Prediction of Changes in Blood Parameters Induced by Low-Frequency Ultrasound
Abstract
:1. Introduction
1.1. Related Work
1.2. Research Objectives
2. Materials and Methods
2.1. Sonication of Blood Samples
2.2. Investigation of Hematological Parameters
2.3. Investigation of Platelet Aggregation
2.4. Kruskal-Wallis Test
2.5. Platelet Number Prediction by Machine Learning
3. Results
3.1. Platelet Aggregation
3.2. Blood Analysis
3.3. Statistical Analysis
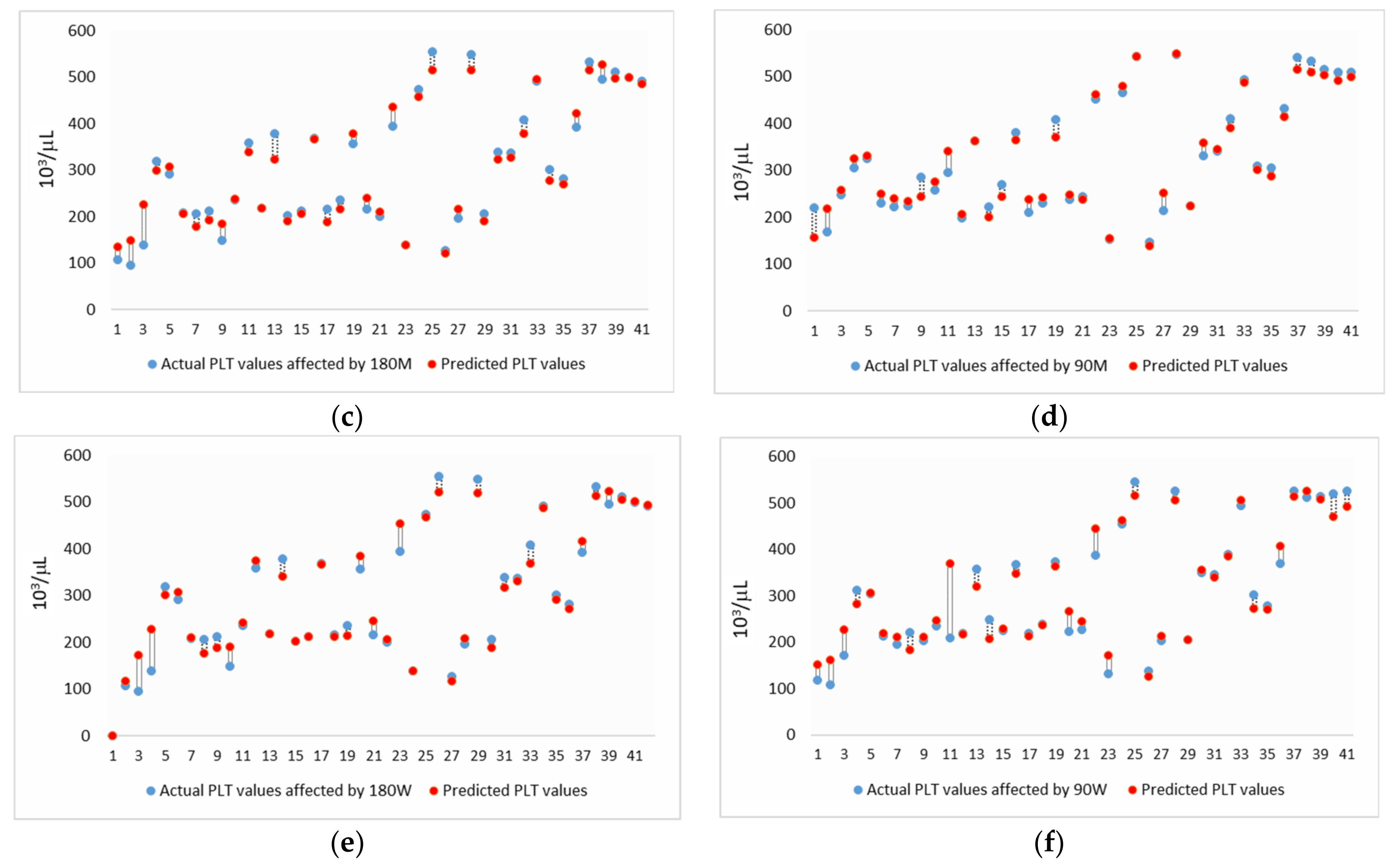
3.4. Platelet Number Prediction
4. Discussion
Suggestions for the Future
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Nandi, S.; Mohanty, K.; Nellenbach, K.; Erb, M. Ultrasound enhanced synthetic platelet therapy for augmented wound repair. ACS Biomater. Sci. Eng. 2020, 6, 3026–3036. [Google Scholar] [CrossRef]
- Voigt, J.; Wendelken, M.; Driver, V.; Alvarez, O.M. Low-frequency ultrasound (20–40 kHz) as an adjunctive therapy for chronic wound healing: A systematic review of the literature and meta-analysis of eight randomized controlled trials. Int. J. Low. Extrem. Wounds 2011, 10, 190–199. [Google Scholar] [CrossRef]
- Otto, C.; Baumann, M.; Schreiner, T.; Bartsch, G.; Borberg, H.; Schmid-Schonbein, P. Standardized ultrasound as a new method to induce platelet aggregation: Evaluation, influence of lipoproteins and of glycoprotein IIb/IIIa antagonist tirofiban. Eur. J. Ultrasound 2001, 14, 157–166. [Google Scholar] [CrossRef]
- Samal, A.B.; Adzerikho, I.D.; Mrochek, A.G.; Loiko, E.N. Platelet aggregation and change in intracellular Ca2+ induced by low-frequency ultrasound in vitro. Eur. J. Ultrasound 2000, 11, 53–59. [Google Scholar] [CrossRef]
- Guo, S.; Shen, S.; Wang, J.; Wang, H.; Li, M.; Hou, F.; Liao, Y.; Bin, J. Detection of high-risk atherosclerotic plaques with ultrasound molecular imaging of glycoprotein IIb/IIIa receptor on activated platelets. Theranostics 2015, 5, 418–430. [Google Scholar] [CrossRef]
- Tian, J.; Weng, Y.; Sun, R.; Zhu, Y.; Zhang, J.; Liu, H. Contrast-enhanced ultrasound molecular Imaging of activated platelets in the progression of atherosclerosis using microbubbles bearing the von willebrand factor A1 domain. Exp. Ther. Med. 2021, 2, 721. [Google Scholar] [CrossRef]
- Signori, L.U.; Teixeira, A.O.; da Silva, A.M.V.; da Costa, S.T. Effects of therapeutic ultrasound on hematological dynamics and fibrinogen during the inflammatory phase after muscle injury in rats. Acta Sci. Health Sci. 2014, 36, 25–31. [Google Scholar] [CrossRef]
- Cherniavsky, E.A.; Strakha, I.S.; Adzerikho, I.E.; Shkumatov, V.M. Effects of low-frequency ultrasound on some properties of fibrinogen and its plasminolysis. BMC Biochem. 2011, 12, 60. [Google Scholar] [CrossRef]
- Ivone, M.; Pappalettere, C.; Watanabe, A.; Tachibana, K. Study of cellular response induced by low intensity ultrasound frequency sweep pattern on myelomonocytic lymphoma U937 cells. J. Ultrasound 2016, 19, 167–174. [Google Scholar] [CrossRef]
- Qin, H.; Du, L.; Luo, Z.; He, Z.; Wang, Q.; Chen, S.; Zhu, Y.-L. The therapeutic effects of low-intensity pulsed ultrasound in musculoskeletal soft tissue injuries: Focusing on the molecular mechanism. Front. Bioeng. Biotechnol. 2022, 10, 1080430. [Google Scholar] [CrossRef]
- Garavand, A.; Behmanesh, A.; Aslani, N.; Sadeghsalehi, H.; Ghaderzadeh, M.; El Kafhali, S. Towards diagnostic aided systems in coronary artery disease detection: A comprehensive multiview survey of the state of the art. Int. J. Intell. Syst. 2023, 2023, 6442756. [Google Scholar] [CrossRef]
- Ghadezadeh, M.; Mehrad, A.; Azamossadat, H.; Farkhondeh, A.; Davood, B.; Hassan, A. A fast and efficient CNN model for B-ALL diagnosis and its subtypes classification using peripheral blood smear images. Int. J. Intell. Syst. 2021, 37, 5113–5133. [Google Scholar] [CrossRef]
- Varghese, N.E. Machine learning techniques for the classification of blood cells and prediction of diseases. Int. J. Comput. Sci. Eng. 2020, 9, 66–75. [Google Scholar]
- Amato, F.; Lopez, A.; Pena-Mendez, E.M.; Vanhara, P.; Hampl, A.; Havel, J. Artificial neural networks in medical diagnosis. J. Appl. Biomed. 2013, 11, 47–58. [Google Scholar] [CrossRef]
- Alsheref, F.K.; Gomaa, W.H. Blood diseases detection using classical machine learning algorithms. Int. J. Adv. Comput. Sci. Appl. 2019, 10, 77–81. [Google Scholar] [CrossRef]
- Neeb, H.; Grieger, S.; Luxem, K.; Strasser, E.F.; Kraus, M.-J. Active or not—Machine-learning based prediction of platelet activation. In Proceedings of the World Congress on Engineering and Computer Science 2014, San Francisco, CA, USA, 22–24 October 2014; Volume I. [Google Scholar]
- Jiang, Y.; Lei, C.; Yasumoto, A.; Kobayashi, H.; Aisaka, Y.; Ito, T.; Guo, B.; Nitta, N.; Kutsuna, N.; Ozeki, Y.; et al. Label-free detection of aggregated platelets in blood by machine-learning-aided optofluidic time-stretch microscopy. Lab Chip 2017, 17, 2426–2434. [Google Scholar] [CrossRef]
- Matsuo, H.; Kamada, M.; Imamura, A.; Shimizu, M.; Inagaki, M.; Tsuji, Y.; Hashimoto, M.; Tanaka, M.; Ito, H.; Fujii, Y. Machine learning-based prediction of relapse in rheumatoid arthritis patients using data on ultrasound examination and blood test. Sci. Rep. 2022, 12, 7224. [Google Scholar] [CrossRef]
- Sampathila, N.; Chadaga, K.; Goswami, N.; Chadaga, R.P.; Pandya, M.; Prabhu, S.; Bairy, M.G.; Katta, S.S.; Bhat, D.; Upadya, S.P. Customized deep learning classifier for detection of acute lymphoblastic leukemia using blood smear images. Healthcare 2022, 10, 1812. [Google Scholar] [CrossRef]
- Hu, Y.; Luo, Y.; Tang, G.; Huang, Y.; Kang, J.; Wang, D. Artificial intelligence and its applications in digital hematopathology. Blood Sci. 2022, 4, 136–142. [Google Scholar] [CrossRef]
- Swelab Alfa PlusUser’s Manual. Available online: https://boule.com/document-folder/?id=230 (accessed on 12 June 2023).
- Riffenburgh, R.H. Statistics in Medicine, 3rd ed.; Academic Press: Cambridge, MA, USA, 2012. [Google Scholar]
- Sherwani, R.A.K.; Shakeel, H.; Awan, W.B.; Faheem, M.; Aslam, M. Analysis of COVID-19 data using neutrosophic Kruskal Wallis H test. BMC Med. Res. Methodol. 2021, 21, 215. [Google Scholar] [CrossRef]
- Bayram, M.; Bayraktar, G.; Akyol, H.; Can, B. Comparing some blood parameters of ski racers and long-distance athletes. Turk. J. Sport Exerc. 2017, 19, 331–336. [Google Scholar] [CrossRef]
- Knapp, H. Intermediate Statistics Using SPSS, 1st ed.; SAGE Publications: Thousand Oaks, CA, USA, 2017; p. 480. [Google Scholar]
- Botchkarev, A. Performance metrics (error measures) in machine learning regression, forecasting and prognostics: Properties and typology. Interdiscip. J. Inf. Knowl. Manag. 2019, 14, 45–79. [Google Scholar]
- Palma-Barqueros, V.; Revilla, N.; Sánchez, A.; Zamora Cánovas, A.; Rodriguez-Alén, A.; Marín-Quílez, A.; González-Porras, J.R.; Vicente, V.; Lozano, M.L.; Bastida, J.M.; et al. Inherited Platelet Disorders: An Updated Overview. Int. J. Mol. Sci. 2021, 22, 4521. [Google Scholar] [CrossRef] [PubMed]
- Mahbobi, M.; Tiemann, T.K. Introductory Business Statistics with Interactive Spreadsheets, 1st Canadian ed.; BCcampus: Victoria, BC, Canada, 2015; p. 102. [Google Scholar]
- Yeom, E.; Nam, K.H.; Paeng, S.J. Effects of red blood cell aggregates dissociation on the estimation of ultrasound speckle image velocimetry. Ultrasonics 2014, 54, 1480–1487. [Google Scholar] [CrossRef] [PubMed]
- Vidallon, M.L.P.; Tabor, R.F.; Bishop, A.I.; Teo, B.M. Ultrasound-assisted fabrication of acoustically active, erythrocyte membrane “bubbles”. Ultrason. Sonochem. 2021, 72, 105429. [Google Scholar] [CrossRef]
- Ostasevicius, V.; Jurenas, V.; Mikuckyte, S.; Vezys, J.; Stankevicius, E.; Bubulis, A.; Venslauskas, M.; Kizauskiene, L. Development of a low-frequency piezoelectric ultrasonic transducer for biological tissue sonication. Sensors 2023, 23, 3608. [Google Scholar] [CrossRef]
- Van der Geest, A.P.J.; Mohseni, M.; Brower, R.; Van der Hoven, B.; Steyerberg, L.W.; Groeneveld, A.B.J. Immature granulocytes predict microbial infection and its adverse sequelae in the intensive care unit. J. Crit. Care 2014, 29, 523–527. [Google Scholar] [CrossRef]
- Wang, Z.; Pan, Y.; Huang, H.; Zhang, Y.; Li, Y.; Zou, C.; Huang, G.; Chen, Y.; Li, Y.; Li, J.; et al. Enhanced thrombolysis by endovascular low-frequency ultrasound with bifunctional microbubbles in venous thrombosis: In vitro and in vivo study. Front. Bioeng. Biotechnol. 2022, 10, 965769. [Google Scholar] [CrossRef]
- Wallace, D.F. The regulation of iron absorption and homeostasis. Clin. Biochem. Rev. 2016, 37, 51–62. [Google Scholar]
- Erriu, M.; Blus, C.; Szmukler-Moncler, S.; Buogo, S.; Levi, R.; Barbato, G.; Madonnaripa, D.; Denotti, G.; Piras, V.; Orrù, G. Microbial biofilm modulation by ultrasound: Current concepts and controversies. Ultrason. Sonochem. 2013, 21, 15–22. [Google Scholar] [CrossRef]
- Messas, E.; Ijsselmuiden, A.; Goudot, G.; Vlieger, S.; Den Heijer, P.; Puymirat, E.; Spaulding, C.; Zarka, S.; Hagege, A.A.; Marijon, E.; et al. Safety, feasibility and performance of valvosoft non-invasive ultrasound therapy in patients with severe symptomatic calcific aortic valve stenosis. First-in-Man. Eur. Heart J. 2020, 41, ehaa946.1932. [Google Scholar] [CrossRef]
- Carlson, R.V.; Boyd, K.M.; Webb, D.J. The revision of the declaration of Helsinki: Past, present and future. Br. J. Clin. Pharmacol. 2004, 57, 695–713. [Google Scholar] [CrossRef] [PubMed]


 the limits of the norm for a particular parameter, the norm area, which defines the normal range for the indicated blood parameter. (a) RDW parameter. (b) MCV parameter. (c) HGB parameter. (d) LYM parameter.
the limits of the norm for a particular parameter, the norm area, which defines the normal range for the indicated blood parameter. (a) RDW parameter. (b) MCV parameter. (c) HGB parameter. (d) LYM parameter.
 the limits of the norm for a particular parameter, the norm area, which defines the normal range for the indicated blood parameter. (a) RDW parameter. (b) MCV parameter. (c) HGB parameter. (d) LYM parameter.
the limits of the norm for a particular parameter, the norm area, which defines the normal range for the indicated blood parameter. (a) RDW parameter. (b) MCV parameter. (c) HGB parameter. (d) LYM parameter.
 shows the limits of the norm for a particular parameter, the norm area, which defines the normal range for the denoted blood parameter. (a) RBC parameter. (b) HTC parameter. (c) MCH parameter. (d) MCHC parameter. (e) MID (%) parameter.
shows the limits of the norm for a particular parameter, the norm area, which defines the normal range for the denoted blood parameter. (a) RBC parameter. (b) HTC parameter. (c) MCH parameter. (d) MCHC parameter. (e) MID (%) parameter.
 shows the limits of the norm for a particular parameter, the norm area, which defines the normal range for the denoted blood parameter. (a) RBC parameter. (b) HTC parameter. (c) MCH parameter. (d) MCHC parameter. (e) MID (%) parameter.
shows the limits of the norm for a particular parameter, the norm area, which defines the normal range for the denoted blood parameter. (a) RBC parameter. (b) HTC parameter. (c) MCH parameter. (d) MCHC parameter. (e) MID (%) parameter.





| Sonication Mode | Ultrasound Exposure, s | Ultrasound Intensity, mW/cm2 | Electric Power, W | Ultrasound Frequency, kHz |
|---|---|---|---|---|
| K | 0 | 0 | 0 | 0 |
| A | 90 | 100–150 | 60 | 48 |
| B | 180 | 100–150 | 60 | 48 |
| C | 90 | 50–70 | 35 | 44 |
| D | 180 | 50–70 | 35 | 44 |
| E | 90 | 5–12 | 10 | 44 |
| F | 180 | 5–12 | 10 | 44 |
| Parameter: | F40,6 | p-Value |
|---|---|---|
| RBC | 13.80 | <0.01 |
| MCV | 12.51 | <0.01 |
| HCT | 12.61 | <0.01 |
| MPV | 14.58 | <0.01 |
| PDW | 15.20 | <0.01 |
| LPCR | 15.31 | <0.01 |
| WBC | 29.43 | <0.01 |
| HGB | 2.25 | 0.039 |
| MCH | 17.34 | <0.01 |
| MCHC | 2.53 | 0.021 |
| LYM | 16.98 | <0.01 |
| GRAN | 32.88 | <0.01 |
| LYM% | 13.52 | <0.01 |
| GRA% | 7.29 | <0.01 |
| MID% | 23.49 | <0.01 |
| Blood Parameters with p-Value < 0.05 | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| RBC | HTC | MPV | PDW | LPCR | WBC | MCH | MCHC | GRA(%) | GRAN | MID(%) |
| <0.001 | <0.001 | 0.037 | 0.044 | 0.015 | 0.010 | <0.001 | <0.001 | 0.006 | 0.002 | <0.001 |
| Blood Parameters with p-Value > 0.05 | ||||||||||
| RDW | MCV | PLT | PCT | HGB | LYM | MID | RDWa | LYM(%) | ||
| 0.990 | 0.842 | 0.885 | 0.808 | 0.584 | 0.166 | 0.467 | 0.977 | 0.157 | ||
| Blood Parameter | p-Values Adjusted by the Bonferroni Correction | |||||
|---|---|---|---|---|---|---|
| 0 C-180 W | 0 C-90 M | 0 C-180 H | 0 C-90 H | 0 C-90 W | 0 C-180 M | |
| RBC | 1.000 | 1.000 | 0.469 | 0.037 | 1.000 | 1.000 |
| HTC | 1.000 | 1.000 | 0.324 | 0.047 | 1.000 | 1.000 |
| MCH | 1.000 | 0.008 | 0.000 | 0.000 | 1.000 | 0.03 |
| MCHC | 1.000 | 0.000 | 0.000 | 0.000 | 1.000 | 0.000 |
| MID, % | 1.000 | 1.000 | 0.028 | 1.000 | 1.000 | 1.000 |
| ML Algorithm | 90 W | 180 W | 90 M | 180 M | 90 H | 180 H |
|---|---|---|---|---|---|---|
| DT | 44.156 | 36.61 | 41.61 | 35.8 | 67.34 | 60.16 |
| RF | 47.822 | 33.68 | 34.49 | 29.75 | 67.98 | 52.63 |
| ANN | 66.04 | 51.84 | 27.04 | 41.75 | 154.24 | 93.96 |
| LR | 48.99 | 42.83 | 43.54 | 38.77 | 76.05 | 82.83 |
| SVR | 23.45 | 27.73 | 22.90 | 27.12 | 35.41 | 55.80 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ostasevicius, V.; Paulauskaite-Taraseviciene, A.; Lesauskaite, V.; Jurenas, V.; Tatarunas, V.; Stankevicius, E.; Tunaityte, A.; Venslauskas, M.; Kizauskiene, L. Prediction of Changes in Blood Parameters Induced by Low-Frequency Ultrasound. Appl. Syst. Innov. 2023, 6, 99. https://doi.org/10.3390/asi6060099
Ostasevicius V, Paulauskaite-Taraseviciene A, Lesauskaite V, Jurenas V, Tatarunas V, Stankevicius E, Tunaityte A, Venslauskas M, Kizauskiene L. Prediction of Changes in Blood Parameters Induced by Low-Frequency Ultrasound. Applied System Innovation. 2023; 6(6):99. https://doi.org/10.3390/asi6060099
Chicago/Turabian StyleOstasevicius, Vytautas, Agnė Paulauskaite-Taraseviciene, Vaiva Lesauskaite, Vytautas Jurenas, Vacis Tatarunas, Edgaras Stankevicius, Agilė Tunaityte, Mantas Venslauskas, and Laura Kizauskiene. 2023. "Prediction of Changes in Blood Parameters Induced by Low-Frequency Ultrasound" Applied System Innovation 6, no. 6: 99. https://doi.org/10.3390/asi6060099






