Optimization of Nanoparticles for Smart Drug Delivery: A Review
Abstract
:1. Introduction

2. Improving Biocompatibility
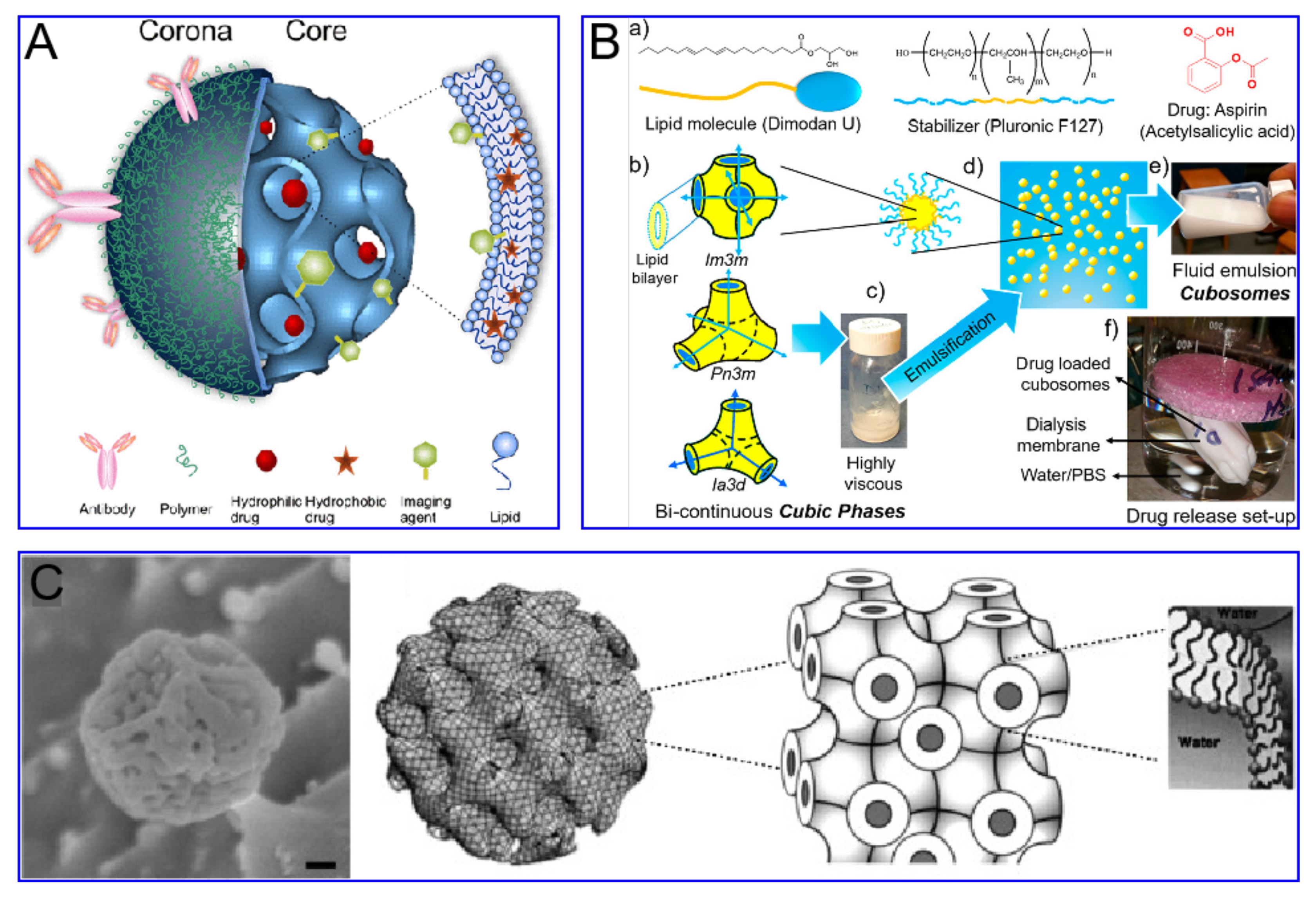
2.1. Liposomal Formulations
2.2. Cubosomes
2.3. Cell Membrane Interface
2.4. Nature Cell
2.5. Biomacromolecule
3. Increasing the Targeting Efficiency
3.1. Cell Membrane
3.1.1. Red Blood Cell Membrane
3.1.2. Platelet Membrane
3.1.3. Cancer Cell Membrane
3.1.4. Immune Cell Membrane
3.1.5. Hybrid Membranes and Others
3.2. Cell Robot
3.2.1. Nanoparticles Coated with Bacteria
3.2.2. Combination Nanoparticles with Cells
3.3. Drug Release Triggered by Different Conditions
4. Increasing the Drug Loading Rate
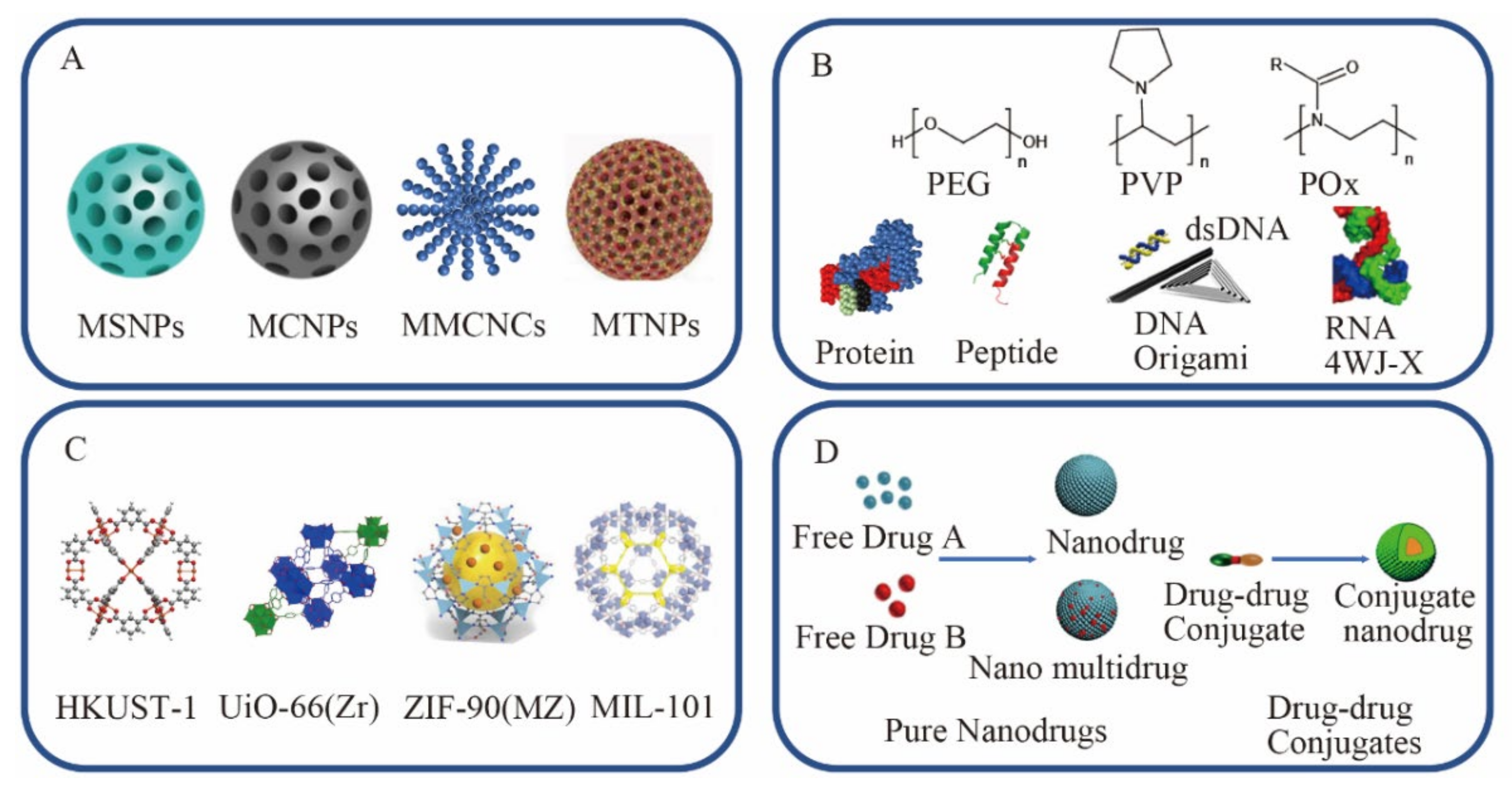
4.1. Inorganic Carrier Nano Drug Delivery System
4.1.1. Mesoporous Silica-Based NPs (MSNPs)
4.1.2. Mesoporous Carbon NPs (MCNPs)
4.1.3. Mesoporous Magnetic Colloidal Nanocrystal Clusters (MCNCs)
4.1.4. Mesoporous TiO2 NPs (MTNPs)
4.2. Organic Carrier Nano Drug Delivery System
4.2.1. Synthetic Polymer
4.2.2. Natural Biopolymers
4.3. MOF Carrier Nano Drug Delivery System
4.4. Carrier-Free Nanomedicines Delivery System
4.4.1. Pure Nanodrugs
4.4.2. Drug–Drug Conjugates
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Wang, B.; Kostarelos, K.; Nelson, B.J.; Zhang, L. Trends in Micro-/Nanorobotics: Materials Development, Actuation, Localization, and System Integration for Biomedical Applications. Adv. Mater. 2020. [Google Scholar] [CrossRef]
- Zhang, W.; Wang, M.; Tang, W.; Wen, R.; Zhou, S.; Lee, C.; Wang, H.; Jiang, W.; Delahunty, I.M.; Zhen, Z.; et al. Nanoparticle-Laden Macrophages for Tumor-Tropic Drug Delivery. Adv. Mater. 2018, 30, e1805557. [Google Scholar] [CrossRef]
- Li, R.; He, Y.; Zhang, S.; Qin, J.; Wang, J. Cell membrane-based nanoparticles: A new biomimetic platform for tumor diagnosis and treatment. Acta Pharm. Sin. B 2018, 8, 14–22. [Google Scholar] [CrossRef]
- Wang, N.; Cheng, X.; Li, N.; Wang, H.; Chen, H. Nanocarriers and Their Loading Strategies. Adv. Health Mater. 2019, 8, 1801002. [Google Scholar] [CrossRef] [PubMed]
- Zhao, N.; Yan, L.; Zhao, X.; Chen, X.; Li, A.; Zheng, D.; Zhou, X.; Dai, X.; Xu, F.-J. Versatile Types of Organic/Inorganic Nanohybrids: From Strategic Design to Biomedical Applications. Chem. Rev. 2019, 119, 1666–1762. [Google Scholar] [CrossRef]
- Chou, L.Y.T.; Ming, K.; Chan, W.C.W. Strategies for the intracellular delivery of nanoparticles. Chem. Soc. Rev. 2011, 40, 233–245. [Google Scholar] [CrossRef]
- Fu, Q.; Lv, P.; Chen, Z.; Ni, D.; Zhang, L.; Yue, H.; Yue, Z.; Wei, W.; Ma, G. Programmed co-delivery of paclitaxel and doxorubicin boosted by camouflaging with erythrocyte membrane. Nanoscale 2015, 7, 4020–4030. [Google Scholar] [CrossRef]
- Rao, L.; Bu, L.L.; Meng, Q.F.; Cai, B.; Deng, W.W.; Li, A.; Li, K.; Guo, S.S.; Zhang, W.F.; Liu, W. Antitumor Platelet-Mimicking Magnetic Nanoparticles. Adv. Funct. Mater. 2017, 27, 1604774. [Google Scholar] [CrossRef]
- Sun, H.P.; Su, J.H.; Meng, Q.S.; Yin, Q.; Chen, L.L.; Gu, W.W.; Zhang, Z.W.; Yu, H.J.; Zhang, P.C.; Wang, S.L. Cancer Cell Membrane-Coated Gold Nanocages with Hyperthermia-Triggered Drug Release and Ho-motypic Target Inhibit Growth and Metastasis of Breast Cancer. Adv. Funct. Mater. 2017, 27, 1604300. [Google Scholar] [CrossRef]
- Kang, T.; Zhu, Q.; Wei, D.; Feng, J.; Yao, J.; Jiang, T.; Song, Q.; Wei, X.; Chen, H.; Gao, X.; et al. Nanoparticles Coated with Neutrophil Membranes Can Effectively Treat Cancer Metastasis. ACS Nano 2017, 11, 1397–1411. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Medina-Sánchez, M.; Maitz, M.F.; Werner, C.; Schmidt, O.G. Sperm Micromotors for Cargo Delivery through Flowing Blood. ACS Nano 2020, 14, 2982–2993. [Google Scholar] [CrossRef]
- Park, S.J.; Park, S.H.; Cho, S.; Kim, D.M.; Lee, Y.; Ko, S.Y.; Hong, Y.; Choy, H.E.; Min, J.J.; Park, J.O. New paradigm for tumor theranostic methodology using bacteria-based microrobot. Sci. Rep. 2013, 3, 3394. [Google Scholar] [CrossRef] [Green Version]
- Safinya, C.R.; Ewert, K.K. Liposomes derived from molecular vases. Nature 2012, 489, 372–374. [Google Scholar] [CrossRef] [PubMed]
- Allen, T.M.; Cullis, P.R. Liposomal drug delivery systems: From concept to clinical applications. Adv. Drug Deliv. Rev. 2013, 65, 36–48. [Google Scholar] [CrossRef]
- Makwana, V.; Karanjia, J.; Haselhorst, T.; Anoopkumar-Dukie, S.; Rudrawar, S. Liposomal doxorubicin as targeted delivery platform: Current trends in surface functionalization. Int. J. Pharm. 2021, 593, 120117. [Google Scholar] [CrossRef]
- Akinc, A.; Maier, M.A.; Manoharan, M.; Fitzgerald, K.; Jayaraman, M.; Barros, S.; Ansell, S.; Du, X.; Hope, M.J.; Madden, T.D.; et al. The Onpattro story and the clinical translation of nanomedicines containing nucleic acid-based drugs. Nat. Nanotechnol. 2019, 14, 1084–1087. [Google Scholar] [CrossRef]
- Hong, H.C.; Kim, K.S.; Park, S.A.; Chun, M.J.; Hong, E.Y.; Chung, S.W.; Kim, H.J.; Shin, B.G.; Cho, Y.J.; Kim, S.-H. An mRNA vaccine against SARS-CoV-2: Lyophilized, liposome-based vaccine candidate EG-COVID induces high levels of virus neutralizing antibodies. bioRxiv 2021. [Google Scholar] [CrossRef]
- Patel, H.M. Serum opsonins and liposomes: Their interaction and opsonophagocytosis. Crit. Rev. Ther. Drug Carr. Syst. 1992, 9, 39–90. [Google Scholar]
- Scherphof, G.; Roerdink, F.; Waite, M.; Parks, J. Disintegration of phosphatidylcholine liposomes in plasma as a result of interaction with high-density lipoproteins. Biochim. Et Biophys. Acta 1978, 542, 296–307. [Google Scholar] [CrossRef]
- Van Rooijen, N. The liposome-mediated macrophage ‘suicide’ technique. J. Immunol. Methods 1989, 124, 1–6. [Google Scholar] [CrossRef]
- Kelly, C.; Jefferies, C.; Cryan, S.-A. Targeted Liposomal Drug Delivery to Monocytes and Macrophages. J. Drug Deliv. 2011, 2011, 727241. [Google Scholar] [CrossRef] [PubMed]
- Rooijen, N.V.; Sanders, A. The macrophage as target or obstacle in liposome-based targeting strategies. Int. J. Pharm. 1998, 162, 45–50. [Google Scholar] [CrossRef]
- Meyers, P.A. Muramyl Tripeptide-Phosphatidyl Ethanolamine Encapsulated in Liposomes (L-MTP-PE) in the Treatment of Os-teosarcoma. In Current Advances in Osteosarcoma: Clinical Perspectives: Past, Present and Future; Kleinerman, E.S., Gorlick, R., Eds.; Springer International Publishing: Cham, Switzerland, 2020; pp. 133–139. [Google Scholar]
- Jain, S.; Mishra, V.; Singh, P.; Dubey, P.; Saraf, D.; Vyas, S. RGD-anchored magnetic liposomes for monocytes/neutrophils-mediated brain targeting. Int. J. Pharm. 2003, 261, 43–55. [Google Scholar] [CrossRef]
- Banerjee, G.; Medda, S.; Basu, M.K. A Novel Peptide-Grafted Liposomal Delivery System Targeted to Macrophages. Antimicrob. Agents Chemother. 1998, 42, 348–351. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Narita, Y.; Shimizu, K.; Ikemoto, K.; Uchino, R.; Kosugi, M.; Maess, M.; Magata, Y.; Oku, N.; Ogawa, M. Macrophage-targeted, enzyme-triggered fluorescence switch-on system for detection of embolism-vulnerable atherosclerotic plaques. J. Control. Release 2019, 302, 105–115. [Google Scholar] [CrossRef] [PubMed]
- Utsugi, T.; Dinney, C.P.N.; Killion, J.J.; Fidler, I.J. In situ activation of mouse macrophages and therapy of spontaneous renal cell cancer metastasis by liposomes containing the lipopeptide CGP 31362. Cancer Immunol. Immunother. 1991, 33, 375–381. [Google Scholar] [CrossRef] [PubMed]
- Mehta, K.; Lopez-Berestein, G.; Hersh, E.M.; Juliano, R.L. Uptake of liposomes and liposome-encapsulated muramyl dipeptide by human peripheral blood monocytes. J. Reticuloendothel. Soc. 1982, 32, 155–164. [Google Scholar] [PubMed]
- Zou, L.; Ding, W.; Zhang, Y.; Cheng, S.; Li, F.; Ruan, R.; Wei, P.; Qiu, B. Peptide-modified vemurafenib-loaded liposomes for targeted inhibition of melanoma via the skin. Biomaterials 2018, 182, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Shahin, M.; Soudy, R.; Aliabadi, H.M.; Kneteman, N.; Kaur, K.; Lavasanifar, A. Engineered breast tumor targeting peptide ligand modified liposomal doxorubicin and the effect of peptide density on anticancer activity. Biomaterials 2013, 34, 4089–4097. [Google Scholar] [CrossRef] [PubMed]
- Liang, B.; Shahbaz, M.; Wang, Y.; Gao, H.; Fang, R.; Niu, Z.; Liu, S.; Wang, B.; Sun, Q.; Niu, W.; et al. Integrinβ6-Targeted Immunoliposomes Mediate Tumor-Specific Drug Delivery and Enhance Therapeutic Efficacy in Colon Carcinoma. Clin. Cancer Res. 2015, 21, 1183–1195. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dhritlahre, R.K.; Saneja, A. Recent advances in HER2-targeted delivery for cancer therapy. Drug Discov. Today 2021, 26, 1319–1329. [Google Scholar] [CrossRef]
- Ternullo, S.; Basnet, P.; Holsæter, A.M.; Flaten, G.E.; de Weerd, L.; Škalko-Basnet, N. Deformable liposomes for skin therapy with human epidermal growth factor: The effect of liposomal surface charge. Eur. J. Pharm. Sci. 2018, 125, 163–171. [Google Scholar] [CrossRef] [Green Version]
- Mamot, C.; Drummond, D.C.; Noble, C.O.; Kallab, V.; Guo, Z.; Hong, K.; Kirpotin, D.B.; Park, J.W. Epidermal Growth Factor Receptor–Targeted Immunoliposomes Significantly Enhance the Efficacy of Multiple Anticancer Drugs In vivo. Cancer Res. 2005, 65, 11631–11638. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Merino, M.; Lozano, T.; Casares, N.; Lana, H.; Troconiz, I.F.; Hagen, T.L.M.T.; Kochan, G.; Berraondo, P.; Zalba, S.; Garrido, M.J. Dual activity of PD-L1 targeted Doxorubicin immunoliposomes promoted an enhanced efficacy of the antitumor immune response in melanoma murine model. J. Nanobio Technol. 2021, 19, 102. [Google Scholar] [CrossRef]
- Zheng, Z.; Ji, H.; Zong, W.; Ran, Q.; Wang, X.; Yang, X.; Zhao, Z.; Yang, C.; Xiao, Y. Construction and characterization of immunoliposomes targeting fibroblast growth factor receptor 3. AMB Express 2019, 9, 150. [Google Scholar] [CrossRef]
- Scavo, M.P.; Cutrignelli, A.; DePalo, N.; Fanizza, E.; Laquintana, V.; Gasparini, G.; Giannelli, G.; Denora, N. Effectiveness of a Controlled 5-FU Delivery Based on FZD10 Antibody-Conjugated Liposomes in Colorectal Cancer In vitro Models. Pharmaceutics 2020, 12, 650. [Google Scholar] [CrossRef]
- Sun, S.; Zou, H.; Li, L.; Liu, Q.; Ding, N.; Zeng, L.; Li, H.; Mao, S. CD123/CD33 dual-antibody modified liposomes effectively target acute myeloid leukemia cells and reduce antigen-negative escape. Int. J. Pharm. 2019, 568, 118518. [Google Scholar] [CrossRef] [PubMed]
- Liu, F.-r.; Jin, H.; Wang, Y.; Chen, C.; Li, M.; Mao, S.-j.; Wang, Q.; Li, H. Anti-CD123 antibody-modified niosomes for targeted delivery of daunorubicin against acute myeloid leukemia. Drug Deliv. 2017, 24, 882–890. [Google Scholar] [CrossRef] [Green Version]
- Demir, B.; Moulahoum, H.; Ghorbanizamani, F.; Barlas, F.B.; Yesiltepe, O.; Gumus, Z.P.; Meral, K.; Demirkol, D.O.; Timur, S. Carbon Dots and Curcumin-Loaded CD44-Targeted Liposomes for Imaging and Tracking Cancer Chemotherapy: A Multi-Purpose Tool for Theranostics. J. Drug Deliv. Sci. Technol. 2021, 62, 102363. [Google Scholar] [CrossRef]
- Kullberg, M.; Francian, A.; Arabi, A.; Olsson, T.; Mann, K.; Martinson, H. Liposome Delivery of Natural STAT3 Inhibitors for the Treatment of Cancer. Pharm. Front. 2019, 1, e190007. [Google Scholar]
- Zhen, S.; Li, X. Liposomal delivery of CRISPR/Cas9. Cancer Gene Ther. 2020, 27, 515–527. [Google Scholar] [CrossRef]
- Ross, C.; Taylor, M.; Fullwood, N.; Allsop, D. Liposome delivery systems for the treatment of Alzheimer’s disease. Int. J. Nanomed. 2018, 13, 8507–8522. [Google Scholar] [CrossRef] [Green Version]
- Koshy, S.T.; Cheung, A.S.; Gu, L.; Graveline, A.R.; Mooney, D.J. Liposomal Delivery Enhances Immune Activation by STING Agonists for Cancer Immunotherapy. Adv. Biosyst. 2017, 1, 1600013. [Google Scholar] [CrossRef]
- Shrestha, I.; Choi, J.-S.; Bae, Y.-U.; Doh, K.-O. Enhancement of Liposomal Plasmid DNA and siRNA Delivery by Itraconazole through Intracellular Cholesterol Accumulation. Pharm. Res. 2020, 37, 126. [Google Scholar] [CrossRef]
- Balazs, D.A.; Godbey, W. Liposomes for Use in Gene Delivery. J. Drug Deliv. 2011, 2011, 326497. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hussain, Z.; Rahim, M.A.; Jan, N.; Shah, H.; Rawas-Qalaji, M.; Khan, S.; Sohail, M.; Thu, H.E.; Ramli, N.A.; Sarfraz, R.M.; et al. Cell membrane cloaked nanomedicines for bio-imaging and immunotherapy of cancer: Improved pharmacokinetics, cell internalization and anticancer efficacy. J. Control. Release 2021, 335, 130–157. [Google Scholar] [CrossRef]
- Tezel, G.; Timur, S.S.; Kuralay, F.; Gürsoy, R.N.; Ulubayram, K.; Öner, L.; Eroğlu, H. Current status of micro/nanomotors in drug delivery. J. Drug Target. 2020, 29, 29–45. [Google Scholar] [CrossRef]
- Fang, R.H.; Kroll, A.V.; Gao, W.; Zhang, L. Cell Membrane Coating Nanotechnology. Adv. Mater. 2018, 30, 1706759. [Google Scholar] [CrossRef] [PubMed]
- Xia, Q.; Zhang, Y.; Li, Z.; Hou, X.; Feng, N. Red blood cell membrane-camouflaged nanoparticles: A novel drug delivery system for antitumor application. Acta Pharm. Sin. B 2019, 9, 675–689. [Google Scholar] [CrossRef]
- Oroojalian, F.; Beygi, M.; Baradaran, B.; Mokhtarzadeh, A.; Shahbazi, M. Immune Cell Membrane-Coated Biomimetic Nanoparticles for Targeted Cancer Therapy. Small 2021, 17, 2006484. [Google Scholar] [CrossRef] [PubMed]
- Hu, C.-M.J.; Fang, R.H.; Wang, K.-C.; Luk, B.T.; Thamphiwatana, S.; Dehaini, D.; Nguyen, P.; Angsantikul, P.; Wen, C.H.; Kroll, A.V.; et al. Nanoparticle biointerfacing by platelet membrane cloaking. Nature 2015, 526, 118–121. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.; Xin, Y.; Cao, H.; Li, W.; Hua, Y.; Webster, T.J.; Zhang, C.; Tang, W.; Liu, Z. Recent advances in mesenchymal stem cell membrane-coated nanoparticles for enhanced drug delivery. Biomater. Sci. 2021, 9, 1088–1103. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, K.; Li, T.; Maruf, A.; Qin, X.; Luo, L.; Zhong, Y.; Qiu, J.; McGinty, S.; Pontrelli, G.; et al. Macrophage membrane functionalized biomimetic nanoparticles for targeted anti-atherosclerosis applications. Theranostics 2021, 11, 164–180. [Google Scholar] [CrossRef]
- Jin, J.; Bhujwalla, Z.M. Biomimetic Nanoparticles Camouflaged in Cancer Cell Membranes and Their Applications in Cancer Theranostics. Front. Oncol. 2020, 9, 1560. [Google Scholar] [CrossRef] [Green Version]
- Xuan, M.; Shao, J.; Dai, L.; He, Q.; Li, J. Macrophage Cell Membrane Camouflaged Mesoporous Silica Nanocapsules for In Vivo Cancer Therapy. Adv. Health Mater. 2015, 4, 1645–1652. [Google Scholar] [CrossRef]
- Xuan, M.; Shao, J.; Dai, L.; Li, J.; He, Q. Macrophage Cell Membrane Camouflaged Au Nanoshells for in Vivo Prolonged Circulation Life and Enhanced Cancer Photothermal Therapy. ACS Appl. Mater. Interfaces 2016, 8, 9610–9618. [Google Scholar] [CrossRef]
- Wang, C.; Ye, M.; Cheng, L.; Li, R.; Zhu, W.; Shi, Z.; Fan, C.; He, J.; Liu, J.; Liu, Z. Simultaneous isolation and detection of circulating tumor cells with a microfluidic silicon-nanowire-array integrated with magnetic upconversion nanoprobes. Biomaterials 2015, 54, 55–62. [Google Scholar] [CrossRef]
- Fu, J.; Wang, D.; Mei, D.; Zhang, H.; Wang, Z.; He, B.; Dai, W.; Zhang, H.; Wang, X.; Zhang, Q. Macrophage mediated biomimetic delivery system for the treatment of lung metastasis of breast cancer. J. Control. Release 2015, 204, 11–19. [Google Scholar] [CrossRef]
- Cao, H.; Dan, Z.; He, X.; Zhang, Z.; Yu, H.; Yin, Q.; Li, Y. Liposomes Coated with Isolated Macrophage Membrane Can Target Lung Metastasis of Breast Cancer. ACS Nano 2016, 10, 7738–7748. [Google Scholar] [CrossRef] [PubMed]
- Zhu, C.; Ma, J.; Ji, Z.; Shen, J.; Wang, Q. Recent Advances of Cell Membrane Coated Nanoparticles in Treating Cardiovascular Disorders. Molecules 2021, 26, 3428. [Google Scholar] [CrossRef] [PubMed]
- Sun, T.; Kwong, C.H.; Gao, C.; Wei, J.; Yue, L.; Zhang, J.; Ye, R.D.; Wang, R. Amelioration of ulcerative colitis via inflammatory regulation by macrophage-biomimetic nanomedicine. Theranostics 2020, 10, 10106–10119. [Google Scholar] [CrossRef]
- Zhang, Q.; Zhou, J.L.; Zhou, J.R.; Fang, R.H.; Gao, W.; Zhang, L. Lure-and-kill macrophage nanoparticles alleviate the severity of experimental acute pancreatitis. NaTure Commun. 2021, 12, 4136. [Google Scholar] [CrossRef]
- Xue, Y.; Zeng, G.; Cheng, J.; Hu, J.; Zhang, M.; Li, Y. Engineered macrophage membrane-enveloped nanomedicine for ameliorating myocardial infarction in a mouse model. Bioeng. Transl. Med. 2021, 6, e10197. [Google Scholar] [CrossRef]
- Hu, C.-M.J.; Zhang, L.; Aryal, S.; Cheung, C.; Fang, R.H. Erythrocyte membrane-camouflaged polymeric nanoparticles as a biomimetic delivery platform. Proc. Natl. Acad. Sci. USA 2011, 108, 10980–10985. [Google Scholar] [CrossRef] [Green Version]
- Rao, L.; Xu, J.-H.; Cai, B.; Liu, H.; Li, M.; Jia, Y.; Xiao, L.; Guo, S.-S.; Liu, W.; Zhao, X.-Z. Synthetic nanoparticles camouflaged with biomimetic erythrocyte membranes for reduced reticuloendothelial system uptake. Nanotechnology 2016, 27, 085106. [Google Scholar] [CrossRef]
- Piao, J.-G.; Wang, L.; Gao, F.; You, Y.-Z.; Xiong, Y.; Yang, L. Erythrocyte Membrane Is an Alternative Coating to Polyethylene Glycol for Prolonging the Circulation Lifetime of Gold Nanocages for Photothermal Therapy. ACS Nano 2014, 8, 10414–10425. [Google Scholar] [CrossRef]
- Lu, B.; Hu, E.; Xie, R.; Yu, K.; Lu, F.; Bao, R.; Wang, C.; Lan, G.; Dai, F. Magnetically Guided Nanoworms for Precise Delivery to Enhance In Situ Production of Nitric Oxide to Combat Focal Bacterial Infection In Vivo. ACS Appl. Mater. Interfaces 2021, 13, 22225–22239. [Google Scholar] [CrossRef]
- Liang, X.; Ye, X.; Wang, C.; Xing, C.; Miao, Q.; Xie, Z.; Chen, X.; Zhang, X.; Zhang, H.; Mei, L. Photothermal cancer immunotherapy by erythrocyte membrane-coated black phosphorus formulation. J. Control. Release 2019, 296, 150–161. [Google Scholar] [CrossRef]
- Shao, J.; Abdelghani, M.; Shen, G.; Cao, S.; Williams, D.S.; van Hest, J.C.M. Erythrocyte Membrane Modified Janus Polymeric Motors for Thrombus Therapy. ACS Nano 2018, 12, 4877–4885. [Google Scholar] [CrossRef]
- Chen, Y.; Li, Y.; Liu, J.; Zhu, Q.; Ma, J.; Zhu, X. Erythrocyte membrane bioengineered nanoprobes via indocyanine green-directed assembly for single NIR laser-induced efficient photodynamic/photothermal theranostics. J. Control. Release 2021, 335, 345–358. [Google Scholar] [CrossRef]
- Wang, H.; Wu, J.; Williams, G.R.; Fan, Q.; Niu, S.; Wu, J.; Xie, X.; Zhu, L.-M. Platelet-membrane-biomimetic nanoparticles for targeted antitumor drug delivery. J. Nanobio Technol. 2019, 17, 60. [Google Scholar] [CrossRef]
- Xu, J.; Zhang, Y.; Xu, J.; Liu, G.; Di, C.; Zhao, X.; Li, X.; Li, Y.; Pang, N.; Yang, C.; et al. Engineered Nanoplatelets for Targeted Delivery of Plasminogen Activators to Reverse Thrombus in Multiple Mouse Thrombosis Models. Adv. Mater. 2020, 32, 1905145. [Google Scholar] [CrossRef]
- Chen, H.-A.; Ma, Y.-H.; Hsu, T.-Y.; Chen, J.-P. Preparation of Peptide and Recombinant Tissue Plasminogen Activator Conjugated Poly(Lactic-Co-Glycolic Acid) (PLGA) Magnetic Nanoparticles for Dual Targeted Thrombolytic Therapy. Int. J. Mol. Sci. 2020, 21, 2690. [Google Scholar] [CrossRef] [Green Version]
- Li, M.; Li, J.; Chen, J.; Liu, Y.; Cheng, X.; Yang, F.; Gu, N. Platelet Membrane Biomimetic Magnetic Nanocarriers for Targeted Delivery and in Situ Generation of Nitric Oxide in Early Ischemic Stroke. ACS Nano 2020, 14, 2024–2035. [Google Scholar] [CrossRef]
- Zhou, M.; Lai, W.; Li, G.; Wang, F.; Liu, W.; Liao, J.; Yang, H.; Liu, Y.; Zhang, Q.; Tang, Q.; et al. Platelet Membrane-Coated and VAR2CSA Malaria Protein-Functionalized Nanoparticles for Targeted Treatment of Primary and Metastatic Cancer. ACS Appl. Mater. Interfaces 2021, 13, 25635–25648. [Google Scholar] [CrossRef]
- Song, Y.; Zhang, N.; Li, Q.; Chen, J.; Wang, Q.; Yang, H.; Tan, H.; Gao, J.; Dong, Z.; Pang, Z.; et al. Biomimetic liposomes hybrid with platelet membranes for targeted therapy of atherosclerosis. Chem. Eng. J. 2021, 408, 127296. [Google Scholar] [CrossRef]
- Xu, L.; Gao, F.; Fan, F.; Yang, L. Platelet membrane coating coupled with solar irradiation endows a photodynamic nanosystem with both improved antitumor efficacy and undetectable skin damage. Biomaterials 2018, 159, 59–67. [Google Scholar] [CrossRef]
- Gao, C.; Lin, Z.; Jurado-Sánchez, B.; Lin, X.; Wu, Z.; He, Q. Stem Cell Membrane-Coated Nanogels for Highly Efficient In Vivo Tumor Targeted Drug Delivery. Small 2016, 12, 4056–4062. [Google Scholar] [CrossRef]
- Zhang, X.; Chen, J.; Jiang, Q.; Ding, X.; Li, Y.; Chen, C.; Yang, W.; Chen, S. Highly biosafe biomimetic stem cell membrane-disguised nanovehicles for cartilage regeneration. J. Mater. Chem. B 2020, 8, 8884–8893. [Google Scholar] [CrossRef]
- Gao, C.; Lin, Z.; Wu, Z.; Lin, X.; He, Q. Stem-Cell-Membrane Camouflaging on Near-Infrared Photoactivated Upconversion Nanoarchitectures for in Vivo Remote-Controlled Photodynamic Therapy. ACS Appl. Mater. Interfaces 2016, 8, 34252–34260. [Google Scholar] [CrossRef]
- Wang, S.; Jiang, R.; Meng, T.; Zhang, F.; Li, J.; Jin, Y.; Lee, J.; Zhu, M.; Jiang, J. Stem cell membrane-coated isotretinoin for acne treatment. J. Nanobio Technol. 2020, 18, 1–12. [Google Scholar] [CrossRef]
- Li, S.-Y.; Cheng, H.; Xie, B.-R.; Qiu, W.-X.; Zeng, J.-Y.; Li, C.-X.; Wan, S.-S.; Zhang, L.; Liu, W.-L.; Zhang, X.-Z. Cancer Cell Membrane Camouflaged Cascade Bioreactor for Cancer Targeted Starvation and Photodynamic Therapy. ACS Nano 2017, 11, 7006–7018. [Google Scholar] [CrossRef] [PubMed]
- Fang, H.; Li, M.; Liu, Q.; Gai, Y.; Yuan, L.; Wang, S.; Zhang, X.; Ye, M.; Zhang, Y.; Gao, M.; et al. Ultra-sensitive Nanoprobe Modified with Tumor Cell Membrane for UCL/MRI/PET Multimodality Precise Imaging of Triple-Negative Breast Cancer. Nano-Micro Lett. 2020, 12, 62. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ding, Y.; Zhu, Y.; Wei, S.; Zhou, J.; Shen, J. Cancer cell membrane as gate keeper of mesoporous silica nanoparticles and photothermal-triggered membrane fusion to release the encapsulated anticancer drug. J. Mater. Sci. 2019, 54, 12794–12805. [Google Scholar] [CrossRef]
- Pan, W.; Ge, Y.; Yu, Z.; Zhou, P.; Cui, B.; Li, N.; Tang, B. A cancer cell membrane-encapsulated MnO2 nanoreactor for combined photodynamic-starvation therapy. Chem. Commun. 2019, 55, 5115–5118. [Google Scholar] [CrossRef]
- Kroll, A.V.; Fang, R.H.; Jiang, Y.; Zhou, J.; Wei, X.; Yu, C.L.; Gao, J.; Luk, B.T.; Dehaini, D.; Gao, W.; et al. Nanoparticulate Delivery of Cancer Cell Membrane Elicits Multiantigenic Antitumor Immunity. Adv. Mater. 2017, 29, 1703969. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Wang, Y.; Ding, Y.; Repp, L.; Kwon, G.S.; Hu, Q. Cell-Based Delivery Systems: Emerging Carriers for Immunotherapy. Adv. Funct. Mater. 2021, 31, 2100088. [Google Scholar] [CrossRef]
- Raza, A.; Rasheed, T.; Nabeel, F.; Hayat, U.; Bilal, M.; Iqbal, H.M.N. Endogenous and Exogenous Stimuli-Responsive Drug Delivery Systems for Programmed Site-Specific Release. Molecules 2019, 24, 1117. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, H.Y.; Kumar, H.; Jo, M.-J.; Kim, J.; Yoon, J.-K.; Lee, J.-R.; Kang, M.; Choo, Y.W.; Song, S.Y.; Kwon, S.P.; et al. Therapeutic Efficacy-Potentiated and Diseased Organ-Targeting Nanovesicles Derived from Mesenchymal Stem Cells for Spinal Cord Injury Treatment. Nano Lett. 2018, 18, 4965–4975. [Google Scholar] [CrossRef]
- Huang, Y.; Guan, Z.; Dai, X.; Shen, Y.; Wei, Q.; Ren, L.; Jiang, J.; Xiao, Z.; Jiang, Y.; Liu, D.; et al. Engineered macrophages as near-infrared light activated drug vectors for chemo-photodynamic therapy of primary and bone metastatic breast cancer. Nat. Commun. 2021, 12, 4310. [Google Scholar] [CrossRef]
- Mai, T.D.; D’Orlyé, F.; Ménager, C.; Varenne, A.; Siaugue, J.-M. Red blood cells decorated with functionalized core–shell magnetic nanoparticles: Elucidation of the adsorption mechanism. Chem. Commun. 2013, 49, 5393–5395. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Li, Y.; Toraldo, G.; Li, A.; Yang, X.; Zhang, H.; Qian, W.-P.; Weitzmann, M.N. B cells and T cells are critical for the preservation of bone homeostasis and attainment of peak bone mass in vivo. Blood 2007, 109, 3839–3848. [Google Scholar] [CrossRef] [Green Version]
- Mura, S.; Nicolas, J.; Couvreur, P. Stimuli-responsive nanocarriers for drug delivery. Nat. Mater. 2013, 12, 991–1003. [Google Scholar] [CrossRef]
- Hata, T.; Kita, T.; Yoneda, R.; Tanada, S. Effects of exogenous stimuli and centrally acting drugs on galvanic skin responses in rats. Jpn. J. Pharmacol. 1981, 31, 23–31. [Google Scholar] [CrossRef]
- Antonelli, A.; Sfara, C.; Manuali, E.; Bruce, I.J.; Magnani, M. Encapsulation of superparamagnetic nanoparticles into red blood cells as new carriers of MRI contrast agents. Nanomedicine 2011, 6, 211–223. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H. Erythrocytes in nanomedicine: An optimal blend of natural and synthetic materials. Biomater. Sci. 2016, 4, 1024–1031. [Google Scholar] [CrossRef]
- Wu, Y.; Song, Z.; Wang, H.; Han, H. Endogenous stimulus-powered antibiotic release from nanoreactors for a combination therapy of bacterial infections. Nat. Commun. 2019, 10, 4464. [Google Scholar] [CrossRef]
- Wang, X.; Han, J.-N.; Zhang, X.; Ma, Y.-Y.; Lin, Y.; Wang, H.; Li, D.-J.; Zheng, T.-R.; Wu, F.-Q.; Ye, J.-W.; et al. Reversible thermal regulation for bifunctional dynamic control of gene expression in Escherichia coli. Nat. Commun. 2021, 12, 1411. [Google Scholar] [CrossRef]
- Cheng, X.; Sun, R.; Yin, L.; Chai, Z.; Shi, H.; Gao, M. Light-Triggered Assembly of Gold Nanoparticles for Photothermal Therapy and Photoacoustic Imaging of Tumors In Vivo. Adv. Mater. 2017, 29, 1604894. [Google Scholar] [CrossRef]
- Qiu, Y.; Park, K. Environment-sensitive hydrogels for drug delivery. Adv. Drug Deliv. Rev. 2001, 53, 321–339. [Google Scholar] [CrossRef]
- Jeong, B.; Kim, S.W.; Bae, Y.H. Thermosensitive sol–gel reversible hydrogels. Adv. Drug Deliv. Rev. 2012, 64, 154–162. [Google Scholar] [CrossRef]
- Guo, W.; Lu, C.-H.; Orbach, R.; Wang, F.; Qi, X.-J.; Cecconello, A.; Seliktar, D.; Willner, I. pH-Stimulated DNA Hydrogels Exhibiting Shape-Memory Properties. Adv. Mater. 2015, 27, 73–78. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.S.; Liu, M.; Ishida, Y.; Ebina, Y.; Osada, M.; Sasaki, T.; Hikima, T.; Takata, M.; Aida, T. Thermoresponsive actuation enabled by permittivity switching in an electrostatically anisotropic hydrogel. Nat. Mater. 2015, 14, 1002–1007. [Google Scholar] [CrossRef] [PubMed]
- Ji, W.; Wu, Q.; Han, X.; Zhang, W.; Wei, W.; Chen, L.; Li, L.; Huang, W. Photosensitive hydrogels: From structure, mechanisms, design to bioapplications. Sci. China Life Sci. 2020, 63, 1813–1828. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Liu, J.; Cui, X.; Wang, X.; Zhang, L.; Tang, P. Recent Advances on Magnetic Sensitive Hydrogels in Tissue Engineering. Front. Chem. 2020, 8, 124. [Google Scholar] [CrossRef]
- Guidotti, G.; Brambilla, L.; Rossi, D. Cell-Penetrating Peptides: From Basic Research to Clinics. Trends Pharmacol. Sci. 2017, 38, 406–424. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.-M.; Kucinic, A.; Johnson, J.A.; Su, H.-J.; Castro, C.E. Integrated computeraided engineering and design for DNA assemblies. Nat. Mater. 2021, 1–8. [Google Scholar] [CrossRef]
- Föller, M.; Huber, S.M.; Lang, F. Erythrocyte programmed cell death. IUBMB Life 2008, 60, 661–668. [Google Scholar] [CrossRef] [PubMed]
- Pierigè, F.; Serafini, S.; Rossi, L.; Magnani, M. Cell-based drug delivery. Adv. Drug Deliv. Rev. 2008, 60, 286–295. [Google Scholar] [CrossRef]
- Oldenborg, P.-A.; Zheleznyak, A.; Fang, Y.-F.; Lagenaur, C.F.; Gresham, H.D.; Lindberg, F.P. Role of CD47 as a Marker of Self on Red Blood Cells. Science 2000, 288, 2051–2054. [Google Scholar] [CrossRef]
- Fang, R.H.; Hu, C.-M.J.; Chen, K.N.H.; Luk, B.T.; Carpenter, C.W.; Gao, W.; Li, S.; Zhang, D.-E.; Lu, W.; Zhang, L. Lipid-insertion enables targeting functionalization of erythrocyte membrane-cloaked nanoparticles. Nanoscale 2013, 5, 8884–8888. [Google Scholar] [CrossRef] [Green Version]
- Ye, S.; Wang, F.; Fan, Z.; Zhu, Q.; Tian, H.; Zhang, Y.; Jiang, B.; Hou, Z.; Li, Y.; Su, G. Light/pH-Triggered Biomimetic Red Blood Cell Membranes Camouflaged Small Molecular Drug Assemblies for Imaging-Guided Combinational Chemo-Photothermal Therapy. ACS Appl. Mater. Interfaces 2019, 11, 15262–15275. [Google Scholar] [CrossRef] [PubMed]
- Wagner, D.D.; Burger, P.C. Platelets in Inflammation and Thrombosis. Arter. Thromb. Vasc. Biol. 2003, 23, 2131–2137. [Google Scholar] [CrossRef]
- Gay, L.J.; Felding-Habermann, B. Contribution of platelets to tumour metastasis. Nat. Rev. Cancer 2011, 11, 123–134. [Google Scholar] [CrossRef] [PubMed]
- Song, Y.; Huang, Z.; Liu, X.; Pang, Z.; Chen, J.; Yang, H.; Zhang, N.; Cao, Z.; Liu, M.; Cao, J.; et al. Platelet membrane-coated nanoparticle-mediated targeting delivery of Rapamycin blocks atherosclerotic plaque development and stabilizes plaque in apolipoprotein E-deficient (ApoE(-/-)) mice. Nanomedicine 2019, 15, 13–24. [Google Scholar] [CrossRef] [PubMed]
- Su, T.; Huang, K.; Ma, H.; Liang, H.; Dinh, P.U.; Chen, J.; Shen, D.; Allen, T.A.; Qiao, L.; Li, Z.; et al. Platelet-Inspired Nanocells for Targeted Heart Repair After Ischemia/Reperfusion Injury. Adv. Funct. Mater. 2019, 29, 1803567. [Google Scholar] [CrossRef]
- Hanahan, D.; Weinberg, R.A. Hallmarks of Cancer: The Next Generation. Cell 2011, 144, 646–674. [Google Scholar] [CrossRef] [Green Version]
- Sherr, C.J. Cancer cell cycles. Science 1996, 274, 1672–1677. [Google Scholar] [CrossRef] [Green Version]
- Choi, B.; Park, W.; Park, S.-B.; Rhim, W.-K.; Han, D.K. Recent trends in cell membrane-cloaked nanoparticles for therapeutic applications. Methods 2020, 177, 2–14. [Google Scholar] [CrossRef]
- Liu, C.M.; Chen, G.B.; Chen, H.H.; Zhang, J.B.; Li, H.Z.; Sheng, M.X.; Weng, W.B.; Guo, S.M. Cancer cell membrane-cloaked mesoporous silica nanoparticles with a pH-sensitive gatekeeper for cancer treatment. Colloids Surf. B Biointerfaces 2019, 175, 477–486. [Google Scholar] [CrossRef]
- Meng, X.; Wang, J.; Zhou, J.; Tian, Q.; Qie, B.; Zhou, G.; Duan, W.; Zhu, Y. Tumor cell membrane-based peptide delivery system targeting the tumor microenvironment for cancer immunotherapy and diagnosis. Acta Biomater. 2021, 127, 266–275. [Google Scholar] [CrossRef]
- Zhang, Y.; He, Z.; Li, Y.; Xia, Q.; Li, Z.; Hou, X.; Feng, N. Tumor cell membrane-derived nano-Trojan horses encapsulating phototherapy and chemotherapy are accepted by homologous tumor cells. Mater. Sci. Eng. C 2021, 120, 111670. [Google Scholar] [CrossRef]
- Rudolph, M.G.; Stanfield, R.L.; Wilson, I.A. How TCRs bind MHCs, peptides, and coreceptors. Annu. Rev. Immunol. 2006, 24, 419–466. [Google Scholar] [CrossRef]
- Yhee, J.Y.; Lee, S.; Kim, K. Advances in targeting strategies for nanoparticles in cancer imaging and therapy. Nanoscale 2014, 6, 13383–13390. [Google Scholar] [CrossRef]
- Swierczak, A.; Mouchemore, K.; Hamilton, J.A.; Anderson, R.L. Neutrophils: Important contributors to tumor progression and metastasis. Cancer Metastasis Rev. 2015, 34, 735–751. [Google Scholar] [CrossRef] [PubMed]
- Parodi, A.; Quattrocchi, N.; Van De Ven, A.L.; Chiappini, C.; Evangelopoulos, M.; Martinez, J.; Brown, B.S.; Khaled, S.Z.; Yazdi, I.; Enzo, M.V.; et al. Synthetic nanoparticles functionalized with biomimetic leukocyte membranes possess cell-like functions. Nat. Nanotechnol. 2013, 8, 61–68. [Google Scholar] [CrossRef] [Green Version]
- Wang, Q.; Ren, Y.; Mu, J.; Egilmez, N.K.; Zhuang, X.; Deng, Z.; Zhang, L.; Yan, J.; Miller, D.; Zhang, H.G. Grapefruit-Derived Nanovectors Use an Activated Leukocyte Trafficking Pathway to Deliver Therapeu-tic Agents to Inflammatory Tumor Sites. Cancer Res. 2015, 75, 2520–2529. [Google Scholar] [CrossRef] [Green Version]
- Greene, J.M.; Wiseman, R.W.; Lank, S.M.; Bimber, B.N.; Karl, J.A.; Burwitz, B.J.; Lhost, J.J.; Hawkins, O.E.; Kunstman, K.J.; Broman, K.W.; et al. Differential MHC class I expression in distinct leukocyte subsets. BMC Immunol. 2011, 12, 39. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Avila, B.E.-F.D.; Angsantikul, P.; Ramirez-Herrera, D.E.; Soto, F.; Teymourian, H.; Dehaini, D.; Chen, Y.; Zhang, L.; Wang, J. Hybrid biomembrane-functionalized nanorobots for concurrent removal of pathogenic bacteria and toxins. Sci. Robot. 2018, 3. [Google Scholar] [CrossRef] [Green Version]
- Sun, M.; Duan, Y.; Ma, Y.; Zhang, Q. Cancer Cell-Erythrocyte Hybrid Membrane Coated Gold Nanocages for Near Infrared Light-Activated Photothermal/Radio/Chemotherapy of Breast Cancer. Int. J. Nanomed. 2020, 15, 6749–6760. [Google Scholar] [CrossRef]
- Huang, C.; Hsu, S.-P.; Chen, Y.-R. Systematic review of the surgery-first approach in orthognathic surgery. Biomed. J. 2014, 37, 184. [Google Scholar] [CrossRef]
- Forbes, N.S. Engineering the perfect (bacterial) cancer therapy. Nat. Rev. Cancer 2010, 10, 785–794. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sowa, Y.; Rowe, A.D.; Leake, M.; Yakushi, T.; Homma, M.; Ishijima, A.; Berry, R.M. Direct observation of steps in rotation of the bacterial flagellar motor. Nature 2005, 437, 916–919. [Google Scholar] [CrossRef] [PubMed]
- Martel, S. Bacterial microsystems and microrobots. Biomed. Microdevices 2012, 14, 1033–1045. [Google Scholar] [CrossRef]
- Goldstein, R.A.; Soyer, O.S. Evolution of Taxis Responses in Virtual Bacteria: Non-Adaptive Dynamics. PLoS Comput. Biol. 2008, 4, e1000084. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Taylor, B.L.; Zhulin, I.B.; Johnson, M.S. Aerotaxis and Other Energy-Sensing Behavior in Bacteria. Annu. Rev. Microbiol. 1999, 53, 103–128. [Google Scholar] [CrossRef]
- Grüll, H.; Langereis, S. Hyperthermia-triggered drug delivery from temperature-sensitive liposomes using MRI-guided high intensity focused ultrasound. J. Control. Release 2012, 161, 317–327. [Google Scholar] [CrossRef]
- Mathieu, J.-B.; Martel, S. Steering of aggregating magnetic microparticles using propulsion gradients coils in an MRI Scanner. Magn. Reson. Med. 2010, 63, 1336–1345. [Google Scholar] [CrossRef]
- Li, D.; Choi, H.; Cho, S.; Jeong, S.; Jin, Z.; Lee, C.; Ko, S.Y.; Park, J.-O.; Park, S. A hybrid actuated microrobot using an electromagnetic field and flagellated bacteria for tumor-targeting therapy. Biotechnol. Bioeng. 2015, 112, 1623–1631. [Google Scholar] [CrossRef]
- Mostaghaci, B.; Yasa, O.; Zhuang, J.; Sitti, M. Bioadhesive Bacterial Microswimmers for Targeted Drug Delivery in the Urinary and Gastroin-testinal Tracts. Adv. Sci. 2017, 4, 1700058. [Google Scholar] [CrossRef]
- Uthaman, S.; Zheng, S.; Han, J.; Choi, Y.J.; Cho, S.; Du Nguyen, V.; Park, J.-O.; Park, S.-H.; Min, J.-J.; Park, S.; et al. Preparation of Engineered Salmonella Typhimurium-Driven Hyaluronic-Acid-Based Microbeads with Both Chemotactic and Biological Targeting Towards Breast Cancer Cells for Enhanced Anticancer Therapy. Adv. Health Mater. 2016, 5, 288–295. [Google Scholar] [CrossRef]
- Choi, J.; Kim, H.-Y.; Ju, E.J.; Jung, J.; Park, J.; Chung, H.-K.; Lee, J.S.; Lee, J.S.; Park, H.J.; Song, S.Y.; et al. Use of macrophages to deliver therapeutic and imaging contrast agents to tumors. Biomaterials 2012, 33, 4195–4203. [Google Scholar] [CrossRef]
- Choi, M.-R.; Stanton-Maxey, K.J.; Stanley, J.K.; Levin, C.S.; Bardhan, R.; Akin, D.; Badve, S.; Sturgis, J.; Robinson, J.P.; Bashir, R.; et al. A Cellular Trojan Horse for Delivery of Therapeutic Nanoparticles into Tumors. Nano Lett. 2007, 7, 3759–3765. [Google Scholar] [CrossRef]
- Li, Z.; Huang, H.; Tang, S.; Li, Y.; Yu, X.-F.; Wang, H.; Li, P.; Sun, Z.; Zhang, H.; Liu, C.; et al. Small gold nanorods laden macrophages for enhanced tumor coverage in photothermal therapy. Biomaterials 2016, 74, 144–154. [Google Scholar] [CrossRef] [PubMed]
- Dai, Y.; Chen, Y.; Feng, Y.; Chen, D.; Feng, L. Magnetized Cell-robot Propelled by Regular Tetrahedron Magnetic Actuation System. In Proceedings of the 2019 International Symposium on Micro-NanoMechatronics and Human Science (MHS), Nagoya, Japan, 1–4 December 2019. [Google Scholar]
- Dai, Y.; Feng, Y.; Feng, L.; Chen, Y.; Arai, F. Magnetized Cell-robot Propelled by Magnetic Field for Cancer Killing. In Proceedings of the 2020 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Las Vegas, NV, USA, 25–29 October 2020. [Google Scholar]
- Nguyen, V.D.; Han, J.; Go, G.; Zheng, S.; Le, V.H.; Park, J.O.; Park, S. Feasibility study of dual-targeting paclitaxel-loaded magnetic liposomes using electromagnetic actu-ation and macrophages. Sens. Actuators B-Chem. 2017, 240, 1226–1236. [Google Scholar] [CrossRef]
- Papayannopoulos, V. Neutrophil extracellular traps in immunity and disease. Nat. Rev. Immunol. 2018, 18, 134–147. [Google Scholar] [CrossRef]
- Jorch, S.K.; Kubes, P. An emerging role for neutrophil extracellular traps in noninfectious disease. Nat. Med. 2017, 23, 279–287. [Google Scholar] [CrossRef]
- Oliveira, S.D.; Rosowski, E.E.; Huttenlocher, A. Neutrophil migration in infection and wound repair: Going forward in reverse. Nat. Rev. Immunol. 2016, 16, 378–391. [Google Scholar] [CrossRef] [Green Version]
- Oliveira, T.H.C.; Marques, P.E.; Proost, P.; Teixeira, M.M.M. Neutrophils: A cornerstone of liver ischemia and reperfusion injury. Lab. Invest. 2018, 98, 51–62. [Google Scholar] [CrossRef] [Green Version]
- Tang, C.; Wang, C.; Zhang, Y.; Xue, L.; Li, Y.; Ju, C.; Zhang, C. Recognition, Intervention, and Monitoring of Neutrophils in Acute Ischemic Stroke. Nano Lett. 2019, 19, 4470–4477. [Google Scholar] [CrossRef] [PubMed]
- Xue, J.; Zhao, Z.; Zhang, L.; Xue, L.; Shen, S.; Wen, Y.; Wei, Z.; Wang, L.; Kong, L.; Sun, H.; et al. Neutrophil-mediated anticancer drug delivery for suppression of postoperative malignant glioma recur-rence. Nat. Nanotechnol. 2017, 12, 692–700. [Google Scholar] [CrossRef] [PubMed]
- Chu, D.; Dong, X.; Shi, X.; Zhang, C.Y.; Wang, Z. Neutrophil-Based Drug Delivery Systems. Adv. Mater. 2018, 30, e1706245. [Google Scholar] [CrossRef]
- Zhang, H.; Li, Z.; Gao, C.; Fan, X.; Pang, Y.; Li, T.; Wu, Z.; Xie, H.; He, Q. Dual-responsive biohybrid neutrobots for active target delivery. Sci. Robot. 2021, 6. [Google Scholar] [CrossRef]
- Oltolina, F.; Peigneux, A.; Colangelo, D.; Clemente, N.; D’Urso, A.; Valente, G.; Iglesias, G.R.; Jiménez-Lopez, C.; Prat, M. Biomimetic Magnetite Nanoparticles as Targeted Drug Nanocarriers and Mediators of Hyper-thermia in an Experimental Cancer Model. Cancers 2020, 12, 2564. [Google Scholar] [CrossRef]
- Vurro, F.; Jabalera, Y.; Mannucci, S.; Glorani, G.; Sola-Leyva, A.; Gerosa, M.; Romeo, A.; Romanelli, M.; Malatesta, M.; Calderan, L.; et al. Improving the Cellular Uptake of Biomimetic Magnetic Nanoparticles. Nanomaterials 2021, 11, 766. [Google Scholar] [CrossRef] [PubMed]
- Jabalera, Y.; Sola-Leyva, A.; Carrasco-Jimenez, M.P.; Iglesias, G.R.; Jimenez-Lopez, C. Synergistic Photothermal-Chemotherapy Based on the Use of Biomimetic Magnetic Nanopar-ticles. Pharmaceutics 2021, 13, 625. [Google Scholar] [CrossRef]
- Jabalera, Y.; Sola-Leyva, A.; Gaglio, S.; Carrasco-Jiménez, M.; Iglesias, G.; Perduca, M.; Jimenez-Lopez, C. Enhanced Cytotoxic Effect of TAT–PLGA-Embedded DOXO Carried by Biomimetic Magnetic Nanoparticles upon Combination with Magnetic Hyperthermia and Photothermia. Pharmaceutics 2021, 13, 1168. [Google Scholar] [CrossRef] [PubMed]
- Shen, S.; Wu, Y.; Liu, Y.; Wu, D. High drug-loading nanomedicines: Progress, current status, and prospects. Int. J. Nanomed. 2017, 12, 4085–4109. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Naz, S.; Shamoon, M.; Wang, R.; Zhang, L.; Zhou, J.; Chen, J. Advances in Therapeutic Implications of Inorganic Drug Delivery Nano-Platforms for Cancer. Int. J. Mol. Sci. 2019, 20, 965. [Google Scholar] [CrossRef] [Green Version]
- Casals, E.; Gusta, M.F.; Cobaleda-Siles, M.; Garcia-Sanz, A.; Puntes, V.F. Cancer resistance to treatment and antiresistance tools offered by multimodal multifunctional nano-particles. Cancer Nanotechnol. 2017, 8, 7. [Google Scholar] [CrossRef]
- Zhang, Y.F.; Fang, F.; Li, L.; Zhang, J.F. Self-Assembled Organic Nanomaterials for Drug Delivery, Bioimaging, and Cancer Therapy. Acs Biomater. Sci. Eng. 2020, 6, 4816–4833. [Google Scholar] [CrossRef] [PubMed]
- Karaosmanoglu, S.; Zhou, M.; Shi, B.; Zhang, X.; Williams, G.R.; Chen, X. Carrier-free nanodrugs for safe and effective cancer treatment. J. Control. Release 2021, 329, 805–832. [Google Scholar] [CrossRef]
- Li, Y.; Zhang, T.; Liu, Q.; He, J. PEG-Derivatized Dual-Functional Nanomicelles for Improved Cancer Therapy. Front. Pharmacol. 2019, 10, 808. [Google Scholar] [CrossRef] [Green Version]
- Zhai, C.; Liu, X.; Yuan, J.; Gao, Q. Synthesis, characterization, and drug delivery research of an amphiphilic biodegradable star-shaped block copolymer. Polym. Bull. 2013, 70, 419–429. [Google Scholar] [CrossRef]
- Hrdlička, L.; Šrámková, P.; Prousek, J.; Kronek, J. Environmental toxicity study of poly(2-oxazoline)s. Chem. Pap. 2018, 72, 1543–1547. [Google Scholar] [CrossRef]
- Lee, S.; Pham, T.C.; Bae, C.; Choi, Y.; Kim, Y.K.; Yoon, J. Nano theranostics platforms that utilize proteins. Co-Ord. Chem. Rev. 2020, 412, 213258. [Google Scholar] [CrossRef]
- Hao, L.Q.; Zhou, Q.; Piao, Y.; Zhou, Z.X.; Tang, J.B.; Shen, Y.Q. Albumin-binding prodrugs via reversible iminoboronate forming nanoparticles for cancer drug deliv-ery. J. Control. Release 2021, 330, 362–371. [Google Scholar] [CrossRef]
- He, W.; Yan, J.; Sui, F.; Wang, S.; Su, X.; Qu, Y.; Yang, Q.; Guo, H.; Ji, M.; Lu, W.; et al. Turning a Luffa Protein into a Self-Assembled Biodegradable Nanoplatform for Multitargeted Cancer Therapy. ACS Nano 2018, 12, 11664–11677. [Google Scholar] [CrossRef]
- He, L.; Mu, J.; Gang, O.; Chen, X. Rationally Programming Nanomaterials with DNA for Biomedical Applications. Adv. Sci. 2021, 8, 2003775. [Google Scholar] [CrossRef]
- Guo, S.; Vieweger, M.; Zhang, K.; Yin, H.; Wang, H.; Li, X.; Li, S.; Hu, S.; Sparreboom, A.; Evers, B.M.; et al. Ultra-thermostable RNA nanoparticles for solubilizing and high-yield loading of paclitaxel for breast cancer therapy. Nat. Commun. 2020, 11, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Huxford, R.C.; Della Rocca, J.; Lin, W. Metal–organic frameworks as potential drug carriers. Curr. Opin. Chem. Biol. 2010, 14, 262–268. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sun, Y.; Zheng, L.; Yang, Y.; Qian, X.; Fu, T.; Li, X.; Yang, Z.; Yan, H.; Cui, C.; Tan, W. Metal–Organic Framework Nanocarriers for Drug Delivery in Biomedical Applications. Nano-Micro Lett. 2020, 12, 1–29. [Google Scholar] [CrossRef] [PubMed]
- Ma, X.; Chai, Y.; Li, P.; Wang, B. Metal–Organic Framework Films and Their Potential Applications in Environmental Pollution Control. Acc. Chem. Res. 2019, 52, 1461–1470. [Google Scholar] [CrossRef]
- Yang, J.; Wang, H.; Liu, J.; Ding, M.; Xie, X.; Yang, X.; Peng, Y.; Zhou, S.; Ouyang, R.; Miao, Y. Recent advances in nanosized metal organic frameworks for drug delivery and tumor therapy. RSC Adv. 2021, 11, 3241–3263. [Google Scholar] [CrossRef]
- Chen, M.-L.; John, M.; Lee, S.L.; Tyner, K.M. Development Considerations for Nanocrystal Drug Products. AAPS J. 2017, 19, 642–651. [Google Scholar] [CrossRef]
- Gigliobianco, M.R.; Casadidio, C.; Censi, R.; Di Martino, P. Nanocrystals of Poorly Soluble Drugs: Drug Bioavailability and Physicochemical Stabil-ity. Pharmaceutics 2018, 10, 134. [Google Scholar] [CrossRef] [Green Version]
- Huang, P.; Wang, D.L.; Su, Y.; Huang, W.; Zhou, Y.F.; Cui, D.X.; Zhu, X.Y.; Yan, D.Y. Combination of Small Molecule Prodrug and Nanodrug Delivery: Amphiphilic Drug-Drug Conju-gate for Cancer Therapy. J. Am. Chem. Soc. 2014, 136, 11748–11756. [Google Scholar] [CrossRef] [PubMed]
- Sun, M.; Qian, Q.; Shi, L.; Xu, L.; Liu, Q.; Zhou, L.; Zhu, X.; Yue, J.-M.; Yan, D. Amphiphilic drug-drug conjugate for cancer therapy with combination of chemotherapeutic and antian-giogenesis drugs. Sci. China Chem. 2020, 63, 35–41. [Google Scholar] [CrossRef]
- Zhang, W.; He, H.; Tian, Y.; Li, H.; Lan, K.; Zu, L.; Xia, Y.; Duan, L.; Li, W.; Zhao, D. Defect-engineering of mesoporous TiO2 microspheres with phase junctions for efficient visible-light driven fuel production. Nano Energy 2019, 66, 104113. [Google Scholar] [CrossRef]
- Jiang, Q.; Song, C.; Nangreave, J.; Liu, X.; Lin, L.; Qiu, D.; Wang, Z.-G.; Zou, G.; Liang, X.; Yan, H.; et al. DNA Origami as a Carrier for Circumvention of Drug Resistance. J. Am. Chem. Soc. 2012, 134, 13396–13403. [Google Scholar] [CrossRef]
- Chen, Q.; Chen, Q.W.; Zhuang, C.; Tang, P.P.; Lin, N.; Wei, L.Q. Controlled release of drug molecules in metal-organic framework material HKUST-1. Inorg. Chem. Commun. 2017, 79, 78–81. [Google Scholar] [CrossRef]
- Ramsahye, N.; Trens, P.; Shepherd, C.; Gonzalez, P.; Trung, T.K.; Ragon, F.; Serre, C. The effect of pore shape on hydrocarbon selectivity on UiO-66(Zr), HKUST-1 and MIL-125(Ti) metal organic frameworks: Insights from molecular simulations and chromatography. Microporous Mesoporous Mater. 2014, 189, 222–231. [Google Scholar] [CrossRef]
- Cao, X.-X.; Liu, S.-L.; Lu, J.-S.; Zhang, Z.-W.; Wang, G.; Chen, Q.; Lin, N. Chitosan coated biocompatible zeolitic imidazolate framework ZIF-90 for targeted delivery of anticancer drug methotrexate. J. Solid State Chem. 2021, 300, 122259. [Google Scholar] [CrossRef]
- Chen, Y.; Zhang, F.F.; Wang, Y.; Yang, C.Y.; Yang, J.F.; Li, J.P. Recyclable ammonia uptake of a MIL series of metal-organic frameworks with high structural stabil-ity. Microporous Mesoporous Mater. 2018, 258, 170–177. [Google Scholar] [CrossRef]
- Vallet-Regi, M.; Rámila, A.; Del Real, R.P.; Perez-Pariente, J. A New Property of MCM-41: Drug Delivery System. Chem. Mater. 2001, 13, 308–311. [Google Scholar] [CrossRef]
- AbouAitah, K.; Lojkowski, W. Delivery of Natural Agents by Means of Mesoporous Silica Nanospheres as a Promising An-ticancer Strategy. Pharmaceutics 2021, 13, 143. [Google Scholar] [CrossRef]
- Barkat, A.; Beg, S.; Panda, S.K.; Alharbi, K.S.; Rahman, M.; Ahmed, F.J. Functionalized mesoporous silica nanoparticles in anticancer therapeutics. In Seminars in Cancer Biology; Elsevier: Amsterdam, The Netherlands, 2019. [Google Scholar]
- Peng, W.L.; Zhang, Z.P.; Rong, M.Z.; Zhang, M.Q. Core-Shell Structure Design of Hollow Mesoporous Silica Nanospheres Based on Thermo-Sensitive PNIPAM and pH-Responsive Catechol-Fe3+ Complex. Polymers 2019, 11, 1832. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ozcelik, N.; Yurtcan, A.B. Drug loading with supercritical carbon dioxide deposition on different silica derivatives: Carvedilol study. J. Drug Deliv. Sci. Technol. 2019, 53, 101213. [Google Scholar] [CrossRef]
- Andreani, T.; Miziara, L.; Lorenzon, E.N.; de Souza, A.L.R.; Kiill, C.P.; Fangueiro, J.F.; Garcia, M.L.; Gremiao, P.D.; Silva, A.M.; Souto, E.B. Effect of mucoadhesive polymers on the in vitro performance of insulin-loaded silica nanoparti-cles: Interactions with mucin and biomembrane models. Eur. J. Pharm. Biopharm. 2015, 93, 118–126. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Farooq, M.A.; Li, T.; Geng, T.; Kutoka, P.T.; Wang, B. Cationic chitosan-modified silica nanoparticles for oral delivery of protein vaccine. J. Biomed. Mater. Res. Part A 2021, 109, 2111–2119. [Google Scholar] [CrossRef]
- Lvov, Y.M.; Wang, W.; Zhang, L.; Fakhrullin, R.F. Halloysite Clay Nanotubes for Loading and Sustained Release of Functional Compounds. Adv. Mater. 2016, 28, 1227–1250. [Google Scholar] [CrossRef]
- Wu, Y.-P.; Yang, J.; Gao, H.-Y.; Shen, Y.; Jiang, L.; Zhou, C.; Li, Y.-F.; He, R.-R.; Liu, M. Folate-Conjugated Halloysite Nanotubes, an Efficient Drug Carrier, Deliver Doxorubicin for Targeted Therapy of Breast Cancer. ACS Appl. Nano Mater. 2018, 1, 595–608. [Google Scholar] [CrossRef]
- Zhou, M.; Zhao, Q.; Wu, Y.; Feng, S.; Wang, D.; Zhang, Y.; Wang, S. Mesoporous Carbon Nanoparticles as Multi-functional Carriers for Cancer Therapy Compared with Mesoporous Silica Nanoparticles. AAPS PharmSciTech 2020, 21, 1–12. [Google Scholar] [CrossRef]
- Xing, Y.; Zhou, M.; Du, X.; Li, X.; Li, J.; Xu, T.; Zhang, X. Hollow mesoporous carbon@Pt Janus nanomotors with dual response of H2O2 and near-infrared light for active cargo delivery. Appl. Mater. Today 2019, 17, 85–91. [Google Scholar] [CrossRef]
- Zhao, Q.; Yang, Y.; Wang, H.; Lei, W.; Liu, Y.; Wang, S. Gold nanoparticles modified hollow carbon system for dual-responsive release and chemo-photothermal synergistic therapy of tumor. J. Colloid Interface Sci. 2019, 554, 239–249. [Google Scholar] [CrossRef]
- Gui, X.; Chen, Y.; Zhang, Z.; Lei, L.; Zhu, F.; Yang, W.; Guo, Y.; Chu, M. Fluorescent hollow mesoporous carbon spheres for drug loading and tumor treatment through 980-nm laser and microwave co-irradiation. Biomaterials 2020, 248, 120009. [Google Scholar] [CrossRef] [PubMed]
- Sanginario, A.; Miccoli, B.; Demarchi, D. Carbon Nanotubes as an Effective Opportunity for Cancer Diagnosis and Treatment. Biosensors 2017, 7, 9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, Z.; Tao, J.; Chen, J.; Liu, Q. Carbon Nanotubes Enhance the Chemotherapy Sensitivity of Tumors with Multidrug Resistance. Lett. Drug Des. Discov. 2020, 17, 366–378. [Google Scholar] [CrossRef]
- Luo, B.; Xu, S.A.; Luo, A.; Wang, W.R.; Wang, S.L.; Guo, J.; Lin, Y.; Zhao, D.Y.; Wang, C.C. Mesoporous Biocompatible and Acid-Degradable Magnetic Colloidal Nanocrystal Clusters with Sustaina-ble Stability and High Hydrophobic Drug Loading Capacity. Acs Nano 2011, 5, 1428–1435. [Google Scholar] [CrossRef] [PubMed]
- Sun, C.; Xu, S.; Guo, J.; Xu, K.; Wang, C. The inhibitory and apoptotic effects of docetaxel-loaded mesoporous magnetic colloidal nanocrystal clusters on bladder cancer T24 cells in vitro. J. Biomed. Nanotechnol. 2014, 10, 455–462. [Google Scholar] [CrossRef] [PubMed]
- He, Y.; Wan, J.Y.; Yang, Y.; Yuan, P.; Yang, C.; Wang, Z.G.; Zhang, L.K. Multifunctional Polypyrrole-Coated Mesoporous TiO2 Nanocomposites for Photothermal, Sonodynamic, and Chemotherapeutic Treatments and Dual-Modal Ultrasound/Photoacoustic Imaging of Tumors. Adv. Healthc. Mate-Rials 2019, 8, 1801254. [Google Scholar] [CrossRef]
- Ren, W.; Iqbal, M.Z.; Zeng, L.; Chen, T.; Pan, Y.; Zhao, J.; Yin, H.; Zhang, L.; Zhang, J.; Li, A.; et al. Black TiO2 based core–shell nanocomposites as doxorubicin carriers for thermal imaging guided synergistic therapy of breast cancer. Nanoscale 2017, 9, 11195–11204. [Google Scholar] [CrossRef] [PubMed]
- Bakmaz, D.; Ulu, A.; Koytepe, S.; Ates, B. Preparation, characterization, and in vitro release study of vincristine sulfate-loaded chitosan-polyethylene glycol-oleic acid composites. Int. J. Polym. Anal. Charact. 2021, 26, 291–308. [Google Scholar] [CrossRef]
- Son, K.; Ueda, M.; Taguchi, K.; Maruyama, T.; Takeoka, S.; Ito, Y. Evasion of the accelerated blood clearance phenomenon by polysarcosine coating of liposomes. J. Control. Release 2020, 322, 209–216. [Google Scholar] [CrossRef] [PubMed]
- Luxenhofer, R.; Han, Y.; Schulz, A.; Tong, J.; He, Z.; Kabanov, A.; Jordan, R. Poly(2-oxazoline)s as Polymer Therapeutics. Macromol. Rapid Commun. 2012, 33, 1613–1631. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dong, S.; Ma, S.; Liu, Z.-L.; Ma, L.-L.; Zhang, Y.; Tang, Z.-H.; Deng, M.-X.; Song, W.-T. Functional Amphiphilic Poly(2-oxazoline) Block Copolymers as Drug Carriers: The Relationship between Structure and Drug Loading Capacity. Chin. J. Polym. Sci. 2021, 39, 865–873. [Google Scholar] [CrossRef]
- Vergaro, V.; Scarlino, F.; Bellomo, C.; Rinaldi, R.; Vergara, D.; Maffia, M.; Baldassarre, F.; Giannelli, G.; Zhang, X.; Lvov, Y.M.; et al. Drug-loaded polyelectrolyte microcapsules for sustained targeting of cancer cells. Adv. Drug Deliv. Rev. 2011, 63, 847–863. [Google Scholar] [CrossRef]
- Shen, H.; Li, F.; Wang, D.; Yang, Z.; Yao, C.; Ye, Y.; Wang, X. Chitosan–alginate BSA-gel-capsules for local chemotherapy against drug-resistant breast cancer. Drug Des. Dev. Ther. 2018, 12, 921–934. [Google Scholar] [CrossRef] [Green Version]
- Zhu, G.; Mei, L.; Vishwasrao, H.D.; Jacobson, O.; Wang, Z.; Liu, Y.; Yung, B.C.; Fuwu, Z.; Jin, A.; Niu, G.; et al. Intertwining DNA-RNA nanocapsules loaded with tumor neoantigens as synergistic nanovaccines for cancer immunotherapy. Nat. Commun. 2017, 8, 1–13. [Google Scholar] [CrossRef]
- Li, S.; Wang, K.; Shi, Y.; Cui, Y.; Chen, B.; He, B.; Dai, W.; Zhang, H.; Wang, X.; Zhong, C. Novel Biological Functions of ZIF-NP as a Delivery Vehicle: High Pulmonary Accumulation, Favorable Biocompatibility, and Improved Therapeutic Outcome. Adv. Funct. Mater. 2016, 26, 2715–2727. [Google Scholar] [CrossRef]
- Ke, X.; Song, X.; Qin, N.; Cai, Y.; Ke, F. Rational synthesis of magnetic Fe3O4@MOF nanoparticles for sustained drug delivery. J. Porous Mater. 2019, 26, 813–818. [Google Scholar] [CrossRef]
- Saleh, T.A. Nanomaterials: Classification, properties, and environmental toxicities. Environ. Technol. Innov. 2020, 20, 101067. [Google Scholar] [CrossRef]

| Ligand | Application | Ref. | |
|---|---|---|---|
| Peptide | Muramyl tripeptide (MTP) | Melanoma treatment | [23] |
| Arginine-glycine-aspartic acid (RGD) | Brain delivery | [24] | |
| N-formyl-methionine-leucine-phenylalanine (fMLP) | Leishmaniasis treatment | [25] | |
| Ac-KGFGGGLK peptide | Atherosclerotic detection | [26] | |
| CGP 31362 | Tumor destruction | [27] | |
| Muramyl dipeptide | Immunomodulating | [28] | |
| TD peptide | Melanoma treatment | [29] | |
| p18-4 (WxEAAYQrFL) | Breast cancer treatment | [30] | |
| Antibody | Integrinβ6 monoclonal antibody | Colon carcinoma treatment | [31] |
| anti-HER2 monoclonal antibody | Breast cancer treatment | [32] | |
| Human epidermal growth factor (hEGF) | Skin therapy | [33] | |
| Breast cancer treatment | [34] | ||
| Programmed Death Ligand-1 monoclonal antibody (α-PD-L1) | Melanoma treatment | [35] | |
| fibroblast growth factor (FGF) ligands | Bladder cancer targeting | [36] | |
| Frizzled 10 (FZD10) antibody | Colorectal cancer treatment | [37] | |
| CD123/CD33 dual-antibody | Reduction of antigen-negative escape | [38] | |
| CD123 antibody | Targeting to acute myeloid leukemia cells | [39] | |
| CD44 antibody | Imaging and therapy of hepatocellular carcinoma | [40] | |
| Others | Natural STAT3 inhibitors | Tumor immunotherapy | [41] |
| CRISPR/Cas9 | Gene silencing efficiency enhancement | [42] | |
| Aβ-targeting ligands | Alzheimer treatment | [43] | |
| STING Agonists | Cancer immunotherapy | [44] | |
| Itraconazole | Enhanced gene delivery of pDNA and siRNA | [45] | |
| Deoxyribonucleic acid (DNA) | Gene’s carriers in transfection assays | [46] |
| Cell Membrane | Nanoparticle | Application | Ref. |
|---|---|---|---|
| Macrophage | silica nanocapsules | 4T1 Subcutaneous tumor treatment | [56] |
| Au Nanoshells | 4T1 Subcutaneous tumor treatment | [57] | |
| NaYF4:Yb,Er@NaYF4 | 4T1 Subcutaneous tumor treatment | [58] | |
| copper sulfide nanoparticles | An allograft tumor of breast cancer treatment | [59] | |
| Emtansine liposomes | 4T1 metastasis lung cancer treatment | [60] | |
| ROS-responsive nanoparticles | Cardiovascular Disorders treatment | [61] | |
| ROS-sensitive β-cyclodextrin | Ulcerative colitis treatment | [62] | |
| Polymeric cores | Acute pancreatitis treatment | [63] | |
| mPEG5K-b-PLGA11K@miR199a-3p | Myocardial infarction treatment | [64] | |
| Erythrocyte | Polymeric nanoparticles | Biomimetic delivery platform | [65] |
| Fe3O4 nanoparticles | Reducing reticuloendothelial system uptake | [66] | |
| Gold nanocages | Photothermal therapy | [67] | |
| All-in-one hollow nanoworms (A-Fe/AuAg@PDA) | Combating Focal Bacterial Infection | [68] | |
| Black phosphorus | Photothermal cancer immunotherapy | [69] | |
| Chitosan, heparin and Au | Thrombus Therapy | [70] | |
| Zinc phthalocyanine and ICG | Photodynamic/photothermal theranostics | [71] | |
| Platelets | Porous nanoparticles | Targeted antitumor drug delivery | [72] |
| Polymeric nanoparticles | Reversing thrombus in mouse models | [73] | |
| PLGA and Fe3O4 nanoparticles | Dual targeted thrombolytic therapy | [74] | |
| γ-Fe2O3 nanoparticles | Ischemic Stroke treatment | [75] | |
| Malaria protein VAR2CSA | Targeted treatment of primary and metastatic Cancer | [76] | |
| Liposomes | Targeted therapy of atherosclerosis | [77] | |
| Photodynamic nanoparticle | Photodynamic therapy | [78] | |
| Stem cell | Nanogels | Tumor targeted drug delivery | [79] |
| Fe3O4 nanoparticles | Cartilage regeneration | [80] | |
| β-NaYF4:Yb3+,Er3+ | Photodynamic therapy | [81] | |
| Isotretinoin | Acne treatment | [82] | |
| Cancer cell | Glucose oxidase (GOx) and porphyrin metal-organic framework (MOF) | Cancer targeted starvation and photodynamic therapy | [83] |
| Upconversion nanoparticles | Imaging of triple-negative breast cancer | [84] | |
| Mesoporous silica nanoparticles | Regulating drug release | [85] | |
| MnO2 nanoreactor | Combined photodynamic-starvation therapy | [86] | |
| Immunostimulatory adjuvant | Eliciting multiantigenic antitumor immunity | [87] |
| Strategy | Component | Advantage | Disadvantage | Refs |
|---|---|---|---|---|
| Inorganic carrier nano drug delivery system | MSNPs; MCNPs; MCNCs; MTNPs | Good drug targeting; potential imaging capabilities | Low drug loading; potential carrier toxicity | [161,162,163,164,165] |
| Organic carrier nano drug delivery system | Synthetic polymer (PEG, PVP, POx); Natural biopolymers (proteins, peptides, nucleic acids) | Good drug targeting; low carrier toxicity; potential imaging capabilities; good biocompatibility | Low drug loading; carrier cleared quickly; poor stability | [3,161,164,165,166,167,168,169,170,171,172] |
| MOF carrier nano drug delivery system | HKUST; UiO; ZIF; MIL | Good drug targeting; potential imaging capabilities; good biocompatibility | Low drug loading; potential carrier toxicity | [161,164,165,173,174,175,176] |
| Carrier-free nanomedicines delivery system | Pure Nanodrugs; Drug–Drug conjugates | High drug loading; no carrier toxicity | Poor drug targeting; residual organic solvent | [161,164,165,177,178,179,180] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jia, L.; Zhang, P.; Sun, H.; Dai, Y.; Liang, S.; Bai, X.; Feng, L. Optimization of Nanoparticles for Smart Drug Delivery: A Review. Nanomaterials 2021, 11, 2790. https://doi.org/10.3390/nano11112790
Jia L, Zhang P, Sun H, Dai Y, Liang S, Bai X, Feng L. Optimization of Nanoparticles for Smart Drug Delivery: A Review. Nanomaterials. 2021; 11(11):2790. https://doi.org/10.3390/nano11112790
Chicago/Turabian StyleJia, Lina, Peng Zhang, Hongyan Sun, Yuguo Dai, Shuzhang Liang, Xue Bai, and Lin Feng. 2021. "Optimization of Nanoparticles for Smart Drug Delivery: A Review" Nanomaterials 11, no. 11: 2790. https://doi.org/10.3390/nano11112790






