1. Introduction
PDMS (polydimethylsiloxane) is a widely used polymer in microfluidic devices for cell and tissue engineering and cell-on-a-chip due to its biocompatibility, permeability to gases, transparency, easy molding and economic affordability. Intrinsic drawbacks of PDMS cause the inappropriate surface for long-term cell analysis [
1,
2,
3,
4]. Although oxygen plasma treatment, chemical functionalization, and protein coating make the surface biocompatible for cell adhesion, the hydrophilicity reaction caused by oxygen plasma is reversible and also depends on reaction time and temperature. On the other hand, cell attachment and cell aggregations are improved only in areas where the protein has been coated [
1,
5,
6,
7]. Given the increasing demand for microfluidics stem cell-based assays, the tailoring of biocompatible and improved biointerfaces to promote cell-surface interactions is highly demanded.
The requirement for advanced stem cell technology has dramatically increased in the last decade, due to the importance of stem cells for medical therapeutics, drug development, and a variety of health-care applications including toxicological studies, disease modeling, and cell replacement therapies [
3,
8,
9]. Mammalian cell adhesion on the substrate surface is pivotal to measure cell viability, proliferation, and differentiation [
1], and cell growing behavior significantly depends on surface chemical properties [
6]. Chemical modification of surfaces can potentially improve cell adhesion and long-term culture. Previous attempts to increase cell viability on PDMS substrate using plasma treatment, silanization, and polymer functionalization have shown improved cell behavior, but the effect was not acceptable. In addition, the use of nanomaterials in the case of PDMS functionalization has not been evaluated so far.
Recently, nano-engineered materials have been widely applied in the areas of drug delivery, biosensing, stem cells, biomedical science, nanotoxicity evaluation, and tissue engineering [
3,
10,
11,
12,
13,
14,
15,
16]. For instance, osteoblast and stem cells cultured on nano-scaffold have long slender morphology on adhesion to neighbor cells; however, the cells cultured in solid scaffold have flat and smooth morphology [
17,
18,
19,
20]. The effective parameters of the micro-electro-mechanical system (MEMS) on cell attachment are surface chemistry (functional group, surface charge, and hydrophilicity/ hydrophobicity), surface roughness, and topography, which can affect protein adsorption and cell attachment [
21]. Tissue engineering strategies require migration and proliferation of the cells to fully populate the scaffold to regenerate and recover the injured tissue. Most of the cells have to attach on the surface to proliferate, migrate, and differentiate; therefore, cell attachment is the first step in recovery development. The extracellular matrix (ECM) induces cellular attachment, migration, proliferation, and differentiation. Indeed, artificial ECM use in tissue engineering can mimics the natural ECM in the extracellular matrix [
6,
19,
22,
23]. Various binding protein-like fibronectin, vitronectin, and laminin are used in nano-scaffold, and protein adsorption in nano-scaffold was improved to become 2–4 times better than solid-walled scaffold due to the increase of surface area [
18,
19]. In the study by Xue et al., fibronectin and collagen type (I) have been covalently bonded to 3-Aminopropyltriethoxysilane (APTES) via glutaraldehyde cross-linker on SU-8 surface [
6]. They showed that alongside the wettability of the matrix, the attachment and proliferation of the cells increased compared with the tissue culture plate (TCP), free fibronectin, and collagen (I). Although this surface treatment method is very effective, the process involves time-consuming intermediate steps and the human error accumulated between each step may potentially lead to batch-to-batch inconsistencies. Furthermore, the various cells have different behavior on the diverse contexts like an increase of proliferation in nano-context compared with TCP [
17,
19,
24]. The formed ECM in the cell grown on the nano-context in comparison to the solid-walled or micro-context has higher cell attachment ability. Cell therapy can regenerate the function of the cured tissue; however, less control on cell surviving, differentiation, and maturation are its limitation factors in order to be used as a powerful therapeutic technique [
25]. The engineered scaffold can control the behavior of stem cells and therefore solve the above-mentioned problems.
The application of nanoparticles (NPs) in regenerative medicine has a very promising future, but NPs can create unpredictable effects on stem cells and also side effects due to small size and penetration ability into the human body [
13,
14,
15,
25]. In general, the NPs used in tissue engineering must have characteristics such as biocompatibility, non-toxicity, preservation of physicochemical properties after surface modification, and no effect on stem cell properties and chemical stability in the physiological environment [
14,
26,
27]. On the other hand, using nanocomposite (NPs and polymer) can improve the cell adhesion, proliferation, and differentiation of stem cells and reduce the potential side effects and risks of nanoparticles [
28]. It has been shown that the addition of NPs to the scaffold increases the biological regulation of cell behavior. In a study, apatite nanocrystal merged inside polymer fiber to improve tissue regeneration and cell-cell adhesion. The effects of nanocrystal are more important than microcrystal on biological behavior [
1]. The mechanism of this phenomenon is still unclear; however, ECM proteins like vitronectin and collagen may easily be absorbed in the substrate in nanoscale compared with microscale [
19]. Using a chemical agent like silane to make hydrophilic PDMS may be harmful to cell growth due to its side effects on regenerative medicine and cell therapy. On the other hand, using NPs in cell differentiation may have some toxicity; however, immobilized NPs in the composite have less toxicity and improve cell growth, proliferation, and differentiation [
1]. In our previous work, a thin-film layer for microfluidics cell-based assays was fabricated without PDMS functionalization [
3]. The nanostructured microfluidics platform was developed to improve human amniotic stem cell differentiation using fibrin/gold nanowires. The result showed that incorporating gold nanowire into fibrin could significantly enhance the differentiation of stem cells to osteo/chondrogenic fates. The synergic role of stiffness and presence of AuNWs have been emphasized in our previous work, where nanotopographical cues created by AuNWs altered the rate of hAMSC differentiation in comparison with the thin-film layer without AuNWs. Nevertheless, PDMS functionalization using nanomaterials has not yet been evaluated for microfluidics cell-based assays. Chuah et al. found that the addition of wettability using polydopamine improves proliferation and differentiation and keeps the multipotency of MSCs [
2]. Therefore, hydrophilic condition and amine formation groups on the surface, which makes a biocompatible surface feasible for mechanobiology and cell analysis purposes. Therefore, the availability of these chemical groups in NPs improves the attachment of the cell to the matrix, and proliferation with regard to most of the protein receptors is located at the cell surface. The rougher surface has a larger surface area, and then the cell adhesion improves on the surface in comparison to a smooth surface, which can lead to increase in cell adhesion [
3,
28,
29,
30,
31]. Many polymeric substrates that are being used in tissue engineering nowadays have no suitable mechanical properties. Thus, in order to improve their mechanical and other properties, NPs, biopolymers, and inorganic fillers have been used to overcome this drawback [
28,
32]. Therefore, a simple, environmentally safe, and effective surface functionalization strategy is crucial for rendering biocompatible PDMS surfaces for long-term cell investigation on PDMS-based lab-on-a-chip devices.
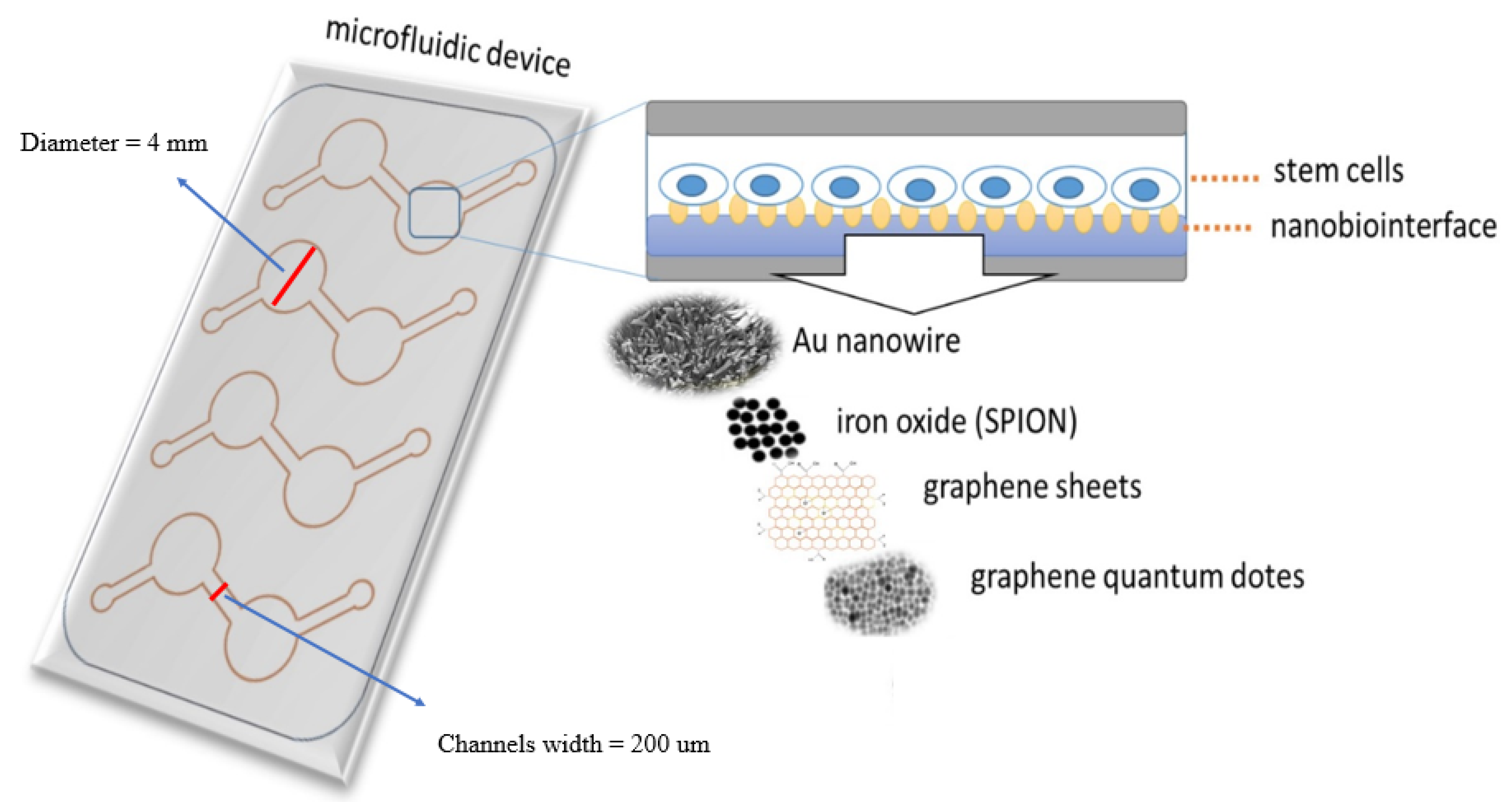
Hence, in the current study, we have doped PDMS with a variety of biocompatible nanomaterials to create a nanomaterial-PDMS composite that presents a biocompatible and tunable nano-biointerface for hAMSC adhesion, toxicity, proliferation, and differentiation. Embedding nanoobjects in the PDMS material thus eliminates tedious surface chemistries and secondary modification steps. In this study, we fabricated and tested various nanomaterial—PDMS composites containing either AuNWs, SPIONs, GO, as well as GQD (see
Figure 1). Based on initial cell adhesion studies and surface characterizations, polymer-composite nano-biointerfaces are fabricated and subsequently used to investigate stem cell adhesion, proliferation, and differentiation capacity.
2. Materials and Methods
2.1. Materials
Gold nanowire (AuNW), graphene oxide (GO), super paramagnetic iron oxide (SPION), and graphene quantum dot (GQD) were synthesized in-house based on our previous research [
3,
13,
15]. Fetal calf serum (FCS) and Dulbecco’s modified Eagle’s medium (DMEM) were obtained from Gibco (all from Gibco, Thermo Fisher Scientific, Waltham, MA, USA) and (3-(4, 5-dimethylthiazol-2-yl)-2, 5-diphenyltetrazolium bromide) tetrazolium assay (MTT) from Sigma Aldrich (Merck KGaA, Darmstadt, Germany). Standard tissue culture grade polystyrene (TCPS) 96-well CELLSTAR
® multi-plates (Greiner Bio-One, Germany) were used and PDMS (Sylgard 184) was purchased from Dow Corning Co. Inc. Double distilled deionized water was produced using a Millipore-Q water system and used in all experiments.
2.2. Preparation of a PDMS-Based Culture Containing NPs
More details about the synthesis and characterization of NPs are in
supplementary materials (S1). Surface modification was performed by immersing the native PDMS surface in six nanoparticles, gold nanowire (AuNW), superparamagnetic iron oxide nanoparticle (SPION), graphene quantum dot (GQD), and graphene oxide (GO). PDMS without any nanomaterials and also tissue culture plate (TCP) were used as a control. Each nanomaterial was mixed with PDMS (elastomer to curing agent 10:1 w/w). The certain amounts of NPs were slowly added to the PDMS under vigorous stirring, spin-coated on glass, and then the mixture was degassed in a vacuum desiccator, incubated at 65 °C for at least 6 h. After complete curing, circles with a radius of 2.1 mm were cut, sterilized for 1–2 h under ultraviolet light, and put in the sterilized condition into a 96-well TCP.
2.3. Surface Characterization
The surface roughness (nanotopography) and Young’s modulus of the PDMS substrates containing SPION, GO and GQD, were determined using atomic force microscopy (AFM, CoreAFM, NanoSurf Co. Ltd, Switzerland and Multi-mode AFM, Ara Research Co., Tehran, Iran) with a tapping mode AFM probe, which comprised a silicon tip with a radius of 28 ± 10 nm and a spring constant range of 0.5–4.4 N m−1. 20 μm × 20 μm topographical images were scanned at 0.8 Hz, a set point of 0.7 V, and a resolution of 256 pixels. At least 3 points of contact were analyzed for each PDMS substrate. To measure the roughness of the AuNW/PDMS substrate, SEM images were considered in this case by using ImageJ software (version 1.52i, Fiji, Madison, WI, USA). To describe the roughness of the surfaces, the topography of the surface, and the roughness parameter for the surface, the Sa, which is the area average or the distance between the highest and the lowest point of the surface irregularities, was shown and calculated using built-in software (NanoSurf™ CoreAFM Software, version 3.8.1.4, Switzerland). For Au-NW sample preparation, a drop of water containing Au-NW was placed on an aluminum substrate and incubated until the water evaporated. It was then sputter-coated with a 2 nm layer of gold to prevent charge build-up using a coater and then characterized using a KYKY-EM3200 digital scanning electron microscope (SEM-Model tech, KYKY Technology Development Ltd., Bejing, China).
2.4. Microfluidics Assay
To create the microfluidics assay, a template for chip fabrication was designed using AUTOCAD 2016 (Autodesk, San Rafael, CA, USA). Then, PDMS sheets were cut using a CAM-1 GS-24 cutter (Roland DGA Corporation, Irvin, CA, USA). Four mm circles from NP/PDMS were cut and used as a substrate in the microfluidic chip (
Figure 1). To bind the PDMS-nanomaterial scaffolds and fabricated template to the glass slide, plasma treatment was applied (Harrick Plasma, High Power, 120 s). A certain amount of cells per mL (based on the surface area of the cell culture chamber) were seeded into the microfluidics system, and after expansion, the hAMSCs medium was replaced with osteogenic stem cell differentiation medium (StemMACS OsteoDiff Media, order No. 130-091-678, Miltenyi Biotec GmbH, Bergisch Gladbach, Germany) supplemented with FCS 10% and 1% penicillin/streptomycin. During the stem cell differentiation on-a-chip, the medium was replaced with OsteoDiff Media every 1–2 days, since the chip was kept under CO
2 (5%), at 37 °C in an incubator. After 7 and 14 days of hAMSCs being treated with OsteoDiff Media, the samples were used to characterize the differentiation rate.
2.5. Immunofluorescence Microscopy and Alizarin Red Staining
Immunohistochemical staining of the differentiated hAMSCs on NP/PDMS was performed using primary antibodies against collagen type I (Abcam; mouse monoclonal, ab6308, 1/1000 dilution, Cambridge, UK) as follows. The samples were rinsed with PBS several times carefully and slowly, fixated and permeabilized with a solution of 4% paraformaldehyde, 0.5% Triton X100, blocking nonspecific antibodies with 3% BSA, and washed with PBS, using the primary antibodies and wash, blocking nonspecific antibodies with 3% BSA, and washed with PBS. They were then stained with Alexa flour secondary antibody (1/200 dilution monoclonal goat anti-rabbit IgG) and washed with PBS, stained with DAPI (4′, 6-Diamidino-2-phenylindole dihydrochloride). Finally, the stained differentiated hAMSCs cells were viewed using an Olympus IX81 and IX71 (Olympus Ltd, Tokyo, Japan), and the images were analyzed using Fiji software for mean fluorescence intensity (RFU) measurement. For the evaluation of osteogenesis on different NP/PDMS surfaces using alizarin red (2%) (Merck KGaA, Darmstadt, Germany), the medium was removed and each cell chamber was washed several times with PBS and fixed with 4% paraformaldehyde (the paraformaldehyde was heated prior to use to 37 °C in a water bath). Then, the differentiated hAMSCs chamber was immersed in alizarin red, and afterward, to remove the nonspecific staining of alizarin red, the samples were washed gently several times with distilled water (DDW). Finally, an image of the samples was captured using an Olympus IX81 and IX71 microscope and the data were analyzed using Fiji software using optical density measurement.
2.6. Cell Culture Assay
As reported in our previous work [
3], human amniotic mesenchymal stem cells (hAMSCs) were used for stem cell differentiation and for investigation of cell adhesion, short-term growth, cell proliferation, cell viability, and cytotoxicity profiles. The study was approved by the ethics committee of the Medical University Vienna (EK791/2008, EK1192/2015), the University Hospital of Lower Austria (GS1-EK-4/312-2015), and the Danube University Krems (Nr.821/2009, 03. Sep. 2015). The placenta was obtained from a healthy delivering woman in accordance with the Austrian Hospital Act (KAG 1982) after written informed consent was signed. The cells were cultured in DMEM medium containing 10% fetal bovine serum and 1% antibiotic solution (Penicillin-Streptomycin) until the desired confluences were reached. Cells were harvested and cultured on NP-PDMS substrates in a 96-well tissue culture plate (TCP) containing DMEM medium containing 10% fetal bovine serum and 1% antibiotic solution [
3]. MTT and neutral red assay were used 1, 3, and 5 days after inoculation. To investigate cell behaviors in 1, 3, and 5 days, 4.5 × 10
3, 3 × 10
3, and 2 × 10
3 cells were inoculated on NP-PDMS substrates in the 96-well plate, respectively. Cell adhesion assay was performed via MTT and a neutral red test, following Mosmann [
33]. Hence, after cell counting and re-suspending in standard medium, stem cells were inoculated on nanoparticle-containing substrates in a microplate and were placed in the incubator for more than 30 minutes allowing cells to attach. Then the medium was removed gently, to eliminate unattached cells. This procedure was repeated three times for the complete elimination of unattached cells. Then, cells were incubated under CO
2 (5%), at 37 °C, for 24 h. After reaching confluence the adhered cells were exposed to MTT reagent for 3 h of forming and also neutral red assay. After removing from MTT reagent, dimethyl sulfoxide (DMSO) (Merck KGaA, Darmstadt, Germany) was added to each well and incubated for 15 min on a shaker. Then, the absorbance of the respective wells was measured at 570 nm using a plate reader (Biotek®, Winooski, VT, USA), and the wells filled with only DMSO were taken as blank reference and their amount was subtracted from the other wells. The cell attachment/viability was expressed relative to control values. The same protocol was used for cell viability, cell proliferation, and other behaviors, without washing at the beginning time.
2.7. Statistical Analysis
After normalizing the collected data, a statistical analysis such as analysis of variance (ANOVA) and mean comparison was performed using statistical analysis software (SAS) version 9.1 (San Diego, CA, USA). Data were subjected to analysis of variance, and means were compared using Tukey’s multiple comparison test with P = 0.05. The means ± SE were used to compare the data. The mean optical density (OD) and mean fluorescence intensity (RFU) of each pixel of visualized differentiated hAMSCs were analyzed using Fiji software. For this, more than 800 pixels of each bright field and fluorescence 8-bit images (after converting RGB-image to 8-bit) were subtracted with mean value pixel of background. The average of the resulting values was used for mean comparison of each substrate (NP/PDMS) for both immunofluorescence and alizarin red staining.
4. Discussion
The current study was carried out to evaluate nanostructured biointerface fabricated using PDMS/NPs composites for stem cell viability and differentiation. Stem cell viability, osteogenic stem cell differentiation, and bone regeneration are largely affected by physical and chemical cues in the surrounding microenvironment [
3,
34,
39]. In this study, it was shown that nanostructures containing SPION, AuNWs, GO, and GQD nanoparticles, due to high surface to volume ratio and their nanoscale size, can promote hAMSCs adhesion, proliferation, and differentiation. Microscopic image processing showed cultured hAMSCs have high cell density on the cell substrate. Moreover, the cell morphology of hAMSCs cultured on the nano-biointerface is different in comparison with the morphology of cells cultured on pristine PDMS (
Supplementary Materials Figure S2). Regarding initial cell viability on the nanostructured biointerface, the substrates containing AuNWs and SPION nanomaterials showed strong cell-substrate interactions. Enhancement of cell proliferation from 30% (pristine PDMS) to 85% (nano-modified scaffolds containing AuNWs and SPIONs) resulted in altering the surface properties of PDMS. In addition, in the case of cell adhesion, nano-modified PDMS with AuNWs and SPIONs had a 46%–47% increase, while pristine PDMS had a 30% increase. Furthermore, the short-term growth rate of hAMSCs on pristine PDMS was 30%, while this rate raised to 74% and more on AuNWs/SPIONs-modified PDMS. This effect can be explained by the fact that pristine PDMS without chemical modifications is a flat and very hydrophobic biointerface, which reduces protein adsorption, which is involved in cell-substrate interactions, and thus reduces proper cell adhesion and spreading. The synergic effects in surface chemistry, topology, stiffness, roughness, and mechanical properties were observed by using various nanoparticles. In this study, the rate of calcification increased from 60% (pristine PDMS) to 95% (PDMS/AuNWs), and cell surface marker expression from 40% in PDMS to 77% in SPION- and AuNWs-PDMS scaffolds at 14 days. Since PDMS-GQD and PDMS-GO substrates when exposed to fluorescence light have intrinsic fluorescence emission, the Coll I biomarkers expression (compared to alizarin red results) could not be well evaluated for the hAMSCs differentiated on GO and GQD/PDMS at the point of analysis, but calcification assays confirmed its positive effects on hAMSCs differentiation. For this, we suggest to carry out more verification for stem cell differentiation using qRT-PCR or immunofluorescence antibodies staining with different emission in the range of emission of these nanoparticles. The results of previous studies showed that the nano-topographical properties of the scaffold are more important than microscale ones in osteogenesis. Moreover, cell responses will be affected by the disorder degree of nanopatterns, while stem cell fate could be determined by the dimension and orientation of nanopatterns. Integrin-related focal adhesion formation along with the reorganization of cytoskeleton are the most important cell functions affected by roughness [
3,
11,
34,
39]. Hence, in this study cell substrates with nanoscale properties seemed to facilitate protein adsorption in the process of initial cell viability, as well as affecting the cytoskeletal changes of hAMSCs and enhancing osteogenesis. Numerous studies have demonstrated that enhanced osteogenic differentiation could be achieved by increasing the roughness profile of a substrate, reducing the surface hydrophobicity, providing functional groups that facilitate surface protein attachment, and subjecting MSCs to nano-topographical cues [
3,
34,
40]. The results showed that the impact of roughness is more important than Young’s modulus, as increased hAMSCs adhesion, proliferation, Coll I expression and calcium deposition were found in hAMSCs cultured on corresponding NP-PDMS substrates. In the case of substrate roughness, Young’s modulus and also the findings of our study indicate that incorporating nanoparticles in PDMS could affect the osteogenic differentiation of hAMSCs through modulating the roughness of substrates. Our study offers beneficial information for the fabrication and development of a nanomaterial-based PDMS platform for different stem cell-based assays and biomedical applications such as tissue engineering scaffolds, drug discovery, disease modeling, and toxicological studies.
As hypothesized, the nanotopography created by the nanoparticle plays an important role in stem cell behavior. The AuNWs and SPION nanostructured surfaces showed the best compatibility conditions for adhesion, proliferation, and differentiation of stem cells. Thus, the nanobiointerfaces prepared in this work can be considered as interesting interfaces which are able to support not only stem cells, but also different cell types. More aspects of the chemical groups of the surfaces, different stiffness, and the properties of nanobiointerfaces and potential biomedical applications of these nanostructured surfaces need to be examined in future works. However, the initial results obtained here including cell viability, mechanical properties, and cell differentiation suggest that this nano-biointerface can be a potential candidate to find applications in on-chip cell-based assays, tissue engineering, and drug screening.