Introduction of 24 h Resident Consultant Cover in a Tertiary Neonatal Unit—Impact on Mortality and Clinical Outcomes
Abstract
:1. Introduction
2. Materials and Methods
2.1. Subjects and Study Design
2.2. Derived Outcomes and Composite Parameters
2.3. Resident Consultants
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dalys, G.B.D.; Collaborators, H. Global, regional, and national disability-adjusted life-years (Dalys) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990–2017: A Systematic Analysis For The Global Burden Of Disease Study 2017. Lancet 2018, 392, 1859–1922. [Google Scholar] [CrossRef] [Green Version]
- Harrison, W.; Goodman, D. Epidemiologic Trends in Neonatal Intensive Care, 2007–2012. JAMA Pediatr. 2015, 169, 855–862. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- RCPCH. Consultant Delivered Care—An Evaluation of New Ways of Working in Paediatrics; RCPCH: London, UK, 2012. [Google Scholar]
- BAPM. Service Standards for Hospitals Providing Neonatal Care, 3rd ed.; BAPM: London, UK, 2010. [Google Scholar]
- Toolkit for High Quality Neonatal Services; Department of Health: London, UK, 2009.
- Egyepong, J.; Woodman, M.; Wari-Pepple, D. G120(P) Current Neonatal Resident Consultant Workforce in Level 3 Nicus in UK. Arch. Dis. Child. 2014, 99, A50–A51. [Google Scholar] [CrossRef]
- Resnick, S.; Jacques, A.; Patole, S.; Simmer, K. Does after-hours in-house senior physician cover improve standard of care and outcomes in high-risk preterm neonates? A Retrospective Cohort Study. J. Paediatr. Child Health 2011, 47, 795–801. [Google Scholar] [CrossRef] [PubMed]
- Lodha, A.; Brown, N.; Soraisham, A.; Amin, H.; Tang, S.; Singhal, N. Twenty-four-hour in-house neonatologist coverage and long-term neurodevelopmental outcomes of preterm infants. Paediatr. Child Health 2017, 22, 249–254. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.K.; Draper, E.S.; Manktelow, B.N.; Field, D.J. Socioeconomic Inequalities in Survival and Provision of Neonatal Care: Population Based Study of Very Preterm Infants. BMJ 2009, 339, B4702. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- BAPM. Categories of Care 2011; BAPM: London, UK, 2011. [Google Scholar]
- Wright, C.M.; Booth, I.W.; Buckler, J.M.; Cameron, N.; Cole, T.J.; Healy, M.J.; Hulse, J.A.; Preece, M.A.; Reilly, J.J.; Williams, A.F. Growth reference charts for use in the united kingdom. Arch. Dis. Child. 2002, 86, 11–14. [Google Scholar] [CrossRef] [PubMed]
- Laptook, A.R.; Bell, E.F.; Shankaran, S.; Boghossian, N.S.; Wyckoff, M.H.; Kandefer, S.; Walsh, M.; Saha, S.; Higgins, R. Admission temperature and associated mortality and morbidity among moderately and extremely preterm infants. J. Pediatr. 2018, 192, 53–59. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- BAPM. Identification and Management of Neonatal Hypoglycaemia in The Full Term Infant; BAPM: London, UK, 2017. [Google Scholar]
- Peng, W.; Zhu, H.; Shi, H.; Liu, E. Volume-Targeted Ventilation Is More Suitable Than Pressure-Limited Ventilation For Preterm Infants: A Systematic Review And Meta-Analysis. Arch. Dis. Child.-Fetal Neonatal Ed. 2014, 99, F158–F165. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shetty, S.; Sundaresan, A.; Hunt, K.; Desai, P.; Greenough, A. Changes in the use of humidified high flow nasal cannula oxygen. Arch. Dis. Child.-Fetal Neonatal Ed. 2016, 101, F371–F372. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- BOOST II United Kingdom Collaborative Group; BOOST II Australia Collaborative Group; BOOST II New Zealand Collaborative Group. Oxygen saturation and outcomes in preterm infants. N. Engl. J. Med. 2013, 368, 2094–2104. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shankaran, S.; Laptook, A.R.; Ehrenkranz, R.A.; Tyson, J.E.; Mcdonald, S.A.; Donovan, E.F.; Fanaroff, A.A.; Poole, W.K.; Wright, L.L.; Higgins, R.D.; et al. Whole-Body hypothermia for neonates with hypoxic-ischemic encephalopathy. N. Engl. J. Med. 2005, 353, 1574–1584. [Google Scholar] [CrossRef] [PubMed]
- Dassios, T.; Williams, E.E.; Hickey, A.; Bunce, C.; Greenough, A. Bronchopulmonary dysplasia and postnatal growth following extremely preterm birth. Arch. Dis. Child.-Fetal Neonatal Ed. 2020, 106, 386–391. [Google Scholar] [CrossRef] [PubMed]
- Wyckoff, M.H. Initial resuscitation and stabilization of the periviable neonate: The golden-hour approach. Semin. Perinatol. 2014, 38, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Scott-Jupp, R.; Carter, E.; Brown, N. Effects of consultant residence out-of-hours on acute paediatric admissions. Arch. Dis. Child. 2020, 105, 661–663. [Google Scholar] [CrossRef] [PubMed]
- Perlman, J.M.; Wyllie, J.; Kattwinkel, J.; Wyckoff, M.H.; Aziz, K.; Guinsburg, R.; Kim, H.S.; Liley, H.G.; Mildenhall, L.; Simon, W.M.; et al. Part 7: Neonatal resuscitation: 2015 International consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations. Circulation 2015, 132, S204–S241. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Pre-Resident N = 2613 | Resident N = 2165 | p Value | |
|---|---|---|---|
| Maternal age (years) | 31 (27–35) | 32 (28–36) | <0.001 |
| Antenatal steroids (in <34 weeks) | 597 of 679 (88) | 551 of 594 (93) | 0.015 |
| Cord arterial pH | 7.24 (7.16–7.30) | 7.22 (7.13–7.29) | 0.001 |
| Inborn at KCH | 2306 (88) | 1740 (80) | <0.001 |
| Gestational age (weeks) | 37.3 (33.7–39.7) | 37.6 (33.3–40.0) | 0.304 |
| Gestation < 28 weeks | 172 (6.6) | 180 (8.3) | 0.023 |
| Birth weight (kg) | 2.66 (1.86–3.37) | 2.76 (1.77–3.41) | 0.518 |
| Birth weight z score | −0.37 (−1.09–0.37) | −0.34 (−1.02–0.35) | 0.705 |
| Male sex | 1452 (56) | 1243 (57) | 0.069 |
| Apgar at 10 min | 10 (9–10) | 10 (9–10) | 0.646 |
| Admissions at night | 1102 (42.2) | 945 (43.6) | 0.305 |
| Admission hypothermia | 816 (31) | 324 (15) | <0.001 |
| Day admission hypothermia | 489 of 1505 (32.5) | 187 of 1220 (15.3) | <0.001 |
| Night admission hypothermia | 327 of 1091 (30.0) | 137 of 944 (14.5) | <0.001 |
| Admission hypoglycaemia | 842 (32.2) | 531 (24.5) | <0.001 |
| Time to first consult (h) | 1.5 (0.6–4.3) | 0.5 (0.3–1.5) | <0.001 |
| First consultation > 6 h | 421 (16.1) | 151(7.0) | <0.001 |
| Mechanical ventilation | 691 (26.4) | 843 (38.9) | <0.001 |
| Days of ventilation (ventilated only) | 3 (1–6) | 3 (1–7) | 0.496 |
| Days of oxygen (in the ones that had oxygen, N = 2179) | 2 (1–4) | 3 (1–9) | <0.001 |
| Days of PN (in the ones that had PN, N = 1332) | 10 (6–18) | 12 (7–22) | <0.001 |
| Days of intensive care (per year) | 1256 | 3940 | N/A |
| Home oxygen | 184 (7.0) | 252 (11.6) | <0.001 |
| IVH grade III-IV or PVL (% of <28 weeks) | 44 (25.6) | 60 (33.3) | 0.239 |
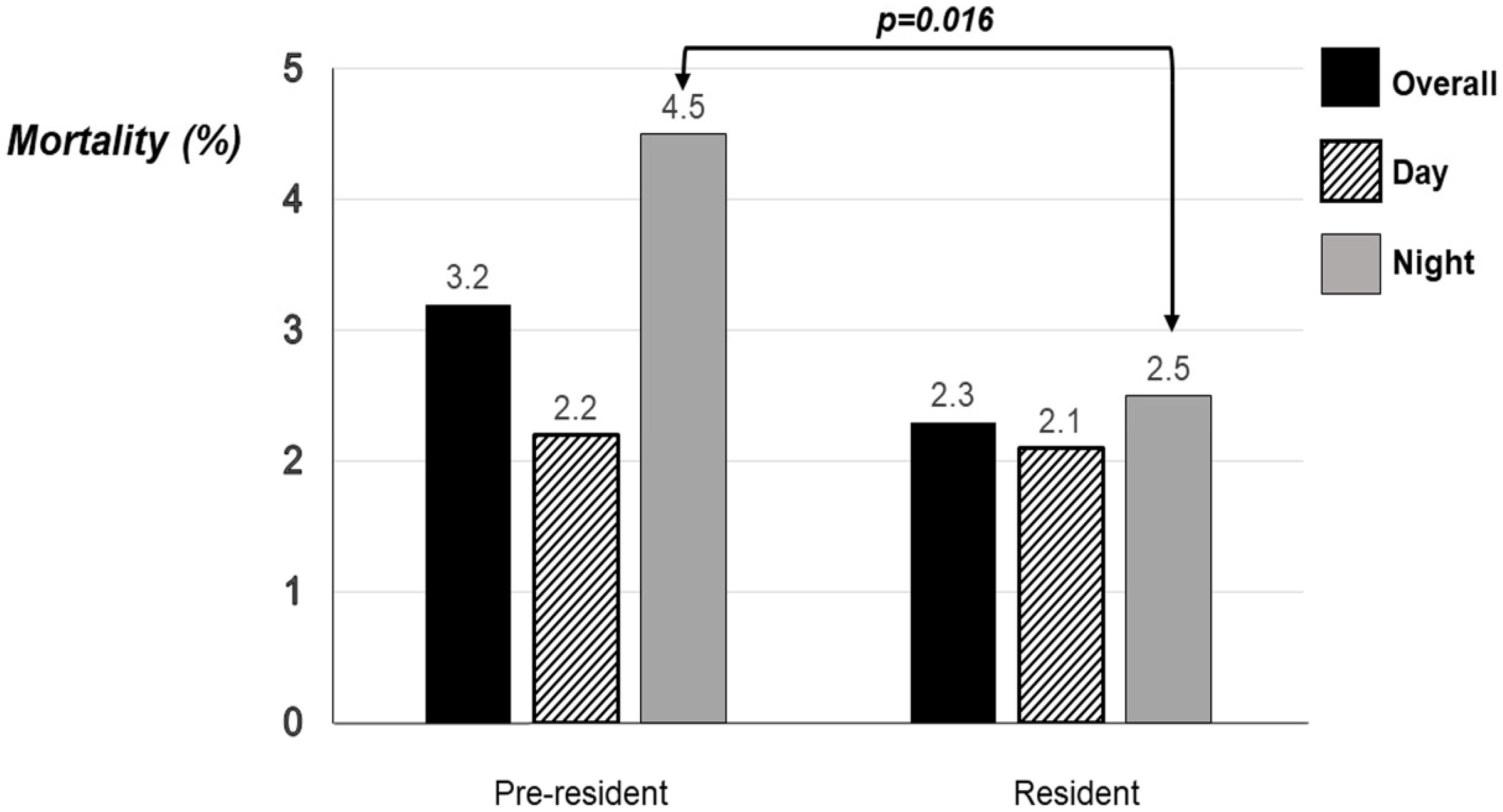
| Overall mortality | 83 (3.2) | 50 (2.3) | 0.077 |
| Day admissions mortality | 33 of 1511 (2.2) | 26 of 1220 (2.1) | 0.925 |
| Night admissions mortality | 50 of 1102 (4.5) | 24 of 945 (2.5) | 0.016 |
| Postmenstrual age at discharge (weeks) | 38.6 (36.4–41.0) | 39.2 (36.3–41.1) | 0.568 |
| Weight at discharge | 2.80 (2.10–3.43) | 2.93 (2.12–3.50) | 0.050 |
| Died N = 133 | Survived N = 4645 | p Value | |
|---|---|---|---|
| Male sex | 79 (59.4) | 2616 (56.3) | p = 0.723 |
| Gestational age (weeks) | 32.9 (25.1–38.3) | 37.4 (33.7–39.9) | p < 0.001 |
| Birth weight z-score | −0.53 (−1.03–0.14) | −0.35 (−1.06–0.37) | p = 0.064 |
| Duration of ventilation (days) | 4 (2–14) | 2 (1–6) | p < 0.001 |
| Admission temperature (°C) | 36.5 (36.1–36.9) | 36.8 (36.5–37.0) | p < 0001 |
| Adjusted p | Odds Ratio | 95% Confidence Intervals | |
|---|---|---|---|
| Resident period | <0.001 | 2.02 | 1.40–3.11 |
| Gestational age | <0.001 | 1.14 | 1.10–1.18 |
| Birth weight z-score | 0.288 | 1.10 | 0.92–1.31 |
| Admission hypothermia | <0.001 | 1.72 | 1.39–2.12 |
| Duration of ventilation | <0.001 | 0.98 | 0.97–0.99 |
| Admission during the night | 0.047 | 0.69 | 0.48–0.88 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zorro, C.; Dassios, T.; Hickey, A.; Arasu, A.; Bhat, R.; Greenough, A. Introduction of 24 h Resident Consultant Cover in a Tertiary Neonatal Unit—Impact on Mortality and Clinical Outcomes. Children 2021, 8, 865. https://doi.org/10.3390/children8100865
Zorro C, Dassios T, Hickey A, Arasu A, Bhat R, Greenough A. Introduction of 24 h Resident Consultant Cover in a Tertiary Neonatal Unit—Impact on Mortality and Clinical Outcomes. Children. 2021; 8(10):865. https://doi.org/10.3390/children8100865
Chicago/Turabian StyleZorro, Carolina, Theodore Dassios, Ann Hickey, Anusha Arasu, Ravindra Bhat, and Anne Greenough. 2021. "Introduction of 24 h Resident Consultant Cover in a Tertiary Neonatal Unit—Impact on Mortality and Clinical Outcomes" Children 8, no. 10: 865. https://doi.org/10.3390/children8100865






