Vaccination Coverage against Tetanus, Diphtheria, Pertussis and Poliomyelitis and Validity of Self-Reported Vaccination Status in Patients with Multiple Sclerosis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Cohort
2.2. Data Acquisition
2.3. Statistics
3. Results
3.1. Sociodemographic and Clinical Data
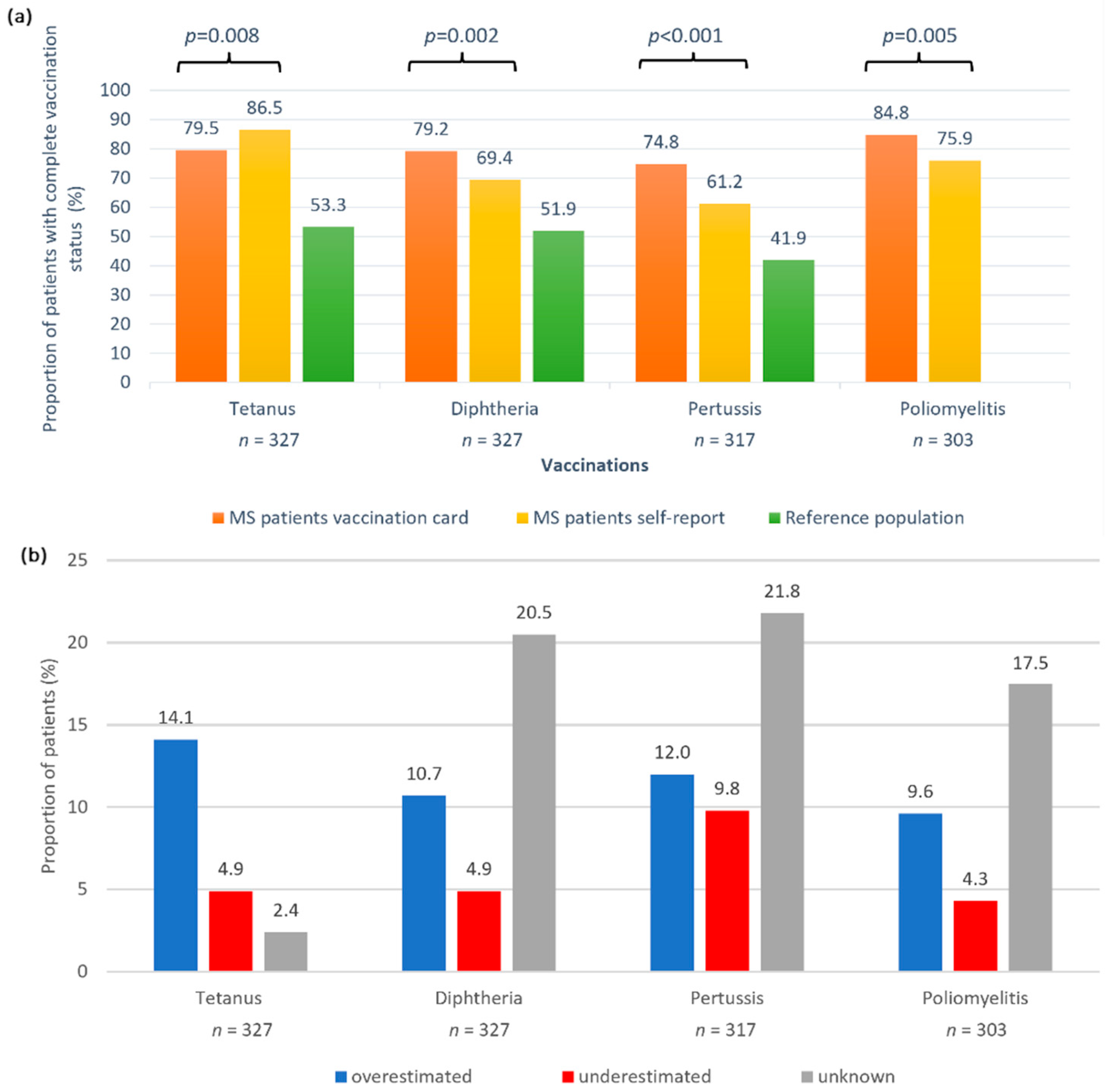
3.2. Vaccination Survey Data
3.3. Comparison between Patients with Complete and Incomplete Vaccination Status
3.4. Comparison between Patients with Correct and Incorrect Vaccination Self-Assessment
3.5. Comparison of Patients with Different Persons Who Regularly Check Their Vaccination Cards
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Filippi, M.; Bar-Or, A.; Piehl, F.; Preziosa, P.; Solari, A.; Vukusic, S.; Rocca, M.A. Multiple Sclerosis. Nat. Rev. Dis. Prim. 2018, 4, 43. [Google Scholar] [CrossRef] [PubMed]
- Reich, D.S.; Lucchinetti, C.F.; Calabresi, P.A. Multiple Sclerosis. N. Engl. J. Med. 2018, 378, 169–180. [Google Scholar] [CrossRef] [PubMed]
- Walton, C.; King, R.; Rechtman, L.; Kaye, W.; Leray, E.; Marrie, R.A.; Robertson, N.; La Rocca, N.; Uitdehaag, B.; van der Mei, I.; et al. Rising Prevalence of Multiple Sclerosis Worldwide: Insights from the Atlas of MS, Third Edition. Mult. Scler. 2020, 26, 1816–1821. [Google Scholar] [CrossRef] [PubMed]
- Leray, E.; Moreau, T.; Fromont, A.; Edan, G. Epidemiology of Multiple Sclerosis. Rev. Neurol. 2016, 172, 3–13. [Google Scholar] [CrossRef]
- Gilmour, H. Multiple Sclerosis: Prevalence and Impact. Health Rep. 2018, 29, 3–8. [Google Scholar]
- Ohle, L.-M.; Ellenberger, D.; Flachenecker, P.; Friede, T.; Haas, J.; Hellwig, K.; Parciak, T.; Warnke, C.; Paul, F.; Zettl, U.K.; et al. Chances and Challenges of a Long-Term Data Repository in Multiple Sclerosis: 20th Birthday of the German MS Registry. Sci. Rep. 2021, 11, 13340. [Google Scholar] [CrossRef]
- Ascherio, A.; Munger, K. Epidemiology of Multiple Sclerosis: From Risk Factors to Prevention—An Update. Semin. Neurol. 2016, 36, 103–114. [Google Scholar] [CrossRef]
- Sospedra, M.; Martin, R. Immunology of Multiple Sclerosis. Semin. Neurol. 2016, 36, 115–127. [Google Scholar] [CrossRef]
- Hecker, M.; Bühring, J.; Fitzner, B.; Rommer, P.S.; Zettl, U.K. Genetic, Environmental and Lifestyle Determinants of Accelerated Telomere Attrition as Contributors to Risk and Severity of Multiple Sclerosis. Biomolecules 2021, 11, 1510. [Google Scholar] [CrossRef]
- Bjornevik, K.; Cortese, M.; Healy, B.C.; Kuhle, J.; Mina, M.J.; Leng, Y.; Elledge, S.J.; Niebuhr, D.W.; Scher, A.I.; Munger, K.L.; et al. Longitudinal Analysis Reveals High Prevalence of Epstein-Barr Virus Associated with Multiple Sclerosis. Science 2022, 375, 296–301. [Google Scholar] [CrossRef]
- Rommer, P.S.; Eichstädt, K.; Ellenberger, D.; Flachenecker, P.; Friede, T.; Haas, J.; Kleinschnitz, C.; Pöhlau, D.; Rienhoff, O.; Stahmann, A.; et al. Symptomatology and Symptomatic Treatment in Multiple Sclerosis: Results from a Nationwide MS Registry. Mult. Scler. 2019, 25, 1641–1652. [Google Scholar] [CrossRef] [PubMed]
- Klineova, S.; Lublin, F.D. Clinical Course of Multiple Sclerosis. Cold Spring Harb. Perspect. Med. 2018, 8, a028928. [Google Scholar] [CrossRef] [PubMed]
- Thompson, A.J.; Banwell, B.L.; Barkhof, F.; Carroll, W.M.; Coetzee, T.; Comi, G.; Correale, J.; Fazekas, F.; Filippi, M.; Freedman, M.S.; et al. Diagnosis of Multiple Sclerosis: 2017 Revisions of the McDonald Criteria. Lancet Neurol. 2018, 17, 162–173. [Google Scholar] [CrossRef]
- Hauser, S.L.; Cree, B.A.C. Treatment of Multiple Sclerosis: A Review. Am. J. Med. 2020, 133, 1380–1390.e2. [Google Scholar] [CrossRef] [PubMed]
- Gholamzad, M.; Ebtekar, M.; Ardestani, M.S.; Azimi, M.; Mahmodi, Z.; Mousavi, M.J.; Aslani, S. A Comprehensive Review on the Treatment Approaches of Multiple Sclerosis: Currently and in the Future. Inflamm. Res. 2019, 68, 25–38. [Google Scholar] [CrossRef]
- Rommer, P.; Zettl, U.K. Treatment Options in Multiple Sclerosis and Neuromyelitis Optica Spectrum Disorders. Curr. Pharm. Des. 2022, 28, 428–436. [Google Scholar] [CrossRef]
- Winkelmann, A.; Loebermann, M.; Reisinger, E.C.; Hartung, H.-P.; Zettl, U.K. Disease-Modifying Therapies and Infectious Risks in Multiple Sclerosis. Nat. Rev. Neurol. 2016, 12, 217–233. [Google Scholar] [CrossRef]
- Marrodan, M.; Alessandro, L.; Farez, M.F.; Correale, J. The Role of Infections in Multiple Sclerosis. Mult. Scler. 2019, 25, 891–901. [Google Scholar] [CrossRef]
- Venkatesan, A.; Johnson, R.T. Infections and Multiple Sclerosis. Handb. Clin. Neurol. 2014, 122, 151–171. [Google Scholar] [CrossRef]
- Rommer, P.S.; Zettl, U.K. Managing the Side Effects of Multiple Sclerosis Therapy: Pharmacotherapy Options for Patients. Expert Opin. Pharmacother. 2018, 19, 483–498. [Google Scholar] [CrossRef]
- Correale, J.; Fiol, M.; Gilmore, W. The Risk of Relapses in Multiple Sclerosis during Systemic Infections. Neurology 2006, 67, 652–659. [Google Scholar] [CrossRef] [PubMed]
- Vollmer, T. The Natural History of Relapses in Multiple Sclerosis. J. Neurol. Sci. 2007, 256, S5–S13. [Google Scholar] [CrossRef] [PubMed]
- Kurtzke, J.F. Rating Neurologic Impairment in Multiple Sclerosis: An Expanded Disability Status Scale (EDSS). Neurology 1983, 33, 1444–1452. [Google Scholar] [CrossRef] [Green Version]
- Buljevac, D.; Flach, H.Z.; Hop, W.C.J.; Hijdra, D.; Laman, J.D.; Savelkoul, H.F.J.; van der Meché, F.G.A.; van Doorn, P.A.; Hintzen, R.Q. Prospective Study on the Relationship between Infections and Multiple Sclerosis Exacerbations. Brain 2002, 125, 952–960. [Google Scholar] [CrossRef] [PubMed]
- Montgomery, S.; Hillert, J.; Bahmanyar, S. Hospital Admission Due to Infections in Multiple Sclerosis Patients. Eur. J. Neurol. 2013, 20, 1153–1160. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nelson, R.E.; Xie, Y.; DuVall, S.L.; Butler, J.; Kamauu, A.W.C.; Knippenberg, K.; Schuerch, M.; Foskett, N.; LaFleur, J. Multiple Sclerosis and Risk of Infection-Related Hospitalization and Death in US Veterans. Int. J. MS Care 2015, 17, 221–230. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Loebermann, M.; Winkelmann, A.; Hartung, H.-P.; Hengel, H.; Reisinger, E.C.; Zettl, U.K. Vaccination against Infection in Patients with Multiple Sclerosis. Nat. Rev. Neurol. 2012, 8, 143–151. [Google Scholar] [CrossRef] [PubMed]
- Hapfelmeier, A.; Gasperi, C.; Donnachie, E.; Hemmer, B. A Large Case-Control Study on Vaccination as Risk Factor for Multiple Sclerosis. Neurology 2019, 93, e908–e916. [Google Scholar] [CrossRef]
- Mailand, M.T.; Frederiksen, J.L. Vaccines and Multiple Sclerosis: A Systematic Review. J. Neurol. 2017, 264, 1035–1050. [Google Scholar] [CrossRef]
- Zrzavy, T.; Kollaritsch, H.; Rommer, P.S.; Boxberger, N.; Loebermann, M.; Wimmer, I.; Winkelmann, A.; Zettl, U.K. Vaccination in Multiple Sclerosis: Friend or Foe? Front. Immunol. 2019, 10, 1883. [Google Scholar] [CrossRef]
- Kennedy, J. Vaccine Hesitancy: A Growing Concern. Pediatr. Drugs 2020, 22, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Heidler, F.; Baldt, J.; Frahm, N.; Langhorst, S.E.; Mashhadiakbar, P.; Streckenbach, B.; Zettl, U.K.; Richter, J. Vaccination Setting of Patients with Autoimmune Diseases in Times of Severe Acute Respiratory Syndrome Coronavirus Type 2 Pandemic Using the Example of Multiple Sclerosis Patients: A Longitudinal Multicenter Study. Eur. Neurol. 2022, 85, 104–111. [Google Scholar] [CrossRef] [PubMed]
- Paul-Ehrlich-Institut-Tetanus-Impfstoffe (Wundstarrkrampf). Available online: https://www.pei.de/DE/arzneimittel/impfstoffe/tetanus-wundstarrkrampf/tetanus-node.html (accessed on 7 April 2021).
- Rieck, T.; Steffen, A.; Schmid-Küpke, N.; Feig, M.; Wichmann, O.; Siedler, A. Impfquoten bei Erwachsenen in Deutschland-Aktuelles aus der KV-Impfsurveillance und der Onlinebefragungn von Krankenhauspersonal OKaPII. Epidemiol. Bull. 2020, 47, 24. [Google Scholar]
- Laroni, A.; Signori, A.; Maniscalco, G.T.; Lanzillo, R.; Russo, C.V.; Binello, E.; Lo Fermo, S.; Repice, A.; Annovazzi, P.; Bonavita, S.; et al. Assessing Association of Comorbidities with Treatment Choice and Persistence in MS: A Real-Life Multicenter Study. Neurology 2017, 89, 2222–2229. [Google Scholar] [CrossRef] [PubMed]
- Marrie, R.A.; Miller, A.; Sormani, M.P.; Thompson, A.; Waubant, E.; Trojano, M.; O’Connor, P.; Fiest, K.; Reider, N.; Reingold, S.; et al. Recommendations for Observational Studies of Comorbidity in Multiple Sclerosis. Neurology 2016, 86, 1446–1453. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- German Standing Committee on Vaccination. Empfehlungen der Standigen Impfkommission (STIKO) am Robert Koch-Institut 2020/2021. Epidemiol. Bull. 2020, 34, 1–68. [Google Scholar]
- Benjamini, Y.; Hochberg, Y. Controlling the False Discovery Rate: A Practical and Powerful Approach to Multiple Testing. J. R. Stat. Soc. Ser. B Methodol. 1995, 57, 289–300. [Google Scholar] [CrossRef]
- Monschein, T.; Hartung, H.-P.; Zrzavy, T.; Barnett, M.; Boxberger, N.; Berger, T.; Chataway, J.; Bar-Or, A.; Rommer, P.S.; Zettl, U.K. Vaccination and Multiple Sclerosis in the Era of the COVID-19 Pandemic. J. Neurol. Neurosurg. Psychiatry 2021, 92, 1033–1043. [Google Scholar] [CrossRef]
- Wagner, N.; Assmus, F.; Arendt, G.; Baum, E.; Baumann, U.; Bogdan, C.; Burchard, G.; Föll, D.; Garbe, E.; Hecht, J.; et al. Impfen bei Immundefizienz: Anwendungshinweise zu den von der Ständigen Impfkommission empfohlenen Impfungen. (IV) Impfen bei Autoimmunkrankheiten, bei anderen chronisch-entzündlichen Erkrankungen und unter immunmodulatorischer Therapie. Bundesgesundheitsblatt-Gesundh.-Gesundh. 2019, 62, 494–515. [Google Scholar] [CrossRef] [Green Version]
- Grebenciucova, E.; Pruitt, A. Infections in Patients Receiving Multiple Sclerosis Disease-Modifying Therapies. Curr. Neurol. Neurosci. Rep. 2017, 17, 88. [Google Scholar] [CrossRef]
- Moiola, L.; Rommer, P.S.; Zettl, U.K. Prevention and Management of Adverse Effects of Disease Modifying Treatments in Multiple Sclerosis. Curr. Opin. Neurol. 2020, 33, 286–294. [Google Scholar] [CrossRef] [PubMed]
- Flachenecker, P.; Eichstädt, K.; Berger, K.; Ellenberger, D.; Friede, T.; Haas, J.; Kleinschnitz, C.; Pöhlau, D.; Rienhoff, O.; Stahmann, A.; et al. Multiple sclerosis in Germany: Updated analysis of the German MS Registry 2014–2018. Fortschr. Neurol. Psychiatr. 2020, 88, 436–450. [Google Scholar] [CrossRef] [PubMed]
- German Standing Committee on Vaccination. Empfehlungen der Ständigen Impfkommission (STIKO) am Robert Koch-Institut Juli 2009. Epidemiol. Bull. 2009, 31, 299–311. [Google Scholar]
- Marshall, G.S.; Happe, L.E.; Lunacsek, O.E.; Szymanski, M.D.; Woods, C.R.; Zahn, M.; Russell, A. Use of Combination Vaccines Is Associated With Improved Coverage Rates. Pediatr. Infect. Dis. J. 2007, 26, 496–500. [Google Scholar] [CrossRef]
- Poethko-Müller, C.; Schmitz, R. Impfstatus von Erwachsenen in Deutschland: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundheitsblatt-Gesundh.-Gesundh. 2013, 56, 845–857. [Google Scholar] [CrossRef]
- Böhmer, M.M.; Walter, D.; Krause, G.; Müters, S.; Gößwald, A.; Wichmann, O. Determinants of Tetanus and Seasonal Influenza Vaccine Uptake in Adults Living in Germany. Hum. Vaccin. 2011, 7, 1317–1325. [Google Scholar] [CrossRef] [Green Version]
- Bödeker, B.; Remschmidt, C.; Müters, S.; Wichmann, O. Impfquoten unter Erwachsenen in Deutschland für die Impfungen gegen saisonale Influenza, Tetanus und Pertussis. Bundesgesundheitsblatt-Gesundh.-Gesundh. 2015, 58, 174–182. [Google Scholar] [CrossRef] [Green Version]
- Chehab, G.; Richter, J.G.; Brinks, R.; Fischer-Betz, R.; Winkler-Rohlfing, B.; Schneider, M. Vaccination Coverage in Systemic Lupus Erythematosus—a Cross-Sectional Analysis of the German Long-Term Study (LuLa Cohort). Rheumatology 2018, 57, 1439–1447. [Google Scholar] [CrossRef] [Green Version]
- Jacques, M.; Letaief, H.; Philippe, G.; Xavier, M.; Bernard, C.; Lukas, C. Low Influenza, Pneumococcal and Diphtheria–Tetanus–Poliomyelitis Vaccine Coverage in Patients with Primary Sjögren’s Syndrome: A Cross-Sectional Study. Vaccines 2019, 8, 3. [Google Scholar] [CrossRef] [Green Version]
- Krasselt, M.; Baerwald, C.; Seifert, O. Insufficient Vaccination Rates in Patients with Systemic Lupus Erythematosus in a German Outpatient Clinic. Z. Rheumatol. 2018, 77, 727–734. [Google Scholar] [CrossRef]
- Krasselt, M.; Ivanov, J.-P.; Baerwald, C.; Seifert, O. Low Vaccination Rates among Patients with Rheumatoid Arthritis in a German Outpatient Clinic. Rheumatol. Int. 2017, 37, 229–237. [Google Scholar] [CrossRef] [PubMed]
- Malhi, G.; Rumman, A.; Thanabalan, R.; Croitoru, K.; Silverberg, M.S.; Hillary Steinhart, A.; Nguyen, G.C. Vaccination in Inflammatory Bowel Disease Patients: Attitudes, Knowledge, and Uptake. J. Crohn’s Colitis 2015, 9, 439–444. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Teich, N.; Klugmann, T.; Tiedemann, A.; Holler, B.; Mössner, J.; Liebetrau, A.; Schiefke, I. Vaccination Coverage in Immunosuppressed Patients. Dtsch. Arztebl. Int. 2011, 108, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Reiter, S.; Poethko-Müller, C. Aktuelle Entwicklung von Impfquoten und Impflücken bei Kindern und Jugendlichen in Deutschland. Bundesgesundheitsblatt-Gesundh.-Gesundh. 2009, 52, 1037–1044. [Google Scholar] [CrossRef] [Green Version]
- Confavreux, C.; Suissa, S.; Saddier, P.; Bourdès, V.; Vukusic, S. Vaccinations and the Risk of Relapse in Multiple Sclerosis. N. Engl. J. Med. 2001, 344, 319–326. [Google Scholar] [CrossRef]
- DeStefano, F. Vaccinations and Risk of Central Nervous System Demyelinating Diseases in Adults. Arch. Neurol. 2003, 60, 504–509. [Google Scholar] [CrossRef] [Green Version]
- Farez, M.F.; Correale, J. Immunizations and Risk of Multiple Sclerosis: Systematic Review and Meta-Analysis. J. Neurol. 2011, 258, 1197–1206. [Google Scholar] [CrossRef]
- Poethko-Müller, C.; Ellert, U.; Kuhnert, R.; Neuhauser, H.; Schlaud, M.; Schenk, L. Vaccination Coverage against Measles in German-Born and Foreign-Born Children and Identification of Unvaccinated Subgroups in Germany. Vaccine 2009, 27, 2563–2569. [Google Scholar] [CrossRef]
- Guthmann, J.-P.; Fonteneau, L.; Antona, D.; Lévy-Bruhl, D. Déterminants de couverture vaccinale antitétanique chez l’adulte en France et de connaissance du statut vaccinal. Méd. Mal. Infect. 2010, 40, 560–567. [Google Scholar] [CrossRef]
- Hamidi, A.A.; Taş, B.G.; Gündüz, A.; Çelebi, S.N.; Esen, E.S.; Toprak, D.; Dökmetaş, İ. Immunization Rates of Pneumococcal, Influenza and Tetanus Vaccines and Knowledge and Attitudes of Adult Patients Who Receive Inpatient Treatment at Hospital: Point Prevalence Study. Hum. Vaccines Immunother. 2018, 14, 2649–2653. [Google Scholar] [CrossRef]
- Ciotti, J.R.; Valtcheva, M.V.; Cross, A.H. Effects of MS Disease-Modifying Therapies on Responses to Vaccinations: A Review. Mult. Scler. Relat. Disord. 2020, 45, 102439. [Google Scholar] [CrossRef] [PubMed]
- Winkelmann, A.; Loebermann, M.; Barnett, M.; Hartung, H.-P.; Zettl, U.K. Vaccination and Immunotherapies in Neuroimmunological Diseases. Nat. Rev. Neurol. 2022, 2022, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Fiks, A.G.; Grundmeier, R.W.; Biggs, L.M.; Localio, A.R.; Alessandrini, E.A. Impact of Clinical Alerts Within an Electronic Health Record on Routine Childhood Immunization in an Urban Pediatric Population. Pediatrics 2007, 120, 707–714. [Google Scholar] [CrossRef]
- Akmatov, M.K.; Rübsamen, N.; Deyneko, I.V.; Karch, A.; Mikolajczyk, R.T. Poor Knowledge of Vaccination Recommendations and Negative Attitudes towards Vaccinations Are Independently Associated with Poor Vaccination Uptake among Adults-Findings of a Population-Based Panel Study in Lower Saxony, Germany. Vaccine 2018, 10, 2417–2426. [Google Scholar] [CrossRef] [PubMed]
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J.A. Vaccine Hesitancy. Hum. Vaccines Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef] [PubMed]
- Auffret, Y.; Rousseaux, J.Y.; Gatineau, F.; Hamoniaux, F.; Gouillou, M.; Abalea Le Dreff, L.; Pina Silas, S.; Rakatobe, F.; Alavi, Z. Should We Believe Emergency Department Patients Self-Reported Tetanus Vaccine Status? Am. J. Emerg. Med. 2019, 37, 983–990. [Google Scholar] [CrossRef]
- Rolnick, S.J.; Parker, E.D.; Nordin, J.D.; Hedblom, B.D.; Wei, F.; Kerby, T.; Jackson, J.M.; Crain, A.L.; Euler, G. Self-Report Compared to Electronic Medical Record across Eight Adult Vaccines: Do Results Vary by Demographic Factors? Vaccine 2013, 31, 3928–3935. [Google Scholar] [CrossRef] [Green Version]
- Lu, P.; O’Halloran, A.; Kennedy, E.D.; Williams, W.W.; Kim, D.; Fiebelkorn, A.P.; Donahue, S.; Bridges, C.B. Awareness among Adults of Vaccine-Preventable Diseases and Recommended Vaccinations, United States, 2015. Vaccine 2017, 35, 3104–3115. [Google Scholar] [CrossRef] [Green Version]
- Cook, T.M.; Protheroe, R.T.; Handel, J.M. Tetanus: A Review of the Literature. Br. J. Anaesth. 2001, 87, 477–487. [Google Scholar] [CrossRef] [Green Version]
- Loulergue, P.; Pulcini, C.; Massin, S.; Bernhard, M.; Fonteneau, L.; Levy-Brühl, D.; Guthmann, J.-P.; Launay, O. Validity of Self-Reported Vaccination Status among French Healthcare Students. Clin. Microbiol. Infect. 2014, 20, O1152–O1154. [Google Scholar] [CrossRef] [Green Version]
- van der Heide, I.; Wang, J.; Droomers, M.; Spreeuwenberg, P.; Rademakers, J.; Uiters, E. The Relationship Between Health, Education, and Health Literacy: Results From the Dutch Adult Literacy and Life Skills Survey. J. Health Commun. 2013, 18, 172–184. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Keil, J.; Brendler, V.; Sachse, C.; Zülke, A.; Zeynalova, S.; Engel, C.; Loeffler, M.; Riedel-Heller, S.G.; König, H.-H.; Stengler, K. Geschlechterspezifische Inanspruchnahme von Gesundheitsleistungen in einer urbanen Erwachsenenpopulation. Gesundheitswesen 2020, 82, e17–e23. [Google Scholar] [CrossRef] [PubMed]



| Vaccination | RKI Recommendations 2020/21 | ||
|---|---|---|---|
| Childhood Basic Immunization | Childhood Booster Immunization | Adult Immunization | |
| Tetanus | Three vaccinations at 2, 4 and 11 months of age | At 5–6 years and 9–16 years of age | All persons in case of missing or incomplete basic immunization or if the last basic immunization or the last booster vaccination is longer than 10 years ago |
| Diphtheria | Three vaccinations at 2, 4 and 11 months of age | At 5–6 years and 9–16 years of age | All persons in case of missing or incomplete basic immunization or if the last basic immunization or the last booster vaccination is longer than 10 years ago |
| Pertussis | Three vaccinations at 2, 4 and 11 months of age | At 5–6 years and 9–16 years of age | It is recommended that the next Td vaccinations given as a single Tdap combination vaccination |
| Poliomyelitis | Three vaccinations at 2, 4 and 11 months of age | Between the ages of 9–16 years | All persons with missing or incomplete basic immunization and all persons without a booster vaccination |
| n (%) | Range | Mean (SD) | Median | |
|---|---|---|---|---|
| Sex | ||||
| Female | 225 (68.8) | |||
| Male | 102 (31.2) | |||
| Age (years) | 19–80 | 47.3 (13.1) | 49.0 | |
| Place of residence | ||||
| Rural area | 133 (40.7) | |||
| Small town | 49 (15.0) | |||
| Medium-sized town | 61 (18.7) | |||
| City | 84 (25.7) | |||
| Partnership | ||||
| Single | 61 (18.7) | |||
| In a relationship | 65 (19.9) | |||
| Married | 181 (55.4) | |||
| Divorced | 12 (3.7) | |||
| Widowed | 8 (2.4) | |||
| Number of children | 0–4 | 1.2 (0.9) | 1.0 | |
| 0 | 91 (27.8) | |||
| 1 | 88 (26.9) | |||
| 2 | 130 (39.8) | |||
| 3 | 15 (4.6) | |||
| 4 | 3 (0.9) | |||
| Number of siblings | 0–9 | 1.5 (1.1) | 1.0 | |
| 0 | 32 (9.8) | |||
| 1 | 169 (51.7) | |||
| ≥2 | 126 (38.5) | |||
| School years | 8–18 | 10.6 (1.3) | 10.0 | |
| Educational level | ||||
| No training | 11 (3.4) | |||
| Skilled worker | 198 (60.6) | |||
| Technical college | 59 (18.0) | |||
| University | 59 (18.0) | |||
| Employment status | ||||
| Training/student | 5 (1.5) | |||
| Fulltime employed | 94 (28.7) | |||
| Part-time employed | 74 (22.6) | |||
| Unemployed | 13 (4.0) | |||
| Disability pension | 105 (32.1) | |||
| Retirement pension | 29 (8.9) | |||
| Other | 7 (2.1) | |||
| Patient care | ||||
| Outpatients | 258 (78.9) | |||
| Inpatients | 69 (21.1) | |||
| Course of disease | ||||
| CIS | 16 (4.9) | |||
| RRMS | 221 (67.6) | |||
| SPMS | 63 (19.3) | |||
| PPMS | 27 (8.3) | |||
| Disease duration (years) | 0–41 | 11.6 (8.6) | 10.0 | |
| EDSS score | 0–8.0 | 3.3 (2.1) | 3.0 | |
| DMD treatment | ||||
| Yes | 258 (78.9) | |||
| No | 69 (21.1) | |||
| Comorbidities | ||||
| Yes | 244 (74.6) | |||
| No | 83 (25.4) |
| Tetanus (n = 327) | Diphtheria (n = 327) | Pertussis (n = 317) | Polio (n = 303) | |||||
|---|---|---|---|---|---|---|---|---|
| Complete vs. Incomplete | p-Value | Complete vs. Incomplete | p-Value | Complete vs. Incomplete | p-Value | Complete vs. Incomplete | p-Value | |
| n | 260 vs. 67 | 259 vs. 68 | 237 vs. 80 | 257 vs. 46 | ||||
| Sex c | 0.077 Fi | 0.056 Fi | 0.069 Fi | 0.302 Fi | ||||
| Female | 185 (71.2) vs. 40 (59.7) | 185 (71.4) vs. 40 (58.8) | 170 (71.7) vs. 48 (60.0) | 179 (69.7) vs. 28 (60.9) | ||||
| Male | 75 (28.8) vs. 27 (40.3) | 74 (28.6) vs. 28 (41.2) | 67 (28.3) vs. 32 (40.0) | 78 (30.3) vs. 18 (39.1) | ||||
| Age (years) a | 47.7 (12.9) vs. 45.9 (13.8) | 0.325 t | 47.7 (12.9) vs. 45.9 (13.7) | 0.306 t | 47.8 (12.9) vs. 45.2 (13.5) | 0.127 t | 46.7 (12.7) vs. 49.2 (14.3) | 0.213 t |
| Place of residence c | 0.284 Chi | 0.322 Chi | 0.135 Chi | 0.010Chi | ||||
| Rural area | 109 (41.9) vs. 24 (35.8) | 108 (41.7) vs. 25 (36.8) | 102 (43.0) vs. 27 (33.8) | 112 (43.6) vs. 15 (32.6) | ||||
| Small town | 34 (13.1) vs. 15 (22.4) | 34 (13.1) vs. 15 (22.0) | 29 (12.2) vs. 18 (22.5) | 33 (12.8) vs. 13 (28.3) | ||||
| Medium-sized town | 50 (19.2) vs. 11 (16.4) | 50 (19.3) vs. 11 (16.2) | 44 (18.6) vs. 14 (17.5) | 40 (15.6) vs. 11 (23.9) | ||||
| City | 67 (25.8) vs. 17 (25.4) | 67 (25.9) vs. 17 (25.0) | 62 (26.2) vs. 21 (26.2) | 72 (28.0) vs. 7 (15.2) | ||||
| Partnership c | 0.872 Chi | 0.773 Chi | 0.898 Chi | 0.143 Chi | ||||
| Single | 48 (18.5) vs. 13 (19.4) | 48 (18.5) vs. 13 (19.1) | 43 (18.1) vs. 17 (21.3) | 48 (18.7) vs. 11 (23.9) | ||||
| In a relationship | 49 (18.8) vs. 16 (23.9) | 48 (18.5) vs. 17 (25.0) | 46 (19.4) vs. 18 (22.5) | 56 (21.8) vs. 6 (13.0) | ||||
| Married | 147 (56.5) vs. 34 (50.7) | 147 (56.8) vs. 34 (50.0) | 134 (56.5) vs. 40 (50.0) | 140 (54.5) vs. 24 (52.2) | ||||
| Divorced | 10 (3.8) vs. 2 (3.0) | 10 (3.9) vs. 2 (2.9) | 8 (3.4) vs. 3 (3.7) | 6 (2.3) vs. 4 (8.7) | ||||
| Widowed | 6 (2.3) vs. 2 (3.0) | 6 (2.3) vs. 2 (2.9) | 6 (2.5) vs. 2 (2.5) | 7 (2.7) vs. 1 (2.2) | ||||
| Number of children a | 1.3 (0.9) vs. 1.2 (0.9) | 0.479 t | 1.3 (0.9) vs. 1.2 (0.9) | 0.542 t | 1.3 (0.9) vs. 1.1 (0.9) | 0.248 t | 1.2 (0.9) vs. 1.2 (1.0) | 0.644 t |
| Number of siblings a | 1.6 (1.2) vs. 1.2 (0.8) | 0.008 *,t | 1.6 (1.2) vs. 1.2 (0.8) | 0.007 *,t | 1.6 (1.1) vs. 1.3 (1.1) | 0.083 t | 1.4 (1.0) vs. 1.7 (1.1) | 0.159 t |
| School years a | 10.6 (1.3) vs. 10.6 (1.2) | 0.959 t | 10.6 (1.3) vs. 10.6 (1.2) | 0.992 t | 10.6 (1.3) vs. 10.7 (1.3) | 0.270 t | 10.7 (1.3) vs. 10.3 (1.1) | 0.090 t |
| Educational level c | 0.826 Chi | 0.813 Chi | 0.131 Chi | 0.160 Chi | ||||
| No training | 8 (3.1) vs. 3 (4.5) | 8 (3.1) vs. 3 (4.4) | 7 (2.9) vs. 4 (5.0) | 5 (2.0) vs. 3 (6.5) | ||||
| Skilled worker | 160 (61.5) vs. 38 (56.7) | 160 (61.8) vs. 38 (55.9) | 148 (62.5) vs. 40 (50.0) | 153 (59.5) vs. 28 (60.9) | ||||
| Technical college | 47 (18.1) vs. 12 (17.9) | 46 (17.8) vs. 13 (19.1) | 44 (18.6) vs. 15 (18.7) | 47 (18.3) vs. 10 (21.7) | ||||
| University | 45 (17.3) vs. 14 (20.9) | 45 (17.4) vs. 14 (25.6) | 38 (16.0) vs. 21 (26.3) | 52 (20.2) vs. 5 (10.9) | ||||
| Employment status c | 0.796 Chi | 0.782 Chi | 0.911 Chi | 0.646 Chi | ||||
| Training/student | 4 (1.5) vs. 1 (1.5) | 4 (1.5) vs. 1 (1.5) | 3 (1.3) vs. 2 (2.5) | 4 (1.6) vs. 1 (2.2) | ||||
| Full time employed | 74 (28.5) vs. 20 (29.8) | 73 (28.2) vs. 21 (30.9) | 70 (29.5) vs. 23 (28.7) | 82 (31.9) vs. 9 (19.5) | ||||
| Part timer employed | 59 (22.7) vs. 15 (22.4) | 59 (22.8) vs. 15 (22.1) | 55 (23.2) vs. 18 (22.5) | 59 (22.9) vs. 11 (23.9) | ||||
| Unemployed | 8 (3.1) vs. 5 (7.5) | 8 (3.1) vs. 5 (7.3) | 8 (3.4) vs. 5 (6.3) | 11 (4.3) vs. 1 (2.2) | ||||
| Disability pension | 85 (32.7) vs. 20 (29.8) | 85 (32.8) vs. 20 (29.4) | 74 (31.2) vs. 24 (30.0) | 74 (28.8) vs. 18 (39.1) | ||||
| Retirement pension | 24 (9.2) vs. 5 (7.5) | 24 (9.3) vs. 5 (7.3) | 22 (9.3) vs. 6 (7.5) | 21 (8.2) vs. 5 (10.9) | ||||
| Other | 6 (2.3) vs. 1 (1.5) | 6 (2.3) vs. 1 (1.5) | 5 (2.1) vs. 2 (2.5) | 6 (2.3) vs. 1 (2.2) | ||||
| Patient care c | 0.507 Fi | 0.617 Fi | 0.160 Fi | 0.243 Fi | ||||
| Outpatients | 207 (79.6) vs. 51 (76.1) | 206 (79.5) vs. 52 (76.5) | 190 (80.2) vs. 58 (72.5) | 205 (79.8) vs. 33 (71.7) | ||||
| Inpatients | 53 (20.4) vs. 16 (23.9) | 53 (20.5) vs. 16 (23.5) | 47 (19.8) vs. 22 (37.5) | 52 (20.2) vs. 13 (28.3) | ||||
| Course of disease c | 0.588 Chi | 0.311 Chi | 0.422 Chi | 0.013 Chi | ||||
| CIS | 11 (4.2) vs. 5 (7.5) | 10 (3.9) vs. 6 (8.8) | 10 (4.2) vs. 6 (7.5) | 12 (4.7) vs. 4 (8.7) | ||||
| RRMS | 179 (68.8) vs. 42 (62.7) | 179 (69.1) vs. 42 (61.8) | 167 (70.5) vs. 49 (61.3) | 185 (72.0) vs. 22 (47.8) | ||||
| SPMS | 48 (18.5) vs. 15 (22.3) | 48 (18.5) vs. 15 (22.1) | 41 (17.3) vs. 17 (21.2) | 42 (16.3) vs. 13 (28.3) | ||||
| PPMS | 22 (8.5) vs. 5 (7.5) | 22 (8.5) vs. 5 (7.3) | 19 (8.0) vs. 8 (10.0) | 18 (7.0) vs. 7 (15.2) | ||||
| Disease duration (years) b | 10.0 vs. 8.0 | 0.096 U | 12.0 vs. 9.8 | 0.059 U | 10.0 vs. 7.5 | 0.050 U | 10.0 vs. 9.0 | 0.468 U |
| EDSS score b | 3.0 vs. 2.5 | 0.550 U | 3.0 vs. 2.5 | 0.416 U | 3.0 vs. 3.0 | 0.641 U | 3.0 vs. 3.5 | 0.331 U |
| DMD treatment c | 1.000 Fi | 0.868 Fi | 0.875 Fi | 0.847 Fi | ||||
| Yes | 205 (78.9) vs. 53 (79.1) | 205 (79.1) vs. 53 (77.9) | 185 (78.1) vs. 64 (80.0) | 200 (77.8) vs. 36 (78.3) | ||||
| No | 55 (21.1) vs. 14 (20.9) | 54 (20.9) vs. 15 (22.1) | 52 (21.9) vs. 16 (20.0) | 57 (22.2) vs. 10 (21.7) | ||||
| Comorbidities c | 0.532 Fi | 0.639 Fi | 0.140 Fi | 0.720 Fi | ||||
| Yes | 196 (75.4) vs. 48 (71.6) | 195 (75.3) vs. 49 (72.1) | 181 (76.4) vs. 54 (67.5) | 187 (72.8) vs. 35 (76.1) | ||||
| No | 64 (24.6) vs. 19 (28.4) | 64 (24.7) vs. 19 (27.9) | 56 (23.6) vs. 26 (32.5) | 70 (27.2) vs. 11 (23.9) | ||||
| Nobody | Family Doctor/ Neurologist | Others | p-Value | |
|---|---|---|---|---|
| n | 56 (17.1%) | 238 (72.8%) | 33 (10.1%) | |
| Sex c | 0.037 Chi | |||
| Female | 31 (55.4) | 168 (70.6) | 26 (78.8) | |
| Male | 25 (44.6) | 70 (29.4) | 7 (21.2) | |
| Age (years) a | 44.8 (13.3) | 47.9 (13.2) | 48.0 (11.5) | 0.270 ANOVA |
| Place of residence c | 0.136 Chi | |||
| Rural area | 25 (44.6) | 91 (38.2) | 17 (51.5) | |
| Small town | 6 (10.7) | 41 (17.2) | 2 (6.1) | |
| Medium-sized town | 13 (23.2) | 39 (16.4) | 9 (27.3) | |
| City | 12 (21.4) | 67 (28.1) | 5 (15.1) | |
| Partnership c | 0.625 Chi | |||
| Single | 14 (25.0) | 41 (17.2) | 6 (18.2) | |
| In a relationship | 12 (21.4) | 44 (18.5) | 9 (27.3) | |
| Married | 26 (46.4) | 137 (57.6) | 18 (54.5) | |
| Divorced | 2 (3.6) | 10 (4.2) | 0 (0.0) | |
| Widowed | 2 (3.6) | 6 (2.5) | 0 (0.0) | |
| Number of children a | 1.0 (0.9) | 1.3 (0.9) | 1.4 (1.1) | 0.121 ANOVA |
| Number of siblings a | 1.1 (0.8) | 1.6 (1.2) | 1.6 (0.9) | 0.016 ANOVA |
| School years a | 10.3 (1.1) | 10.6 (1.3) | 10.8 (1.3) | 0.151 ANOVA |
| Educational level c | 0.126 Chi | |||
| No training | 2 (3.6) | 8 (3.4) | 1 (3.0) | |
| Skilled worker | 37 (66.1) | 142 (59.7) | 19 (57.6) | |
| Technical college | 7 (12.5) | 50 (21.0) | 2 (6.1) | |
| University | 10 (17.9) | 38 (16.0) | 11 (33.3) | |
| Employment status c | 0.797 Chi | |||
| Training/student | 2 (3.6) | 3 (1.3) | 0 (0.0) | |
| Fulltime employed | 18 (32.1) | 68 (28.6) | 8 (24.2) | |
| Part-timer employed | 9 (16.1) | 54 (22.7) | 11 (33.3) | |
| Unemployed | 3 (5.4) | 9 (3.8) | 1 (3.0) | |
| Disability pensioned | 20 (35.7) | 75 (31.5) | 10 (30.3) | |
| Retirement pensioned | 3 (5.4) | 23 (9.7) | 3 (9.1) | |
| Other | 1 (1.8) | 6 (2.5) | 0 (0.0) | |
| Patient care c | 0.616 Chi | |||
| Outpatients | 45 (80.4) | 185 (77.7) | 28 (84.8) | |
| Inpatients | 11 (19.6) | 53 (22.3) | 5 (15.2) | |
| Course of disease | 0.833 Chi | |||
| CIS | 4 (7.1) | 11 (4.6) | 1 (3.0) | |
| RRMS | 36 (64.3) | 161 (67.6) | 24 (72.7) | |
| SPMS | 12 (21.4) | 44 (18.5) | 7 (21.2) | |
| PPMS | 4 (7.1) | 22 (9.2) | 1 (3.0) | |
| Disease duration (years) b | 8.5 | 10.0 | 12.0 | 0.216 H |
| EDSS score b | 3.0 | 3.0 | 2.5 | 0.886 H |
| DMD treatment c | 0.769 Chi | |||
| Yes | 42 (75.0) | 189 (79.4) | 26 (78.8) | |
| No | 14 (25.0) | 49 (20.6) | 7 (21.2) | |
| Comorbidities c | 0.643 Chi | |||
| Yes | 39 (69.6) | 180 (75.6) | 25 (75.8) | |
| No | 17 (30.4) | 58 (24.4) | 8 (24.2) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Langhorst, S.E.; Frahm, N.; Hecker, M.; Mashhadiakbar, P.; Streckenbach, B.; Baldt, J.; Heidler, F.; Zettl, U.K. Vaccination Coverage against Tetanus, Diphtheria, Pertussis and Poliomyelitis and Validity of Self-Reported Vaccination Status in Patients with Multiple Sclerosis. J. Pers. Med. 2022, 12, 677. https://doi.org/10.3390/jpm12050677
Langhorst SE, Frahm N, Hecker M, Mashhadiakbar P, Streckenbach B, Baldt J, Heidler F, Zettl UK. Vaccination Coverage against Tetanus, Diphtheria, Pertussis and Poliomyelitis and Validity of Self-Reported Vaccination Status in Patients with Multiple Sclerosis. Journal of Personalized Medicine. 2022; 12(5):677. https://doi.org/10.3390/jpm12050677
Chicago/Turabian StyleLanghorst, Silvan Elias, Niklas Frahm, Michael Hecker, Pegah Mashhadiakbar, Barbara Streckenbach, Julia Baldt, Felicita Heidler, and Uwe Klaus Zettl. 2022. "Vaccination Coverage against Tetanus, Diphtheria, Pertussis and Poliomyelitis and Validity of Self-Reported Vaccination Status in Patients with Multiple Sclerosis" Journal of Personalized Medicine 12, no. 5: 677. https://doi.org/10.3390/jpm12050677






