1. Introduction
By the beginning of 2022, the number of internet users had reached a global 4.95 billion, which means 65% of the world population is online [
1]. The Internet has undoubtedly become one of the most popular sources of medical information in the field for the definition, symptoms, and diagnosis of diseases, as well as healthy lifestyles, medications, alternative medicine, medical devices, and the functioning of the entire medical care system [
2,
3,
4,
5]. Studies confirm that searching for health-related content is not the only reason to use Internet—consumers more and more frequently before seeing a doctor ask Dr. Google for online consultations [
3,
6,
7,
8,
9]. Researchers pointed out that people who seek health materials on the Web differ in age, income, and education levels from those seeking information offline [
8]. However, searching for digital information on diseases is not only using search engines. More and more websites are being created. Virtual symptoms checkers exist, where users can quickly (in about 5 min), free of charge, and without registration identify possible conditions after entering the symptoms and providing the answer to additional questions, thus making for an initial diagnosis. There are data indicating that younger people who are in worse health condition seek access to this information more often [
10]. They are also the ones with a higher socio-economic status and are better educated, most often women [
11]. Interestingly, half of all searches are made on behalf of another person [
11]. The high percentage of the above indications was determined by the quick access to information guaranteed, the ease of obtaining it, and the possibility of better preparation for a doctor’s visit [
9]. The offer of the global network in the health area is plenteous: from pharmacies and clinics search engines, through expert advice, discussion forums, blogs of patients, and professionals, virtual support groups, tests, symptom checkers, and ending with websites devoted to specific health-related issues (e.g., diet, activity, prevention), diseases, and drugs.
This situation begins to occupy an equal place in the doctor–patient interaction. Previous studies suggested that the relationship between consumers and healthcare professionals may be a motivation to search for health information online [
2,
12,
13]. Research indicates that Internet-based decision-making, independent of the physician, can improve patients’ self-efficacy and reduce unnecessary visits to physicians [
14]. On the other hand, doctors are particularly critical in the process of implementing digital health in the healthcare sector. They mainly report a lack of proper preparation and training [
15] and difficulties in adapting to the rapidly progressing changes in this area. Some initiatives are known to provide specialization training on medical informatics, such as Topol review [
16], but they have not been developed in all countries. At the same time, the situation of clinicians who are aware that their patients seek the popular Web domains for health information was examined [
17,
18,
19]. This phenomenon, known as “Dr. Google”, identifies the complex effects and consequences of searching for online health information—a kind of medical autonomy for patients, as well as the role of professionals with their appropriate knowledge and practice [
14].
Despite digital health popularity, the literature suggests that patients still value the health professionals’ advice [
14,
19], which might be a suggestion that physicians can play an important role in online health navigation, and the need to have a proficiency in digital skills is even more vital. The implementation of information communication technology (ICT) may be the answer to this challenge and can provoke us to remain open to technological opportunities and the possession of skills to manage them [
20]. For physicians, ICT competences might be relevant for several reasons, starting with the fact that medical technology is advancing and daily tasks handling health data is challenging (e.g., electronic health records, electronic documentation, and health information systems) and ending with patient–consumer personalized and individualized demands [
21]. However, today’s profession practice is not only dependent on this duo. There is ample evidence that technology solutions increase the efficiency of health services and improve patient outcomes. Electronic medical records (EMR) have been shown to significantly reduce the incidence of medical errors, and e-prescriptions have been shown to improve prescribing errors and patient adherence to treatment regimens [
22]. Moreover, there is evidence that e-Health systems have led to fewer hospital visits and cost savings in the healthcare system [
23].
In the new European Skills Agenda, the European Commission sets objectives for upskilling (improving existing skills) and reskilling (training in new skills) the workforce in the next five years [
24]. In its policy paper on digital skills for doctors, the Standing Committee of European Doctors highlights the three main areas of digital skills: general, technical, and related to patient–doctor relationship [
25]. These new competences should be included in the future medical programs of study and adapted to a doctor’s medical speciality, and they should keep current and future physicians up to date with tech innovations.
Few years ago, the European Commission defined resources to efficiently use the possibilities of new technology as digital literacy [
26]. According to Bawden, digitally literate people have the knowledge and ability to effectively and critically navigate, evaluate, and create information using a range of digital technologies, as well as using Internet and technology tools to achieve academic, professional, and personal goals [
27]. The medical education of Polish physicians is evidence-based, but, in the context of the challenges related to Dr. Google, technological development, and the ubiquity of the Internet, it might not be sufficient. Health technologies provide broad access to resources, enable easy search for information, and support initiatives related to global health care. These technologies have become a trend, transforming healthcare systems in the context of creating ones that are largely open to all patient needs. Due to the development of such technologies, the need for digitally trained personnel arose.
3. Materials and Methods
3.1. Study Design
This is a cross-sectional, descriptive study conducted among 307 professionally active physicians between December 2019 to April 2020, in the South-Eastern Poland. The sample was representative of the group of doctors, which consisted of 4600 specialists in 2018 in the Podkarpackie Voivodeship. Additionally, the number of doctors living in Poland with the right to practice in 2019 amounted to 140,420, of which 58.9% were women. The most common specialization of Polish doctors was internal medicine (20.9%), the second largest was family medicine (11.8%), the third—paediatrics (8.2%) [
47]. The current study is a part of a larger ongoing project conducted to explore attitudes towards e-health, digital literacy, and online health information among healthcare sector representatives (physicians, nurses [
48]) and patients. The self-designed questionnaire used in this research was distributed among the following healthcare facilities employing physicians: primary healthcare (PHC), outpatient specialist care (AOS), hospitals (at different levels of locality), and private sector. Respondents participated in this study ensured sample diversity working in southeastern Poland (the error threshold was 5%, i.e., the test power was 0.95). Before participating in the survey, respondents were provided with detailed information about the purpose of the study, assured of its anonymity, and that they have the option to opt out at any stage of it.
3.2. Questionnaires
This survey adopted a structured self-designed questionnaire to obtain data from physicians and included a sociodemographic section with questions about age, gender, specialization, workplace, and number of patients seen per month. Surveyed physicians were also asked to indicate the frequency of using the Internet and electronic devices.
The questionnaire had also four sections that included:
“Digital Literacy” section on self-assessment of the ability to use digital devices and solutions, and evaluation the frequency of using digital devices and solutions in private and professional life (smartphone, computer, e-mail, mobile applications, and tablet);
“The impact of the Internet/new technologies on healthcare and modern life” section concerning the general assessment and opinion on the use of the search engine/Internet in the context of health;
“Recommendation of e-Health solutions” section containing statements regarding the present/future recommending or not recommending e-health solutions to the patients,
“Evaluation of e-Health solutions” section with self-assessment of the relevance of the proposed e-health solutions;
3.3. Ethics
The study was approved by the institutional Bioethics Committee of the Rzeszow University (Resolution No. 6/12/2019) and all relevant administrative bodies.
3.4. Data Analysis
In this study principal component analysis (PCA), using the Anderson–Rubin method, was carried out to determine constructs in questionnaire regarding: “Digital literacy”, “The impact of the Internet/new technologies on healthcare and modern life”, “Recommendation of e-Health solutions”, and “Evaluation of e-Health solutions”. The reliability of each construct was also determined by the Cronbach’s alpha coefficient. A significance level of p < 0.05 was assumed.
Descriptive statistics were conducted to present the data: frequency (n), percentage (%), arithmetic mean (M), the value of which determines the average level of a given variable, and standard deviation (SD), a statistical measure of scattering the results around the expected value.
Then, correlation analyses were performed. The t-tests and chi-square tests for two-group comparisons in sociodemographic variables (gender and workplace) were performed. Nonparametric Spearman Rho correlation coefficient test was used to compare the non-normally distributed numerical data in correlation analysis with age. Differences in mean values in the cross-sectional analysis were calculated using the one-way analysis of variance for the cross-sectional groups ANOVA (F test). To measure the linear relationship between all digital indicators, the Pearson correlation (r) was used.
Statistical significance was evaluated at p < 0.05.
Calculations were performed with the IBM SPSS program Statistics 20 (IMB, Armonk, NY, USA).
5. Discussion
We live in a world of rapid technological, demographic, and social changes, in which digitization has become a factor of advantage and an element of the competitiveness of economies and health systems, as well as health policies. These changes are becoming a fact that needs to be documented in various aspects: technological, human, qualitative, financial, etc. Especially in the case of Poland and many other countries in the region, the development and popularization of digital e-health services is a priority direction for the development of the local health care system [
49].
Our purpose in this study was to investigate physicians’ self-digital literacy, analyze their perception of online health knowledge obtained by patients, and identify attitudes towards e-health solutions. It is also important to characterize and describe the phenomenon of Dr. Google, which affects the existing doctors–patients’ relationships, and shapes the modern understanding of health information.
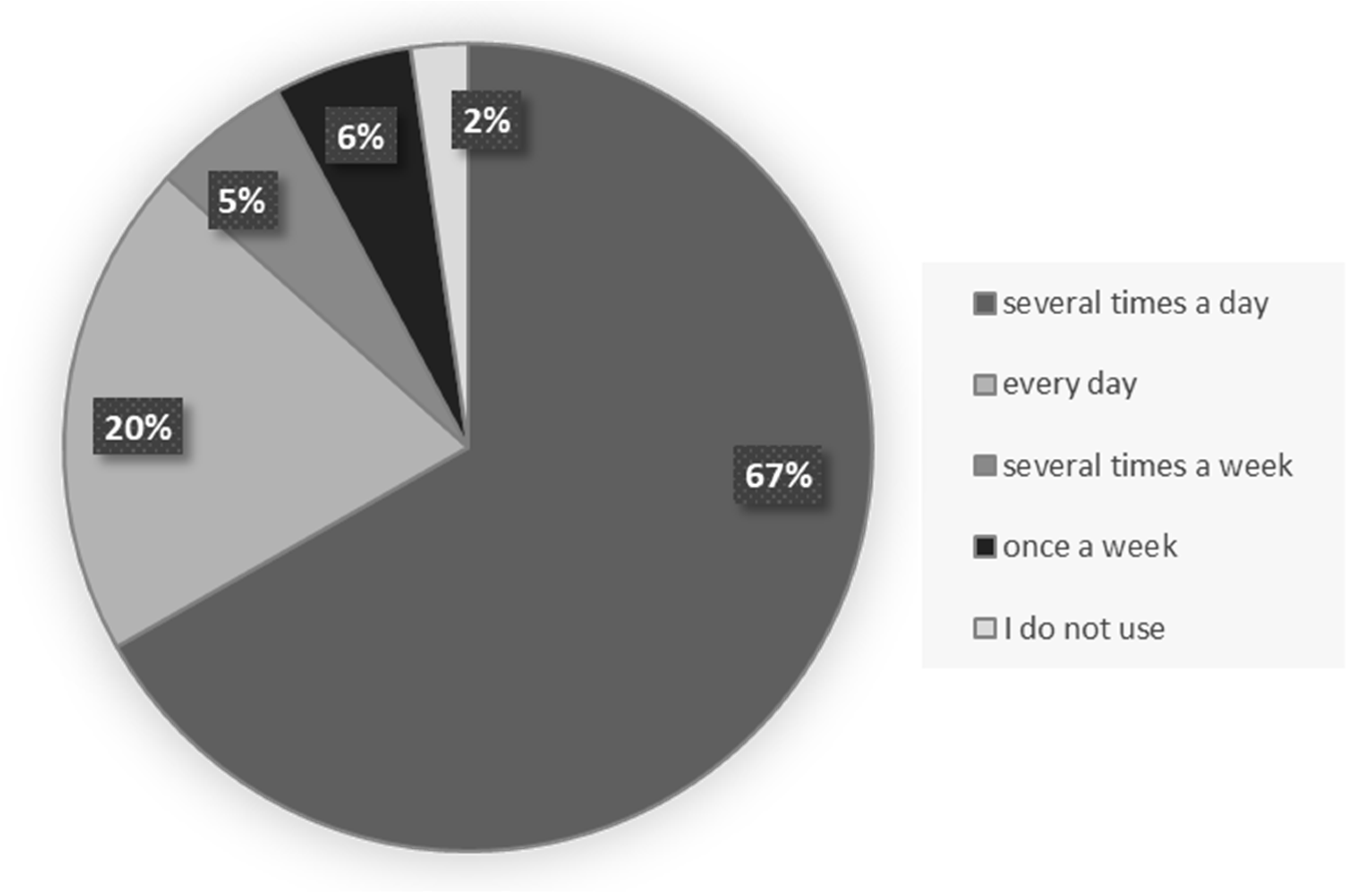
In general, the majority of 307 physicians who participated in the study were familiar with new technologies. Both in their private and professional life, they use a smartphone (83.4% vs. 47.6%), a computer (65.8% vs. 85.0%), and e-mail (70.7 % vs. 30.9%). Respondents reported using the Internet mainly several times a day (66.8%) or every day (19.9%), which does not differ significantly from the statistics in previous studies [
2,
8,
21,
47,
50]. In the “Internet in the life of Poles” report commissioned by the Ministry of Digitization in June 2019, the professional group most willing to use the Internet and e-services were physicians [
51].
A similar situation applied to the skills to use e-health—clinicians described them as very good (33.6%) or good (32.6%). Moreover, our study has demonstrated that the more intensive the Internet use, the higher digital skills (
F = 13.167;
p < 0.0001). However, according to the CPME Policy on Digital Competencies for Doctors, neither the practicing health professionals nor the generation in training are adequately prepared, and there is still a gap between understanding how digital solutions may support their capabilities, as well as the actual use of them [
25]. The self-reported level of digital skills in this study reflects professionals’ confidence and understanding the status new technologies in healthcare.
In this context, interesting results were obtained: although 70% of respondents felt prepared to support e-health solutions, still a significant percentage (84%) reported the need for additional training or courses in the field of shaping digital skills. Additionally, the more the use of electronic devices (computer, tablet, smartphone, e-mail, and mobile apps), the greater the need for training in the field of digital literacy that was reported. The study prepared for the European Parliament confirms these fears: of the participants that received digital skills training, 54% rated it as insufficient. A survey of more than 200 physicians found that a large majority (80%) of the questioned professionals indicated that the currently available e-health/m-health training is inadequate [
52]. Especially since digital skills have been shown to deteriorate with the age of surveyed physicians. These are important findings, according to the dominant opinion (77.9%) among physicians that the Internet would revolutionize modern healthcare. The awareness of the importance of digitization, in the case of the surveyed doctors, was connected with the explicit doubt regarding whether the educational programs in medical studies follow the technological challenges of the 21st century. It is a paradox that, in times of an unprecedented technological boom, medical education in this field is still insufficient, as multiplicity studies from different countries have reported [
53,
54,
55].
The use of the Internet for health purposes is increasing, but its impact on healthcare is still unclear. Undeniably seeking health information online will keep increasing [
56]. People indicate the Internet as the first source of health information primarily because of limited time consultation and barriers to accessing professional health services [
57]. However, how the above translates into interaction: physician-the Web-patient? Cocco et al. found that seeking online health information by patients had positive effects on the doctor–patient relationship and improved their communication. However, at the same time, it was noticed, that the Internet-sourced information did cause some anxiety for 40% of searchers [
58].
Polish Internet users most often (almost 59%) pointed that data they can find on the Internet does not require leaving home. Almost equally important (53%) was the opportunity to find the information 24/7. Another reason indicated by 32% of respondents was to supplement the information that they did not receive during a medical visit. Thanks to the information obtained earlier, almost 25% of respondents felt better prepared to visit a doctor. The next places were: the possibility of finding information that is not elsewhere (23%), anonymity (20%), or the ability to contact other people in a similar situation (16%) [
59]. Based on the national survey conducted in 2013 by the Pew Research Center’s Internet and American Life Project, 1 in 3 American adults said they went online to determine their medical condition, and 35% of the respondents said they do not need any professional opinion [
11]. In our study, every third physician (33.2%) acknowledged that more than 10% of her/his patients access health information on the Internet within a month. A total of 85% physicians questioned by Murray et al. had experienced a patient bringing Internet information to a visit [
13]. The quality assessment of this information in physician’s opinion in our study was most often perceived as sometimes reliable (53.4%). Potts and Wyatt came to similar conclusions, reporting that over two thirds of the questioned professionals considered online health information to be usually (20%) or sometimes (48%) reliable [
60]. Again, data from our study showed that physicians who assessed the effects of using the online health knowledge by patients very positively had greater digital skills, recommended e-health solutions, and rated e-health solutions higher. At the same time, those who assessed the effects of the use of the Internet by patients negatively indicated the need for training in digital literacy. We did not check whether these results significantly affect the doctors–patients’ relationship, but Murray et al. reported that physicians did have an impression that their authority was challenged because of Dr. Google [
13]. Moreover, this reaction was associated with harms to the quality of care, health outcomes, and time efficiency. The results of other studies indicate that physicians’ attitude to online health information seeking is critical [
43], and they are not very familiar or confident with patients who ‘Google’ [
61].
In the context of recommending and assessing e-health solutions, Polish physicians remained favourable and expressed a definite desire to recommend such solutions to their patients. It is a limitation that our study was conducted before the strongest influence of COVID-19 pandemic, which further shows the positive attitude of doctors to this type of solutions. The pandemic has forced changes in digital health, which should be investigated, but in its source, modern health care refers to the educational role of a doctor who can have an active impact on the patient, providing reliable and trustworthy recommendations of new technological solutions dedicated to health [
17,
62]. However, as our research showed, with the lower digital skills of physician, the recommendation of e-health solutions decreased, and the assessment of e-health solutions for the patient was reduced.
To sum up, the strategic importance of digital skills goes beyond the issue of the short-term development of e-health itself—it should be considered as a key factor of the development of conscious information society, both on the side of the professionals and the recipients of services, neither in highly developed nor in developing countries. Smartphones, universal access to the Internet, and mobile applications meeting patients’ expectations are revolutionizing the sector. Additionally, telemedicine began filling into clinical practice, medical universities began including e-health in their curricula, and health systems are introducing legal regulations supporting digital health.
The issue of digitization in healthcare is often referred to as a process depending only on the technology to which people should adapt. Digital reality, however, is not only the e-development, but also the need for a holistic approach to the entire sector, organizational processes, legal regulations, and standards that guarantee interoperability and cooperation between the physician, the Web, and the patient.