Job Insecurity in Nursing: A Bibliometric Analysis
Abstract
:1. Introduction
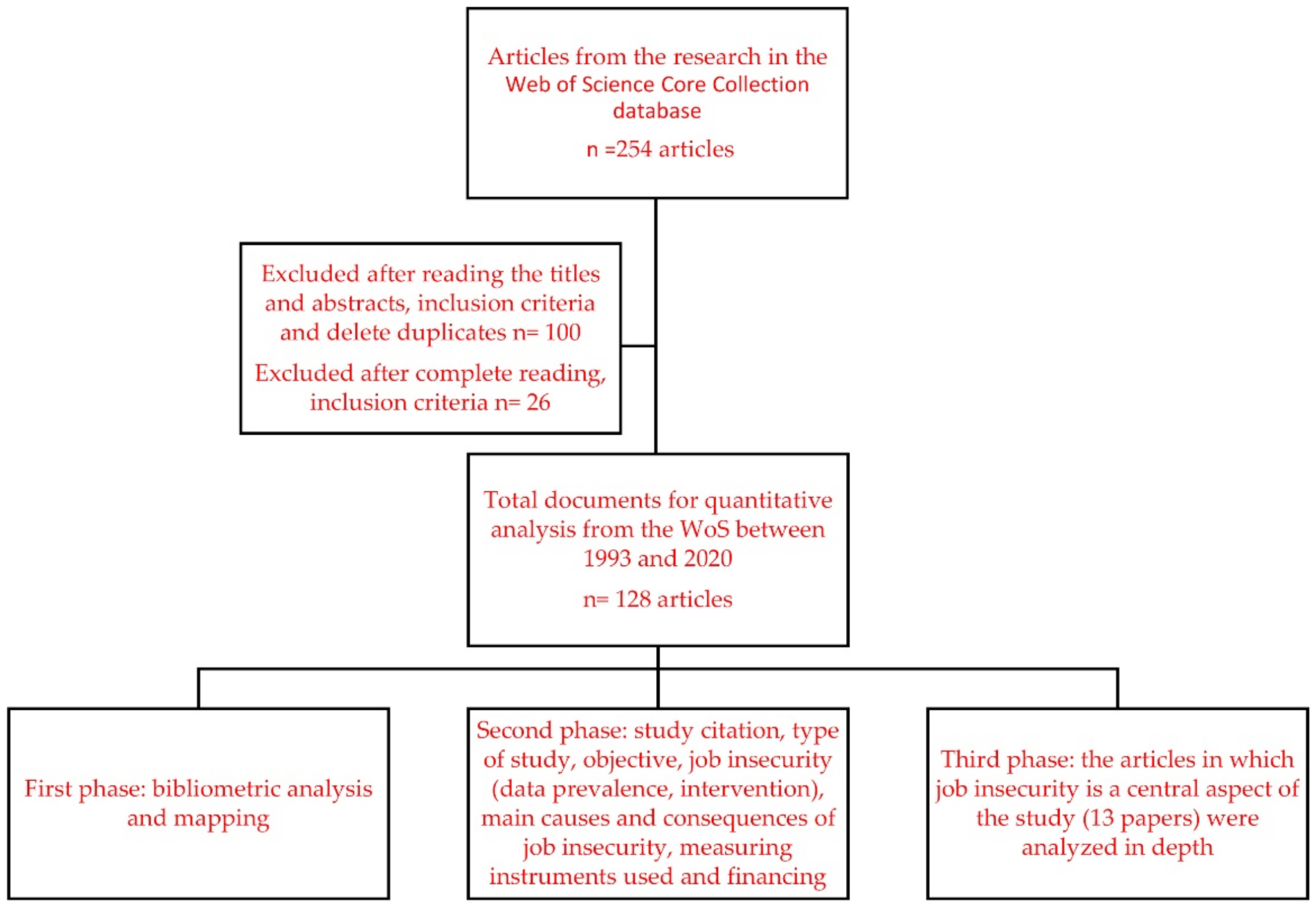
2. Materials and Methods
3. Results
3.1. Main Bibliometric Indicators
3.1.1. Co-Author Network
3.1.2. Co-Citations Network
3.1.3. Thematic Analysis
3.2. Main Results
3.2.1. Causes and Consequences of Job Insecurity
3.2.2. In-Depth Analysis of Papers in Which Job Insecurity is a Central Topic
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bakker, A.B.; Demerouti, E. Job demands-resources theory: Taking stock and looking forward. J. Occup. Health Psychol. 2017, 22, 273–285. [Google Scholar] [CrossRef]
- Topcic, M.; Baum, M.; Kabst, R. Are high-performance work practices related to individually perceived stress? A job demands-resources perspective. Int. J. Hum. Resour. Manag. 2016, 27, 45–66. [Google Scholar] [CrossRef]
- Cox, T.; Griffiths, A. The nature and measurement of work-related stress: Theory and practice. In Evaluation of Human Work; Routledge: Abingdon, UK, 2005. [Google Scholar]
- Shoss, M.K. Job insecurity: An integrative review and agenda for future research. J. Manag. 2017, 43, 1911–1939. [Google Scholar] [CrossRef]
- Sverke, M.; Hellgren, J.; Näswall, K. No security: A meta-analysis and review of job insecurity and its consequences. J. Occup. Health Psychol. 2002, 7, 242–263. [Google Scholar] [CrossRef] [PubMed]
- De Witte, H.; Vander Elst, T.; De Cuyper, N. Job insecurity, health and well-being. In Sustainable Working Lives; Springer: Dordrecht, The Netherlands, 2015; pp. 109–128. [Google Scholar]
- Cheng, G.H.L.; Chan, D.K.S. Who suffers more from job insecurity? A meta-analytic review. Appl. Psychol. Int. Rev. 2008, 57, 272–303. [Google Scholar] [CrossRef]
- Ruokolainen, M.; Mauno, S.; Cheng, T. Are the most dedicated nurses more vulnerable to job insecurity? Age-Specific analyses on family-related outcomes. J. Nurs. Manag. 2014, 22, 1042–1053. [Google Scholar] [CrossRef] [PubMed]
- Karasek, R.; Theorell, T. Healthy Work. Stress, Productivity, and the Reconstruction of Working Life; Basic Books: New York, NY, USA, 1990. [Google Scholar]
- Kalil, A.; Ziol-Guest, K.M.; Hawkley, L.C.; Cacioppo, J.T. Job insecurity and change over time in health among older men and women. J. Gerontol. B Psychol. Sci. Soc. Sci. 2010, 65B, 81–90. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Johnson, J.V.; Hall, E.M. Job strain, work place social support and cardiovascular disease: A cross-sectional study of a random sample of the Swedish working population. Am. J. Public Health 1988, 78, 1336–1342. [Google Scholar] [CrossRef] [Green Version]
- Hijzen, A.; Menyhert, B. Measuring Labour Market Security and Assessing Its Implications for Individual Well-Being; OECD Publishing: Paris, France, 2016. [Google Scholar]
- De Witte, H.; Pienaar, J.; De Cuyper, N. Review of 30 years of longitudinal studies on the association between job insecurity and health and well-being: Is there causal evidence? Aust. Psychol. 2016, 51, 18–31. [Google Scholar] [CrossRef]
- Fischmann, G.; De Witte, H.; Sulea, C.; Iliescu, D. Qualitative job insecurity and in-role performance: A bidirectional longitudinal relationship? Eur. J. Work Organ. Psychol. 2018, 27, 603–615. [Google Scholar] [CrossRef]
- Sverke, M.; Låstad, L.; Hellgren, J.; Richter, A.; Näswall, K. A meta-analysis of job insecurity and employee performance: Testing temporal aspects, rating source, welfare regimes, and union density as moderators. Int. J. Environ. Res. Public Health 2019, 16, 2536. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- OECD. Towards a Multi-Dimensional Framework for Inclusive Growth. Inclusive Growth; OECD Publishing: Paris, France, 2014. [Google Scholar]
- World Health Organization. State of the World’s Nursing 2020: Investing in Education, Jobs and Leadership. License: CC BY-NC-SA 3.0 IG. Available online: http://apps.who.int/iris (accessed on 15 August 2020).
- Antwi, Y.A.; Bowblis, J.R. The impact of nurse turnover on quality of care and mortality in nursing homes: Evidence from the great recession. Am. J. Health Econ. 2018, 4, 131–163. [Google Scholar] [CrossRef] [Green Version]
- Galbany-Estragués, P.; Millán-Martínez, P.; Pastor-Bravo, M.; Nelson, S. Emigration and job security: An analysis of workforce trends for Spanish-trained nurses (2010–2015). J. Nurs. Manag. 2019, 27, 1224–1232. [Google Scholar] [CrossRef] [PubMed]
- Llop-Gironés, A.; Tarafa, G.; Benach, J. Personal de enfermería, condiciones de trabajo y su impacto en la salud [Nursing Staff, Working Conditions and Their Impact on Health]. Gaceta Sanitaria 2015, 29, 155–156. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wisniewski, D.; Silva, E.S.; Évora, Y.D.M.; Matsuda, L.M. The professional satisfaction of the nursing team vs. work conditions and relations: A relational study. Texto e Contexto Enfermagem 2015, 24, 850–858. [Google Scholar] [CrossRef]
- Yasin, Y.M.; Kerr, M.S.; Wong, C.A.; Bélanger, C.H. Factors affecting job satisfaction among acute care nurses working in rural and urban settings. J. Adv. Nurs. 2020, 76, 2359–2368. [Google Scholar] [CrossRef] [PubMed]
- Aiken, L.H.; Sloane, D.M.; Bruyneel, L.; Van den Heede, K.; Griffiths, P.; Busse, R.; Diomidous, M.; Kinnunen, J.; Kózka, M.; Lesaffre, E.; et al. Nurse staffing and education and hospital mortality in nine European countries: A retrospective observational study. Lancet 2014, 383, 1824–1830. [Google Scholar] [CrossRef]
- Rhéaume, A.; Dionne, S.; Gaudet, D.; Allain, M.; Belliveau, E.; Boudreau, L.; Brown, L. The changing boundaries of nursing: A qualitative study of the transition to a new nursing care delivery model. J. Clin. Nurs. 2015, 24, 2529–2537. [Google Scholar] [CrossRef]
- Vaughan, B. How experienced practitioners gain knowledge. Creat. Nurs. 2014, 20, 30–36. [Google Scholar] [CrossRef]
- Jiang, L.; Lavaysse, L.M. Cognitive and affective job insecurity: A meta-analysis and a primary study. J. Manag. 2018, 44, 2307–2342. [Google Scholar] [CrossRef]
- Kalleberg, A.L. Precarious Lives: Job Insecurity and Well-Being in Rich Democracies; Polity Press: Cambridge, UK, 2018. [Google Scholar]
- Haddad, M. Use and relevance of bibliometrics for nursing. Nurs. Stand. 2017, 31, 55–63. [Google Scholar] [CrossRef] [PubMed]
- Aromataris, E.; Pearson, A. The systematic review: An overview. Am. J. Nurs. Sci. 2014, 114, 53–58. [Google Scholar] [CrossRef] [Green Version]
- Triana-Palencia, E.; Cárdenas-Cárdenas, L.M.; Juárez-García, A.; Quiroz-Muysina, J.; Idrovo, A.J. Use of assessment scales, turnover and job strain in nursing staff: A study in a Colombian hospital. J. Nurs. Manag. 2019, 27, 42–51. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nicoll, L.H.; Oermann, M.H.; Carter-Templeton, H.; Owens, J.K.; Edie, A.H. A Bibliometric Analysis of Articles Identified by Editors as Representing Excellence in Nursing Publication: Replication and Extension. J. Adv. Nurs. 2020, 76, 1247–1254. [Google Scholar] [CrossRef]
- Hunt, G.E.; Happell, B.; Chan, S.W.; Cleary, M. Citation analysis of mental health nursing journals: How should we rank thee? Int. J. Ment. Health Nurs. 2012, 21, 576–580. [Google Scholar] [CrossRef] [PubMed]
- Jensen, P.; Rouquier, J.B.; Croissant, Y. Testing bibliometric indicators by their prediction of scientists promotions. Scientometrics 2009, 78, 467–479. [Google Scholar] [CrossRef] [Green Version]
- Wang, X.; Sukthankar, G. Link prediction in heterogeneous collaboration networks. In Social Network Analysis-Community Detection and Evolution; Springer: Berlin/Heidelberg, Germany, 2014; pp. 165–192. [Google Scholar]
- Viana, M.P.; Amancio, D.R.; Costa, L.d.F. On time-varying collaboration networks. J. Informetr. 2013, 7, 371–378. [Google Scholar] [CrossRef] [Green Version]
- Schulz, C.; Mazloumian, A.; Petersen, A.M.; Penner, O.; Helbing, D. Exploiting citation networks for large-scale author name disambiguation. Eur. Phys. J. Data Sci. 2014, 3, 11. [Google Scholar] [CrossRef] [Green Version]
- Giménez-Espert, M.D.C.; Prado-Gascó, V.J. Bibliometric analysis of six nursing journals from the Web of Science, 2012–2017. J. Adv. Nurs. 2019, 75, 543–554. [Google Scholar] [CrossRef]
- Ashford, S.J.; Lee, C.; Bobko, P. Content, cause, and consequences of job insecurity: A theory-based measure and substantive test. Acad. Manag. J. 1989, 32, 803–829. [Google Scholar]
- Hellgren, J.; Sverke, M.; Isaksson, K. A two-dimensional approach to job insecurity: Consequences for employee attitudes and well-being. Eur. J. Work Organ. Psychol. 1999, 8, 179–195. [Google Scholar] [CrossRef]
- Vander Elst, T.; De Witte, H.; De Cuyper, N. The job insecurity scale: A psychometric evaluation across five European countries. Eur. J. Work Organ. Psychol. 2014, 23, 364–380. [Google Scholar] [CrossRef]
- Karasek, R.; Brisson, C.; Kawakami, N.; Houtman, I.; Bongers, P.; Amick, B. The Job Content Questionnaire (JCQ): An instrument for internationally comparative assessments of psychosocial job characteristics. J. Occup. Health Psychol. 1998, 3, 322–355. [Google Scholar] [CrossRef] [PubMed]
- Siegrist, J.; Starke, D.; Chandola, T.; Godin, I.; Marmot, M.; Niedhammer, I.; Peter, R. The measurement of effort-reward imbalance at work: European comparisons. Soc. Sci. Med. 2004, 58, 1483–1499. [Google Scholar] [CrossRef]
- Kristensen, T.S.; Borg, V. Copenhagen Psychosocial Questionnaire (COPSOQ); National Institute of Occupational Health: Copenhagen, Denmark, 2003. [Google Scholar]
- Zeytinoglu, I.U.; Denton, M.; Plenderleith, J.; Chowhan, J. Associations between workers’ health, and non-standard hours and insecurity: The case of home care workers in Ontario, Canada. Int. J. Hum. Resour. Manag. 2015, 26, 2503–2522. [Google Scholar] [CrossRef]
- Burke, R.J.; Ng, E.S.; Wolpin, J. Economic austerity and healthcare restructuring: Correlates and consequences of nursing job insecurity. Int. J. Hum. Resour. Manag. 2015, 26, 640–656. [Google Scholar] [CrossRef]
- Boya, F.Ö.; Demiral, Y.; Ergör, A.; Akvardar, Y.; De Witte, H. Effects of perceived job insecurity on perceived anxiety and depression in nurses. Ind. Health 2008, 46, 613–619. [Google Scholar] [CrossRef] [Green Version]
- Juárez-García, A. Psychosocial work factors associated to blood pressure and cardiovascular symptoms among Mexican nurses. Salud Publica de Mexico 2007, 49, 109–117. [Google Scholar] [CrossRef] [Green Version]
- Lee, S.; Colditz, G.A.; Berkman, L.F.; Kawachi, I. Prospective study of job insecurity and coronary heart disease in US women. Ann. Epidemiol. 2004, 14, 24–30. [Google Scholar] [CrossRef]
- Araújo-dos-Santos, T.; Silva-Santos, H.; Silva, M.N.D.; Coelho, A.C.C.; Pires, C.G.D.S.; Melo, C.M.M.D. Job insecurity among nurses, nursing technicians and nursing aides in public hospitals. Revista da Escola de Enfermagem da USP 2018, 52, e03411. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cheng, T.; Huang, G.H.; Lee, C.; Ren, X. Longitudinal effects of job insecurity on employee outcomes: The moderating role of emotional intelligence and the leader-member exchange. Asia Pac. J. Manag. 2012, 29, 709–728. [Google Scholar] [CrossRef]
- Näswall, K.; Sverke, M.; Hellgren, J. The moderating role of personality characteristics on the relationship between job insecurity and strain. Work Stress 2005, 19, 37–49. [Google Scholar] [CrossRef]
- Heponiemi, T.; Elovainio, M.; Kouvonen, A.; Noro, A.; Finne-Soveri, H.; Sinervo, T. The association of ownership type with job insecurity and worry about job stability: The moderating effects of fair management, positive leadership, and employment type. Adv. Nurs. Sci. 2012, 35, 39–50. [Google Scholar] [CrossRef] [PubMed]
- Sarwar, A.; Naseer, S.; Zhong, J.Y. Effects of bullying on job insecurity and deviant behaviours in nurses: Roles of resilience and support. J. Nurs. Manag. 2020, 28, 267–276. [Google Scholar] [CrossRef] [PubMed]
- Santos, K.O.B.; Carvalho, F.M.; de Araújo, T.M. Factor Structure and Validity Indicators of the Job Content Questionnaire: Discussing Stress in the Work Contexts. Psychology 2016, 7, 1424–1437. [Google Scholar] [CrossRef] [Green Version]
- Virtanen, P.; Janlert, U.; Hammarstrom, A. Exposure to temporary employment and job insecurity: A longitudinal study of the health effects. Occup. Environ. Med. 2011, 68, 570–574. [Google Scholar] [CrossRef] [Green Version]
- Siegrist, J. Emotions and health in occupational life: New scientific findings and policy implications. Patient Educ. Couns. 1995, 25, 227–236. [Google Scholar] [CrossRef]
- Klandermans, B.; Klein Hesselink, J.; van Vuuren, T. Employment status and job insecurity: On the subjective appraisal of an objective status. Econ. Ind. Democr. 2010, 31, 557–577. [Google Scholar] [CrossRef]
- Kausto, J.; Elo, A.L.; Lipponen, J.; Elovainio, M. Moderating effects of job insecurity in the relationships between procedural justice and employee well-being: Gender differences. Eur. J. Work Organ. Psychol. 2005, 14, 431–452. [Google Scholar] [CrossRef]
- De Cuyper, N.; Bernhard-Oettel, C.; Berntson, E.; De Witte, H.; Alarco, B. Employability and employees’ well-being: Mediation by job insecurity. Appl. Psychol. Int. Rev. 2008, 57, 488–509. [Google Scholar] [CrossRef]
- Mauno, S.; Kinnunen, U.; Makikangas, A.; Natti, J. Psychological consequences of fixed-term employment and perceived job insecurity among health care staff. Eur. J. Work Organ. Psychol. 2005, 14, 209–237. [Google Scholar] [CrossRef]
- Buchan, J.; Duffield, C.; Jordan, A. Solving’ nursing shortages: Do we need a new agenda? J. Nurs. Manag. 2015, 23, 543–545. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.W.; Dai, Y.T.; Park, C.G.; McCreary, L.L. Predicting quality of work life on nurses’ intention to leave. J. Nurs. Scholarsh. 2013, 45, 160–168. [Google Scholar] [CrossRef] [PubMed]
- Schaufeli, W.B. Job insecurity research is still alive and kicking twenty years later: A commentary. Aust. Psychol. 2016, 51, 32–35. [Google Scholar] [CrossRef]
- Huang, G.H.; Niu, X.; Lee, C.; Ashford, S.J. Differentiating cognitive and affective job insecurity: Antecedents and outcomes. J. Organ. Behav. 2012, 33, 752–769. [Google Scholar] [CrossRef] [Green Version]
- Probst, T.M. Countering the negative effects of job insecurity through participative decision making: Lessons from the demand-control model. J. Occup. Health Psychol. 2005, 10, 320–329. [Google Scholar] [CrossRef]
- Kang, D.; Gold, J.; Kim, D. Responses to job insecurity. The impact of discretionary extra-role and impression management behaviours and the moderating role of employability. Career Dev. 2012, 17, 314–332. [Google Scholar] [CrossRef]



| AUTHOR | PAPERS | % | GCS | GCS/T |
|---|---|---|---|---|
| 4 | 3.1 | 136 | 9.02 |
| 4 | 3.1 | 136 | 9.02 |
| 2 | 1.6 | 114 | 6.55 |
| 1 | 0.8 | 96 | 5.05 |
| 1 | 0.8 | 92 | 5.75 |
| 1 | 0.8 | 92 | 5.75 |
| 1 | 0.8 | 92 | 5.75 |
| 3 | 2.4 | 81 | 6.18 |
| 1 | 0.8 | 73 | 3.32 |
| 1 | 0.8 | 73 | 3.32 |
| 1 | 0.8 | 70 | 4.12 |
| 1 | 0.8 | 70 | 4.12 |
| 1 | 0.8 | 70 | 4.12 |
| 1 | 0.8 | 70 | 4.12 |
| 2 | 1.6 | 62 | 3.01 |
| 1 | 0.8 | 54 | 3.18 |
| 1 | 0.8 | 54 | 2.7 |
| 1 | 0.8 | 54 | 3.18 |
| PAPERS | GCS | GCS/T |
|---|---|---|
| 96 | 5.05 |
| 92 | 5.75 |
| 73 | 3.32 |
| 70 | 4.12 |
| 54 | 2.70 |
| 54 | 3.18 |
| 47 | 3.13 |
| 47 | 5.22 |
| 44 | 2.93 |
| 43 | 5.38 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Prado-Gascó, V.; Giménez-Espert, M.d.C.; De Witte, H. Job Insecurity in Nursing: A Bibliometric Analysis. Int. J. Environ. Res. Public Health 2021, 18, 663. https://doi.org/10.3390/ijerph18020663
Prado-Gascó V, Giménez-Espert MdC, De Witte H. Job Insecurity in Nursing: A Bibliometric Analysis. International Journal of Environmental Research and Public Health. 2021; 18(2):663. https://doi.org/10.3390/ijerph18020663
Chicago/Turabian StylePrado-Gascó, Vicente, María del Carmen Giménez-Espert, and Hans De Witte. 2021. "Job Insecurity in Nursing: A Bibliometric Analysis" International Journal of Environmental Research and Public Health 18, no. 2: 663. https://doi.org/10.3390/ijerph18020663







