Frailty and Medication Appropriateness in Rural Adults: Proposing Interventions through Pharmacist–Physician Collaborative Efforts
Abstract
:1. Introduction
2. Materials and Methods
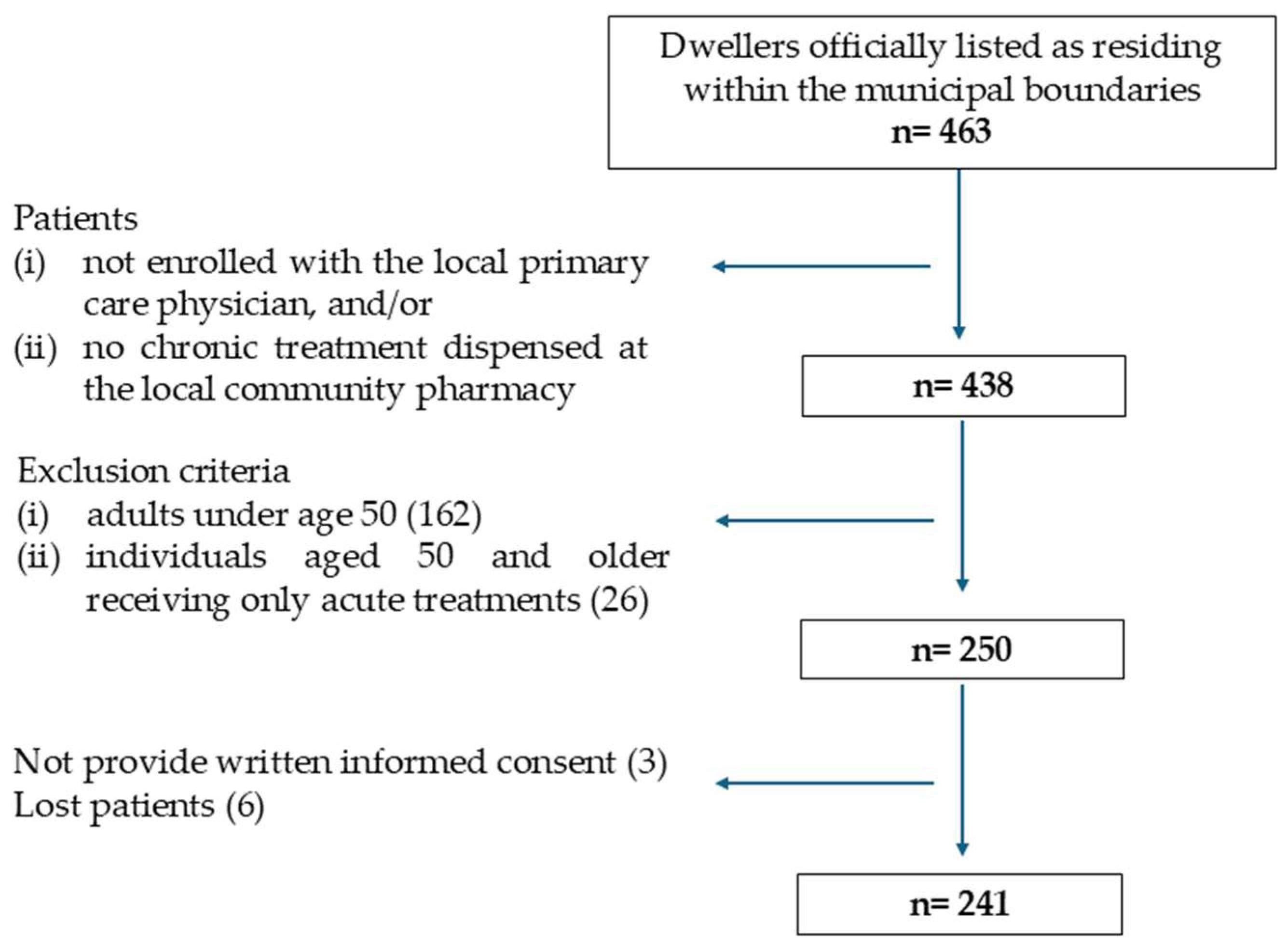
2.1. Participants and Study Procedure
2.2. Data Collection
2.3. Statistical Analysis
2.4. Ethical Approval
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
References
- Junius-Walker, U.; Onder, G.; Soleymani, D.; Wiese, B.; Albaina, O.; Bernabei, R.; Marzetti, E. The Essence of Frailty: A Systematic Review and Qualitative Synthesis on Frailty Concepts and Definitions. Eur. J. Intern. Med. 2018, 56, 3–10. [Google Scholar] [CrossRef] [PubMed]
- Pazan, F.; Wehling, M. Polypharmacy in Older Adults: A Narrative Review of Definitions, Epidemiology and Consequences. Eur. Geriatr. Med. 2021, 12, 443–452. [Google Scholar] [CrossRef] [PubMed]
- Varghese, D.; Ishida, C.; Patel, P.; Haseer Koya, H. Polypharmacy. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2024. [Google Scholar]
- Griese-Mammen, N.; Hersberger, K.E.; Messerli, M.; Leikola, S.; Horvat, N.; van Mil, J.W.F.; Kos, M. PCNE Definition of Medication Review: Reaching Agreement. Int. J. Clin. Pharm. 2018, 40, 1199–1208. [Google Scholar] [CrossRef] [PubMed]
- Hilmer, S.N.; Gnjidic, D. Prescribing for Frail Older People. Aust. Prescr. 2017, 40, 174–178. [Google Scholar] [CrossRef]
- Naharci, M.I.; Tasci, I. Frailty Status and Increased Risk for Falls: The Role of Anticholinergic Burden. Arch. Gerontol. Geriatr. 2020, 90, 104136. [Google Scholar] [CrossRef]
- American Geriatrics Society 2023 Updated AGS Beers Criteria® for Potentially Inappropriate Medication Use in Older Adults. J. Am. Geriatr. Soc. 2023, 71, 2052–2081. [CrossRef]
- O’Mahony, D.; Cherubini, A.; Guiteras, A.R.; Denkinger, M.; Beuscart, J.-B.; Onder, G.; Gudmundsson, A.; Cruz-Jentoft, A.J.; Knol, W.; Bahat, G.; et al. STOPP/START Criteria for Potentially Inappropriate Prescribing in Older People: Version 3. Eur. Geriatr. Med. 2023, 14, 625–632. [Google Scholar] [CrossRef]
- Foro de Atención Farmacéutica-Farmacia Comunitaria (Foro AF-FC), Panel de Expertos Practical Guide to Clinical Professional Pharmacy Services in Community Pharmacy. Available online: https://www.farmaceuticos.com/wp-content/uploads/2021/02/ON_GUIA_SPFA_FORO_2022_ING_PGs.pdf (accessed on 25 May 2024).
- INE Instituto Nacional de Estadística. (Spanish Statistical Institute). Available online: https://www.ine.es/nomen2/index.do (accessed on 25 May 2024).
- NIPH—Norwegian Institute of Public Health ATCDDD—ATC/DDD Index. Available online: https://atcddd.fhi.no/atc_ddd_index/ (accessed on 30 May 2024).
- Morley, J.E.; Malmstrom, T.K.; Miller, D.K. A Simple Frailty Questionnaire (FRAIL) Predicts Outcomes in Middle Aged African Americans. J. Nutr. Health Aging 2012, 16, 601–608. [Google Scholar] [CrossRef]
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in Older Adults: Evidence for a Phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, M146–M156. [Google Scholar] [CrossRef]
- Ministry of Health. Update of the Consensus Document on Prevention of Frailty in Elderly People (2022). Available online: https://www.sanidad.gob.es/areas/promocionPrevencion/envejecimientoSaludable/fragilidadCaidas/estrategiaSNS/docs/Update_of_the_consensus_document_on_prevention_of_frailty_in_elderly_people_2022_ACCESIBLE.pdf (accessed on 25 May 2024).
- Ramos, H.; Moreno, L.; Pérez-Tur, J.; Cháfer-Pericás, C.; García-Lluch, G.; Pardo, J. CRIDECO Anticholinergic Load Scale: An Updated Anticholinergic Burden Scale. Comparison with the ACB Scale in Spanish Individuals with Subjective Memory Complaints. J. Pers. Med. 2022, 12, 207. [Google Scholar] [CrossRef]
- Rudolph, J.L.; Salow, M.J.; Angelini, M.C.; McGlinchey, R.E. The Anticholinergic Risk Scale and Anticholinergic Adverse Effects in Older Persons. Arch. Intern. Med. 2008, 168, 508–513. [Google Scholar] [CrossRef] [PubMed]
- Seppala, L.J.; Petrovic, M.; Ryg, J.; Bahat, G.; Topinkova, E.; Szczerbińska, K.; van der Cammen, T.J.M.; Hartikainen, S.; Ilhan, B.; Landi, F.; et al. STOPPFall (Screening Tool of Older Persons Prescriptions in Older Adults with High Fall Risk): A Delphi Study by the EuGMS Task and Finish Group on Fall-Risk-Increasing Drugs. Age Ageing 2021, 50, 1189–1199. [Google Scholar] [CrossRef] [PubMed]
- Curcio, C.-L.; Henao, G.-M.; Gomez, F. Frailty among Rural Elderly Adults. BMC Geriatr. 2014, 14, 2. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Garcia, F.J.; Gutierrez Avila, G.; Alfaro-Acha, A.; Amor Andres, M.S.; De Los Angeles De La Torre Lanza, M.; Escribano Aparicio, M.V.; Humanes Aparicio, S.; Larrion Zugasti, J.L.; Gomez-Serranillo Reus, M.; Rodriguez-Artalejo, F.; et al. The Prevalence of Frailty Syndrome in an Older Population from Spain. The Toledo Study for Healthy Aging. J. Nutr. Health Aging 2011, 15, 852–856. [Google Scholar] [CrossRef]
- Jürschik, P.; Nunin, C.; Botigué, T.; Escobar, M.A.; Lavedán, A.; Viladrosa, M. Prevalence of Frailty and Factors Associated with Frailty in the Elderly Population of Lleida, Spain: The FRALLE Survey. Arch. Gerontol. Geriatr. 2012, 55, 625–631. [Google Scholar] [CrossRef]
- Jürschik Giménez, P.; Escobar Bravo, M.Á.; Nuin Orrio, C.; Botigué Satorra, T. Frailty criteria in the elderly: A pilot study. Aten. Primaria 2011, 43, 190–196. [Google Scholar] [CrossRef]
- Menéndez-González, L.; Izaguirre-Riesgo, A.; Tranche-Iparraguirre, S.; Montero-Rodríguez, Á.; Orts-Cortés, M.I. Prevalence and associated factors of frailty in adults over 70 years in the community. Aten. Primaria 2021, 53, 102128. [Google Scholar] [CrossRef]
- Abizanda Soler, P.; López-Torres Hidalgo, J.; Romero Rizos, L.; López Jiménez, M.; Sánchez Jurado, P.M.; Atienzar Núñez, P.; Esquinas Requena, J.L.; García Nogueras, I.; Hernández Zegarra, P.; Bardales Mas, Y.; et al. Frailty and dependence in Albacete (FRADEA study): Reasoning, design and methodology. Rev. Esp. Geriatr. Gerontol. 2011, 46, 81–88. [Google Scholar] [CrossRef] [PubMed]
- Gordon, E.H.; Hubbard, R.E. Do Sex Differences in Chronic Disease Underpin the Sex-Frailty Paradox? Mech. Ageing Dev. 2019, 179, 44–50. [Google Scholar] [CrossRef]
- Ofori-Asenso, R.; Chin, K.L.; Mazidi, M.; Zomer, E.; Ilomaki, J.; Zullo, A.R.; Gasevic, D.; Ademi, Z.; Korhonen, M.J.; LoGiudice, D.; et al. Global Incidence of Frailty and Prefrailty Among Community-Dwelling Older Adults: A Systematic Review and Meta-Analysis. JAMA Netw. Open 2019, 2, e198398. [Google Scholar] [CrossRef]
- Andrew, M.K.; Mitnitski, A.B.; Rockwood, K. Social Vulnerability, Frailty and Mortality in Elderly People. PLoS ONE 2008, 3, e2232. [Google Scholar] [CrossRef] [PubMed]
- Rochon, P.A.; Petrovic, M.; Cherubini, A.; Onder, G.; O’Mahony, D.; Sternberg, S.A.; Stall, N.M.; Gurwitz, J.H. Polypharmacy, Inappropriate Prescribing, and Deprescribing in Older People: Through a Sex and Gender Lens. Lancet. Healthy Longev. 2021, 2, e290–e300. [Google Scholar] [CrossRef] [PubMed]
- Khera, S.; Abbasi, M.; Dabravolskaj, J.; Sadowski, C.A.; Yua, H.; Chevalier, B. Appropriateness of Medications in Older Adults Living With Frailty: Impact of a Pharmacist-Led Structured Medication Review Process in Primary Care. J. Prim. Care Community Health 2019, 10, 2150132719890227. [Google Scholar] [CrossRef] [PubMed]
- Ramos, H.; Pardo, J.; Sánchez, R.; Puchades, E.; Pérez-Tur, J.; Navarro, A.; Moreno, L. Pharmacist-Physician Interprofessional Collaboration to Promote Early Detection of Cognitive Impairment: Increasing Diagnosis Rate. Front. Pharmacol. 2021, 12, 579489. [Google Scholar] [CrossRef]
- Nicieza-Garcia, M.L.; Salgueiro-Vázquez, M.E.; Jimeno-Demuth, F.J.; Manso, G. Beers versus STOPP Criteria in Polyharmacy Community-Dwelling Older Patients. Farm. Hosp. 2016, 40, 150–164. [Google Scholar] [CrossRef]
- Salgueiro, E.; Elizarde, B.C.; Elola, A.I.; García-Pulido, B.; Nicieza-García, M.L.; Manso, G. The most common STOPP/START criteria in Spain. A review of the literature. Rev. Esp. Geriatr. Gerontol. 2018, 53, 274–278. [Google Scholar] [CrossRef]
- Tommelein, E.; Mehuys, E.; Petrovic, M.; Somers, A.; Colin, P.; Boussery, K. Potentially Inappropriate Prescribing in Community-Dwelling Older People across Europe: A Systematic Literature Review. Eur. J. Clin. Pharmacol. 2015, 71, 1415–1427. [Google Scholar] [CrossRef]
- Bernal-Delgado, E.; Garcia-Armesto, S.; Oliva, J.; Sanchez Martinez, F.I.; Repullo, J.R.; Pena-Longobardo, L.M.; Ridao-Lopez, M.; Hernandez-Quevedo, C. Spain: Health System Review. Health Syst. Transit. 2018, 20, 1–179. [Google Scholar]
- Lunghi, C.; Domenicali, M.; Vertullo, S.; Raschi, E.; De Ponti, F.; Onder, G.; Poluzzi, E. Adopting STOPP/START Criteria Version 3 in Clinical Practice: A Q&A Guide for Healthcare Professionals. Drug Saf. 2024, 1–14. [Google Scholar] [CrossRef]
- Ba, M.; Crawford, C.; Grecia, C.H.D.; Francia, I.D.; Di, E.; Reino, A.; Suiza, O.H.F.; Fisher, M.; Unido, R.; Alemania, D.F.; et al. Guıía ESC 2021 Sobre La Prevención de La Enfermedad Cardiovascular En La Práctica Clínica. Rev. Esp. Cardiol. 2022, 75, 429.e1–429.e104. [Google Scholar] [CrossRef]
- Álvarez, F.; Ávila, L.; Guede, C.; Hernández, C.; Lapena Estella, C.; López Simarro, F.; Murillo García, D.; Romera Liébana, L.; Urbina Juez, A. Recomendaciones En El Manejo de La Hiperglucemia En Pacientes Con Diabetes Mellitus Según Grado de Fragilidad. Diabetes Práctica 2023, 14, 37–75. [Google Scholar] [CrossRef]
- Joosten, L.P.T.; van Doorn, S.; van de Ven, P.M.; Köhlen, B.T.G.; Nierman, M.C.; Koek, H.L.; Hemels, M.E.W.; Huisman, M.V.; Kruip, M.; Faber, L.M.; et al. Safety of Switching From a Vitamin K Antagonist to a Non-Vitamin K Antagonist Oral Anticoagulant in Frail Older Patients With Atrial Fibrillation: Results of the FRAIL-AF Randomized Controlled Trial. Circulation 2024, 149, 279–289. [Google Scholar] [CrossRef] [PubMed]
- van Poelgeest, E.; Paoletti, L.; Özkök, S.; Pinar, E.; Bahat, G.; Vuong, V.; Topinková, E.; Daams, J.; McCarthy, L.; Thompson, W.; et al. The Effects of Diuretic Deprescribing in Adult Patients: A Systematic Review to Inform an Evidence-Based Diuretic Deprescribing Guideline. Br. J. Clin. Pharmacol. 2024, 1–17. [Google Scholar] [CrossRef]
- Bertolotti, M.; Lancellotti, G.; Mussi, C. Management of High Cholesterol Levels in Older People. Geriatr. Gerontol. Int. 2019, 19, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Harned, M.; Sloan, P. Safety Concerns with Long-Term Opioid Use. Expert Opin. Drug Saf. 2016, 15, 955–962. [Google Scholar] [CrossRef]
- Brandt, J.; Bressi, J.; Lê, M.-L.; Neal, D.; Cadogan, C.; Witt-Doerring, J.; Witt-Doerring, M.; Wright, S. Prescribing and Deprescribing Guidance for Benzodiazepine and Benzodiazepine Receptor Agonist Use in Adults with Depression, Anxiety, and Insomnia: An International Scoping Review. EClinicalMedicine 2024, 70, 102507. [Google Scholar] [CrossRef] [PubMed]
- Brown, P.J.; Ciarleglio, A.; Roose, S.P.; Garcia, C.M.; Chung, S.; Alvarez, J.; Stein, A.; Gomez, S.; Rutherford, B.R. Frailty Worsens Antidepressant Treatment Outcomes in Late Life Depression. Am. J. Geriatr. Psychiatry 2021, 29, 944–955. [Google Scholar] [CrossRef]
- Krishnamoorthy, Y.; Rajaa, S.; Rehman, T. Diagnostic Accuracy of Various Forms of Geriatric Depression Scale for Screening of Depression among Older Adults: Systematic Review and Meta-Analysis. Arch. Gerontol. Geriatr. 2020, 87, 104002. [Google Scholar] [CrossRef]
- Harding, C.K.; Lapitan, M.C.; Arlandis, S.; Bø, K.; Costantini, E.; Groen, J. EAU Guidelines on Management of Non-Neurogenic Female Lower Urinary Tract Symptoms (LUTS). Eur. Assoc. Urol. Guidel. 2023, 1–146. Available online: https://uroweb.org/guidelines/non-neurogenic-female-luts (accessed on 19 September 2024).
- Cornu, J.N.; Gacci, M.; Hashim, H.; Herrmann, T.R.W.; Malde, S.; Netsch, C. EAU Guidelines on Management of Non-Neurogenic Male Lower Urinary Tract Symptoms (LUTS). Eur. Assoc. Urol. Guidel. 2023, 1–124. Available online: https://uroweb.org/guidelines/management-of-non-neurogenic-male-luts (accessed on 19 September 2024).
| Variables | Groups | Total n (%) 241 (100) | Non-Frail n (%) 191 (79.3) | Frail n (%) 50 (20.8) | p-Value |
|---|---|---|---|---|---|
| Gender | Male | 106 (44.0) | 93 (48.7) | 13 (26.0) | 0.004 a ** |
| Female | 135 (56.0) | 98 (51.3) | 37 (74.0) | ||
| Age | 68.9 ± 12.8 | 64.9 ± 10.8 | 83.9 ± 7.7 | <0.001 b *** | |
| 66.0 [50.0, 98.0] | 62.0 [50.0, 94.0] | 85.0 [57.0, 98.0] | <0.001 c *** | ||
| [50, 65) | 116 (48.1) | 115 (60.2) | 1 (2.0) | <0.001 d *** | |
| [65, 80) | 62 (25.7) | 52 (27.2) | 10 (20.0) | ||
| [80, 98] | 63 (26.1) | 24 (12.6) | 39 (78.0) | ||
| NOM | 6.2 ± 4.4 | 5.2 ± 3.7 | 10.0 ± 5 | <0.001 b *** | |
| 5.0 [1.0, 21.0] | 4.0 [1.0, 17.0] | 10.0 [3.0, 21.0] | <0.001 c *** | ||
| FRID | 1.4 ± 1.5 | 1.1 ± 1.3 | 2.5 ± 1.7 | <0.001 b *** | |
| 1.0 [0.0, 7.0] | 1.0 [0.0, 6.0] | 2.0 [0.0, 7.0] | <0.001 c *** | ||
| Benzodiazepines and z-drugs | 62 (25.7) | 42 (22.0) | 20 (40.0) | 0.009 a ** | |
| Antidepressants | 63 (26.1) | 33 (17.3) | 30 (60.0) | <0.001 a *** | |
| Opioids | 28 (11.6) | 15 (7.9) | 13 (26.0) | <0.001 a *** | |
| Diuretics | 81 (33.6) | 54 (28.3) | 27 (54.0) | <0.001 a *** | |
| CALS score | 1.3 ± 1.8 | 1.0 ± 1.3 | 2.8 ± 2.5 | <0.001 b *** | |
| 1.0 [0.0, 10.0] | 1.0 [0.0, 7.0] | 2.0 [0.0, 10.0] | <0.001 c *** | ||
| CALS score < 3 | 199 (82.6) | 167 (87.4) | 32 (64.0) | <0.001 a *** | |
| CALS score ≥ 3 | 42 (17.4) | 24 (12.6) | 18 (36.0) | ||
| Treated with | <2 drugs with ACB | 173 (71.8) | 150 (78.5) | 23 (46.0) | <0.001 a *** |
| ≥2 drugs with ACB | 68 (28.2) | 41 (21.5) | 27 (54.0) | ||
| Model 1: Gender + Age | Model 2: Gender + Age + NOM | Model 3: Gender + Age + FRID | Model 4: Gender + Age + CALS | ||
|---|---|---|---|---|---|
| Variables | Groups | OR [95% CI] | OR [95% CI] | OR [95% CI] | OR [95% CI] |
| Gender | Male | 1 | 1 | 1 | 1 |
| Female | 3.5 [1.5, 9.0] ** | 3.6 [1.5, 9.6] ** | 3.2 [1.3, 8.4] * | 3.4 [1.3, 9.3] * | |
| Age | 1.2 [1.1, 1.2] *** | 1.2 [1.1, 1.2] *** | 1.2 [1.1, 1.2] *** | 1.2 [1.1, 1.2] *** | |
| NOM | - | 1.1 [1.0, 1.3] ** | - | - | |
| FRID | - | - | 1.4 [1.1, 1.9] * | - | |
| CALS score | - | - | - | 1.5 [1.2, 2.0] ** | |
| p-value of the Hosmer–Lemeshow test | 0.5290 | 0.8413 | 0.6428 | 0.7969 | |
| Akaike Information Criterion | 146.0 | 140.1 | 141.1 | 134.5 | |
| Drug | ACB | FRID | STOPP Criteria (n) | Primary Care Interventions | Type |
| A02B—Peptic Ulcer Agents | |||||
| Omeprazole | 0 | no | A1: Prescribed without a clinical indication (28). F2: Proton pump inhibitor for uncomplicated peptic ulcer disease at full therapeutic dosage for > 8 weeks (2). | Comprehensive review of the medical and pharmaceutical records. Withdrawal of the drug in the absence of an appropriate indication. | PI |
| Pantoprazole | 0 | no | |||
| Rabeprazole | 0 | no | |||
| Lansoprazole | 0 | no | |||
| Esomeprazole | 0 | no | |||
| A10B—Hypoglycemic Drugs | |||||
| Metformin | 1 | no | - | Drug of choice in frailty. | ‡ |
| B01A—Antithrombotic Agents | |||||
| Acetylsalicylic acid | 0 | no | C16: Acetylsalicylic acid for primary prevention in cardiovascular disease (11). | Comprehensive review of the medical and pharmaceutical records to confirm the history of cardiovascular events. Reconsider treatment appropriateness. | PI |
| Direct oral anticoagulants (DOAC) | 0 | no | C14: DOAC and P-glycoprotein drug efflux pump inhibitors (12). | Assess the risk of bleeding. Evaluate P-glycoprotein inhibitor deprescription. | CI |
| Anti vitamin K (Acenocoumarol) | 0 | no | C11: Vitamin K antagonist as a first-line anticoagulant for atrial fibrillation (3). | Comprehensive review of the medical and pharmaceutical records. Reconsider treatment appropriateness. | CI |
| C03—Diuretics | |||||
| Furosemide | 1 | yes | B10: Loop diuretic for treatment of hypertension with concurrent urinary incontinence (9). | Monitor adverse reactions. | CI |
| Spironolactone | 0 | yes | B13: Aldosterone antagonists together with other drugs may increase potassium levels (2). | Monitor serum levels. | PI |
| C10—Lipid-Modifying Agents | |||||
| Statins | 0 | no | B16: Statins for primary cardiovascular prevention in persons aged ≥ 85 and established frailty (7). | Comprehensive review of the medical and pharmaceutical records to confirm the history of cardiovascular events. | PI |
| Reconsider treatment appropriateness. | CI | ||||
| N02—Analgesics | |||||
| Tramadol | 2 | yes | L1: Strong oral or transdermal opioids as first-line treatment for mild pain (11). L2: Use of daily opioids without concomitant laxatives (10). | Gradual reduction in the drug dosage and withdrawal. Alternative: paracetamol or NSAIDs. Add laxative. | PI |
| Tapentadol | 1 | yes | |||
| Fentanyl | 1 | yes | |||
| Buprenorphine | 0 | yes | |||
| Gabapentin, pregabalin | 0 | no | L5: Gabapentinoids for non-neuropathic pain (4). | Evaluate pain type. Alternative: paracetamol or NSAIDs. | PI |
| N05—Psycholeptics | |||||
| Lorazepam | 1 | yes | D8: Benzodiazepines ≥ 4 weeks (21). | Referral and gradual withdrawal. Cognitive behavioral therapy. Evaluate the use of melatonin in patients receiving benzodiazepine for insomnia. | CI |
| Diazepam | 1 | yes | G4: Benzodiazepines with acute or chronic respiratory failure (4). | ||
| Potassium chlorazepate | 1 | yes | A3: Duplicate drug class prescription (diazepam-potassium chlorazepate) (1). | ||
| Zolpidem | 0 | yes | D11: Z-drugs for insomnia ≥ 2 weeks (1). | ||
| N06A—Antidepressants | |||||
| Amitriptyline | 3 | yes | D2: Initiation of TriCyclic Antidepressants as first-line treatment for major depression (1). | Assess the origin of the symptomatology. | PI |
| A3: Duplicate drug class prescription (amitriptyline-duloxetine) (1). | |||||
| Paroxetine | 2 | yes | |||
| Sertraline | 1 | yes | A3: Duplicate drug class prescription (sertraline-mirtazapine) (1). | ||
| Trazodone | 1 | yes | |||
| Duloxetine | 0 | yes | I7: Duloxetine in the presence of urinary urgency or urinary incontinence due to urgency (1). | A specialist physician referral is suggested for deprescription. Prioritize drugs without anticholinergic load. | CI |
| Escitalopram | 1 | yes | |||
| Mirtazapine | 1 | yes | |||
| Fluoxetine | 1 | yes | |||
| Desvenlafaxine | 1 | yes | A3: Duplicate drug class prescription (desvenlafaxine-duloxetine) (1). | ||
| G04BD—Urinary Antispasmodics | |||||
| Fesoterodine | 3 | yes | I1: Systemic antimuscarinic drugs in the presence of dementia or chronic cognitive impairment (1). | Assess the effectiveness of the antispasmodic. Alternative: mirabegron. Non-pharmacological treatments are suggested. | PI |
| Solifenacine | yes | ||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
García, C.; Ocaña, J.M.; Alacreu, M.; Moreno, L.; Martínez, L.A. Frailty and Medication Appropriateness in Rural Adults: Proposing Interventions through Pharmacist–Physician Collaborative Efforts. J. Clin. Med. 2024, 13, 5755. https://doi.org/10.3390/jcm13195755
García C, Ocaña JM, Alacreu M, Moreno L, Martínez LA. Frailty and Medication Appropriateness in Rural Adults: Proposing Interventions through Pharmacist–Physician Collaborative Efforts. Journal of Clinical Medicine. 2024; 13(19):5755. https://doi.org/10.3390/jcm13195755
Chicago/Turabian StyleGarcía, Cristina, José M. Ocaña, Mónica Alacreu, Lucrecia Moreno, and Luis A. Martínez. 2024. "Frailty and Medication Appropriateness in Rural Adults: Proposing Interventions through Pharmacist–Physician Collaborative Efforts" Journal of Clinical Medicine 13, no. 19: 5755. https://doi.org/10.3390/jcm13195755





