R.T. Staffing levels and COVID-19 cases and outbreaks in U.S. nursing homes. J. Am. Geriatr. Soc. 2020, 68, 2462–2466. [Google Scholar] [CrossRef] [PubMed]
- Malikov, K.; Huang, Q.; Shi, S.; Stall, N.M.; Tuite, A.R.; Hillmer, M.P. Temporal Associations between Community Incidence of COVID-19 and Nursing Home Outbreaks in Ontario, Canada. J. Am. Med. Dir. Assoc. 2021, 22, 260–262. [Google Scholar] [CrossRef] [PubMed]
- Gardner, W.; States, D.; Bagley, N. The Coronavirus and the Risks to the Elderly in Long-Term Care. J. Aging Soc. Policy 2020, 32, 310–315. [Google Scholar] [CrossRef] [Green Version]
- He, M.; Li, Y.; Fang, F. Is There a Link between Nursing Home Reported Quality and COVID-19 Cases? Evidence from California Skilled Nursing Facilities. J. Am. Med. Dir. Assoc. 2020, 21, 905–908. [Google Scholar] [CrossRef] [PubMed]
- Braun, R.T.; Yun, H.; Casalino, L.P.; Myslinski, Z.; Kuwonza, F.M.; Jung, H.Y.; Unruh, M.A. Comparative Performance of Private Equity-Owned US Nursing Homes During the COVID-19 Pandemic. JAMA Netw. Open. 2020, 3, e2026702. [Google Scholar] [CrossRef]
- Fisman, D.N.; Bogoch, I.; Lapointe-Shaw, L.; McCready, J.; Tuite, A.R. Risk Factors Associated With Mortality Among Residents With Coronavirus Disease 2019 (COVID-19) in Long-term Care Facilities in Ontario, Canada. JAMA Netw. Open. 2020, 3, e2015957. [Google Scholar] [CrossRef]
- Unruh, M.A.; Yun, H.; Zhang, Y.; Braun, R.T.; Jung, H.-Y. Nursing home characteristics associated with COVID-19 deaths in Connecticut, New Jersey, and New York. J. Am. Med. Dir. Assoc. 2020, 21, 1001–1003. [Google Scholar] [CrossRef]
- Gopal, R.; Han, X.; Yaraghi, N. Compress the curve: A cross-sectional study of variations in COVID-19 infections across California nursing homes. BMJ Open. 2021, 11, e042804. [Google Scholar] [CrossRef]
- Stall, N.M.; Jones, A.; Brown, K.A.; Rochon, P.A.; Costa, A.P. For-profit long-term care homes and the risk of COVID-19 outbreaks and resident deaths. CMAJ 2020, 192, E946–E955. [Google Scholar] [CrossRef]
- Gmehlin, C.G.; Munoz-Price, L.S. Coronavirus disease 2019 (COVID-19) in long-term care facilities: A review of epidemiology, clinical presentations, and containment interventions. Infect. Control Hosp. Epidemiol. 2020, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Public Health England. Factors Associated with COVID-19 in CARE homes and Domiciliary Care, and Effectiveness of Interventions: A Rapid Review. 2020. Available online: https://phe.koha-ptfs.co.uk/cgi-bin/koha/opac-retrieve-file.pl?id=1bc5eb8d6e5ef9a43c248ef08549ee53 (accessed on 20 May 2021).
- Zimmerman, S.; Dumond-Stryker, C.; Tandan, M.; Preisser, J.S.; Wretman, C.J.; Howell, A.; Ryan, S. Nontraditional Small House Nursing Homes Have Fewer COVID-19 Cases and Deaths. J. Am. Med. Dir. Assoc. 2021, 22, 489–493. [Google Scholar] [CrossRef]
- Abrams, H.R.; Loomer, L.; Gandhi, A.; Grabowski, D.C. Characteristics of U.S. Nursing Homes with COVID-19 Cases. J. Am. Geriatr. Soc. 2020, 68, 1653–1656. [Google Scholar] [CrossRef]
- Figueroa, J.F.; Wadhera, R.K.; Papanicolas, I.; Riley, K.; Zheng, J.; Orav, E.J.; Jha, A.K. Association of nursing home ratings on health inspections, quality of care, and nurse staffing with COVID-19 cases. JAMA 2020, 324, 1103–1105. [Google Scholar] [CrossRef] [PubMed]
- Bui, D.P.; See, I.; Hesse, E.M.; Varela, K.; Harvey, R.R.; August, E.M.; Winquist, A.; Mullins, S.; McBee, S.; Thomasson, E.; et al. Association Between CMS Quality Ratings and COVID-19 Outbreaks in Nursing Homes—West Virginia, 17 March–11 June 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 1300–1304. [Google Scholar] [CrossRef]
- Harrington, C.; Ross, L.; Chapman, S.; Halifax, E.; Spurlock, B.; Bakerjian, D. Nurse Staffing and Coronavirus Infections in California Nursing Homes. Policy Polit. Nurs. Pract. 2020, 21, 174–186. [Google Scholar] [CrossRef]
- Chatterjee, P.; Kelly, S.; Qi, M.; Werner, R.M. Characteristics and Quality of US Nursing Homes Reporting Cases of Coronavirus Disease 2019 (COVID-19). JAMA Netw. Open. 2020, 3, e2016930. [Google Scholar] [CrossRef] [PubMed]
- Rolland, Y.; Lacoste, M.H.; de Mauleon, A.; Ghisolfi, A.; De Souto Barreto, P.; Blain, H.; Villars, H. Guidance for the Prevention of the COVID-19 Epidemic in Long-Term Care Facilities: A Short-Term Prospective Study. J. Nutr. Health Aging 2020, 24, 812–816. [Google Scholar] [CrossRef]
- Herzig, C.T.; Stone, P.W.; Castle, N.; Pogorzelska-Maziarz, M.; Larson, E.L.; Dick, A.W. Infection Prevention and Control Programs in US Nursing Homes: Results of a National Survey. J. Am. Med. Dir. Assoc. 2016, 17, 85–88. [Google Scholar] [CrossRef] [Green Version]
- Kariya, N.; Sakon, N.; Komano, J.; Tomono, K.; Iso, H. Current prevention and control of health care-associated infections in long-term care facilities for the elderly in Japan. J. Infect. Chemother. 2018, 24, 347–352. [Google Scholar] [CrossRef]
- Lee, M.H.; Lee, G.A.; Lee, S.H.; Park, Y.H. Effectiveness and core components of infection prevention and control programmes in long-term care facilities: A systematic review. J. Hosp. Infect. 2019, 102, 377–393. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rios, P.; Radhakrishnan, A.; Williams, C.; Ramkissoon, N.; Pham, B.; Cormack, G.V.; Grossman, M.R.; Muller, M.P.; Straus, S.E.; Tricco, A.C. Preventing the transmission of COVID-19 and other coronaviruses in older adults aged 60 years and above living in long-term care: A rapid review. Syst. Rev. 2020, 9, 218. [Google Scholar] [CrossRef] [PubMed]
- U.S. Government Accountability Office (GAO). Infection Control Deficiencies Were Widespread and Persistent in Nursing Homes Prior to COVID-19 Pandemic. Available online: https://www.gao.gov/products/gao-20-576r (accessed on 20 May 2021).
- Tinelli, M.; Tiseo, G.; Falcone, M.; ESCMID Study Group for Infections in the Elderly. Prevention of the spread of multidrug-resistant organisms in nursing homes. Aging Clin. Exp. Res. 2021, 33, 679–687. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Infection Prevention and Control during Health Care When Coronavirus Disease (COVID-19) Is Suspected or Confirmed: Interim Guidance, 29 June 2020. Available online: https://apps.who.int/iris/handle/10665/332879 (accessed on 20 May 2021).
- Lombardo, F.L.; Bacigalupo, I.; Salvi, E.; Lacorte, E.; Piscopo, P.; Mayer, F.; Ancidoni, A.; Remoli, G.; Bellomo, G.; Losito, G.; et al. Italian National Institute of Health Nursing Home Study Group. The Italian national survey on Coronavirus disease 2019 epidemic spread in nursing homes. Int. J. Geriatr. Psychiatry 2021, 36, 873–882. [Google Scholar] [CrossRef]
- Islam, M.S.; Rahman, K.M.; Sun, Y.; Qureshi, M.O.; Abdi, I.; Chughtai, A.A.; Seale, H. Current knowledge of COVID-19 and infection prevention and control strategies in healthcare settings: A global analysis. Infect. Control Hosp. Epidemiol. 2020, 41, 1196–1206. [Google Scholar] [CrossRef]
- Anderson, D.C.; Grey, T.; Kennelly, S.; O’Neill, D. Nursing Home Design and COVID-19: Balancing Infection Control, Quality of Life, and Resilience. J. Am. Med. Dir. Assoc. 2020, 21, 1519–1524. [Google Scholar] [CrossRef]
- Behrens, L.L.; Naylor, M.D. We are Alone in This Battle: A Framework for a Coordinated Response to COVID-19 in Nursing Homes. J. Aging Soc. Policy. 2020, 32, 316–322. [Google Scholar] [CrossRef]
- Heckman, G.A.; Kay, K.; Morrison, A.; Grabowski, D.C.; Hirdes, J.P.; Mor, V.; Shaw, G.; Benjamin, S.; Boscart, V.M.; Costa, A.P.; et al. Proceedings from an International Virtual Townhall: Reflecting on the COVID-19 Pandemic: Themes from Long-Term Care. J. Am. Med. Dir. Assoc. 2021, 22, 1128–1132. [Google Scholar] [CrossRef]


| Variables | |
|---|---|
| Infection prevention and control measures (presence of), n (% facilities) | |
| Specific training on infection control and prevention | 11 (24.4%) |
| Presence of a committee for infection control and prevention | 3 (6.7%) |
| Procedure for management of residents with suspected communicable diseases | 32 (71.1%) |
| Policies for management of personnel at risk of infection | 23 (51.1%) |
| Training of staff on the management of occupational exposures to biohazards | 32 (71.1%) |
| Established infection surveillance program | 19 (42.2%) |
| Training of staff on the correct hand hygiene procedure | 43 (95.6%) |
| Procedure on standard and additional precautions | 35 (77.8%) |
| Training of staff on the correct use of personal protective equipment (PPE) | 33 (73.3%) |
| Availability of hand hygiene supplies | 33 (73.3%) |
| Training of staff on how to prevent the spread of respiratory infections | 21 (46.7%) |
| Compliance with operations of routine and terminal cleaning/sanitation/disinfection | 37 (82.2%) |
| Official protocols/procedures on infection control and prevention | 19 (42.2%) |
| Outbreak management | 5 (11.1%) |
| Hand hygiene | 43 (95.6%) |
| Use of PPE | 42 (93.3%) |
| Isolation measures | 25 (55.6%) |
| Sanitation | 33 (73.3%) |
| Variable | Median Cumulative Incidence of COVID-19 Cases (%) [p25–p75] | p |
|---|---|---|
| Facility size | 0.930 | |
| Small–medium (≤70 beds), (16) | 1.8 [0–48] | |
| Large (>70 beds), (29) | 7.4 [0–36] | |
| General characteristics | ||
| Special care units | 0.174 | |
| yes (22) | 19 [0–40] | |
| no (23) | 1.1 [0–39] | |
| Dementia | 0.421 | |
| yes (13) | 14 [0–45] | |
| no (32) | 1.6 [0–37] | |
| Complex clinical problems | 0.444 | |
| yes (9) | 24 [0.53–36] | |
| no (36) | 1.8 [0–40] | |
| Conformity to quality standards | 0.990 | |
| yes (25) | 1.6 [0–42] | |
| no (20) | 10 [0–32] | |
| Metropolitan status | 0.567 | |
| Urban (11) | 0.53 [0–36] | |
| Rural (34) | 3.8 [0–42] | |
| Geographical region | 0.002 | |
| North (5) | 1.1 [0–44.6] | |
| South (15) | 0 [0–24.2] | |
| East (14) | 0.8 [0–4.8] | |
| West (11) | 45.2 [24–55.9] | |
| Infection control measures | ||
| Specific training on infection control and prevention | 0.388 | |
| yes (11) | 14 [0–47.9] | |
| no (34) | 1.8 [0–28.1] | |
| Presence of a committee for infection control and prevention | 0.081 | |
| yes (3) | 47.9 [14–54.8] | |
| no (42) | 1.8 [0–35.9] | |
| Procedure for management of residents with suspected communicable diseases | 0.871 | |
| yes (32) | 4.4 [0–39] | |
| no (13) | 1.9 [0.5–35.9] | |
| Policies for management of personnel at risk of infection | 0.341 | |
| yes (23) | 1.6 [0–28] | |
| no (22) | 13.5 [0–44.6] | |
| Training of staff on the management of occupational exposures to biohazards | 0.952 | |
| yes (32) | 3.8 [0–39.4] | |
| no (13) | 1.9 [0–35.9] | |
| Established infection surveillance program | 0.749 | |
| yes (19) | 2.9 [0–24.5] | |
| no (26) | 3.3 [0–42] | |
| Training of staff on the correct hand hygiene procedure | 0.553 | |
| yes (43) | 2.9 [0–38.5] | |
| no (2) | 23.1 [1.6–44.6] | |
| Procedure on standard and additional precautions | 0.365 | |
| yes (35) | 1.6 [0–40.3] | |
| no (10) | 18.6 [1.9–38.5] | |
| Training of staff on the correct use of PPE | 0.301 | |
| yes (33) | 4.8 [0–40.3] | |
| no (12) | 0.8 [0–30] | |
| Availability of hand hygiene supplies | 0.571 | |
| yes (33) | 1.6 [0–35.9] | |
| no (12) | 8.8 [0–44.9] | |
| Training of staff on how to prevent the spread of respiratory infections | 0.269 | |
| yes (21) | 4.8 [0–24.5] | |
| no (24) | 2.4 [0–44.9] | |
| Compliance with operations of routine and terminal cleaning/sanitation/disinfection | 0.553 | |
| yes (37) | 1.9 [0–38.5] | |
| no (8) | 9.4 [0.8–40] | |
| Regular checks of the quality of the cleaning/sanitation/disinfection | 0.918 | |
| yes (37) | 2.9 [0–35.9] | |
| no (8) | 14.1 [0–43.3] | |
| Official protocols/procedures on | ||
| infection control and prevention | 0.123 | |
| yes (19) | 24 [0–45.2] | |
| no (26) | 1.6 [0–24.2] | |
| Outbreak management | 0.087 | |
| yes (5) | 0 [0–0] | |
| no (40) | 5.4 [0–40.3] | |
| Hand hygiene | 0.915 | |
| yes (43) | 2.9 [0–40.3] | |
| no (2) | 7.8 [1.6–14] | |
| use of PPE | 0.742 | |
| yes (42) | 3.8 [0–40.3] | |
| no (3) | 0.5 [0–38.5] | |
| Isolation measures | 0.941 | |
| yes (25) | 2.9 [0–40] | |
| no (20) | 3.3 [0.3–24.2] | |
| Sanitation | 0.408 | |
| yes (33) | 1.6 [0–40.3] | |
| no (12) | 9.4 [0.8–31.4] | |
| Variable | Confirmed COVID-19 Cases | p | |
|---|---|---|---|
| Yes (N = 37) | No (N = 20) | ||
| Residents, mean ± SD | 95.8 ± 47.8 | 80.0 ± 30.3 | 0.188 |
| Beds, mean ± SD | 96.7 ± 48.0 | 84.2 ± 33.0 | 0.306 |
| Facility size | 0.716 | ||
| Small–medium (≤70 beds), n | 13 (35.1%) | 8 (40%) | |
| Large (>70 beds), n | 24 (64.9%) | 12 (60%) | |
| General characteristics | |||
| Special care units | 0.169 | ||
| yes, n | 20 (54%) | 7 (35%) | |
| no, n | 17 (45%) | 13 (65%) | |
| Dementia | 0.749 | ||
| yes, n | 10 (27%) | 4 (20%) | |
| no, n | 27 (73%) | 16 (80%) | |
| Complex clinical problems | 0.346 | ||
| yes, n | 10 (27%) | 3 (15%) | |
| no, n | 27 (73%) | 17 (85%) | |
| Conformity to quality standards | 0.492 | ||
| yes, n | 22 (59.5%) | 10 (50%) | |
| no, n | 15 (40.5%) | 10 (50%) | |
| Metropolitan status | 0.683 | ||
| Urban, n | 11 (29.7%) | 7 (35%) | |
| Rural, n | 26 (70.1%) | 13 (65%) | |
| Geographical region | 0.100 | ||
| North, n | 6 (16.2%) | 2 (10%) | |
| South, n | 12 (32.4%) | 9 (45%) | |
| East, n | 8 (21.6%) | 8 (40%) | |
| West, n | 11 (29.7%) | 1 (5%) | |
| Single-occupancy rooms | |||
| (% over total rooms per facility), median [p25–p75] | 18 [13–34] | 27 [12–32] | 0.620 |
| Full-time equivalent nurses, median [p25–p75] | 9.8 [7.3–14] | 9 [7–10] | 0.391 |
| Full-time equivalent physicians, median [p25–p75] | 1 [0.7–1.4] | 1 [1–1] | 0.732 |
| Full-time equivalent aid staff, median [p25–p75] | 37 [30–64] | 38 [28–52] | 0.622 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cazzoletti, L.; Zanolin, M.E.; Tocco Tussardi, I.; Alemayohu, M.A.; Zanetel, E.; Visentin, D.; Fabbri, L.; Giordani, M.; Ruscitti, G.; Benetollo, P.P.; et al. Risk Factors Associated with Nursing Home COVID-19 Outbreaks: A Retrospective Cohort Study. Int. J. Environ. Res. Public Health 2021, 18, 8434. https://doi.org/10.3390/ijerph18168434
Cazzoletti L, Zanolin ME, Tocco Tussardi I, Alemayohu MA, Zanetel E, Visentin D, Fabbri L, Giordani M, Ruscitti G, Benetollo PP, et al. Risk Factors Associated with Nursing Home COVID-19 Outbreaks: A Retrospective Cohort Study. International Journal of Environmental Research and Public Health. 2021; 18(16):8434. https://doi.org/10.3390/ijerph18168434
Chicago/Turabian StyleCazzoletti, Lucia, Maria Elisabetta Zanolin, Ilaria Tocco Tussardi, Mulubirhan Assefa Alemayohu, Ernesto Zanetel, Donatella Visentin, Luca Fabbri, Massimo Giordani, Giancarlo Ruscitti, Pier Paolo Benetollo, and et al. 2021. "Risk Factors Associated with Nursing Home COVID-19 Outbreaks: A Retrospective Cohort Study" International Journal of Environmental Research and Public Health 18, no. 16: 8434. https://doi.org/10.3390/ijerph18168434






