Cross Sectional Analysis of Eurasian Skull Anatomy for 3D Cephalometry—Normative Data Reveal Four Different Skull Types
Abstract
1. Introduction
2. Materials and Methods
2.1. Evaluating Sexual Dimorphism
2.2. Identifying Sub-Phenotypes within the Sex-Specific Groups
2.3. Creating Template Skulls
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Meyer, U. (Ed.) Fundamentals of Craniofacial Malformations; Springer: Berlin/Heidelberg, Germany, 2021; ISBN 978-3-030-46023-5. [Google Scholar]
- Kerkfeld, V.; Schorn, L.; Depprich, R.; Lommen, J.; Wilkat, M.; Kübler, N.; Rana, M.; Meyer, U. Simultaneous PSI-Based Orthognathic and PEEK Bone Augmentation Surgery Leads to Improved Symmetric Facial Appearance in Craniofacial Malformations. J. Pers. Med. 2022, 12, 1653. [Google Scholar] [CrossRef]
- Proffit, W.R.; Fields, H.W.; Sarver, D.M. Contemporary Orthodontics e-Book; Elsevier Health Sciences: Amsterdam, The Netherlands, 2014. [Google Scholar]
- Broadbent, B.H. A new X-ray technique and its application to orthodontia. Angle Orthod. 1931, 1, 45–66. [Google Scholar]
- Wang, R.H.; Ho, C.T.; Lin, H.H.; Lo, L.J. Three-dimensional cephalometry for orthognathic planning: Normative data and analyses. J. Formos. Med. Assoc. 2020, 119, 191–203. [Google Scholar] [CrossRef] [PubMed]
- Ho, C.T.; Denadai, R.; Lo, L.J.; Lin, H.H. Average 3D Skeletofacial Model as a Template for Maxillomandibular Repositioning During Virtual Orthognathic Surgical Planning. Plast. Reconstr. Surg. 2023; epub ahead of print. [Google Scholar] [CrossRef]
- Andriola, F.D.O.; Haas Junior, O.L.; Guijarro-Martínez, R.; Hernández-Alfaro, F.; Oliveira, R.B.D.; Pagnoncelli, R.M.; Swennen, G.R. Computed tomography imaging superimposition protocols to assess outcomes in orthognathic surgery: A systematic review with comprehensive recommendations. Dentomaxillofac. Radiol. 2022, 51, 20210340. [Google Scholar] [CrossRef] [PubMed]
- van Vlijmen, O.J.; Maal, T.J.; Berge, S.J.; Bronkhorst, E.M.; Katsaros, C.; Kuijpers-Jagtman, A.M. A comparison between two-dimensional and three-dimensional cephalometry on frontal radiographs and on cone beam computed tomography scans of human skulls. Eur. J. Oral Sci. 2009, 117, 300–305. [Google Scholar] [CrossRef]
- Yitschaky, O.; Redlich, M.; Abed, Y.; Faerman, M.; Casap, N.; Hiller, N. Comparison of common hard tissue cephalometric measurements between computed tomography 3D reconstruction and conventional 2D cephalometric images. Angle Orthod. 2011, 81, 11–16. [Google Scholar] [CrossRef]
- Gateno, J.; Xia, J.J.; Teichgraeber, J.F. New 3-dimensional cephalometric analysis for orthognathic surgery. J. Oral Maxillofac. Surg. 2011, 69, 606–622. [Google Scholar] [CrossRef]
- Devanna, R. Two-dimensional to three-dimensional: A new three-dimensional cone-beam computed tomography cephalometric analysis. J. Orthod. Res. 2015, 3, 30–37. [Google Scholar] [CrossRef]
- Jacobson, A.; Jacobson, R.L. Radiographic Cephalometry: From Basics to 3-D Imaging; Quintessence: New Malden, UK, 2007; ISBN 0-86715-461-6. [Google Scholar]
- Swennen, G.R.; Schutyser, F. Three-dimensional cephalometry: Spiral multi-slice vs cone-beam computed tomography. Am. J. Orthod. Dentofac. Orthop. 2006, 130, 410–416. [Google Scholar] [CrossRef]
- Swennen, G.R.J.; Schutyser, F.A.C.; Hausamen, J.E. Three-Dimensional Cephalometry: A Color Atlas and Manual; Springer: Berlin/Heidelberg, Germany, 2005; ISBN 978-3-540-29011-7. [Google Scholar]
- Bayome, M.; Park, J.H.; Kook, Y.A. New three-dimensional cephalometric analyses among adults with a skeletal class I pattern and normal occlusion. Korean J. Orthod. 2013, 43, 62–73. [Google Scholar] [CrossRef]
- Cheung, L.K.; Chan, Y.M.; Jayaratne, Y.S.; Lo, J. Three-dimensional cephalometric norms of Chinese adults in Hong Kong with balanced facial profile. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endodontol. 2011, 112, 56–73. [Google Scholar] [CrossRef] [PubMed]
- Vahdettin, L.; Aksoy, S.; Oz, U.; Orhan, K. Three-dimensional cephalometric norms of Turkish Cypriots using CBCT images reconstructed from a volumetric rendering program in vivo. Turk. J. Med. Sci. 2016, 46, 848–861. [Google Scholar] [CrossRef] [PubMed]
- Gu, Y.; McNamara, J.A., Jr.; Sigler, L.M.; Baccetti, T. Comparison of craniofacial characteristics of typical Chinese and Caucasian young adults. Eur. J. Orthod. 2011, 33, 205–211. [Google Scholar] [CrossRef] [PubMed]
- Hwang, H.S.; Kim, W.S.; McNamara, J.A., Jr. Ethnic differences in the soft tissue profile of Korean and European-American adults with normal occlusions and well-balanced faces. Angle Orthod. 2002, 72, 72–80. [Google Scholar] [CrossRef]
- Adams, G.L.; Gansky, S.A.; Miller, A.J.; Harrell, W.E., Jr.; Hatcher, D.C. Comparison between traditional 2-dimensional cephalometry and a 3-dimensional approach on human dry skulls. Am. J. Orthod. Dentofac. Orthop. 2004, 126, 397–409. [Google Scholar] [CrossRef]
- Nalcaci, R.; Öztürk, F.; Sökücü, O. A comparison of two-dimensional radiography and three-dimensional computed tomography in angular cephalometric measurements. Dentomaxillofac. Radiol. 2010, 39, 100–106. [Google Scholar] [CrossRef]
- Lee, S.H.; Kil, T.J.; Park, K.R.; Kim, B.C.; Kim, J.G.; Piao, Z.; Corre, P. Three-dimensional architectural and structural analysis—A transition in concept and design from Delaire’s cephalometric analysis. Int. J. Oral Maxillofac. Surg. 2014, 43, 1154–1160. [Google Scholar] [CrossRef]
- Dryden, I.L.; Mardia, K.V. Statistical Shape Analysis, 2nd ed.; Wiley: Chichester, UK, 2016; pp. 125–132. [Google Scholar]
- Schlager, S. Morpho and R. In Statistical Shape and Deformation Analysis; Zheng, G., Li, S., Székely, G., Eds.; Academic Press: London, UK, 2017; pp. 217–256. [Google Scholar]
- Celebi, A.A.; Tan, E.; Gelgor, I.E.; Colak, T.; Ayyildiz, E. Comparison of soft tissue cephalometric norms between Turkish and European-American adults. Sci. World J. 2013, 2013, 806203. [Google Scholar] [CrossRef]
- Mozzo, P.; Procacci, C.; Tacconi, A.; Martini, P.T.; Andreis, I.A. A new volumetric CT machine for dental imaging based on the conebeamtechnique: Preliminary results. Eur. Radiol. 1998, 8, 1558–1564. [Google Scholar] [CrossRef]
- Lopes, P.M.; Moreira, C.R.; Perrella, A.; Antunes, J.L.; Cavalcanti, M.G. 3-D volume rendering maxillofacial analysis of angular measurements by multislice CT. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endodontol. 2008, 105, 224–230. [Google Scholar] [CrossRef]
- Farkas, L.G.; Tompson, B.; Phillips, J.H.; Katic, M.J.; Cornfoot, M.L. Comparison of anthropometric and cephalometric measurements of the adult face. J. Craniofac. Surg. 1999, 10, 18–25. [Google Scholar] [CrossRef] [PubMed]
- Oz, U.; Orhan, K.; Abe, N. Comparison of linear and angular measurements using two-dimensional conventional methods and three-dimensional cone beam CT images reconstructed from a volumetric rendering program in vivo. Dentomaxillofac. Radiol. 2011, 40, 492–500. [Google Scholar] [CrossRef] [PubMed]
- Ursi, W.J.; Trotman, C.A.; McNamara, J.A., Jr.; Behrents, R.G. Sexual dimorphism in normal craniofacial growth. Angle Orthod. 1993, 63, 47–56. [Google Scholar] [CrossRef] [PubMed]
- Humphrey, L.T. Growth patterns in the modern human skeleton. Am. J. Phys. Anthropol. 1998, 105, 57–72. [Google Scholar] [CrossRef]
- Rosas, A.; Bastir, M. Thin-plate spline analysis of allometry and sexual dimorphism in the human craniofacial complex. Am. J. Phys. Anthropol. 2002, 117, 236–245. [Google Scholar] [CrossRef] [PubMed]
- Bastir, M. A systems-model for the morphological analysis of integration and modularity in human craniofacial evolution. J. Anthropol. Sci. 2008, 86, 37–58. [Google Scholar]
- Fearon, J.A.; Ditthakasem, K.; Herbert, M.; Kolar, J. An appraisal of the cephalic index in sagittal craniosynostosis, and the unseen third dimension. Plast. Reconstr. Surg. 2017, 140, 138–145. [Google Scholar] [CrossRef]
- Muralidhar, N.V.; Ranjan, A.; Jayashankar Rao, J.S.; Sreeshyla, H.S.; Nitin, P. Cephalic index, facial index and dental parameters: A correlative study to evaluate their significance in facial reconstruction. J. Oral Maxillofac. Pathol. 2021, 25, 537–542. [Google Scholar] [CrossRef]
- Bianchi, A.; Seidita, F.; Badiali, G.; Lusetti, L.; Saporosi, C.; Pironi, M.; Marchetti, C.; Crimi, S. Is Beauty a Matter of Volume Distribution? Proposal of a New Aesthetic Three-Dimensional Guide in Orthognathic Surgery. J. Pers. Med. 2023, 13, 936. [Google Scholar] [CrossRef]
- Baldini, B.; Cavagnetto, D.; Baselli, G.; Sforza, C.; Tartaglia, G.M. Cephalometric measurements performed on CBCT and reconstructed lateral cephalograms: A cross-sectional study providing a quantitative approach of differences and bias. BMC Oral Health 2022, 22, 98. [Google Scholar] [CrossRef]
- Farronato, M.; Baselli, G.; Baldini, B.; Favia, G.; Tartaglia, G.M. 3D Cephalometric Normality Range: Auto Contractive Maps (ACM) Analysis in Selected Caucasian Skeletal Class I Age Groups. Bioengineering 2022, 9, 216. [Google Scholar] [CrossRef] [PubMed]
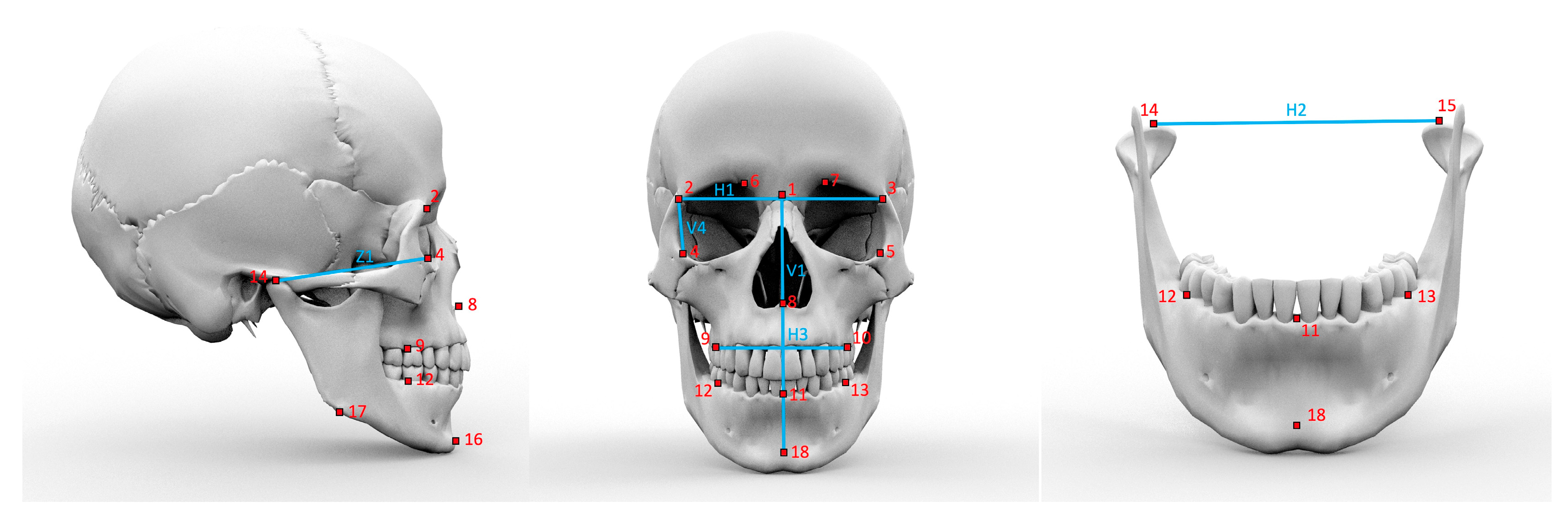







| No | Landmark | Abbreviation | Definition |
|---|---|---|---|
| 1 | Nasion | N | Intersection point of frontonasal and internasal suture |
| 2 | Frontoorbital suture right | FOS r | Intersection midpoint of processus zygomaticus and Os frontale |
| 3 | Frontoorbital suture left | FOS l | Intersection midpoint of proceccus zygomaticus and Os frontale |
| 4 | Inferior orbital edge right | IOE r | Midpoint in the curvature of the lateral orbita right |
| 5 | Inferior orbital edge left | IOE l | Midpoint in the curvature of the lateral orbita left |
| 6 | Incisura frontalis right | IF r | Medial border of the incisura frontalis right |
| 7 | Incisura frontalis left | IF l | Medial border of the incisura frontalis left |
| 8 | Spina nasalis anterior | SPA | The point on the tip of the Spina |
| 9 | First upper molar distobuccal root bone level right | UpMdbrbl r | Crestal edge of the upper right first molar distobuccal root |
| 10 | First upper molar distobuccal root bone level left | UpMdbrbl l | Crestal edge of the upper left first molar distobuccal root |
| 11 | Lower incisor bone level | LIbl | Crestal midpoint between lower first incisor roots |
| 12 | First lower molar distal root bone level right | LoMdbrbl r | Crestal edge of the lower right first molar distal root |
| 13 | First lower molar distal root bone level left | LoMdbrbl l | Crestal edge of the lower left first molar distal root |
| 14 | Condyle right | Co r | Most superior point on the midline of the condyle right |
| 15 | Condyle left | Co l | Most superior point on the midline of the condyle left |
| 16 | Pogonion | Po | Most anterior point of the mandibular symphysis |
| 17 | Posterior inferior mandibular point right | Pom r | Most caudal and most posterior point of the right mandibular |
| 18 | Posterior inferior mandibular point left | Pom l | Most caudal and most posterior point of the left mandibular |
| Abbr. | Distance |
|---|---|
| V1 | Nasion (1)—Pogonion (16) |
| V2 | Nasion (1)—SPA (8) |
| V3 | SPA (8)—Pogonion (16) |
| V4 | FOS r (2)—IOE r (4) |
| H1 | FOS r (2)—FOS l (3) |
| H2 | Co r (14)—Co l (15) |
| H3 | UpMdbrbl r (9)—UpMdbrbl l (10) |
| Z1 | IOE r (4)—Co r (14) |
| Abbr. | Proportion |
|---|---|
| P01 | V1/H1 |
| P02 | V1/H3 |
| P03 | V1/H2 |
| P04 | V1/V3 |
| P05 | V1/V6 |
| P06 | V1/Z1 |
| P07 | V3–H1 |
| P08 | H1/H3 |
| Proportion | Female | Male | Adj. p-Value |
|---|---|---|---|
| P01 | 1.08 | 1.115 | 0.031 |
| P02 | 1.877 | 2.008 | 0.001 |
| P03 | 1.04 | 1.082 | 0.015 |
| P04 | 0.962 | 0.986 | 0.275 |
| P05 | 4.851 | 5.293 | 0 |
| P06 | 1.806 | 1.874 | 0.031 |
| P07 | 1.816 | 1.785 | 0.344 |
| P08 | 1.738 | 1.802 | 0.009 |
| Proportion | Cluster m1 | Cluster m2 | Adj. p-Value |
|---|---|---|---|
| P01 | 1.178 | 1.071 | 0 |
| P02 | 2.146 | 1.912 | 0 |
| P03 | 1.136 | 1.043 | 0 |
| P04 | 0.94 | 1.019 | 0.005 |
| P05 | 5.535 | 5.123 | 0.007 |
| P06 | 1.977 | 1.802 | 0 |
| P07 | 1.643 | 1.884 | 0 |
| P08 | 1.823 | 1.786 | 0.197 |
| Proportion | Cluster f1 | Cluster f2 | Adj. p-Value |
|---|---|---|---|
| P01 | 1.164 | 1.034 | 0 |
| P02 | 2.001 | 1.791 | 0 |
| P03 | 1.092 | 1.003 | 0 |
| P04 | 0.921 | 0.989 | 0.039 |
| P05 | 4.979 | 4.763 | 0.147 |
| P06 | 1.9 | 1.742 | 0 |
| P07 | 1.67 | 1.917 | 0 |
| P08 | 1.746 | 1.733 | 0.713 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ludwigs, L.; Pape, C.; Visse, H.S.; Runte, C.; Meyer, U.; Dirksen, D. Cross Sectional Analysis of Eurasian Skull Anatomy for 3D Cephalometry—Normative Data Reveal Four Different Skull Types. J. Pers. Med. 2023, 13, 1018. https://doi.org/10.3390/jpm13061018
Ludwigs L, Pape C, Visse HS, Runte C, Meyer U, Dirksen D. Cross Sectional Analysis of Eurasian Skull Anatomy for 3D Cephalometry—Normative Data Reveal Four Different Skull Types. Journal of Personalized Medicine. 2023; 13(6):1018. https://doi.org/10.3390/jpm13061018
Chicago/Turabian StyleLudwigs, Leon, Christian Pape, Helena Sophie Visse, Christoph Runte, Ulrich Meyer, and Dieter Dirksen. 2023. "Cross Sectional Analysis of Eurasian Skull Anatomy for 3D Cephalometry—Normative Data Reveal Four Different Skull Types" Journal of Personalized Medicine 13, no. 6: 1018. https://doi.org/10.3390/jpm13061018
APA StyleLudwigs, L., Pape, C., Visse, H. S., Runte, C., Meyer, U., & Dirksen, D. (2023). Cross Sectional Analysis of Eurasian Skull Anatomy for 3D Cephalometry—Normative Data Reveal Four Different Skull Types. Journal of Personalized Medicine, 13(6), 1018. https://doi.org/10.3390/jpm13061018






