1. Introduction
Malaria is an infectious disease caused by protozoan parasites which belong to the genus
Plasmodium and can be transmitted by female
Anopheles mosquitos [
1,
2]. Despite a major reduction in malaria morbidity and mortality in the past decades [
3,
4,
5], malaria remains the sixth leading cause of under-five mortality [
6]. The COVID-19 pandemic also disrupted health services for malaria prevention and treatment, and it led to the increase in malaria cases from 227 million in 2019 to 241 million in 2020 [
7]. Malaria deaths also increased from 558,000 to 627,000 during the same time period [
7].
Use of insecticide-treated nets (ITNs) including long-lasting insecticidal nets (LLINs) is a cost-effective intervention to prevent malaria [
8,
9]. ITNs have been distributed through mass campaigns and continuous distributions at fixed locations such as health facilities and schools [
10]. Since 2004, approximately 2 billion ITNs have been provided to Sub-Saharan Africa (SSA), and 65% of households had access to at least one ITN by 2020 [
7].
Previous studies examined the potential determinants of long-lasting insecticidal net (LLIN) ownership and use in SSA countries such as Zimbabwe, Rwanda, and Ethiopia [
11,
12,
13]. The findings from these studies revealed that LLIN ownership was significantly associated with household head or respondent’s biological sex, age, education levels, awareness of LLIN as a preventive measure, household assets and characteristics (e.g., type of roof, type of cooking fuel, availability of electricity), household wealth levels, geographic regions, and type of residence. LLIN utilization was associated with household head’s age and sex, household assets and characteristics (e.g., number of sleeping rooms, mosquito net hanged), pregnancy, household wealth levels, awareness of LLIN, and type of residence. Accordingly, demographic, socio-economic, and geographic or environmental factors have been identified as key determinants of LLIN ownership and use.
The United Nations Children’s Fund (UNICEF) is supporting the mass distribution of LLINs in Somalia in 2022. Understanding what influences the ownership and use of LLINs is of vital importance to accelerate malaria prevention efforts in Somalia. Few studies, however, have been conducted to characterize and explore malaria prevention practices in the country. To fill the knowledge gap and inform future malaria interventions, this study explored what factors are associated with mosquito net ownership and use in Somalia.
2. Methods
2.1. Study Context
Somalia is a malaria-endemic country in Sub-Saharan Africa with over 15.8 million people, and 51% of the population is estimated to live in a high transmission area (e.g., more than one case per population of 1000) [
7,
14]. WHO estimated that in 2020, Somalia had 829,649 malaria cases (491,000–1,247,000) and 2123 deaths (57–4730) [
7]. From 2005 to 2019, malaria incidence declined from 136.6 to 49.2 per population of1000 [
15]. Over 1.5 million LLINs were sold or delivered in 2020 in the country [
7].
2.2. Data Source
This study analyzed secondary data from the Micronutrient Survey 2019, a cross-sectional household survey that mainly aimed to explore the nutritional status of women and children and their living conditions in Somalia. As with the major household surveys (e.g., Demographic and Health Survey, Multiple Cluster Indicator Survey), the Micronutrient Survey used the multi-stage stratified cluster sampling. More specifically, this survey included six strata (1. Somaliland, 2. Puntland, 3. Hirshabelle and Galmudug, 4. Jubaland and South-West, 5. Banadir, and 6. internally displaced populations [IDP] camps in the aforementioned strata). For the first five strata, 25 clusters or primary sampling units were randomly selected with probability proportional to size. For the IDP camp selection, this survey referred to UNHCR’s IDP database to determine the sampling frame, which included all IDP camps and household information. Based on the available household lists, 16 households were randomly selected in each cluster. Additional information on the sampling procedure and sample size calculation is described elsewhere [
16,
17]. The survey teams visited a total of 2,400 households and collected data from 2172 households with a response rate of 90.5%.
2.3. Variables
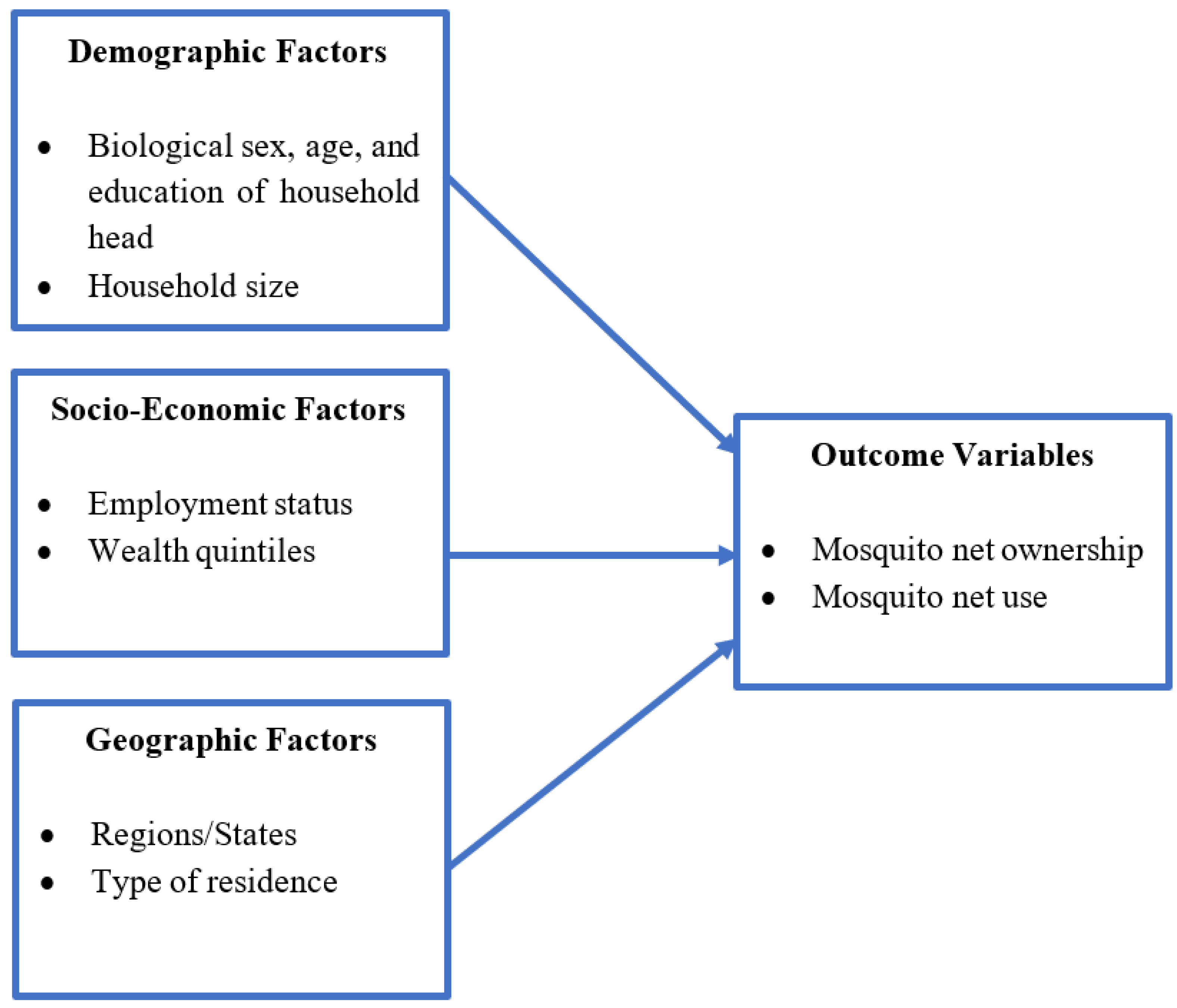
The main dependent variables are the household ownership of at least one mosquito net (1. No, 2. Yes) and the household utilization of all mosquito nets owned in the previous night (1. No, 2. Yes). The independent variables consist of demographic, socioeconomic, and geographic factors (
Figure 1). Demographic variables include household head’s biological sex (1. Male, 2. Female), age group (1. 25 years old or younger, 2. 26 to 35 years old, 3. 36 to 45 years old, 4. 46 years old or older), educational level (1. None or pre-school, 2. Koranic, 3. Primary school or higher), household size (1. 1 to 3 people, 2. 4 to 7 people, 3. 8 or more). Socioeconomic variables are employment status of household members (1. No household member with an employment, 2. Any household member with an employment) and wealth quintile (1. Poorest, 2. Poorer, 3. Middle, 4. Richer, 5. Richest). The wealth quintile was estimated through the principal component analysis of household characteristics such as type of water source, sanitation facility, livestock ownership, materials used for floors and walls). Geographic variables consist of states (1. Banadir, 2. Somaliland, 3. Puntland, 4. Hirshabelle, 5. Galmudug, 6. Southwest, 7. Jubaland) and type of residence (1. Rural, 2. Urban, 3. IDP camps).
2.4. Data Analysis
Univariate analysis was conducted to characterize the frequency of each study variable. For bivariate analysis, simple logistic regression was conducted to assess the association between independent and dependent variables. The F statistic and p-value of 0.05 were used to assess statistical associations between study variables. For multivariate analysis, multiple logistic regression was conducted to estimate the way each independent variable was associated with a dependent variable by holding other variables constant. The results of bivariate and multivariate analysis were presented in odd ratios. All analyses were performed with STATA 14, adjusting for the complex survey design.
2.5. Ethical Approval
This study used secondary data without any personally identifiable information. Thus, it did not require ethical approval. However, the original Micronutrient Survey 2019 obtained ethical approval from the Federal Ministry of Health and Ministries of Health in Puntland and Somaliland. The household-level data were obtained from the household heads (or spouse/other adult members in case of their absence) who provided written informed consent to participate in the survey. For those household heads who could not read and write at the time of data collection, the informed consent form was read out loud, and a fingerprint was collected as evidence of consent.
3. Results
Table 1 presents the household characteristics of survey participants. At least 87% of households were female headed, and the majority of household heads were 35 years old or younger. Over 75% of household heads received no formal education or preschool education, and less than 14% of them completed primary education or higher. Approximately half of households had up to three household members, and the other half had four or more household members. About 33% of households had at least one person who was employed with income. The wealth quintiles were distributed at 20%. The representation of states ranged from Hirshabelle at 4.5% to Somaliland at 26.4%. About one third of households were located in rural areas, while 49% of households were from urban areas. Over 15% of households were from IDP camps. The majority of households owned at least one mosquito net, and of those households with at least one mosquito net, 92.3% of households reported that they used all mosquito nets in the previous night.
Table 2 presents the summary of bivariate analysis between study variables. The biological sex of household heads was not significantly associated with the ownership of mosquito net (
p = 0.222) or the full utilization of mosquito nets in the previous night (
p = 0.637). The age and educational attainment of household head, household size, employment status of household members, wealth quintiles, states, and type of residence were significantly associated with the ownership of mosquito net (
p < 0.05). For mosquito net use, the educational attainment of household head, employment status, and states had a significant association (
p < 0.05).
Table 3 presents the results of multiple logistic regression on the ownership of mosquito net. The odds of having at least one mosquito net among households whose heads were 26–35 years old and 36–45 years old at the time of survey is 2.25 times and 2.09 times that of households whose heads were 25 years old or younger (
p < 0.001). The household heads who received Koranic education are associated with 33.6% lower odds of having any mosquito net than those of household heads without any formal education or with pre-school education only (
p < 0.025). Large households are associated with a 38.9% lower odds of mosquito net ownership than those of small households (
p = 0.035).
Having at least one household member with an employment or income is associated with 48.0% higher odds of mosquito net ownership than those of households without any employed individual (p = 0.020). Compared to the households in the lowest wealth quintile, households with higher quintiles are associated with significantly higher odds of mosquito net ownership. The odds of having at least one mosquito net for the highest wealth quintile is 12.82 times those of the lowest wealth quintile (<0.001).
Compared to the households in Banadir, households in other states have a significantly higher odds of mosquito net ownership. The odds of mosquito net ownership in Hirshabelle, for instance, are approximately 3.93 times those of Banadir (p < 0.001). Urban households are associated with 92.5% higher odds than those of rural households (p = 0.013).
Table 4 summarizes the results of multiple logistic regression on the use of household-owned mosquito nets in the previous night. Compared to the households whose heads were 25 years old or younger, households with older household heads were associated with lower odds of using all mosquito nets in the previous night. More specifically, the households whose heads were 26 to 35 years old, 36 to 45 years old, and 46 years old or older had 55.5% (
p = 0.027), 55.0% (
p = 0.042), and 63.4% (
p = 0.006) lower odds of mosquito net use, respectively. The odds of mosquito net use in Galmudug and Southwest were 69.7% and 78.7% lower than those of Banadir, respectively (
p = 0.002).
4. Discussion
This is one of the first quantitative studies with a nationally representative sample that explored the potential determinants of mosquito net ownership and use in Somalia. The results suggested that household head’s age, educational attainment, household size, employment status of household members, socioeconomic status, geographic regions and type of residence are significantly associated with mosquito net ownership. The analysis also highlighted household head’s age as an influential factor in mosquito net use.
In this study, over 42% of households did not confirm mosquito net ownership, suggesting that they would not be able to reduce the risk of malaria and other vector-borne diseases such as dengue and yellow fever [
18]. Although 57% of households reported the ownership of at least one mosquito net, promoting mosquito net ownership and use remains vital to protecting the population in Somalia. Given that 75% of household heads reported to have no formal education, public health interventions may be planned for people with varying literacy levels.
As with previous research [
11,
12,
13], this study revealed that household ownership and use could be influenced by different factors. The age of household heads was positively associated with mosquito net ownership. However, it was negatively associated with mosquito net use. This finding suggests that families with older household heads may have more opportunities to obtain mosquito nets, but they may not use them as opposed to other families with younger household heads. The household wealth level and employment status were also key determinants of mosquito net ownership, but they did not influence mosquito net use. Addressing individual perceptions, behavioral intention, and social norms would be vital to further understanding of these findings and translating mosquito net ownership into use [
19,
20,
21].
The findings on geographic regions and states also provided insights into the regions where malaria prevention efforts can be accelerated. The multivariate analysis revealed that households in Somaliland, Puntland, Hirshabelle, Galmudug, Southwest and Jubaland were associated with higher odds of owning mosquito nets than those in Banadir. As one of the most populated regions in Somalia, Banadir may be considered for additional interventions to enhance mosquito net ownership at the household level. Galmudug and Southwest states may also implement behavioral change communication interventions to enhance mosquito net use. Despite the current challenges with estimating malaria burden in Somalia, some regions—Bay, Lower Shabelle, and Gedo—have been associated with high malaria incidence [
22]. The findings of this study and sub-national data on malaria incidence may be reviewed together to better compile the locations where malaria interventions can be implemented as priority areas.
This study noted a number of limitations and opportunities for future studies. First, limited malaria-related data were available in this study because the purpose of Micronutrient Survey 2019 was to collect in-depth information on maternal and child nutrition. Future studies and surveys may collect additional data on intrapersonal and psychosocial factors (e.g., motivation, perceived importance) to understand what additional factors influence mosquito net ownership and use in Somalia. Second, the findings of this study are not generalizable at the district level. To better inform malaria interventions with geographic priorities, additional data collection and quantitative analysis at the district level may be needed. Third, self-reported data of mosquito net ownership and use may be subject to social desirability bias [
23]. Due to this potential challenge, the true percentage of mosquito net ownership and use may be lower. By collecting self-reported data with direct observations, this risk may be mitigated in the future. Lastly, the Micronutrient Survey 2019 did not specifically assess the ownership and use of ITNs or LLINs but was only able to characterize if households owned and used any type of mosquito nets as a proxy measure. Future studies may directly assess the ownership and use of ITNs and LLINs in Somalia to explore their determinants.
5. Conclusions
Despite the limitations, this study revealed some of the key household characteristics as the potential determinants of mosquito net ownership and use in Somalia. To enhance mosquito net ownership in Somalia, public health programs may focus on providing mosquito nets to households with a low socioeconomic status, without any employed household members, with a large household size, with a young household head, and in rural areas. Use of mosquito nets may be facilitated through behavior change communication with older household heads. By further exploring and understanding the psychosocial determinants of mosquito net ownership and use, malaria prevention interventions can be more effective in Somalia.
Author Contributions
Conceptualization, M.H.; Methodology, M.H.; Validation, A.A.O.; Formal analysis, M.H.; Writing–original draft, M.H.; Writing–review & editing, M.H., U.U., P.D., A.A.O., A.M., A.M.J., C.M. and M.K.; Supervision, M.K. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data presented in this study is available upon request from the corresponding author.
Acknowledgments
This manuscript is dedicated to one of co-authors Carolyn Masheti who recently passed away. Her dedication and contributions to malaria prevention and treatment in Somalia are truly appreciated and acknowledged.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Cox, F.E. History of the discovery of the malaria parasites and their vectors. Parasites Vectors 2010, 3, 1–9. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tuteja, R. Malaria—An overview. FEBS J. 2007, 274, 4670–4679. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Murray, C.J.L.; Rosenfeld, L.C.; Lim, S.S.; Andrews, K.G.; Foreman, K.J.; Haring, D.; Fullman, N.; Naghavi, M.; Lozano, R.; Lopez, A.D. Global malaria mortality between 1980 and 2010: A systematic analysis. Lancet 2012, 379, 413–431. [Google Scholar] [CrossRef]
- Cibulskis, R.E.; Alonso, P.; Aponte, J.; Aregawi, M.; Barrette, A.; Bergeron, L.; Fergus, C.A.; Knox, T.; Lynch, M.; Patouillard, E.; et al. Malaria: Global progress 2000–2015 and future challenges. Infect. Dis. Poverty 2016, 5, 1–8. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Weiss, D.J.; Lucas, T.C.; Nguyen, M.; Nandi, A.K.; Bisanzio, D.; Battle, K.E.; Cameron, E.; Twohig, K.A.; Pfeffer, D.A.; Rozier, J.A.; et al. Mapping the global prevalence, incidence, and mortality of Plasmodium falciparum, 2000–2017: A spatial and temporal modelling study. Lancet 2019, 394, 322–331. [Google Scholar] [CrossRef] [Green Version]
- Institute for Health Metrics and Evaluation (IHME). GBD Compare. Seattle, WA: IHME, University of Washington. 2015. Available online: http://vizhub.healthdata.org/gbd-compare (accessed on 18 February 2022).
- World Health Organization. World Malaria Report 2021; World Health Organization: Geneva, Switzerland, 2021. [Google Scholar]
- Wangdi, K.; Furuya-Kanamori, L.; Clark, J.; Barendregt, J.J.; Gatton, M.L.; Banwell, C.; Kelly, G.C.; Doi, S.A.; Clements, A.C. Comparative effectiveness of malaria prevention measures: A systematic review and network meta-analysis. Parasites Vectors 2018, 11, 1–13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- White, M.T.; Conteh, L.; Cibulskis, R.; Ghani, A.C. Costs and cost-effectiveness of malaria control interventions-a systematic review. Malar. J. 2011, 10, 1–14. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Scates, S.S.; Finn, T.P.; Wisniewski, J.; Dadi, D.; Mandike, R.; Khamis, M.; Greer, G.; Serbantez, N.; Segbaya, S.; Owusu, P.; et al. Costs of insecticide-treated bed net distribution systems in sub-Saharan Africa. Malar. J. 2020, 19, 1–18. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tapera, O. Determinants of long-lasting insecticidal net ownership and utilization in malaria transmission regions: Evidence from Zimbabwe Demographic and Health Surveys. Malar. J. 2019, 18, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kateera, F.; Ingabire, C.M.; Hakizimana, E.; Rulisa, A.; Karinda, P.; Grobusch, M.P.; Mutesa, L.; van Vugt, M.; Mens, P.F. Long-lasting insecticidal net source, ownership and use in the context of universal coverage: A household survey in eastern Rwanda. Malar. J. 2015, 14, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Tassew, A.; Hopkins, R.; Deressa, W. Factors influencing the ownership and utilization of long-lasting insecticidal nets for malaria prevention in Ethiopia. Malar. J. 2017, 16, 1–9. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Somalia. 2018. Available online: https://www.who.int/malaria/publications/country-profiles/profile_som_en.pdf?ua=1 (accessed on 17 March 2022).
- World Health Organization. Estimated Malaria Incidence (per 1000 Population at Risk). 2022. Available online: https://www.who.int/data/gho/data/indicators/indicator-details/GHO/malaria-incidence-(per-1000-population-at-risk) (accessed on 17 March 2022).
- Federal Ministry of Health; Ministry of Health [Somaliland]; Ministry of Health [Puntland]; UNICEF. BrandPro, GroundWork, 2020. Somalia Micronutrient Survey 2019. Available online: https://www.unicef.org/somalia/media/1681/file/Somalia-Micronutient-Survey-2019.pdf (accessed on 17 March 2022).
- Donkor, W.E.; Mbai, J.; Sesay, F.; Ali, S.I.; Woodruff, B.A.; Hussein, S.M.; Mohamud, K.M.; Muse, A.; Mohamed, W.S.; Mohamoud, A.M.; et al. Risk factors of stunting and wasting in Somali pre-school age children: Results from the 2019 Somalia micronutrient survey. BMC Public Health 2022, 22, 1–11. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Vector-Borne Diseases. 2020. Available online: https://www.who.int/news-room/fact-sheets/detail/vector-borne-diseases (accessed on 30 October 2022).
- Ernst, K.C.; Hayden, M.H.; Olsen, H.; Cavanaugh, J.L.; Ruberto, I.; Agawo, M.; Munga, S. Comparing ownership and use of bed nets at two sites with differential malaria transmission in western Kenya. Malar. J. 2016, 15, 1–16. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Perkins, J.M.; Krezanoski, P.; Takada, S.; Kakuhikire, B.; Batwala, V.; Tsai, A.C.; Christakis, N.A.; Bangsberg, D.R. Social norms, misperceptions, and mosquito net use: A population-based, cross-sectional study in rural Uganda. Malar. J. 2019, 18, 1–13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pulford, J.; Hetzel, M.W.; Bryant, M.; Siba, P.M.; Mueller, I. Reported reasons for not using a mosquito net when one is available: A review of the published literature. Malar. J. 2011, 10, 1–10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Federal Ministry of Health. National Health Data Warehouse. 2022. Available online: https://hmissomalia.net/dhis-web-commons/security/login.action (accessed on 25 March 2022).
- Krumpal, I. Determinants of social desirability bias in sensitive surveys: A literature review. Qual. Quant. 2013, 47, 2025–2047. [Google Scholar] [CrossRef]
| Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).