1. Introduction
A report published in January 2014 stated that the global orthopedic devices market, valued at 29.2 billion United States Dollars (USD) in 2012, will rise to 41.2 billion USD in 2019 [
1]. One major type of metal biomaterial used in orthopedic applications is titanium and titanium-based alloys. Permanent metallic implant materials have been successfully applied in medicine for decades, but their life span remains limited, possibly due to septic and aseptic loosening, which often warrants surgical revision [
2]. To increase implant life span, several optimization approaches are under consideration, such as mechanical properties and microstructure improvements [
3,
4]. Another method involves surface modification to enhance cell adhesion and/or cell matrix production and, therefore, bone formation. Several coatings have been developed in recent years, such as coatings made of calcium phosphate [
5], hydroxyapatite [
6], proteins [
7], growth factors [
8], collagen [
9], and peptides [
10].
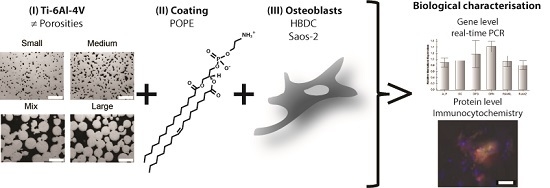
In this study, the synergistic effect of different material porosities and phospholipid coating on osteogenic differentiation was examined.
Previously characterized [
11] materials (see scanning electron microscopy (SEM) and optical microscopy (OM) photographs in
Figure 1A) were produced by metal injection molding (MIM) and exhibited various mechanical properties ranging from solid Ti-6Al-4V to bone-like properties that diminished stress shielding effects [
12] (see
Table 1). Two-dimensional (2D) pore analysis via optical microscopy indicated pore volumes of 5% ± 1%, 11% ± 1%, 33% ± 5%, and 34% ± 1%, which were named Small, Medium, Mixed, and Large, respectively (see
Table 1). The pore diameters were further clustered in 25 µm steps (see
Figure 1B).
Furthermore, the scaffolds offered a structure mimicking bone architecture, enabling bone-cell colonization, biological anchorage and, therefore, osseointegration [
20]. The material names were assigned according to increasing porosity (mirror polished (“MP”), “Small”, “Medium”, “Mixed”, and “Large”). Titanium scaffolds are already successfully employed in preclinical and clinical studies for bone regeneration [
21]. However, the application of MIM remains rather rare compared with other more classical metalworking processes, such as selective electron beam melting [
22], 3D fiber (3DF) deposition [
23], and the space holder method [
24]. MIM allows tailoring of material porosity (and, therefore, the
E modulus) by adjusting, for example, the sizes and shapes of metal powder particles [
25]. Furthermore, MIM permits production of numerous complex parts in a single operation.
Phospholipids are a promising coating material that should mimic natural cell membranes, hide artificial implant material, and strengthen the intimate interface between metallic implant surfaces and bone tissue [
26,
27].
Phospholipids are the most abundant eukaryotic membrane lipid. Phospholipids are asymmetrically distributed in plasma membranes, of which the majority are phosphatidylserine (PS) and phosphatidylethanolamine (PE), which are mainly located in the cytoplasmic leaflet, and phosphatidylcholine (PC), sphingomyelin (SM), and glycosphingolipids, which are mostly found in the exoplasmic leaflet [
28]. Biological membranes are crucial for molecular functions [
29], and membrane lipids are essential for proper protein interactions [
30]. Phospholipids account for 20% to 30% of total lipids [
31] in bone and cartilage tissues and are, thus, excellent candidates for biomimetic coatings. PS, due to its ability to bind calcium phosphate and its indirect role in bacterial adhesion inhibition [
32,
33,
34,
35], and PC are able to reduce platelet adhesion [
36,
37] and are the main phospholipids studied. However, few studies are available on the biological applications of these lipids (for more details refer to [
27]). It has been shown that PE is essential for cytokinesis [
38]. Furthermore, POPE has an inductive effect on osteogenic differentiation in human mesenchymal stem cells and can promote extracellular matrix mineralization [
27,
39].
Human bone derived cells (HBDCs) and the osteosarcoma cell line Saos-2 were cultured on these materials with and without POPE coating to study a possible synergistic effect on osteogenic differentiation. To monitor these effects, the expressions of six target genes (i.e., alkaline phosphatase (ALPL), osteocalcin (OC), osteopontin (OPN), osteoprotegerin (OPG), receptor activator of nuclear factor kappa-β ligand (RANKL) and runt-related transcription factor 2 (RUNX2)) and two target proteins (osteocalcin (OC) and osteopontin (OPN)) were studied via real-time polymerase chain reaction (PCR) and immunocytochemistry, respectively, for up to five weeks (5 W).
4. Discussion
A previous study indicated that porous Ti-Al6-V4 processed by MIM may be a well-suited net-shaped material for medical applications and osseointegration (e.g., a completely interconnected pore volume of approximately 30% and pore diameters up to 175 µm, allowing cell ingrowth) [
11]. Furthermore, improved OPN and collagen I (COL1A1) gene expressions and bone nodule formation (OC immunocytochemistry) were observed for human mesenchymal stem cells (MSCs) only on POPE-coated surfaces [
39]. Further investigation on POPE coating demonstrated that this phospholipid was able to potentiate MSC differentiation and accelerate their mineralization process [
27]. Therefore, primary cells (
i.e., HBDCs) and an osteoblast cell model (
i.e., Saos-2 cells) were cultured on native or POPE-coated surfaces of different porous materials and driven towards an osteoblastogenesis pathway for up to 5 W to further study the influence of material porosity on bone cells and a possible synergistic effect of POPE coating.
Osteogenesis is characterized by decreased proliferation and increased differentiation. The osteoblastic differentiation time course started with the commitment of MSCs to preosteoblasts. Then, the number of committed cells increased (condensation phase), and the preosteoblasts started to transform into osteoblasts. Afterwards, extracellular matrix (ECM) deposition began, followed by terminal differentiation and mineralization. The expression of six classical bone markers was studied:
RUNX2,
OPN,
OC,
ALPL,
OPG, and
RANKL. RUNX2 is a key multifunctional transcription factor involved in osteoprogenitor commitment [
46,
47]. Its expression is upregulated in immature osteoblasts and is required for osteoblast lineage determination [
48].
RUNX2 induces the expression of several bone matrix genes, such as collagen 1a1 (
COL1a1), bone sialoprotein (
BSP),
OPN, and
OC [
49]). During osteogenesis, the organic component of the ECM, of which approximately 90% was composed of COL1a1 [
50], was first synthesized by osteoblasts and was then colonized by other proteins secreted by osteoblasts (e.g., OC, BSP, and OPN; [
51]). OC regulated osteoblast and osteoclast activity, participating in the mineralization [
52].
OC is highly expressed in mature (post-proliferative phase) osteoblasts (
i.e., “late marker”) [
53,
54,
55]. OPN belongs to the small integrin binding ligand N-linked glycoprotein (SIBLING), which is a mediator of environmental stress and a potential chemoattractant for osteoclasts [
56] and is considered an inhibitor of mineralization [
57]. Expression of
RANKL is also influenced by RUNX2 [
58]. RANKL is a cytokine responsible for osteoclast recruitment and is necessary for osteoclast differentiation (via its binding to osteoclast receptor RANK or tumor necrosis factor receptor superfamily member 11a (TNFRSF11A), an NFKB activator). Its soluble decoy receptor, OPG, is also mainly secreted by osteoblasts and inhibits osteoclastogenesis [
59]. ALPL, another marker of bone formation, is an early marker of mineralization [
57].
At the gene level (
Table 2 and
Table 3), it is rather difficult to see a clear effect of porosity on HBDC and Saos-2 osteoblastogenesis. For HBDCs,
OPG, and
OC were upregulated at 3 W and 5 W only on Mixed samples,
RUNX2 was upregulated on Mixed and Large samples, and
OPN was downregulated on Mixed samples. It may be that, for HBDCs, to a certain extent, increased porosity (bell-shape distribution showing a maximum with a Mixed sample) tended to facilitate osteoblastogenesis (RUNX2) and OC collagen matrix colonization and to decrease osteoclast-mediated bone remodeling via
OPN downregulation and
OPG upregulation. Furthermore,
ALPL expression was downregulated on all porous samples, except for Large, compared with MP samples. Previous data showed that the metabolic activities of the HBDCs were highest on mixed and Large samples after one day [
11]; therefore, porosity may positively affect osteogenesis but may delay the final step of differentiation and decrease cell proliferation. However, Saos-2 cells exhibited the opposite trend, preferring the lowest porosities (highest gene upregulations (except
OPN) on Small and Medium). Moreover, these observations were seen via immunocytochemistry, in which slightly more fluorescence could be seen on Medium and Mixed samples for HBDCs and on Small and Medium samples for Saos-2 cells without POPE coating (
Figure 2). These porosity preferences may be explained by general inherent differences between cell lines and primary cells [
43,
60,
61], cell relative sizes (mean diameters of approximately 6500 µm
2 and 1000 µm
2 for HBDCs and Saos-2 cells, respectively; differences in cell nuclei sizes can also be appreciated in
Figure 2) and the shorter cell doubling time of Saos-2 cells compared with HBDCs [
61]. Primary cell sizes would allow them to bridge the pore’s rims, and their low proliferation rate would also allow other bone remodeling processes, such as vascularization, thus diminishing nutrient source hindrance. The previously described trends (
i.e., HBDC gene upregulation for higher porosities or higher downregulation for less porous material and vice-versa for Saos-2 cells) are more pronounced with POPE coating (
Table 4 and
Table 5), especially when analyzing immunocytochemistry images (
Figure 2).
Another interesting aspect is the
RANKL:
OPG ratio. This ratio is a useful marker for monitoring fracture healing [
62] and, thus, bone turnover and mineralization [
63]. As previously described, RANKL potentiates osteoclastogenesis, whereas OPG prevents the RANKL effect; therefore, when the ratio is above 1, bone resorption/osteoclast activation predominates, and when it is below 1, bone formation/osteoclast inhibition predominates. For HBDCs (
Figure 3) at 3 W and for all samples without coating,
OPG expression was much higher than
RANKL expression, resulting in a really low ratio. At 5 W (without coating),
RANKL and
OPG expressions tended to be at the same level, and the ratio was approximately 1. However, at 3 W with POPE coating,
RANKL increased drastically, whereas
OPG decreased (ratio ≥ 1), and at 5 W, both expressions were higher with POPE than without POPE, but resulted in a ratio oscillating at approximately 1 (except for MP, 1.4). From these results, it may be concluded that POPE coating potentiates and accelerates osteoblastogenesis and, therefore, likely assists bone remodeling. For Saos-2 cells (
Figure 4), the results were very different, and it is difficult to find a common trend. It could be said for MP and Small that POPE coating potentiates (increases) the ratio; however, (via an
OPG increase), for the other materials, contrasting results (decreases) were observed. However, no special tendency was observed to explain this phenomenon.
In conclusion, it can be said that a preference for lower porosity was seen for Saos-2 cells, whereas primary cells, i.e., HBDCs, preferred higher porosity. However, POPE coating increased this trend. Furthermore, RANKL/OPG expressions and ratio analyses were able to highlight a special effect of POPE on faster bone remodeling/turnover for HBDCs. Here, Saos-2 cells exhibited a completely different behavior pattern than HBDCs, supporting that primary cells should be preferred relative to cell lines. Porous material could improve tissue implantation via cell colonization and POPE coating could further strengthen the intimate interface between tissue and material via faster mineralization and tissue remodeling.