Connective Tissue Disorders and Fragile X Molecular Status in Females: A Case Series and Review
Abstract
1. Introduction
2. Results
3. Discussion
4. Materials and Methods
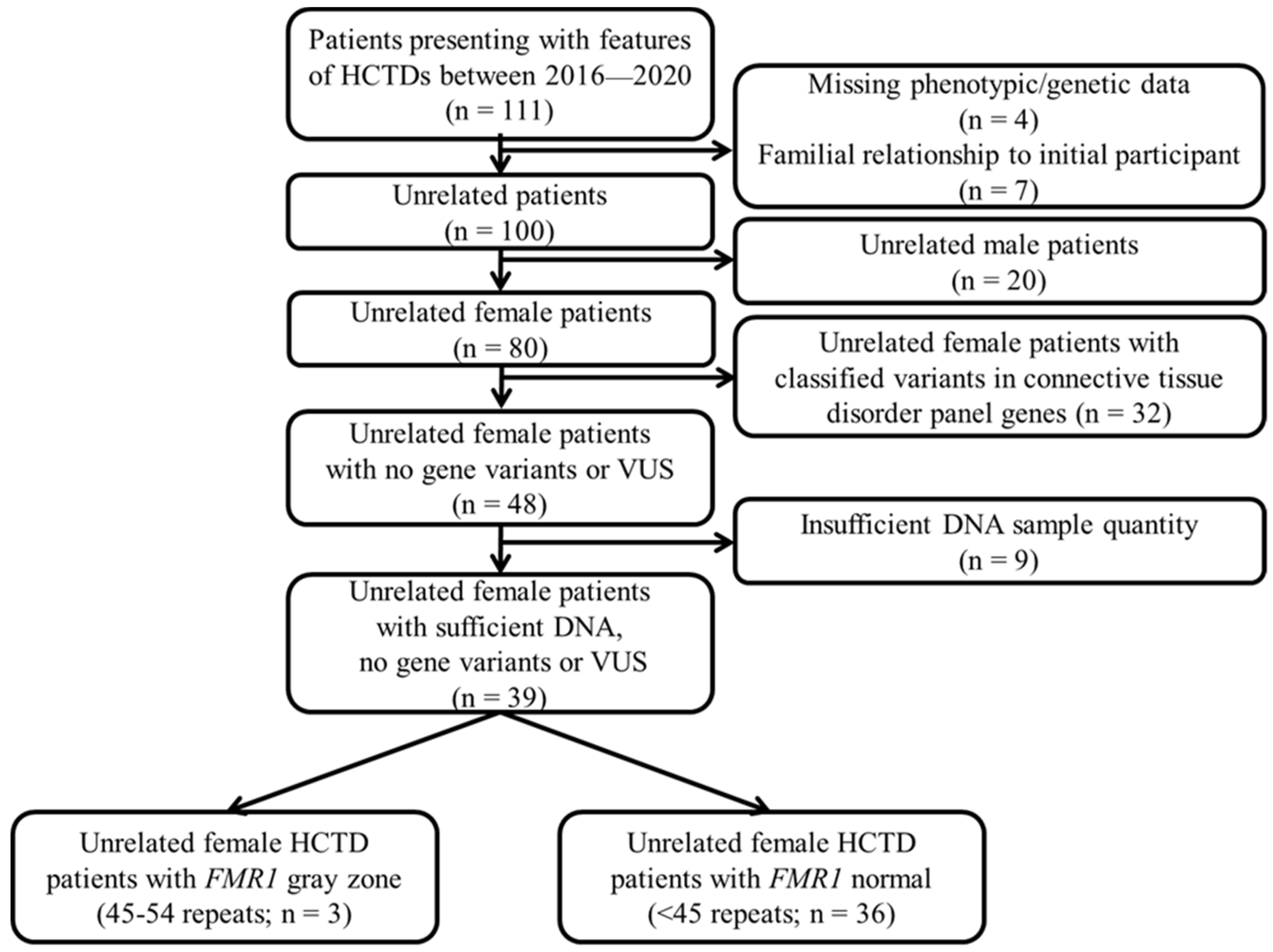
4.1. Subjects
4.2. Molecular Genetics and Case Reports
4.2.1. Molecular Genetics
4.2.2. Case Reports
Case #1
Case #2
Case #3
4.3. Statistical Analyses
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- McLennan, Y.; Polussa, J.; Tassone, F.; Hagerman, R. Fragile X Syndrome. Eur. J. Hum. Genet. 2011, 12, 216–224. [Google Scholar] [CrossRef]
- Hagerman, R.J.; Berry-Kravis, E.; Hazlett, H.C.; Bailey, D.B.; Moine, H.; Kooy, R.F.; Tassone, F.; Gantois, I.; Sonenberg, N.; Mandel, J.L.; et al. Fragile X Syndrome. Nat. Rev. Dis. Primers 2017, 3, 17065. [Google Scholar] [CrossRef] [PubMed]
- Hunter, J.; Rivero-Arias, O.; Angelov, A.; Kim, E.; Fotheringham, I.; Leal, J. Epidemiology of Fragile X Syndrome: A Systematic Review and Meta-Analysis. Am. J. Med. Genet. A 2014, 164A, 1648–1658. [Google Scholar] [CrossRef] [PubMed]
- Ciaccio, C.; Fontana, L.; Milani, D.; Tabano, S.; Miozzo, M.; Esposito, S. Fragile X Syndrome: A Review of Clinical and Molecular Diagnoses. Ital. J. Pediatr. 2017, 43, 39. [Google Scholar] [CrossRef] [PubMed]
- Ramírez-Cheyne, J.A.; Duque, G.A.; Ayala-Zapata, S.; Saldarriaga-Gil, W.; Hagerman, P.; Hagerman, R.; Payán-Gómez, C. Fragile X Syndrome and Connective Tissue Dysregulation. Clin. Genet. 2019, 95, 262–267. [Google Scholar] [CrossRef] [PubMed]
- Tassanakijpanich, N.; McKenzie, F.J.; McLennan, Y.A.; Makhoul, E.; Tassone, F.; Jasoliya, M.J.; Romney, C.; Petrasic, I.C.; Napalinga, K.; Buchanan, C.B.; et al. Hypermobile Ehlers-Danlos Syndrome (HEDS) Phenotype in Fragile X Premutation Carriers: Case Series. J. Med. Genet. 2022, 59, 687–690. [Google Scholar] [CrossRef]
- Butler, M.G.; Allen, G.A.; Haynes, J.L.; Singh, D.N.; Watson, M.S.; Breg, W.R. Anthropometric Comparison of Mentally Retarded Males with and without the Fragile X Syndrome. Am. J. Med. Genet. 1991, 38, 260–268. [Google Scholar] [CrossRef]
- Butler, M.G.; Pratesi, R.; Watson, M.S.; Breg, W.R.; Singh, D.N. Anthropometric and Craniofacial Patterns in Mentally Retarded Males with Emphasis on the Fragile X Syndrome. Clin. Genet. 1993, 44, 129–138. [Google Scholar] [CrossRef]
- Hagerman, R.; Hoem, G.; Hagerman, P. Fragile X and Autism: Intertwined at the Molecular Level Leading to Targeted Treatments. Mol. Autism 2010, 1, 12. [Google Scholar] [CrossRef]
- Rajaratnam, A.; Shergill, J.; Salcedo-Arellano, M.; Saldarriaga, W.; Duan, X.; Hagerman, R. Fragile X Syndrome and Fragile X-Associated Disorders. F1000Research 2017, 6, 2112. [Google Scholar] [CrossRef]
- Baeza-Velasco, C.; Cohen, D.; Hamonet, C.; Vlamynck, E.; Diaz, L.; Cravero, C.; Cappe, E.; Guinchat, V. Autism, Joint Hypermobility-Related Disorders and Pain. Front. Psychiatry 2018, 9, 656. [Google Scholar] [CrossRef] [PubMed]
- Malfait, F.; Francomano, C.; Byers, P.; Belmont, J.; Berglund, B.; Black, J.; Bloom, L.; Bowen, J.M.; Brady, A.F.; Burrows, N.P.; et al. The 2017 International Classification of the Ehlers-Danlos Syndromes. Am. J. Med. Genet. C Semin. Med. Genet. 2017, 175, 8–26. [Google Scholar] [CrossRef] [PubMed]
- Coffey, S.M.; Cook, K.; Tartaglia, N.; Tassone, F.; Nguyen, D.V.; Pan, R.; Bronsky, H.E.; Yuhas, J.; Borodyanskaya, M.; Grigsby, J.; et al. Expanded Clinical Phenotype of Women with the FMR1 Premutation. Am. J. Med. Genet. A 2008, 146A, 1009–1016. [Google Scholar] [CrossRef]
- Rodriguez-Revenga, L.; Madrigal, I.; Pagonabarraga, J.; Xunclà, M.; Badenas, C.; Kulisevsky, J.; Gomez, B.; Milà, M. Penetrance of FMR1 Premutation Associated Pathologies in Fragile X Syndrome Families. Eur. J. Hum. Genet. 2009, 17, 1359–1362. [Google Scholar] [CrossRef]
- Winarni, T.I.; Chonchaiya, W.; Sumekar, T.A.; Ashwood, P.; Morales, G.M.; Tassone, F.; Nguyen, D.V.; Faradz, S.M.H.; Van de Water, J.; Cook, K.; et al. Immune-Mediated Disorders among Women Carriers of Fragile X Premutation Alleles. Am. J. Med. Genet. A 2012, 158A, 2473–2481. [Google Scholar] [CrossRef]
- Nolin, S.L.; Glicksman, A.; Ersalesi, N.; Dobkin, C.; Brown, W.T.; Cao, R.; Blatt, E.; Sah, S.; Latham, G.J.; Hadd, A.G. Fragile X Full Mutation Expansions Are Inhibited by One or More AGG Interruptions in Premutation Carriers. Genet. Med. 2015, 17, 358–364. [Google Scholar] [CrossRef]
- Friedman-Gohas, M.; Kirshenbaum, M.; Michaeli, A.; Domniz, N.; Elizur, S.; Raanani, H.; Orvieto, R.; Cohen, Y. Does the Presence of AGG Interruptions within the CGG Repeat Tract Have a Protective Effect on the Fertility Phenotype of Female FMR1 Premutation Carriers? J. Assist. Reprod. Genet. 2020, 37, 849–854. [Google Scholar] [CrossRef] [PubMed]
- Steinle, J.; Hossain, W.A.; Veatch, O.J.; Strom, S.P.; Butler, M.G. Next-generation Sequencing and Analysis of Consecutive Patients Referred for Connective Tissue Disorders. Am. J. Med. Genet. Part A, 2022; ajmg.a.62905, ahead of print. [Google Scholar] [CrossRef]
- Tassone, F.; Iong, K.P.; Tong, T.-H.; Lo, J.; Gane, L.W.; Berry-Kravis, E.; Nguyen, D.; Mu, L.Y.; Laffin, J.; Bailey, D.B.; et al. FMR1 CGG Allele Size and Prevalence Ascertained through Newborn Screening in the United States. Genome Med. 2012, 4, 100. [Google Scholar] [CrossRef] [PubMed]
- Desai, A.; Connolly, J.J.; March, M.; Hou, C.; Chiavacci, R.; Kim, C.; Lyon, G.; Hadley, D.; Hakonarson, H. Systematic Data-Querying of Large Pediatric Biorepository Identifies Novel Ehlers-Danlos Syndrome Variant. BMC Musculoskelet. Disord. 2016, 17, 80. [Google Scholar] [CrossRef]
- Jacquemont, S.; Hagerman, R.J.; Leehey, M.A.; Hall, D.A.; Levine, R.A.; Brunberg, J.A.; Zhang, L.; Jardini, T.; Gane, L.W.; Harris, S.W.; et al. Penetrance of the Fragile X-Associated Tremor/Ataxia Syndrome in a Premutation Carrier Population. JAMA 2004, 291, 460–469. [Google Scholar] [CrossRef]
- Tassone, F.; Hagerman, R.J.; Taylor, A.K.; Gane, L.W.; Godfrey, T.E.; Hagerman, P.J. Elevated Levels of FMR1 MRNA in Carrier Males: A New Mechanism of Involvement in the Fragile-X Syndrome. Am. J. Hum. Genet. 2000, 66, 6–15. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Arocena, D.; Hagerman, P.J. Advances in Understanding the Molecular Basis of FXTAS. Hum. Mol. Genet. 2010, 19, R83–R89. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dai, R.; Ahmed, S.A. MicroRNA, a New Paradigm for Understanding Immunoregulation, Inflammation, and Autoimmune Diseases. Transl. Res. 2011, 157, 163–179. [Google Scholar] [CrossRef] [PubMed]
- Chang, L.; Sundaresh, S.; Elliott, J.; Anton, P.A.; Baldi, P.; Licudine, A.; Mayer, M.; Vuong, T.; Hirano, M.; Naliboff, B.D.; et al. Dysregulation of the Hypothalamic-Pituitary-Adrenal (HPA) Axis in Irritable Bowel Syndrome. Neurogastroenterol. Motil. 2009, 21, 149–159. [Google Scholar] [CrossRef]
- Evsyukova, I.; Somarelli, J.A.; Gregory, S.G.; Garcia-Blanco, M.A. Alternative Splicing in Multiple Sclerosis and Other Autoimmune Diseases. RNA Biol. 2010, 7, 462–473. [Google Scholar] [CrossRef]
- Otsuka, M.; Zheng, M.; Hayashi, M.; Lee, J.-D.; Yoshino, O.; Lin, S.; Han, J. Impaired MicroRNA Processing Causes Corpus Luteum Insufficiency and Infertility in Mice. J. Clin. Investig. 2008, 118, 1944–1954. [Google Scholar] [CrossRef]
- Nolin, S.L.; Sah, S.; Glicksman, A.; Sherman, S.L.; Allen, E.; Berry-Kravis, E.; Tassone, F.; Yrigollen, C.; Cronister, A.; Jodah, M.; et al. Fragile X AGG Analysis Provides New Risk Predictions for 45-69 Repeat Alleles. Am. J. Med. Genet. A 2013, 161A, 771–778. [Google Scholar] [CrossRef]
- Wijnhoven, H.A.H.; de Vet, H.C.W.; Picavet, H.S.J. Explaining Sex Differences in Chronic Musculoskeletal Pain in a General Population. Pain 2006, 124, 158–166. [Google Scholar] [CrossRef]
- Hall, D.A. In the Gray Zone in the Fragile X Gene: What Are the Key Unanswered Clinical and Biological Questions? Tremor Other Hyperkinetic Mov. 2014, 4, 208. [Google Scholar] [CrossRef]
- Debrey, S.M.; Leehey, M.A.; Klepitskaya, O.; Filley, C.M.; Shah, R.C.; Kluger, B.; Berry-Kravis, E.; Spector, E.; Tassone, F.; Hall, D.A. Clinical Phenotype of Adult Fragile X Gray Zone Allele Carriers: A Case Series. Cerebellum 2016, 15, 623–631. [Google Scholar] [CrossRef]
- Fernandez-Carvajal, I.; Walichiewicz, P.; Xiaosen, X.; Pan, R.; Hagerman, P.J.; Tassone, F. Screening for Expanded Alleles of the FMR1 Gene in Blood Spots from Newborn Males in a Spanish Population. J. Mol. Diagn. 2009, 11, 324–329. [Google Scholar] [CrossRef] [PubMed]
- Hall, D.A.; Nag, S.; Ouyang, B.; Bennett, D.A.; Liu, Y.; Ali, A.; Zhou, L.; Berry-Kravis, E. Fragile X Gray Zone Alleles Are Associated with Signs of Parkinsonism and Earlier Death. Mov. Disord. 2020, 35, 1448–1456. [Google Scholar] [CrossRef] [PubMed]
- Loesch, D.; Hagerman, R. Unstable Mutations in the FMR1 Gene and the Phenotypes. Adv. Exp. Med. Biol. 2012, 769, 78–114. [Google Scholar] [CrossRef] [PubMed]
- Sitzmann, A.F.; Hagelstrom, R.T.; Tassone, F.; Hagerman, R.J.; Butler, M.G. Rare FMR1 Gene Mutations Causing Fragile X Syndrome: A Review. Am. J. Med. Genet. A 2018, 176, 11–18. [Google Scholar] [CrossRef] [PubMed]
| Participants | Age (Years) | CGG Repeats | AGG Interruptions (Number; Allele Size) | Immune-Mediated Disorder or Inflammation | Beighton Hyperflexibility Score |
|---|---|---|---|---|---|
| Case #1 | 26 | 20, 51 * | (1; 20 or 51 *) (1; 51 *) | Polyarthralgia, hypothyroidism, migraines | 7 out of 9 |
| Case #2 | 45 | 33, 48 * | (1; 33 or 48 *) (1; 48 *) | Positive anti-nuclear antibody (ANA), migraines | 3 out of 8 |
| Case #3 | 44 | 24, 50 * | (0; 24) (2; 50 *) | Fibromyalgia, polymyositis, lupus, migraines, family history of Churg–Strauss vasculitis | 4 out of 6 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Butler, M.G.; Hossain, W.A.; Steinle, J.; Gao, H.; Cox, E.; Niu, Y.; Quach, M.; Veatch, O.J. Connective Tissue Disorders and Fragile X Molecular Status in Females: A Case Series and Review. Int. J. Mol. Sci. 2022, 23, 9090. https://doi.org/10.3390/ijms23169090
Butler MG, Hossain WA, Steinle J, Gao H, Cox E, Niu Y, Quach M, Veatch OJ. Connective Tissue Disorders and Fragile X Molecular Status in Females: A Case Series and Review. International Journal of Molecular Sciences. 2022; 23(16):9090. https://doi.org/10.3390/ijms23169090
Chicago/Turabian StyleButler, Merlin G., Waheeda A. Hossain, Jacob Steinle, Harry Gao, Eleina Cox, Yuxin Niu, May Quach, and Olivia J. Veatch. 2022. "Connective Tissue Disorders and Fragile X Molecular Status in Females: A Case Series and Review" International Journal of Molecular Sciences 23, no. 16: 9090. https://doi.org/10.3390/ijms23169090
APA StyleButler, M. G., Hossain, W. A., Steinle, J., Gao, H., Cox, E., Niu, Y., Quach, M., & Veatch, O. J. (2022). Connective Tissue Disorders and Fragile X Molecular Status in Females: A Case Series and Review. International Journal of Molecular Sciences, 23(16), 9090. https://doi.org/10.3390/ijms23169090








