New Class of Anti-Inflammatory Therapeutics Based on Gold (III) Complexes in Intestinal Inflammation–Proof of Concept Based on In Vitro and In Vivo Studies
Abstract
:1. Introduction
2. Results
2.1. Characterization of TGS 121
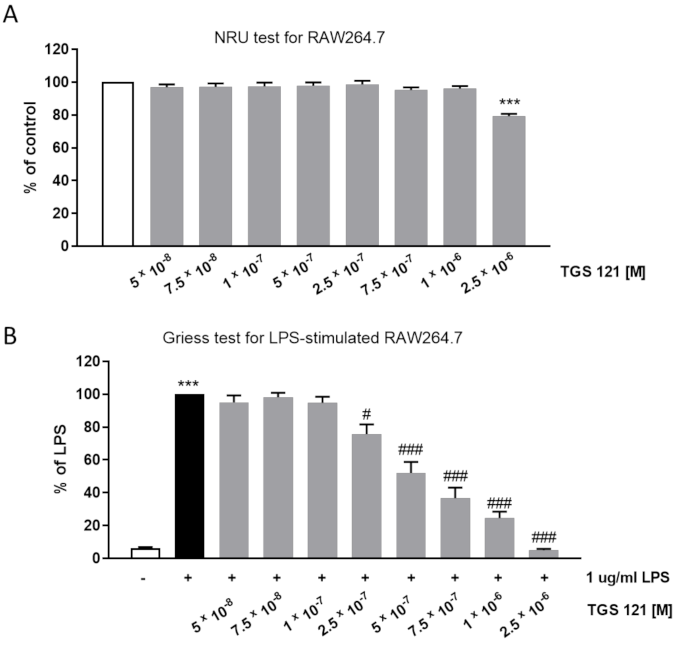
2.2. TGS 121 Showed an Anti-Inflammatory Profile In Vitro in RAW264.7 Macrophages
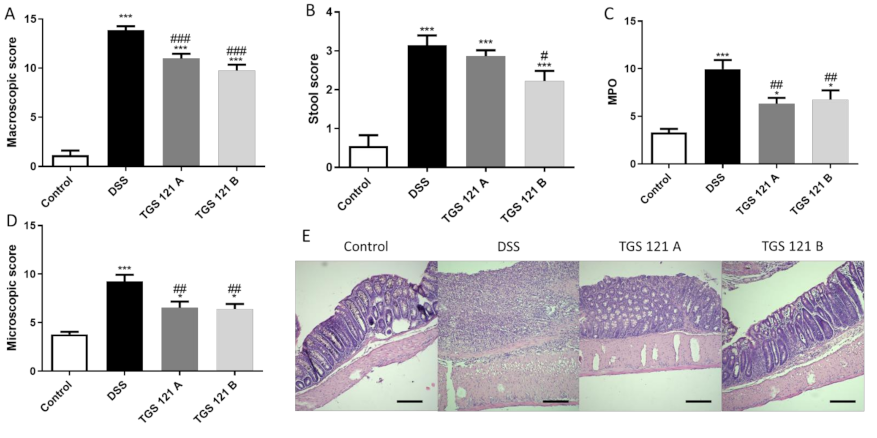
2.3. TGS 121 Attenuated Colitis in DSS-Induced Mouse Model
2.4. TGS 121 Influenced the Antioxidant Profile in the Mouse Colon
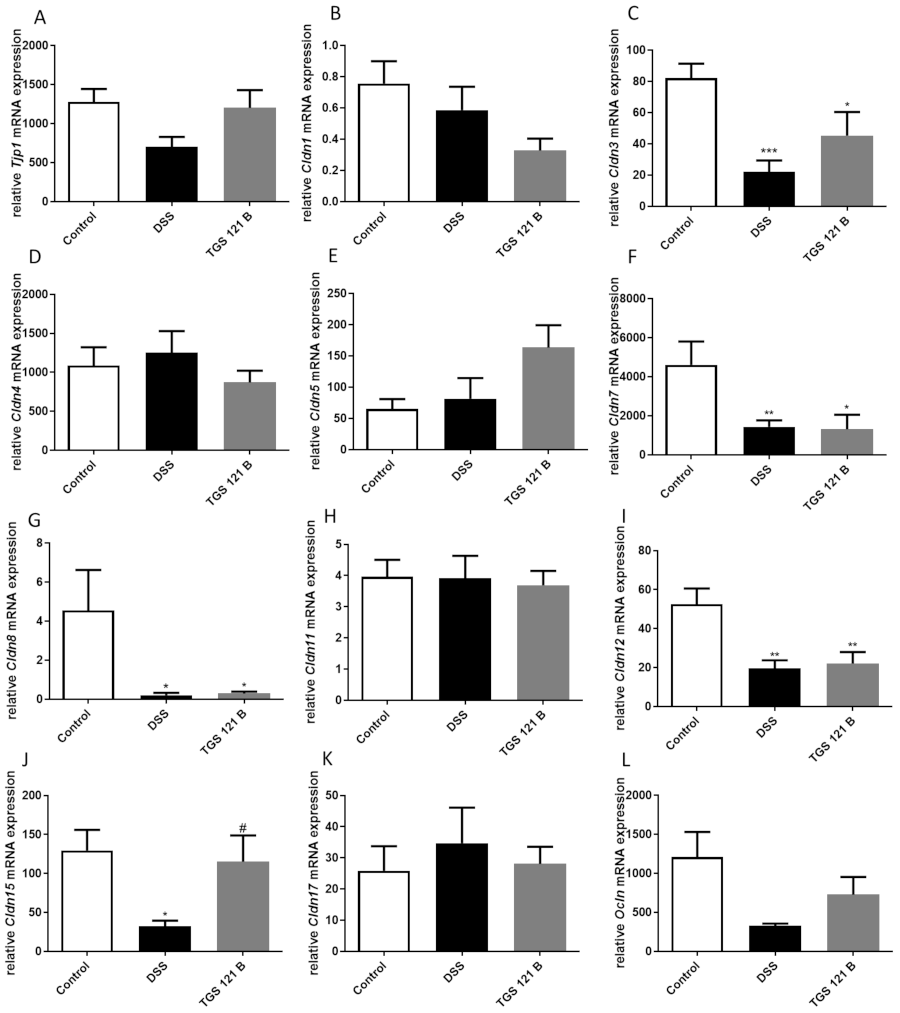
2.5. TGS 121 Induced Changes in the Tight Junction Complexes Expression
3. Discussion
4. Materials and Methods
4.1. Synthesis of TGS 121
4.2. Other Drugs and Reagents
4.3. Cell Line Culture
4.4. Cytotoxicity Assessment
4.5. Griess Assay
4.6. Animals
4.7. Induction of Colitis
4.8. Pharmacological Treatment
4.9. Evaluation of Colonic Damage
4.10. Microscopic Score Evaluation
4.11. Determination of Tissue Myeloperoxidase Activity
4.12. Oxidative Measurements
4.13. Assessment of Tight Junction Complexes Expression
4.13.1. RNA Isolation
4.13.2. Reverse Transcription and Real-Time PCR
4.14. Statistical Analysis
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Guo, J.; Rahme, K.; He, Y.; Li, L.L.; Holmes, J.D.; O’Driscoll, C.M. Gold nanoparticles enlighten the future of cancer theranostics. Int. J. Nanomedicine 2017, 12, 6131–6152. [Google Scholar] [CrossRef] [Green Version]
- Aminabad, N.S.; Farshbaf, M.; Akbarzadeh, A. Recent Advances of Gold Nanoparticles in Biomedical Applications: State of the Art. Cell Biochem. Biophys. 2019, 77, 123–137. [Google Scholar] [CrossRef]
- Singh, P.; Pandit, S.; Mokkapati, V.R.S.S.; Garg, A.; Ravikumar, V.; Mijakovic, I. Gold nanoparticles in diagnostics and therapeutics for human cancer. Int. J. Mol. Sci. 2018, 19, 1979. [Google Scholar] [CrossRef]
- Sztandera, K.; Gorzkiewicz, M.; Klajnert-Maculewicz, B. Gold Nanoparticles in Cancer Treatment. Mol. Pharm. 2019, 16, 1–23. [Google Scholar] [CrossRef]
- de Araújo, R.F.; de Araújo, A.A.; Pessoa, J.B.; Freire Neto, F.P.; da Silva, G.R.; Leitão Oliveira, A.L.C.S.; de Carvalho, T.G.; Silva, H.F.O.; Eugênio, M.; Sant’Anna, C.; et al. Anti-inflammatory, analgesic and anti-tumor properties of gold nanoparticles. Pharmacol. Reports 2017, 69, 119–129. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.A.; Khan, M.J. Nano-gold displayed anti-inflammatory property via NF-kB pathways by suppressing COX-2 activity. Artif. Cells Nanomedicine Biotechnol. 2018, 46, 1149–1158. [Google Scholar] [CrossRef] [Green Version]
- Gao, W.; Wang, Y.; Xiong, Y.; Sun, L.; Wang, L.; Wang, K.; Lu, H.Y.; Bao, A.; Turvey, S.E.; Li, Q.; et al. Size-dependent anti-inflammatory activity of a peptide-gold nanoparticle hybrid in vitro and in a mouse model of acute lung injury. Acta Biomater. 2019, 85, 203–217. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Zhang, H.; Sun, L.; Gao, W.; Xiong, Y.; Ma, A.; Liu, X.; Shen, L.; Li, Q.; Yang, H. Manipulation of macrophage polarization by peptide-coated gold nanoparticles and its protective effects on acute lung injury. J. Nanobiotechnol. 2020, 18, 38. [Google Scholar] [CrossRef] [Green Version]
- Bertrand, B.; Williams, M.R.M.; Bochmann, M. Gold(III) Complexes for Antitumor Applications: An Overview. Chem. A Eur. J. 2018, 24, 11840–11851. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.H.; Reeder, E.; Parkin, S.; Awuah, S.G. Gold(I/III)-Phosphine Complexes as Potent Antiproliferative Agents. Sci. Rep. 2019, 9, 12335. [Google Scholar] [CrossRef] [PubMed]
- Gomes, S.Q.; Vitoriano, L.; de Arruda, E.G.R.; Ruiz, A.L.T.G.; Candido, T.; de Carvalho, J.E.; Lustri, W.R.; Abbehausen, C. Linear gold(I) complex with tris-(2-carboxyethyl)phosphine (TCEP): Selective antitumor activity and inertness toward sulfur proteins. J. Inorg. Biochem. 2018, 186, 104–115. [Google Scholar] [CrossRef] [PubMed]
- Mármol, I.; Virumbrales-Muñoz, M.; Quero, J.; Sánchez-de-Diego, C.; Fernández, L.; Ochoa, I.; Cerrada, E.; Yoldi, M.J.R. Alkynyl gold(I) complex triggers necroptosis via ROS generation in colorectal carcinoma cells. J. Inorg. Biochem. 2017, 176, 123–133. [Google Scholar] [CrossRef] [Green Version]
- Trommenschlager, A.; Chotard, F.; Bertrand, B.; Amor, S.; Richard, P.; Bettaïeb, A.; Paul, C.; Connat, J.L.; Le Gendre, P.; Bodio, E. Gold(I)–Coumarin–Caffeine-Based Complexes as New Potential Anti-Inflammatory and Anticancer Trackable Agents. ChemMedChem 2018, 13, 2408–2414. [Google Scholar] [CrossRef] [PubMed]
- Frank Shaw, C. Gold-Based Therapeutic Agents. Chem. Rev. 1999, 99, 2589–2600. [Google Scholar] [CrossRef] [PubMed]
- Zou, T.; Lum, C.T.; Lok, C.N.; Zhang, J.J.; Che, C.M. Chemical biology of anticancer gold(III) and gold(i) complexes. Chem. Soc. Rev. 2015, 44, 8786–8801. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Selvaraju, K.; Saei, A.A.; D’Arcy, P.; Zubarev, R.A.; Arnér, E.S.; Linder, S. Repurposing of auranofin: Thioredoxin reductase remains a primary target of the drug. Biochimie 2019, 162, 46–54. [Google Scholar] [CrossRef]
- AbdelKhalek, A.; Abutaleb, N.S.; Mohammad, H.; Seleem, M.N. Antibacterial and antivirulence activities of auranofin against Clostridium difficile. Int. J. Antimicrob. Agents 2019, 53, 54–62. [Google Scholar] [CrossRef]
- AbdelKhalek, A.; Abutaleb, N.S.; Elmagarmid, K.A.; Seleem, M.N. Repurposing auranofin as an intestinal decolonizing agent for vancomycin-resistant enterococci. Sci. Rep. 2018, 8, 8353. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Krajewska, J.B.; Długosz, O.; Sałaga, M.; Banach, M.; Fichna, J. Silver nanoparticles based on blackcurrant extract show potent anti-inflammatory effect in vitro and in DSS-induced colitis in mice. Int. J. Pharm. 2020, 585, 119549. [Google Scholar] [CrossRef] [PubMed]
- Trávníček, Z.; Štarha, P.; Vančo, J.; Šilha, T.; Hošek, J.; Suchý, P.; Pražanová, G. Anti-inflammatory active gold(I) complexes involving 6-substituted-purine derivatives. J. Med. Chem. 2012, 55, 4568–4579. [Google Scholar] [CrossRef] [PubMed]
- Vančo, J.; Gálikova, J.; Hošek, J.; Dvořák, Z.; Paráková, L.; Travníček, Z. Gold(I) complexes of 9-deazahypoxanthine as selective antitumor and anti-inflammatory agents. PLoS ONE 2014, 9, e109901. [Google Scholar] [CrossRef] [PubMed]
- Křikavová, R.; Hošek, J.; Suchý, P.; Vančo, J.; Trávníček, Z. Diverse in vitro and in vivo anti-inflammatory effects of trichlorido-gold(III) complexes with N6-benzyladenine derivatives. J. Inorg. Biochem. 2014, 134, 92–99. [Google Scholar] [CrossRef]
- Reddy, T.S.; Pooja, D.; Privér, S.H.; Luwor, R.B.; Mirzadeh, N.; Ramesan, S.; Ramakrishna, S.; Karri, S.; Kuncha, M.; Bhargava, S.K. Potent and Selective Cytotoxic and Anti-inflammatory Gold(III) Compounds Containing Cyclometalated Phosphine Sulfide Ligands. Chem. A Eur. J. 2019, 25, 14089–14100. [Google Scholar] [CrossRef]
- Piechota-Polanczyk, A.; Fichna, J. Review article: The role of oxidative stress in pathogenesis and treatment of inflammatory bowel diseases. Naunyn. Schmiedebergs. Arch. Pharmacol. 2014, 387, 605–620. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pereira, C.; Grácio, D.; Teixeira, J.P.; Magro, F. Oxidative Stress and DNA Damage: Implications in Inflammatory Bowel Disease. Inflamm. Bowel Dis. 2015, 21, 2403–2417. [Google Scholar] [CrossRef]
- Jena, G.; Trivedi, P.P.; Sandala, B. Oxidative stress in ulcerative colitis: An old concept but a new concern. Free Radic. Res. 2012, 46, 1339–1345. [Google Scholar] [CrossRef]
- Vijayan, V.; Mueller, S.; Baumgart-Vogt, E.; Immenschuh, S. Heme oxygenase-1 as a therapeutic target in inflammatory disorders of the gastrointestinal tract. World J. Gastroenterol. 2010, 16, 3112–3119. [Google Scholar] [CrossRef] [PubMed]
- Berberat, P.O.; A-Rahim, Y.I.; Yamashita, K.; Warney, M.M.; Csizmadia, E.; Robson, S.C.; Bach, F.H. Heme oxygenase-1-generated biliverdin ameliorates experimental murine colitis. Inflamm. Bowel Dis. 2005, 11, 350–359. [Google Scholar] [CrossRef]
- Onyiah, J.C.; Sheikh, S.Z.; Maharshak, N.; Steinbach, E.C.; Russo, S.M.; Kobayashi, T.; Mackey, L.C.; Hansen, J.J.; Moeser, A.J.; Rawls, J.F.; et al. Carbon monoxide and heme oxygenase-1 prevent intestinal inflammation in mice by promoting bacterial clearance. Gastroenterology 2013, 144, 789–798. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Onyiah, J.C.; Schaefer, R.E.M.; Colgan, S.P. A Central Role for Heme Oxygenase-1 in the Control of Intestinal Epithelial Chemokine Expression. J. Innate Immun. 2018, 10, 228–238. [Google Scholar] [CrossRef]
- Barrett, K.E.; McCole, D.F. Hydrogen peroxide scavenger, catalase, alleviates ion transport dysfunction in murine colitis. Clin. Exp. Pharmacol. Physiol. 2016, 43, 1097–1106. [Google Scholar] [CrossRef] [Green Version]
- Pervin, M.; Hasnat, M.A.; Lim, J.H.; Lee, Y.M.; Kim, E.O.; Um, B.H.; Lim, B.O. Preventive and therapeutic effects of blueberry (Vaccinium corymbosum) extract against DSS-induced ulcerative colitis by regulation of antioxidant and inflammatory mediators. J. Nutr. Biochem. 2016, 28, 103–113. [Google Scholar] [CrossRef] [PubMed]
- El-Akabawy, G.; El-Sherif, N.M. Zeaxanthin exerts protective effects on acetic acid-induced colitis in rats via modulation of pro-inflammatory cytokines and oxidative stress. Biomed. Pharmacother. 2019, 111, 841–851. [Google Scholar] [CrossRef] [PubMed]
- Güvenç, M.; Cellat, M.; Özkan, H.; Tekeli, İ.O.; Uyar, A.; Gökçek, İ.; İşler, C.T.; Yakan, A. Protective Effects of Tyrosol Against DSS-Induced Ulcerative Colitis in Rats. Inflammation 2019, 42, 1680–1691. [Google Scholar] [CrossRef]
- Sido, B.; Hack, V.; Hochlehnert, A.; Lipps, H.; Herfarth, C.; Dröge, W. Impairment of intestinal glutathione synthesis in patients with inflammatory bowel disease. Gut 1998, 42, 485–492. [Google Scholar] [CrossRef] [Green Version]
- Rafeeq, M.; Murad, H.A.S.; Abdallah, H.M.; El-Halawany, A.M. Protective effect of 6-paradol in acetic acid-induced ulcerative colitis in rats. BMC Complement. Med. Ther. 2021, 21, 28. [Google Scholar] [CrossRef]
- Amirshahrokhi, K. Febuxostat attenuates ulcerative colitis by the inhibition of NF-κB, proinflammatory cytokines, and oxidative stress in mice. Int. Immunopharmacol. 2019, 76, 105884. [Google Scholar] [CrossRef]
- El-Mahdy, N.A.; Saleh, D.A.; Amer, M.S.; Abu-Risha, S.E.S. Role of allopurinol and febuxostat in the amelioration of dextran-induced colitis in rats. Eur. J. Pharm. Sci. 2020, 141, 105116. [Google Scholar] [CrossRef] [PubMed]
- Anzoise, M.L.; Basso, A.R.; Del Mauro, J.S.; Carranza, A.; Ordieres, G.L.; Gorzalczany, S. Potential usefulness of methyl gallate in the treatment of experimental colitis. Inflammopharmacology 2018, 26, 839–849. [Google Scholar] [CrossRef]
- Pei, R.; Liu, J.; Martin, D.A.; Valdez, J.C.; Jeffery, J.; Barrett-Wilt, G.A.; Liu, Z.; Bolling, B.W. Aronia Berry supplementation mitigates inflammation in T cell transfer-induced colitis by decreasing oxidative stress. Nutrients 2019, 11, 1316. [Google Scholar] [CrossRef] [Green Version]
- Kruidenier, L.; Kuiper, I.; van Duijn, W.; Mieremet-Ooms, M.A.C.; van Hogezand, R.A.; Lamers, C.B.H.W.; Verspaget, H.W. Imbalanced secondary mucosal antioxidant response in inflammatory bowel disease. J. Pathol. 2003, 201, 17–27. [Google Scholar] [CrossRef]
- Peng, X.; Li, J.; Tan, S.; Xu, M.; Tao, J.; Jiang, J.; Liu, H.; Wu, B. COX-1/PGE2/EP4 alleviates mucosal injury by upregulating β-arr1-mediated Akt signaling in colitis. Sci. Rep. 2017, 7, 1055. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sakamoto, C. Roles of COX-1 and COX-2 in gastrointestinal pathophysiology. J. Gastroenterol. 1998, 33, 618–624. [Google Scholar] [CrossRef]
- Wang, Z.; Liang, Y.; Zhang, D.; Wu, X.; Yu, J.; Zhang, Z.; Li, Y.; Sun, C.; Tang, Z.; Liu, L. Protective Effects of Polysaccharide Extracted from Portulacae oleracea L. on Colitis Induced by Dextran Sulfate Sodium. J. Med. Food 2020, 23, 125–131. [Google Scholar] [CrossRef] [PubMed]
- Yin, Y.; Ye, L.; Niu, Z.; Fang, W. Anti-inflammatory effects of Vicenin-2 on dextran sulfate sodium-induced colitis in mice. Drug Dev. Res. 2019, 80, 546–555. [Google Scholar] [CrossRef]
- Luo, X.; Yue, B.; Yu, Z.; Ren, Y.; Zhang, J.; Ren, J.; Wang, Z.; Dou, W. Obacunone Protects Against Ulcerative Colitis in Mice by Modulating Gut Microbiota, Attenuating TLR4/NF-κB Signaling Cascades, and Improving Disrupted Epithelial Barriers. Front. Microbiol. 2020, 11, 497. [Google Scholar] [CrossRef] [PubMed]
- Landy, J.; Ronde, E.; English, N.; Clark, S.K.; Hart, A.L.; Knight, S.C.; Ciclitira, P.J.; Al-Hassi, H.O. Tight junctions in inflammatory bowel diseases and inflammatory bowel disease associated colorectal cancer. World J. Gastroenterol. 2016, 22, 3117–3126. [Google Scholar] [CrossRef]
- Ahmad, R.; Sorrell, M.F.; Batra, S.K.; Dhawan, P.; Singh, A.B. Gut permeability and mucosal inflammation: Bad, good or context dependent. Mucosal Immunol. 2017, 10, 307–317. [Google Scholar] [CrossRef] [Green Version]

| Gene | Primer | Sequence |
|---|---|---|
| Cldn1 | Forward | TTTTAATTTCAGGTCTGGCG |
| Reverse | CAAATTCATACCTGGCATTG | |
| Cldn3 | Forward | ATTTCTATAACCCGTTGGTG |
| Reverse | AGAATAGAGGATCTTGGTGG | |
| Cldn4 | Forward | GACTGTGCAAAGTTACTAGC |
| Reverse | ACCAGCAATTTGGATGTAAG | |
| Cldn5 | Forward | AACAGTTCCTACTGAGATCC |
| Reverse | CTTTTTAACACGTCCCTCTG | |
| Cldn7 | Forward | CATTGTTTTCATTGTGGCAG |
| Reverse | CTCGTACTTAACGTTCATGG | |
| Cldn8 | Forward | GAAGTCATATCATGCAAGGG |
| Reverse | TGAGTGTCAGGAGTTAGAAG | |
| Cldn11 | Forward | CTGGTGGACATCCTCATC |
| Reverse | AGAGAGCCAGCAGAATAAG | |
| Cldn12 | Forward | ATTATCTCTGCTTTGTGTGC |
| Reverse | TTCAAGGTAATCAGCGTTTC | |
| Cldn15 | Forward | ACATGGATCTCTCCAAGAAG |
| Reverse | CATACTTGGTTCCAGCATAC | |
| Cldn17 | Forward | TCGGCAGCAACATTATTATC |
| Reverse | ATGCCAATAATGAGAGCAAC | |
| Ocln | Forward | GGAGAGTGAAGAGTACATGG |
| Reverse | TGTCATAATCTCCCACCATC | |
| Tjp1 | Forward | ACTAGCATCAGACCATTCAG |
| Reverse | CGTCTACATGTTTTACAGGAG | |
| Hprt1 | Forward | AGGGATTTGAATCACGTTTG |
| Reverse | TTTACTGGCAACATCAACAG |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Krajewska, J.B.; Włodarczyk, J.; Jacenik, D.; Kordek, R.; Taciak, P.; Szczepaniak, R.; Fichna, J. New Class of Anti-Inflammatory Therapeutics Based on Gold (III) Complexes in Intestinal Inflammation–Proof of Concept Based on In Vitro and In Vivo Studies. Int. J. Mol. Sci. 2021, 22, 3121. https://doi.org/10.3390/ijms22063121
Krajewska JB, Włodarczyk J, Jacenik D, Kordek R, Taciak P, Szczepaniak R, Fichna J. New Class of Anti-Inflammatory Therapeutics Based on Gold (III) Complexes in Intestinal Inflammation–Proof of Concept Based on In Vitro and In Vivo Studies. International Journal of Molecular Sciences. 2021; 22(6):3121. https://doi.org/10.3390/ijms22063121
Chicago/Turabian StyleKrajewska, Julia B., Jakub Włodarczyk, Damian Jacenik, Radzisław Kordek, Przemysław Taciak, Remigiusz Szczepaniak, and Jakub Fichna. 2021. "New Class of Anti-Inflammatory Therapeutics Based on Gold (III) Complexes in Intestinal Inflammation–Proof of Concept Based on In Vitro and In Vivo Studies" International Journal of Molecular Sciences 22, no. 6: 3121. https://doi.org/10.3390/ijms22063121







