Effect of a Conditional Cash Transfer Program on Nutritional Knowledge and Food Practices among Caregivers of 3–5-Year-Old Left-Behind Children in the Rural Hunan Province
Abstract
:1. Introduction
2. Methods
2.1. Trial Design
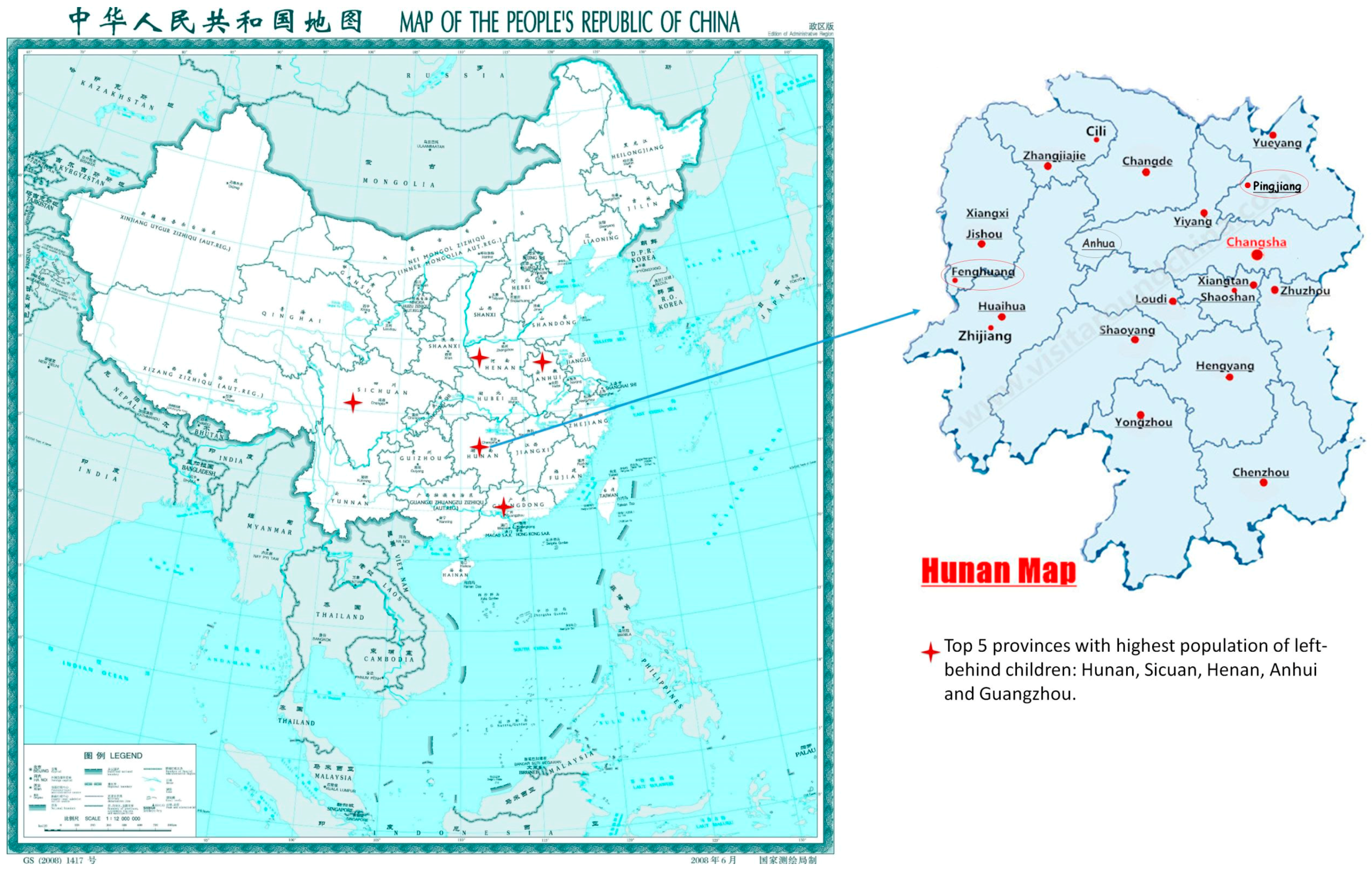
2.2. Participants
2.3. CCT Interventions
- Workshop 1—Introduction of basic public health services for LBC
- Workshop 2—Importance of health examination for LBC
- Workshop 3—Importance of nutrition and diet diversity for LBC’s health
- Workshop 4—Common nutrition problems for LBC (stunting)
- Workshop 5—Common nutrition problems for LBC (Iron Deficiency Anemia, DA)
- Workshop 6—Health evaluation and its importance for LBC
2.4. Outcome Measures
2.5. Sample Size
2.6. Randomization
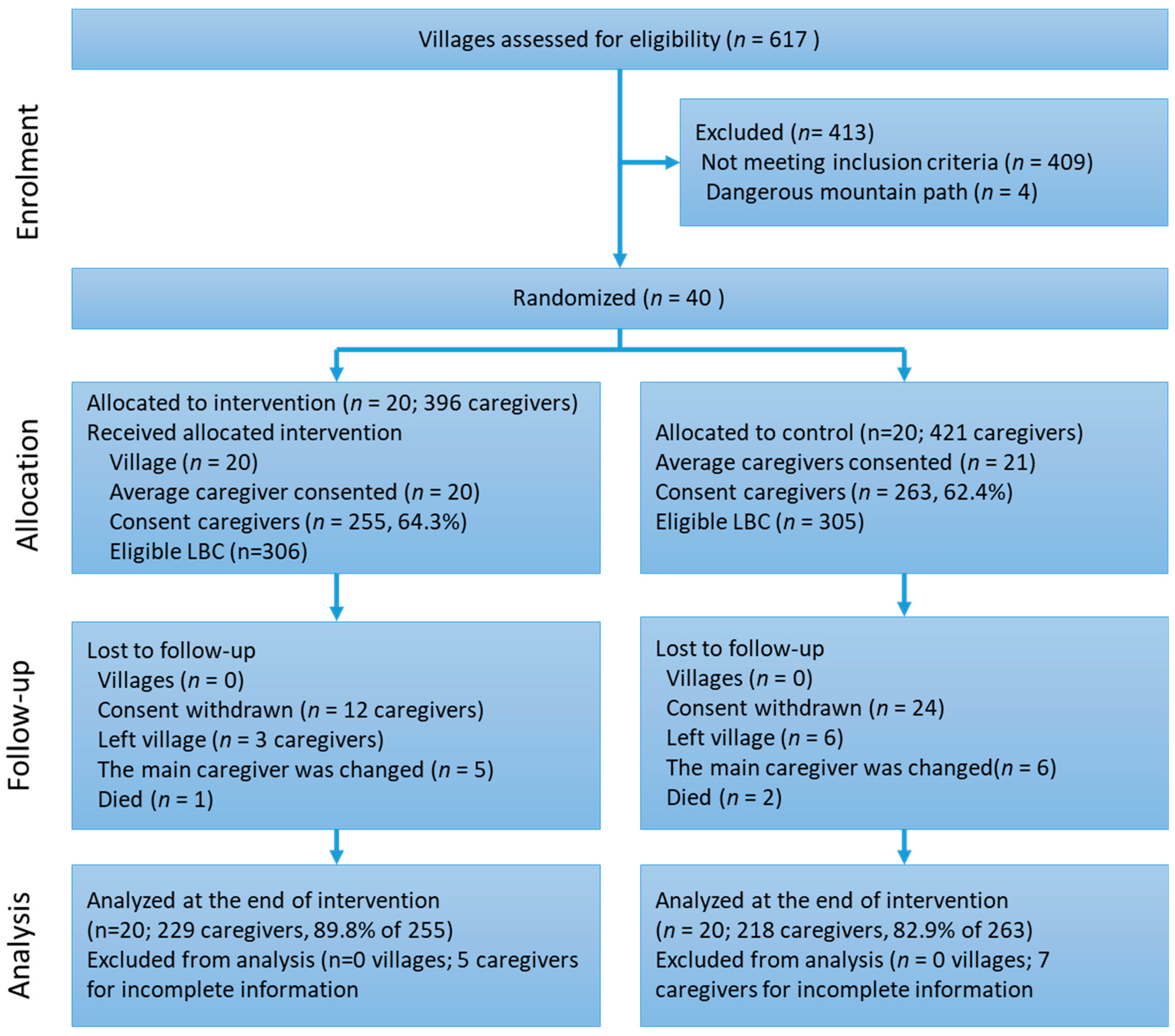
2.7. Participant Recruitment
2.8. Ethical Approval
2.9. Statistical Analysis
3. Results
3.1. General Characteristics of Participants
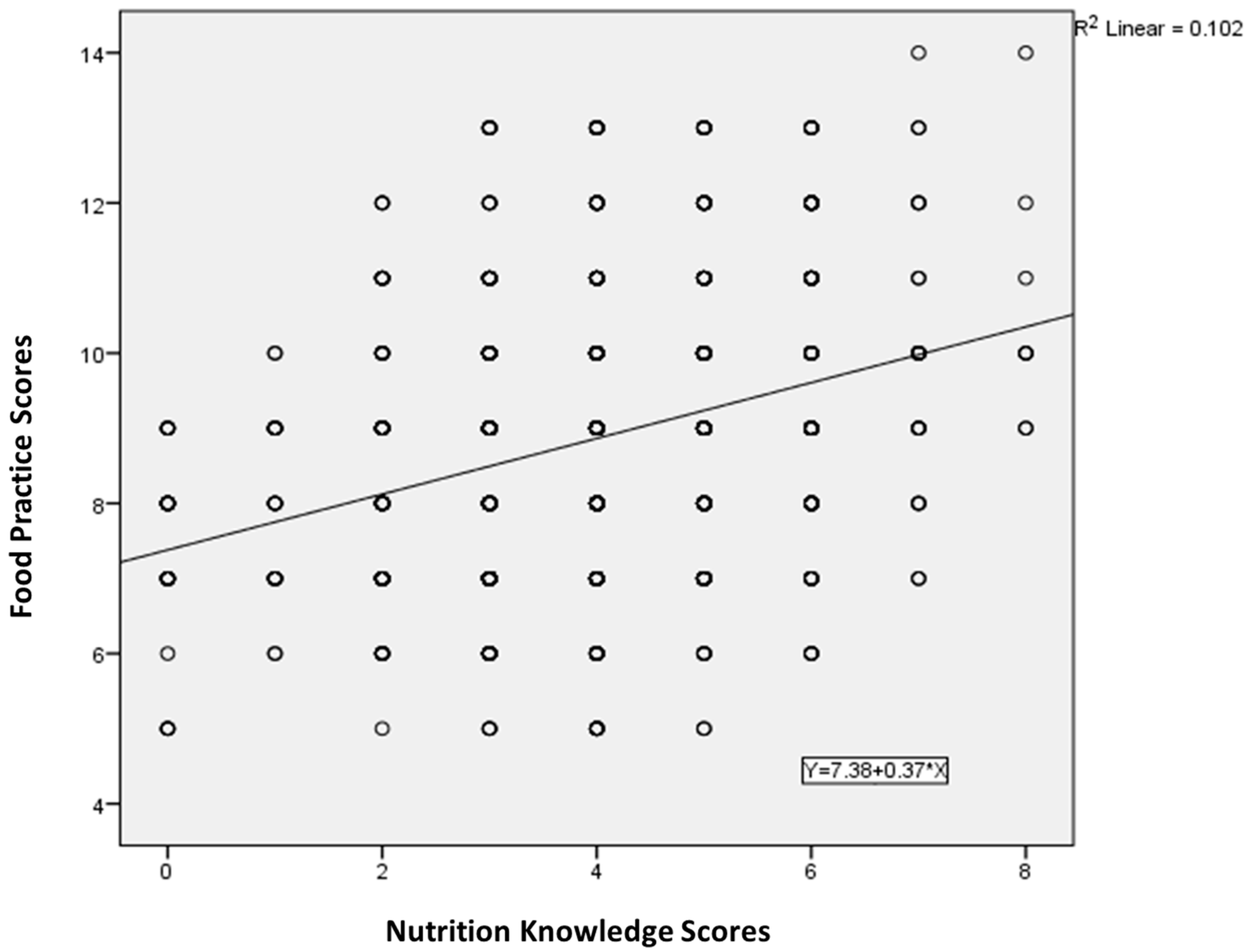
3.2. Knowledge of Nutrition and Food Practices Related to Children among CLBC
3.3. The Effectiveness of the Intervention on Nutrition Knowledge and Food Practice Behaviors
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| CLBC | Caregivers of left-behind children |
| LBC | Left-behind children |
| CCT | Conditional cash transfer |
References
- Duan, C.R.; Yang, G. The Left-behind Children in Rural China. Popul. Res. 2008, 32, 15–25. [Google Scholar] [CrossRef]
- Duan, C.R.; Lv, L.D.; Guo, J.; Wang, Z.P. Survival and Development of Left-behind Children in Rural China: Based on the Analysis of Sixth Census Data. Popul. Res. 2013, 35, 39–49. [Google Scholar] [CrossRef]
- Chen, C.M.; He, W.; Wang, Y.Y.; Deng, L.N.; Jia, F.M. Nutritional Status of Children during and PostGlobal Economic Crisis in China. Biomed. Environ. Sci. 2011, 24, 321–328. [Google Scholar] [CrossRef] [PubMed]
- Ji, M.M.; Zhang, Y.F.; Zou, J.J. Study on the Status of Health Service Utilization among Caregivers of Left-Behind Children in Poor Rural Areas of Hunan Province: A Baseline Survey. Int. J. Environ. Res. Public Health 2017, 14, 910. [Google Scholar] [CrossRef] [PubMed]
- Hu, X.J.; Yu, M. Analyzing the Mode of Conditional Cash Transfers for Demander of Health Services. Chin. Health Serv. Manag. 2014, 3, 487–490. [Google Scholar]
- Tang, L.X.; Zhao, L.X.; Li, X.Y. International Experience of Conditional Cash Transfer Payment Scheme for Poverty Alleviation. Guizhou Soc. Sci. 2012, 2, 89–93. [Google Scholar] [CrossRef]
- Ebenezer, O. Perceived Impact of Ghana’s Conditional Cash Transfer on Child Health. Health Promot. Int. 2016, 31, 33–43. [Google Scholar] [CrossRef]
- Fiszbein, A.; Schady, N.; Ferreira, F. Conditional Cash Transfers. Reducing Present and Future Poverty. World Bank Publ. 2009, 9, 465–468. [Google Scholar]
- Kusuma, D.; McConnell, M.; Berman, P.; Cohen, J. The Impact of Household and Community Cash Transfers on Children’s Food Consumption in Indonesia. Prev. Med. 2017, 152–158. [Google Scholar] [CrossRef] [PubMed]
- Martins, A.P.B.; Canella, D.S.; Baraldi, L.G.; Monteiro, C.A. Cash Transfer in Brazil and Nutritional Outcomes: A Systematic Review. Rev. Saúde Públ. 2013, 47, 1159–1171. [Google Scholar] [CrossRef]
- Kandpal, E.; Alderman, H.; Friedman, J.; Filmer, D.; Onishi, J.; Avalos, J. A Conditional Cash Transfer Program in the Philippines Reduces Severe Stunting. J. Nutr. 2016, 146, 1793. [Google Scholar] [CrossRef] [PubMed]
- De Bem Lignani, J.; Sichieri, R.; Luciene, B.; Salles-Costa, R. Changes in Food Consumption among the Programa Bolsa Famı´lia Participant Families in Brazil. Public Health Nutr. 2011, 14, 785–792. [Google Scholar] [CrossRef] [PubMed]
- Lin, Q.; Peymané, A.; Karla, H. Health Allowance for Improving the Nutritional Status and Development of 3–5-Year-Old Left-Behind Children in Poor Rural Areas of China: Study Protocol for a Cluster Randomised Trial. Trials 2015, 16, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Li, C.M.; Yang, N.; Zhang, H.J. Investigation of Physical Development among Left-Behind Children in Rural Areas in Western Hunan Province. Chin. Gen. Pract. 2011, 1000–1002 and 1005. [Google Scholar]
- Carter, B.R.; Hood, K. Balance Algorithm for Cluster Randomized Trials. BMC Med. Res. Methodol. 2008, 8, 65. [Google Scholar] [CrossRef] [PubMed]
- Duan, D.H. Investigation of the Diet and Nutritional Status of the Left-Behind Children Aged 2–6 Years in Rural China. Master’s Thesis, Central south University, Changsha, China, 2010. [Google Scholar]
- Hui, G. Investigation of the Nutritional Status and Its Effective Factors of the Rural Left-Behind School-Children in Hanchuan City. Master’s Thesis, Wuhan University of Science and Technology, Wuhan, China, 2015. [Google Scholar]
- Zhan, J.J. Survey on Health Literacy Knowledge, Attitude, Practice and Family Parenting of Preschool Left-Behind Children’s Guardian in Countryside. Master’s Thesis, Shangdong University, Jinan, China, 2015. [Google Scholar]
- Fernald, L.C.H. Promise, and Risks, of Conditional Cash Transfer Programmes. Lancet 2013, 382. [Google Scholar] [CrossRef]
- Bailey, S.H. The Impact of Cash Transfers on Nutrition in Emergency and Transitional Context: A Review of Evidence. Ann. Diagn. Pathol. 2012, 16, 260–266. [Google Scholar]
- Manley, J.; Gitte, S.; Slavchevska, V. How Effective are Cash Transfers at Improving Nutritional Status? World Dev. 2013, 48, 133–155. [Google Scholar] [CrossRef]
- Wang, Z.X. Dietary Guidelines for Children Aged 0–6 Years in CHINA. In Proceedings of the 10th National Nutrition Academic Conference and the 7th Congress of the Chinese Nutrition Society, Beijing, China, 22 October 2008. [Google Scholar]
- Wu, Z.H.; Li, J.M. The Investigation Report of Survival Status for Left-behind Children in Rural Areas. China Agric. Univ. J. Soc. Sci. Ed. 2015, 32. [Google Scholar] [CrossRef]
- Pan, C.M.; Chen, X.R. Growth and Nutritional Status among Rural Left-Behind Children. Chin. J. Public Health 2014, 30. [Google Scholar] [CrossRef]
| Variables | Baseline, January–March 2015 (n = 518) | Endpoint, June–July 2016 (n = 447) | ||||
|---|---|---|---|---|---|---|
| Control (n = 263) | Intervention (n = 255) | p | Control (n = 218) | Intervention (n = 229) | p | |
| Household Size | 6.7 ± 2.2 | 6.8 ± 2.0 | 0.643 | 6.7 ± 2.1 | 6.8 ± 2.0 | 0.824 |
| Female Caregivers (n, %) | 165 (62.7%) | 178 (69.8%) | 0.095 | 143 (65.6%) | 166 (72.5%) | 0.125 |
| Minorities (n, %) | 95 (36.1%) | 98 (38.4%) | 0.325 | 80 (36.7%) | 87 (38.0%) | 0.427 |
| Age of Caregivers (years) | 54.3 ± 12.6 | 56.2 ± 12.0 | 0.075 | 55.9 ± 13.0 | 57.6 ± 12.4 | 0.172 |
| Number of 3–5-year-old LBC being taken care of #: | ||||||
| 1 | 205 (78.5%) | 196 (77.5%) | 0.856 | 174 (79.8%) | 181 (79.0%) | 0.979 |
| 2 | 48 (18.4%) | 47 (18.6%) | 35 (16.1%) | 38 (16.6%) | ||
| 3 and above | 8 (3.1%) | 10 (4.0%) | 9 (4.1%) | 10 (4.4%) | ||
| Education level of caregivers | ||||||
| No education (n, %) | 81 (30.9%) | 74 (29.0%) | 0.324 | 67 (30.7%) | 73 (32.0%) | 0.803 |
| Less than 3 years (n, %) | 47 (17.9%) | 61 (23.9%) | 43 (19.7%) | 46 (20.2%) | ||
| 3–6 years (n, %) | 74 (28.2%) | 68 (26.7%) | 64 (29.4%) | 57 (25.0%) | ||
| Middle school level (n, %) | 52 (19.8%) | 40 (15.7%) | 37 (17.0%) | 41 (18.0%) | ||
| High school level (n, %) | 8 (3.1%) | 12 (4.7%) | 7 (3.2%) | 11 (4.8%) | ||
| Caregiver–LBC relationship | ||||||
| Mother (n, %) | 29 (11.0%) | 23 (9.0%) | 0.560 | 23 (10.6%) | 21 (9.2%) | 0.636 |
| Father (n, %) | 12 (4.6%) | 12 (4.7%) | 8 (3.7%) | 5 (2.2%) | ||
| Grandparent (n, %) | 211 (80.2%) | 214 (83.9%) | 180 (82.6%) | 198 (86.5) | ||
| Other (n, %) | 11 (4.2%) | 6 (2.4%) | 7 (3.2%) | 12 (2.7%) | ||
| Caregiver career | ||||||
| Unemployed | 16 (6.1%) | 14 (5.5%) | 0.376 | 14 (6.4%) | 10 (4.4%) | 0.487 |
| Farmer | 239 (90.9%) | 227 (89.0%) | 199 (91.3%) | 211 (92.1%) | ||
| Employed | 8 (3.0%) | 14 (5.5%) | 5 (2.3%) | 8 (3.5%) | ||
| Caregiver marital status | ||||||
| Married | 182(83.1%) | 198 (86.8%) | 0.615 | 178 (81.3%) | 194 (85.1%) | 0.514 |
| Separated | 3 (1.4%) | 3 (1.3%) | 7 (3.2%) | 3 (1.3%) | ||
| Divorced | 6 (2.7%) | 3 (1.3%) | 5 (2.3%) | 4 (1.8%) | ||
| Widowed | 28 (12.8%) | 24 (10.5%) | 29 (13.2%) | 27 (11.8%) | ||
| Socioeconomic status (tertiles) * | ||||||
| Low | 83 (31.6%) | 89 (35.0%) | 0.418 | 66 (30.3%) | 80 (35.2%) | 0.158 |
| Middle | 95 (36.1%) | 78 (30.7%) | 82 (37.6%) | 66 (29.1%) | ||
| High | 85 (32.3%) | 87 (34.3%) | 70 (32.1%) | 81 (35.7%) | ||
| Number of LBC in the family | 2.0 ± 1.0 | 2.1 ± 1.0 | 0.537 | 2.1 ± 1.1 | 2.2 ± 1.1 | 0.345 |
| Knowledge Item | Correct Responses (%) | p | |
|---|---|---|---|
| Control Group (n = 218) | Intervention Group (n = 229) | ||
| K1: It is important to know the child’s height and weight. | 144 (66.1%) | 196 (85.6%) | <0.001 |
| K2: When child is not hungry this means he/she gets enough nutrients. | 37 (17.0%) | 42 (18.3%) | 0.712 |
| K3: Skipping breakfast is not good for the child. | 61 (28.0%) | 81 (35.4%) | 0.104 |
| K4: Eating a variety of food is good for the child. | 165 (75.7%) | 209(88.2%) | 0.001 |
| K5: Eggs are a healthy food choice for the child. | 167 (76.6%) | 209 (91.3%) | <0.001 |
| K6: Dairy products are a healthy food choice for the child. | 150 (68.8%) | 182 (79.5%) | 0.013 |
| K7: Is able to recognize the symptoms of iron deficiency anemia (pale skin, weakness, dizziness, headache, etc.) | 49 (22.5%) | 75 (32.8%) | 0.02 |
| K8: Is able to identify iron-rich food (can give examples, like liver, beef, pork, and fish, etc.). | 19 (8.7%) | 54 (23.6%) | <0.001 |
| Variables | Control Group (n = 218) | Intervention Group (n = 229) | p |
|---|---|---|---|
| B1: Prepares breakfast for the family. | |||
| Less than 2 times per week | 22 (10.0%) | 31 (13.6%) | 0.149 |
| 3–4 times per week | 18 (8.2%) | 10 (4.4%) | |
| 5–7 times per week | 179 (81.7%) | 187 (82.0%) | |
| B2: Prepares a separate meal for child (meat, fish, etc.) | |||
| Less than 2 times per week | 165 (75.3%) | 162 (71.1%) | 0.325 |
| 3–4 times per week | 25 (11.4%) | 24 (10.5%) | |
| 5–7 times per week | 29 (13.2%) | 42 (18.4%) | |
| B3: Prepares two dishes or more for each meal. | |||
| Less than 2 times per week | 79 (36.1%) | 64 (28.1%) | 0.129 |
| 3–4 times per week | 73 (33.3%) | 77 (33.8%) | |
| 5–7 times per week | 67 (30.6%) | 87 (38.2%) | |
| B4: Provides eggs for the child. | |||
| Less than 2 times per week | 146 (66.7%) | 129 (56.6%) | 0.040 |
| 3–4 times per week | 44 (20.1%) | 69 (30.3%) | |
| 5–7 times per week | 29 (13.2%) | 30 (13.2%) | |
| B5: Provides dairy products for the child. | |||
| Less than 2 times per week | 159 (72.6%) | 140 (61.4%) | 0.034 |
| 3–4 times per week | 35 (16.0%) | 56 (24.6%) | |
| 5–7 times per week | 25 (11.4%) | 32 (14.0%) | |
| Variables | Baseline | Endpoint | p-Value | p-Value Adjusted ϕ |
|---|---|---|---|---|
| Nutrition Knowledge Score | ||||
| Intervention (n = 228) | 3.68 ± 1.43 | 4.47 ± 1.44 | 0.02 * | 0.007 ** |
| Control (n = 219) | 3.72 ± 1.56 | 3.67 ± 1.73 | ||
| Food Practice Score | ||||
| Intervention (n = 228) | 8.65 ± 1.85 | 9.35 ± 1.80 | 0.057 | 0.031 * |
| Control (n = 219) | 8.54 ± 1.80 | 8.89 ± 1.95 | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, Y.; Ji, M.; Zou, J.; Yuan, T.; Deng, J.; Yang, L.; Li, M.; Qin, H.; Chen, J.; Lin, Q. Effect of a Conditional Cash Transfer Program on Nutritional Knowledge and Food Practices among Caregivers of 3–5-Year-Old Left-Behind Children in the Rural Hunan Province. Int. J. Environ. Res. Public Health 2018, 15, 525. https://doi.org/10.3390/ijerph15030525
Zhang Y, Ji M, Zou J, Yuan T, Deng J, Yang L, Li M, Qin H, Chen J, Lin Q. Effect of a Conditional Cash Transfer Program on Nutritional Knowledge and Food Practices among Caregivers of 3–5-Year-Old Left-Behind Children in the Rural Hunan Province. International Journal of Environmental Research and Public Health. 2018; 15(3):525. https://doi.org/10.3390/ijerph15030525
Chicago/Turabian StyleZhang, Yefu, Meimei Ji, Jiaojiao Zou, Tong Yuan, Jing Deng, Lina Yang, Mingzhi Li, Hong Qin, Jihua Chen, and Qian Lin. 2018. "Effect of a Conditional Cash Transfer Program on Nutritional Knowledge and Food Practices among Caregivers of 3–5-Year-Old Left-Behind Children in the Rural Hunan Province" International Journal of Environmental Research and Public Health 15, no. 3: 525. https://doi.org/10.3390/ijerph15030525






