Journal Description
Gastrointestinal Disorders
Gastrointestinal Disorders
is an international, open access, peer-reviewed journal on gastroenterology, published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions; authors retain copyright.
- High Visibility: indexed within Scopus, ESCI (Web of Science), FSTA, and other databases.
- Journal Rank: CiteScore - Q2 (Immunology and Microbiology (miscellaneous))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 21.3 days after submission; acceptance to publication is undertaken in 5.2 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Reliable service: rigorous peer review and professional production.
Impact Factor:
0.7 (2022)
Latest Articles
Factors Affecting Diagnostic Yields of Capsule Endoscopy for Obscure Gastrointestinal Bleeding
Gastrointest. Disord. 2024, 6(2), 468-477; https://doi.org/10.3390/gidisord6020032 - 22 May 2024
Abstract
Background/Aims: The purpose of this study was to determine the factors affecting positive diagnostic yields in patients with obscure gastrointestinal bleeding (OGIB) according to the guideline of small bowel capsule endoscopy (SBCE). Method: Patients with a complaint of melena or hematochezia who were
[...] Read more.
Background/Aims: The purpose of this study was to determine the factors affecting positive diagnostic yields in patients with obscure gastrointestinal bleeding (OGIB) according to the guideline of small bowel capsule endoscopy (SBCE). Method: Patients with a complaint of melena or hematochezia who were admitted were consecutively enrolled. In patients with gastrointestinal bleeding, examination was performed according to the guideline. When OGIB was suspected, SBCE was performed. Patients were categorized into two subgroups based on the SBCE results: a positive group (n = 78) and a negative group (n = 67). Results: The rate of the positive diagnostic yield of SBCE was 53.8% (78/145). In patients over 60 years, the diagnostic yield was 61.5%, which was higher than in patients younger than 60 years (40.7%). In the multivariate analysis, there was a significant difference in the positive diagnostic yield in the patients aged over 60 years (p < 0.01). Factors related to the procedure and clinical characteristics also showed significant differences in the positive predictive rates according to the degree of bowel preparation, small bowel transit time, and transfusion requirements. Conclusions: SBCE could be recommended as a diagnostic tool for OGIB, especially in those with old ages (>60 years) and those who need transfusion, because of its relatively high diagnostic yields in these populations. Proper bowel preparation and a prolonged small bowel transit time may have clinical significance in relation to the positive diagnostic yield of SBCE in patients with OGIB.
Full article
(This article belongs to the Topic Advances in Gastrointestinal and Liver Disease: From Physiological Mechanisms to Clinical Practice)
►
Show Figures
Open AccessBrief Report
Food Insecurity Is Associated with a Higher Risk of Mortality among Colorectal Cancer Survivors
by
Jagdish Khubchandani, Srikanta Banerjee, Rafael Gonzales-Lagos and Karen Kopera-Frye
Gastrointest. Disord. 2024, 6(2), 461-467; https://doi.org/10.3390/gidisord6020031 - 17 May 2024
Abstract
Purpose: Food insecurity and colorectal cancer (CRC) are widely prevalent problems in the U.S. However, the long-term effects of food insecurity among people living with CRC are not well explored (e.g., risk of mortality). Methods: Data from the U.S. National Health and Nutrition
[...] Read more.
Purpose: Food insecurity and colorectal cancer (CRC) are widely prevalent problems in the U.S. However, the long-term effects of food insecurity among people living with CRC are not well explored (e.g., risk of mortality). Methods: Data from the U.S. National Health and Nutrition Examination Survey (years 1999–2010) were linked with mortality data from the National Death Index up to 31 December 2019. Results: A total of 30,752 adults comprised the analytic sample; 222 were living with CRC and more than a tenth were food-insecure (11.6%). In our adjusted analysis, individuals who were food insecure and had CRC were 4.13 times more likely to die of any cause and 9.57 times more likely to die of cardiovascular diseases (compared to those without CRC and food insecurity). Conclusions: Colorectal cancer is among the top cancers diagnosed in American adults and more than a tenth of adult Americans with CRC live with food insecurity. Given the higher risk of mortality with co-occurring CRC and food insecurity, collaborative healthcare models can help address food insecurity and other social needs of people with CRC, and surveillance measures for food insecurity should be widely implemented across health systems.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
Open AccessReview
Role of IL-33/ST2 Pathway in Inflammatory Bowel Disease: An Overview and Future Perspectives
by
Walter Giordano, Gabriele Ricciardi, Marco Casciaro, Vincenzo Fiorentino, Cristina Pizzimenti, Anna Viola, Maurizio Martini, Giovanni Tuccari and Antonio Ieni
Gastrointest. Disord. 2024, 6(2), 446-460; https://doi.org/10.3390/gidisord6020030 - 10 May 2024
Abstract
Inflammatory bowel disease (IBD) represents a heterogenous and complex group of idiopathic chronic inflammatory conditions affecting the gastrointestinal tract and other extraintestinal systems with rising global incidences. The interplay of genetic predisposition and environmental factors contributes to its pathogenesis. Among the key cytokines
[...] Read more.
Inflammatory bowel disease (IBD) represents a heterogenous and complex group of idiopathic chronic inflammatory conditions affecting the gastrointestinal tract and other extraintestinal systems with rising global incidences. The interplay of genetic predisposition and environmental factors contributes to its pathogenesis. Among the key cytokines implicated in IBD molecular alterations, IL-33 stands out for its multifaceted roles in both pathogenesis and repair mechanisms. IL-33, known for its action in initiating immune responses, is closely associated with Th2 immunity and is considered a potent inflammatory factor with dual functions, acting both as a pro-inflammatory cytokine and a transcriptional regulator. Primarily expressed by non-hematopoietic cells in the gastrointestinal tract, IL-33 interacts with its receptor, ST2, to modulate immune responses. In IBD, dysregulated IL-33 expression exacerbates mucosal inflammation, compromising barrier integrity and promoting tissue damage and fibrosis. Additionally, IL-33 plays a complex role in IBD-related colorectal cancer (CRC), affecting tumor progression and angiogenesis. This review summarizes the multifaceted roles of IL-33 in gastrointestinal health and disease, emphasizing its significance in the pathogenesis of IBD and CRC. Moreover, we thought it of interest to provide new insights into potential therapeutic avenues targeting IL-33 signaling for the management of these debilitating conditions.
Full article
(This article belongs to the Special Issue Factors Affecting Disease Activity in Children and Adults with Inflammatory Bowel Disease: An Exploration of Pro-Inflammatory and Anti-Inflammatory Elements)
►▼
Show Figures

Figure 1
Open AccessReview
Gut Microbiota and Immune System in Necrotizing Enterocolitis and Related Sepsis
by
Emilio Jirillo, Skender Topi, Ioannis Alexandros Charitos, Luigi Santacroce, Elona Gaxhja and Marica Colella
Gastrointest. Disord. 2024, 6(2), 431-445; https://doi.org/10.3390/gidisord6020029 - 10 May 2024
Abstract
A severe condition of sepsis can be a complication of necrotizing enterocolitis (NEC), which can occur in premature infants and becomes a medical challenge in the neonatal intensive care unit (NICU). It is a multifactorial intestinal disease (can affect both the small and
[...] Read more.
A severe condition of sepsis can be a complication of necrotizing enterocolitis (NEC), which can occur in premature infants and becomes a medical challenge in the neonatal intensive care unit (NICU). It is a multifactorial intestinal disease (can affect both the small and large intestine) that can lead to ischemia of the intestinal tissues that evolves into acute organ necrosis. One of these factors is that different types of nutrition can influence the onset or the progression of the disease. Cow-milk-based infant formulas have been shown to cause it in premature infants more frequently than human milk. Recently, nutrition has been shown to be beneficial after surgery. Several issues still under study, such as the pathogenesis and the insufficient and often difficult therapeutic approach, as well as the lack of a common and effective prevention strategy, make this disease an enigma in daily clinical practice. Recent studies outlined the emerging role of the host immune system and resident gut microbiota, showing their close connection in NEC pathophysiology. In its initial stages, broad-spectrum antibiotics, bowel rest, and breastfeeding are currently used, as well as probiotics to help the development of the intestinal microbiota and its eubiosis. This paper aims to present the current knowledge and potential fields of research in NEC pathophysiology and therapeutic assessment.
Full article
(This article belongs to the Special Issue Factors Affecting Disease Activity in Children and Adults with Inflammatory Bowel Disease: An Exploration of Pro-Inflammatory and Anti-Inflammatory Elements)
►▼
Show Figures
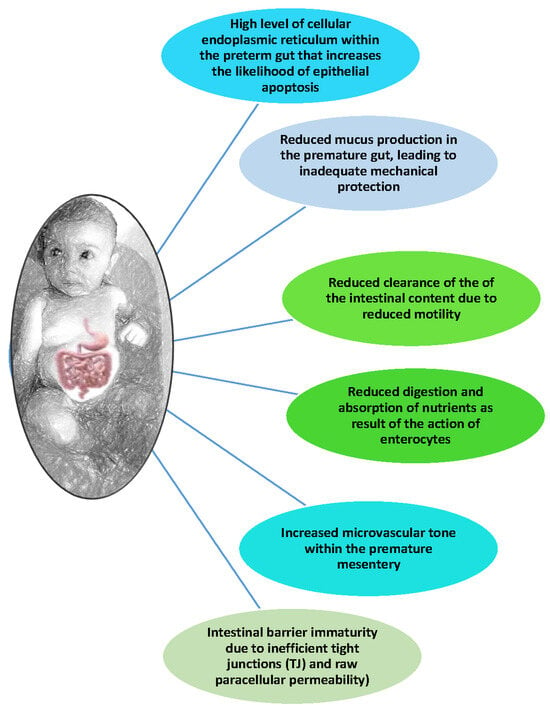
Figure 1
Open AccessArticle
Survey on the Knowledge and the Management of Helicobacter pylori Infection by Italian General Practitioners and Doctors in General Practice Training
by
Cesare Tosetti, Enzo Ubaldi, Edoardo Benedetto, Luciano Bertolusso, Luigi Napoli, Carmelo Cottone, Riccardo Scoglio, Alessandra Belvedere, Giovanni Casella, Maurizio Mancuso, Gennaro Abagnale, Guido Sanna and Rudi De Bastiani
Gastrointest. Disord. 2024, 6(2), 421-430; https://doi.org/10.3390/gidisord6020028 - 30 Apr 2024
Abstract
The management of gastric Helicobacter pylori (H. pylori) infection represents a significant concern in primary healthcare. This survey evaluates the approaches, attitudes, and knowledge regarding gastric H. pylori infection among Italian general practitioners (GPs) and young doctors undergoing general practice training
[...] Read more.
The management of gastric Helicobacter pylori (H. pylori) infection represents a significant concern in primary healthcare. This survey evaluates the approaches, attitudes, and knowledge regarding gastric H. pylori infection among Italian general practitioners (GPs) and young doctors undergoing general practice training (ITGPs). The survey enrolled 466 GPs and 70 ITGPs. Among GPs, specialist recommendations and the Maastricht–Florence guidelines were frequently referenced sources, while ITGPs relied more on the Maastricht–Florence guidelines and internet resources. ITGPs demonstrated more proactive approaches than GPs in investigating and treating conditions such as gastric ulcers, atrophic gastritis, and iron-deficiency anemia. However, there was limited attention given to the role of H. pylori treatment in first-degree relatives of gastric cancer patients. The most used diagnostic methods were the urea breath test and fecal test. Triple therapy was the most frequently chosen initial treatment regimen, with quadruple bismuth therapy becoming the primary option after initial treatment failure, followed by quinolone therapy and concomitant therapy. This survey underscores a disparity between real-world practices and the recommendations outlined in current guidelines, indicating a need for improved understanding of H. pylori guidelines among both GPs and ITGPs.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
Open AccessArticle
Prognostic Factors after Hepatectomy for Hepatocellular Carcinoma—The Importance of Pathological Immunophenotyping, the Steatohepatitic Subtype and the Impact of the Hepatic Pedicle Clamping
by
Lorrane Viana, Rui Caetano Oliveira, Ricardo Martins, Henrique Alexandrino, Maria Augusta Cipriano and José Guilherme Tralhão
Gastrointest. Disord. 2024, 6(2), 402-420; https://doi.org/10.3390/gidisord6020027 - 15 Apr 2024
Abstract
►▼
Show Figures
Introduction: Hepatectomy (HP) is, along with liver transplantation, the only potentially curative treatment for Hepatocellular Carcinoma (HCC). The high prevalence of Metabolic Syndrome (MS) may be causing a shift in the HCC spectrum. Hepatic Pedicle Clamping (HPC), used to reduce perioperative bleeding during
[...] Read more.
Introduction: Hepatectomy (HP) is, along with liver transplantation, the only potentially curative treatment for Hepatocellular Carcinoma (HCC). The high prevalence of Metabolic Syndrome (MS) may be causing a shift in the HCC spectrum. Hepatic Pedicle Clamping (HPC), used to reduce perioperative bleeding during HP, has been theorized to increase the risk of recurrence. Cytokeratin 19 (CK19) and glypican-3 (GLP-3) have been identified as markers of worse prognosis in HCC. Materials and Methods: A clinical and pathological review of 59 patients undergoing HP for HCC between 2005 and 2013 was performed. Chronic liver disease was observed in 53 patients (89.8%), with cirrhosis in 54.2% [most frequent etiologies: ethylism (47.5%), HCV (25.4%) and HBV (11.9%)]. MS was in 36% of patients. In addition, 95% of patients had Child–Pugh class A and 5% class B, and there was a median MELD of 8 (6–18). A single nodule was observed in 46 patients (78%) with an average size of 5.4 cm. Microscopic vascular invasion (MiVI) was in 49% of patients and macroscopic (MaVI) in 17. HPC was in 43 patients (74.1%). Statistical analysis was performed with SPSS™ 21.0. Survival tests (Kaplan–Meier, log-rank and Cox regression). Statistical significance was with p < 0.05. Results: Major morbidity in 22% of patients. Mortality in 5.1%. Median overall survival (OS) of 71 months and median disease-free survival (DFS) of 37. In a multivariate analysis: MaVI (p = 0.001), MiVI (p = 0.005) and HCV infection (p = 0.002) were associated with worse OS; MS was associated with better OS (p = 0.001); MaVI (p = 0.000), MiVI (p = 0.035) and HPC (p = 0.012) were associated with worse DFS. CK19+/GLP-3− (p = 0.007) and CK19−/GLP-3+ (p = 0.029) patients were associated with worse DFS and CK19−/GLP-3− (p = 0.031) with better DFS. Discussion/Conclusions: HPC was an independent factor of worse DFS. The ischemia-reperfusion injury (IRI) produced by HPC could promote a more angiogenic and angioinvasive phenotype of tumor cells, resulting in higher recurrence. HCV etiology was associated with worse OS. MS was associated with better OS, highlighting the importance of a hepatectomy in these cases. The combined detection of CK19 and GLP-3 was an independent prognostic factor in HCC patients allowing for the identification of more aggressive tumors.
Full article
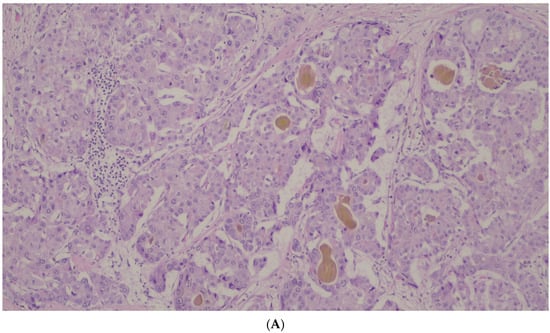
Figure 1
Open AccessReview
Focused Ultrasound as Targeted Therapy for Colorectal Cancer: A Comprehensive Review
by
Muhammad Awais Farooqi, Mahnoor Mahnoor, Kaylee Marie Delgado, Wylie Thien-Tam Dahlgren, Chul-Ung Kang and Hafiz Muhammad Umer Farooqi
Gastrointest. Disord. 2024, 6(2), 380-401; https://doi.org/10.3390/gidisord6020026 - 13 Apr 2024
Abstract
►▼
Show Figures
Traditional cancer treatments have not significantly improved the survival rates for individuals with colorectal cancer. As a result, there is a dire need to explore novel treatment modalities that can target cancer-specific niches, transform cold colorectal tumors into hot ones, and disrupt the
[...] Read more.
Traditional cancer treatments have not significantly improved the survival rates for individuals with colorectal cancer. As a result, there is a dire need to explore novel treatment modalities that can target cancer-specific niches, transform cold colorectal tumors into hot ones, and disrupt the tumor niche. Therapeutic focused ultrasound, recognized for its capacity to induce thermal and mechanical impacts on tissue, can potentially eliminate cancer cells and elicit the body’s anticancer reaction by disrupting the tumor microenvironment. This article provides an overview of recent developments in employing therapeutic focused ultrasound (TFUS) to enhance the body’s natural defenses against colorectal cancers. It also discusses studies examining the utility of TFUS in treating colorectal cancer patients and recent research indicating its potential to stimulate the body’s anticancer response in various in vitro and in vivo colorectal cancer models. Furthermore, it explores the therapeutic effects of TFUS on the immune system in colorectal cancers. This article also highlights the safety and effectiveness of TFUS in managing colorectal cancer, providing relief from pain, and potentially improving survival rates. Given the indications that TFUS may bolster the body’s immune response and augment the impacts of TFUS therapy in clinical and preclinical colorectal cancer models, it has the potential to emerge as a pivotal tool in clinical settings.
Full article
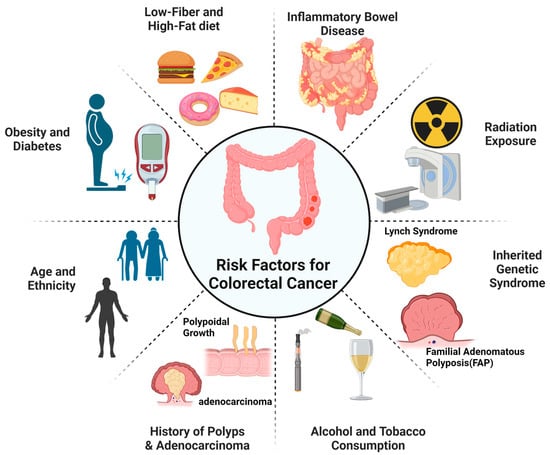
Figure 1
Open AccessReview
Enteric Nervous System Alterations in Inflammatory Bowel Disease: Perspectives and Implications
by
Shubhankar Suman
Gastrointest. Disord. 2024, 6(2), 368-379; https://doi.org/10.3390/gidisord6020025 - 28 Mar 2024
Abstract
►▼
Show Figures
The enteric nervous system (ENS), consisting of neurons and glial cells, is situated along the gastrointestinal (GI) tract’s wall and plays a crucial role in coordinating digestive processes. Recent research suggests that the optimal functioning of the GI system relies on intricate connections
[...] Read more.
The enteric nervous system (ENS), consisting of neurons and glial cells, is situated along the gastrointestinal (GI) tract’s wall and plays a crucial role in coordinating digestive processes. Recent research suggests that the optimal functioning of the GI system relies on intricate connections between the ENS, the intestinal epithelium, the immune system, the intestinal microbiome, and the central nervous system (CNS). Inflammatory bowel disease (IBD) encompasses a group of chronic inflammatory disorders, such as Crohn’s disease (CD) and ulcerative colitis (UC), characterized by recurring inflammation and damage to the GI tract. This review explores emerging research in the dynamic field of IBD and sheds light on the potential role of ENS alterations in both the etiology and management of IBD. Specifically, we delve into IBD-induced enteric glial cell (EGC) activation and its implications for persistent enteric gliosis, elucidating how this activation disrupts GI function through alterations in the gut–brain axis (GBA). Additionally, we examine IBD-associated ENS alterations, focusing on EGC senescence and the acquisition of the senescence-associated secretory phenotype (SASP). We highlight the pivotal role of these changes in persistent GI inflammation and the recurrence of IBD. Finally, we discuss potential therapeutic interventions involving senotherapeutic agents, providing insights into potential avenues for managing IBD by targeting ENS-related mechanisms. This approach might represent a potential alternative to managing IBD and advance treatment of this multifaceted disease.
Full article
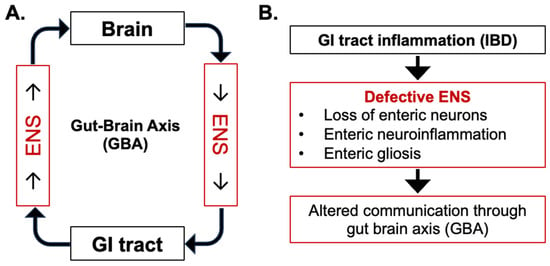
Figure 1
Open AccessBrief Report
Bowel Cleansing Preparations Are Associated with Gastroduodenal Lesions
by
Anas Khouri, Cesar G. Moreno and Jack A. Di Palma
Gastrointest. Disord. 2024, 6(1), 359-367; https://doi.org/10.3390/gidisord6010024 - 15 Mar 2024
Abstract
►▼
Show Figures
Background: During esophagogastroduodenoscopy performed with colonoscopy, gastric and duodenal erythema, erosions, and ulcerations are often observed. This investigation was designed to review the prevalence of gastroduodenal lesions in patients who have undergone wireless capsule endoscopy using standard bowel cleansing preparations, but no endoscopy
[...] Read more.
Background: During esophagogastroduodenoscopy performed with colonoscopy, gastric and duodenal erythema, erosions, and ulcerations are often observed. This investigation was designed to review the prevalence of gastroduodenal lesions in patients who have undergone wireless capsule endoscopy using standard bowel cleansing preparations, but no endoscopy or sedation. Methods: A retrospective analysis was conducted on patients referred for capsule endoscopy. Records and capsule reports were reviewed for the patient demographics, preparation prescribed, procedural indications, and gastroduodenal findings. The preparations studied included polyethylene glycol lavage (PEG), PEG plus bisacodyl (PEG + bis), bisacodyl (bis), oral sulfate solution (OSS), and no prep. Results: Among the 1236 records, 498 (40.3%) were men and 738 (59.7%) were women. The mean age was 56 years +/− 18 years SD. The percentage of patients with lesions after any bowel preparation was 52.7% for gastric lesions and 23.6% for duodenal lesions. The percentage of patients with gastroduodenal lesions was 58.3% with prep, compared to 38.2% without prep. These findings were statistically significant, with an RR of 1.53 [1.19–1.94] (p-value = 0.00004). This difference was more pronounced in the OSS group RR of 1.65 [1.29–2.1] and bisacodyl group RR of 1.64 [1.25–2.15] compared to the PEG group RR of 0.95 [0.7–1.3]. Conclusions: This study showed that patients undergoing wireless capsule endoscopy who received bowel preparations had a significant increase in gastric and duodenal lesions. Of the preparations studied, OSS was associated with a greater number of gastroduodenal lesions, while PEG was the least associated with lesions, with an occurrence similar to the non-prep group. The clinical significance of these lesions remains undetermined. Endoscopists should be aware that preparations are associated with gastroduodenal lesions to avoid the misinterpretation and misdiagnosis of these lesions.
Full article
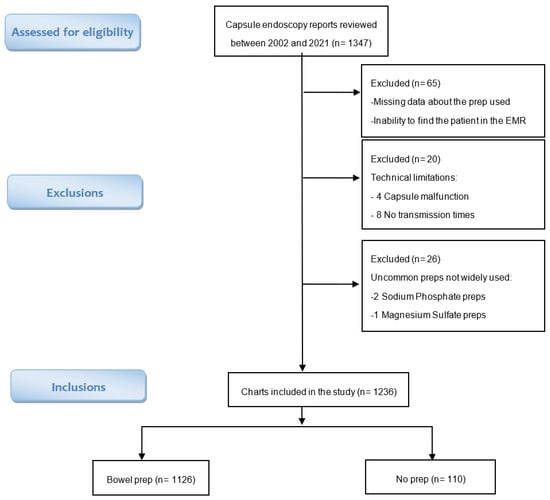
Figure 1
Open AccessReview
A Critical Review on In Vitro and Ex Vivo Models of the Intestinal Epithelium of Humans and Monogastric Animals
by
Célia Maria Costa, Nelson Mota de Carvalho, Diana Luazi de Oliveira and Ana Raquel Madureira
Gastrointest. Disord. 2024, 6(1), 337-358; https://doi.org/10.3390/gidisord6010023 - 14 Mar 2024
Abstract
►▼
Show Figures
Recently, the bioactive potential of several functional ingredients and biomolecules has been evaluated regarding human and animal nutrition. The digestive process from food intake to absorption and metabolism are important events that induce changes in ingredients, which affect their bioactivity. Consequently, there is
[...] Read more.
Recently, the bioactive potential of several functional ingredients and biomolecules has been evaluated regarding human and animal nutrition. The digestive process from food intake to absorption and metabolism are important events that induce changes in ingredients, which affect their bioactivity. Consequently, there is a need to assess the bioavailability and bioaccessibility of these compounds. The methodology for the simulation of the human gastrointestinal tract has been standardized (INFOGEST protocol), while a gastrointestinal protocol for other animals (e.g., ruminants or broilers) has yet to be established. However, INFOGEST allows us only to predict bioaccessibility, leaving a gap regarding a methodology able to assess bioavailability by mimicking intestinal permeability and absorption. Several approaches—including in vitro, ex vivo, in situ and in vivo methods—can be found in the literature, aiming to tackle transepithelial routes, but leading to different results concerning the bioefficiency of the compounds studied. Therefore, this review aims to assess the current state-of-the-art regarding monogastric intestinal dynamics, absorption, and permeability events. Moreover, it compiled methodologies for simulating intestinal absorption in several biological systems, while reasoning their advantages, disadvantages, applications in ingredient development and the existing gaps.
Full article
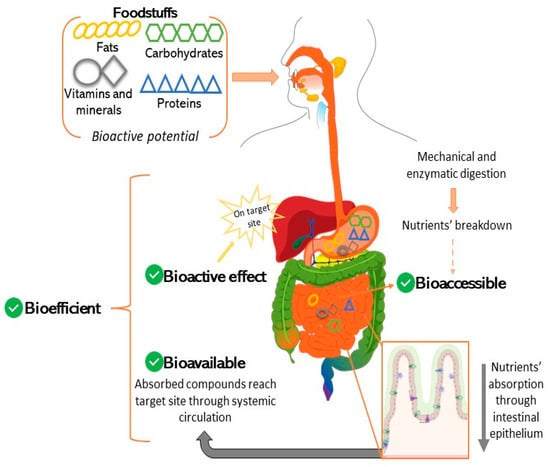
Figure 1
Open AccessReview
Main Disorders of Gastrointestinal Tract in Older People: An Overview
by
Antonella Gallo, Simona Pellegrino, Erika Pero, Maria Chiara Agnitelli, Caterina Parlangeli, Francesco Landi and Massimo Montalto
Gastrointest. Disord. 2024, 6(1), 313-336; https://doi.org/10.3390/gidisord6010022 - 10 Mar 2024
Abstract
►▼
Show Figures
From a physiological standpoint, aging is a progressive reduction in each organ system’s capacity to maintain homeostasis in the face of illness or stressors. With advancing age, gastrointestinal (GI) symptoms and signs may increase, not only due to the aging processes but also
[...] Read more.
From a physiological standpoint, aging is a progressive reduction in each organ system’s capacity to maintain homeostasis in the face of illness or stressors. With advancing age, gastrointestinal (GI) symptoms and signs may increase, not only due to the aging processes but also to the superimposed effects of comorbidities, which can badly affect digestive functions (i.e., diabetes, malignancy, etc.) and environmental exposure. In general, gastrointestinal symptoms in older people more often underlie organic pathologies, while GI functional disorders are less frequently diagnosed in this age group. Moreover, gastrointestinal disease can also present in a nuanced and atypical manner, making the diagnostic hypothesis and, consequently, the correct diagnosis and therapy more challenging. In addition, with reference to this age group, the clinical implications of gastrointestinal pathologies can be more severe due to a decreased physiologic reserve, with a higher risk for malnutrition resulting in falls, depression, social isolation, and a deterioration of functional status. In this review, we focused on the most frequent GI tract disorders, highlighting the main age-related changes, their epidemiological, pathophysiological and clinical implications, and any differences with younger patients.
Full article

Figure 1
Open AccessEditorial
Editorial: Pediatric Functional Gastrointestinal Disorders: Challenges in Diagnosis and Treatment
by
Angharad Vernon-Roberts, Mark Safe and Andrew S. Day
Gastrointest. Disord. 2024, 6(1), 308-312; https://doi.org/10.3390/gidisord6010021 - 8 Mar 2024
Abstract
Functional gastrointestinal disorders (FGIDs) are classified as those with no organic cause and those not attributable to structural or biochemical abnormalities [...]
Full article
(This article belongs to the Special Issue Pediatric Functional Gastrointestinal Disorders: Challenges in Diagnosis and Treatment)
Open AccessArticle
Detection of Ulcerative Colitis Lesions from Weakly Annotated Colonoscopy Videos Using Bounding Boxes
by
Safaa Al-Ali, John Chaussard, Sébastien Li-Thiao-Té, Éric Ogier-Denis, Alice Percy-du-Sert, Xavier Treton and Hatem Zaag
Gastrointest. Disord. 2024, 6(1), 292-307; https://doi.org/10.3390/gidisord6010020 - 7 Mar 2024
Abstract
►▼
Show Figures
Ulcerative colitis is a chronic disease characterized by bleeding and ulcers in the colon. Disease severity assessment via colonoscopy videos is time-consuming and only focuses on the most severe lesions. Automated detection methods enable fine-grained assessment but depend on the training set quality.
[...] Read more.
Ulcerative colitis is a chronic disease characterized by bleeding and ulcers in the colon. Disease severity assessment via colonoscopy videos is time-consuming and only focuses on the most severe lesions. Automated detection methods enable fine-grained assessment but depend on the training set quality. To suit the local clinical setup, an internal training dataset containing only rough bounding box annotations around lesions was utilized. Following previous works, we propose to use linear models in suitable color spaces to detect lesions. We introduce an efficient sampling scheme for exploring the set of linear classifiers and removing trivial models i.e., those showing zero false negative or positive ratios. Bounding boxes lead to exaggerated false detection ratios due to mislabeled pixels, especially in the corners, resulting in decreased model accuracy. Therefore, we propose to evaluate the model sensitivity on the annotation level instead of the pixel level. Our sampling strategy can eliminate up to 25% of trivial models. Despite the limited quality of annotations, the detectors achieved better performance in comparison with the state-of-the-art methods. When tested on a small subset of endoscopic images, the best models exhibit low variability. However, the inter-patient model performance was variable suggesting that appearance normalization is critical in this context.
Full article

Figure 1
Open AccessReview
Mesenchymal Tumors of the Gastrointestinal Tract—Beyond GIST—A Review
by
João Martins Gama and Rui Caetano Oliveira
Gastrointest. Disord. 2024, 6(1), 257-291; https://doi.org/10.3390/gidisord6010019 - 4 Mar 2024
Abstract
►▼
Show Figures
Sarcomas are rare lesions and encompass a wide variety of entities, depending on their nature. In recent years new entities have been described and new knowledge, especially that provided by molecular studies, has been increasing. This makes it very difficult to be updated
[...] Read more.
Sarcomas are rare lesions and encompass a wide variety of entities, depending on their nature. In recent years new entities have been described and new knowledge, especially that provided by molecular studies, has been increasing. This makes it very difficult to be updated with all the described entities, since only some of the centers have the desired ancillary studies for the correct diagnosis. Some lesions are extremely rare and may appear once or twice during the lifetime of a general pathologist. When we refer to sarcomas of the gastrointestinal tract, the gastrointestinal stromal tumor (GIST) is the most well-known lesion that the pathologist will most frequently find in daily practice. This paper aims to comprehensively review the sarcomas associated with the gastrointestinal tract, emphasizing histopathology and going beyond GIST. This review highlights the histopathology of rare types of sarcomas so it may increase awareness of common and rare lesions, prompting an easy and effective diagnosis.
Full article
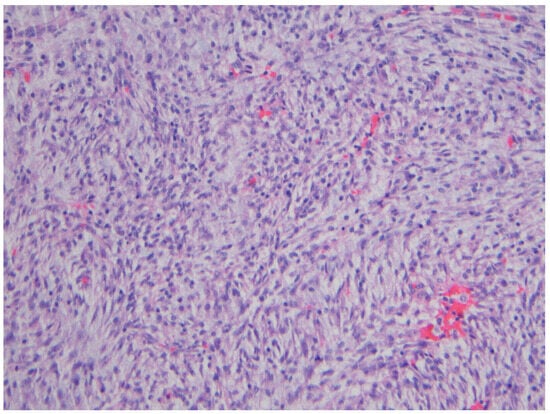
Figure 1
Open AccessReview
Biologics in Focus: A Comprehensive Review of the Current Biological Therapies for Ulcerative Colitis in the United Arab Emirates (UAE)
by
Ahmed El-Sayed, Ceyhun Oztumer, Camellia Richards, Omar-Adam Salim, Mathuri Sivakumar and Laith Alrubaiy
Gastrointest. Disord. 2024, 6(1), 241-256; https://doi.org/10.3390/gidisord6010018 - 1 Mar 2024
Abstract
Background: Ulcerative colitis (UC) is a relapsing–remitting inflammatory condition that has an increasing incidence across the world, including in the Middle East. Biological monoclonal antibody drugs (biologics) have been shown to be advantageous in treating UC. We undertook a review of the currently
[...] Read more.
Background: Ulcerative colitis (UC) is a relapsing–remitting inflammatory condition that has an increasing incidence across the world, including in the Middle East. Biological monoclonal antibody drugs (biologics) have been shown to be advantageous in treating UC. We undertook a review of the currently available biological and small-molecule therapies, with a particular emphasis on those currently licensed in the United Arab Emirates (UAE). Methods: We conducted a literature search for studies on biological therapies using the PubMed, MEDLINE, and Embase databases using a list of keywords that were generated following referral to existing treatment guidelines for UC. Papers looking at biological and small-molecule treatments for UC in adult populations were included. Pediatric, pregnancy, and cost-effectiveness studies were excluded. Results and Discussion: There are currently three classes of biologics (anti-tumor necrosis factors (anti-TNFs), anti-integrins, and anti-interleukins) and one class of small-molecule therapy (Janus kinase (JAK) inhibitor) licensed for UC treatment in the UAE. Within the anti-TNF class, three medications have been approved: infliximab, adalimumab, and golimumab. For JAK inhibitors, there are two: tofacitinib and upadacitinib. There is only one licensed medication in the remaining classes: vedolizumab (anti-integrin) and ustekinumab (anti-interleukin). The length of studies varied from 6–8 weeks for induction studies and 52 weeks for maintenance studies. The studies demonstrated increased efficacy in these medications compared to placebos when clinical response, clinical remission, and other secondary measures such as mucosal healing were assessed following the induction and maintenance phases. Biosimilars of infliximab and adalimumab are also available for treating UC, and their safety and efficacy were compared to their biologic originators. Conclusions: The introduction of biologics has been proven to be beneficial for the treatment of UC. This review summarizes the efficacy and safety of each biological class in the treatment of the disease; however, biological drug registries and further studies are required to offer more insight into the comparative efficacy and safety of these agents.
Full article
Open AccessArticle
Prospective Visual Inspection of the Ventrum of Tongue (VIVOT) Vasculature Predicts the Presence of Esophageal Varices
by
Martin Tobi, Monina Pascua, Rebecca Rodriguez, Yu-Xiao Yang, John Lieb, Douglas Weinstein and David E. Kaplan
Gastrointest. Disord. 2024, 6(1), 230-240; https://doi.org/10.3390/gidisord6010017 - 26 Feb 2024
Abstract
►▼
Show Figures
Venous collateral shunting of blood from the splanchnic to systemic venous systems due to portal hypertension increases the pressure in the ventral lingual venous bed. We hypothesized that the appearance of sublingual varices evaluated by pre-endoscopy/bedside visual inspection of ventrum of tongue (VIVOT)
[...] Read more.
Venous collateral shunting of blood from the splanchnic to systemic venous systems due to portal hypertension increases the pressure in the ventral lingual venous bed. We hypothesized that the appearance of sublingual varices evaluated by pre-endoscopy/bedside visual inspection of ventrum of tongue (VIVOT) might predict the presence of esophageal varices (EVs). Methods: To test this hypothesis, we prospectively enrolled patients with cirrhosis (CP) referred for EV screening for assessment of lingual vasculature after informed consent. Non-cirrhosis control patients were also enrolled. Methods: VIVOT was scored based on the presence of vessels > 2 mm and/or serpiginous veins. VIVOT scores were then correlated with endoscopic findings. Results: A total of 59 patients with cirrhosis (Group 1) were enrolled, as were 62 patients without cirrhosis (Group 2). Group 1 consisted of 100% male patients with mean age 59.5 ± 5.4 years; 39.0% were African American (AA). Group 2 consisted of 86% male patients, 59.0 ± 13 years and 53% AA. Among Group 1 patients, varices were present in 29% (16 esophageal and 3 gastric). There were no demographic differences among Group 1 patients with or without varices. Positive VIVOT scores were associated with EVs on endoscopy in 11 of 16 patients (sensitivity 68.75%). Positive VIVOT findings were present in 8 of 40 patients without EVs (specificity 80%). False-positive VIVOT scores were present in 6 of 62 non-cirrhotic controls. Overall, the positive predictive value among patients with cirrhosis was 59% with a negative predictive value of 84%. Conclusions: VIVOT has modest values in predicting EVs and should not be used alone to stratify patients for endoscopic evaluation when elastography and laboratory tests are available; however, its use in resource-limited settings to identify high-risk patients may be considered.
Full article
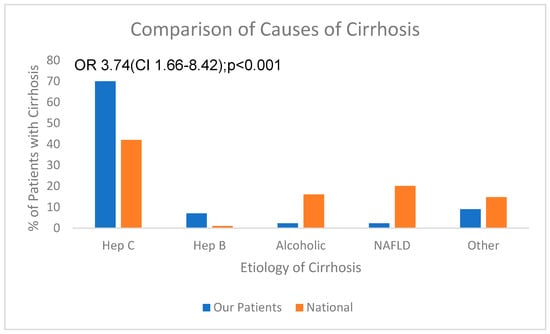
Figure 1
Open AccessReview
Diabetic Gastroparesis: Navigating Pathophysiology and Nutritional Interventions
by
Alfredo Caturano, Massimiliano Cavallo, Davide Nilo, Gaetano Vaudo, Vincenzo Russo, Raffaele Galiero, Luca Rinaldi, Raffaele Marfella, Marcellino Monda, Giovanni Luca and Ferdinando Carlo Sasso
Gastrointest. Disord. 2024, 6(1), 214-229; https://doi.org/10.3390/gidisord6010016 - 22 Feb 2024
Abstract
Diabetic gastroparesis (DGP) delays gastric emptying in diabetes patients, notably impacting those with type 1 and long-standing type 2 diabetes. Symptoms include early satiety, fullness, appetite loss, bloating, abdominal pain, and vomiting, arising from slow stomach-to-intestine food movement. DGP’s unpredictable nature complicates diagnosis
[...] Read more.
Diabetic gastroparesis (DGP) delays gastric emptying in diabetes patients, notably impacting those with type 1 and long-standing type 2 diabetes. Symptoms include early satiety, fullness, appetite loss, bloating, abdominal pain, and vomiting, arising from slow stomach-to-intestine food movement. DGP’s unpredictable nature complicates diagnosis and blood glucose management, leading to severe complications like dehydration, malnutrition, and bezoar formation. Understanding DGP’s mechanisms is crucial for effective management. Vagal dysfunction, disturbances in the interstitial cells of Cajal, reduced neural nitric oxide synthase, and increased oxidative stress contribute to the complex pathophysiology. Accurate diagnosis demands a comprehensive approach, utilizing tools like gastric scintigraphy and the Gastric Emptying Breath Test. Considering the complex relationship between DGP and glycemia, managing blood glucose levels becomes paramount. Nutritional interventions, tailored to each patient, address malnutrition risks, emphasizing smaller, more frequent meals and liquid consistency. DGP’s complex nature necessitates collaborative efforts for enhanced diagnostic strategies, improved pathophysiological understanding, and compassionate management approaches. This comprehensive approach offers hope for a future where individuals with DGP can experience improved well-being and quality of life.
Full article
(This article belongs to the Special Issue Feature Papers in Gastrointestinal Disorders in 2023-2024)
►▼
Show Figures
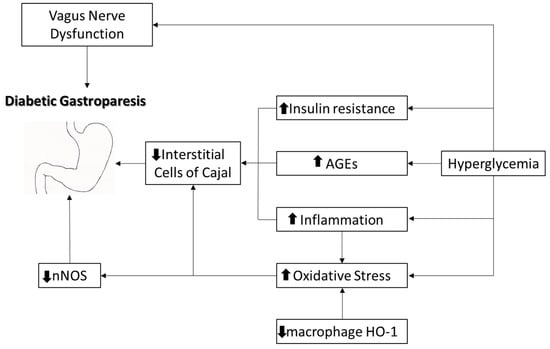
Figure 1
Open AccessArticle
An Evaluation of the Efficacy and Safety of TAMIXAM®, Based on Hyaluronic Acid and Tamarind Seed Extract, for Esophageal Mucosal Protection from Acid Insult
by
Marisa Francesca Motta, Giuseppe Pulitano, Antonino Bagnulo, Giampaolo Buriani, Umberto Di Maio, Fabio Amone, Vincenzo Nobile and Rocco Malivindi
Gastrointest. Disord. 2024, 6(1), 202-213; https://doi.org/10.3390/gidisord6010015 - 18 Feb 2024
Abstract
►▼
Show Figures
TAMIXAM® is a novel technology that combines hyaluronic acid and tamarind seed extract in its formulation. It is designed to protect the esophageal mucosa by creating a barrier through its filmogenic properties. The aim of this study is to evaluate the safety
[...] Read more.
TAMIXAM® is a novel technology that combines hyaluronic acid and tamarind seed extract in its formulation. It is designed to protect the esophageal mucosa by creating a barrier through its filmogenic properties. The aim of this study is to evaluate the safety and efficacy of this technology through mucoadhesion tests, a cell viability assay, TEER measurements, and morphological analysis on reconstructed esophageal mucosa exposed to 10% hydrochloric acid before and after treatment. The mucoadhesion test highlighted the synergistic bioadhesive effect of the technology’s components. Cell viability assays revealed the substantial mucoprotective and barrier effects of the technology, preserving tissue viability when applied before exposure to acid insult. A morphological analysis illustrated TAMIXAM®’s efficacy in countering acid-induced damage, reducing erosion, necrosis, and tissue degeneration compared to the positive control, both pre- and post-acid insult. An evaluation of epithelial integrity through TEER measurements indicated a minimal reduction in tissues treated with the invention before acid exposure, demonstrating its ability to maintain epithelial integrity in the presence of an acid insult. However, this effect was less pronounced in tissues treated with the technology after the acid insult, implying a potential partial recovery of epithelial integrity. Furthermore, comprehensive in vitro and in vivo studies supported the safety profile of the invention. In conclusion, TAMIXAM® emerged as a compelling solution, providing enhanced mechanical action to maintain epithelial balance and shield the esophageal mucosa from acid-induced damage.
Full article
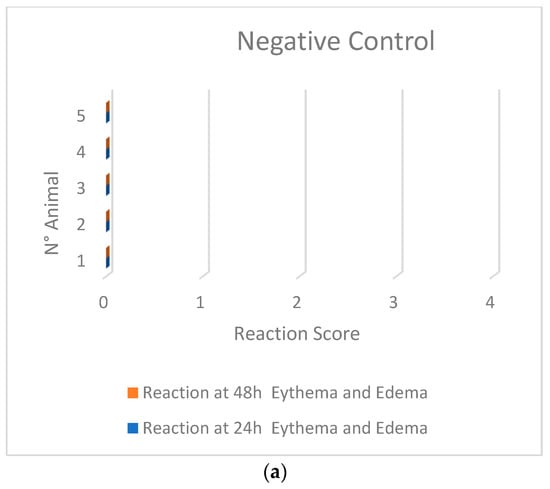
Figure 1
Open AccessArticle
Investigating the Role of Gastrointestinal-Specific Anxiety and Perceived Disability in the Adjustment to Inflammatory Bowel Disease
by
Angela Seaman and Nuno Ferreira
Gastrointest. Disord. 2024, 6(1), 191-201; https://doi.org/10.3390/gidisord6010014 - 17 Feb 2024
Abstract
►▼
Show Figures
In this study, an exploratory model was tested to investigate the mediating role of gastrointestinal-specific anxiety and perceived disability in the relation between disease activity and the outcomes of quality of life and depression in patients with inflammatory bowel disease (IBD). In a
[...] Read more.
In this study, an exploratory model was tested to investigate the mediating role of gastrointestinal-specific anxiety and perceived disability in the relation between disease activity and the outcomes of quality of life and depression in patients with inflammatory bowel disease (IBD). In a cross-sectional design, data from an online survey of patients with IBD (over the age of 16) recruited through a UK-based IBD charity were used to test a model of serial mediation. Measures targeted disease activity (self-reported), gastrointestinal-specific anxiety (Visceral Sensitivity Index), perceived disability (Perceived Disability Scale), IBD-specific quality of life (UK Inflammatory Bowel Disease Questionnaire), and depression (Depression subscale of the Depression, Anxiety, and Stress Scale). The theoretical model was investigated using model 6 of the PROCESS macro for SPSS. Bootstrapped 95% confidence intervals were constructed for each estimate A total of 320 participants provided valid responses to the survey. Gastrointestinal-specific anxiety and perceived disability were found to serially mediate the relationship between disease activity and quality of life (95%CI = −0.80 to −0.19) and disease activity and depression (95%CI = 0.13 to 0.59). Findings suggested that the effect of multiple psychosocial variables in the experience of people living with IBD and its respective outcomes should be taken into account when planning treatment. The theoretical and clinical implications of these findings are discussed.
Full article
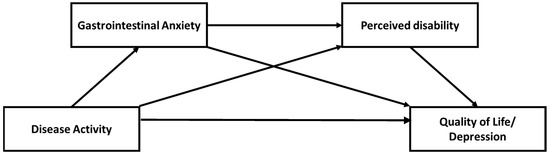
Figure 1
Open AccessReview
Metabolic Endoscopy: Should Gastroenterologists Be Treating Type 2 Diabetes?
by
Benjamin Charles Norton, Apostolis Papaefthymiou, Andrea Telese, Ritwika Mallik, Alberto Murino, Gavin Johnson, Charles Murray, Janine Makaronidis and Rehan Haidry
Gastrointest. Disord. 2024, 6(1), 180-190; https://doi.org/10.3390/gidisord6010013 - 15 Feb 2024
Abstract
Type 2 diabetes (T2D) is one of the most significant and fast-growing health challenges of the 21st century. Despite the variety of available glucose-lowering agents, many patients do not attain or maintain adequate glycaemic control. Bariatric surgery demonstrates a profound anti-diabetic effect, which
[...] Read more.
Type 2 diabetes (T2D) is one of the most significant and fast-growing health challenges of the 21st century. Despite the variety of available glucose-lowering agents, many patients do not attain or maintain adequate glycaemic control. Bariatric surgery demonstrates a profound anti-diabetic effect, which is almost immediate and weight-loss independent. The significant improvement in diabetes after bariatric surgery together with the endoscopic accessibility of the duodenum has led to the development of new metabolic endoscopic procedures that capitalise on the importance of the proximal small bowel in glycaemic control. Clinical trials have shown a clear efficacy signal, and now, several devices are undergoing evaluation as primary T2D treatments. Establishing where these procedures fit into the treatment algorithms for T2D and how they can be combined with modern pharmacotherapies is needed in a rapidly changing landscape. Ultimately, through metabolic endoscopy, gastroenterologists are on the cusp of providing safe and effective treatments for the multidisciplinary management of T2D.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomedicines, Current Oncology, Diagnostics, Gastrointestinal Disorders, JCM
Advances in Gastrointestinal and Liver Disease: From Physiological Mechanisms to Clinical Practice
Topic Editors: Davide Giuseppe Ribaldone, Gian Paolo CavigliaDeadline: 20 June 2024
Topic in
Cancers, Diagnostics, JCM, Current Oncology, Gastrointestinal Disorders, Biomedicines
Hepatobiliary and Pancreatic Diseases: Novel Strategies of Diagnosis and Treatments
Topic Editors: Alessandro Coppola, Damiano Caputo, Roberta Angelico, Domenech Asbun, Chiara MazzarelliDeadline: 20 July 2024
Topic in
Cancers, Current Oncology, Gastrointestinal Disorders, IJMS, JCM
Metastatic Colorectal Cancer: From Laboratory to Clinical Studies
Topic Editors: Ioannis Ntanasis-Stathopoulos, Diamantis I. TsilimigrasDeadline: 30 November 2024

Conferences
Special Issues
Special Issue in
Gastrointestinal Disorders
Factors Affecting Disease Activity in Children and Adults with Inflammatory Bowel Disease: An Exploration of Pro-Inflammatory and Anti-Inflammatory Elements
Guest Editors: Angharad Hurley (Vernon-Roberts), Andrew DayDeadline: 30 September 2024
Special Issue in
Gastrointestinal Disorders
Feature Papers in Gastrointestinal Disorders in 2023-2024
Guest Editor: Richard W. McCallumDeadline: 31 December 2024






