Enhancement of the Solubility and Dissolution Rate of Telmisartan by Surface Solid Dispersions Employing Superdisintegrants, Hydrophilic Polymers and Combined Carriers
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Preparation of Primary Surface Solid Dispersions (P-SSD) Employing Superdisintegrants
2.3. Preparation of Primary Surface Solid Dispersions (P-SSD) Employing Hydrophilic Polymers
2.4. Preparing Combined Carrier-Solid Dispersions (C-SSDs) Employing Superdisintegrants and Hydrophilic Polymers
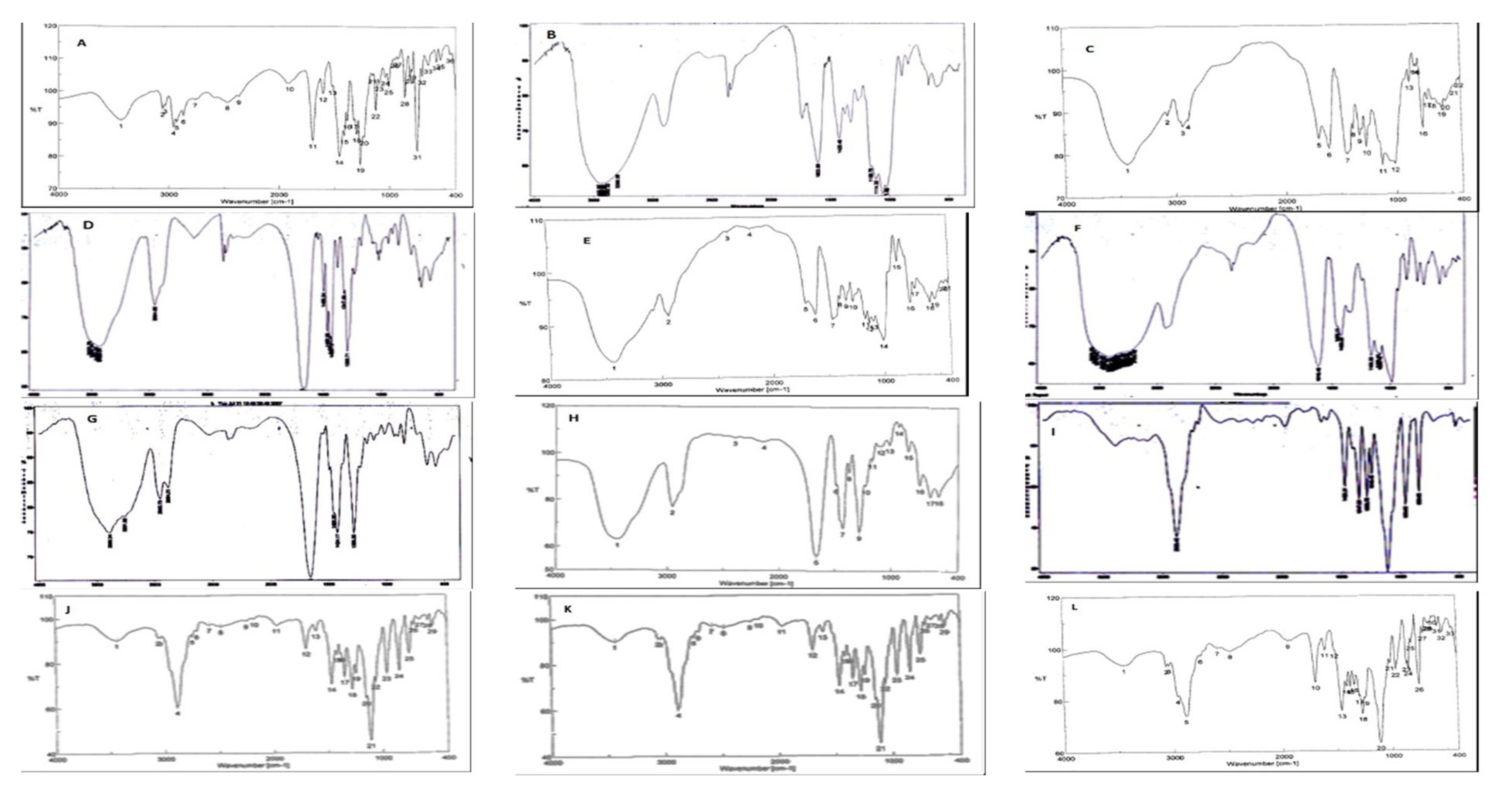
2.5. Compatibility Evaluation of Telmisartan with Different Carriers Using Fourier-Transform Infrared Spectroscopy (FTIR)
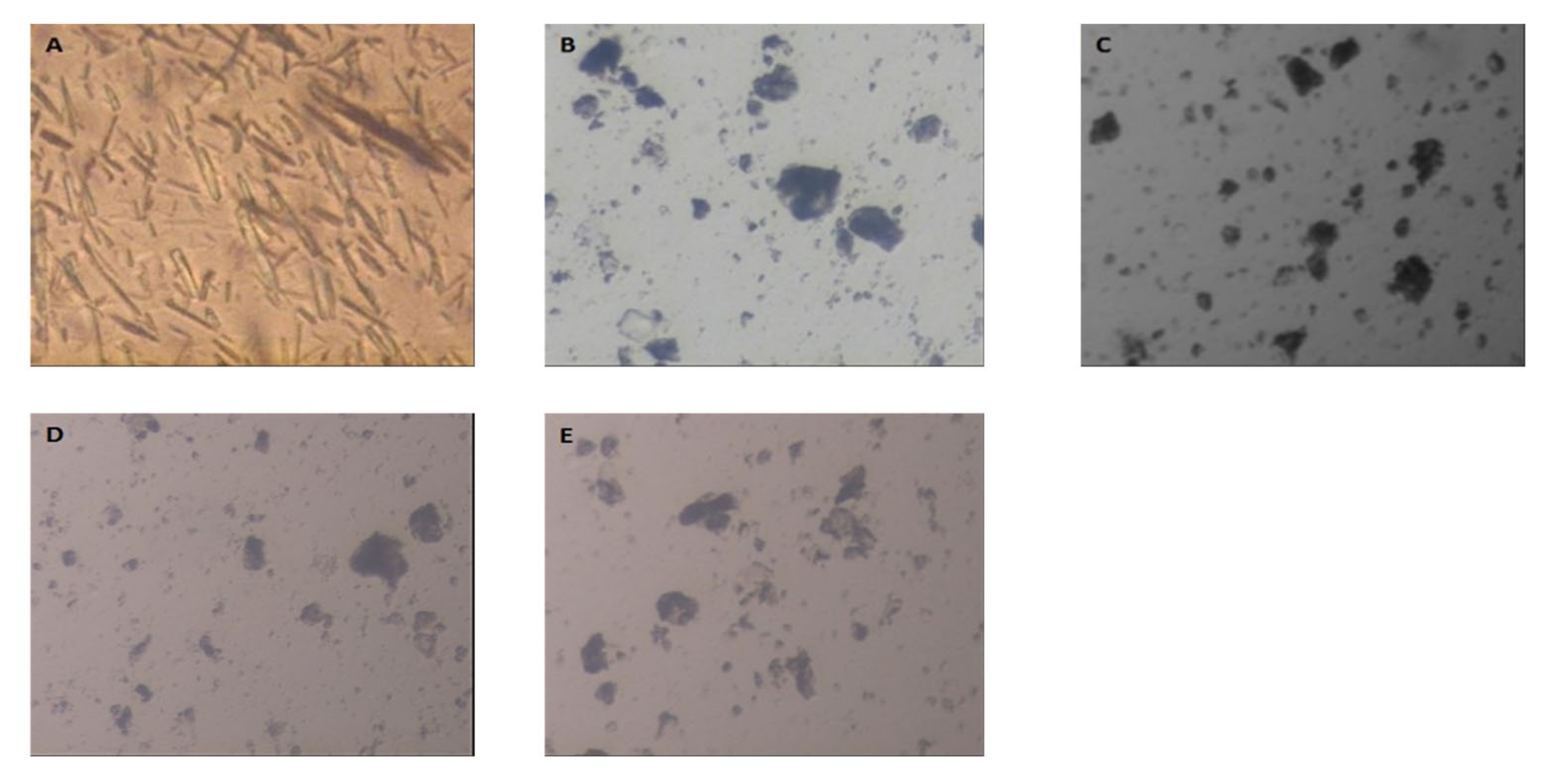
2.6. Optical Microscope Examination of Tel-SSDs
2.7. Determination of Telmisartan Content in Tel-SSDs
2.8. Determination of the Percentage Yield
2.9. Saturation Aqueous Solubility Study
2.10. Dissolution Study
2.10.1. Development of Dissolution Media
2.10.2. In Vitro Dissolution Profiles
2.10.3. In Vitro Dissolution Profiles Study
2.10.4. Comparison of Dissolution Data Profiles Using Ddsolver Software Program
- Model selection,
- Characterizing the release curves and establishment of corresponding kinetic parameters,
- Dissolution profile comparison,
- Selection of the best formulae that caused the highest improvement in release rates.
2.10.5. Kinetic Analysis of Dissolution Data
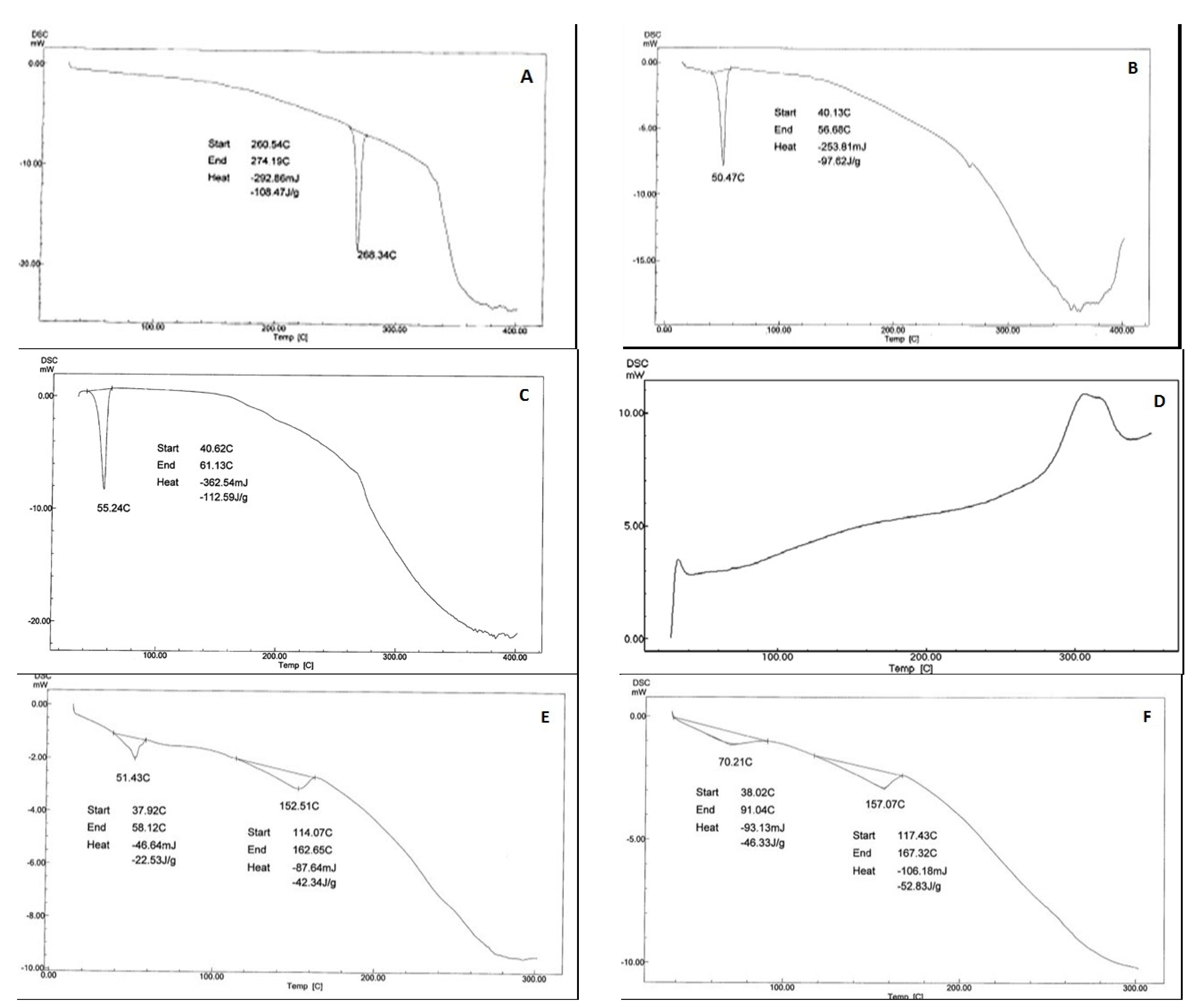
2.10.6. Differential Scanning Salorimetry (DSC)
2.10.7. Effect of Aging
3. Results and Discussion
3.1. Compatibility Evaluation of Telmisartan with Different Carriers Using FTIR
3.2. Optical Microscope Examination
3.3. Telmisartan SSDs Drug Content and Percentage Yield
3.4. Saturation Aqueous Solubility Study
3.5. Development of Dissolution Media
3.6. In Vitro Dissolution Profiles
3.7. Comparison of Dissolution Data Profiles Using Ddsolver Software Program
| Model | Parameter | Tel | F1 | F2 | F3 | F4 | F5 | F6 | F7 | F8 | F9 | F10 | F11 | F12 | F13 | F14 | F15 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Weibull | R2 | 0.99 | 0.99 | 0.99 | 0.98 | 0.99 | 0.99 | 0.99 | 0.99 | 0.98 | 0.99 | 0.99 | 0.99 | 0.99 | 0.99 | 0.99 | 0.99 |
| MSE | 1.56 | 3.10 | 0.47 | 4.76 | 2.33 | 1.33 | 2.27 | 4.50 | 4.82 | 3.43 | 3.18 | 9.46 | 2.23 | 1.91 | 3.78 | 4.49 | |
| WSS | 7.79 | 15.52 | 2.34 | 23.82 | 11.65 | 6.64 | 11.36 | 22.48 | 24.10 | 17.16 | 15.91 | 47.32 | 11.13 | 9.54 | 18.92 | 22.45 | |
| AIC | 18.37 | 23.19 | 9.97 | 26.19 | 21.19 | 17.25 | 21.01 | 25.79 | 26.28 | 23.90 | 23.37 | 31.00 | 20.87 | 19.79 | 24.58 | 25.78 | |
| MSC | 3.41 | 3.11 | 5.10 | 2.69 | 3.20 | 3.48 | 3.06 | 3.20 | 2.66 | 3.05 | 3.27 | 1.75 | 3.41 | 3.67 | 2.58 | 2.60 | |
| α | 11.10 | 6.47 | 8.86 | 5.31 | 3.82 | 2.58 | 2.89 | 2.36 | 1.67 | 1.76 | 2.76 | 1.93 | 1.85 | 1.84 | 1.39 | 1.66 | |
| Td | 294.28 | 114.20 | 128.66 | 92.35 | 71.27 | 40.87 | 48.71 | 5.95 | 3.50 | 3.48 | 17.71 | 11.05 | 6.11 | 3.61 | 2.31 | 2.81 | |
| β | 0.42 | 0.39 | 0.45 | 0.37 | 0.31 | 0.26 | 0.27 | 0.48 | 0.41 | 0.45 | 0.35 | 0.27 | 0.34 | 0.47 | 0.40 | 0.49 | |
| T1/2 | 123.84 | 45.04 | 56.89 | 34.19 | 22.17 | 9.76 | 12.73 | 2.78 | 1.43 | 1.56 | 6.28 | 2.88 | 2.09 | 1.67 | 0.91 | 1.33 | |
| First order Model | R2 | 0.92 | 0.91 | 0.93 | 0.89 | 0.87 | 0.85 | 0.85 | 0.97 | 0.97 | 0.98 | 0.92 | 0.89 | 0.95 | 0.98 | 0.98 | 0.98 |
| MSE | 65.91 | 129.59 | 91.49 | 162.55 | 221.54 | 299.46 | 278.83 | 73.47 | 74.21 | 52.84 | 210.83 | 270.27 | 152.78 | 45.19 | 53.36 | 32.02 | |
| WSS | 461.36 | 907.15 | 640.40 | 1137.85 | 1550.79 | 2096.19 | 1951.84 | 514.30 | 519.44 | 369.87 | 1475.84 | 1891.87 | 1069.46 | 316.35 | 373.51 | 224.15 | |
| AIC | 51.07 | 56.48 | 53.70 | 58.30 | 60.77 | 63.18 | 62.61 | 51.94 | 52.02 | 49.31 | 60.38 | 62.36 | 57.80 | 48.05 | 49.38 | 45.30 | |
| MSC | −0.16 | −0.38 | 0.00 | −0.56 | −0.95 | −1.30 | −1.20 | 0.95 | 0.75 | 1.14 | −0.46 | −0.88 | −0.10 | 1.31 | 1.01 | 1.61 | |
| K | 0.012 | 0.019 | 0.017 | 0.022 | 0.027 | 0.038 | 0.035 | 0.125 | 0.168 | 0.181 | 0.056 | 0.070 | 0.108 | 0.181 | 0.218 | 0.221 | |
| T1/2 | 60.09 | 36.03 | 41.88 | 31.22 | 25.33 | 18.20 | 20.06 | 5.53 | 4.12 | 3.84 | 12.42 | 9.90 | 6.43 | 3.82 | 3.18 | 3.13 | |
| Zero Order | R2 | 0.90 | 0.86 | 0.88 | 0.84 | 0.78 | 0.71 | 0.73 | 0.73 | 0.68 | 0.67 | 0.77 | 0.71 | 0.70 | 0.67 | 0.64 | 0.64 |
| MSE | 36.34 | 86.13 | 66.12 | 114.34 | 169.62 | 263.85 | 237.27 | 525.80 | 634.29 | 668.21 | 301.02 | 379.79 | 489.87 | 675.16 | 728.86 | 766.35 | |
| WSS | 218.03 | 516.79 | 396.69 | 686.02 | 1017.72 | 1583.08 | 1423.60 | 3154.81 | 3805.73 | 4009.24 | 1806.13 | 2278.74 | 2939.24 | 4050.95 | 4373.18 | 4598.12 | |
| AIC | 47.08 | 53.98 | 51.87 | 56.25 | 59.40 | 62.94 | 62.09 | 68.45 | 69.95 | 70.37 | 63.99 | 65.85 | 67.89 | 70.45 | 71.07 | 71.47 | |
| MSC | 0.34 | −0.07 | 0.23 | −0.31 | −0.78 | −1.27 | −1.14 | −1.11 | −1.49 | −1.50 | −0.91 | −1.32 | −1.36 | −1.49 | −1.70 | −1.66 | |
| K | 0.55 | 0.71 | 0.69 | 0.74 | 0.73 | 0.73 | 0.73 | 1.11 | 1.04 | 1.05 | 0.93 | 0.89 | 0.98 | 1.06 | 1.01 | 1.02 | |
| T1/2 | 58.54 | 42.06 | 46.01 | 39.05 | 35.82 | 32.05 | 33.05 | 21.93 | 21.36 | 21.00 | 27.42 | 26.29 | 23.62 | 20.95 | 20.83 | 20.49 | |
| Higuchi Model | R2 | 0.86 | 0.66 | 0.86 | 0.46 | −0.26 | −2.27 | −1.48 | −1.37 | −4.41 | −4.41 | −0.67 | −3.02 | −3.08 | −4.27 | −8.35 | −6.92 |
| MSE | 9.50 | 35.03 | 16.13 | 56.19 | 106.78 | 208.36 | 176.42 | 385.80 | 551.85 | 579.70 | 205.50 | 323.75 | 406.82 | 582.55 | 688.22 | 708.41 | |
| WSS | 57.00 | 210.20 | 96.78 | 337.14 | 640.65 | 1250.18 | 1058.53 | 2314.80 | 3311.10 | 3478.21 | 1232.99 | 1942.50 | 2440.93 | 3495.31 | 4129.32 | 4250.46 | |
| AIC | 30.30 | 39.44 | 34.01 | 42.74 | 47.24 | 51.92 | 50.75 | 56.23 | 58.74 | 59.08 | 51.82 | 55.00 | 56.60 | 59.11 | 60.28 | 60.48 | |
| MSC | 1.70 | 0.79 | 1.67 | 0.32 | −0.52 | −1.47 | −1.19 | −1.15 | −1.97 | −1.97 | −0.80 | −1.68 | −1.69 | −1.95 | −2.52 | −2.36 | |
| K | 5.67 | 7.97 | 7.24 | 8.63 | 9.53 | 10.79 | 10.43 | 15.71 | 16.26 | 16.56 | 12.48 | 13.12 | 14.65 | 16.60 | 16.78 | 17.07 | |
| T1/2 | 77.75 | 39.37 | 47.69 | 33.54 | 27.54 | 21.47 | 22.97 | 10.13 | 9.45 | 9.12 | 16.05 | 14.52 | 11.64 | 9.07 | 8.88 | 8.58 |
3.8. Differential Scanning Calorimetry (DSC)
3.9. Effect of Aging
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Roth, G.A.; Mensah, G.A.; Johnson, C.O.; Addolorato, G.; Ammirati, E.; Baddour, L.M.; Barengo, N.C.; Beaton, A.Z.; Benjamin, E.J.; Benziger, C.P.; et al. Global burden of cardiovascular diseases and risk factors, 1990–2019: Update from the gbd 2019 study. J. Am. Coll. Cardiol. 2020, 76, 2982–3021. [Google Scholar] [CrossRef] [PubMed]
- Giri, B.R.; Kwon, J.; Vo, A.Q.; Bhagurkar, A.M.; Bandari, S.; Kim, D.W. Hot-melt extruded amorphous solid dispersion for solubility, stability, and bioavailability enhancement of telmisartan. Pharmaceuticals 2021, 14, 73. [Google Scholar] [CrossRef] [PubMed]
- Wienen, W.; Entzeroth, M.; van Meel, J.C.A.; Stangier, J.; Busch, U.; Ebner, T.; Schmid, J.; Lehmann, H.; Matzek, K.; Kempthorne-Rawson, J.; et al. A review on telmisartan: A novel, long-acting angiotensin ii-receptor antagonist. Cardiovasc. Drug Rev. 2000, 18, 127–154. [Google Scholar] [CrossRef]
- Al-Japairai, K.A.S.; Alkhalidi, H.M.; Mahmood, S.; Almurisi, S.H.; Doolaanea, A.A.; Al-Sindi, T.A.; Chatterjee, B. Lyophilized amorphous dispersion of telmisartan in a combined carrier–alkalizer system: Formulation development and in vivo study. ACS Omega 2020, 5, 32466–32480. [Google Scholar] [CrossRef] [PubMed]
- Kundu, S.; Kumari, N.; Soni, S.R.; Ranjan, S.; Kumar, R.; Sharon, A.; Ghosh, A. Enhanced solubility of telmisartan phthalic acid cocrystals within the ph range of a systemic absorption site. ACS Omega 2018, 3, 15380–15388. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bhujbal, S.V.; Mitra, B.; Jain, U.; Gong, Y.; Agrawal, A.; Karki, S.; Taylor, L.S.; Kumar, S.; Zhou, Q. Pharmaceutical amorphous solid dispersion: A review of manufacturing strategies. Acta Pharm. Sin. B 2021, 11, 2505–2536. [Google Scholar] [CrossRef]
- Frank, D.; Schenck, L.; Koynov, A.; Su, Y.; Li, Y.; Variankaval, N. Optimizing solvent selection and processing conditions to generate high bulk-density, co-precipitated amorphous dispersions of posaconazole. Pharmaceutics 2021, 13, 2017. [Google Scholar] [CrossRef]
- Iyer, R.; Petrovska Jovanovska, V.; Berginc, K.; Jaklič, M.; Fabiani, F.; Harlacher, C.; Huzjak, T.; Sanchez-Felix, M.V. Amorphous solid dispersions (asds): The influence of material properties, manufacturing processes and analytical technologies in drug product development. Pharmaceutics 2021, 13, 1682. [Google Scholar] [CrossRef]
- Vasconcelos, T.; Sarmento, B.; Costa, P. Solid dispersions as strategy to improve oral bioavailability of poor water soluble drugs. Drug Discov. Today 2007, 12, 1068–1075. [Google Scholar] [CrossRef]
- Vo, C.L.-N.; Park, C.; Lee, B.-J. Current trends and future perspectives of solid dispersions containing poorly water-soluble drugs. Eur. J. Pharm. Biopharm. 2013, 85, 799–813. [Google Scholar] [CrossRef]
- Sandeep, D.; Vidyadhara, S.; Sailaja, Y.; Lakshmi, B.S.; Vanya, N. Formulation and evaluation of atorvastatin solid dispersions using entada scandens seed starch as superdisintegrant. Res. J. Pharm. Technol. 2021, 14, 5141–5149. [Google Scholar]
- Qushawy, M.; Nasr, A.; Swidan, S.; Mortagi, Y. Development and characterization of glimepiride novel solid nanodispersion for improving its oral bioavailability. Sci. Pharm. 2020, 88, 52–69. [Google Scholar] [CrossRef]
- Ismail, E.A.; Elamin, E.S.; Ahmed, E.M.M.; Abdelrahman, M. Enhancement of aqueous solubility of meloxicam using solid dispersions based on ziziphus spina-christi gums. Drug Des. 2021, 10, 188. [Google Scholar]
- Rohrs, B. Dissolution method development for poorly soluble compounds. Dissolution Technol. 2001, 8, 6–12. [Google Scholar] [CrossRef]
- Ha, E.S.; Kim, J.S.; Baek, I.H.; Yoo, J.W.; Jung, Y.; Moon, H.R.; Kim, M.S. Development of megestrol acetate solid dispersion nanoparticles for enhanced oral delivery by using a supercritical antisolvent process. Drug Des. Dev. Ther. 2015, 9, 4269–4277. [Google Scholar]
- Rane, Y.; Mashru, R.; Sankalia, M.; Sankalia, J. Effect of hydrophilic swellable polymers on dissolution enhancement of carbamazepine solid dispersions studied using response surface methodology. AAPS PharmSciTech 2007, 8, 27. [Google Scholar] [CrossRef] [Green Version]
- Dastmalchi, S.; Garjani, A.; Maleki, N.; Sheikhee, G.; Baghchevan, V.; Jafari-Azad, P.; Valizadeh, H.; Barzegar-Jalali, M. Enhancing dissolution, serum concentrations and hypoglycemic effect of glibenclamide using solvent deposition technique. J. Pharm. Pharm. Sci. 2005, 8, 175–181. [Google Scholar]
- Zhang, Y.; Huo, M.; Zhou, J.; Zou, A.; Li, W.; Yao, C.; Xie, S. Ddsolver: An add-in program for modeling and comparison of drug dissolution profiles. AAPS J. 2010, 12, 263–271. [Google Scholar] [CrossRef] [Green Version]
- Hambisa, S.; Yohannes, S.; Suleman, S. In vitro comparative quality assessment of different brands of norfloxacin tablets available in jimma, southwest ethiopia. Drug Des. Dev. Ther. 2019, 13, 1241–1249. [Google Scholar] [CrossRef] [Green Version]
- Lokhandwala, H.; Deshpande, A.; Deshpande, S. Kinetic modeling and dissolution profiles comparison: An overview. Int. J. Pharma Bio Sci. 2013, 4, 728–737. [Google Scholar]
- Higuchi, T. Mechanism of sustained-action medication. Theoretical analysis of rate of release of solid drugs dispersed in solid matrices. J. Pharm. Sci. 1963, 52, 1145–1149. [Google Scholar] [CrossRef] [PubMed]
- Hameed, H.A.; Khan, S.; Shahid, M.; Ullah, R.; Bari, A.; Ali, S.S.; Hussain, Z.; Sohail, M.; Khan, S.U.; Htar, T.T. Engineering of naproxen loaded polymer hybrid enteric microspheres for modified release tablets: Development, characterization, in silico modelling and in vivo evaluation. Drug Des. Dev. Ther. 2020, 14, 27–41. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Adams, E.; Coomans, D.; Smeyers-Verbeke, J.; Massart, D.L. Non-linear mixed effects models for the evaluation of dissolution profiles. Int. J. Pharm. 2002, 240, 37–53. [Google Scholar] [CrossRef]
- Karagianni, A.; Kachrimanis, K.; Nikolakakis, I. Co-amorphous solid dispersions for solubility and absorption improvement of drugs: Composition, preparation, characterization and formulations for oral delivery. Pharmaceutics 2018, 10, 98. [Google Scholar] [CrossRef] [Green Version]
- Sangwai, M.; Vavia, P. Amorphous ternary cyclodextrin nanocomposites of telmisartan for oral drug delivery: Improved solubility and reduced pharmacokinetic variability. Int. J. Pharm. 2013, 453, 423–432. [Google Scholar] [CrossRef]
- Markl, D.; Zeitler, J.A. A review of disintegration mechanisms and measurement techniques. Pharm. Res. 2017, 34, 890–917. [Google Scholar] [CrossRef] [Green Version]
- Quodbach, J.; Kleinebudde, P. Systematic classification of tablet disintegrants by water uptake and force development kinetics. J. Pharm. Pharmacol. 2014, 66, 1429–1438. [Google Scholar] [CrossRef]
- Quodbach, J.; Kleinebudde, P. Performance of tablet disintegrants: Impact of storage conditions and relative tablet density. Pharm. Dev. Technol. 2015, 20, 762–768. [Google Scholar] [CrossRef]
- Costa, P.; Sousa Lobo, J.M. Modeling and comparison of dissolution profiles. Eur. J. Pharm. Sci. 2001, 13, 123–133. [Google Scholar] [CrossRef]
- Uebbing, L.; Klumpp, L.; Webster, G.K.; Löbenberg, R. Justification of disintegration testing beyond current fda criteria using in vitro and in silico models. Drug Des. Dev. Ther. 2017, 11, 1163–1174. [Google Scholar] [CrossRef] [Green Version]
- Lee, H.G.; Park, Y.S.; Jeong, J.H.; Kwon, Y.B.; Shin, D.H.; Kim, J.Y.; Rhee, Y.S.; Park, E.S.; Kim, D.W.; Park, C.W. Physicochemical properties and drug-release mechanisms of dual-release bilayer tablet containing mirabegron and fesoterodine fumarate. Drug Des. Dev. Ther. 2019, 13, 2459–2474. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rescigno, A.; Marzo, A.; Thyroff-Friesinger, U. Mefenamic acid bioequivalence assessment with a new statistical procedure. Pharmacol. Res. 1996, 34, 149–152. [Google Scholar] [CrossRef] [PubMed]
- Cardot, J.M.; Roudier, B.; Schütz, H. Dissolution comparisons using a multivariate statistical distance (msd) test and a comparison of various approaches for calculating the measurements of dissolution profile comparison. AAPS J. 2017, 19, 1091–1101. [Google Scholar] [CrossRef]
- Podczeck, F. Comparison of in vitro dissolution profiles by calculating mean dissolution time (mdt) or mean residence time (mrt). Int. J. Pharm. 1993, 97, 93–100. [Google Scholar] [CrossRef]
- Liu, P.; Zhou, J.Y.; Chang, J.H.; Liu, X.G.; Xue, H.F.; Wang, R.X.; Li, Z.S.; Li, C.S.; Wang, J.; Liu, C.Z. Soluplus-mediated diosgenin amorphous solid dispersion with high solubility and high stability: Development, characterization and oral bioavailability. Drug Des. Dev. Ther. 2020, 14, 2959–2975. [Google Scholar] [CrossRef] [PubMed]
- Kate, V.K.; Payghan, S.A.; Shinde, A.J. Effect of aging conditions on the dissolution stability of piroxicam mucoadhesive fast disintegrating tablet. Inventi Rapid NDDS 2013, 2013, 1–6. [Google Scholar]




| Code | SSDs Ingredients | Ratio (T:S:H) | % Yield | Drug Content% | Solubility (µg/mL) | |||
|---|---|---|---|---|---|---|---|---|
| Tel (T) | Superdisintegrant (S) | Hydrophilic Carrier (H) | ||||||
| P-SSDs with (S) | F1 | T | (SSG) | - | 1:1:0 | 90.1 | 98.73 | 6.23 |
| F2 | T | (CP) | - | 1:1:0 | 96.4 | 97.27 | 7.84 | |
| F3 | T | (CCS) | - | 1:1:0 | 90.8 | 98.73 | 5.44 | |
| P-SSDs with (H) | F4 | T | - | PVP K30 | 1:0:1 | 92.7 | 102.73 | 11.37 |
| F5 | T | - | PEG 4000 | 1:0:1 | 89.6 | 98.64 | 10.29 | |
| F6 | T | - | Poloxamer 407 | 1:0:1 | 95.4 | 100.19 | 12.35 | |
| C-SSDs combined carrier | F7 | T | SSG | PVP K30 | 1:1:1 | 91.8 | 97.27 | 19.60 |
| F8 | T | SSG | PEG 4000 | 1:1:1 | 93.2 | 94.15 | 24.96 | |
| F9 | T | SSG | Poloxamer 407 | 1:1:1 | 94.9 | 96.98 | 27.76 | |
| F10 | T | CP | PVP K30 | 1:1:1 | 95.2 | 104.39 | 21.13 | |
| F11 | T | CP | PEG 4000 | 1:1:1 | 90.6 | 100.58 | 23.07 | |
| F12 | T | CP | Poloxamer 407 | 1:1:1 | 93.1 | 101.85 | 23.85 | |
| F13 | T | CCS | PVP K30 | 1:1:1 | 91.5 | 95.42 | 20.77 | |
| F14 | T | CCS | PEG 4000 | 1:1:1 | 92.8 | 95.52 | 26.70 | |
| F15 | T | CCS | Poloxamer 407 | 1:1:1 | 93.3 | 97.66 | 28.52 | |
| Different Dissolution Media | Solubility cs (μg/mL) | Sink Condition cs/cd |
|---|---|---|
| Water | 2.931 | 0.07 |
| Stimulated saliva Fluid pH 6.8 | 4.647 | 0.12 |
| Stimulated saliva Fluid pH 6.8 + 0.5% tween 80 | 12.75 | 0.32 |
| Stimulated saliva Fluid pH 6.8 + 1.0% tween 80 | 18.23 | 0.46 |
| Stimulated saliva Fluid pH 6.8 + 2.0% tween 80 | 33.72 | 0.84 |
| Stimulated saliva Fluid pH 6.8 + 3.0% tween 80 | 25.82 | 0.65 |
| Stimulated saliva Fluid pH 6.8 + 6.0% tween 80 | 43.92 | 1.09 |
| Stimulated saliva Fluid pH 6.8 + 1.5% SLS | 12.49 | 0.312 |
| Stimulated saliva Fluid pH 6.8 + 2.0% SLS | 11.96 | 0.29 |
| Phosphate buffer 7.4 | 4.84 | 0.12 |
| Phosphate buffer 7.4 + 0.5% tween 80 | 30.19 | 0.75 |
| Phosphate buffer 7.4 + 1.0% tween 80 | 54.90 | 1.37 |
| Phosphate buffer 7.4 + 2.0% tween 80 | 110.01 | 2.75 |
| Phosphate buffer 7.4 + 0.5% SLS | 58.82 | 1.47 |
| Phosphate buffer 7.4 + 1.0% SLS | 94.31 | 2.36 |
| Phosphate buffer 7.4 + 1.5% SLS | 130.39 | 3.26 |
| Model | Parameter | Tel | F1 | F2 | F3 | F4 | F5 | F6 | F7 | F8 | F9 | F10 | F11 | F12 | F13 | F14 | F15 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Weibull | α | 11.10 | 6.47 | 8.86 | 5.31 | 3.82 | 2.58 | 2.89 | 2.36 | 1.67 | 1.76 | 2.76 | 1.93 | 1.85 | 1.84 | 1.39 | 1.66 |
| Td | 294.28 | 114.2 | 128.66 | 92.35 | 71.27 | 40.87 | 48.71 | 5.95 | 3.50 | 3.48 | 17.71 | 11.05 | 6.11 | 3.61 | 2.31 | 2.81 | |
| β | 0.42 | 0.39 | 0.45 | 0.37 | 0.31 | 0.26 | 0.27 | 0.48 | 0.41 | 0.45 | 0.35 | 0.27 | 0.34 | 0.47 | 0.40 | 0.49 | |
| T1/2 | 123.84 | 45.04 | 56.89 | 34.19 | 22.17 | 9.76 | 12.73 | 2.78 | 1.43 | 1.56 | 6.28 | 2.88 | 2.09 | 1.67 | 0.91 | 1.33 |
| Formula | f1 | f2 | f1’ | ξ1 | ξ2 | Sd | D1 | D2 | Description |
|---|---|---|---|---|---|---|---|---|---|
| F1 | 42.40 | 45.75 | 35.01 | 0.17 | 0.17 | 0.16 | 11.99 | 12.12 | Different |
| F2 | 27.69 | 54.09 | 24.32 | 0.13 | 0.13 | 0.10 | 7.82 | 8.22 | Different |
| F3 | 55.45 | 40.02 | 43.42 | 0.21 | 0.21 | 0.20 | 15.67 | 15.80 | Different |
| F4 | 74.04 | 33.85 | 54.04 | 0.26 | 0.26 | 0.26 | 20.92 | 21.02 | Different |
| F5 | 100.24 | 27.32 | 66.77 | 0.32 | 0.32 | 0.33 | 28.32 | 28.40 | Different |
| F6 | 92.75 | 28.98 | 63.37 | 0.30 | 0.30 | 0.31 | 26.21 | 26.31 | Different |
| F7 | 189.94 | 13.43 | 97.42 | 0.48 | 0.47 | 0.49 | 53.67 | 53.88 | Different |
| F8 | 203.91 | 11.95 | 100.97 | 0.49 | 0.49 | 0.51 | 57.62 | 57.68 | Different |
| F9 | 209.61 | 11.34 | 102.35 | 0.50 | 0.49 | 0.52 | 59.23 | 59.31 | Different |
| F10 | 129.01 | 21.84 | 78.42 | 0.38 | 0.38 | 0.38 | 36.45 | 36.57 | Different |
| F11 | 144.18 | 19.48 | 83.78 | 0.40 | 0.40 | 0.42 | 40.74 | 40.75 | Different |
| F12 | 172.74 | 15.55 | 92.69 | 0.45 | 0.44 | 0.46 | 48.81 | 48.86 | Different |
| F13 | 210.35 | 11.26 | 102.52 | 0.50 | 0.50 | 0.52 | 59.44 | 59.54 | Different |
| F14 | 215.87 | 10.72 | 103.82 | 0.50 | 0.50 | 0.53 | 60.99 | 61.04 | Different |
| F15 | 221.01 | 10.19 | 104.99 | 0.51 | 0.51 | 0.54 | 62.45 | 62.55 | Different |
| Parameters | PD15 | PD45 | AUC | MRT | MDT | DE45% | DEAll% | SD |
|---|---|---|---|---|---|---|---|---|
| Tel | 23.53 | 35.66 | 1745.05 | 27.842 | 17.991 | 19.91 | 29.084 | 0.01 |
| F1 | 34.93 | 49.26 | 2462.55 | 26.708 | 16.315 | 30.23 | 41.043 | 0.05 |
| F2 | 31.37 | 45.83 | 2243.75 | 26.955 | 15.988 | 24.5 | 37.396 | 0.02 |
| F3 | 39.22 | 50.74 | 2663.28 | 26.534 | 16.095 | 33.74 | 44.388 | 0.06 |
| F4 | 44.61 | 57.97 | 2987.55 | 26.273 | 11.240 | 39.4 | 49.793 | 0.01 |
| F5 | 52.57 | 64.09 | 3391.08 | 25.999 | 8.566 | 47.48 | 56.518 | 0.08 |
| F6 | 50.37 | 62.38 | 3276.68 | 26.106 | 9.073 | 44.81 | 54.611 | 0.01 |
| F7 | 77.1 | 94.41 | 4929.50 | 14.743 | 9.405 | 67.6 | 82.158 | 0.08 |
| F8 | 81.99 | 95.96 | 5113.43 | 13.561 | 7.907 | 74.655 | 85.224 | 0.04 |
| F9 | 84.56 | 97.55 | 5209.50 | 11.517 | 7.453 | 75.6733 | 86.825 | 0.01 |
| F10 | 60.91 | 75.12 | 3894.38 | 23.303 | 11.707 | 52.94 | 64.906 | 0.05 |
| F11 | 63.73 | 77.94 | 4097.78 | 23.175 | 10.901 | 60.455 | 68.296 | 0.02 |
| F12 | 73.99 | 85.5 | 4582.10 | 20.262 | 9.725 | 66.1083 | 76.368 | 0.03 |
| F13 | 84.56 | 97.79 | 5222.03 | 11.241 | 7.327 | 75.55 | 87.034 | 0.06 |
| F14 | 86.4 | 97.92 | 5282.45 | 11.191 | 6.717 | 79.575 | 88.041 | 0.01 |
| F15 | 86.39 | 98.7 | 5379.35 | 8.355 | 6.104 | 79.51 | 89.656 | 0.02 |
| Formula | Drug Content% before Aging | Drug Content% after Aging |
|---|---|---|
| F14 | 95.52 | 94.38 n.s |
| F15 | 97.66 | 96.03 n.s |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aldeeb, R.A.; El-Miligi, M.F.; El-Nabarawi, M.; Tag, R.; Amin, H.M.S.; Taha, A.A. Enhancement of the Solubility and Dissolution Rate of Telmisartan by Surface Solid Dispersions Employing Superdisintegrants, Hydrophilic Polymers and Combined Carriers. Sci. Pharm. 2022, 90, 71. https://doi.org/10.3390/scipharm90040071
Aldeeb RA, El-Miligi MF, El-Nabarawi M, Tag R, Amin HMS, Taha AA. Enhancement of the Solubility and Dissolution Rate of Telmisartan by Surface Solid Dispersions Employing Superdisintegrants, Hydrophilic Polymers and Combined Carriers. Scientia Pharmaceutica. 2022; 90(4):71. https://doi.org/10.3390/scipharm90040071
Chicago/Turabian StyleAldeeb, Reem A., Mohamed Farid El-Miligi, Mohamed El-Nabarawi, Randa Tag, Hany M. S. Amin, and A. A. Taha. 2022. "Enhancement of the Solubility and Dissolution Rate of Telmisartan by Surface Solid Dispersions Employing Superdisintegrants, Hydrophilic Polymers and Combined Carriers" Scientia Pharmaceutica 90, no. 4: 71. https://doi.org/10.3390/scipharm90040071





