A Randomized, Controlled Animal Study: 21% or 100% Oxygen during Cardiopulmonary Resuscitation in Asphyxiated Infant Piglets
Abstract
:1. Introduction
2. Methods
2.1. Inclusion and Exclusion Criteria
2.2. Randomization
2.3. Sample Size and Power Estimates
2.4. Blinding
2.5. Animal Preparation
2.6. Hemodynamic Parameters
2.7. Respiratory Parameters
2.8. Cerebral Perfusion
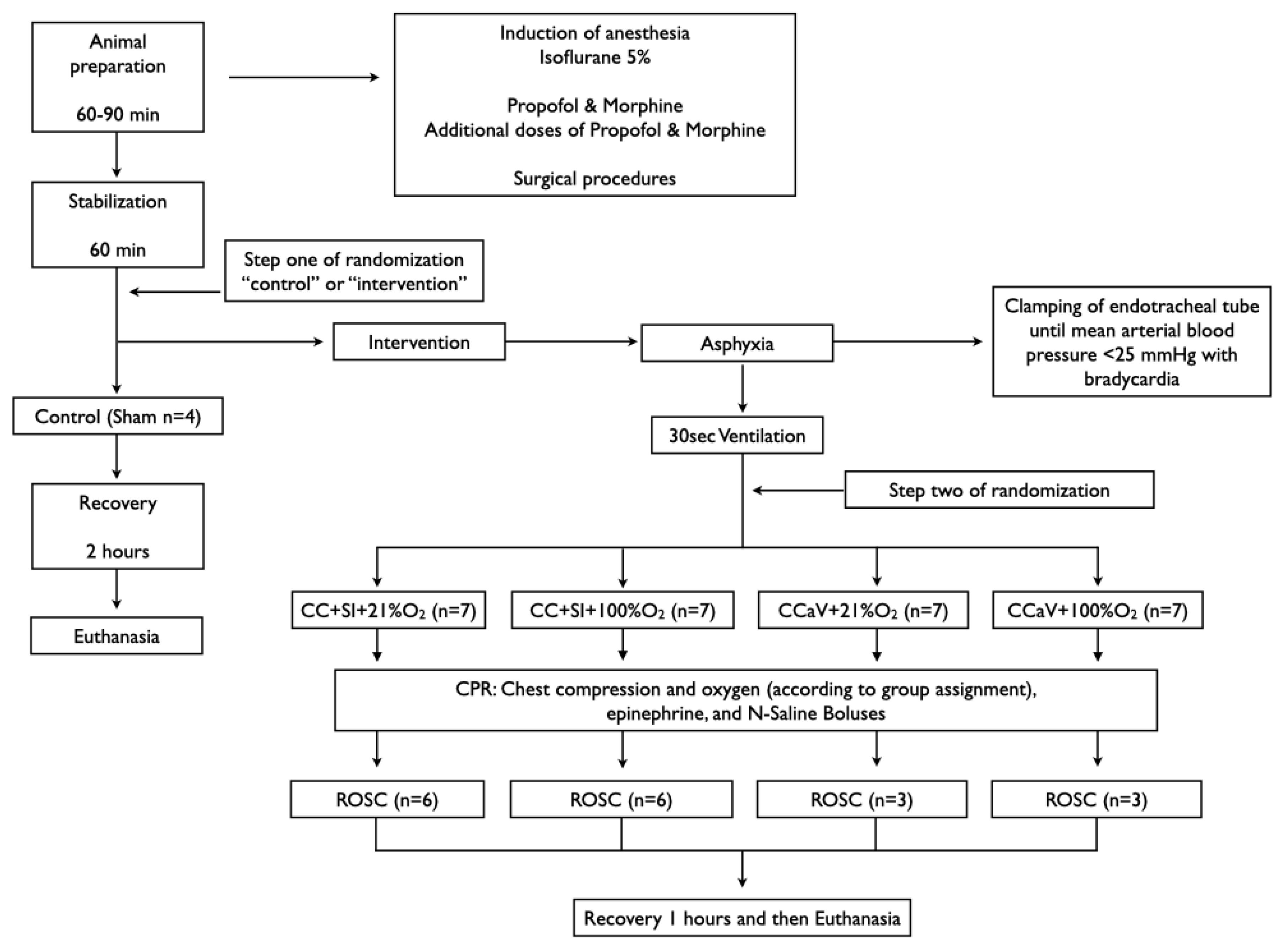
2.9. Experimental Protocol
3. Data Collection and Analysis
4. Results
4.1. Resuscitation and Primary Outcome
4.2. Respiratory and Hemodynamic Parameters
4.3. Injury Markers
5. Discussion
6. Limitations
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
A 140-character Tweet
Abbreviations
| CC | Chest compression |
| CPR | Cardiopulmonary resuscitation |
| ROSC | Return of spontaneous circulation |
| SI | Sustained Inflation |
| O2 | Oxygen |
| PPV | Positive pressure ventilation |
| 3:1 | Compression to Ventilation ratio |
| IQR | Interquartile range |
References
- Wyckoff, M.H.; Singletary, E.M.; Soar, J.; Olasveengen, T.M.; Greif, R.; Liley, H.G.; Zideman, D.; Bhanji, F.; Andersen, L.W.; Avis, S.R.; et al. 2021 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations: Summary from the Basic Life Support; Advanced Life Support; Neonatal Life Support; Education, Implementation, and Teams; First Aid Task Forces; and the COVID-19 Working Group. Circulation 2021, 145, e645–e721. [Google Scholar] [CrossRef] [PubMed]
- Aziz, K.; Lee, C.H.C.; Escobedo, M.B.; Hoover, A.V.; Kamath-Rayne, B.D.; Kapadia, V.S.; Magid, D.J.; Niermeyer, S.; Schmölzer, G.M.; Szyld, E.; et al. Part 5: Neonatal Resuscitation 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Pediatrics 2021, 147 (Suppl. S1), e2020038505E. [Google Scholar] [CrossRef] [PubMed]
- Topjian, A.A.; Raymond, T.T.; Atkins, D.; Chan, M.; Duff, J.P.; Joyner, B.L., Jr.; Lasa, J.J.; Lavonas, E.J.; Levy, A.; Mahgoub, M.; et al. Part 4: Pediatric Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2020, 142 (Suppl. S2), S469–S523. [Google Scholar] [CrossRef]
- Wyckoff, M.H.; Wyllie, J.P.; Aziz, K.; de Almeida, M.F.; Fabres, J.W.; Fawke, J.; Guinsburg, R.; Hosono, S.; Isayama, T.; Kapadia, V.S.; et al. Neonatal Life Support: 2020 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Circulation 2020, 142 (Suppl. S1), 329–337. [Google Scholar] [CrossRef]
- Aziz, K.; Lee, H.C.; Escobedo, M.B.; Hoover, A.V.; Kamath-Rayne, B.D.; Kapadia, V.S.; Magid, D.J.; Niermeyer, S.; Schmölzer, G.M.; Szyld, E.G.; et al. Part 5: Neonatal Resuscitation: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2020, 142 (Suppl. S2), S524–S550. [Google Scholar] [CrossRef] [PubMed]
- Davis, P.G.; Tan, A.; O’Donnell, C.P.F.; Schulze, A. Resuscitation of newborn infants with 100% oxygen or air: A systematic review and meta-analysis. Lancet 2004, 364, 1329–1333. [Google Scholar] [CrossRef]
- Kilgannon, J.H.; Jones, A.E.; Shapiro, N.I.; Angelos, M.G.; Milcarek, B.; Hunter, K.; Parrillo, J.E.; Trzeciak, S. Investigators for the EMSRN (EMShockNet). Association Between Arterial Hyperoxia following Resuscitation from Cardiac Arrest and in-Hospital Mortality. JAMA 2010, 303, 2165–2171. [Google Scholar] [CrossRef] [Green Version]
- Barreto, J.A.; Weiss, N.S.; Nielsen, K.R.; Farris, R.; Roberts, J.S. Hyperoxia after pediatric cardiac arrest: Association with survival and neurological outcomes. Resuscitation 2022, 171, 8–14. [Google Scholar] [CrossRef]
- Saugstad, O.D.; Ramji, S.; Soll, R.; Vento, M. Resuscitation of newborn infants with 21% or 100% oxygen: An updated systematic review and meta-analysis. Neonatology 2008, 94, 176–182. [Google Scholar] [CrossRef]
- Vento, M.; Saugstad, O.D. Oxygen Supplementation in the Delivery Room: Updated Information. J. Pediatr. 2011, 158, e5–e7. [Google Scholar] [CrossRef]
- Schmölzer, G.M.; Patel, S.D.; Monacelli, S.; Kim, S.Y.; Shim, G.; Lee, T.; O’Reilly, M.; Cheung, P. Sustained Inflation During Chest Compression: A New Technique of Pediatric Cardiopulmonary Resuscitation That Improves Recovery and Survival in a Pediatric Porcine Model. J. Am. Heart Assoc. 2020, 10, e019136. [Google Scholar] [CrossRef]
- Schmölzer, G.M.; O’Reilly, M.; Fray, C.; Os S van Cheung, P.-Y. Chest compression during sustained inflation versus 3:1 chest compression:ventilation ratio during neonatal cardiopulmonary resuscitation: A randomised feasibility trial. Arch. Dis. Child.-Fetal Neonatal Ed. 2018, 103, F455–F460. [Google Scholar] [CrossRef]
- Schmölzer, G.M.; Pichler, G.; Solevåg, A.; Fray, C.; van Os, S.; Cheung, P.-Y. The SURV1VE trial—Sustained inflation and chest compression versus 3:1 chest compression-to-ventilation ratio during cardiopulmonary resuscitation of asphyxiated newborns: Study protocol for a cluster randomized controlled trial. Trials 2019, 20, 139. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Li, E.S.; Cheung, P.-Y.; Lee, T.-F.; Lu, M.; O’Reilly, M.; Schmölzer, G.M. Return of spontaneous Circulation Is Not Affected by Different Chest Compression Rates Superimposed with Sustained Inflations during Cardiopulmonary Resuscitation in Newborn Piglets. PLoS ONE 2016, 11, e0157249. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Schmölzer, G.M.; O’Reilly, M.; LaBossiere, J.; Lee, T.-F.; Cowan, S.; Qin, S.; Bigam, D.L.; Cheung, P.-Y. Cardiopulmonary resuscitation with chest compressions during sustained inflations: A new technique of neonatal resuscitation that improves recovery and survival in a neonatal porcine model. Circulation 2013, 128, 2495–2503. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mustofa, J.; Cheung, P.-Y.; Patel, S.; Lee, T.-F.; Lu, M.; Pasquin, M.P.; O’Reilly, M.; Schmölzer, G.M. Effects of different durations of sustained inflation during cardiopulmonary resuscitation on return of spontaneous circulation and hemodynamic recovery in severely asphyxiated piglets. Resuscitation 2018, 129, 82–89. [Google Scholar] [CrossRef]
- Li, E.S.; Görens, I.; Cheung, P.-Y.; Lee, T.-F.; Lu, M.; O’Reilly, M.; Schmölzer, G.M. Chest Compressions during Sustained Inflations Improve Recovery When Compared to a 3:1 Compression:Ventilation Ratio during Cardiopulmonary Resuscitation in a Neonatal Porcine Model of Asphyxia. Neonatology 2017, 112, 337–346. [Google Scholar] [CrossRef]
- Schmölzer, G.M. Chest Compressions During Sustained Inflation During Cardiopulmonary Resuscitation in Newborn Infants Translating Evidence From Animal Studies to the Bedside. JACC Basic Transl. Sci. 2019, 4, 116–121. [Google Scholar] [CrossRef]
- Solevåg, A.L.; Garcia-Hidalgo, C.; Cheung, P.-Y.; Lee, T.-F.; O’Reilly, M.; Schmölzer, G.M. Ventilation with 18, 21, or 100% Oxygen during Cardiopulmonary Resuscitation of Asphyxiated Piglets: A Randomized Controlled Animal Trial. Neonatology 2020, 117, 102–110. [Google Scholar] [CrossRef]
- Garcia-Hidalgo, C.; Solevåg, A.; Kim, S.Y.; Shim, G.-H.; Cheung, P.-Y.; Lee, T.-F.; O’Reilly, M.; Schmölzer, G.M. Sustained inflation with 21% versus 100% oxygen during cardiopulmonary resuscitation of asphyxiated newborn piglets—A randomized controlled animal study. Resuscitation 2020, 155, 39–47. [Google Scholar] [CrossRef]
- Garcia-Hidalgo, C.; Cheung, P.-Y.; Vento, M.; O’Reilly, M.; Schmölzer, G.M. A Review of Oxygen Use During Chest Compressions in Newborns—A Meta-Analysis of Animal Data. Front. Pediatr. 2018, 6, S196–S197. [Google Scholar] [CrossRef] [Green Version]
- Wang, C.-H.; Chang, W.-T.; Huang, C.-H.; Tsai, M.-S.; Yu, P.-H.; Wang, A.-Y.; Chen, N.-C.; Chen, W.-J. The effect of hyperoxia on survival following adult cardiac arrest: A systematic review and meta-analysis of observational studies. Resuscitation 2014, 85, 1142–1148. [Google Scholar] [CrossRef] [PubMed]
- Pilcher, J.; Weatherall, M.; Shirtcliffe, P.; Bellomo, R.; Young, P.; Beasley, R. The effect of hyperoxia following cardiac arrest—A systematic review and meta-analysis of animal trials. Resuscitation 2012, 83, 417–422. [Google Scholar] [CrossRef] [PubMed]
- Marquez, A.M.; Morgan, R.W.; Ko, T.; Landis, W.P.; Hefti, M.M.; Mavroudis, C.D.; McManus, M.J.; Karlsson, M.; Starr, J.; Roberts, A.L.; et al. Oxygen Exposure During Cardiopulmonary Resuscitation Is Associated with Cerebral Oxidative Injury in a Randomized, Blinded, Controlled, Preclinical Trial. J. Am. Heart Assoc. 2020, 9, e015032. [Google Scholar] [CrossRef] [PubMed]
- Kilkenny, C.; Altman, D.G.; Browne, W.J.; Cuthill, I.C.; Emerson, M. Improving Bioscience Research Reporting: The ARRIVE Guidelines for Reporting Animal Research. PLoS Biol. 2010, 8, e1000412. [Google Scholar] [CrossRef]
- Os, S.; Cheung, P.; Pichler, G.; Aziz, K.; O’Reilly, M.; Schmölzer, G.M. Exhaled carbon dioxide can be used to guide respiratory support in the delivery room. Acta Paediatr. 2014, 103, 796–806. [Google Scholar] [PubMed]
- Schmölzer, G.M.; Kamlin, C.O.F.; Dawson, J.A.; te Pas, A.B.; Morley, C.J.; Davis, P.G. Respiratory monitoring of neonatal resuscitation. Arch. Dis. Child.-Fetal Neonatal Ed. 2010, 95, F295–F303. [Google Scholar] [CrossRef]
- Pichler, G.; Binder, C.; Avian, A.; Beckenbach, E.; Schmölzer, G.M.; Urlesberger, B. Reference Ranges for Regional Cerebral Tissue Oxygen Saturation and Fractional Oxygen Extraction in Neonates during Immediate Transition after Birth. J. Pediatrics 2013, 163, 1558–1563. [Google Scholar] [CrossRef]
- Walson, K.H.; Tang, M.; Glumac, A.; Alexander, H.; Manole, M.D.; Ma, L.; Hsia, C.J.; Clark, R.S.; Kochanek, P.M.; Kagan, V.E.; et al. Normoxic versus hyperoxic resuscitation in pediatric asphyxial cardiac arrest: Effects on oxidative stress. Crit. Care Med. 2011, 39, 335–343. [Google Scholar]
- Liu, Y.; Rosenthal, R.E.; Haywood, Y.; Miljkovic-Lolic, M.; Vanderhoek, J.Y.; Fiskum, G. Normoxic Ventilation After Cardiac Arrest Reduces Oxidation of Brain Lipids and Improves Neurological Outcome. Stroke 1998, 29, 1679–1686. [Google Scholar] [CrossRef] [Green Version]
- De Caen, A.R.; Kleinman, M.E.; Chameides, L.; Atkins, D.L.; Berg, R.A.; Berg, M.D.; Bhanji, F.; Biarent, D.; Bingham, R.M.; Coovadia, A.H.; et al. Part 10: Paediatric basic and advanced life support: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Resuscitation 2010, 81 (Suppl. S1), e213–e259. [Google Scholar] [CrossRef] [PubMed]
- Kleinman, M.E.; Chameides, L.; Schexnayder, S.M.; Samson, R.A.; Hazinski, M.F.; Atkins, D.L.; Berg, M.D.; de Caen, A.R.; Fink, E.L.; Freid, E.B.; et al. Part 14: Pediatric Advanced Life Support. Circulation 2010, 122 (Suppl. S3), S876–S908. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sutton, R.M.; Reeder, R.W.; Landis, W.P.; Meert, K.L.; Yates, A.R.; Morgan, R.W.; Berger, J.T.; Newth, C.J.; Carcillo, J.A.; McQuillen, P.S.; et al. Ventilation Rates and Pediatric In-Hospital Cardiac Arrest Survival Outcomes. Crit. Care Med. 2019, 47, 1627–1636. [Google Scholar] [CrossRef] [PubMed]

| Sham(n = 4) | CC + SI | CCaV | p-Value | |||
|---|---|---|---|---|---|---|
| 21% Oxygen (n = 7) | 100% Oxygen (n = 7) | 21% Oxygen (n = 7) | 100% Oxygen (n = 7) | |||
| Age (days) | 22 (21–22) | 22 (21–23) | 22 (21–22) | 23 (21–25) | 22 (21–24) | 0.286 |
| Weight (kg) | 8.0 (7.4–8.6) | 7.9 (7.7–8.1) | 7.9 (7.0–8.6) | 7.8 (7.5–9.1) | 8.1 (6.9–9.3) | 0.889 |
| Sex (male/female) | 1/3 | 4/3 | 4/3 | 6/1 | 2/5 | 0.196 |
| Heart rate (bpm) | 147 (117–224) | 134 (127–145) | 144 (139–158) | 132 (128–148) | 154 (136–173) | 0.235 |
| MAP (mmHg) | 73 (64–82) | 68 (62–77) | 61 (55–72) | 70 (61–88) | 63 (60–65) | 0.198 |
| Carotid flow (mL/min) | 73 (62–96) | 71 (52–85) | 77 (66–129) | 74 (55–82) | 66 (46–85) | 0.574 |
| Cerebral oxygenation (%) | 52 (49–53) | 51 (46–57) | 67 (45–77) | 57 (53–67) | 60 (44–75) | 0.489 |
| pH | 7.39 (7.33–7.46) | 7.42 (7.35–7.46) | 7.46 (7.42–7.49) | 7.47 (7.41–7.48) | 7.44 (7.40–7.49) | 0.351 |
| Base excess (mmol/L) | 2 (−3.3~4.3) | 0 (−2.0~4.0) | 2 (0~3.0) | 2 (1.0~3.1) | 2 (1.0~3.0) | 0.649 |
| paCO2 (torr) | 39 (32–40) | 39 (36–42) | 37 (36–38) | 36 (35–39) | 38 (36–42) | 0.942 |
| SaO2 (%) | 97 (97–99) | 98 (96–98) | 98 (94–99) | 99 (99–99) | 96 (94–99) | 0.181 |
| Lactate (mmol/L) | 2.1 (1.6–4.8) | 2.1 (1.8–2.9) | 2.4 (2.2–2.9) | 2.1 (1.7–3.3) | 2.4 (1.8–2.5) | 0.878 |
| CC + SI | CCaV | p-Value | ||||
|---|---|---|---|---|---|---|
| 21% Oxygen (n = 7) | 100% Oxygen (n = 7) | 21% Oxygen (n = 7) | 100% Oxygen (n = 7) | |||
| Asphyxia time (s) † | 330 (305–451) | 350 (324–429) | 315 (263–435) | 335 (240–435) | 0.91 | |
| Immediately before resuscitation | pH† | 6.94 (6.93–7.07) | 7.02 (6.89–7.12) | 7.09 (6.94–7.14) | 7.04 (6.95–7.13) | 0.46 |
| paCO2 (torr) † | 107 (83–114) | 88 (74–103) | 89 (80–110) | 94 (84–105) | 0.52 | |
| Lactate (mmol/L) † | 9.7 (8.8–10.4) | 9.0 (7.4–11.9) | 8.2 (6.3–9.1) | 7.6 (6.5–9.5) | 0.24 | |
| Base excess (mmol/L) | −8 (−10~−6) | −8 (-11~−5) | −6 (−9~−2) | −3 (−9~−2) | 0.19 | |
| Resuscitation | Received epinephrine (n) | 6 (86%) | 7 (100%) | 5 (71%) | 7 (100%) | 0.25 |
| Epinephrine doses (n) † | 1 (1–7) | 2 (1–3) | 9 (0–9) | 9 (1–9) | 0.33 | |
| Ringer solution bolus (mL) † | 10 (10–80) | 20 (5–25) | 75 (0–90) | 70 (5–90) | 0.37 | |
| Achieving ROSC | 6 (86%) | 6 (86%) | 3 (43%) | 3 (43%) | 0.13 | |
| ROSC time (s) † | 107 (90–440) | 140 (105–200) | 600 (50–600) | 600 (95–600) | 0.27 | |
| Survival after ROSC | 5 (83%) | 6 (100%) | 3 (100%) | 3 (100%) | 0.55 | |
| Sham | CC + SI | CCaV | p-Value | |||
|---|---|---|---|---|---|---|
| 21% Oxygen | 100% Oxygen | 21% Oxygen | 100% Oxygen | |||
| pH | ||||||
| Baseline | 7.39 (7.33–7.46) | 7.42 (7.35–7.46) | 7.46 (7.42–7.49) | 7.47 (7.41–7.48) | 7.44 (7.40–7.49) | 0.351 |
| After asphyxiation | N/A | 6.94 (6.93–7.07) # | 7.02 (6.89–7.12) # | 7.09 (6.94–7.14) # | 7.04 (6.96–7.13) # | 0.460 |
| 30 min after resuscitation | 7.42 (7.38–7.463) | 7.35 (7.26–7.40) | 7.29 (7.17–7.34) | 7.32 (7.19–7.36) | 7.38 (7.24–7.46) | 0.178 |
| PaCO2 (torr) | ||||||
| Baseline | 39 (32–40) | 39 (36–42) | 37 (36–38) | 36 (35–39) | 38 (36–42) | 0.942 |
| After asphyxiation | N/A | 106 (83–114) # | 88 (74–103) # | 89 (80–110) # | 94 (84–105) # | 0.516 |
| 30 min after resuscitation | 36 (34–40) | 39 (29–44) | 40 (38–56) | 37 (36–52) | 37 (31–42) | 0.456 |
| Base excess (mmol/L) | ||||||
| Baseline | 2 (−3~4) | 0 (−2~4) | 2 (0~3) | 2 (1~ 3) | 2 (1~3) | 0.649 |
| After asphyxiation | N/A | −8 (−10~−6) # | −8 (−11~−5) # | −6 (−9~ −2) # | −5 (−9~−3) # | 0.335 |
| 30 min after resuscitation | 1 (−4~3) | −6 (−9~−4) * # | −7 (−11~−6) * # | −7 (−8~ −5) * # | −9 (−10~−4) * # | 0.033 |
| Lactate (mmol/L) | ||||||
| Baseline | 2.1 (1.6–4.8) | 2.1 (1.8–2.9) | 2.4 (2.2–2.9) | 2.1 (1.7–3.3) | 2.4 (1.8–2.5) | 0.878 |
| After asphyxiation | N/A | 9.7 (8.8–10.5) # | 9.0 (7.4–11.9) # | 8.2 (6.3–9.1) # | 7.6 (6.5–9.5) # | 0.235 |
| 30 min after resuscitation | 2.4 (1.8–4.8) | 6.9 (5.6–8.6) * # | 8.2 (6.7–10.2) * # | 7.3 (6.5–8.6) * # | 7.0 (6.8–8.7) * # | 0.007 |
| Respiratory Parameter | CC + SI + 21% O2 (n = 7) | CC + SI + 100% O2 (n = 7) | CCaV + 21% O2 (n = 7) | CCaV + 100% O2 (n = 7) | p-Value |
|---|---|---|---|---|---|
| Positive End Expiratory Pressure (cmH2O) | 31.6 (4.3) * | 27.3 (3.1) * | 6.8 (0.6) | 7.2 (1.1) | <0.001 |
| Peak Inflation Flow (mL/min) | 7.4 (1.2) | 6.8 (1.1) | 3.7 (1.2) | 4.2 (-1.5) | 0.794 |
| Peak Expiratory Flow (mL/min) | −15.5 (3.4) | −13.4 (2.0) | −8.0 (3.5) | −7.3 (3.8) | 0.618 |
| Tidal Volume (mL/kg) # | 25.4 (6.2) | 22.4 (6.9) | 19.8 (8.2) | 18.8 (9.9) | 0.675 |
| Minute Ventilation (mL/min) # | 2678 (664) * | 2418 (591) * | 401 (172) | 530 (436) | 0.003 |
| Sham | CC + SI | CCaV | p-Value | |||
|---|---|---|---|---|---|---|
| (n = 4) | 21% Oxygen (n = 5) | 100% Oxygen (n = 6) | 21% Oxygen (n = 3) | 100% Oxygen (n = 3) | ||
| Left ventricle | ||||||
| GSSG (µM/mg protein) | 171 (28) | 191 (54) | 248 (123) | 177 (49) | 177 (52) | 0.53 |
| GSH (µM/mg protein) | 879 (158) | 805 (158) | 1029 (394) | 1130 (311) | 662 (60) | 0.44 |
| GSSG/GSH | 0.19 (0.05) | 0.24 (0.07) | 0.26 (0.1) | 0.17 (0.03) | 0.27 (0.08) | 0.32 |
| Lactate (µM/mg protein) | 0.11 (0.05) | 0.33 (0.15)* | 0.28 (0.06) | 0.23 (0.04) | 0.29 (0.06) | 0.015 |
| Lung | ||||||
| GSSG (µM/mg protein) | 138 (32) | 185 (59) | 198 (51) | 169 (46) | 201 (31) | 0.47 |
| GSH (µM/mg protein) | 909 (121) | 883 (155) | 802 (314) | 712 (173) | 583 (197) | 0.49 |
| GSSG/GSH | 0.15 (0.04) | 0.21 (0.09) | 0.28 (0.1) | 0.25 (0.09) | 0.41 (0.21) | 0.07 |
| Lactate (µM/mg protein) | 0.15 (0.02) | 0.25 (0.03) | 0.27 (0.03)* | 0.25 (0.03) | 0.34 (0.3) * | 0.004 |
| Brain | ||||||
| GSSG (µM/mg protein) | 129 (31) | 119 (41) | 197 (48) | 117 (28) | 106 (22) | 0.07 |
| GSH (µM/mg protein) | 797 (226) | 638 (205) | 606 (235) | 633 (307) | 438 (213) | 0.55 |
| GSSG/GSH | 0.19 (0.05) | 0.22 (0.12) | 0.35 (0.13) | 0.25 (0.17) | 0.34 (0.21) | 0.39 |
| Lactate (µM/mg protein) | 0.12 (0.02) | 0.25 (0.05) * | 0.22 (0.01) | 0.23 (0.04) | 0.29 (0.13) * | 0.010 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nyame, S.; Cheung, P.-Y.; Lee, T.-F.; O’Reilly, M.; Schmölzer, G.M. A Randomized, Controlled Animal Study: 21% or 100% Oxygen during Cardiopulmonary Resuscitation in Asphyxiated Infant Piglets. Children 2022, 9, 1601. https://doi.org/10.3390/children9111601
Nyame S, Cheung P-Y, Lee T-F, O’Reilly M, Schmölzer GM. A Randomized, Controlled Animal Study: 21% or 100% Oxygen during Cardiopulmonary Resuscitation in Asphyxiated Infant Piglets. Children. 2022; 9(11):1601. https://doi.org/10.3390/children9111601
Chicago/Turabian StyleNyame, Solomon, Po-Yin Cheung, Tez-Fun Lee, Megan O’Reilly, and Georg M. Schmölzer. 2022. "A Randomized, Controlled Animal Study: 21% or 100% Oxygen during Cardiopulmonary Resuscitation in Asphyxiated Infant Piglets" Children 9, no. 11: 1601. https://doi.org/10.3390/children9111601






