PVA-Based Hydrogels Loaded with Diclofenac for Cartilage Replacement
Abstract
:1. Introduction
2. Results
2.1. Morphology
2.2. Water Uptake
2.3. Wettability
2.4. Mechanical Behavior
2.5. Rheological Behavior
2.6. Friction Coefficient
2.7. Drug Loading and Release
2.8. HET-CAM Test
3. Discussion
4. Conclusions
- (1)
- PAA was added to the formulation of hydrogels to obtain PVA/PAA samples;
- (2)
- PVA/PAA was further immersed in PEG to obtain PVA/PAA+PEG samples;
- (3)
- PVA/PAA+PEG was annealed at 120 °C, giving rise to PVA/PAA+PEG+A samples.
5. Materials and Methods
5.1. Materials
5.2. Methods
5.2.1. Samples Preparation
Hydrogels
Cartilage
5.2.2. Samples Characterization
Morphology
Water Uptake
Wettability
Mechanical Behavior
Rheological Behavior
Friction Coefficient
Drug Loading and Release
HET–CAM Test
Statistics
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Katz, J. Promoting Clinical and Basic Research in Osteoarthritis. OARSI World Congr. Osteoarthr. Promot. Clin. Basic Res. Osteoarthr. 2019, 27, S1–S538. [Google Scholar]
- Yelin, E.; Weinstein, S.; King, T. The Burden of Musculoskeletal Diseases in the United States. In Seminars in Arthritis and Rheumatism; United States Bone and Joint Iniciative: Lombard, IL, USA, 2016; Volume 46, pp. 259–260. [Google Scholar]
- Vahedi, P.; Moghaddamshahabi, R.; Webster, T.J.; Koyuncu, A.C.C.; Ahmadian, E.; Khan, W.S.; Mohamed, A.J.; Eftekhari, A. The use of infrapatellar fat pad-derived Mesenchymal stem cells in Articular cartilage regeneration: A review. Int. J. Mol. Sci. 2021, 22, 9215. [Google Scholar] [CrossRef] [PubMed]
- Shirley, P.Y.; Hunter, D.J. Managing osteoarthritis. Aust. Prescr. 2015, 38, 115–119. [Google Scholar]
- Chuang, E.Y.; Chiang, C.W.; Wong, P.C.; Chen, C.H. Hydrogels for the Application of Articular Cartilage Tissue Engineering: A Review of Hydrogels. Adv. Mater. Sci. Eng. 2018, 2018, 4368910. [Google Scholar] [CrossRef] [Green Version]
- Freedman, B.R.; Mooney, D.J. Biomaterials to Mimic and Heal Connective Tissues. Adv. Mater. 2019, 31, 1806695. [Google Scholar] [CrossRef]
- Sefat, F.; Israr Raja, T.; Sohai lZafar, M.; Khurshid, Z.; Najeeb, S.; Zohail, S.; Ahmadi, E.D.; Rahmati, M.; Mozafari, M. Chapter 3—Nanoengineered biomaterials for cartilage repair. In Nanoengineered Biomaterials for Regenerative Medicine; Elsevier: Amsterdam, The Netherlands, 2019; pp. 39–71. [Google Scholar]
- Bicho, D.; Pina, S.; Reis, R.L.; Oliveira, J.M. Commercial Products for Osteochondral Tissue Repair and Regeneration. Adv. Exp. Med. Biol. 2018, 1058, 415–428. [Google Scholar] [CrossRef] [Green Version]
- Rongen, J.J.; van Tienen, T.G.; van Bochove, B.; Grijpma, D.W.; Buma, P. Biomaterials in search of a meniscus substitute. Biomaterials 2014, 35, 3527–3540. [Google Scholar] [CrossRef]
- Spiller, K.L.; Maher, S.A.; Lowman, A.M. Hydrogels for the repair of articular cartilage defects. Tissue Eng.—Part B Rev. 2011, 17, 281–299. [Google Scholar] [CrossRef] [Green Version]
- Li, J.; Mooney, D.J. Designing hydrogels for controlled drug delivery. Nat. Rev. Mater. 2016, 1, 16071. [Google Scholar] [CrossRef]
- Oliveira, A.S.; Seidi, O.; Ribeiro, N.; Colaço, R.; Serro, A.P. Tribomechanical comparison between PVA hydrogels obtained using different processing conditions and human cartilage. Materials 2019, 12, 3413. [Google Scholar] [CrossRef] [Green Version]
- Eftekhari, A.; Dizaj, S.M.; Sharifi, S.; Salatin, S.; Saadat, Y.R.; Vahed, S.Z.; Samiei, M.; Ardalan, M.; Rameshrad, M.; Ahmadian, E.; et al. The use of nanomaterials in tissue engineering for cartilage regeneration; current approaches and future perspectives. Int. J. Mol. Sci. 2020, 21, 536. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chamkouri1, H.; Chamkouri, M. A Review of Hydrogels, Their Properties and Applications in Medicine. Am. J. Biomed. Sci. Res. 2021, 11, 485–493. [Google Scholar] [CrossRef]
- Peppas, N.A.; Hassan, C.M. Structure and applications of poly (vinyl alcohol) hydrogels produced by conventional crosslinking or by freezing/thawing methods. In Biopolymers—PVA Hydrogels, Anionic Polymerisation Nanocomposites; Springer: Berlin/Heidelberg, Germany, 2000; Volume 153, pp. 37–65. [Google Scholar]
- Moreau, D. Design and Characterization of Hydrogel Films and Hydrogel-Ceramic Composites for Biomedical Applications. Doctoral Dissertation, PSL Research University, Paris, France, 2016. [Google Scholar]
- Kawanishi, K.; Komatsu, M.; Inoue, T. Thermodynamic consideration of the sol-gel transition in polymer solutions. Polymer 1987, 28, 980–984. [Google Scholar] [CrossRef]
- Kanca, Y.; Milner, P.; Dini, D.; Amis, A.A. Tribological properties of PVA/PVP blend hydrogels against articular cartilage. J. Mech. Behav. Biomed. Mater. 2018, 78, 36–45. [Google Scholar] [CrossRef] [Green Version]
- Wu, X.; Li, W.; Chen, K.; Zhang, D.; Xu, L.; Yang, X. A tough PVA/HA/COL composite hydrogel with simple process and excellent mechanical properties. Mater. Today Commun. 2019, 21, 100702. [Google Scholar] [CrossRef]
- Luo, X.; Akram, M.Y.; Yuan, Y.; Nie, J.; Zhu, X. Silicon dioxide/poly(vinyl alcohol) composite hydrogels with high mechanical properties and low swellability. J. Appl. Polym. Sci. 2019, 136, 46895. [Google Scholar] [CrossRef] [Green Version]
- Barbon, S.; Contran, M.; Stocco, E.; Todros, S.; Macchi, V.; De Caro, R.; Porzionato, A. Enhanced biomechanical properties of polyvinyl alcohol-based hybrid scaffolds for cartilage tissue engineering. Processes 2021, 9, 730. [Google Scholar] [CrossRef]
- Jiang, Y.; Yang, Y.; Zheng, X.; Yi, Y.; Chen, X.; Li, Y.; Sun, D.; Zhang, L. Multifunctional load-bearing hybrid hydrogel with combined drug release and photothermal conversion functions. NPG Asia Mater. 2020, 12, 18. [Google Scholar] [CrossRef]
- Gonzalez, J.S.; Alvarez, V.A. The effect of the annealing on the poly(vinyl alcohol) obtained by freezing-thawing. Thermochim. Acta 2011, 521, 184–190. [Google Scholar] [CrossRef]
- Rey-Rico, A.; Madry, H.; Cucchiarini, M. Hydrogel-Based Controlled Delivery Systems for Articular Cartilage Repair. Biomed Res. Int. 2016, 2016, 1215263. [Google Scholar] [CrossRef] [Green Version]
- Westin, C.B.; Nagahara, M.H.T.; Decarli, M.C.; Kelly, D.J.; Moraes, Â.M. Development and characterization of carbohydrate-based thermosensitive hydrogels for cartilage tissue engineering. Eur. Polym. J. 2020, 129, 109637. [Google Scholar] [CrossRef]
- Gao, Y.; Li, K.; Guo, L.; Fan, H.; Fan, Y.; Zhang, X. Fabrication of biomimetic hydrogel for chondrocyte delivery. Mater. Lett. 2020, 258, 126660. [Google Scholar] [CrossRef]
- Joshi, N.; Yan, J.; Levy, S.; Bhagchandani, S.; Slaughter, K.V.; Sherman, N.E.; Amirault, J.; Wang, Y.; Riegel, L.; He, X.; et al. Towards an arthritis flare-responsive drug delivery system. Nat. Commun. 2018, 9, 1275. [Google Scholar] [CrossRef] [PubMed]
- Jung, Y.S.; Park, W.; Park, H.; Lee, D.K.; Na, K. Thermo-sensitive injectable hydrogel based on the physical mixing of hyaluronic acid and Pluronic F-127 for sustained NSAID delivery. Carbohydr. Polym. 2017, 156, 403–408. [Google Scholar] [CrossRef] [PubMed]
- Petit, A.; Sandker, M.; Müller, B.; Meyboom, R.; van Midwoud, P.; Bruin, P.; Redout, E.M.; Versluijs-Helder, M.; van der Lest, C.H.A.; Buwalda, S.J.; et al. Release behavior and intra-articular biocompatibility of celecoxib-loaded acetyl-capped PCLA-PEG-PCLA thermogels. Biomaterials 2014, 35, 7919–7928. [Google Scholar] [CrossRef]
- Oliveira, A.S.; Schweizer, S.; Nolasco, P.; Barahona, I.; Saraiva, J.; Colaço, R.; Serro, A.P. Tough and low friction polyvinyl alcohol hydrogels loaded with anti-inflammatories for cartilage replacement. Lubricants 2020, 8, 36. [Google Scholar] [CrossRef] [Green Version]
- Lindgren, U.; Djupsjö, H. Diclofenac for pain after hip surgery. Acta Orthop. 1985, 56, 28–31. [Google Scholar] [CrossRef]
- Cosmo, G.; Congedo, E. The Use of NSAIDs in the Postoperative Period: Advantage and Disadvantages. J. Anesth. Crit. Care Open Access 2015, 3, 107–118. [Google Scholar] [CrossRef]
- Gunaydin, C.; Bilge, S.S. Effects of nonsteroidal anti-inflammatory drugs at the molecular level. Eurasian J. Med. 2018, 50, 116–121. [Google Scholar] [CrossRef]
- Filipe, H.P.; Henriques, J.; Reis, P.; Silva, P.C.; Quadrado, M.J.; Serro, A.P. Contact lenses as drug controlled release systems: A narrative review. Rev. Bras. Oftalmol. 2016, 75, 241–247. [Google Scholar] [CrossRef] [Green Version]
- Franco, P.; De Marco, I. Contact lenses as ophthalmic drug delivery systems: A review. Polymers 2021, 13, 1102. [Google Scholar] [CrossRef] [PubMed]
- Jeong, J.O.; Park, J.S.; Kim, E.J.; Jeong, S.I.; Lee, J.Y.; Lim, Y.M. Preparation of radiation cross-linked poly(Acrylic acid) hydrogel containing metronidazole with enhanced antibacterial activity. Int. J. Mol. Sci. 2020, 21, 187. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vasi, A.M.; Popa, M.I.; Tanase, E.C.; Butnaru, M.; Verestiuc, L. Poly(Acrylic Acid)-Poly(Ethylene Glycol) nanoparticles designed for ophthalmic drug delivery. J. Pharm. Sci. 2014, 103, 676–686. [Google Scholar] [CrossRef] [PubMed]
- Kobayashi, M.; Koide, T.; Hyon, S.H. Tribological characteristics of polyethylene glycol (PEG) as a lubricant for wear resistance of ultra-high-molecular-weight polyethylene (UHMWPE) in artificial knee join. J. Mech. Behav. Biomed. Mater. 2014, 38, 33–38. [Google Scholar] [CrossRef]
- Zhang, S.; Hu, F.; Li, J.; Lv, L.; Lu, H. Lubrication Effect of Polyvinyl Alcohol/Polyethylene Glycol Gel for Artificial Joints. Adv. Mater. Sci. Eng. 2021, 2021, 2588784. [Google Scholar] [CrossRef]
- Davis, J.; McLister, A. Passive and Interactive Dressing Materials. In Smart Bandage Technologies; Academic Press: Cambridge, MA, USA, 2016; pp. 93–144. [Google Scholar] [CrossRef]
- Choi, J.; Kung, H.J.; MacIas, C.E.; Muratoglu, O.K. Highly lubricious poly(vinyl alcohol)-poly(acrylic acid) hydrogels. J. Biomed. Mater. Res.—Part B Appl. Biomater. 2012, 100, 524–532. [Google Scholar] [CrossRef]
- Ricciardi, R.; Auriemma, F.; De Rosa, C. Structure and properties of poly(vinyl alcohol) hydrogels obtained by freeze/thaw techniques. Macromol. Symp. 2005, 222, 49–64. [Google Scholar] [CrossRef]
- Teodorescu, M.; Morariu, S.; Bercea, M. Advanced Materials Based on Multicomponent Polymeric Systems. In Multiphase Polymer Systems; CRC Press: Boca Raton, FL, USA, 2016; pp. 59–78. [Google Scholar] [CrossRef]
- Sanchez, L.M.; Alvarez, V.A. Development of potentially biocompatible hydrogels with cylindrical pores prepared from polyvinyl alcohol and low-molecular weight polyacrylic acid. Polym. Eng. Sci. 2019, 59, 1479–1488. [Google Scholar] [CrossRef]
- Muratoglu, O.K.; Choi, J.; Bodugoz-Senturk, H.; Braithwaite, G.J.C.; Spiegelberg, S.H. Tough Hydrogels. Patent 9394384, 19 July 2016. [Google Scholar]
- Choi, J.; Muratoglu, O.K.; Choi, J.; Muratoglu, O.K. PVA-PAA Hydrogels. Patent WO2008131451A2, 30 October 2008. [Google Scholar]
- Liu, P.; Chen, W.; Liu, C.; Tian, M.; Liu, P. A novel poly (vinyl alcohol)/poly (ethylene glycol) scaffold for tissue engineering with a unique bimodal open-celled structure fabricated using supercritical fluid foaming. Sci. Rep. 2019, 9, 9534. [Google Scholar] [CrossRef]
- Park, J.S.; Kim, H.A.; Choi, J.B.; Gwon, H.J.; Shin, Y.M.; Lim, Y.M.; Khil, M.S.; Nho, Y.C. Effects of annealing and the addition of PEG on the PVA based hydrogel by gamma ray. Radiat. Phys. Chem. 2012, 81, 857–860. [Google Scholar] [CrossRef]
- Sophia Fox, A.J.; Bedi, A.; Rodeo, S.A. The basic science of articular cartilage: Structure, composition, and function. Sports Health 2009, 1, 461–468. [Google Scholar] [CrossRef] [PubMed]
- Arakawa, C.K.; DeForest, C.A. Polymer Design and Development. In Biology and Engineering of Stem Cell Niches; Academic Press: Cambridge, MA, USA, 2017; pp. 295–314. [Google Scholar]
- Bhalani, D.V.; Trivedi, J.S.; Jewrajka, S.K. Selective grafting of morphologically modified poly(vinylidene fluoride) ultrafiltration membrane by poly(acrylic acid) for inducing antifouling property. Appl. Surf. Sci. 2021, 544, 148905. [Google Scholar] [CrossRef]
- Wu, J.; Zhao, C.; Lin, W.; Hu, R.; Wang, Q.; Chen, H.; Li, L.; Chen, S.; Zheng, J. Binding characteristics between polyethylene glycol (PEG) and proteins in aqueous solution. J. Mater. Chem. B 2014, 2, 2983–2992. [Google Scholar] [CrossRef] [PubMed]
- Pawlak, Z.; Petelska, A.D.; Urbaniak, W.; Yusuf, K.Q.; Oloyede, A. Relationship Between Wettability and Lubrication Characteristics of the Surfaces of Contacting Phospholipid-Based Membranes. Cell Biochem. Biophys. 2013, 65, 335–345. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ahmed, A.S.; Mandal, U.K.; Taher, M.; Susanti, D.; Jaffri, J.M. PVA-PEG physically cross-linked hydrogel film as a wound dressing: Experimental design and optimization. Pharm. Dev. Technol. 2018, 23, 751–760. [Google Scholar] [CrossRef]
- Shi, Y.; Xiong, D.; Li, J.; Li, L.; Liu, Q.; Dini, D. Tribological Rehydration and Its Role on Frictional Behavior of PVA/GO Hydrogels for Cartilage Replacement under Migrating and Stationary Contact Conditions. Tribol. Lett. 2021, 69, 7. [Google Scholar] [CrossRef]
- Liu, T.; Jiao, C.; Peng, X.; Chen, Y.N.; Chen, Y.; He, C.; Liu, R.; Wang, H. Super-strong and tough poly(vinyl alcohol)/poly(acrylic acid) hydrogels reinforced by hydrogen bonding. J. Mater. Chem. B 2018, 6, 8105–8114. [Google Scholar] [CrossRef]
- Tanaka, E.; Rego, E.B.; Iwabuchi, Y.; Inubushi, T.; Koolstra, J.H.; Van Eijden, T.M.G.J.; Kawai, N.; Kudo, Y.; Takata, T.; Tanne, K. Biomechanical response of condylar cartilage-on-bone to dynamic shear. J. Biomed. Mater. Res.—Part A 2008, 85, 127–132. [Google Scholar] [CrossRef]
- Perni, S.; Prokopovich, P. Rheometer enabled study of cartilage frequency-dependent properties. Sci. Rep. 2020, 10, 20696. [Google Scholar] [CrossRef]
- Li, F.; Su, Y.; Wang, J.; Wu, G.; Wang, C. Influence of dynamic load on friction behavior of human articular cartilage, stainless steel and polyvinyl alcohol hydrogel as artificial cartilage. J. Mater. Sci. Mater. Med. 2010, 21, 147–154. [Google Scholar] [CrossRef]
- Oungoulian, S.R.; Durney, K.M.; Jones, B.K.; Ahmad, C.S.; Hung, C.T.; Ateshian, G.A. Wear and damage of articular cartilage with friction against orthopedic implant materials. J. Biomech. 2015, 48, 1957–1964. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Siboro, S.A.P.; Anugrah, D.S.B.; Ramesh, K.; Park, S.H.; Kim, H.R.; Lim, K.T. Tunable porosity of covalently crosslinked alginate-based hydrogels and its significance in drug release behavior. Carbohydr. Polym. 2021, 260, 117779. [Google Scholar] [CrossRef] [PubMed]
- Sanli, O.; Asman, G. Release of Diclofenac through Gluteraldehyde Crosslinked Poly (vinyl alcohol)/Poly (acrylic acid). J. Appl. Polym. Sci. 2003, 91, 72–77. [Google Scholar] [CrossRef]
- Jalil, A.; Khan, S.; Naeem, F.; Haider, M.S.; Sarwar, S.; Riaz, A.; Ranjha, N.M. The structural, morphological and thermal properties of grafted ph-sensitive interpenetrating highly porous polymeric composites of sodium alginate/acrylic acid copolymers for controlled delivery of diclofenac potassium. Des. Monomers Polym. 2017, 20, 308–324. [Google Scholar] [CrossRef] [Green Version]
- Chen, R.; Li, G.; Han, A.; Wu, H.; Guo, S. Controlled release of diclofenac sodium from polylactide acid-based solid dispersions prepared by hot-melt extrusion. J. Biomater. Sci. Polym. Ed. 2016, 27, 529–543. [Google Scholar] [CrossRef]
- Ritger, P.L.; Peppas, N.A. A simple equation for description of solute release I. Fickian and non-fickian release from non-swellable devices in the form of slabs, spheres, cylinders or discs. J. Control. Release 1987, 5, 23–26. [Google Scholar] [CrossRef]
- Rezaei, A.; Nasirpour, A. Evaluation of Release Kinetics and Mechanisms of Curcumin and Curcumin-β-Cyclodextrin Inclusion Complex Incorporated in Electrospun Almond Gum/PVA Nanofibers in Simulated Saliva and Simulated Gastrointestinal Conditions. Bionanoscience 2019, 9, 438–445. [Google Scholar] [CrossRef] [Green Version]
- Flory, P.J.; Rehner, J. Statistical mechanics of cross-linked polymer networks II. Swelling. J. Chem. Phys. 1943, 11, 521–526. [Google Scholar] [CrossRef]
- Kuijpers, A.J.; Engbers, G.H.M.; Feijen, J.; De Smedt, S.C.; Meyvis, T.K.L.; Demeester, J.; Krijgsveld, J.; Zaat, S.A.J.; Dankert, J. Characterization of the network structure of carbodiimide cross-linked gelatin gels. Macromolecules 1999, 32, 3325–3333. [Google Scholar] [CrossRef]
- Pimenta, A.F.R.; Ascenso, J.; Fernandes, J.C.S.; Colaço, R.; Serro, A.P.; Saramago, B. Controlled drug release from hydrogels for contact lenses: Drug partitioning and diffusion. Int. J. Pharm. 2016, 515, 467–475. [Google Scholar] [CrossRef] [Green Version]
- Pal, K.; Banthia, A.K.; Majumdar, D.K. Polymeric hydrogels: Characterization and biomedical applications. Des. Monomers Polym. 2009, 12, 197–220. [Google Scholar] [CrossRef] [Green Version]
- Gibas, I.; Janik, H. Review: Synthetic Polymer Hydrogels for Biomedical Applications. Chem. Chem. Technol. 2010, 4, 297–304. [Google Scholar] [CrossRef]
- Silva, D.; de Sousa, H.C.; Gil, M.H.; Santos, L.F.; Oom, M.S.; Alvarez-Lorenzo, C.; Saramago, B.; Serro, A.P. Moxifloxacin-imprinted silicone-based hydrogels as contact lens materials for extended drug release. Eur. J. Pharm. Sci. 2021, 156, 105591. [Google Scholar] [CrossRef] [PubMed]
- ICCVAM. The Hen’s Egg Test—Chorioallantoic Membrane Test Method. In ICCVAM Test Method Evaluation Report: Current Validation Status of In Vitro Test Methods Proposed for Identifying Eye Injury Hazard Potential of Chemicals and Products; NIH Publication No. 10-7553; National Institute of Environmental Health Sciences: Research Triangle Park, NC, USA, 2010; pp. 19–25. [Google Scholar]
- Loftsson, T.; Stefánsson, E. Cyclodextrins and topical drug delivery to the anterior and posterior segments of the eye. Int. J. Pharm. 2017, 531, 413–423. [Google Scholar] [CrossRef] [PubMed]






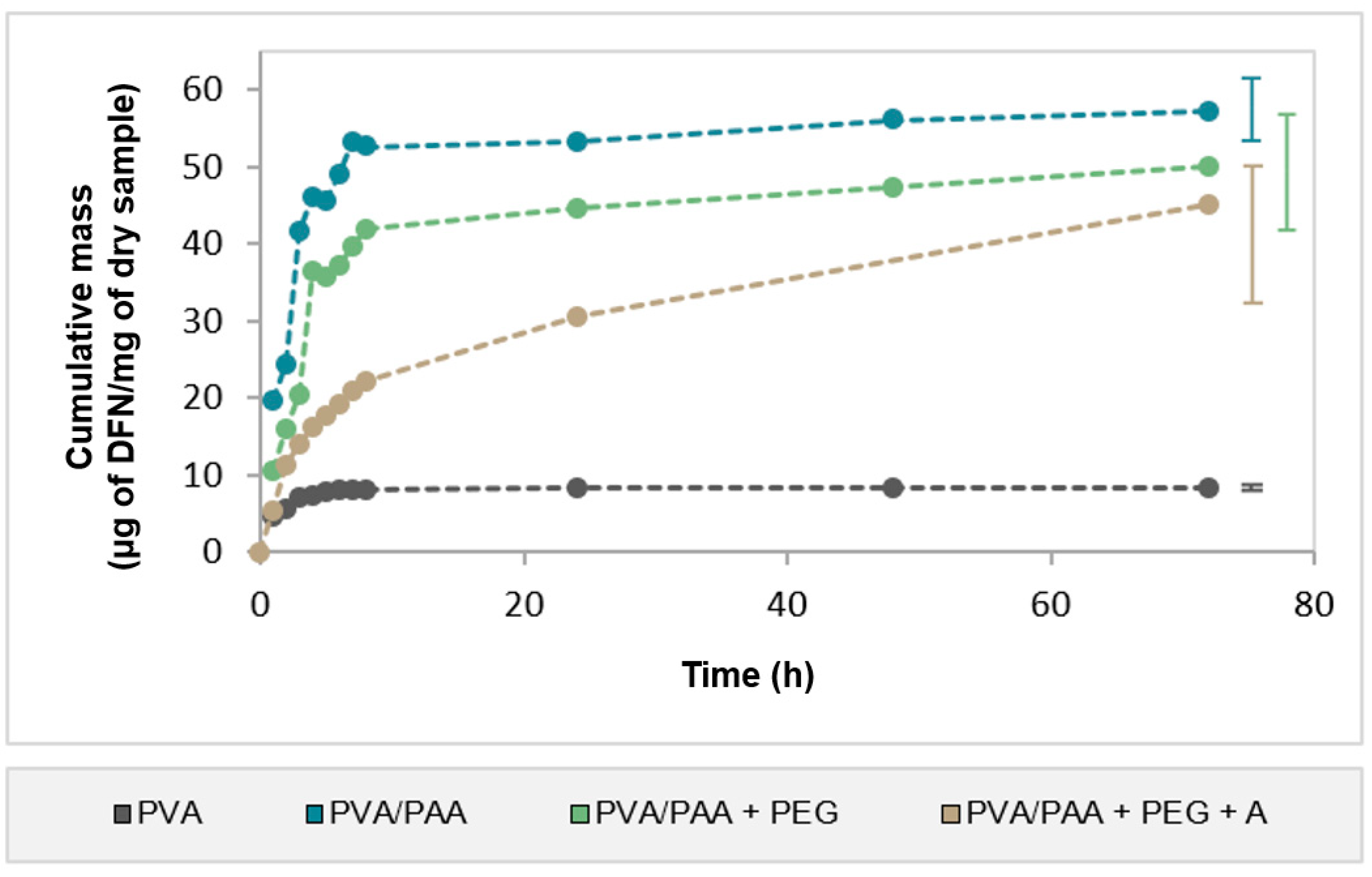


| PVA | PVA/PAA | PVA/PAA+PEG | PVA/PAA+PEG+A | |
|---|---|---|---|---|
| DFN amount loaded (μg DFN/mg dry sample) | 14.6 ± 0.9 | 125.5 ± 9.2 | 77.9 ± 4.8 | 81.7 ± 11.6 |
| DFN released (%) | 57.8 ± 3.6 | 45.7 ± 3.3 | 64.3 ± 4.0 | 55.3 ± 7.9 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Branco, A.C.; Oliveira, A.S.; Monteiro, I.; Nolasco, P.; Silva, D.C.; Figueiredo-Pina, C.G.; Colaço, R.; Serro, A.P. PVA-Based Hydrogels Loaded with Diclofenac for Cartilage Replacement. Gels 2022, 8, 143. https://doi.org/10.3390/gels8030143
Branco AC, Oliveira AS, Monteiro I, Nolasco P, Silva DC, Figueiredo-Pina CG, Colaço R, Serro AP. PVA-Based Hydrogels Loaded with Diclofenac for Cartilage Replacement. Gels. 2022; 8(3):143. https://doi.org/10.3390/gels8030143
Chicago/Turabian StyleBranco, Ana C., Andreia S. Oliveira, Inês Monteiro, Pedro Nolasco, Diana C. Silva, Célio G. Figueiredo-Pina, Rogério Colaço, and Ana P. Serro. 2022. "PVA-Based Hydrogels Loaded with Diclofenac for Cartilage Replacement" Gels 8, no. 3: 143. https://doi.org/10.3390/gels8030143







