Abstract
In the present scenario, the research is now being focused on the naturally occurring polymers that can gradually replace the existing synthetic polymers for the development of bio composites having applications in medical surgeries and human implants. With promising mechanical properties and bio compatibility with human tissues, poly lactic acid (PLA) is now being viewed as a future bio material. In order to examine the applicability of PLA in human implants, the current article sheds light on the synthesis of PLA and its various copolymers used to alter its physical and mechanical properties. In the latter half, various processes used for the fabrication of biomaterials are discussed in detail. Finally, biomaterials that are currently in use in the field of biomedical (Scaffolding, drug delivery, tissue engineering, medical implants, derma, cosmetics, medical surgeries, and human implants) are represented with respective advantages in the sphere of biomaterials.
1. Introduction
Poly lactic acid (PLA) is a thermoplastic polymer derived from various natural resources such as corn starch, sugarcane, biomass, and other vegetable wastes by the process of fermentation. It was first discovered in the 1920s by Wallace Carothers and commercialized in the 1990s at a larger scale owing to its better physical, mechanical, and thermal characteristics. Today, it has made a decent place in various food processing, textile, agriculture, and cosmetic sectors [1,2,3]. Apart from these sectors, its presence can also be felt in mechanically driven plastic equipment used on daily basis. The scope of PLA further widens due to its biodegradable nature particularly, in the field of medicine and in instruments and surgery [4,5]. The medical devices made of PLA are increasing rapidly in numbers due to their desired physical and mechanical properties and will hopefully rise in near future. The most important role which is currently being played by PLA is in medical surgeries and is also the topic of discussion in the present articles. Due to many unfortunate reasons, medical surgeries are performed. These medical surgeries require pre-surgery medications and implant material or devices [6,7]. Due to its desirable characteristics such as compatibility with human tissues, biodegradability, stiffness, non-toxicity, durability, and ease to resorb, PLA is now being considered one of the best-suited biomaterials. However, its applications are restrained due to its low strength, low heat resistance, and difficulty in machining. These characteristics can be improved by bringing various physical and chemical changes in the PLA. For example, blending PLA with other copolymers can bring significant changes in the structure of PLA with improved strength, toughness, and thermal properties, which can be used as a bone implantable material [8]. The strength of PLA can also be improved by reinforcing it with carbon fiber or other synthetic fiber but at the cost of biodegradability and resorbability. Using natural fiber in place of synthetic fiber, the biodegradable nature of PLA can be maintained but decreases the mechanical performance when compared with synthetic fiber. Several research works have been carried out in the past dealing with the physical, mechanical, and compatibility nature of PLA to make it better and better over a period of time for its implementation in medical surgeries and implants [9].
Poly lactic acid in medical implants is being used in many forms such as film, sphere, hydrogels, foam, blends, fiber, particulates, capsules, etc. Its composite offers the ability to embrace surgical applications such as the malfunctioning of tissue or cell in in vitro or in vivo surgeries like the malfunctioning of tissue or cell in in vitro or in vivo surgeries. However, work is still to be done for its improved functioning, longevity, and durability, which cannot be accomplished without past background information and suggestive measures that need to be taken care of [10,11]. The present article, therefore, provides a detailed review of the synthesis of PLA, its behavior with copolymers upon blending, its fabrication for medical devices, and its current application in the medical field. The discussion carried out in this article will not only provide valuable evidence about PLA but also frame a comprehensive background to project PLA as a promising biomaterial. The article also discusses several issues regarding its compatibility with other polymers and with human tissues as a medical implant.
2. Poly Lactic Acid and Its Synthesis
The starting substrate to produce PLA is lactic acid (LA), which is basically acidic in nature and at its core structure, the carbon atoms are present in an asymmetrical form. Lactic acid exists in two isomers viz: (i) levorotatory form (D or R (−) lactic acid) and (ii) dextrorotatory form (L or S (+) lactic acid) [12]. D-Lactic acid is extracted from the muscles of animals while L-LA is produced by the fermentation of sugar through the action of bacteria. Beans, peas, corn, sugar beet, soymilk, and potato are some of the chief sources of L-LA. In biomedical applications, L-LA is preferred over D-LA due to several disadvantages such as metabolism rate, synthesis, and lack of optical purity [13]. Apart from PLA, several chemicals, e.g., propylene glycol, acrylic acid, and acetaldehyde are also synthesized from LA [14]. Lactic acid does not possess any charge and, it is very small in molecular size which enables it to infuse in the lipid membranes of cells [15]. It can serve as an energy source and provide antioxidant characteristics that protect from cell damage upon reaching the core of the cell via a monocarboxylate transporter. A large portion of Lactic acid is processed chemically by fermentation in the presence of bacteria whereas a small part of LA is obtained by the process of hydrolysis [16]. Usually, the process of fermentation yields a racemic mixture of LA, L-LA, and D-LA with optical purity [17]. The percentage of L and D in the LA depends upon the strain selected for the process. The biological advantage of lactic acid is not one but many. It is biocompatible with human tissue, provides support to cell tissues, allows accelerating growth of cell generation, and gets absorbs easily if the need arises [18].
The production of LA is carried out either by hetero fermentation or homo fermentation in the presence of various catalysts. The isomers formed during the process depend on the enzymes used [19] as shown in Figure 1. The input sources such as glucose, sugar, carbohydrates, etc. used in the production are very costly but can be brought down by using alternate sources such as agriculture waste, biomass residue, and waste collected from the food industry provided the chemical process and the enzymes used are different from the conventional ones [20].

Figure 1.
Fermentation of lactic acid.
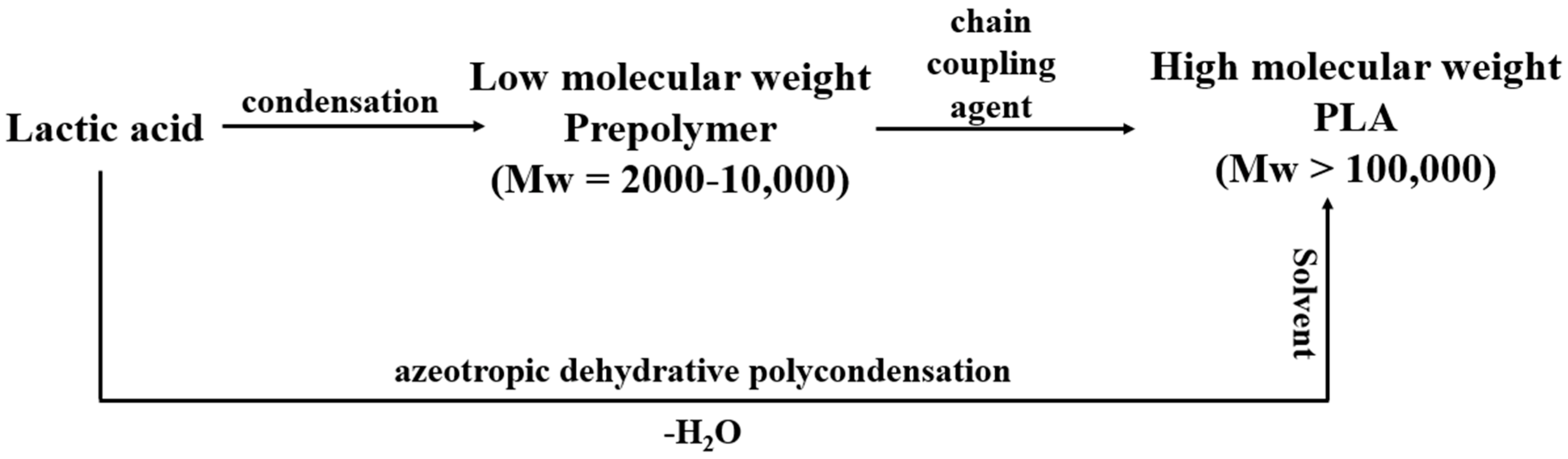
Formation of Poly lactic acid is a follow-up process performed after the formation of lactic acid. It is carried out via three processes namely (i) direct poly condensation, (ii) azeotropic dehydrative condensation, and (iii) ring opening polymerization. In direct poly condensation, as depicted in Figure 2, LA is dehydrated into oligomers. These oligomers are further dehydrated in the presence of chain coupling agents to form PLA. The whole process is executed without any delay since the chances of degradation of polymer compounds are higher [21]. This process is quite easy to perform but rarely preferred due to the entrapment of moisture in the viscous polymer melt leading to a decrease in the overall molecular weight of the polymer.
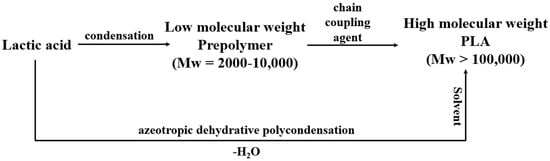
Figure 2.
Direct and azeotropic poly condensation.
In order to produce PLA of high molecular weight, azeotropic dehydrative condensation is performed. It is a time-consuming process and requires solvents of higher boiling points for the removal of dissociative molecules of water from the PLA compound. Longer reaction times and the use of inorganic solvents make this process very unsuitable and uneconomical for large production [22]. Another way of converting LA into PLA is ring-opening polymerization (ROP). In this process, the dehydrated and condensed LA is converted to oligomers under high temperature and low pressure thus releasing excess moisture from the small chain molecule of PLA. These small chains of PLA are termed meso-lactides. Thereafter, depolymerization of meso-lactides at a temperature higher than the melting point of lactides but lower than the degradation temperature of PLA is performed, resulting in the yield of poly lactic acid of high optical purity [23]. The PLA extracted in ROP is converted into pallets after the crystallization of the liquid resin.
2.1. Copolymerization of PLA
Despite being the most influential polymer for biomedical devices, a large scope for improvement still exists in various properties of PLA such as degradation characteristics, improved biocompatibility, rheological characteristics, crystallinity, and mechanical strength. These properties can be enhanced by the copolymerization of PLA with several other biocompatible polymers. With the help of copolymerization, PLA can be used in a wider range of biomedical applications. The advantages of various copolymerizations of PLA have been tabulated in Table 1.

Table 1.
Various copolymers with PLA and their properties.
2.2. Fabrication of PLA Composites for Biomedical Applications
Manufacturing of PLA-based composite particularly for medical implants has picked up a noticeable pace due to a continuous increase in demand [45]. Various techniques have evolved over the period such as freeze drying, melt blending, solvent casting, bioprinting, electrospinning, Supercritical fluid (SCF) technology, etc. with respective merits and demerits and have shown their potential of manufacturing bio material efficiently [46]. These processes work at different temperatures and pressures. In some, an organic solvent is used to achieve the required pattern at the surface while in others, composites are soaked in a solution to obtain a uniform structure throughout the volume [47]. The changes brought in the PLA matrix for the making of biomaterials are discussed for the following processes: freeze drying, electrospinning, SFC, and solvent casting.
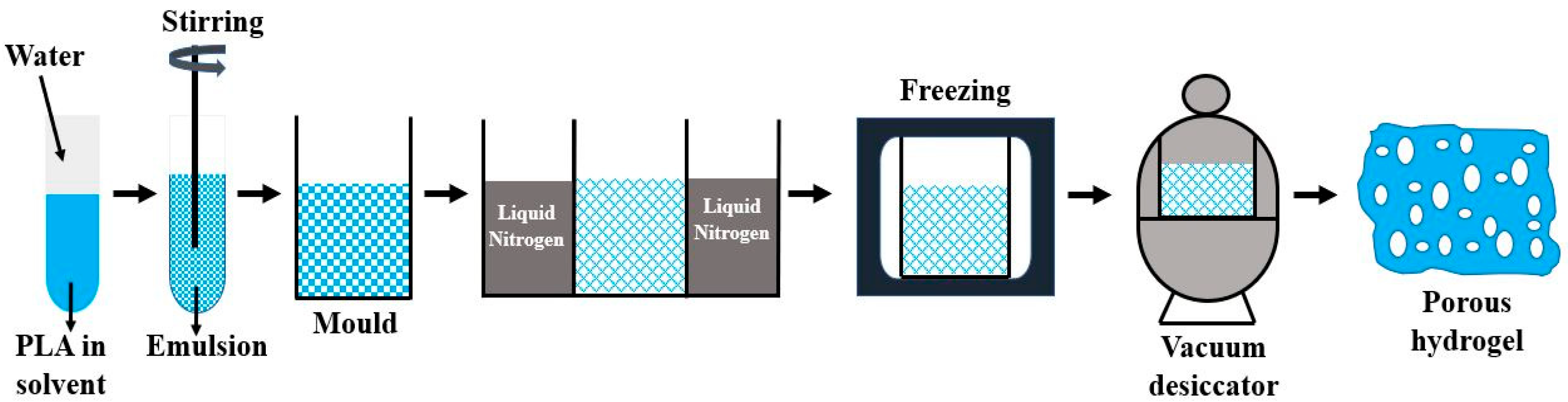
(a) PLA scaffolds for tissue engineering can be efficiently prepared by the method of freeze drying. Liquid PLA is dissolved in water and undergoes stirring to achieve a homogeneous polymeric solution. This solution is cast in a mold along with cooling at freezing temperature. Ice crystal is then formed at the interstitial sites, which leads to the aggregation of polymeric molecules. A vacuum desiccator is used to evaporate the solvent through sublimation forming the porous hydrogel having interconnected pores as shown in Figure 3. The hydrogel obtained in the process is highly porous, which can be altered by controlling parameters such as freezing temperature, concentration of solution, size of ice crystal, and Ph value of solution. This hydrogel is readily applied for cell seeding in tissue engineering. The degradation rate and solubility of the hydrogel can also be modified by its cross-linking with ultraviolet radiation and treatment with citric acid, carbodiimide, and glutaraldehyde [48]. This process limits its application for scaffold fabrication due to the presence of harmful residue, consumption of high energy, and very long hours of dehydration [49].
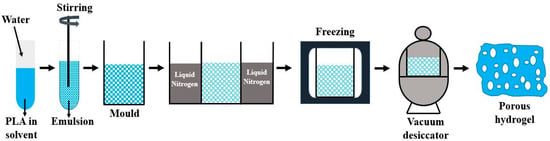
Figure 3.
Freeze drying technique for making porous hydrogels.
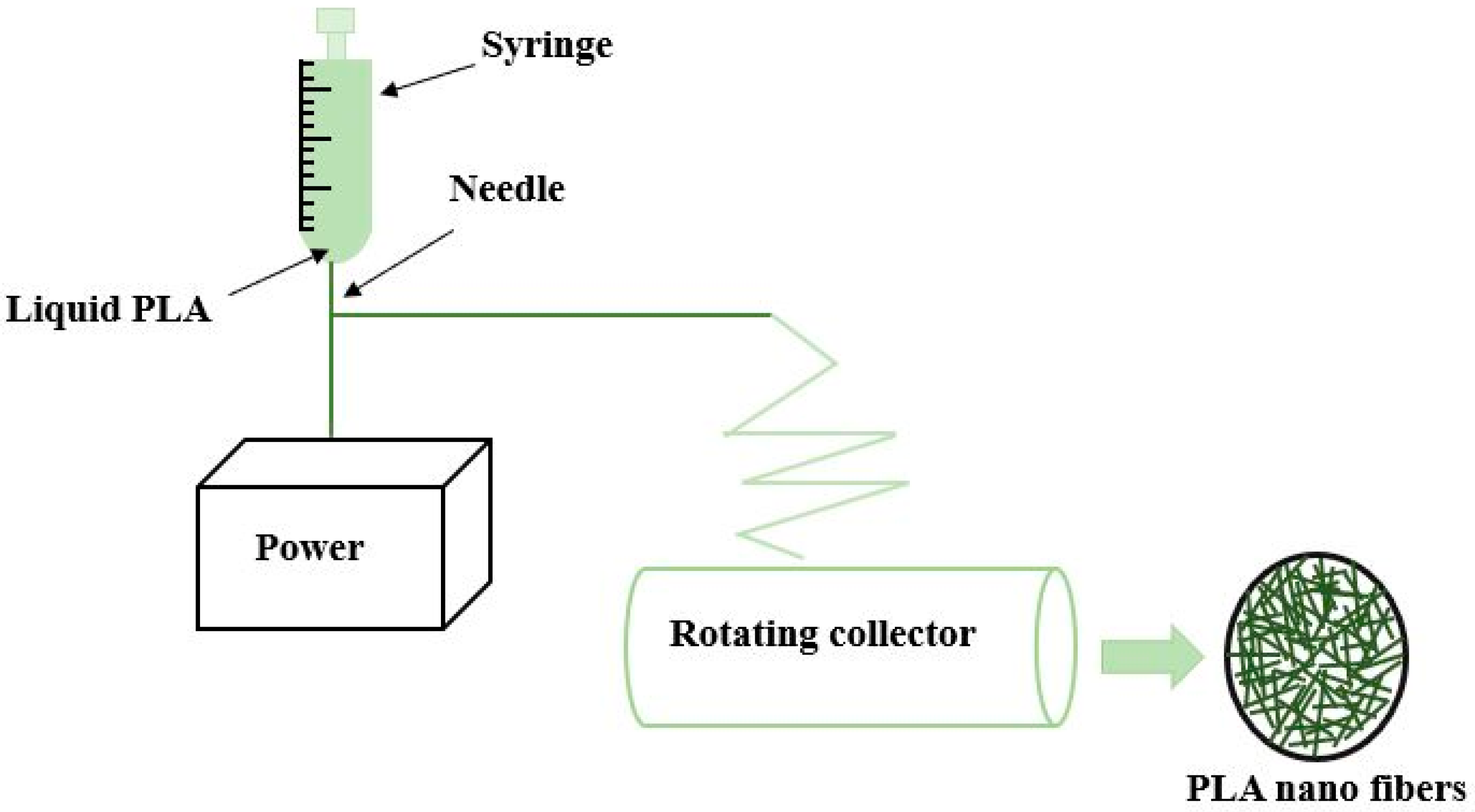
(b) To produce fibers ranging from tens of micrometers to nanometers, electrospinning is used as depicted in Figure 4. A highly concentrated solution of PLA in melt form under the influence of a strong electric field is pushed through a fine needle and collected at the rotating cylinder for the production of continuous fiber [50]. The fiber characteristics such as strength, porosity, texture, surface area, etc. are controlled by maintaining the rate of flow through the syringe and applied voltage. Nano fibers produced in this process exhibit exclusive characteristics such as a large surface-to-volume ratio, high porosity, and light weight. The native collagen fibrils found in the extracellular matrix are remarkably intimated by the morphology of nanofiber produced by electrospinning. In addition, exchanging of nutrients and gaseous are also possible provided the macropores at the scaffolds should be maintained. For the purpose of regenerative medicine, electrospinning is mostly preferred over other processes due to its ease of fabrication and flexibility. Electrospun fibers have the capability to mimic the characteristics of the extracellular matrix but the use of toxic solvents limits the horizon of this process. Insufficient cell infiltration and inhomogeneous cell distribution are other demerits of this process. Apart from PLA, various other polymers such as polyurethane, polycaprolactone, nylon-6 poly (glycolic acid), etc. can also be electrospun [51].
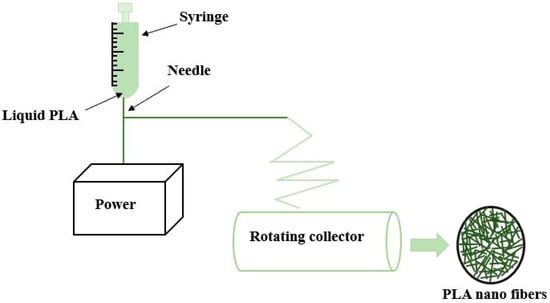
Figure 4.
Electrospinning method for producing nano fiber.
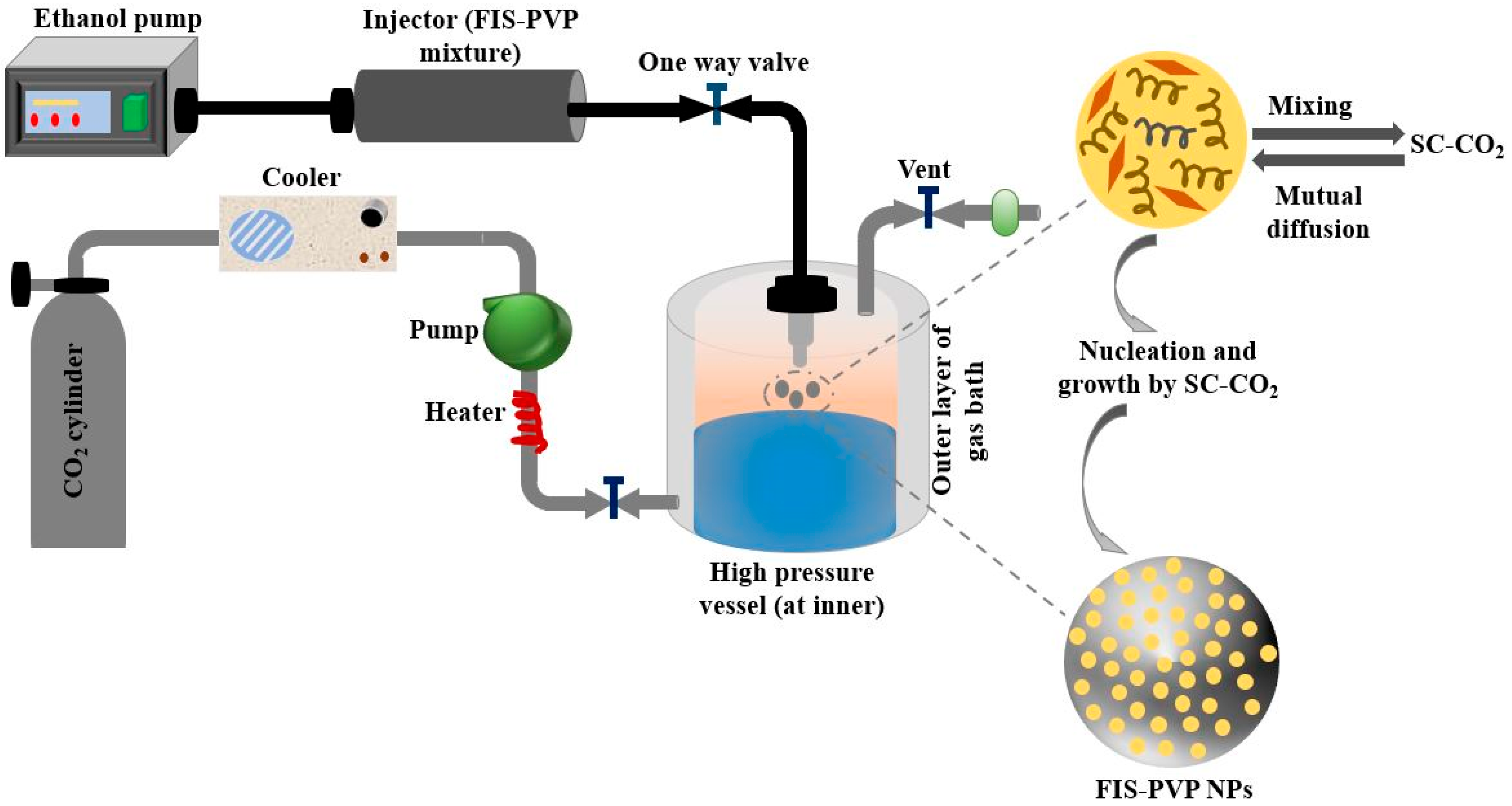
(c) Another way of making bio material (3-D scaffolds) for tissue engineering without using solvents is Super critical fluid (SFC) as represented in Figure 5. The advantage of using supercritical fluid is its control over architectural activities of internal porosity, elimination of solvent, and mimicking the growth of bioactive material at the surface [52]. The coexistence of liquid and gas makes it an exclusive method as compared to other methods that exist in either liquid or gas form at normal temperature and pressure. Till now, the most widely used supercritical fluid is carbon dioxide due to its favorable characteristics such as availability, user-friendliness, low cost, and non-toxic behavior. Due to its low critical conditions, CO2 is extensively used to process thermal sensitive/biological compounds. This technique is highly versatile that various biopolymers like PLLA, PGLA, forms of poly saccharides, and proteins can be easily processed for the fabrication of very highly porous scaffolds [53]. In an experimental analysis, it was observed that 95% seeding efficiency with a viability of 40% was obtained in a single day of culturing in the rats [54]. Apart from the above-said advantages, the control of particle size and morphology is very difficult in this process, which happens due to polymer solubility in super critical fluid.
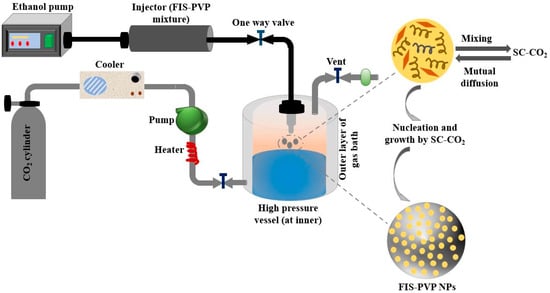
Figure 5.
Schematic illustration of super critical fluid CO2 method for preparing Fisetin-Encapsulated Poly (Vinyl Pyrrolidone) Nano particles.
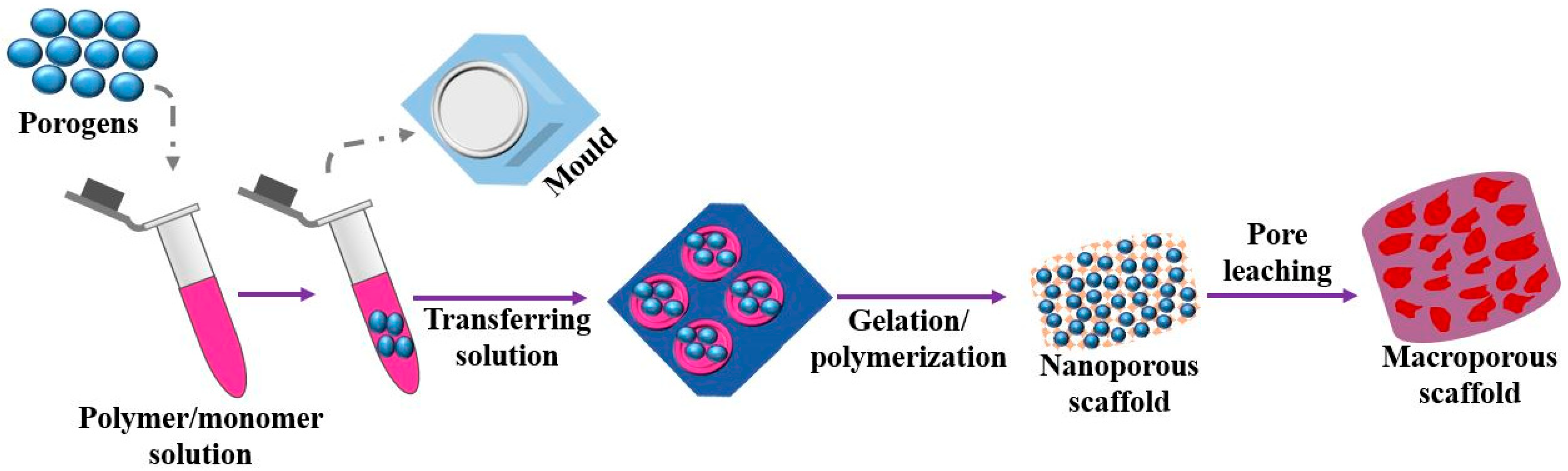
(d) One of the simplest techniques of processing scaffolds for tissue engineering is solvent casting as shown in Figure 6, which does not require any specific equipment. Here, the liquid PLA is dissolved in a solvent followed by the addition of salt of a specific size in the solution to make it homogenous. The mixture obtained is molded in a 3-D through casting. The solvent is made to evaporate from the solution leading to the formation of a matrix with uniform distribution of particles of salt. Afterward, water is added to the polymer matrix to filter out the salt particles from the matrix resulting in the formation of a porous structure capable of seeding cells [55]. The selection of solvent is the crucial parameter that decides the final surface texture of the matrix such as heterogeneity, the orientation of crystals, swelling parameter, and physical characteristics like deformation rate. These characteristics will decide the specific domain where the produced scaffold is used. This process has several advantages such as short processing time and low maintenance cost, and it can produce scaffolds of different porosity by varying the size of the porogens [56]. Various biopolymers such as PLLA and PGLA can be easily processed by this technique. The chief advantage of this method is pore size and its porosity can be easily modulated. In addition, drug incorporation becomes easier within the scaffolds. Besides having such attractive characteristics, solvent casting is very often used for making scaffolds due to the use of harmful solvents in the solution [57].
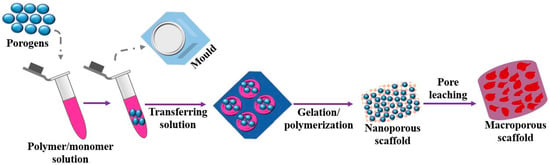
Figure 6.
Solvent casting method for fabricating macro porous scaffold.
3. Scope of PLA in Biomedical Applications
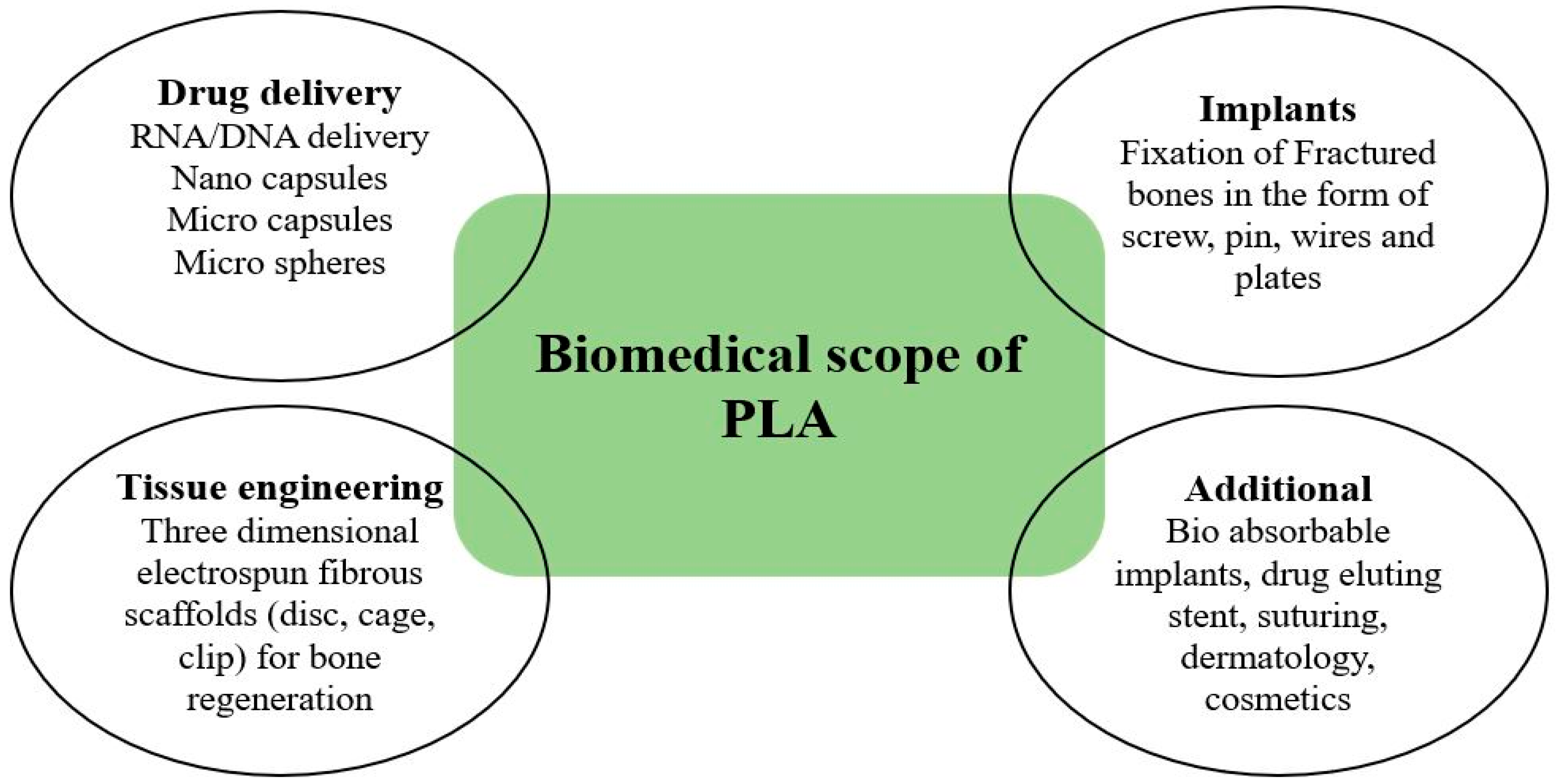
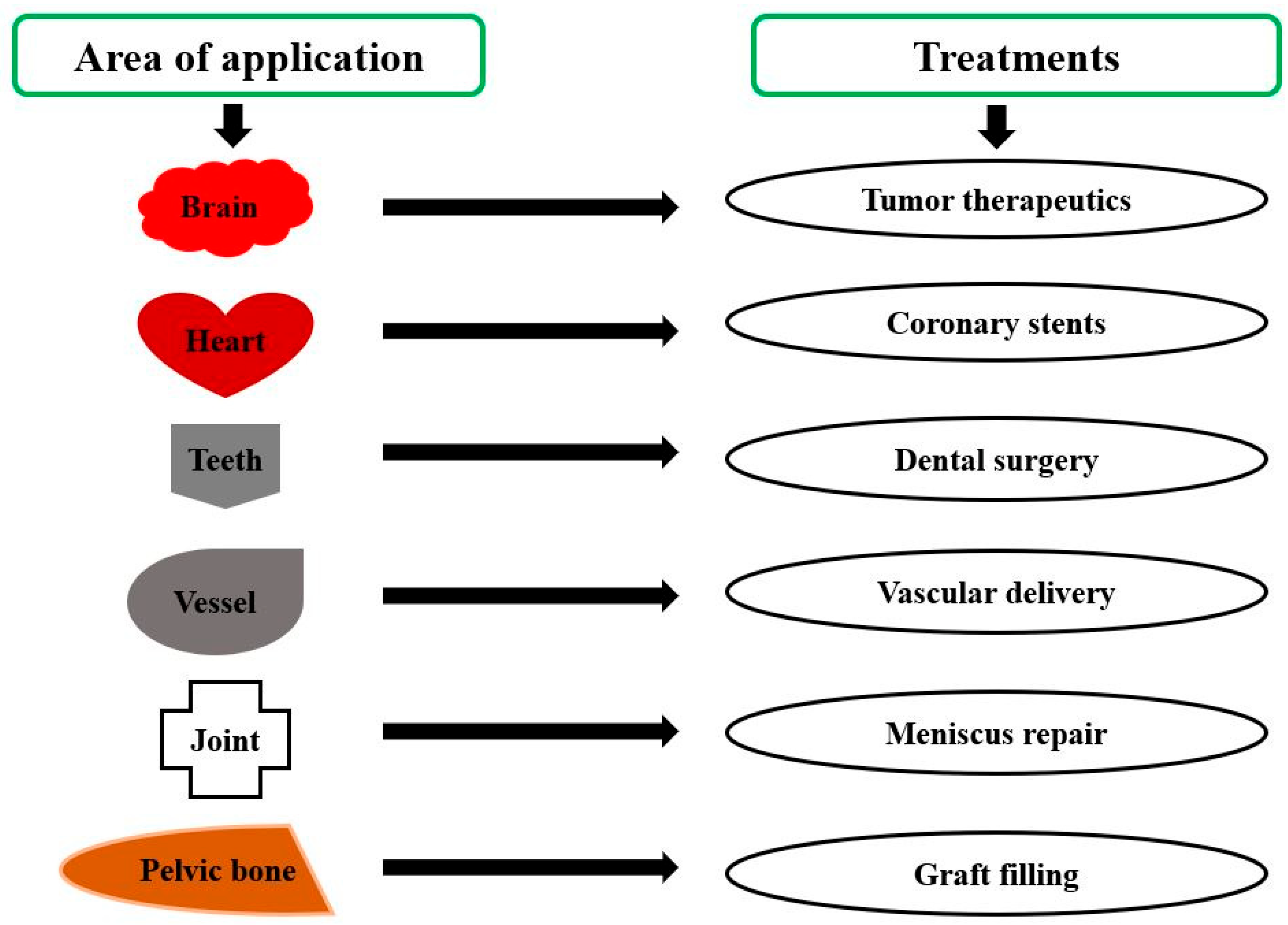
Polylactic acid has a notable reputation in many biomedical applications due to its bioresorbability and biocompatibility with human tissues. Scaffolding, drug delivery, medical implants, suturing, membrane covering, derma, cosmetics, etc., are some of the major fields of biomedical, as depicted in Figure 7, where the role of PLA has been appreciable in the last decade [58]. Physical and chemical modification of PLA is required to render its service in a diversified form in medical applications. Sometimes, surface modifications of PLA, such as plasma treatment, radiation-induced technique, etc., are carried out for enhancing the biocompatibility of PLA. Blending of PLA with copolymer is also performed to achieve the desired behavior. Polydioxanone (PDS), Polyglycolide (PGA), and PLA are the most common biopolymers used extensively in biomedical applications [59], but due to favorable properties, more attention is being given to PLA as a biomaterial.
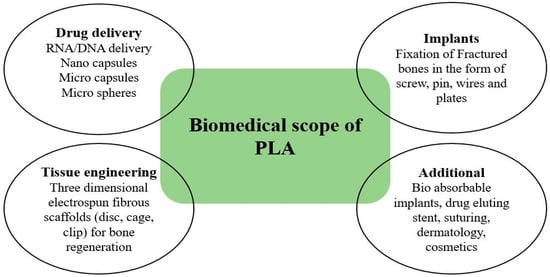
Figure 7.
Biomedical applications of polylactic acid.
3.1. Polylactic Acid in Drug Delivery
Developing a drug delivery system (DDS) to address new challenges is only possible through innovative approaches. Supplying the drug to various parts of the human body at a specific quantity with maximum therapeutic potential and minimum side effects has always been a longstanding desire of medical practitioners [60]. Various systems have been evolved as drug carriers, for example, nano capsules (NC), nanospheres (NS), liquid crystal, multifunctional dendritic polymers, vesicles, micelles, etc., but still, the oral route is restricted to small molecules like NC or NS [61]. Some typical DDS based on PLA are represented in Figure 8. Drug delivery based on PLA is showing promising results for diagnosis, therapy, and imaging. For instance, micro and nano particles (NPs) delivery systems produced by the blends of methoxypoly (ethylene glycol)/PLA (mPEG/PLA) are being considered as a good replacement for conventional Kolliphor EL [62]. A range of properties of the blend, like drug loading, particle size, release profile, etc., can be easily controlled by varying the percentage of mPEG/PLA in the blend [63].
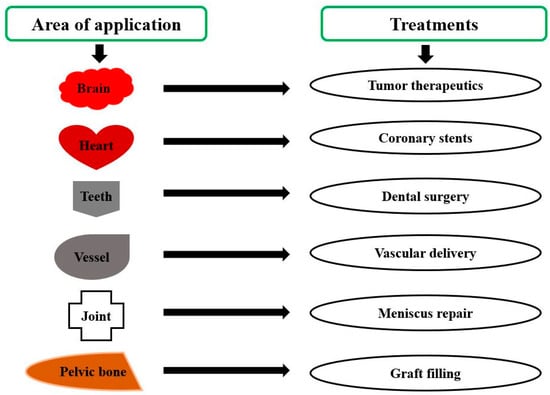
Figure 8.
Poly lactic acid-based drug delivery systems (Adapted from the reference [64]).
PLA can be transformed into micro capsules (MCs), dosage, pallets, and NPs due to its biodegradability, biocompatibility, strength, and solubility in various solvents [65]. Several sustainable drugs like protein/peptide and DNA/RNA for delivery purposes can be made from modified and unmodified microparticles (MPs) and NPs of PLA [66]. MPs and NPs are very small particles that enable them to permeate through biological barriers, especially blood barriers of the brain. Polylactic acid-based MCs are extensively applied in the delivery of drugs for prolonged administration in a large variety of medical agents [67,68,69], such as local anesthetics and vaccines, contraceptives, and antagonists.
Peptides and proteins-based PLA DDS are designed for specific purposes and receive significant attention due to their effectiveness even at comparatively lower dosages [70]. Reconstructive surgery of the face can be carried out by temporary filling of the microsphere of PLLA. Transcatheter arterial embolization, an efficient procedure for managing hemorrhages, tumors, and fistula malformation, can be healed with embolic material composed of microsphere of PLLA [71]. It has been seen that PLA-based bio materials lack cell interaction due to the deficiency in chemical functionality, which also restricts the continuous release of hydrophilic molecules, especially proteins [72,73,74]. These limitations can be overcome by introducing an amine functional group in the PLA-based DDS and additives fabricated by direct conjugation. PLA-based nanomaterials are also used for stimuli response. These stimuli responses effectively target delivery where DDS acts as an active member rather than a passive carrier [75,76,77].
Nanofibers of PLA-poly butylene adipate (PBA) blends are very effective for the transdermal delivery of teriflunomide (an antirheumatic agent). These nanofibers quickly degrade and dissolve in the cells [78]. The PLA particulate system is important for stimuli and targeted DDS because it can target decayed cells [79]. The synchronization of stimuli-responsive PLA nanocarriers with pathology by in vivo hydrogelation is helpful in the healing of diseases such as tumors by maintaining the pH value of extracellular tissues [80,81,82]. PLA can also be synthesized to design dendritic core shells for enhanced transport capacity by mixing Polyethylene glycol (PEG) monomethyl ether shells in PLA blend through imine bonding [16].
Films based on PLA have been extensively explored for drug delivery systems [83]. Paclitaxel-eluting stents were developed by blending ethylene-vinyl acetate copolymer (EVA) with PLA and examined the effect of varying the ratio of EVA and PLA in the blend on the rate of drug release [84]. It was reported that the ratio of EVA and PLA in the blend has a significant effect on the rate of drug release. Films for wound dressing applications for the drug release of metronidazole and gentamicin sulfate are also being developed by the blend of PLA and PEG. Nanoparticles based on PLA with monoclonal anti-bodies (mAb) characteristics are being developed for the drug delivery of specific antigens on breast epithelial cancer cell lines [85]. Both small and large molecules can be efficiently targeted to the cell or tissue of interest.
3.2. Polylactic Acid in Implants
Several metals such as titanium and its alloys, stainless steel, cobalt, and chromium have been implanted in the human body in the forms of plates, pins, screws, and wires for operating bone fixation [86]. These metals have shown incredible potential in bone fixation surgery in the last 3 to 4 decades. However, a few disadvantages related to metal implants, such as low corrosion, high density, and low biocompatibility, make way for biodegradable polymers, particularly PLA, to replace metal implants [87]. Polylactic acid has sufficient mechanical strength that it can serve as bone implants satisfactorily. Furthermore, it is biodegradable; thus, the chances of side effects in human bones are negligible. The current state of PLA as a bone fixation material has uncovered many possibilities for development in bone implants [88]. By synthesizing the PLA with L-PLA and D-PLA, plates and screws for fracture fixation can be made. For orthopedic applications, films of PLA have been fabricated that showed good compatibility with fibroblast, nasal septum cells, and osteosarcoma cells [89,90].
A blend of PLA and polyvinylpyrrolidone (PVP) for ocular implants is being prepared for the enhanced release rate of fluorometholone delivery [91]. By adding surfactants such as ethylene oxide or propylene oxide in the blend of PDLLA/PLLA, a potential implant for orthopedic and dental applications can be prepared [92]. The commercialization of drug-eluting stents prepared from the blend of PLA is under consideration by several pharma companies [93]. Nanofibers produced from PLA/PCL embedded by 5-fluoro uracil are also used as drug-eluting stents to treat cancer [94,95,96]. The release of cancerous drugs is higher for hybrid nanofibers than pure polymers because of the combined effect of immiscible polymers due to their superior potential in therapeutic implants [97].
The biodegradability of polymer within the human body is one of the most important characteristics a polymer should demonstrate. As far as PLA is concerned, it is used to reconstruct ligaments and tendons due to its high retention characteristics [98]. Stents are also prepared from PLA for urological and vascular surgery [99]. Three-dimensional scaffolds of PLA are extensively made for the gene therapy of diseases like cardiovascular, bone, and cartilage regeneration and to cultivate different types of cells during orthopedic and neurological treatment [100]. Therapeutic implants like bone formation, intramembrane, endochondral ossification, etc., can be performed with the biomaterial prepared by seeding osteogenic stem cells on PLA scaffolds [101].
Plates and screws used in maxillofacial osteosynthetic surgery are made from platinum, but with several disadvantages such as mutagenetic effects, problems in removal and palpability, etc., their extensive implementation is restricted. To resolve these problems, PLA is being put forward as an alternative to performing maxillofacial osteosynthetic surgery in the near future [102].
3.3. Polylactic Acid in Tissue Engineering
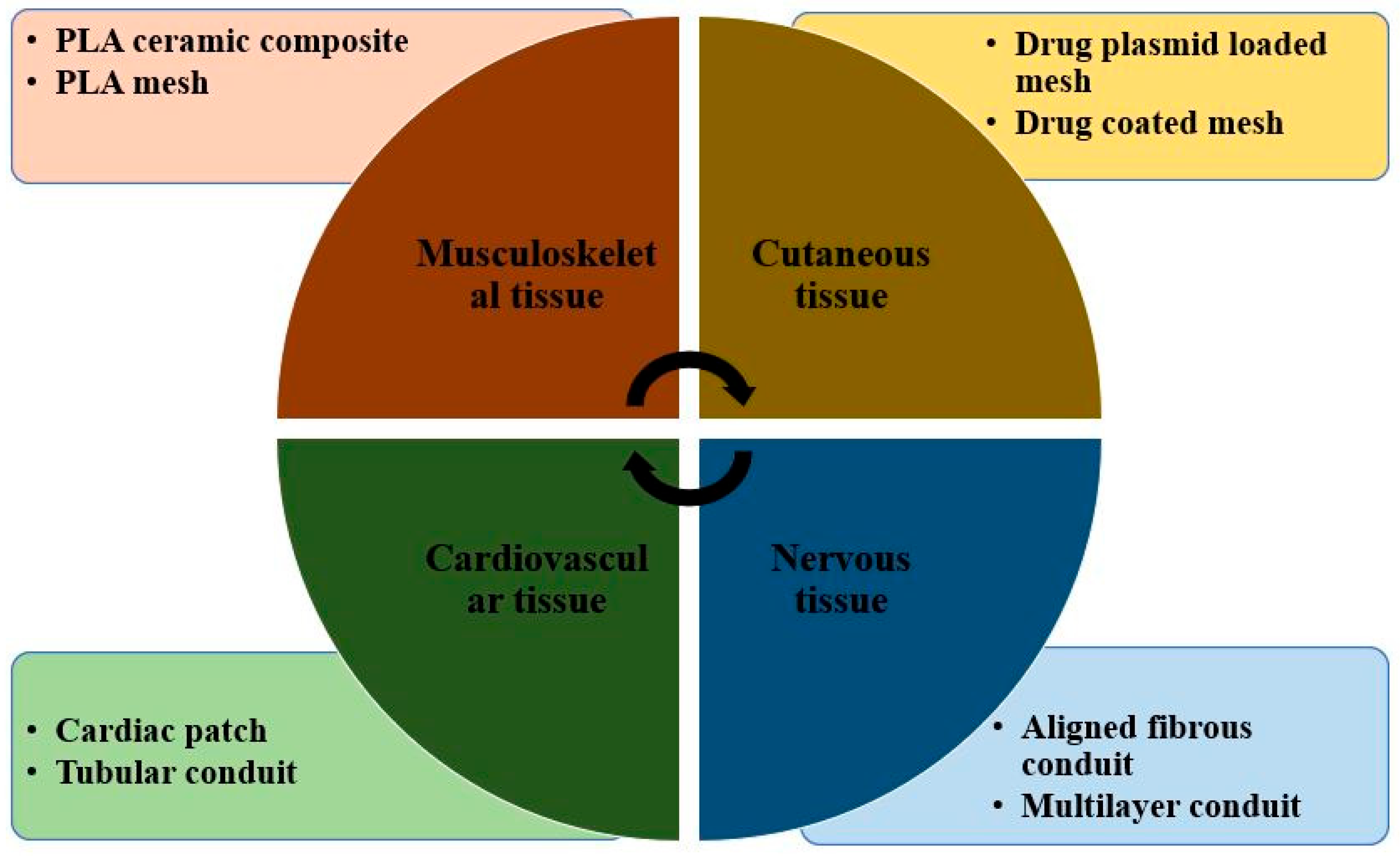
With recent developments in biomedical engineering, PLA-based biomaterials are gradually making their place in tissue engineering as demonstrated in Figure 9. Although numerous promising results were obtained with few metal implants due to the non-biodegradability of metal, biopolymers are now being projected as a potential scaffolds application [103]. In addition, due to their flexibility and tailorable properties, biopolymers find greater scope in tissue engineering than metals. The most common biopolymers used for scaffoldings are PLA, PGA, and PLGA, having approval from the Food and drugs administration [104]. At the same time, constructing scaffolds is the most important thing to be taken care of for the adhesion of cells with polymer. Polylactic acid is hydrophobic and has a slow rate of degradation in the environment of water. Using PLA in scaffolding in its pure form will not be a good idea; therefore, its copolymerization through blending and forming with other biopolymers is usually carried out to enhance its degradability and biocompatibility [105]. In recent years, several techniques have evolved for making porous PLA scaffolds. These are particles leaching, foaming, and electrospinning.
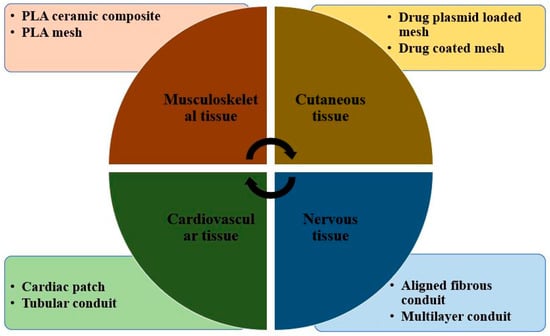
Figure 9.
Poly lactic acid-based tissue engineering bio materials [Adapted from the reference [105].
Till now, many PLA-based composites for tissue engineering and scaffolding have been prepared. For instance, PLA-based octadecyl amine composites fabricated via solution preparation technique in the presence of chloroform and nanodiamond showed improved mechanical properties [106]. The basic requirements for the scaffolding and grafting of vascular tissues are antithrombogenicity, application-oriented, sufficient mechanical strength, and bio compatibility to match with the tissue or blood vessels [107]. Presently, matrices based on collagen and hyaluronan are the most prevalent scaffolds applied in clinical applications because they deliver substrates, a necessary element in articular cartilage [108]. Under the trade name of BioSeed-B and BioSeed-C (Bio Tissue Technologies AG, Freiburg, Germany), scaffolds of PGA/PLA, polydioxanone, and polyglactin are also used for the reparation of cartilage.
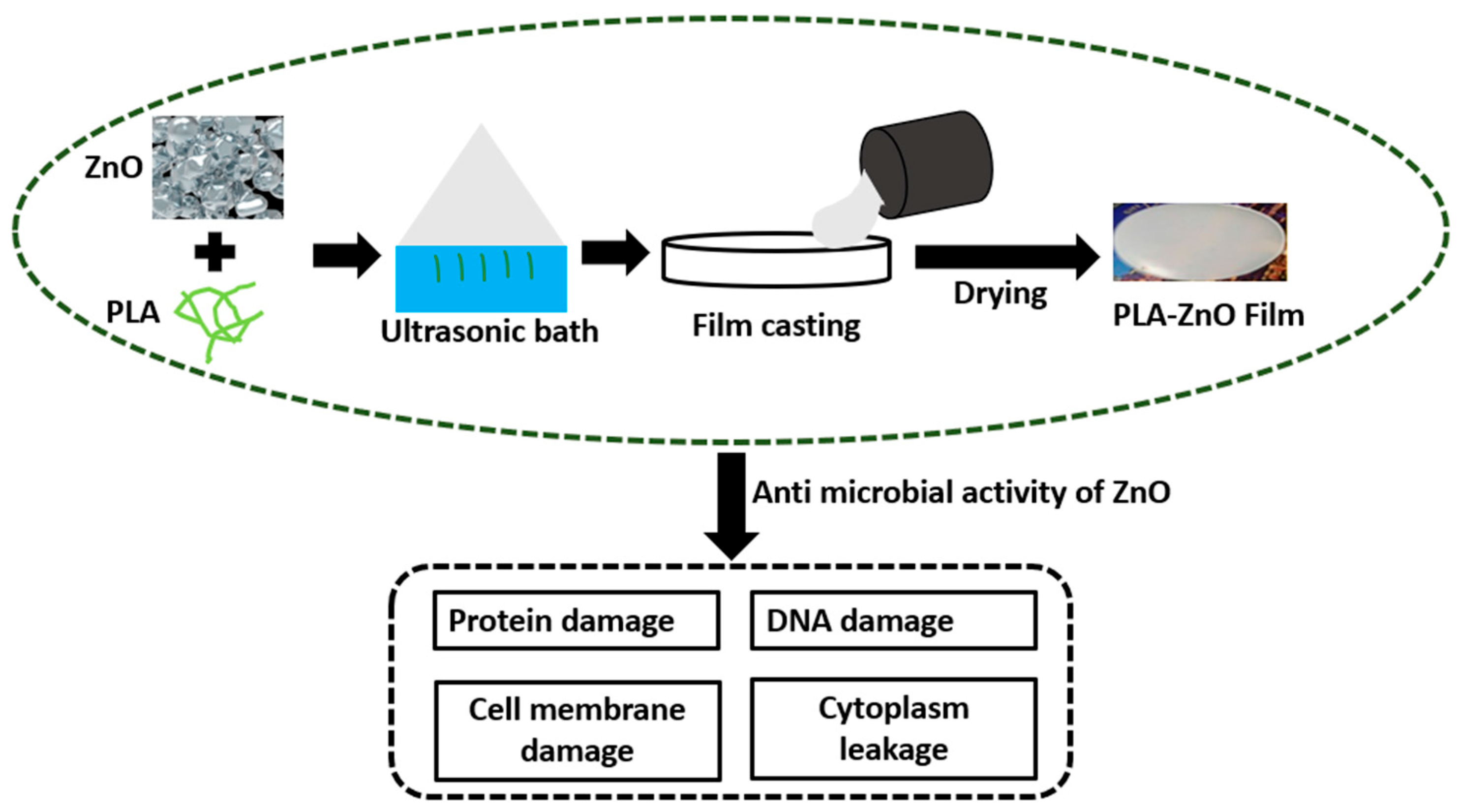
For the regeneration of bone, three-dimensional (3D) fibrous scaffolds are mostly recommended. A 3D micro fibrous scaffold prepared via electrospinning technique followed by mechanical expansion showed huge potential in the proliferation of osteoblast by offering a suitable substrate for bone formation and cell infiltration. For this, an experiment on rabbits was carried out which showed noticeable changes in 2 to 4 weeks [109]. To modulate biodegradability and enhance the compatibility of PLA for tissue growth, recovery, and scaffolds, it can be synthesized with various copolymers. A novel technique for creating tissue scaffolds for bone tissue is 3D printing [110]. Several types of scaffolds made of PLA, such as porous cages, solid disc PLA-filled and coated scaffolds, can be created by 3D printing [111]. PLA-coated scaffolds filled with collagen were tested for biocompatibility and endotoxin production. It was found that the scaffold showed enhanced compatibility with tissue, and the endotoxin level was far below the permissible limit [112]. Printed discs based on PLA have shown rapid growth and expansion of different cells such as endothelial cells, osteoblasts, and osteoblast-like cells. The steady release of stromal-derived factors that helps in the growth of endothelial cells and encourages the formation of neo-vessel can be achieved by cages made of PLA, thus verifying the potential of 3D PLA scaffolds [113]. To increase the rate of vascularization and healthy bioactivity of osteoinductive cells in bone tissue engineering, the biodegradability of 3D scaffolds plays a crucial role. Because of the favorable properties like flexibility, practicality, bioresorbability, and biocompatibility, 3D-printed PLA scaffolds can be used to control the release of deferoxamine necessary for osteogenesis and angiogenesis for the construction and development of fractured bone [114]. Poly hydroxyapatite (PHA)/PLA 3D composite scaffolds have also been explored for inflammation and bone repair. It was observed that PHA/PLA 3D scaffolds showed better compatibility, bioactivity, and osteoinductivity with a low chance of inflammation [115]. To further enhance osteogenic activity in bone tissue engineering, PHA/PLA scaffolds functionalized with citric acid and polyethyleneimine have been developed in the recent past [116]. The successful development of 3D printed PLA/PHA/silk scaffolds clip for the bone support showed improved strength and biocompatibility as compared to conventional clip [117,118,119] is another indication of the potential of PLA in bone tissue engineering. Recently, more attention has been given to regenerative treatments using stem cell therapies. The available reports suggest that Mesenchymal stem/stromal cells are the best-fitting materials in tissue replacement [120]. Poly lactic acid-based bio dental implants are under development. The latest report suggests that silica nano filler reinforced PLA bio material can serve the purpose of dental filling in the tooth cavity. Moreover, the biodegradability and compatibility of the prepared amalgam showed satisfactory results [121]. However, research and development need to be carried out continuously to obtain the best-fitting PLA-based dental implant. Poly lactic acid can efficiently host the ZnO particle to activate the antimicrobial activity for the regeneration of tissue or cell [122]. Figure 10 illustrates the biological activity of PLA-filled ZnO nano particles in which Gram-negative and Gram-positive bacteria are reduced by 99% due to the high interfacial interaction between nano filler and PLA.
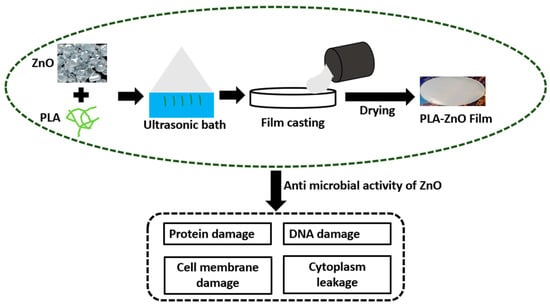
Figure 10.
Antimicrobial activity of PLA-ZnO films to eliminate gram negative and gram positive bacteria (Adopted from [122]).
Table 2 summarizes some typical composites based on PLA, which are commonly adapted in the form of organs, implants, and scaffolds.

Table 2.
PLA-based composites for medical.
4. Food and Drug Administration Approved PLA Formulations Used in Medicine
The use of PLA in various medical surgeries, implants, and drug deliveries is often encountered with several physical and biological issues such as poor retention at delivery sites, poor bio availability, longevity, limited water solubility, etc. [129,130,131]. To overcome these problems, PLA is coupled with various other biocompatible polymers for the fabrication of nano formulations used in medical therapeutic deliveries as approved by the FDA [132,133,134]. For instance, a formulation based on PLGA-b-PEG-b-PLGA of size 77–84 nano meter (nm) has the advantage of sustaining oral formulation and therefore extensively used in oncology [135]. While PLA-PEG nano formulation of size greater than 200 nm has good healing characteristics in healing bacterial infections [136]. Hydrogels of PLA-based formulation also have a significant role in medicinal therapeutics. It has a vital role in birth control gene therapy with the formulation of PLGA-b-.
PEG-b-PLGA [137]. Moreover, nano formulation of size ranging between 200 nm to 300 nm is very much beneficial in the application of oncology [138,139,140]. In the field of vesicle therapy, PLA-b-PEG with a formulation size under 200 nm is highly useful in pH-responsive release systems [23,139,141].
5. Current Limitations
Poly lactic acid is more often avoided due to its high price since it is more expensive than petrochemicals. Its method of manufacturing is more intense and its yield is not as good as compared to any other conventional polymer. Its working temperature is very low due to its low melting point and its coblending with another polymer is very hard to carry out. It is highly permeable and thus releases oxygen and water molecule very easily. Moreover, it takes more time to decompose as compared to other bio polymers. Techniques are under development to enhance its decomposition rate and hoping to see an improved PLA with a better decomposition rate.
6. Conclusions and Future Scope
The kind of characteristics PLA possesses makes it suitable for bio implants and medical surgeries with the advantage of being processed at a relatively low cost as compared to other polymers. Its compatibility with other polymers to obtain improved mechanical and thermal characteristics widens its scope for the fabrication of medical devices. Poly lactic acid has proved to be a versatile polymer, which gives it an added advantage of being tailored into different forms such as nano fiber, micro capsules, nano particles, and hydrogels. By incorporating various fibers in PLA, a significant improvement in strength can be achieved that in near future can replace metallic material in bone implants. Various favorable properties of PLA such as bioresorbable, biocompatible, good endurance, ease of fabrication, and compostability are signaling toward its higher exploitation in near future for the development of biomaterial implants. The properties enhancement of PLA by blending it with various copolymers is playing a crucial part in expanding its scope in the biomedical domain (Scaffolding, drug delivery, tissue engineering, medical implants, membranes covering, derma, cosmetics, medical surgeries, and human implants). As far as its applications are concerned, PLA is found suitable for drug delivery, implants, and tissue engineering, which is expected to grow in near future with continuous research and developments. Although PLA has several limitations such as various attributes of degradability, strength, ease of processing, etc., it is expected to remain the preferred polymer for the development of biomaterial. However, as far as the literature is concerned, various aspects such as interfacial energy, barriers and optical properties, influence of processing temperature, environment, and storage (aging) on the properties of PLA have not been fully evaluated yet. Therefore, a lot of work is still to be done to make PLA viable as a permanent, cost-effective, and safe solution for its implementation as a biomaterial in the human body.
Author Contributions
Conceptualization, L.R., B.G., P.B., T.S., S.S. (Shubham Sharma), J.S.; formal analysis, L.R., B.G., P.B., T.S., S.S. (Shubham Sharma), J.S.; investigation, L.R., B.G., P.B., T.S., S.S. (Shubham Sharma), J.S.; writing—original draft preparation, L.R., B.G., P.B., T.S., S.S. (Shubham Sharma), J.S.; writing—review and editing, S.S. (Shubham Sharma), S.S. (Sunpreet Singh); supervision, S.S. (Shubham Sharma), S.S. (Sunpreet Singh); project administration, S.S. (Shubham Sharma), S.S. (Sunpreet Singh); funding acquisition, S.S. (Shubham Sharma), S.S. (Sunpreet Singh). All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Kotrocz, L.; Bakonyi, P. Pinpoint Loading Examinations of Poly(lactic acid) Biopolymers. Acta Tech. Jaurinensis 2018, 11, 206–217. [Google Scholar] [CrossRef][Green Version]
- Tábi, T.; Hajba, S. Investigation of long cellulose fibre reinforced and injection moulded poly (lactic acid) biocomposites. Acta Tech. Jaurinensis 2018, 11, 150–164. [Google Scholar]
- Mishra, S.K.; Dahiya, S.; Gangil, B.; Ranakoti, L.; Agrawal, N. Mechanical properties of fibre/filler based poly(Lactic Acid) (Pla) composites: A brief review. Acta Innov. 2021, 41, 5–18. [Google Scholar] [CrossRef]
- Lendvai, L.; Brenn, D. Mechanical, morphological and thermal characterization of compatibilized poly (lactic acid)/thermoplastic starch blends. Acta Tech. Jaurinensis 2020, 13, 1–13. [Google Scholar] [CrossRef]
- Ranakoti, L.; Gangil, B.; Mishra, S.K.; Singh, T.; Sharma, S.; Ilyas, R.; El-Khatib, S. Critical Review on Polylactic Acid: Properties, Structure, Processing, Biocomposites, and Nanocomposites. Materials 2022, 15, 4312. [Google Scholar] [CrossRef]
- Lendvai, L.; Omastova, M.; Patnaik, A.; Dogossy, G.; Singh, T. Valorization of Waste Wood Flour and Rice Husk in Poly(Lactic Acid)-Based Hybrid Biocomposites. J. Polym. Environ. 2022, 1–11. [Google Scholar] [CrossRef]
- Singh, T.; Pattnaik, P.; Kumar, S.R.; Fekete, G.; Dogossy, G.; Lendvai, L. Optimization on physicomechanical and wear properties of wood waste filled poly (lactic acid) biocomposites using integrated entropy-simple additive weighting approach. S. Afr. J. Chem. Eng. 2022, 41, 193–202. [Google Scholar] [CrossRef]
- Fekete, I.; Ronkay, F.; Lendvai, L. Highly toughened blends of poly(lactic acid) (PLA) and natural rubber (NR) for FDM-based 3D printing applications: The effect of composition and infill pattern. Polym. Test. 2021, 99, 107205. [Google Scholar] [CrossRef]
- Lalit, R.; Mayank, P.; Ankur, K. Natural fibers and biopolymers characterization: A future potential composite material. Stroj. Časopis-J. Mech. Eng. 2018, 68, 33–50. [Google Scholar] [CrossRef]
- Ranakoti, L.; Rakesh, P.K.; Gangil, B. Effect of Tasar Silk Waste on the Mechanical Properties of Jute/Grewia Optiva Fibers Reinforced Epoxy Laminates. J. Nat. Fibers 2021, 19, 10462–10474. [Google Scholar] [CrossRef]
- DeStefano, V.; Khan, S.; Tabada, A. Applications of PLA in modern medicine. Eng. Regen. 2020, 1, 76–87. [Google Scholar] [CrossRef]
- Majgaonkar, P.; Hanich, R.; Malz, F.; Brüll, R. Chemical recycling of post-consumer PLA waste for sustainable production of ethyl lactate. Chem. Eng. J. 2021, 423, 129952. [Google Scholar] [CrossRef]
- Cuker, B.E. Instead of Eating Fish: The Health Consequences of Eating Seafood from the Chesapeake Bay Compared to Other Choices. In Diet for a Sustainable Ecosystem; Springer: Cham, Switzerland, 2021; pp. 247–268. [Google Scholar] [CrossRef]
- Pramod, C.V.; Fauziah, R.; Seshan, K.; Lange, J.P. Bio-based acrylic acid from sugar via propylene glycol and allyl alcohol. Catal. Sci. Technol. 2018, 8, 289–296. [Google Scholar] [CrossRef]
- James, R.; Manoukian, O.S.; Kumbar, S.G. Poly(lactic acid) for delivery of bioactive macromolecules. Adv. Drug Deliv. Rev. 2016, 107, 277–288. [Google Scholar] [CrossRef]
- Singhvi, M.S.; Zinjarde, S.S.; Gokhale, D.V. Polylactic acid: Synthesis and biomedical applications. J. Appl. Microbiol. 2019, 127, 1612–1626. [Google Scholar] [CrossRef] [PubMed]
- López-Gómez, J.P.; Alexandri, M.; Schneider, R.; Latorre-Sánchez, M.; Lozano, C.C.; Venus, J. Organic fraction of municipal solid waste for the production of L-lactic acid with high optical purity. J. Clean. Prod. 2020, 247, 119165. [Google Scholar] [CrossRef]
- Muhialdin, B.J.; Saari, N.; Hussin, A.S.M. Review on the Biological Detoxification of Mycotoxins Using Lactic Acid Bacteria to Enhance the Sustainability of Foods Supply. Molecules 2020, 25, 2655. [Google Scholar] [CrossRef]
- Juturu, V.; Wu, J.C. Microbial production of lactic acid: The latest development. Crit. Rev. Biotechnol. 2016, 36, 967–977. [Google Scholar] [CrossRef]
- Byers, J.A.; Biernesser, A.B.; Chiaie, K.R.D.; Kaur, A.; Kehl, J.A. Catalytic Systems for the Production of Poly(lactic acid). In Synthesis, Structure and Properties of Poly(lactic acid); Springer: Cham, Switzerland, 2017; pp. 67–118. [Google Scholar] [CrossRef]
- Sin, L.T.; Rahmat, A.R.; Rahman, W.A.W.A. Applications of Poly(lactic Acid); William Andrew Publishing: Oxford, UK, 2013; pp. 301–327. [Google Scholar] [CrossRef]
- Mustățea, G.; Ungureanu, E.L.; Belc, N. Polylactic acid (pla) for food packaging applications—A short overview. Ann. Food Sci. Technol. 2019, 20, 9–14. [Google Scholar]
- Hu, Y.; Daoud, W.A.; Cheuk, K.K.L.; Lin, C.S.K. Newly developed techniques on polycondensation, ringopening polymerization and polymer modification: Focus on poly (lactic acid). Materials 2016, 9, 133. [Google Scholar] [CrossRef]
- Li, J.; Stayshich, R.M.; Meyer, T.Y. Exploiting Sequence To Control the Hydrolysis Behavior of Biodegradable PLGA Copolymers. J. Am. Chem. Soc. 2011, 133, 6910–6913. [Google Scholar] [CrossRef] [PubMed]
- Marszałek-Harych, A.; Jędrzkiewicz, D.; Ejfler, J. Bio- and chemocatalysis cascades as a bridge between biology and chemistry for green polymer synthesis. Cell. Mol. Biol. Lett. 2017, 22, 28. [Google Scholar] [CrossRef] [PubMed]
- Zeng, F.-R.; Liang, Y.; Li, Z.-L. Precision Aliphatic Polyesters via Segmer Assembly Polymerization. Molecules 2018, 23, 452. [Google Scholar] [CrossRef]
- Cameron, D.J.A.; Shaver, M.P. Aliphatic polyester polymer stars: Synthesis, properties and applications in biomedicine and nanotechnology. Chem. Soc. Rev. 2010, 40, 1761–1776. [Google Scholar] [CrossRef]
- Johnson, R.M.; Fraser, C.L. Metalloinitiation Routes to Biocompatible Poly(lactic acid) and Poly(acrylic acid) Stars with Luminescent Ruthenium Tris(bipyridine) Cores. Biomacromolecules 2004, 5, 580–588. [Google Scholar] [CrossRef] [PubMed]
- Barón, M.; Hellwich, K.-H.; Hess, M.; Horie, K.; Jenkins, A.D.; Jones, R.G.; Kahovec, J.; Kratochvíl, P.; Metanomski, W.V.; Mormann, W.; et al. Glossary of class names of polymers based on chemical structure and molecular architecture (IUPAC Recommendations 2009). Pure Appl. Chem. 2009, 81, 1131–1186. [Google Scholar] [CrossRef]
- Buwalda, S.J.; Dijkstra, P.J.; Feijen, J. In Situ Forming Poly (ethylene glycol)-Poly (l-lactide) Hydrogels via Michael Addition: Mechanical Properties, Degradation, and Protein Release. Macromol. Chem. Phys. 2012, 213, 766–775. [Google Scholar] [CrossRef]
- Velthoen, I.W.; Tijsma, E.J.; Dijkstra, P.J.; Feijen, J. Thermo-Responsive Hydrogels Based on Branched Poly(L-lactide)-poly(ethylene glycol) Copolymers. Macromol. Symp. 2008, 272, 13–27. [Google Scholar] [CrossRef]
- Salaam, L.E.; Dean, D.; Bray, T.L. In vitro degradation behaviour of biodegradable 4-star micelles. Polymer 2006, 47, 310–318. [Google Scholar] [CrossRef]
- Liu, M.-J.; Chen, S.-C.; Yang, K.-K.; Wang, Y.-Z. Biodegradable polylactide based materials with improved crystallinity, mechanical properties and rheological behaviour by introducing a long-chain branched copolymer. RSC Adv. 2015, 5, 42162–42173. [Google Scholar] [CrossRef]
- Song, C.X.; Feng, X.D. Synthesis of ABA triblock copolymers of iε-caprolactone and DL-lactide. Macromolecules 1984, 17, 2764–2767. [Google Scholar] [CrossRef]
- Jeong, S.I.; Kim, B.S.; Lee, Y.M.; Ihn, K.J.; Kim, S.H.; Kim, Y.H. Morphology of elastic poly (L-lactide-co-ε-caprolactone) copolymers and in vitro and in vivo degradation behavior of their scaf-folds. BioMacromolecules 2004, 5, 1303–1309. [Google Scholar] [CrossRef]
- Rozga-Wijas, K.; Stanczyk, W.A.; Kurjata, J.; Kazmierski, S. Star-shaped and linear POSS-polylactide hybrid copolymers. Materials 2015, 8, 4400–4420. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.; Ding, J.; Li, J.; Liu, Y.; Hao, J. Blends of poly (d, l-lactide) with polyhedral oligomeric silsesquioxanes-based biodegradable polyester: Synthesis, morphology, miscibility, and mechanical property. J. Appl. Polym. Sci. 2014, 131, 40776. [Google Scholar] [CrossRef]
- Zhang, W.; Wang, S.; Li, X.; Yuan, J.; Wang, S. Organic/inorganic hybrid star-shaped block copolymers of poly(l-lactide) and poly(N-isopropylacrylamide) with a polyhedral oligomeric silsesquioxane core: Synthesis and self-assembly. Eur. Polym. J. 2012, 48, 720–729. [Google Scholar] [CrossRef]
- Breitenbach, A.; Kissel, T. Biodegradable comb polyesters: Part 1 synthesis, characterization and structural analysis of poly (lactide) and poly (lactide-coglycolide) grafted onto water-soluble poly (vinyl alcohol) as backbone. Polymer 1998, 39, 3261–3271. [Google Scholar] [CrossRef]
- Wang, X.; Xie, X.; Cai, C.; Rytting, E.; Steele, T.; Kissel, T. Biodegradable branched polyesters poly (vinyl sulfonatecovinyl alcohol)-graft poly (D, L-lactic-coglycolic acid) as a negatively charged polyelectrolyte platform for drug delivery: Synthesis and characterization. Macromolecules 2008, 41, 2791–2799. [Google Scholar] [CrossRef]
- Bednarek, M. Branched aliphatic polyesters by ring-opening (co)polymerization. Prog. Polym. Sci. 2016, 58, 27–58. [Google Scholar] [CrossRef]
- Basko, M.; Bednarek, M.; Kubisa, P. Cationic copolymerization of L, L-lactide with hydroxyl substituted cyclic ethers. Polym. Adv. Technol. 2015, 26, 804–813. [Google Scholar] [CrossRef]
- Kubisa, P.; Penczek, S. Cationic activated monomer polymerization of heterocyclic monomers. Prog. Polym. Sci. 1999, 24, 1409–1437. [Google Scholar] [CrossRef]
- Tasaka, F.; Ohya, Y.; Ouchi, T. Synthesis of Novel Comb-Type Polylactide and Its Biodegradability. Macromolecules 2001, 34, 5494–5500. [Google Scholar] [CrossRef]
- Burke, J.F.; Yannas, I.V.; Quinby Jr, W.C.; Bondoc, C.C.; Jung, W.K. Successful use of a physiologically acceptable artificial skin in the treatment of extensive burn injury. Ann. Surg. 1981, 194, 413. [Google Scholar] [CrossRef] [PubMed]
- Lu, L.; Mikos, A.G. The Importance of New Processing Techniques in Tissue Engineering. MRS Bull. 1996, 21, 28–32. [Google Scholar] [CrossRef] [PubMed]
- Dhandayuthapani, B.; Yoshida, Y.; Maekawa, T.; Kumar, D.S. Polymeric Scaffolds in Tissue Engineering Application: A Review. Int. J. Polym. Sci. 2011, 2011, 290602. [Google Scholar] [CrossRef]
- Bajaj, P.; Schweller, R.M.; Khademhosseini, A.; West, J.L.; Bashir, R. 3D Biofabrication Strategies for Tissue Engineering and Regenerative Medicine. Annu. Rev. Biomed. Eng. 2014, 16, 247–276. [Google Scholar] [CrossRef]
- Brougham, C.M.; Levingstone, T.J.; Shen, N.; Cooney, G.M.; Jockenhoevel, S.; Flanagan, T.C.; O’Brien, F.J. Freeze-drying as a novel biofabrication method for achieving a controlled microarchitecture within large, complex natural biomaterial scaffolds. Adv. Healthc. Mater. 2017, 6, 1700598. [Google Scholar] [CrossRef]
- Mi, H.-Y.; Jing, X.; Napiwocki, B.N.; Li, Z.-T.; Turng, L.-S.; Huang, H.-X. Fabrication of fibrous silica sponges by self-assembly electrospinning and their application in tissue engineering for three-dimensional tissue regeneration. Chem. Eng. J. 2018, 331, 652–662. [Google Scholar] [CrossRef]
- Rogina, A. Electrospinning process: Versatile preparation method for biodegradable and natural polymers and bio-composite systems applied in tissue engineering and drug delivery. Appl. Surf. Sci. 2014, 296, 221–230. [Google Scholar] [CrossRef]
- Tsai, W.C.; Wang, Y. Progress of supercritical fluid technology in polymerization and its applications in biomedical engineering. Prog. Polym. Sci. 2019, 98, 101161. [Google Scholar] [CrossRef]
- Salerno, A.; Pascual, C.D. Bio-based polymers, supercritical fluids and tissue engineering. Process. Biochem. 2015, 50, 826–838. [Google Scholar] [CrossRef]
- Duarte, A.R.C.; Mano, J.F.; Reis, R.L. Supercritical fluids in biomedical and tissue engineering applications: A review. Int. Mater. Rev. 2009, 54, 214–222. [Google Scholar] [CrossRef]
- Sola, A.; Bertacchini, J.; D’Avella, D.; Anselmi, L.; Maraldi, T.; Marmiroli, S.; Messori, M. Development of solvent-casting particulate leaching (SCPL) polymer scaffolds as improved three-dimensional supports to mimic the bone marrow niche. Mater. Sci. Eng. C 2018, 96, 153–165. [Google Scholar] [CrossRef] [PubMed]
- Wahid, F.; Khan, T.; Hussain, Z.; Ullah, H. Nanocomposite scaffolds for tissue engineering; properties, preparation and applications. In Applications of Nanocomposite Materials in Drug Delivery; Woodhead Publishing: Sawston, Cambridge, 2018; pp. 701–735. [Google Scholar]
- Huang, R.; Zhu, X.; Tu, H.; Wan, A. The crystallization behavior of porous poly(lactic acid) prepared by modified solvent casting/particulate leaching technique for potential use of tissue engineering scaffold. Mater. Lett. 2014, 136, 126–129. [Google Scholar] [CrossRef]
- Mondal, S.; Nguyen, T.P.; Pham, V.H.; Hoang, G.; Manivasagan, P.; Kim, M.H.; Nam, S.Y.; Oh, J. Hydroxyapatite nano bioceramics optimized 3D printed poly lactic acid scaffold for bone tissue engineering application. Ceram. Int. 2020, 46, 3443–3455. [Google Scholar] [CrossRef]
- Gurunathan, T.; Mohanty, S.; Nayak, S.K. A review of the recent developments in biocomposites based on natural fibres and their application perspectives. Compos. Part A Appl. Sci. Manuf. 2015, 77, 1–25. [Google Scholar] [CrossRef]
- Agrahari, V.; Agrahari, V.; Chou, M.L.; Chew, C.H.; Noll, J.; Burnouf, T. Intelligent micro-/nanorobots as drug and cell carrier devices for biomedical therapeutic advancement: Promising development opportunities and translational challenges. Biomaterials 2020, 260, 120163. [Google Scholar] [CrossRef]
- Shen, S.; Wu, Y.; Liu, Y.; Wu, D. High drug-loading nanomedicines: Progress, current status, and prospects. Int. J. Nanomed. 2017, 12, 4085–4109. [Google Scholar] [CrossRef]
- Saini, P.; Arora, M.; Ravi Kumar, M.N.V. Poly(lactic acid) blends in biomedical applications. Adv. Drug Deliv. Rev. 2016, 107, 47–59. [Google Scholar] [CrossRef]
- Senapati, S.; Mahanta, A.K.; Kumar, S.; Maiti, P. Controlled drug delivery vehicles for cancer treatment and their performance. Signal Transduct. Target. Ther. 2018, 3, 7. [Google Scholar] [CrossRef]
- Tyler, B.; Gullotti, D.; Mangraviti, A.; Utsuki, T.; Brem, H. Polylactic acid (PLA) controlled delivery carriers for biomedical applications. Adv. Drug Deliv. Rev. 2016, 107, 163–175. [Google Scholar] [CrossRef]
- Shishir, M.R.I.; Xie, L.; Sun, C.; Zheng, X.; Chen, W. Advances in micro and nano-encapsulation of bioactive compounds using biopolymer and lipid-based transporters. Trends Food Sci. Technol. 2018, 78, 34–60. [Google Scholar] [CrossRef]
- Nahar, M.; Dutta, T.; Murugesan, S.; Asthana, A.; Mishra, D.; Rajkumar, V.; Tare, M.; Saraf, S.; Jain, N.K. Functional Polymeric Nanoparticles: An Efficient and Promising Tool for Active Delivery of Bioactives. Crit. Rev. Ther. Drug Carr. Syst. 2006, 23, 259–318. [Google Scholar] [CrossRef] [PubMed]
- Bhatia, S. Nanoparticles Types, Classification, Characterization, Fabrication Methods and Drug Delivery Applications. In Natural Polymer Drug Delivery Systems: Nanoparticles, Plants, and Algae; Bhatia, S., Ed.; Springer International Publishing: Cham, Switzerlands, 2016; pp. 33–93. [Google Scholar] [CrossRef]
- Wong, C.Y.; Al-Salami, H.; Dass, C.R. Microparticles, microcapsules and microspheres: A review of recent developments and prospects for oral delivery of insulin. Int. J. Pharm. 2018, 537, 223–244. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Wang, J.; Wu, W.; Tony To, S.S.; Zhao, H.; Wang, J. Advances in lipid-based drug delivery: Enhancing efficiency for hydrophobic drugs. Expert Opin. Drug Deliv. 2015, 12, 1475–1499. [Google Scholar] [CrossRef]
- Siegel, R.A. Stimuli sensitive polymers and self regulated drug delivery systems: A very partial review. J. Control. Release 2014, 190, 337–351. [Google Scholar] [CrossRef]
- Blasi, P. Poly (lactic acid)/poly (lactic-co-glycolic acid)-based microparticles: An overview. J. Pharm. Investig. 2019, 49, 337–346. [Google Scholar] [CrossRef]
- Vishwakarma, A.; Bhise, N.S.; Evangelista, M.B.; Rouwkema, J.; Dokmeci, M.R.; Ghaemmaghami, A.M.; Vrana, N.E.; Khademhosseini, A. Engineering Immunomodulatory Biomaterials to Tune the Inflammatory Response. Trends Biotechnol. 2016, 34, 470–482. [Google Scholar] [CrossRef]
- Goor, O.J.; Hendrikse, S.I.; Dankers, P.Y.; Meijer, E.W. From supramolecular polymers to multi-component biomaterials. Chem. Soc. Rev. 2017, 46, 6621–6637. [Google Scholar] [CrossRef]
- Ogueri, K.S.; Jafari, T.; Ivirico, J.L.E.; Laurencin, C.T. Polymeric Biomaterials for Scaffold-Based Bone Regenerative Engineering. Regen. Eng. Transl. Med. 2018, 5, 128–154. [Google Scholar] [CrossRef]
- Srivastava, P.; Hira, S.K.; Paladhi, A.; Singh, R.; Gupta, U.; Srivastava, D.N.; Manna, P.P. Studies on interaction po-tency model based on drug synergy and therapeutic potential of triple stimuli-responsive delivery of doxorubicin and 5-fluoro-2-deoxyuridine against lymphoma using disulfide-bridged cysteine over mesoporous silica nanoparticles. J. Mater. Chem. B 2020, 8, 1411–1421. [Google Scholar] [CrossRef]
- Miao, T.; Wang, J.; Zeng, Y.; Liu, G.; Chen, X. Polysaccharide-Based Controlled Release Systems for Therapeutics Delivery and Tissue Engineering: From Bench to Bedside. Adv. Sci. 2018, 5, 1700513. [Google Scholar] [CrossRef] [PubMed]
- Askari, E.; Seyfoori, A.; Amereh, M.; Gharaie, S.S.; Ghazali, H.S.; Ghazali, Z.S.; Khunjush, B.; Akbari, M. Stimuli-Responsive Hydrogels for Local Post-Surgical Drug Delivery. Gels 2020, 6, 14. [Google Scholar] [CrossRef] [PubMed]
- Yadav, M.; Paritosh, K.; Pareek, N.; Vivekanand, V. Composites based on bioderived polymers: Potential role in tissue engineering: Vol VI: Resorbable polymer fibers. Mater. Biomed. Eng. 2019, 259–296. [Google Scholar] [CrossRef]
- Li, R.; Peng, F.; Cai, J.; Yang, D.; Zhang, P. Redox dual-stimuli responsive drug delivery systems for improving tumor-targeting ability and reducing adverse side effects. Asian J. Pharm. Sci. 2020, 15, 311–325. [Google Scholar] [CrossRef] [PubMed]
- Lavrador, P.; Esteves, M.R.; Gaspar, V.M.; Mano, J.F. Stimuli-Responsive Nanocomposite Hydrogels for Biomedical Applications. Adv. Funct. Mater. 2020, 31, 2005941. [Google Scholar] [CrossRef]
- Fu, X.; Hosta-Rigau, L.; Chandrawati, R.; Cui, J. Multi-Stimuli-Responsive Polymer Particles, Films, and Hydrogels for Drug Delivery. Chem 2018, 4, 2084–2107. [Google Scholar] [CrossRef]
- Cheng, H.; Chawla, A.; Yang, Y.; Li, Y.; Zhang, J.; Jang, H.L.; Khademhosseini, A. Development of nanomaterials for bone-targeted drug delivery. Drug Discov. Today 2017, 22, 1336–1350. [Google Scholar] [CrossRef]
- Pellis, A.; Silvestrini, L.; Scaini, D.; Coburn, J.M.; Gardossi, L.; Kaplan, D.L.; Acero, E.H.; Guebitz, G.M. Enzyme-catalyzed functionalization of poly(L-lactic acid) for drug delivery applications. Process. Biochem. 2017, 59, 77–83. [Google Scholar] [CrossRef]
- Maghsoudi, S.; Shahraki, B.T.; Rabiee, N.; Fatahi, Y.; Dinarvand, R.; Tavakolizadeh, M.; Ahmadi, S.; Rabiee, M.; Bagherzadeh, M.; Pourjavadi, A.; et al. Burgeoning Polymer Nano Blends for Improved Controlled Drug Release: A Review. Int. J. Nanomed. 2020, 15, 4363–4392. [Google Scholar] [CrossRef]
- Prasad, M.; Ghosh, M.; Kumar, R.; Brar, B.; Surjith, K.P.; Lambe, U.P.; Ranjan, K.; Banerjee, S.; Prasad, G.; Khurana, S.K.; et al. The Importance of Nanomedicine in Prophylactic and Theranostic Intervention of Bacterial Zoonoses and Reverse Zoonoses in the Era of Microbial Resistance. J. Nanosci. Nanotechnol. 2021, 21, 3404–3452. [Google Scholar] [CrossRef]
- Tian, L.; Tang, N.; Ngai, T.; Wu, C.; Ruan, Y.; Huang, L.; Qin, L. Hybrid fracture fixation systems developed for orthopaedic applications: A general review. J. Orthop. Transl. 2019, 16, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Manam, N.S.; Harun, W.S.W.; Shri, D.N.A.; Ghani, S.A.C.; Kurniawan, T.; Ismail, M.H.; Ibrahim, M.H.I. Study of corrosion in biocompatible metals for implants: A review. J. Alloys Compd. 2017, 701, 698–715. [Google Scholar] [CrossRef]
- Chindamo, G.; Sapino, S.; Peira, E.; Chirio, D.; Gonzalez, M.C.; Gallarate, M. Bone Diseases: Current Approach and Future Perspectives in Drug Delivery Systems for Bone Targeted Therapeutics. Nanomaterials 2020, 10, 875. [Google Scholar] [CrossRef]
- Da Silva, D.; Kaduri, M.; Poley, M.; Adir, O.; Krinsky, N.; Shainsky-Roitman, J.; Schroeder, A. Biocompatibility, biodegradation and excretion of polylactic acid (PLA) in medical implants and theranostic systems. Chem. Eng. J. 2018, 340, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Sheikh, Z.; Najeeb, S.; Khurshid, Z.; Verma, V.; Rashid, H.; Glogauer, M. Biodegradable Materials for Bone Repair and Tissue Engineering Applications. Materials 2015, 8, 5744–5794. [Google Scholar] [CrossRef] [PubMed]
- Torres-Luna, C.; Fan, X.; Domszy, R.; Hu, N.; Wang, N.S.; Yang, A. Hydrogel-based ocular drug delivery systems for hydrophobic drugs. Eur. J. Pharm. Sci. 2020, 154, 105503. [Google Scholar] [CrossRef]
- Budama-Kilinc, Y.; Cakir-Koc, R.; Kurt, I.; Gozutok, K.; Ozkan, B.; Ozkan, B.; Isildak, I. Polymer-Based Biocomposites. Biomater. Tissue Eng. 2017, 4, 49–89. [Google Scholar]
- Lim, K.S.; Park, J.K.; Jeong, M.H.; Bae, I.H.; Nah, J.W.; Park, D.S.; Kang, J.C. Effect of stents coated with a combination of sirolimus and alpha-lipoic acid in a porcine coronary restenosis model. J. Mater. Sci. Mater. Med. 2016, 27, 66. [Google Scholar] [CrossRef]
- Haroosh, H.J.; Dong, Y.; Lau, K.T. Tetracycline hydrochloride (TCH)-loaded drug carrier based on PLA: PCL nan-ofibre mats: Experimental characterisation and release kinetics modelling. J. Mater. Sci. 2014, 49, 6270–6281. [Google Scholar] [CrossRef]
- Son, J.S.; Hwang, E.J.; Kwon, L.S.; Ahn, Y.G.; Moon, B.K.; Kim, J.; Lee, S.Y. Antibacterial Activity of Propo-lis-Embedded Zeolite Nanocomposites for Implant Application. Materials 2021, 14, 1193. [Google Scholar] [CrossRef]
- Ramachandran, R.; Junnuthula, V.R.; Gowd, G.S.; Ashokan, A.; Thomas, J.; Peethambaran, R.; Thomas, A.; Unni, A.K.K.; Panikar, D.; Nair, S.V.; et al. Theranostic 3-Dimensional nano brain-implant for prolonged and localized treatment of recurrent glioma. Sci. Rep. 2017, 7, srep43271. [Google Scholar] [CrossRef]
- Nagam Hanumantharao, S.; Rao, S. Multi-functional electrospun nanofibers from polymer blends for scaffold tissue engineering. Fibers 2019, 7, 66. [Google Scholar] [CrossRef]
- Narayanan, G.; Vernekar, V.N.; Kuyinu, E.L.; Laurencin, C.T. Poly (lactic acid)-based biomaterials for orthopaedic regenerative engineering. Adv. Drug Deliv. Rev. 2016, 107, 247–276. [Google Scholar] [CrossRef] [PubMed]
- Krlová, K.; Malachová, K.; Muñoz-Bonilla, A.; Měřinská, D.; Rybková, Z.; Fernández-García, M.; Plachá, D. Biocompatible polymer materials with antimicrobial properties for preparation of stents. Nanomaterials 2019, 9, 1548. [Google Scholar] [CrossRef] [PubMed]
- Kelly, D.C.; Raftery, R.M.; Curtin, C.M.; O’Driscoll, C.M.; O’Brien, F.J. Scaffold-Based Delivery of Nucleic Acid Therapeutics for Enhanced Bone and Cartilage Repair. J. Orthop. Res. 2019, 37, 1671–1680. [Google Scholar] [CrossRef]
- Thompson, E.M.; Matsiko, A.; Kelly, D.J.; Gleeson, J.P.; O’Brien, F.J. An Endochondral Ossification-Based Approach to Bone Repair: Chondrogenically Primed Mesenchymal Stem Cell-Laden Scaffolds Support Greater Repair of Critical-Sized Cranial Defects Than Osteogenically Stimulated Constructs In Vivo. Tissue Eng. Part A 2016, 22, 556–567. [Google Scholar] [CrossRef]
- Sukegawa, S.; Kanno, T.; Matsumoto, K.; Sukegawa-Takahashi, Y.; Masui, M.; Furuki, Y. Complications of a poly-l-lactic acid and polyglycolic acid osteosynthesis device for internal fixation in maxillofacial surgery. Odontology 2018, 106, 360–368. [Google Scholar] [CrossRef]
- Zhang, C.; Wang, L.; Zhai, T.; Wang, X.; Dan, Y.; Turng, L.-S. The surface grafting of graphene oxide with poly(ethylene glycol) as a reinforcement for poly(lactic acid) nanocomposite scaffolds for potential tissue engineering applications. J. Mech. Behav. Biomed. Mater. 2016, 53, 403–413. [Google Scholar] [CrossRef]
- Abdal-Hay, A.; Hussein, K.H.; Casettari, L.; Khalil, K.A.; Hamdy, A.S. Fabrication of novel high performance ductile poly(lactic acid) nanofiber scaffold coated with poly(vinyl alcohol) for tissue engineering applications. Mater. Sci. Eng. C 2016, 60, 143–150. [Google Scholar] [CrossRef]
- Santoro, M.; Shah, S.R.; Walker, J.L.; Mikos, A.G. Poly(lactic acid) nanofibrous scaffolds for tissue engineering. Adv. Drug Deliv. Rev. 2016, 107, 206–212. [Google Scholar] [CrossRef]
- Zhang, C.; Salick, M.R.; Cordie, T.M.; Ellingham, T.; Dan, Y.; Turng, L.S. Incorporation of poly (ethylene glycol) grafted cellulose nanocrystals in poly (lactic acid) electrospun nanocomposite fibers as potential scaffolds for bone tissue en-gineering. Mater. Sci. Eng. C 2015, 49, 463–471. [Google Scholar] [CrossRef] [PubMed]
- Kucinska-Lipka, J.; Gubańska, I.C.; Janik, H.; Sienkiewicz, M. Fabrication of polyurethane and polyurethane based composite fibres by the electrospinning technique for soft tissue engineering of cardiovascular system. Mater. Sci. Eng. C 2015, 46, 166–176. [Google Scholar] [CrossRef] [PubMed]
- Eftekhari, A.; Dizaj, S.M.; Sharifi, S.; Salatin, S.; Saadat, Y.R.; Vahed, S.Z.; Samiei, M.; Ardalan, M.; Rameshrad, M.; Ahmadian, E.; et al. The Use of Nanomaterials in Tissue Engineering for Cartilage Regeneration; Current Approaches and Future Perspectives. Int. J. Mol. Sci. 2020, 21, 536. [Google Scholar] [CrossRef]
- Shim, I.K.; Jung, M.R.; Kim, K.H.; Seol, Y.J.; Park, Y.J.; Park, W.H.; Lee, S.J. Novel three-dimensional scaffolds of poly(L-lactic acid) microfibers using electrospinning and mechanical expansion: Fabrication and bone regeneration. J. Biomed. Mater. Res. Part B Appl. Biomater. 2010, 95B, 150–160. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Lee, H.; Cheon, K.H.; Park, C.; Jang, T.S.; Kim, H.E.; Jung, H.D. Fabrication of poly (lactic acid)/Ti composite scaffolds with enhanced mechanical properties and biocompatibility via fused filament fabrication (FFF)–based 3D printing. Addit. Manuf. 2019, 30, 100883. [Google Scholar] [CrossRef]
- Nabilla, F.; Widiyanti, P.; Hikmawati, D. Fabrication and Characterizations of Gelatin/Chitosan with Aloe Vera and Achatina Fulica sp Mucus as Scaffold for Skin Tissue Engineering. J. Teknol. 2019, 81, 51–57. [Google Scholar] [CrossRef]
- Ritz, U.; Gerke, R.; Götz, H.; Stein, S.; Rommens, P.M. A New Bone Substitute Developed from 3D-Prints of Polylactide (PLA) Loaded with Collagen I: An In Vitro Study. Int. J. Mol. Sci. 2017, 18, 2569. [Google Scholar] [CrossRef]
- Zhang, H.; Mao, X.; Du, Z.; Jiang, W.; Han, X.; Zhao, D.; Li, Q. Three dimensional printed macroporous polylactic ac-id/hydroxyapatite composite scaffolds for promoting bone formation in a critical-size rat calvarial defect model. Sci. Technol. Adv. Mater. 2016, 17, 136–148. [Google Scholar] [CrossRef]
- Zhang, H.; Mao, X.; Zhao, D.; Jiang, W.; Du, Z.; Li, Q.; Han, D. Three dimensional printed polylactic ac-id-hydroxyapatite composite scaffolds for prefabricating vascularized tissue engineered bone: An in vivo bioreactor model. Sci. Rep. 2017, 7, 15255. [Google Scholar] [CrossRef]
- Jaidev, L.R.; Chatterjee, K. Surface functionalization of 3D printed polymer scaffolds to augment stem cell response. Mater. Des. 2019, 161, 44–54. [Google Scholar] [CrossRef]
- Yeon, Y.K.; Park, H.S.; Lee, J.M.; Lee, J.S.; Lee, Y.J.; Sultan, M.T.; Park, C.H. New concept of 3D printed bone clip (polylactic acid/hydroxyapatite/silk composite) for internal fixation of bone fractures. J. Biomater. Sci. Polym. Ed. 2018, 29, 894–906. [Google Scholar] [CrossRef] [PubMed]
- Mauney, J.R.; Nguyen, T.; Gillen, K.; Kirker-Head, C.; Gimble, J.M.; Kaplan, D.L. Engineering adipose-like tissue in vitro and in vivo utilizing human bone marrow and adipose-derived mesenchymal stem cells with silk fibroin 3D scaffolds. Biomaterials 2009, 28, 5280–5290. [Google Scholar] [CrossRef] [PubMed]
- Park, S.Y.; Ki, C.S.; Park, Y.H.; Jung, H.M.; Woo, K.M.; Kim, H.J. Electrospun Silk Fibroin Scaffolds with Macropores for Bone Regeneration: An In Vitro and In Vivo Study. Tissue Eng. Part A 2010, 16, 1271–1279. [Google Scholar] [CrossRef] [PubMed]
- Mandal, B.B.; Grinberg, A.; Gil, E.S.; Panilaitis, B.; Kaplan, D.L. High-strength silk protein scaffolds for bone repair. Proc. Natl. Acad. Sci. USA 2012, 109, 7699–7704. [Google Scholar] [CrossRef] [PubMed]
- Soudi, A.; Yazdanian, M.; Ranjbar, R.; Tebyanian, H.; Yazdanian, A.; Tahmasebi, E.; Keshvad, A.; Seifalian, A. Role and application of stem cells in dental regeneration: A comprehensive overview. Excli J. 2021, 20, 454. [Google Scholar]
- Hussain, A.; Tebyaniyan, H.; Khayatan, D. The Role of Epigenetic in Dental and Oral Regenerative Medicine by Different Types of Dental Stem Cells: A Comprehensive Overview. Stem Cells Int. 2022, 2022, 5304860. [Google Scholar] [CrossRef]
- Boro, U.; Kashyap, N.; Moholkar, V.S. Sonochemical Synthesis of Poly(lactic acid) Nanocomposites with ZnO Nanoflowers: Effect of Nanofiller Morphology on Physical Properties. ACS Eng. Au 2021, 2, 46–60. [Google Scholar] [CrossRef]
- Fattahi, F.S.; Khoddami, A.; Avinc, O. Poly (lactic acid) (PLA) nanofibers for bone tissue engineering. J. Text. Polym. 2019, 7, 47–64. [Google Scholar]
- Fattahi, F.S. Poly (lactic acid) nano-structures for cartilage regeneration and joint repair: Strategies and ideas. Recent Trends Nanosci. Technol. 2020, 1, 1–19. [Google Scholar]
- Cao, H.; Chen, M.-M.; Liu, Y.; Liu, Y.-Y.; Huang, Y.-Q.; Wang, J.-H.; Chen, J.-D.; Zhang, Q.-Q. Fish collagen-based scaffold containing PLGA microspheres for controlled growth factor delivery in skin tissue engineering. Colloids Surf. B Biointerfaces 2015, 136, 1098–1106. [Google Scholar] [CrossRef]
- Sha, L.; Chen, Z.; Chen, Z.; Zhang, A.; Yang, Z. Polylactic Acid Based Nanocomposites: Promising Safe and Biodegradable Materials in Biomedical Field. Int. J. Polym. Sci. 2016, 2016, 6869154. [Google Scholar] [CrossRef]
- Erten, E.; Arslan, Y.E. The Great Harmony in Translational Medicine: Biomaterials and Stem Cells. Adv. Exp. Med. Biol. 2018, 1119, 21–39. [Google Scholar] [CrossRef] [PubMed]
- Yan, C.; Ren, Y.; Sun, X.; Jin, L.; Liu, X.; Chen, H.; Wang, K.; Yu, M.; Zhao, Y. Photoluminescent functionalized carbon quantum dots loaded electroactive Silk fibroin/PLA nanofibrous bioactive scaffolds for cardiac tissue engineering. J. Photochem. Photobiol. B Biol. 2019, 202, 111680. [Google Scholar] [CrossRef] [PubMed]
- Yang, R.; Hou, E.; Cheng, W.; Yan, X.; Zhang, T.; Li, S.; Yao, H.; Liu, J.; Guo, Y. Membrane-Targeting Neolignan-Antimicrobial Peptide Mimic Conjugates to Combat Methicillin-Resistant Staphylococcus aureus (MRSA) Infections. J. Med. Chem. 2022, 65, 24. [Google Scholar] [CrossRef]
- Zhang, W.; Guan, X.; Qiu, X.; Gao, T.; Yu, W.; Zhang, M.; Song, L.; Liu, D.; Dong, J.; Jiang, Z. Bioactive composite Janus nanofibrous membranes loading Ciprofloxacin and Astaxanthin for enhanced healing of full-thickness skin defect wounds. Appl. Surf. Sci. 2023, 610, 155290. [Google Scholar] [CrossRef]
- Li, J.; Zhao, J.; Tan, T.; Liu, M.; Zeng, Z.; Zeng, Y.; Zhang, L.; Fu, C.; Chen, D.; Xie, T. Nanoparticle Drug Delivery System for Glioma and Its Efficacy Improvement Strategies: A Comprehensive Review. Int. J. Nanomed. 2020, 15, 2563–2582. [Google Scholar] [CrossRef]
- Shi, Y.; Li, L. Current advances in sustained-release systems for parenteral drug delivery. Expert Opin. Drug Deliv. 2005, 2, 1039–1058. [Google Scholar] [CrossRef]
- Sun, S.-J.; Deng, P.; Peng, C.-E.; Ji, H.-Y.; Mao, L.-F.; Peng, L.-Z. Extraction, Structure and Immunoregulatory Activity of Low Molecular Weight Polysaccharide from Dendrobium officinale. Polymers 2022, 14, 2899. [Google Scholar] [CrossRef]
- Pan, Z.-Y.; Zhong, H.-J.; Huang, D.-N.; Wu, L.-H.; He, X.-X. Beneficial Effects of Repeated Washed Microbiota Transplantation in Children With Autism. Front. Pediatr. 2022, 10, 928785. [Google Scholar] [CrossRef]
- Chen, X.; Chen, J.; Li, B.; Yang, X.; Zeng, R.; Liu, Y.; Li, T.; Ho, R.J.; Shao, J. PLGA-PEG-PLGA triblock copolymeric micelles as oral drug delivery system: In vitro drug release and in vivo pharmacokinetics assessment. J. Colloid Interface Sci. 2017, 490, 542–552. [Google Scholar] [CrossRef]
- Chen, L.; Xie, Z.; Hu, J.; Chen, X.; Jing, X. Enantiomeric PLA–PEG block copolymers and their stereocomplex micelles used as rifampin delivery. J. Nanopart. Res. 2006, 9, 777–785. [Google Scholar] [CrossRef]
- Chen, S.; Singh, J. In vitro release of levonorgestrel from phase sensitive and thermosensitive smart polymer delivery systems. Pharm. Dev. Technol. 2005, 10, 319–325. [Google Scholar] [CrossRef] [PubMed]
- Danafar, H.; Rostamizadeh, K.; Davaran, S.; Hamidi, M. PLA-PEG-PLA copolymer-based polymersomes as nanocarriers for delivery of hydrophilic and hydrophobic drugs: Preparation and evaluation with atorvastatin and lisinopril. Drug Dev. Ind. Pharm. 2014, 40, 1411–1420. [Google Scholar] [CrossRef] [PubMed]
- Kelly, J.M.; Gross, A.L.; Martin, D.R.; E Byrne, M. Polyethylene glycol-b-poly(lactic acid) polymersomes as vehicles for enzyme replacement therapy. Nanomedicine 2017, 12, 2591–2606. [Google Scholar] [CrossRef]
- Ahmad, A.; Banat, F.; Taher, H. A review on the lactic acid fermentation from low-cost renewable materials: Recent developments and challenges. Environ. Technol. Innov. 2020, 20, 101138. [Google Scholar] [CrossRef]
- Bernardo, P.; Jansen, J.C.; Bazzarelli, F.; Tasselli, F.; Fuoco, A.; Friess, K.; Izák, P.; Jarmarová, V.; Kačírková, M.; Clarizia, G. Gas transport properties of Pebax®/room temperature ionic liquid gel membranes. Sep. Purif. Technol. 2012, 97, 73–82. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).