Perceived Changes in Emotions, Worries and Everyday Behaviors in Children and Adolescents Aged 5–18 Years with Type 1 Diabetes during the COVID-19 Pandemic
Abstract
:1. Introduction
2. Materials and Methods
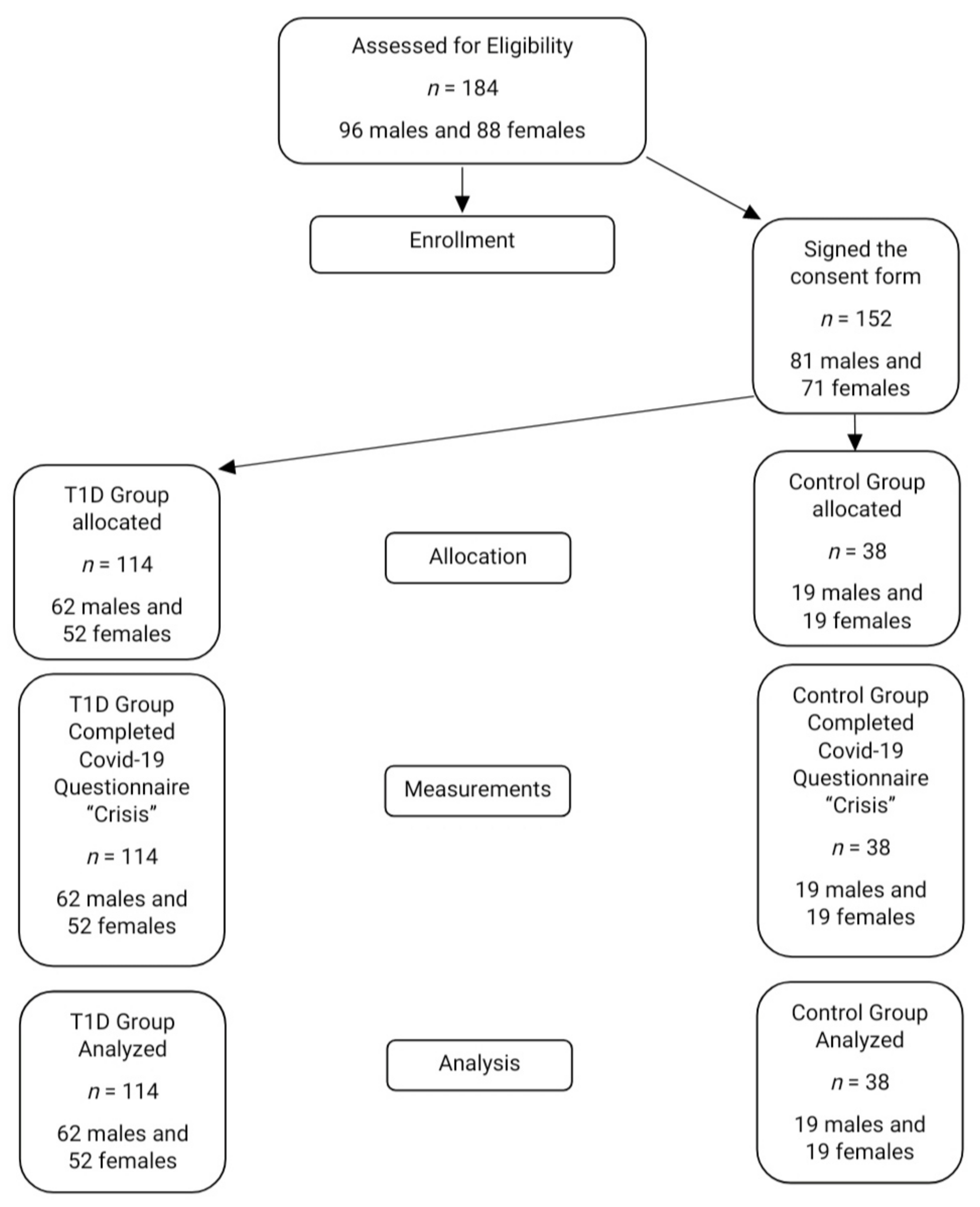
2.1. Procedure
2.2. Participants
2.3. Questionnaire
2.4. Statistical Analysis
2.4.1. Variables Extrapolated from the CRISIS Questionnaire
2.4.2. Outcome and Types of Analyses
3. Results
3.1. Descriptive Statistics
3.2. Exploratory Analyses
3.3. SEM for the EW-D
3.4. Changes in Items in the Domains “Daily behaviors” and “Use of digital media”
4. Discussion
4.1. Emotional and Psychological Effects
4.2. Behavioral Effects
5. Strengths, Limitations and Suggestions for Future Research
6. Conclusions—Future Perspectives
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CRISIS | The CoRonavIruS Health Impact Survey |
| T1D | Type 1 Diabetes |
| HV | Healthy Volunteers |
| EW | Emotion/Worries |
| EW-B | Emotions/Worries-Before |
| EW-D | Emotions/Worries-During |
| LC | Life Changes due to COVID-19 Crisis in the past two weeks |
| ICC SEM | Intraclass Correlation Coefficient structural equation model analysis |
| RMSEA | root mean square error of approximation |
| SRMR | standardized root mean squared residual |
| CDet | coefficient of determination |
| AIC | Akaike information criterion |
| BIC | Bayesian information criterion |
References
- WHO Novel Coronavirus—China. Available online: http://www.who.int/csr/don/12-january-2020-novel-coronavirus-china/en/ (accessed on 12 January 2020).
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [Green Version]
- Valencia, D.N. Brief Review on COVID-19: The 2020 Pandemic Caused by SARS-CoV-2. Cureus 2020, 12, e7386. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- WHO Coronavirus Disease (COVID-19) Pandemic. 2020. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 20 March 2020).
- Centers for Disease Control and Prevention. 2020. Available online: https://www.cdc.gov/coronavirus/2019-ncov/cases-updates/summary.html (accessed on 20 March 2020).
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical Characteristics of 138 Hospitalized Patients with 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA 2020, 323, 1061–1069. [Google Scholar] [CrossRef] [PubMed]
- Greek Ministry of Health. Preventive Measures for COVID-19 Pandemic. COVID-19. gov. gr. Available online: https://covid19.gov.gr/category/proliptika-metra-gia-tin-pandimia/ (accessed on 5 April 2020).
- Dong, L.; Bouey, J. Public Mental Health Crisis during COVID-19 Pandemic, China. Emerg. Infect. Dis. 2020, 26, 1616–1618. [Google Scholar] [CrossRef] [PubMed]
- Tucci, V.; Moukaddam, N.; Meadows, J.; Shah, S.; Galwankar, S.C.; Kapur, G.B. The Forgotten Plague: Psychiatric Manifestations of Ebola, Zika, and Emerging Infectious Diseases. J. Glob. Infect. Dis. 2017, 9, 151–156. [Google Scholar] [CrossRef]
- Bai, Y.; Lin, C.C.; Lin, C.Y.; Chen, J.Y.; Chue, C.M.; Chou, P. Survey of stress reactions among health care workers involved with the SARS outbreak. Psychiatr. Serv. 2004, 55, 1055–1057. [Google Scholar] [CrossRef]
- Hawryluck, L.; Gold, W.L.; Robinson, S.; Pogorski, S.; Galea, S.; Styra, R. SARS control and psychological effects of quarantine, Toronto, Canada. Emerg. Infect. Dis. 2004, 10, 1206–1212. [Google Scholar] [CrossRef]
- Wu, P.; Fang, Y.; Guan, Z.; Fan, B.; Kong, J.; Yao, Z.; Liu, X.; Fuller, C.J.; Susser, E.; Lu, J.; et al. The psychological impact of the SARS epidemic on hospital employees in China: Exposure, risk perception, and altruistic acceptance of risk. Can. J. Psychiatry 2009, 54, 302–311. [Google Scholar] [CrossRef]
- Maunder, R.; Hunter, J.; Vincent, L.; Bennett, J.; Peladeau, N.; Leszcz, M.; Sadavoy, J.; Verhaeghe, L.M.; Steinberg, R.; Mazzulli, T. The immediate psychological and occupational impact of the 2003 SARS outbreak in a teaching hospital. CMAJ 2003, 168, 1245–1251. [Google Scholar]
- Prati, G.; Mancini, A.D. The psychological impact of COVID-19 pandemic lockdowns: A review and meta-analysis of longitudinal studies and natural experiments. Psychol. Med. 2021, 51, 201–211. [Google Scholar] [CrossRef]
- Ludvigsson, J.F. Systematic review of COVID-19 in children shows milder cases and a better prognosis than adults. Acta Paediatr. 2020, 109, 1088–1095. [Google Scholar] [CrossRef] [PubMed]
- Ezpeleta, L.; Navarro, J.B.; de la Osa, N.; Trepat, E.; Penelo, E. Life Conditions during COVID-19 Lockdown and Mental Health in Spanish Adolescents. Int. J. Environ. Res. Public Health 2020, 17, 7327. [Google Scholar] [CrossRef] [PubMed]
- Panda, P.K.; Gupta, J.; Chowdhury, S.R.; Kumar, R.; Meena, A.K.; Madaan, P.; Sharawat, I.K.; Gulati, S. Psychological and Behavioral Impact of Lockdown and Quarantine Measures for COVID-19 Pandemic on Children, Adolescents and Caregivers: A Systematic Review and Meta-Analysis. J. Trop. Pediatr. 2021, 67, fmaa122. [Google Scholar] [CrossRef]
- Bornstein, S.R.; Rubino, F.; Khunti, K.; Mingrone, G.; Hopkins, D.; Birkenfeld, A.L.; Boehm, B.; Amiel, S.; Holt, R.I.; Skyler, J.S.; et al. Practical recommendations for the management of diabetes in patients with COVID-19. Lancet Diabetes Endocrinol. 2020, 8, 546–550. [Google Scholar] [CrossRef]
- Hespanhol, V.; Bárbara, C. Pneumonia mortality, comorbidities matter? Pulmonology 2020, 26, 123–129. [Google Scholar] [CrossRef]
- Zou, Q.; Zheng, S.; Wang, X.; Liu, S.; Bao, J.; Yu, F.; Wu, W.; Wang, X.; Shen, B.; Zhou, T.; et al. Influenza A-associated severe pneumonia in hospitalized patients: Risk factors and NAI treatments. Int. J. Infect. Dis. 2020, 92, 208–213. [Google Scholar] [CrossRef] [Green Version]
- Cardona-Hernandez, R.; Cherubini, V.; Iafusco, D.; Schiaffini, R.; Luo, X.; Maahs, D.M. Children and youth with diabetes are not at increased risk for hospitalization due to COVID-19. Pediatr. Diabetes 2021, 22, 202–206. [Google Scholar] [CrossRef]
- Brazendale, K.; Beets, M.W.; Weaver, R.G.; Pate, R.R.; Turner-McGrievy, G.M.; Kaczynski, A.T.; Chandler, J.L.; Bohnert, A.; von Hippel, P.T. Understanding differences between summer vs. school obesogenic behaviors of children: The structured days hypothesis. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 100. [Google Scholar] [CrossRef]
- Leggett, C.; Giles, L.; Anderson, J.; Doogue, M.; Couper, J.; Pena, A.S. Adherence to metformin is reduced during school holidays and weekends in children with type 1 diabetes participating in a randomised controlled trial. Arch. Dis. Child. 2019, 104, 890–894. [Google Scholar] [CrossRef]
- The Coronavirus Impact Health Survey (Crisis). Available online: http://www.crisissurvey.org/ (accessed on 3 May 2020).
- Nikolaidis, A.; Paksarian, D.; Alexander, L.; Derosa, J.; Dunn, J.; Nielson, D.M.; Droney, I.; Kang, M.; Douka, I.; Bromet, E.; et al. The Coronavirus Health and Impact Survey (CRISIS) reveals reproducible correlates of pandemic-related mood states across the Atlantic. Sci. Rep. 2021, 11, 8139. [Google Scholar] [CrossRef]
- Korpa, T.; Pappa, T.; Chouliaras, G.; Sfinari, A.; Eleftheriades, A.; Katsounas, M.; Kanaka-Gantenbein, C.; Pervanidou, P. Daily Behaviors, Worries and Emotions in Children and Adolescents with ADHD and Learning Difficulties during the COVID-19 Pandemic. Children 2021, 8, 995. [Google Scholar] [CrossRef] [PubMed]
- Hossain, M.M.; Sultana, A.; Purohit, N. Mental health outcomes of quarantine and isolation for infection prevention: A systematic umbrella review of the global evidence. Epidemiol. Health 2020, 42, e2020038. [Google Scholar] [CrossRef]
- Chen, Y.; Feeley, T.H. Social support, social strain, loneliness, and well-being among older adults: An analysis of the Health and Retirement Study *. J. Soc. Pers. Relatsh. 2014, 31, 141–161. [Google Scholar] [CrossRef]
- Jiao, W.Y.; Wang, L.N.; Liu, J.; Fang, S.F.; Jiao, F.Y.; Pettoello-Mantovani, M.; Somekh, E. Behavioral and Emotional Disorders in Children during the COVID-19. Epidemic. J. Pediatr. 2020, 221, 264–266.e1. [Google Scholar] [CrossRef]
- Wang, G.; Zhang, Y.; Zhao, J.; Zhang, J.; Jiang, F. Mitigate the effects of home confinement on children during the COVID-19 outbreak. Lancet 2020, 395, 945–947. [Google Scholar] [CrossRef]
- Ravaldi, C.; Ricca, V.; Wilson, A.; Homer, C.; Vannacci, A. Previous psychopathology predicted severe COVID-19 concern, anxiety, and PTSD symptoms in pregnant women during “lockdown” in Italy. Arch. Women’s Ment. Health 2020, 23, 783–786. [Google Scholar] [CrossRef] [PubMed]
- Kovacs, M.; Goldston, D.; Obrosky, D.S.; Bonar, L.K. Psychiatric disorders in youths with IDDM: Rates and risk factors. Diabetes Care 1997, 20, 36–44. [Google Scholar] [CrossRef]
- Merikangas, K.R.; He, J.P.; Burstein, M.; Swanson, S.A.; Avenevoli, S.; Cui, L.; Benjet, C.; Georgiades, K.; Swendsen, J. Lifetime prevalence of mental disorders in U.S. adolescents: Results from the National Comorbidity Survey Replication—Adolescent Supplement (NCS-A). J. Am. Acad. Child Adolesc. Psychiatry 2010, 49, 980–989. [Google Scholar] [CrossRef] [Green Version]
- United Nations Educational, Scientific and Cultural Organization (UNESCO). COVID-19 Educational Disruption and Response. Available online: https://en.unesco.org/covid19/educationresponse (accessed on 10 May 2020).
- Zhou, S.J.; Zhang, L.G.; Wang, L.L.; Guo, Z.C.; Wang, J.Q.; Chen, J.C.; Liu, M.; Chen, X.; Chen, J.X. Prevalence and socio-demographic correlates of psychological health problems in Chinese adolescents during the outbreak of COVID-19. Eur. Child Adolesc. Psychiatry 2020, 29, 749–758. [Google Scholar] [CrossRef]
- Monzon, A.; Kahhan, N.; Marker, A.; Patton, S. Challenges and Considerations for Reducing Diabetes Distress and Fear of Hypoglycemia in Parents of Youth with Type 1 Diabetes During the COVID-19 Pandemic. JMIR Pediatr. Parent. 2021, 4, e25106. [Google Scholar] [CrossRef]
- Gruhn, M.A.; Lord, J.H.; Jaser, S.S. Collaborative and Overinvolved Parenting Differentially Predict Outcomes in Adolescents with Type 1 Diabetes. Health Psychol. 2016, 35, 652. [Google Scholar] [CrossRef] [PubMed]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Xie, X.; Xue, Q.; Zhou, Y.; Zhu, K.; Liu, Q.; Zhang, J.; Song, R. Mental Health Status Among Children in Home Confinement During the Coronavirus Disease 2019 Outbreak in Hubei Province, China. JAMA Pediatr. 2020, 174, 898–900. [Google Scholar] [CrossRef] [Green Version]
- Faccioli, S.; Lombardi, F.; Bellini, P.; Costi, S.; Sassi, S.; Pesci, M.C. How Did Italian Adolescents with Disability and Parents Deal with the COVID-19 Emergency? Int. J. Environ. Res. Public Health 2021, 18, 1687. [Google Scholar] [CrossRef]
- Rosenberg, A.R.; Bradford, M.C.; Barton, K.S.; Etsekson, N.; McCauley, E.; Curtis, J.R.; Wolfe, J.; Baker, K.S.; Yi-Frazier, J.P. Hope and benefit finding: Results from the PRISM randomized controlled trial. Pediatr. Blood Cancer 2019, 66, e27485. [Google Scholar] [CrossRef] [PubMed]
- Tran, V.; Wiebe, D.J.; Fortenberry, K.T.; Butler, J.M.; Berg, C.A. Benefit finding, affective reactions to diabetes stress, and diabetes management among early adolescents. Health Psychol. 2011, 30, 212–219. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tang, S.; Xiang, M.; Cheung, T.; Xiang, Y.T. Mental health and its correlates among children and adolescents during COVID-19 school closure: The importance of parent-child discussion. J. Affect. Disord. 2021, 279, 353–360. [Google Scholar] [CrossRef] [PubMed]
- Cancello, R.; Soranna, D.; Zambra, G.; Zambon, A.; Invitti, C. Determinants of the Lifestyle Changes during COVID-19 Pandemic in the Residents of Northern Italy. Int. J. Environ. Res. Public Health 2020, 17, 6287. [Google Scholar] [CrossRef]
- Morin, C.M.; Carrier, J.; Bastien, C.; Godbout, R. Canadian Sleep and Circadian Network. Sleep and circadian rhythm in response to the COVID-19 pandemic. Can. J. Public Health 2020, 111, 654–657. [Google Scholar] [CrossRef]
- Sinha, M.; Pande, B.; Sinha, R. Impact of COVID-19 lockdown on sleep-wake schedule and associated lifestyle related behavior: A national survey. J. Public Health Res. 2020, 9, 1826. [Google Scholar] [CrossRef]
- Di Renzo, L.; Gualtieri, P.; Pivari, F.; Soldati, L.; Attinà, A.; Cinelli, G.; Leggeri, C.; Caparello, G.; Barrea, L.; Scerbo, F.; et al. Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J. Transl. Med. 2020, 18, 229. [Google Scholar] [CrossRef] [PubMed]
- López-Bueno, R.; Calatayud, J.; Casaña, J.; Casajús, J.A.; Smith, L.; Tully, M.A.; Andersen, L.L.; López-Sánchez, G.F. COVID-19 Confinement and Health Risk Behaviors in Spain. Front. Psychol. 2020, 11, 1426. [Google Scholar] [CrossRef] [PubMed]
- Dellagiulia, A.; Lionetti, F.; Fasolo, M.; Verderame, C.; Sperati, A.; Alessandri, G. Early impact of COVID-19 lockdown on children’s sleep: A 4-week longitudinal study. J. Clin. Sleep Med. 2020, 16, 1639–1640. [Google Scholar] [CrossRef] [PubMed]
- Ammar, A.; Brach, M.; Trabelsi, K.; Chtourou, H.; Boukhris, O.; Masmoudi, L.; Bouaziz, B.; Bentlage, E.; How, D.; Ahmed, M.; et al. Effects of COVID-19 Home Confinement on Eating Behaviour and Physical Activity: Results of the ECLB-COVID19 International Online Survey. Nutrients 2020, 12, 1583. [Google Scholar] [CrossRef]
- Romero-Blanco, C.; Rodríguez-Almagro, J.; Onieva-Zafra, M.D.; Parra-Fernández, M.L.; Prado-Laguna, M.D.C.; Hernández-Martínez, A. Physical Activity and Sedentary Lifestyle in University Students: Changes during Confinement Due to the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 6567. [Google Scholar] [CrossRef]
- Huckins, J.F.; da Silva, A.W.; Wang, W.; Hedlund, E.; Rogers, C.; Nepal, S.K.; Wu, J.; Obuchi, M.; Murphy, E.I.; Meyer, M.L.; et al. Mental Health and Behavior of College Students during the Early Phases of the COVID-19 Pandemic: Longitudinal Smartphone and Ecological Momentary Assessment Study. J. Med. Internet Res. 2020, 22, e20185. [Google Scholar] [CrossRef]
- Deschasaux-Tanguy, M.; Druesne-Pecollo, N.; Esseddik, Y.; de Edelenyi, F.S.; Allès, B.; Andreeva, V.A.; Baudry, J.; Charreire, H.; Deschamps, V.; Egnell, M.; et al. Diet and physical activity during the coronavirus disease 2019 (COVID-19) lockdown (March–May 2020): Results from the French NutriNet-Santé cohort study. Am. J Clin. Nutr. 2021, 113, 924–938. [Google Scholar] [CrossRef]
- Dunton, G.F.; Do, B.; Wang, S.D. Early effects of the COVID-19 pandemic on physical activity and sedentary behavior in children living in the U.S. BMC Public Health 2020, 20, 1351. [Google Scholar] [CrossRef]
- Pietrobelli, A.; Pecoraro, L.; Ferruzzi, A.; Heo, M.; Faith, M.; Zoller, T.; Antoniazzi, F.; Piacentini, G.; Fearnbach, S.N.; Heymsfield, S.B. Effects of COVID-19 Lockdown on Lifestyle Behaviors in Children with Obesity Living in Verona, Italy: A Longitudinal Study. Obesity 2020, 28, 1382–1385. [Google Scholar] [CrossRef]
- Jung, S.J.; Winning, A.; Roberts, A.L.; Nishimi, K.; Chen, Q.; Gilsanz, P.; Sumner, J.A.; Fernandez, C.A.; Rimm, E.B.; Kubzansky, L.D.; et al. Posttraumatic stress disorder symptoms and television viewing patterns in the Nurses’ Health Study II: A longitudinal analysis. PLoS ONE 2019, 14, e0213441. [Google Scholar] [CrossRef]
- Šmotek, M.; Fárková, E.; Manková, D.; Kopřivová, J. Evening and night exposure to screens of media devices and its association with subjectively perceived sleep: Should “light hygiene” be given more attention? Sleep Health 2020, 6, 498–505. [Google Scholar] [CrossRef] [PubMed]
- Ryan, T.; Chester, A.; Reece, J.; Xenos, S. The uses and abuses of Facebook: A review of Facebook addiction. J. Behav. Addict. 2014, 3, 133–148. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- von der Heiden, J.M.; Braun, B.; Müller, K.W.; Egloff, B. The Association between Video Gaming and Psychological Functioning. Front. Psychol. 2019, 10, 1731. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chóliz, M. The Challenge of Online Gambling: The Effect of Legalization on the Increase in Online Gambling Addiction. J. Gambl. Stud. 2016, 32, 749–756. [Google Scholar] [CrossRef]
- American Diabetes Association. 5. Facilitating Behavior Change and Well-being to Improve Health Outcomes: Standards of Medical Care in Diabetes-2020. Diabetes Care 2020, 43 (Suppl. S1), S48–S65. [Google Scholar] [CrossRef] [Green Version]
- De Pasquale, C.; Chiappedi, M.; Sciacca, F.; Martinelli, V.; Hichy, Z. Online Videogames Use and Anxiety in Children during the COVID-19 Pandemic. Children 2021, 8, 205. [Google Scholar] [CrossRef]
- Ko, C.H.; Yen, J.Y. Impact of COVID-19 on gaming disorder: Monitoring and prevention. J. Behav. Addict. 2020, 9, 187–189. [Google Scholar] [CrossRef]

| T1D-Patients | Controls | p-Value | |
|---|---|---|---|
| Caregiver age, years | 44.4 ± 5.9, 45 (40, 48) | 43.4 ± 6.2, 44.5 (38, 49) | 0.37 |
| Caregiver relation to child | 0.14 | ||
| Mother | 80 (70.2) | 21 (55.3) | |
| Father | 32 (28.1) | 17 (44.7) | |
| Grandparent | 2 (1.7) | 0 (0.0) | |
| Greek origin | 104 (91.2) | 35 (92.1) | 0.99 |
| Living area | 0.015 | ||
| Large city | 70 (61.4) | 30 (79.0) | |
| Small city | 27 (23.7) | 8 (21.0) | |
| Village | 17 (14.9) | 0 (0.0) | |
| Single parent family | 13 (11.4) | 6 (15.8) | 0.57 |
| Presence of elderly people at home | 5 (4.4) | 2 (5.3) | 0.99 |
| Presence of other children at home | 79 (69.3) | 27 (71.1) | 0.99 |
| Number of other persons at home | 2.9 ± 1.0, 3 (2, 3) | 2.8 ± 0.9, 3 (2, 3) | 0.48 |
| Working during lockdown | 84 (73.7) | 35 (92.1) | 0.022 |
| Working but living at home | 84 (100.0) | 35 (100.0) | n.a a |
| Health care worker | 2 (2.4) | 0 (0.0) | 0.99 |
| Number of rooms at home | 5.2 ± 1.1, 5 (5, 6) | 5.4 ± 1.0, 5 (5, 6) | 0.46 |
| Insurance | 114 (100.0) | 38 (100.0) | n.a a |
| Subsidy | 108 (94.7) | 2 (5.3) | <0.001 |
| Child’s physical health status according to caregiver, n (%) | <0.001 | ||
| Excellent | 49 (43.0) | 32 (84.2) | |
| Very good | 49 (43.0) | 6 (15.8) | |
| Good | 10 (8.8) | 0 (0.0) | |
| Fair | 6 (5.2) | 0 (0.0) | |
| Poor | 0 (0.0) | 0 (0.0) | |
| Child’s mental health status according to caregiver, n (%) | <0.001 | ||
| Excellent | 45 (39.5) | 34 (89.5) | |
| Very good | 56 (49.1) | 4 (10.5) | |
| Good | 8 (7.0) | 0 (0.0) | |
| Fair | 5 (4.4) | 0 (0.0) | |
| Poor | 0 (0.0) | 0 (0.0) |
| logEW-B | β-Coefficient | 95% ci | p-Value |
|---|---|---|---|
| Single parent family, yes vs. no | 0.121 | 0.024, 0.218 | 0.014 |
| Child’s age | 0.012 | 0.004, 0.021 | 0.005 |
| Health support, yes vs. no | 0.105 | 0.026, 0.185 | 0.009 |
| logEW-D | |||
| logEW-B | 0.435 | 0.335, 0.535 | <0.001 |
| logCOVID-worries | 0.080 | 0.023, 0.137 | 0.006 |
| Number of persons at home | 0.035 | 0.009, 0.061 | 0.007 |
| Stress due to restrictions | 0.036 | 0.011, 0.061 | 0.005 |
| Stress due to changes in relations with friends | 0.026 | 0.002, 0.050 | 0.035 |
| Optimism about a hopeful ending | −0.029 | −0.050, −0.008 | 0.008 |
| Stress due to change in family relations | 0.146 | 0.054, 0.237 | 0.002 |
| Interaction quality of family relations × family stress | −0.072 | −0.102, −0.042 | <0.001 |
| Interaction T1D-patients × number of children at home | −0.118 | −0.171, −0.065 | <0.001 |
| Interaction T1D-patients × financial problems | 0.057 | 0.031, 0.082 | <0.001 |
| Interaction T1D-patients × event cancellation | 0.029 | 0.013, 0.045 | 0.001 |
| Gender, females vs. males | −0.061 | −0.102, −0.021 | 0.003 |
| Child’s age | −0.006 | −0.011, −0.0003 | 0.038 |
| Interaction T1D-patients × number of children at home | |||
| Number of children at home | 0.755 | 0.687, 0.824 | <0.001 |
| T1D-patients vs. controls | 0.705 | 0.632, 0.778 | <0.001 |
| Interaction T1D-patients × financial problems | |||
| Financial problems | 0.958 | 0.926, 0.990 | <0.001 |
| T1D-patients vs. controls | 1.117 | 1.061, 1.173 | <0.001 |
| Interaction T1D-patients × event cancellation | |||
| Event cancellation | 0.782 | 0.716, 0.848 | <0.001 |
| T1D-patients vs. controls | 2.152 | 1.960, 2.345 | <0.001 |
| Interaction quality of family relations × family stress | |||
| Change in quality of family relations | 1.037 | 1.009, 1.065 | <0.001 |
| Stress due to changes in family relations | 2.964 | 2.929, 3.000 | <0.001 |
| Measure of Goodness-of-Fit | Result |
|---|---|
| Chi-square test a | 81.145 (81), 0.475 |
| RMSEA b | 0.003 (<0.001, 0.046), 0.973 |
| SRMR c | 0.042 |
| CDet d | 1.000 |
| Item (Probability of Worsening) | T1D Patients (n = 114) | Controls (n = 38) | p-Value |
|---|---|---|---|
| Bedtime weekdays (later) | 77 (67.5%) | 33 (86.8%) | 0.022 |
| Bedtime weekend (later) | 71 (62.3%) | 26 (68.4%) | 0.56 |
| Sleeping hours weekdays (more) | 52 (45.6%) | 21 (55.3%) | 0.35 |
| Sleeping hours weekend (more) | 50 (43.9%) | 12 (31.6%) | 0.25 |
| Physical exercise (less) | 45 (39.5%) | 20 (52.6%) | 0.19 |
| Time spent outdoors (less) | 84 (73.7%) | 32 (84.2%) | 0.27 |
| TV (more) | 98 (86.0%) | 37 (97.4%) | 0.07 |
| Social media (more) | 52 (45.6%) | 20 (52.6%) | 0.46 |
| Video games (more) | 60 (52.6%) | 17 (44.7%) | 0.45 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sfinari, A.; Pervanidou, P.; Chouliaras, G.; Zoumakis, E.; Vasilakis, I.A.; Nicolaides, N.C.; Kanaka-Gantenbein, C. Perceived Changes in Emotions, Worries and Everyday Behaviors in Children and Adolescents Aged 5–18 Years with Type 1 Diabetes during the COVID-19 Pandemic. Children 2022, 9, 736. https://doi.org/10.3390/children9050736
Sfinari A, Pervanidou P, Chouliaras G, Zoumakis E, Vasilakis IA, Nicolaides NC, Kanaka-Gantenbein C. Perceived Changes in Emotions, Worries and Everyday Behaviors in Children and Adolescents Aged 5–18 Years with Type 1 Diabetes during the COVID-19 Pandemic. Children. 2022; 9(5):736. https://doi.org/10.3390/children9050736
Chicago/Turabian StyleSfinari, Anastasia, Panagiota Pervanidou, Giorgos Chouliaras, Emmanouil Zoumakis, Ioannis A. Vasilakis, Nicolas C. Nicolaides, and Christina Kanaka-Gantenbein. 2022. "Perceived Changes in Emotions, Worries and Everyday Behaviors in Children and Adolescents Aged 5–18 Years with Type 1 Diabetes during the COVID-19 Pandemic" Children 9, no. 5: 736. https://doi.org/10.3390/children9050736







