Shear Bond Strength and Film Thickness of a Naturally Antimicrobial Modified Dental Luting Cement
Abstract
:1. Introduction
2. Results and Discussion
2.1. Results
2.1.1. Shear Bond Strength
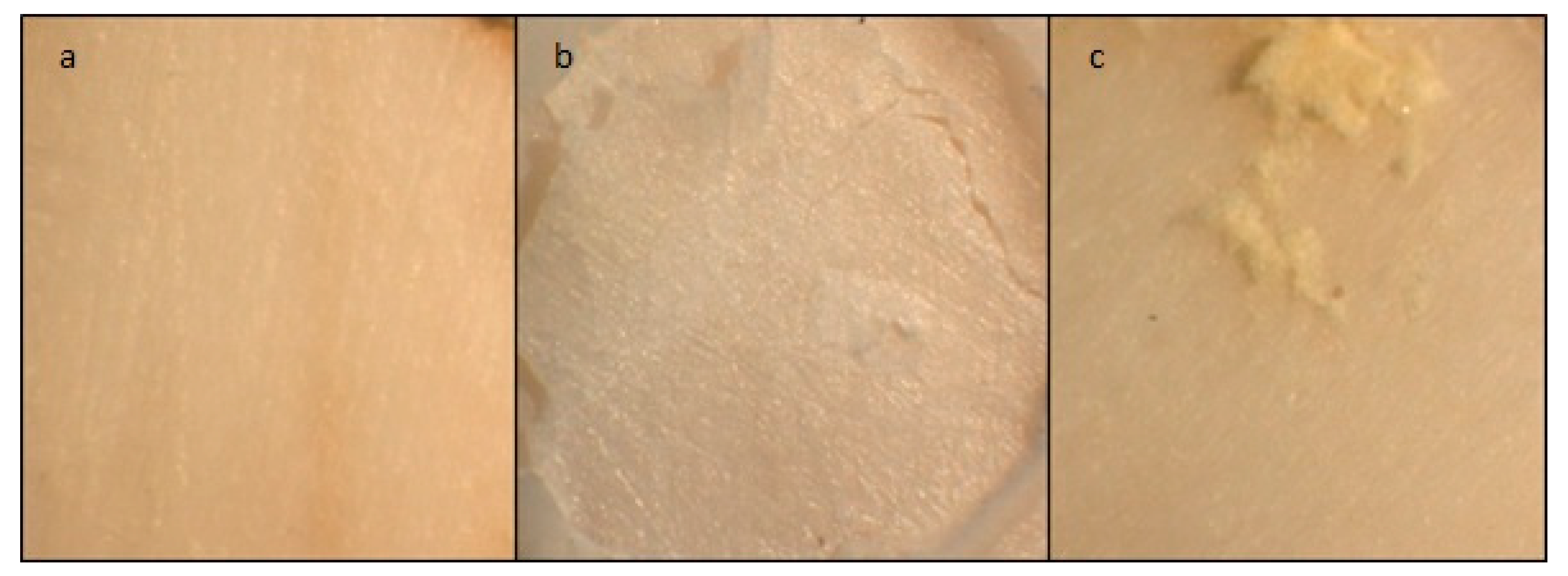
Failure Mode
2.1.2. Film Thickness
2.2. Discussion
2.2.1. Shear Bond Strength
Failure Mode
2.2.2. Film Thickness
3. Materials and Methods
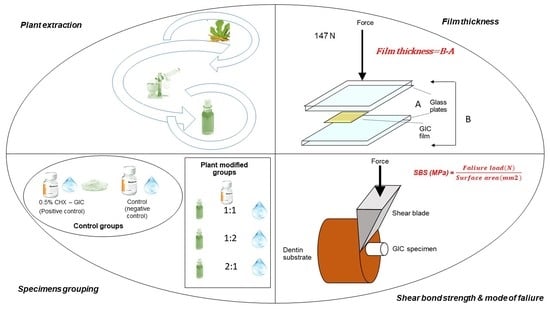
3.1. Plants Extraction and GIC Modification
3.1.1. Plant Extraction
3.1.2. Modification, Preparation and Specimens Grouping of GIC
- Negative control: prepared by mixing the powder of GIC with the exact amount of distilled water as per the manufacturer’s instructions (1:2), without any modification.
- Positive control: prepared by adding 0.5% CHX diacetate powder (w/w) (Merck KGaA, Darmstadt, Germany) to GIC powder (CHX-GIC) to be mixed with distilled water (1:2).
- Control: (unmodified GIC).
- CHX-GIC: (0.5% CHX modified GIC).
- Extract- mixture modified groups:
- 1:2 (extract: water).
- 1:1 (extract: water).
- 2:1 (extract: water).
3.2. Shear Bond Strength
Failure Mode Analysis
3.3. Film Thickness
3.4. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- McLean, J.W.; Nicholson, J.W.; Wilson, A.D. Guest Editorial: Proposed nomenclature for glass-ionomer dental cements and related materials. Quintessence Int. 1994, 25, 587–589. [Google Scholar] [PubMed]
- Lohbauer, U. Dental glass ionomer cements as permanent filling materials? Properties, limitations and future trends. Materials 2010, 3, 76. [Google Scholar] [CrossRef]
- Lad, P.P.; Kamath, M.; Tarale, K.; Kusugal, P.B. Practical clinical considerations of luting cements: A review. J. Int. Oral Health 2014, 6, 116–120. [Google Scholar]
- Sidhu, S.K.; Nicholson, J.W. A review of glass-Ionomer cements for clinical dentistry. J. Funct. Biomater. 2016, 7, 16. [Google Scholar] [CrossRef] [PubMed]
- Rosenstiel, S.F.; Land, M.F.; Crispin, B.J. Dental luting agents: A review of the current literature. J. Prosthet. Dent. 1998, 80, 280–301. [Google Scholar] [CrossRef]
- Frencken, J.E. The ART approach using glass-ionomers in relation to global oral health care. Dent. Mater. 2010, 26, 1–6. [Google Scholar] [CrossRef]
- Weintraub, J.A. The effectiveness of pit and fissure sealants. J. Public Health Dent. 1989, 49, 317–330. [Google Scholar] [CrossRef]
- Mickenautsch, S.; Mount, G.J.; Yengopal, V. Therapeutic effect of glass ionomers: An overview of evidence. Aust. Dent. J. 2011, 56, 10–15. [Google Scholar] [CrossRef]
- Yengopal, V.; Mickenauisch, S.; Bezerra, A.C.; Leal, S.C. Caries-preventive effect of glass ionomer and resin-based fissure sealants on permanent teeth: A metanalysis. J. Oral Sci. 2009, 51, 373–382. [Google Scholar] [CrossRef] [Green Version]
- Forss, H. Release of fluoride and other elements from light-cured glass ionomers in neutral and acidic conditions. J. Dent. Res. 1993, 72, 1257–1262. [Google Scholar] [CrossRef]
- Manuja, N.; Pandit, I.K.; Srivastava, N.; Gugnani, N.; Nagpal, R. Comparative evaluation of shear bond strength of various esthetic restorative materials to dentin: An in vitro study. J. Indian Soc. Pedod. Prev. Dent. 2011, 29, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Suresh, K.S.; Nagarathna, J. Evaluation of shear bond strengths of FUJI II and FUJI IX with and without salivary contamination on deciduous molars- an in vitro study. AOSR 2011, 1, 139–145. [Google Scholar]
- Somani, R.; Jaidka, S.; Singh, D.J.; Sibal, G.K. Comparative evaluation of shear bond strength of various glass ionomer cements to dentin of primary teeth: An in vitro Study. Int. J. Clin. Pediatr. Dent. 2016, 9, 192–196. [Google Scholar] [CrossRef] [PubMed]
- Khajuria, R.R.; Singh, R.; Barua, P.; Hajira, N.; Gupta, N.; Thakkar, R. Comparison of film thickness of two commercial brands of glass. ionomer cement and one dual-cured composite: An in vitro study. J. Contemp. Dent. Pract. 2017, 18, 670–674. [Google Scholar] [CrossRef]
- Brackett, W.W.; Vickery, J.M. The influence of mixing temperature and powder/liquid ratio on the film thickness of three glass-ionomer cements. Int. J. Prosthodont. 1994, 7, 13–16. [Google Scholar]
- Ekor, M. The growing use of herbal medicines: Issues relating to adverse reactions and challenges in monitoring safety. Front. Pharmacol. 2014, 4, 177. [Google Scholar] [CrossRef] [Green Version]
- Chatterjee, S. Phytomedicines in Dentistry. IOSR J. Pharm. 2014, 4, 1–3. [Google Scholar]
- Cruz Martínez, C.; Diaz Gómez, M.; Oh, M.S. Use of traditional herbal medicine as an alternative in dental treatment in Mexican dentistry: A review. Pharm. Biol. 2017, 55, 1992–1998. [Google Scholar] [CrossRef] [Green Version]
- Kabil, N.S.; Badran, A.S.; Wassel, M.O. Effect of the addition of chlorhexidine and miswak extract on the clinical performance and antibacterial properties of conventional glass ionomer: An in vivo study. Int. J. Paediatr. Dent. 2017, 27, 380–387. [Google Scholar] [CrossRef] [PubMed]
- Hattab, F.N. Meswak: The natural toothbrush. J. Clin. Dent. 1997, 8, 125–129. [Google Scholar]
- Naseem, S.; Hashmi, K.; Fasih, F.; Sharafat, S.; Khanani, R. In vitro evaluation of antimicrobial effect of miswak against common oral pathogens. Pak. J. Med. Sci. 2014, 30, 398–403. [Google Scholar] [CrossRef]
- Canal, J.R.; Torres, M.D.; Romero, A.; Pérez, C. A chloroform extract obtained from a decoction of Ficus carica leaves improves the cholesterolaemic status of rats with streptozotocin-induced diabetes. Acta Physiol. Hung. 2000, 87, 71–76. [Google Scholar] [CrossRef] [PubMed]
- Azreg Aref, H.; Gaaliche, B.; Fekih, A.; Mars, M.; Aouni, M.; Pierre Chaumon, J.; Said, K. In vitro cytotoxic and antiviral activities of Ficus carica latex extracts. Nat. Prod. Res. 2011, 25, 310–319. [Google Scholar] [CrossRef]
- Taamalli, A.; Arráez-Román, D.; Zarrouk, M.; Valverde, J.; Segura-Carretero, A.; Fernández-Gutiérrez, A. The occurrence and bioactivity of polyphenols in Tunisian olive products and by-products: A review. J. Food Sci. 2012, 77, 83–92. [Google Scholar] [CrossRef]
- Oni, M.G.; Burdock, G.A.; Christian, M.S.; Bitler, C.M.; Crea, R. Safety assessment of aqueous olive pulp extract as an antioxidant or antimicrobial agent in foods. Food Chem. Toxicol. 2006, 44, 903–915. [Google Scholar] [CrossRef]
- Hook, E.R.; Owen, O.J.; Bellis, C.A.; Holder, J.A.; O’Sullivan, D.J.; Barbour, M.E. Development of a novel antimicrobial-releasing glass ionomer cement functionalized with chlorhexidine hexametaphosphate nanoparticles. J. Nanobiotechnol. 2014, 12, 3. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yengopal, V.; Harneker, S.Y.; Patel, N.; Siegfried, N. Dental fillings for the treatment of caries in the primary dentition. Cochrane Database Syst Rev. 2009, 15. [Google Scholar] [CrossRef]
- Singer, L.; Bierbaum, G.; Kehl, K.; Bourauel, C. Evaluation of the antimicrobial activity and compressive strength of a dental cement modified using plant extract mixture. J. Mater. Sci. Mater. Med. 2020, 31, 116. [Google Scholar] [CrossRef]
- Deepalakshmi, M.; Poorni, S.; Miglani, R.; Rajamani, I.; Ramachandran, S. Evaluation of the antibacterial and physical properties of glass ionomer cements containing chlorhexidine and cetrimide: An in-vitro study. Indian J. Dent. Res. 2010, 21, 552–556. [Google Scholar] [CrossRef]
- Hosida, T.Y.; Delbem, A.C.B.; Morais, L.A.; Moraes, J.C.S.; Duque, C.; Souza, J.A.S.; Pedrini, D. Ion release, antimicrobial and physio-mechanical properties of glass ionomer cement containing micro or nanosized hexametaphosphate, and their effect on enamel demineralization. Clin. Oral Investig. 2019, 23, 2345–2354. [Google Scholar] [CrossRef] [PubMed]
- Alhalawani, A.M.; Curran, D.J.; Boyd, D.; Towler, M.R. The role of poly (acrylic acid) in conventional glass polyalkenoate cements. J. Polym. Eng. 2016, 36, 221–237. [Google Scholar] [CrossRef] [Green Version]
- Mount, G.J.; Ngo, H.G.; Peters, M.C.R.B. A study of glass-ionomer cement and its interface with enamel and dentin using a low-temperature, high-resolution scanning electron microscopic technique. Quintessence Int. 1997, 28, 63–69. [Google Scholar]
- Ngo, H.C.; Mount, G.; McIntyre, J.; Tuisuva, J.; Von Doussa, R.J. Chemical exchange between glass-ionomer restorations nd residual carious dentine in permanent molars: An in vivo study. J. Dent. 2006, 34, 608–613. [Google Scholar] [CrossRef] [PubMed]
- Poitevin, A.; De Munck, J.; Cardoso, M.V.; Mine, A.; Peumans, M.; Lambrechts, P.; Van Meerbeek, B. Dynamic versus static bond-strength testing of adhesive interfaces. Dent. Mater. 2010, 26, 1068–1076. [Google Scholar] [CrossRef] [PubMed]
- Cattani-Lorente, M.A.; Godin, C.; Meyer, J.M. Early strength of glass ionomer cements. Dent. Mater. 1993, 9, 57–62. [Google Scholar] [CrossRef]
- Swift, E.J., Jr.; Perdigão, J.; Heymann, H.O. Bonding to enamel and dentin: A brief history and state of the art. Quintessence Int. 1995, 26, 95–110. [Google Scholar] [PubMed]
- Cantekin, K.; Avci, S. Evaluation of shear bond strength of two resin-based composites and glass ionomer cement to pure tricalcium silicate-based cement (Biodentine®). J. Appl. Oral Sci. 2014, 22, 302–306. [Google Scholar] [CrossRef] [Green Version]
- Powis, D.R.; Follerås, T.; Merson, S.A.; Wilson, A.D. Improved adhesion of a glass ionomer cement to dentin and enamel. J. Dent. Res. 1982, 61, 1416–1422. [Google Scholar] [CrossRef]
- de Oliveira, B.A.C.; Marti., L.M.; Zuanon, A.C.C.; Brighenti, F.L.; Spolidório, D.M.P.; Giro, E.M.A. Influence of the addition of chlorhexidine diacetate on bond strength of a high-viscosity glass ionomer cement to sound and artificial caries-affected dentin. Rev. Odontol. 2014, 43, 1–7. [Google Scholar] [CrossRef]
- Jaidka, S.; Somani, R.; Singh, D.J.; Shafat, S. Comparative evaluation of compressive strength, diametral tensile strength and shear bond strength of GIC type IX, chlorhexidine-incorporated GIC and triclosan-incorporated GIC: An in vitro study. J. Int. Soc. Prev. Community Dent. 2016, 1, 64–69. [Google Scholar] [CrossRef] [Green Version]
- Prentice, L.; Tyas, M.; Burrow, M. The effect of oxalic acid incorporation on the setting time and strength of a glass-ionomer cement. Acta Biomater. 2006, 2, 109–112. [Google Scholar] [CrossRef]
- Nujella, B.P.; Choudary, M.T.; Reddy, S.P.; Kumar, M.K.; Gopal, T. Comparison of shear bond strength of aesthetic restorative materials. Contemp. Clin. Dent. 2012, 3, 22–26. [Google Scholar] [CrossRef]
- Choi, K.; Oshida, Y.; Platt, J.; Cochran, M.; Matis, B.; Yi, K. Microtensile bond strength of glass ionomer cements to artificially created carious dentin. Oper. Dent. 2006, 31, 590–597. [Google Scholar] [CrossRef] [PubMed]
- Lucas, M.; Arita, K.; Nishino, M. Toughness, bonding and fluoride release properties of hydroxyapatite-added glass ionomer cement. Biomaterials 2003, 24, 3787–3794. [Google Scholar] [CrossRef]
- Palma-Dibb, R.G.; de Castro, C.G.; Ramos, R.P.; Chimello, D.T.; Chinelatti, M.A. Bond strength of glass-ionomer cements to carious-affected dentin. J. Adhes Dent. 2003, 51, 57–62. [Google Scholar]
- Carvalho, T.S.; van Amerongen, W.E.; de Gee, A.; Bönecker, M.; Sampaio, F.C. Shear bond strengths of three glass ionomer cements to enamel and dentine. Med. Oral Patol. Oral Circ. Bucal. 2011, 16, 406–410. [Google Scholar] [CrossRef]
- Almuammar, M.F.; Schulman, A.; Salama, F.S. Shear bond strength of six restorative materials. J. Clin. Pediatr. Dent. 2001, 25, 221–225. [Google Scholar] [CrossRef]
- Tanumiharja, M.; Burrow, M.F.; Tyas, M.J. Microtensile bond strengths of glass ionomer (polyalkenoate) cements to dentine using four conditioners. J. Dent. 2000, 28, 361–366. [Google Scholar] [CrossRef]
- El Wakeel, A.M.; Elkassas, D.W.; Yousry, M.M. Bonding of contem-porary glass ionomer cements to different tooth substrates; microshear bond strength and scanning electron microscope study. Eur. J. Dent. 2015, 9, 176–182. [Google Scholar]
- Berg, J.H. Glass ionomer cements. Pediatr. Dent. 2002, 24, 430–438. [Google Scholar]
- Bhandari, S.; Aras, M.; Chitre, V. An In Vitro Evaluation of the Microleakage under Complete Metal Crowns Using Three Adhesive Luting Cements. J. Indian Prosthodont. Soc. 2012, 12, 65–71. [Google Scholar] [CrossRef]
- Tan, K.; Ibbetson, R. The effect of cement volume on crown seating. Int. J. Prosthodont. 1996, 9, 445–451. [Google Scholar] [PubMed]
- International Organization for Standardization. ISO 9917-2:2017–Dentistry—Water Based Cements. Part 2: Resin-Modified Cements; ISO: Geneva, Switzerland, 2017. [Google Scholar]
- Sulaiman, T.A.; Abdulmajeed, A.A.; Altitinch, I.A.; Ahmed, S.N.; Donovan, T.E. Physical properties, film thickness, and bond strengths of resin-modified glass ionomer cements according to their delivery method. J. Prosthodont. 2019, 28, 85–90. [Google Scholar] [CrossRef] [Green Version]
- Kious, A.R.; Roberts, H.W.; Brackett, W.W. Film thicknesses of recently introduced luting cements. J. Prosthet. Dent. 2009, 101, 189–192. [Google Scholar] [CrossRef]
- Osman, S.A.; McCabe, J.F.; Walls, A.W. Film thickness and rheological properties of luting agents for crown cementation. Eur. J. Prosthodont. Restor. Dent. 2006, 14, 23–27. [Google Scholar]
- Cefaly, D.F.G.; Franco, E.B.; Mondelli, R.F.L.; Francisconi, P.A.S.; Navarro, M.F.D.L. Diametral tensile strength and water sorption of glass-ionomer cements used in Atraumatic Restorative Treatment. J. Appl. Oral Sci. 2003, 11, 96–101. [Google Scholar] [CrossRef] [Green Version]
- El-Tatari, A.; de Soet, J.; de Gee, J.; Shelib, A.; van Amerongen, E. Influence of salvadora persica (miswak) extract on physical and antimicrobial properties of glass ionomer cement. Eur. Arch. Paediatr. Dent. 2011, 12, 22–25. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bhattacharya, P.; Naidu, J.; Tambakad, P.B. Comparative evaluation of shear bond strength and flexural strength of new zirconia reinforced glass ionomer cement with commonly used glass ionomer cements used in atraumatic restorative treatment: An In Vitro Study. J. Dent. Endod. 2018, 3, 83–91. [Google Scholar] [CrossRef]
- Pisaneschi, E.; Carvalho, R.C.R.D.; Matson, E. Shear bond strength of glass-ionomer cements to dentin: Effects of dentin depth and type of material activation. Rev Odontol Univ São Paulo. 1997, 11. [Google Scholar] [CrossRef]
- Deepa, V.L.; Dhamaraju, B.; Bollu, I.P.; Balaji, T.S. Shear bond strength evaluation of resin composite bonded to three different liners: TheraCal LC, Biodentine, and resin-modified glass ionomer cement using universal adhesive: An in vitro study. J. Conserv. Dent. 2016, 19, 166–170. [Google Scholar] [CrossRef]
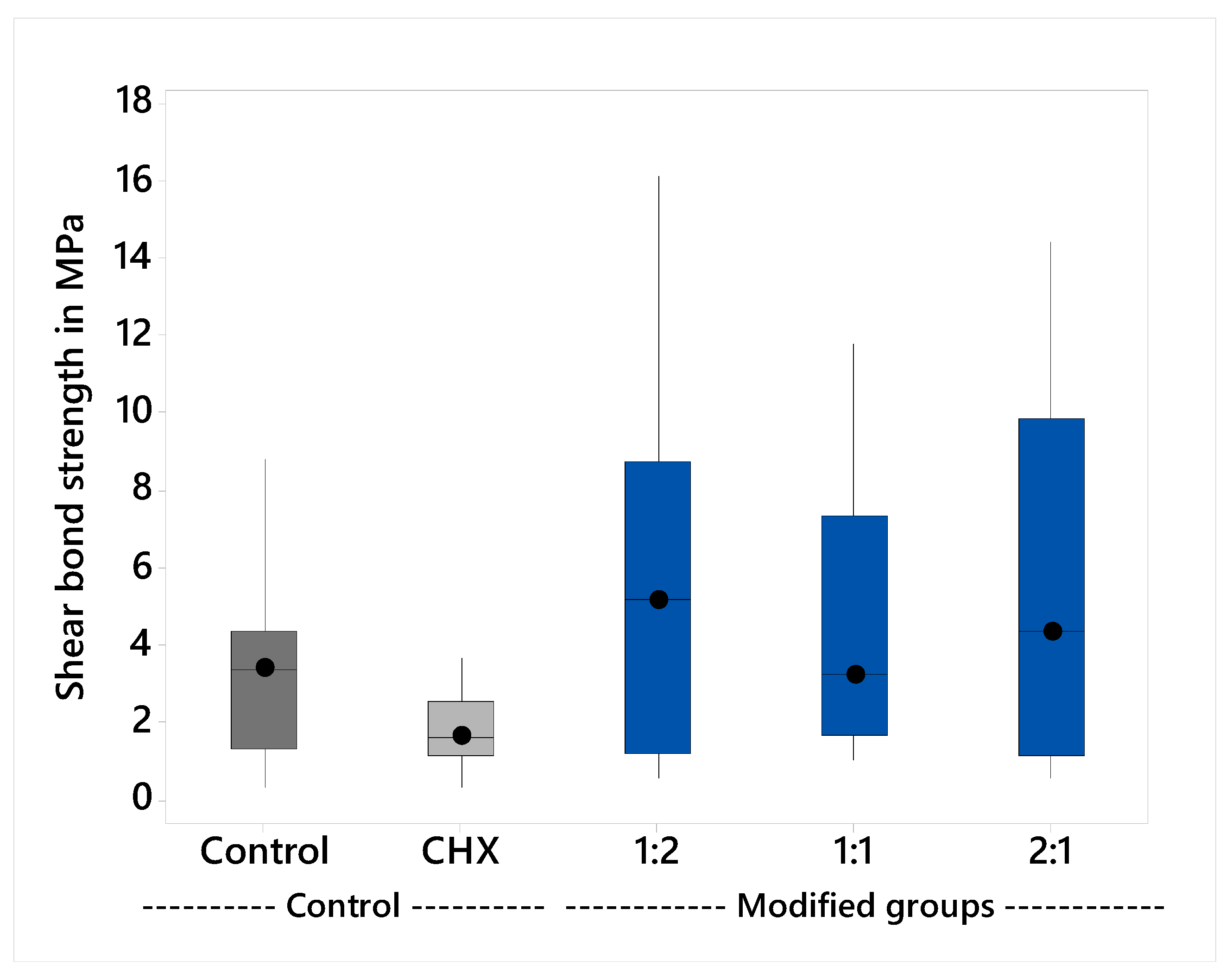





| Groups | n | Median (MPa) | Interquartile Range | p * | Pairwise Comparison ** | |
|---|---|---|---|---|---|---|
| Control | 20 | 3.4 | 3.0 | 0.046 | A | B |
| CHX | 18 | 1.7 | 1.4 | A | ||
| 1:2 | 21 | 5.1 | 7.5 | B | ||
| 1:1 | 20 | 3.2 | 5.6 | B | ||
| 2:1 | 18 | 4.3 | 8.7 | B | ||
| Failure Mode | Control | CHX | 1:2 | 1:1 | 2:1 |
|---|---|---|---|---|---|
| Adhesive % | 10 | 15 | 14 | 21 | 0 |
| Cohesive % | 50 | 38 | 57 | 36 | 40 |
| Mixed % | 40 | 46 | 29 | 43 | 60 |
| Groups | n | Median (μm) | Interquartile Range | p * | Pairwise Comparison ** | |
|---|---|---|---|---|---|---|
| Control | 10 | 20 | 2.8 | <0.001 | A | |
| CHX | 10 | 20 | 4.0 | A | ||
| 1:2 | 10 | 22 | 3.0 | A | ||
| 1:1 | 10 | 22 | 1.8 | A | B | |
| 2:1 | 10 | 24 | 1.3 | B | ||
Sample Availability: Samples of the compounds are not available from the authors. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Singer, L.; Bourauel, C.P. Shear Bond Strength and Film Thickness of a Naturally Antimicrobial Modified Dental Luting Cement. Molecules 2021, 26, 1276. https://doi.org/10.3390/molecules26051276
Singer L, Bourauel CP. Shear Bond Strength and Film Thickness of a Naturally Antimicrobial Modified Dental Luting Cement. Molecules. 2021; 26(5):1276. https://doi.org/10.3390/molecules26051276
Chicago/Turabian StyleSinger, Lamia, and Christoph P. Bourauel. 2021. "Shear Bond Strength and Film Thickness of a Naturally Antimicrobial Modified Dental Luting Cement" Molecules 26, no. 5: 1276. https://doi.org/10.3390/molecules26051276