Journal Description
Cells
Cells
is an international, peer-reviewed, open access journal on cell biology, molecular biology, and biophysics, published semimonthly online by MDPI. The Spanish Society for Biochemistry and Molecular Biology (SEBBM), Nordic Autophagy Society (NAS), Spanish Society of Hematology and Hemotherapy (SEHH) and Society for Regenerative Medicine (Russian Federation) (RPO) are affiliated with Cells and their members receive discounts on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, MEDLINE, PMC, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q2 (Cell Biology) / CiteScore - Q1 (General Biochemistry, Genetics and Molecular Biology)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 16.6 days after submission; acceptance to publication is undertaken in 2.8 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Sections: published in 21 topical sections.
- Companion journal: Organoids.
Impact Factor:
6.0 (2022);
5-Year Impact Factor:
6.7 (2022)
Latest Articles
Deciphering the Molecular Mechanisms behind Drug Resistance in Ovarian Cancer to Unlock Efficient Treatment Options
Cells 2024, 13(9), 786; https://doi.org/10.3390/cells13090786 (registering DOI) - 04 May 2024
Abstract
Ovarian cancer is a highly lethal form of gynecological cancer. This disease often goes undetected until advanced stages, resulting in high morbidity and mortality rates. Unfortunately, many patients experience relapse and succumb to the disease due to the emergence of drug resistance that
[...] Read more.
Ovarian cancer is a highly lethal form of gynecological cancer. This disease often goes undetected until advanced stages, resulting in high morbidity and mortality rates. Unfortunately, many patients experience relapse and succumb to the disease due to the emergence of drug resistance that significantly limits the effectiveness of currently available oncological treatments. Here, we discuss the molecular mechanisms responsible for resistance to carboplatin, paclitaxel, polyadenosine diphosphate ribose polymerase inhibitors, and bevacizumab in ovarian cancer. We present a detailed analysis of the most extensively investigated resistance mechanisms, including drug inactivation, drug target alterations, enhanced drug efflux pumps, increased DNA damage repair capacity, and reduced drug absorption/accumulation. The in-depth understanding of the molecular mechanisms associated with drug resistance is crucial to unveil new biomarkers capable of predicting and monitoring the kinetics during disease progression and discovering new therapeutic targets.
Full article
(This article belongs to the Special Issue Unlocking the Secrets behind Drug Resistance at the Cellular Level)
Open AccessArticle
Systemic LPS Administration Stimulates the Activation of Non-Neuronal Cells in an Experimental Model of Spinal Muscular Atrophy
by
Eleni Karafoulidou, Evangelia Kesidou, Paschalis Theotokis, Chrystalla Konstantinou, Maria-Konstantina Nella, Iliana Michailidou, Olga Touloumi, Eleni Polyzoidou, Ilias Salamotas, Ofira Einstein, Athanasios Chatzisotiriou, Marina-Kleopatra Boziki and Nikolaos Grigoriadis
Cells 2024, 13(9), 785; https://doi.org/10.3390/cells13090785 (registering DOI) - 04 May 2024
Abstract
Spinal muscular atrophy (SMA) is a neurodegenerative disease caused by deficiency of the survival motor neuron (SMN) protein. Although SMA is a genetic disease, environmental factors contribute to disease progression. Common pathogen components such as lipopolysaccharides (LPS) are considered significant contributors to inflammation
[...] Read more.
Spinal muscular atrophy (SMA) is a neurodegenerative disease caused by deficiency of the survival motor neuron (SMN) protein. Although SMA is a genetic disease, environmental factors contribute to disease progression. Common pathogen components such as lipopolysaccharides (LPS) are considered significant contributors to inflammation and have been associated with muscle atrophy, which is considered a hallmark of SMA. In this study, we used the SMNΔ7 experimental mouse model of SMA to scrutinize the effect of systemic LPS administration, a strong pro-inflammatory stimulus, on disease outcome. Systemic LPS administration promoted a reduction in SMN expression levels in CNS, peripheral lymphoid organs, and skeletal muscles. Moreover, peripheral tissues were more vulnerable to LPS-induced damage compared to CNS tissues. Furthermore, systemic LPS administration resulted in a profound increase in microglia and astrocytes with reactive phenotypes in the CNS of SMNΔ7 mice. In conclusion, we hereby show for the first time that systemic LPS administration, although it may not precipitate alterations in terms of deficits of motor functions in a mouse model of SMA, it may, however, lead to a reduction in the SMN protein expression levels in the skeletal muscles and the CNS, thus promoting synapse damage and glial cells’ reactive phenotype.
Full article
(This article belongs to the Collection Feature Papers in 'Cells of the Nervous System' Section)
►▼
Show Figures
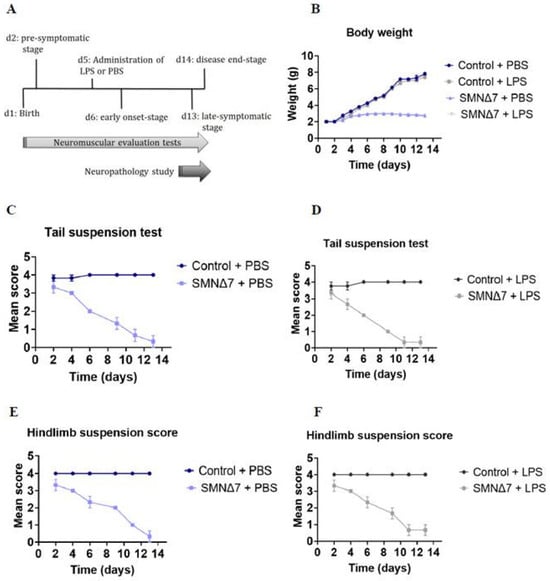
Figure 1
Open AccessReview
Ketone Bodies after Cardiac Arrest: A Narrative Review and the Rationale for Use
by
Filippo Annoni, Elisa Gouvea Bogossian, Lorenzo Peluso, Fuhong Su, Anthony Moreau, Leda Nobile, Stefano Giuseppe Casu, Elda Diletta Sterchele, Lorenzo Calabro, Michele Salvagno, Mauro Oddo and Fabio Silvio Taccone
Cells 2024, 13(9), 784; https://doi.org/10.3390/cells13090784 (registering DOI) - 04 May 2024
Abstract
Cardiac arrest survivors suffer the repercussions of anoxic brain injury, a critical factor influencing long-term prognosis. This injury is characterised by profound and enduring metabolic impairment. Ketone bodies, an alternative energetic resource in physiological states such as exercise, fasting, and extended starvation, are
[...] Read more.
Cardiac arrest survivors suffer the repercussions of anoxic brain injury, a critical factor influencing long-term prognosis. This injury is characterised by profound and enduring metabolic impairment. Ketone bodies, an alternative energetic resource in physiological states such as exercise, fasting, and extended starvation, are avidly taken up and used by the brain. Both the ketogenic diet and exogenous ketone supplementation have been associated with neuroprotective effects across a spectrum of conditions. These include refractory epilepsy, neurodegenerative disorders, cognitive impairment, focal cerebral ischemia, and traumatic brain injuries. Beyond this, ketone bodies possess a plethora of attributes that appear to be particularly favourable after cardiac arrest. These encompass anti-inflammatory effects, the attenuation of oxidative stress, the improvement of mitochondrial function, a glucose-sparing effect, and the enhancement of cardiac function. The aim of this manuscript is to appraise pertinent scientific literature on the topic through a narrative review. We aim to encapsulate the existing evidence and underscore the potential therapeutic value of ketone bodies in the context of cardiac arrest to provide a rationale for their use in forthcoming translational research efforts.
Full article
(This article belongs to the Special Issue Molecular and Cellular Mechanisms of Cerebral Ischemia—2nd Edition)
►▼
Show Figures

Figure 1
Open AccessArticle
Withaferin A as a Potential Therapeutic Target for the Treatment of Angiotensin II-Induced Cardiac Cachexia
by
Vasa Vemuri, Nicholas Kratholm, Darini Nagarajan, Dakotah Cathey, Ahmed Abdelbaset-Ismail, Yi Tan, Alex Straughn, Lu Cai, Jiapeng Huang and Sham S. Kakar
Cells 2024, 13(9), 783; https://doi.org/10.3390/cells13090783 - 03 May 2024
Abstract
In our previous studies, we showed that the generation of ovarian tumors in NSG mice (immune-compromised) resulted in the induction of muscle and cardiac cachexia, and treatment with withaferin A (WFA; a steroidal lactone) attenuated both muscle and cardiac cachexia. However, our studies
[...] Read more.
In our previous studies, we showed that the generation of ovarian tumors in NSG mice (immune-compromised) resulted in the induction of muscle and cardiac cachexia, and treatment with withaferin A (WFA; a steroidal lactone) attenuated both muscle and cardiac cachexia. However, our studies could not address if these restorations by WFA were mediated by its anti-tumorigenic properties that might, in turn, reduce the tumor burden or WFA’s direct, inherent anti-cachectic properties. To address this important issue, in our present study, we used a cachectic model induced by the continuous infusion of Ang II by implanting osmotic pumps in immunocompetent C57BL/6 mice. The continuous infusion of Ang II resulted in the loss of the normal functions of the left ventricle (LV) (both systolic and diastolic), including a significant reduction in fractional shortening, an increase in heart weight and LV wall thickness, and the development of cardiac hypertrophy. The infusion of Ang II also resulted in the development of cardiac fibrosis, and significant increases in the expression levels of genes (ANP, BNP, and MHCβ) associated with cardiac hypertrophy and the chemical staining of the collagen abundance as an indication of fibrosis. In addition, Ang II caused a significant increase in expression levels of inflammatory cytokines (IL-6, IL-17, MIP-2, and IFNγ), NLRP3 inflammasomes, AT1 receptor, and a decrease in AT2 receptor. Treatment with WFA rescued the LV functions and heart hypertrophy and fibrosis. Our results demonstrated, for the first time, that, while WFA has anti-tumorigenic properties, it also ameliorates the cardiac dysfunction induced by Ang II, suggesting that it could be an anticachectic agent that induces direct effects on cardiac muscles.
Full article
(This article belongs to the Collection Cardiovascular Disease: From Molecular and Cellular Mechanisms to Therapeutic Opportunities)
►▼
Show Figures
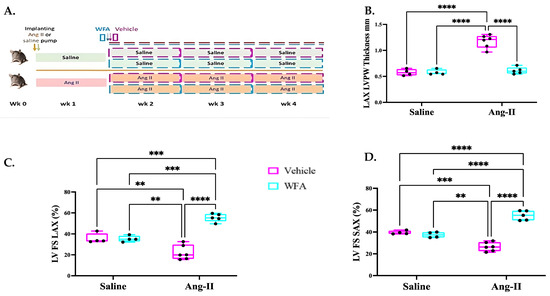
Figure 1
Open AccessArticle
Comprehensive Analysis of CXCR4, JUNB, and PD-L1 Expression in Circulating Tumor Cells (CTCs) from Prostate Cancer Patients
by
Argyro Roumeliotou, Areti Strati, Foteini Chamchougia, Anastasia Xagara, Victoria Tserpeli, Stavroula Smilkou, Elina Lagopodi, Athina Christopoulou, Emmanouil Kontopodis, Ioannis Drositis, Nikolaos Androulakis, Vassilis Georgoulias, Filippos Koinis, Athanasios Kotsakis, Evi Lianidou and Galatea Kallergi
Cells 2024, 13(9), 782; https://doi.org/10.3390/cells13090782 - 03 May 2024
Abstract
CXCR4, JUNB and PD-L1 are implicated in cancer progression and metastasis. The current study investigated these biomarkers in CTCs isolated from metastatic prostate cancer (mPCa) patients at the RNA and protein levels. CTCs were isolated from 48 mPCa patients using the Ficoll density
[...] Read more.
CXCR4, JUNB and PD-L1 are implicated in cancer progression and metastasis. The current study investigated these biomarkers in CTCs isolated from metastatic prostate cancer (mPCa) patients at the RNA and protein levels. CTCs were isolated from 48 mPCa patients using the Ficoll density gradient and ISET system (17 out of 48). The (CK/PD-L1/CD45) and (CK/CXCR4/JUNB) phenotypes were identified using two triple immunofluorescence stainings followed by VyCAP platform analysis. Molecular analysis was conducted with an EpCAM-dependent method for 25/48 patients. CK-8, CK-18, CK-19, JUNB, CXCR4, PD-L1, and B2M (reference gene) were analyzed with RT-qPCR. The (CK+/PD-L1+/CD45–) and the (CK+/CXCR4+/JUNB+) were the most frequent phenotypes (61.1% and 62.5%, respectively). Furthermore, the (CK+/CXCR4+/JUNB–) phenotype was correlated with poorer progression-free survival [(PFS), HR: 2.5, p = 0.049], while the (CK+/PD-L1+/CD45–) phenotype was linked to decreased overall survival [(OS), HR: 262.7, p = 0.007]. Molecular analysis revealed that 76.0% of the samples were positive for CK-8,18, and 19, while 28.0% were positive for JUNB, 44.0% for CXCR4, and 48.0% for PD-L1. Conclusively, CXCR4, JUNB, and PD-L1 were highly expressed in CTCs from mPCa patients. The CXCR4 protein expression was associated with poorer PFS, while PD-L1 was correlated with decreased OS, providing new biomarkers with potential clinical relevance.
Full article
(This article belongs to the Special Issue Cancer-Related Signaling Cascades: Current Knowledge and Potential Therapeutic Targets)
Open AccessReview
Nuclear mTOR Signaling Orchestrates Transcriptional Programs Underlying Cellular Growth and Metabolism
by
Tinghan Zhao, Jialin Fan, Ahmed Abu-Zaid, Stephen K. Burley and X.F. Steven Zheng
Cells 2024, 13(9), 781; https://doi.org/10.3390/cells13090781 - 03 May 2024
Abstract
mTOR is a central regulator of cell growth and metabolism in response to mitogenic and nutrient signals. Notably, mTOR is not only found in the cytoplasm but also in the nucleus. This review highlights direct involvement of nuclear mTOR in regulating transcription factors,
[...] Read more.
mTOR is a central regulator of cell growth and metabolism in response to mitogenic and nutrient signals. Notably, mTOR is not only found in the cytoplasm but also in the nucleus. This review highlights direct involvement of nuclear mTOR in regulating transcription factors, orchestrating epigenetic modifications, and facilitating chromatin remodeling. These effects intricately modulate gene expression programs associated with growth and metabolic processes. Furthermore, the review underscores the importance of nuclear mTOR in mediating the interplay between metabolism and epigenetic modifications. By integrating its functions in nutrient signaling and gene expression related to growth and metabolism, nuclear mTOR emerges as a central hub governing cellular homeostasis, malignant transformation, and cancer progression. Better understanding of nuclear mTOR signaling has the potential to lead to novel therapies against cancer and other growth-related diseases.
Full article
(This article belongs to the Special Issue mTOR Signaling in Metabolism and Cancer 2.0)
►▼
Show Figures
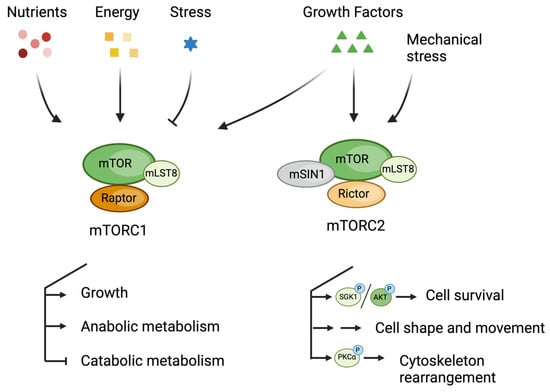
Figure 1
Open AccessArticle
Actin Cytoskeleton Remodeling Accompanied by Redistribution of Adhesion Proteins Drives Migration of Cells in Different EMT States
by
Alla S. Ilnitskaya, Nikita I. Litovka, Svetlana N. Rubtsova, Irina Y. Zhitnyak and Natalya A. Gloushankova
Cells 2024, 13(9), 780; https://doi.org/10.3390/cells13090780 - 02 May 2024
Abstract
Epithelial–mesenchymal transition (EMT) is a process during which epithelial cells lose epithelial characteristics and gain mesenchymal features. Here, we used several cell models to study migratory activity and redistribution of cell–cell adhesion proteins in cells in different EMT states: EGF-induced EMT of epithelial
[...] Read more.
Epithelial–mesenchymal transition (EMT) is a process during which epithelial cells lose epithelial characteristics and gain mesenchymal features. Here, we used several cell models to study migratory activity and redistribution of cell–cell adhesion proteins in cells in different EMT states: EGF-induced EMT of epithelial IAR-20 cells; IAR-6-1 cells with a hybrid epithelial–mesenchymal phenotype; and their more mesenchymal derivatives, IAR-6-1-DNE cells lacking adherens junctions. In migrating cells, the cell–cell adhesion protein α-catenin accumulated at the leading edges along with ArpC2/p34 and α-actinin. Suppression of α-catenin shifted cell morphology from fibroblast-like to discoid and attenuated cell migration. Expression of exogenous α-catenin in MDA-MB-468 cells devoid of α-catenin drastically increased their migratory capabilities. The Y654 phosphorylated form of β-catenin was detected at integrin adhesion complexes (IACs). Co-immunoprecipitation studies indicated that α-catenin and pY654-β-catenin were associated with IAC proteins: vinculin, zyxin, and α-actinin. Taken together, these data suggest that in cells undergoing EMT, catenins not participating in assembly of adherens junctions may affect cell migration.
Full article
(This article belongs to the Special Issue Cytoskeletal Remodeling in Health and Disease)
Open AccessEditorial
Mesenchymal Stem Cells and Their Role in Neurodegenerative Diseases
by
Vincenzo Mattei and Simona Delle Monache
Cells 2024, 13(9), 779; https://doi.org/10.3390/cells13090779 - 02 May 2024
Abstract
Mesenchymal stem cells (MSCs) have garnered significant interest in the field of regenerative medicine for their ability to potentially treat various diseases, especially neurodegenerative disorders [...]
[...] Read more.
Mesenchymal stem cells (MSCs) have garnered significant interest in the field of regenerative medicine for their ability to potentially treat various diseases, especially neurodegenerative disorders [...]
Full article
(This article belongs to the Special Issue Mesenchymal Stem Cells and Their Role in Neurodegenerative Diseases)
Open AccessArticle
The Long Non-Coding RNA Gene AC027288.3 Plays a Role in Human Endometrial Stromal Fibroblast Decidualization
by
Rupak Thapa, Kevin Marmo, Liang Ma, Donald S. Torry and Brent M. Bany
Cells 2024, 13(9), 778; https://doi.org/10.3390/cells13090778 - 02 May 2024
Abstract
During the secretory phase of the menstrual cycle, endometrial fibroblast cells begin to change into large epithelial-like cells called decidual cells in a process called decidualization. This differentiation continues more broadly in the endometrium and forms the decidual tissue during early pregnancy. The
[...] Read more.
During the secretory phase of the menstrual cycle, endometrial fibroblast cells begin to change into large epithelial-like cells called decidual cells in a process called decidualization. This differentiation continues more broadly in the endometrium and forms the decidual tissue during early pregnancy. The cells undergoing decidualization as well as the resulting decidual cells, support successful implantation and placentation during early pregnancy. This study was carried out to identify new potentially important long non-coding RNA (lncRNA) genes that may play a role in human endometrial stromal fibroblast cells (hESF) undergoing decidualization in vitro, and several were found. The expression of nine was further characterized. One of these, AC027288.3, showed a dramatic increase in the expression of hESF cells undergoing decidualization. When AC027288.3 expression was targeted, the ability of the cells to undergo decidualization as determined by the expression of decidualization marker protein-coding genes was significantly altered. The most affected markers of decidualization whose expression was significantly reduced were FOXO1, FZD4, and INHBA. Therefore, AC027288.3 may be a major upstream regulator of the WNT-FOXO1 pathway and activin-SMAD3 pathways previously shown as critical for hESF decidualization. Finally, we explored possible regulators of AC027288.3 expression during human ESF decidualization. Expression was regulated by cAMP and progesterone. Our results suggest that AC027288.3 plays a role in hESF decidualization and identifies several other lncRNA genes that may also play a role.
Full article
(This article belongs to the Special Issue Select Topics in Molecular and Cellular Mechanisms of Mammalian Reproduction)
►▼
Show Figures

Figure 1
Open AccessArticle
CD133 Stimulates Cell Proliferation via the Upregulation of Amphiregulin in Melanoma
by
Cynthia M Simbulan-Rosenthal, Nusrat Islam, Yogameenakshi Haribabu, Ryyan Alobaidi, Azadeh Shalamzari, Garrett Graham, Li-Wei Kuo, Peter Sykora and Dean S Rosenthal
Cells 2024, 13(9), 777; https://doi.org/10.3390/cells13090777 - 02 May 2024
Abstract
CD133, a cancer stem cell (CSC) marker in tumors, including melanoma, is associated with tumor recurrence, chemoresistance, and metastasis. Patient-derived melanoma cell lines were transduced with a Tet-on vector expressing CD133, generating doxycycline (Dox)-inducible cell lines. Cells were exposed to Dox for 24
[...] Read more.
CD133, a cancer stem cell (CSC) marker in tumors, including melanoma, is associated with tumor recurrence, chemoresistance, and metastasis. Patient-derived melanoma cell lines were transduced with a Tet-on vector expressing CD133, generating doxycycline (Dox)-inducible cell lines. Cells were exposed to Dox for 24 h to induce CD133 expression, followed by RNA-seq and bioinformatic analyses, revealing genes and pathways that are significantly up- or downregulated by CD133. The most significantly upregulated gene after CD133 was amphiregulin (AREG), validated by qRT-PCR and immunoblot analyses. Induced CD133 expression significantly increased cell growth, percentage of cells in S-phase, BrdU incorporation into nascent DNA, and PCNA levels, indicating that CD133 stimulates cell proliferation. CD133 induction also activated EGFR and the MAPK pathway. Potential mechanisms highlighting the role(s) of CD133 and AREG in melanoma CSC were further delineated using AREG/EGFR inhibitors or siRNA knockdown of AREG mRNA. Treatment with the EGFR inhibitor gefitinib blocked CD133-induced cell growth increase and MAPK pathway activation. Importantly, siRNA knockdown of AREG reversed the stimulatory effects of CD133 on cell growth, indicating that AREG mediates the effects of CD133 on cell proliferation, thus serving as an attractive target for novel combinatorial therapeutics in melanoma and cancers with overexpression of both CD133 and AREG.
Full article
(This article belongs to the Special Issue Melanoma: From Molecular Mechanisms to Therapeutic Opportunities—Series 2)
►▼
Show Figures

Figure 1
Open AccessArticle
Mesenchymal Stem Cell Therapy for Bone Repair of Human Hip Osteonecrosis with Bilateral Match-Control Evaluation: Impact of Tissue Source, Cell Count, Disease Stage, and Volume Size on 908 Hips
by
Philippe Hernigou, Yasuhiro Homma, Jacques Hernigou, Charles Henri Flouzat Lachaniette, Helène Rouard and Sophie Verrier
Cells 2024, 13(9), 776; https://doi.org/10.3390/cells13090776 - 01 May 2024
Abstract
We investigated the impact of mesenchymal stem cell (MSC) therapy on treating bilateral human hip osteonecrosis, analyzing 908 cases. This study assesses factors such as tissue source and cell count, comparing core decompression with various cell therapies. This research emphasizes bone repair according
[...] Read more.
We investigated the impact of mesenchymal stem cell (MSC) therapy on treating bilateral human hip osteonecrosis, analyzing 908 cases. This study assesses factors such as tissue source and cell count, comparing core decompression with various cell therapies. This research emphasizes bone repair according to pre-treatment conditions and the specificities of cell therapy in osteonecrosis repair, indicating a potential for improved bone repair strategies in hips without femoral head collapse. This study utilized a single-center retrospective analysis to investigate the efficacy of cellular approaches in the bone repair of osteonecrosis. It examined the impact on bone repair of tissue source (autologous bone marrow concentrate, allogeneic expanded, autologous expanded), cell quantity (from none in core decompression alone to millions in cell therapy), and osteonecrosis stage and volume. Excluding hips with femoral head collapse, it focused on patients who had bilateral hip osteonecrosis, both pre-operative and post-operative MRIs, and a follow-up of over five years. The analysis divided these patients into seven groups based on match control treatment variations in bilateral hip osteonecrosis, primarily investigating the outcomes between core decompression, washing effect, and different tissue sources of MSCs. Younger patients (<30 years) demonstrated significantly better repair volumes, particularly in stage II lesions, than older counterparts. Additionally, bone repair volume increased with the number of implanted MSCs up to 1,000,000, beyond which no additional benefits were observed. No significant difference was observed in repair outcomes between different sources of MSCs (BMAC, allogenic, or expanded cells). The study also highlighted that a ‘washing effect’ was beneficial, particularly for larger-volume osteonecrosis when combined with core decompression. Partial bone repair was the more frequent event observed, while total bone repair of osteonecrosis was rare. The volume and stage of osteonecrosis, alongside the number of injected cells, significantly affected treatment outcomes. In summary, this study provides comprehensive insights into the effectiveness and variables influencing the use of mesenchymal stem cells in treating human hip osteonecrosis. It emphasizes the potential of cell therapy while acknowledging the complexity and variability of results based on factors such as age, cell count, and disease stage.
Full article
(This article belongs to the Special Issue Stem and Progenitor Cells in Bone Regeneration)
Open AccessArticle
Neuroretinal Cell Culture Model as a Tool for the Development of New Therapeutic Approaches for Oxidative Stress-Induced Ocular Diseases, with a Focus on Glaucoma
by
Kristian Nzogang Fomo, Natarajan Perumal, Caroline Manicam, Norbert Pfeiffer and Franz H. Grus
Cells 2024, 13(9), 775; https://doi.org/10.3390/cells13090775 - 01 May 2024
Abstract
Glaucoma is a heterogeneous group of optic neuropathies characterized by a progressive degeneration of the retinal ganglion cells (RGCs), leading to irreversible vision loss. Nowadays, the traditional therapeutic approach to glaucoma consists of lowering the intraocular pressure (IOP), which does not address the
[...] Read more.
Glaucoma is a heterogeneous group of optic neuropathies characterized by a progressive degeneration of the retinal ganglion cells (RGCs), leading to irreversible vision loss. Nowadays, the traditional therapeutic approach to glaucoma consists of lowering the intraocular pressure (IOP), which does not address the neurodegenerative features of the disease. Besides animal models of glaucoma, there is a considerable need for in vitro experimental models to propose new therapeutic strategies for this ocular disease. In this study, we elucidated the pathological mechanisms leading to neuroretinal R28 cell death after exposure to glutamate and hydrogen peroxide (H2O2) in order to develop new therapeutic approaches for oxidative stress-induced retinal diseases, including glaucoma. We were able to show that glutamate and H2O2 can induce a decrease in R28 cell viability in a concentration-dependent manner. A cell viability of about 42% was found after exposure to 3 mM of glutamate and about 56% after exposure to 100 µM of H2O2 (n = 4). Label-free quantitative mass spectrometry analysis revealed differential alterations of 193 and 311 proteins in R28 cells exposed to 3 mM of glutamate and 100 µM of H2O2, respectively (FDR < 1%; p < 0.05). Bioinformatics analysis indicated that the protein changes were associated with the dysregulation of signaling pathways, which was similar to those observed in glaucoma. Thus, the proteomic alteration induced by glutamate was associated with the inhibition of the PI3K/AKT signaling pathway. On the other hand, H2O2-induced toxicity in R28 cells was linked to the activation of apoptosis signaling and the inhibition of the mTOR and ERK/MAPK signaling pathways. Furthermore, the data show a similarity in the inhibition of the EIF2 and AMPK signaling pathways and the activation of the sumoylation and WNT/β-catenin signaling pathways in both groups. Our findings suggest that the exposure of R28 cells to glutamate and H2O2 could induce glaucoma-like neurodegenerative features and potentially provide a suitable tool for the development of new therapeutic strategies for retinal diseases.
Full article
(This article belongs to the Section Cellular Pathology)
►▼
Show Figures
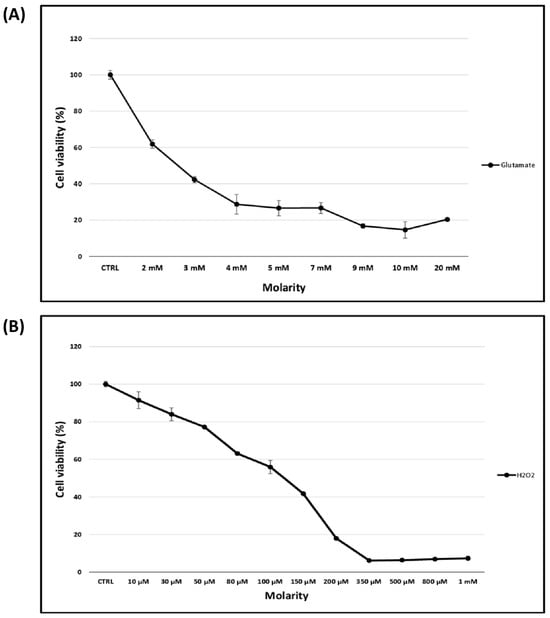
Figure 1
Open AccessArticle
Transcriptomic Signature and Pro-Osteoclastic Secreted Factors of Abnormal Bone-Marrow Stromal Cells in Fibrous Dysplasia
by
Zachary Michel, Layne N. Raborn, Tiahna Spencer, Kristen S. Pan, Daniel Martin, Kelly L. Roszko, Yan Wang, Pamela G. Robey, Michael T. Collins, Alison M. Boyce and Luis Fernandez de Castro
Cells 2024, 13(9), 774; https://doi.org/10.3390/cells13090774 - 30 Apr 2024
Abstract
►▼
Show Figures
Fibrous dysplasia (FD) is a mosaic skeletal disorder caused by somatic activating variants of GNAS encoding for Gαs and leading to excessive cyclic adenosine monophosphate signaling in bone-marrow stromal cells (BMSCs). The effect of Gαs activation in the BMSC transcriptome and
[...] Read more.
Fibrous dysplasia (FD) is a mosaic skeletal disorder caused by somatic activating variants of GNAS encoding for Gαs and leading to excessive cyclic adenosine monophosphate signaling in bone-marrow stromal cells (BMSCs). The effect of Gαs activation in the BMSC transcriptome and how it influences FD lesion microenvironment are unclear. We analyzed changes induced by Gαs activation in the BMSC transcriptome and secretome. RNAseq analysis of differential gene expression of cultured BMSCs from patients with FD and healthy volunteers, and from an inducible mouse model of FD, was performed, and the transcriptomic profiles of both models were combined to build a robust FD BMSC genetic signature. Pathways related to Gαs activation, cytokine signaling, and extracellular matrix deposition were identified. To assess the modulation of several key secreted factors in FD pathogenesis, cytokines and other factors were measured in culture media. Cytokines were also screened in a collection of plasma samples from patients with FD, and positive correlations of several cytokines to their disease burden score, as well as to one another and bone turnover markers, were found. These data support the pro-inflammatory, pro-osteoclastic behavior of FD BMSCs and point to several cytokines and other secreted factors as possible therapeutic targets and/or circulating biomarkers for FD.
Full article
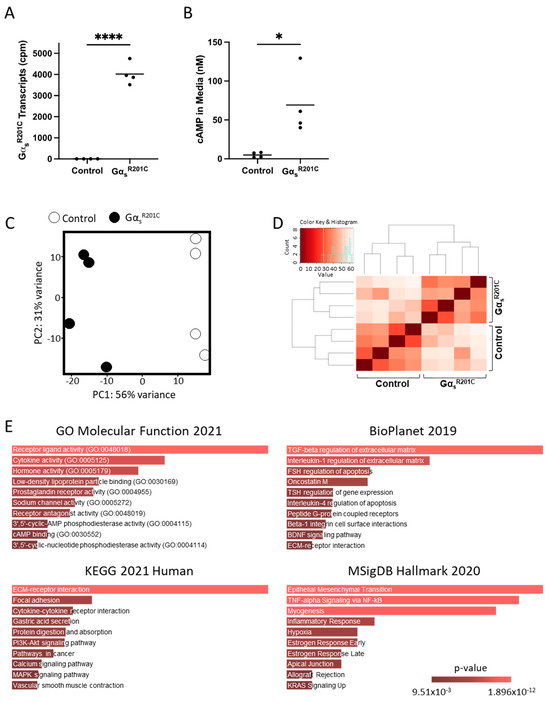
Figure 1
Open AccessArticle
Effects of Chronic Inflammatory Activation of Murine and Human Arterial Endothelial Cells at Normal Lipoprotein and Cholesterol Levels In Vivo and In Vitro
by
Marion Mussbacher, José Basílio, Barbora Belakova, Anita Pirabe, Elisabeth Ableitner, Manuel Campos-Medina and Johannes A. Schmid
Cells 2024, 13(9), 773; https://doi.org/10.3390/cells13090773 - 30 Apr 2024
Abstract
The activation of endothelial cells is crucial for immune defense mechanisms but also plays a role in the development of atherosclerosis. We have previously shown that inflammatory stimulation of endothelial cells on top of elevated lipoprotein/cholesterol levels accelerates atherogenesis. The aim of the
[...] Read more.
The activation of endothelial cells is crucial for immune defense mechanisms but also plays a role in the development of atherosclerosis. We have previously shown that inflammatory stimulation of endothelial cells on top of elevated lipoprotein/cholesterol levels accelerates atherogenesis. The aim of the current study was to investigate how chronic endothelial inflammation changes the aortic transcriptome of mice at normal lipoprotein levels and to compare this to the inflammatory response of isolated endothelial cells in vitro. We applied a mouse model expressing constitutive active IκB kinase 2 (caIKK2)—the key activator of the inflammatory NF-κB pathway—specifically in arterial endothelial cells and analyzed transcriptomic changes in whole aortas, followed by pathway and network analyses. We found an upregulation of cell death and mitochondrial beta-oxidation pathways with a predicted increase in endothelial apoptosis and necrosis and a simultaneous reduction in protein synthesis genes. The highest upregulated gene was ACE2, the SARS-CoV-2 receptor, which is also an important regulator of blood pressure. Analysis of isolated human arterial and venous endothelial cells supported these findings and also revealed a reduction in DNA replication, as well as repair mechanisms, in line with the notion that chronic inflammation contributes to endothelial dysfunction.
Full article
(This article belongs to the Section Cells of the Cardiovascular System)
Open AccessArticle
Globospiramine from Voacanga globosa Exerts Robust Cytotoxic and Antiproliferative Activities on Cancer Cells by Inducing Caspase-Dependent Apoptosis in A549 Cells and Inhibiting MAPK14 (p38α): In Vitro and Computational Investigations
by
Joe Anthony H. Manzano, Elian Angelo Abellanosa, Jose Paolo Aguilar, Simone Brogi, Chia-Hung Yen, Allan Patrick G. Macabeo and Nicanor Austriaco
Cells 2024, 13(9), 772; https://doi.org/10.3390/cells13090772 - 30 Apr 2024
Abstract
Bisindole alkaloids are a source of inspiration for the design and discovery of new-generation anticancer agents. In this study, we investigated the cytotoxic and antiproliferative activities of three spirobisindole alkaloids from the traditional anticancer Philippine medicinal plant Voacanga globosa, along with their
[...] Read more.
Bisindole alkaloids are a source of inspiration for the design and discovery of new-generation anticancer agents. In this study, we investigated the cytotoxic and antiproliferative activities of three spirobisindole alkaloids from the traditional anticancer Philippine medicinal plant Voacanga globosa, along with their mechanisms of action. Thus, the alkaloids globospiramine (1), deoxyvobtusine (2), and vobtusine lactone (3) showed in vitro cytotoxicity and antiproliferative activities against the tested cell lines (L929, KB3.1, A431, MCF-7, A549, PC-3, and SKOV-3) using MTT and CellTiter-Blue assays. Globospiramine (1) was also screened against a panel of breast cancer cell lines using the sulforhodamine B (SRB) assay and showed moderate cytotoxicity. It also promoted the activation of apoptotic effector caspases 3 and 7 using Caspase–Glo 3/7 and CellEvent-3/7 apoptosis assays. Increased expressions of cleaved caspase 3 and PARP in A549 cells treated with 1 were also observed. Apoptotic activity was also confirmed when globospiramine (1) failed to promote the rapid loss of membrane integrity according to the HeLa cell membrane permeability assay. Network pharmacology analysis, molecular docking, and molecular dynamics simulations identified MAPK14 (p38α), a pharmacological target leading to cancer cell apoptosis, as a putative target. Low toxicity risks and favorable drug-likeness were also predicted for 1. Overall, our study demonstrated the anticancer potentials and apoptotic mechanisms of globospiramine (1), validating the traditional medicinal use of Voacanga globosa.
Full article
(This article belongs to the Special Issue Apoptosis in Cancers)
Open AccessArticle
Small-Molecule Inhibitors of TIPE3 Protein Identified through Deep Learning Suppress Cancer Cell Growth In Vitro
by
Xiaodie Chen, Zhen Lu, Jin Xiao, Wei Xia, Yi Pan, Houjun Xia, Youhai H. Chen and Haiping Zhang
Cells 2024, 13(9), 771; https://doi.org/10.3390/cells13090771 - 30 Apr 2024
Abstract
Tumor necrosis factor-α-induced protein 8-like 3 (TNFAIP8L3 or TIPE3) functions as a transfer protein for lipid second messengers. TIPE3 is highly upregulated in several human cancers and has been established to significantly promote tumor cell proliferation, migration, and invasion and inhibit the apoptosis
[...] Read more.
Tumor necrosis factor-α-induced protein 8-like 3 (TNFAIP8L3 or TIPE3) functions as a transfer protein for lipid second messengers. TIPE3 is highly upregulated in several human cancers and has been established to significantly promote tumor cell proliferation, migration, and invasion and inhibit the apoptosis of cancer cells. Thus, inhibiting the function of TIPE3 is expected to be an effective strategy against cancer. The advancement of artificial intelligence (AI)-driven drug development has recently invigorated research in anti-cancer drug development. In this work, we incorporated DFCNN, Autodock Vina docking, DeepBindBC, MD, and metadynamics to efficiently identify inhibitors of TIPE3 from a ZINC compound dataset. Six potential candidates were selected for further experimental study to validate their anti-tumor activity. Among these, three small-molecule compounds (K784-8160, E745-0011, and 7238-1516) showed significant anti-tumor activity in vitro, leading to reduced tumor cell viability, proliferation, and migration and enhanced apoptotic tumor cell death. Notably, E745-0011 and 7238-1516 exhibited selective cytotoxicity toward tumor cells with high TIPE3 expression while having little or no effect on normal human cells or tumor cells with low TIPE3 expression. A molecular docking analysis further supported their interactions with TIPE3, highlighting hydrophobic interactions and their shared interaction residues and offering insights for designing more effective inhibitors. Taken together, this work demonstrates the feasibility of incorporating deep learning and MD simulations in virtual drug screening and provides inhibitors with significant potential for anti-cancer drug development against TIPE3−.
Full article
Open AccessReview
From the Gut to the Brain: Is Microbiota a New Paradigm in Parkinson’s Disease Treatment?
by
Cristiana Vilela, Bruna Araújo, Carla Soares-Guedes, Rita Caridade-Silva, Joana Martins-Macedo, Catarina Teixeira, Eduardo D. Gomes, Cristina Prudêncio, Mónica Vieira and Fábio G. Teixeira
Cells 2024, 13(9), 770; https://doi.org/10.3390/cells13090770 - 30 Apr 2024
Abstract
►▼
Show Figures
Parkinson’s disease (PD) is recognized as the second most prevalent primary chronic neurodegenerative disorder of the central nervous system. Clinically, PD is characterized as a movement disorder, exhibiting an incidence and mortality rate that is increasing faster than any other neurological condition. In
[...] Read more.
Parkinson’s disease (PD) is recognized as the second most prevalent primary chronic neurodegenerative disorder of the central nervous system. Clinically, PD is characterized as a movement disorder, exhibiting an incidence and mortality rate that is increasing faster than any other neurological condition. In recent years, there has been a growing interest concerning the role of the gut microbiota in the etiology and pathophysiology of PD. The establishment of a brain–gut microbiota axis is now real, with evidence denoting a bidirectional communication between the brain and the gut microbiota through metabolic, immune, neuronal, and endocrine mechanisms and pathways. Among these, the vagus nerve represents the most direct form of communication between the brain and the gut. Given the potential interactions between bacteria and drugs, it has been observed that the therapies for PD can have an impact on the composition of the microbiota. Therefore, in the scope of the present review, we will discuss the current understanding of gut microbiota on PD and whether this may be a new paradigm for treating this devastating disease.
Full article
Figure 1
Open AccessArticle
Thapsigargin and Tunicamycin Block SARS-CoV-2 Entry into Host Cells via Differential Modulation of Unfolded Protein Response (UPR), AKT Signaling, and Apoptosis
by
Abeer Al Otaibi, Sindiyan Al Shaikh Mubarak, Fatimah Al Hejji, Abdulrahman Almasaud, Haya Al Jami, Jahangir Iqbal, Ali Al Qarni, Naif Khalaf Al Harbi and Ahmed Bakillah
Cells 2024, 13(9), 769; https://doi.org/10.3390/cells13090769 - 30 Apr 2024
Abstract
Background: SARS-Co-V2 infection can induce ER stress-associated activation of unfolded protein response (UPR) in host cells, which may contribute to the pathogenesis of COVID-19. To understand the complex interplay between SARS-Co-V2 infection and UPR signaling, we examined the effects of acute pre-existing ER
[...] Read more.
Background: SARS-Co-V2 infection can induce ER stress-associated activation of unfolded protein response (UPR) in host cells, which may contribute to the pathogenesis of COVID-19. To understand the complex interplay between SARS-Co-V2 infection and UPR signaling, we examined the effects of acute pre-existing ER stress on SARS-Co-V2 infectivity. Methods: Huh-7 cells were treated with Tunicamycin (TUN) and Thapsigargin (THA) prior to SARS-CoV-2pp transduction (48h p.i.) to induce ER stress. Pseudo-typed particles (SARS-CoV-2pp) entry into host cells was measured by Bright GloTM luciferase assay. Cell viability was assessed by cell titer Glo® luminescent assay. The mRNA and protein expression was evaluated by RT-qPCR and Western Blot. Results: TUN (5 µg/ml) and THA (1 µM) efficiently inhibited the entry of SARS-CoV-2pp into host cells without any cytotoxic effect. TUN and THA's attenuation of virus entry was associated with differential modulation of ACE2 expression. Both TUN and THA significantly reduced the expression of stress-inducible ER chaperone GRP78/BiP in transduced cells. In contrast, the IRE1-XBP1s and PERK-eIF2α-ATF4-CHOP signaling pathways were downregulated with THA treatment, but not TUN in transduced cells. Insulin-mediated glucose uptake and phosphorylation of Ser307 IRS-1 and downstream p-AKT were enhanced with THA in transduced cells. Furthermore, TUN and THA differentially affected lipid metabolism and apoptotic signaling pathways. Conclusions: These findings suggest that short-term pre-existing ER stress prior to virus infection induces a specific UPR response in host cells capable of counteracting stress-inducible elements signaling, thereby depriving SARS-Co-V2 of essential components for entry and replication. Pharmacological manipulation of ER stress in host cells might provide new therapeutic strategies to alleviate SARS-CoV-2 infection.
Full article
Open AccessReview
Important Factors Affecting Induction of Cell Death, Oxidative Stress and DNA Damage by Nano- and Microplastic Particles In Vitro
by
Kamil Płuciennik, Paulina Sicińska, Weronika Misztal and Bożena Bukowska
Cells 2024, 13(9), 768; https://doi.org/10.3390/cells13090768 - 30 Apr 2024
Abstract
►▼
Show Figures
We have described the influence of selected factors that increase the toxicity of nanoplastics (NPs) and microplastics (MPs) with regard to cell viability, various types of cell death, reactive oxygen species (ROS) induction, and genotoxicity. These factors include plastic particle size (NPs/MPs), zeta
[...] Read more.
We have described the influence of selected factors that increase the toxicity of nanoplastics (NPs) and microplastics (MPs) with regard to cell viability, various types of cell death, reactive oxygen species (ROS) induction, and genotoxicity. These factors include plastic particle size (NPs/MPs), zeta potential, exposure time, concentration, functionalization, and the influence of environmental factors and cell type. Studies have unequivocally shown that smaller plastic particles are more cytotoxic, penetrate cells more easily, increase ROS formation, and induce oxidative damage to proteins, lipids, and DNA. The toxic effects also increase with concentration and incubation time. NPs with positive zeta potential are also more toxic than those with a negative zeta potential because the cells are negatively charged, inducing stronger interactions. The deleterious effects of NPs and MPs are increased by functionalization with anionic or carboxyl groups, due to greater interaction with cell membrane components. Cationic NPs/MPs are particularly toxic due to their greater cellular uptake and/or their effects on cells and lysosomal membranes. The effects of polystyrene (PS) vary from one cell type to another, and normal cells are more sensitive to NPs than cancerous ones. The toxicity of NPs/MPs can be enhanced by environmental factors, including UV radiation, as they cause the particles to shrink and change their shape, which is a particularly important consideration when working with environmentally-changed NPs/MPs. In summary, the cytotoxicity, oxidative properties, and genotoxicity of plastic particles depends on their concentration, duration of action, and cell type. Also, NPs/MPs with a smaller diameter and positive zeta potential, and those exposed to UV and functionalized with amino groups, demonstrate higher toxicity than larger, non-functionalized and environmentally-unchanged particles with a negative zeta potential.
Full article
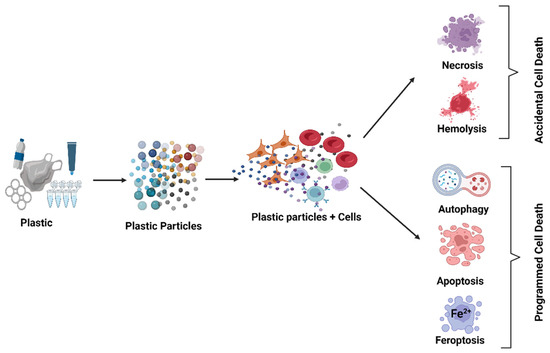
Figure 1
Open AccessArticle
Cholesterol-Modified Anti-Il6 siRNA Reduces the Severity of Acute Lung Injury in Mice
by
Ivan V. Chernikov, Irina K. Bachkova, Aleksandra V. Sen’kova, Mariya I. Meschaninova, Innokenty A. Savin, Valentin V. Vlassov, Marina A. Zenkova and Elena L. Chernolovskaya
Cells 2024, 13(9), 767; https://doi.org/10.3390/cells13090767 - 30 Apr 2024
Abstract
Small interfering RNA (siRNA) holds significant therapeutic potential by silencing target genes through RNA interference. Current clinical applications of siRNA have been primarily limited to liver diseases, while achievements in delivery methods are expanding their applications to various organs, including the lungs. Cholesterol-conjugated
[...] Read more.
Small interfering RNA (siRNA) holds significant therapeutic potential by silencing target genes through RNA interference. Current clinical applications of siRNA have been primarily limited to liver diseases, while achievements in delivery methods are expanding their applications to various organs, including the lungs. Cholesterol-conjugated siRNA emerges as a promising delivery approach due to its low toxicity and high efficiency. This study focuses on developing a cholesterol-conjugated anti-Il6 siRNA and the evaluation of its potency for the potential treatment of inflammatory diseases using the example of acute lung injury (ALI). The biological activities of different Il6-targeted siRNAs containing chemical modifications were evaluated in J774 cells in vitro. The lead cholesterol-conjugated anti-Il6 siRNA after intranasal instillation demonstrated dose-dependent therapeutic effects in a mouse model of ALI induced by lipopolysaccharide (LPS). The treatment significantly reduced Il6 mRNA levels, inflammatory cell infiltration, and the severity of lung inflammation. IL6 silencing by cholesterol-conjugated siRNA proves to be a promising strategy for treating inflammatory diseases, with potential applications beyond the lungs.
Full article
(This article belongs to the Special Issue RNA in Focus)
►▼
Show Figures
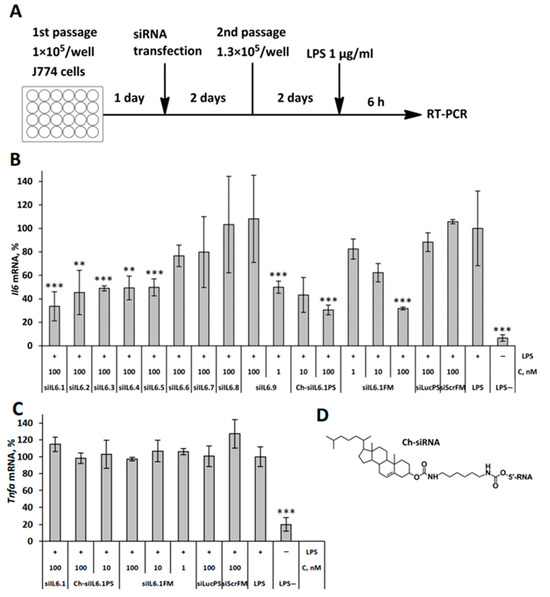
Figure 1

Journal Menu
► ▼ Journal Menu-
- Cells Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomedicines, Cells, IJMS, Life, Oxygen
Oxidative Stress and Inflammation, 2nd Volume
Topic Editors: Mohamad Allaw, Ines Castangia, Maria Letizia Manca, Matteo Perra, Amparo NacherDeadline: 31 May 2024
Topic in
Cancers, Cells, JCM, Radiation, Pharmaceutics, Applied Sciences, Nanomaterials, Current Oncology
Innovative Radiation Therapies
Topic Editors: Gérard Baldacchino, Eric Deutsch, Marie Dutreix, Sandrine Lacombe, Erika Porcel, Charlotte Robert, Emmanuelle Bourneuf, João Santos Sousa, Aurélien de la LandeDeadline: 30 June 2024
Topic in
Cells, Diseases, Healthcare, IJMS, Vaccines
Inflammation: The Cause of all Diseases 2.0
Topic Editors: Vasso Apostolopoulos, Jack Feehan, Vivek P. ChavdaDeadline: 31 July 2024
Topic in
Applied Sciences, Cancers, Cells, Electronics, AI
Explainable AI for Health
Topic Editors: Yudong Zhang, Juan Manuel Gorriz, Zhengchao DongDeadline: 8 August 2024

Conferences
Special Issues
Special Issue in
Cells
Molecular Insights: Bridging the Gap between Aging, Neurodegenerative Disease, and Cancer from Bench to Bedside
Guest Editor: Maurizio RomanoDeadline: 10 May 2024
Special Issue in
Cells
Microglia in Neurological Diseases
Guest Editors: Kate Lykke Lambertsen, Bente FinsenDeadline: 15 May 2024
Special Issue in
Cells
Cellular Reprogramming during Sepsis and Potential Therapeutic Targets
Guest Editor: Brendon SciclunaDeadline: 31 May 2024
Special Issue in
Cells
Reprogrammed Cells in Disease Modeling and Drug Discovery II
Guest Editor: Xuefeng LiuDeadline: 20 June 2024
Topical Collections
Topical Collection in
Cells
Role of Autophagy in Viral Infection
Collection Editor: Grant R. Campbell
Topical Collection in
Cells
Tumor Metabolism and Therapy
Collection Editors: Guohui Sun, Jianhua Wang
Topical Collection in
Cells
Molecular signaling, Circuit Neuroplasticity and the Cognitive Function
Collection Editor: Francisco Monje