Identification of a Novel de Novo Variant in the CASZ1 Causing a Rare Type of Dilated Cardiomyopathy
Abstract
1. Introduction
2. Case Presentation
2.1. Clinical Evaluation
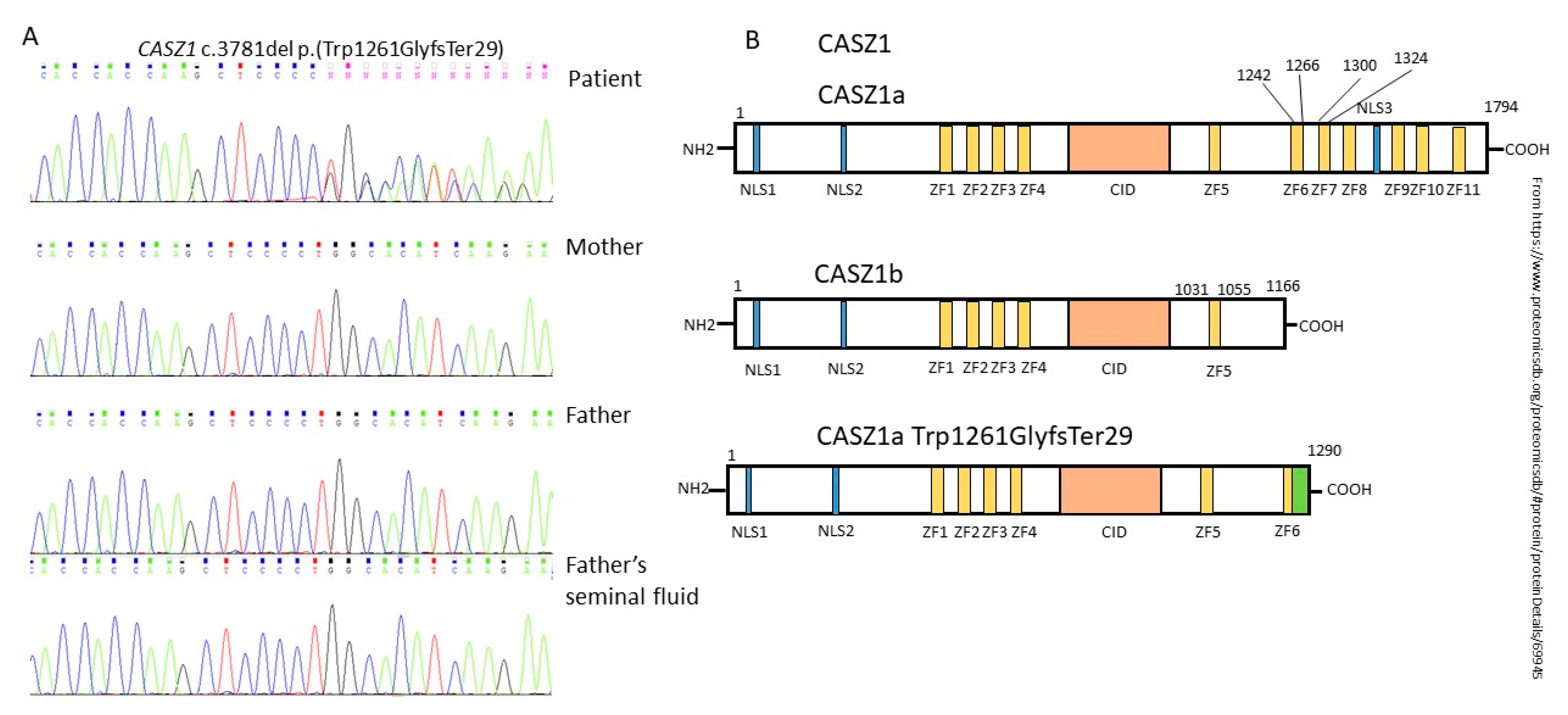
2.2. Genetic Analysis
3. Discussion
4. Materials and Methods
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bharucha, T.; Lee, K.J.; Daubeney, P.E.F.; Nugent, A.W.; Turner, C.; Sholler, G.F.; Robertson, T.; Justo, R.; Ramsay, J.; Carlin, J.B.; et al. Sudden Death in Childhood Cardiomyopathy: Results from a Long-Term National Population-Based Study. J. Am. Coll. Cardiol. 2015, 65, 2302–2310. [Google Scholar] [CrossRef] [PubMed]
- Burke, M.A.; Cook, S.A.; Seidman, J.G.; Seidman, C.E. Clinical and Mechanistic Insights into the Genetics of Cardiomyopathy. J. Am. Coll. Cardiol. 2016, 68, 2871–2886. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Benjamin, E.J.; Go, A.S.; Arnett, D.K.; Blaha, M.J.; Cushman, M.; De Ferranti, S.; Després, J.P.; Fullerton, H.J.; Howard, V.J.; et al. Heart Disease and Stroke Statistics-2015 Update: A Report from the American Heart Association. Circulation 2015, 131, e29–e39. [Google Scholar] [CrossRef] [PubMed]
- Andersen, T.A.; Troelsen, K.D.L.L.; Larsen, L.A. Of Mice and Men: Molecular Genetics of Congenital Heart Disease. Cell. Mol. Life Sci. 2014, 71, 1327–1352. [Google Scholar] [CrossRef] [PubMed]
- Fahed, A.C.; Gelb, B.D.; Seidman, J.G.; Seidman, C.E. Genetics of Congenital Heart Disease: The Glass Half Empty. Circ. Res. 2013, 112, 707–720. [Google Scholar] [CrossRef]
- McCulley, D.J.; Black, B.L. Transcription Factor Pathways and Congenital Heart Disease. Curr. Top. Dev. Biol. 2012, 100, 253–277. [Google Scholar] [CrossRef]
- Dorr, K.M.; Amin, N.M.; Kuchenbrod, L.M.; Labiner, H.; Charpentier, M.S.; Pevny, L.H.; Wessels, A.; Conlon, F.L. Casz1 Is Required for Cardiomyocyte G1-to-S Phase Progression during Mammalian Cardiac Development. Development 2015, 142, 2037–2047. [Google Scholar] [CrossRef]
- Liu, Z.; Li, W.; Ma, X.; Ding, N.; Spallotta, F.; Southon, E.; Tessarollo, L.; Gaetano, C.; Mukouyama, Y.S.; Thiele, C.J. Essential Role of the Zinc Finger Transcription Factor Casz1 for Mammalian Cardiac Morphogenesis and Development. J. Biol. Chem. 2014, 289, 29801–29816. [Google Scholar] [CrossRef]
- Liu, Z.; Yang, X.; Tan, F.; Cullion, K.; Thiele, C.J. Molecular Cloning and Characterization of Human Castor, a Novel Human Gene Upregulated during Cell Differentiation. Biochem. Biophys. Res. Commun. 2006, 344, 834–844. [Google Scholar] [CrossRef][Green Version]
- Amin, N.M.; Gibbs, D.; Conlon, F.L. Differential Regulation of CASZ1 Protein Expression during Cardiac and Skeletal Muscle Development. Dev. Dyn. 2014, 243, 948–956. [Google Scholar] [CrossRef]
- Lek, M.; Karczewski, K.J.; Minikel, E.V.; Samocha, K.E.; Banks, E.; Fennell, T.; O’Donnell-Luria, A.H.; Ware, J.S.; Hill, A.J.; Cummings, B.B.; et al. Analysis of protein-coding genetic variation in 60,706 humans. Nature 2016, 536, 285–291. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.; Hoekzema, K.; Vecchio, D.; Wu, H.; Sulovari, A.; Coe, B.P.; Gillentine, M.A.; Wilfert, A.B.; Perez-Jurado, L.A.; Kvarnung, M.; et al. Large-Scale Targeted Sequencing Identifies Risk Genes for Neurodevelopmental Disorders. Nat. Commun. 2020, 11, 4932. [Google Scholar] [CrossRef] [PubMed]
- Al-Hassnan, Z.N.; Almesned, A.; Tulbah, S.; Alakhfash, A.; Alhadeq, F.; Alruwaili, N.; Alkorashy, M.; Alhashem, A.; Alrashdan, A.; Faqeih, E.; et al. Categorized Genetic Analysis in Childhood-Onset Cardiomyopathy. Circ. Genom. Precis. Med. 2020, 13, 504–514. [Google Scholar] [CrossRef] [PubMed]
- Qiu, X.B.; Qu, X.K.; Li, R.G.; Liu, H.; Xu, Y.J.; Zhang, M.; Shi, H.Y.; Hou, X.M.; Liu, X.; Yuan, F.; et al. CASZ1 Loss-of-Function Mutation Contributes to Familial Dilated Cardiomyopathy. Clin. Chem. Lab. Med. 2017, 55, 1417–1425. [Google Scholar] [CrossRef] [PubMed]
- Guo, J.; Li, Z.; Hao, C.; Guo, R.; Hu, X.; Qian, S.; Zeng, J.; Gao, H.; Li, W. A Novel de Novo CASZ1 Heterozygous Frameshift Variant Causes Dilated Cardiomyopathy and Left Ventricular Noncompaction Cardiomyopathy. Mol. Genet. Genom. Med. 2019, 7, e828. [Google Scholar] [CrossRef]
- Huang, R.T.; Xue, S.; Wang, J.; Gu, J.Y.; Xu, J.H.; Li, Y.J.; Li, N.; Yang, X.X.; Liu, H.; Zhang, X.D.; et al. CASZ1 Loss-of-Function Mutation Associated with Congenital Heart Disease. Gene 2016, 595, 62–68. [Google Scholar] [CrossRef]
- He, S.; Virden, R.; Liu, Z.; Thiele, C. Abstarct 5040: CASZ1 haploinsufficiency in murine embryonic stem cells causes increased MYC expression, aberrant lineage commitment, and prevents neurogenesis. Cancer Res. 2013, 73, 5040. [Google Scholar] [CrossRef]
- Virden, R.A.; Thiele, C.J.; Liu, Z. Characterization of Critical Domains within the Tumor Suppressor CASZ1 Required for Transcriptional Regulation and Growth Suppression. Mol. Cell. Biol. 2012, 32, 1518–1528. [Google Scholar] [CrossRef]
- Rehwinkel, J.; Raes, J.; Izaurralde, E. Nonsense-mediated mRNA decay: Target genes and functional diversification of effectors. Trends Biochem. Sci. 2006, 31, 639–646. [Google Scholar] [CrossRef]
- Page, M.F.; Carr, B.; Anders, K.R.; Grimson, A.; Anderson, P. SMG-2 is a phosphorylated protein required for mRNA surveillance in Caenorhabditis elegans and related to Upf1p of yeast. Mol. Cell. Biol. 1999, 19, 5943–5951. [Google Scholar] [CrossRef]
- Maquat, L.E. Nonsense-mediated mRNA decay: Splicing, translation and mRNP dynamics. Nat. Rev. Mol. Cell Biol. 2004, 5, 89–99. [Google Scholar] [CrossRef] [PubMed]
- Yan, Q.; Weyn-Vanhentenryck, S.M.; Wu, J.; Sloan, S.A.; Zhang, Y.; Chen, K.; Wu, J.Q.; Barres, B.A.; Zhang, C. Systematic discovery of regulated and conserved alternative exons in the mammalian brain reveals NMD modulating chromatin regulators. Proc. Natl. Acad. Sci. USA 2015, 112, 3445–3450. [Google Scholar] [CrossRef]
- Grimson, A.; O’Connor, S.; Newman, C.L.; Anderson, P. SMG-1 is a phosphatidylinositol kinase-related protein kinase required for nonsense-mediated mRNA Decay in Caenorhabditis elegans. Mol. Cell. Biol. 2004, 24, 7483–7490. [Google Scholar] [CrossRef] [PubMed]
- Hsu, M.-K.; Lin, H.-Y.; Chen, F.-C. NMD Classifier: A reliable and systematic classification tool for nonsense-mediated decay events. PLoS ONE 2017, 12, e0174798. [Google Scholar] [CrossRef] [PubMed]
- Bruel, A.L.; Nambot, S.; Quéré, V.; Vitobello, A.; Thevenon, J.; Assoum, M.; Moutton, S.; Houcinat, N.; Lehalle, D.; Jean-Marçais, N.; et al. Increased Diagnostic and New Genes Identification Outcome Using Research Reanalysis of Singleton Exome Sequencing. Eur. J. Hum. Genet. 2019, 27, 1519–1531. [Google Scholar] [CrossRef] [PubMed]
 —zinc finger domain;
—zinc finger domain;  —low-complexity regions;
—low-complexity regions;  —internal repeats;
—internal repeats;  —both CASZ1a and CASZ1b sequences (NMD region);
—both CASZ1a and CASZ1b sequences (NMD region);  —CASZ1b sequence (NMD region);
—CASZ1b sequence (NMD region);  —CASZ1a non-NMD region;
—CASZ1a non-NMD region;  —CASZ1b non-NMD region;
—CASZ1b non-NMD region;  mutation location.
mutation location.
 —zinc finger domain;
—zinc finger domain;  —low-complexity regions;
—low-complexity regions;  —internal repeats;
—internal repeats;  —both CASZ1a and CASZ1b sequences (NMD region);
—both CASZ1a and CASZ1b sequences (NMD region);  —CASZ1b sequence (NMD region);
—CASZ1b sequence (NMD region);  —CASZ1a non-NMD region;
—CASZ1a non-NMD region;  —CASZ1b non-NMD region;
—CASZ1b non-NMD region;  mutation location.
mutation location.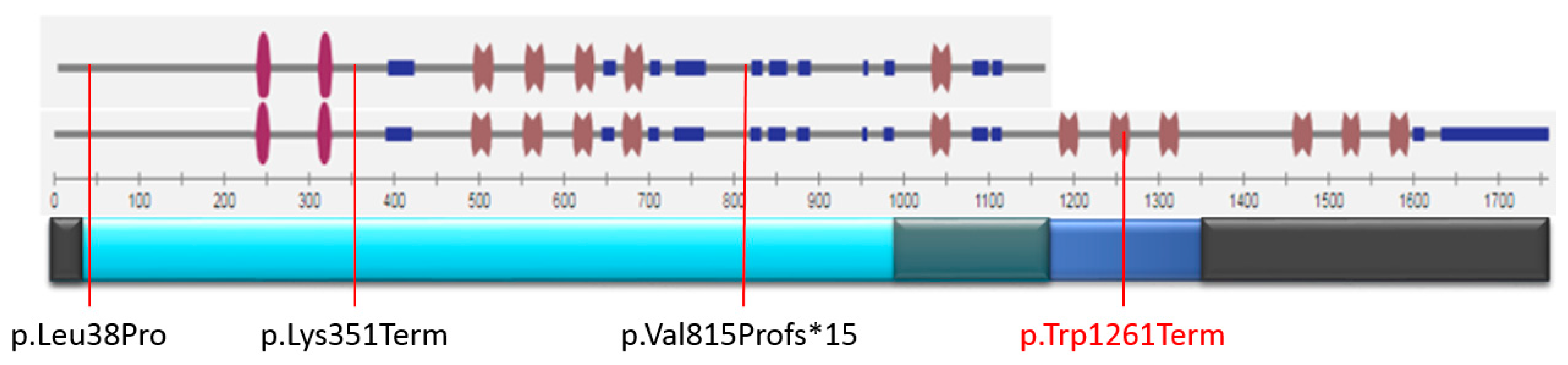
| Family | Affected Member of Family (Male) | Age (Enrollment/Initial Diagnosis of DCM) | Diagnosis 1 | LVEF % | LVFS % | LVESD mm | LVEDD mm | Another Symptoms 2 | Mutation | Ref. |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Proband (m) | 51 / 41 | DCM | 30 | 17 | 63 | 76 | c.1051A > T, p.K351X | Xing-Biao Qiu [14] | |
| Brother | 48 / 45 | DCM | 32 | 20 | 43 | 54 | ||||
| Sister | 39 / 33 | DCM | 30 | 14 | 49 | 55 | ||||
| Daughter | 25 / 25 | DCM, VSD | 39 | 23 | 44 | 58 | ||||
| 2 | Proband (f) | 2 | VSD, DORV | - | - | - | - | c.113T > C, L38P | Ri-Tai Huang [16] | |
| Grandfather | 59 | VSD | - | - | - | - | ||||
| Father | 31 | VSD | - | - | - | - | ||||
| Aunt | 26 | VSD | ||||||||
| 3 | Patient | 11 mo/11 mo | DCM, LVNC | 25 | - | - | 51 | Mild mitral regurgitation, pneumonia, died due to VF | c.2443_2459del17, p.Val815Profs*14 | Jun Guo [15] |
| 4 | Patient * | 1y10 mo/3 mo | DCM | 12 | - | 42 | 45 | Mild mitral and aortal regurgitation, died due to MODS | * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Orlova, A.; Guseva, D.; Ryzhkova, O. Identification of a Novel de Novo Variant in the CASZ1 Causing a Rare Type of Dilated Cardiomyopathy. Int. J. Mol. Sci. 2022, 23, 12506. https://doi.org/10.3390/ijms232012506
Orlova A, Guseva D, Ryzhkova O. Identification of a Novel de Novo Variant in the CASZ1 Causing a Rare Type of Dilated Cardiomyopathy. International Journal of Molecular Sciences. 2022; 23(20):12506. https://doi.org/10.3390/ijms232012506
Chicago/Turabian StyleOrlova, Anna, Daria Guseva, and Oxana Ryzhkova. 2022. "Identification of a Novel de Novo Variant in the CASZ1 Causing a Rare Type of Dilated Cardiomyopathy" International Journal of Molecular Sciences 23, no. 20: 12506. https://doi.org/10.3390/ijms232012506
APA StyleOrlova, A., Guseva, D., & Ryzhkova, O. (2022). Identification of a Novel de Novo Variant in the CASZ1 Causing a Rare Type of Dilated Cardiomyopathy. International Journal of Molecular Sciences, 23(20), 12506. https://doi.org/10.3390/ijms232012506






