Associations between Environmental Tobacco Smoke Exposure in Early Life and Astigmatism among Chinese Preschool Children
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Data Collection
2.3. Assessment of ETS Exposure
2.4. Presence of Astigmatism
2.5. Confounding Variables
2.6. Data Analysis
3. Results
3.1. Comparison of Children’s Baseline Characteristics
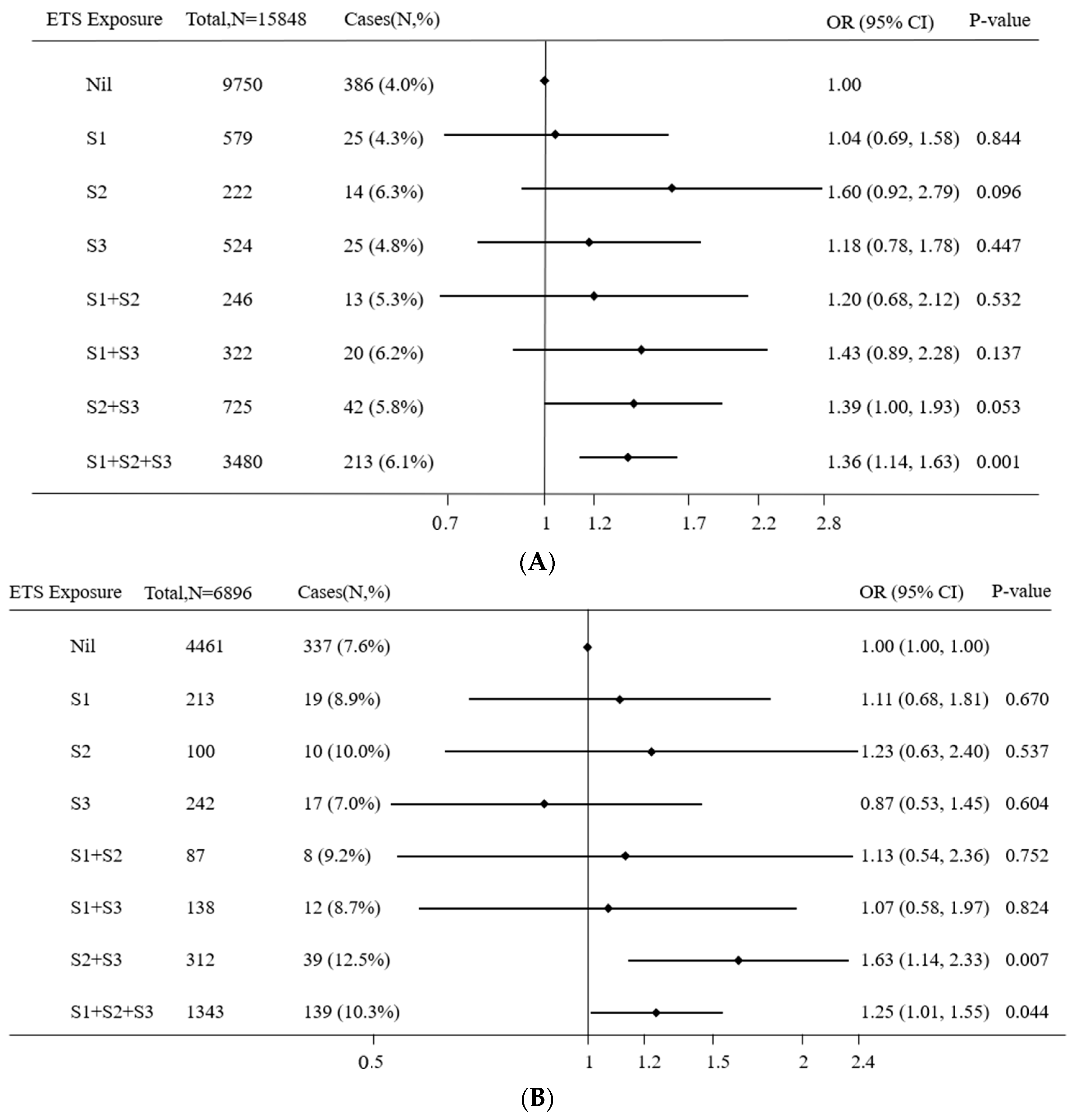
3.2. Association of Astigmatism with Combinations of Prenatal and Postnatal ETS Exposure
3.3. Sensitivity Analysis
3.4. Interaction Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Read, S.A.; Collins, M.J.; Carney, L.G. A review of astigmatism and its possible genesis. Clin. Exp. Optom. 2007, 90, 5–19. [Google Scholar] [CrossRef] [PubMed]
- Shih, Y.F.; Hsiao, C.K.; Tung, Y.L.; Lin, L.L.; Chen, C.J.; Hung, P.T. The prevalence of astigmatism in Taiwan schoolchildren. Optom. Vis. Sci. 2004, 81, 94–98. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; He, X.; Qu, X.; You, X.; Wang, B.; Shi, H.; Tan, H.; Zou, H.; Zhu, J. Refraction and Ocular Biometry of Preschool Children in Shanghai, China. J. Ophthalmol. 2018, 2018, 5205946. [Google Scholar] [CrossRef] [PubMed]
- McKean-Cowdin, R.; Varma, R.; Cotter, S.A.; Tarczy-Hornoch, K.; Borchert, M.S.; Lin, J.H.; Wen, G.; Azen, S.P.; Torres, M.; Tielsch, J.M.; et al. Risk factors for astigmatism in preschool children: The multi-ethnic pediatric eye disease and Baltimore pediatric eye disease studies. Ophthalmology 2011, 118, 1974–1981. [Google Scholar] [CrossRef]
- Gwiazda, J.; Grice, K.; Held, R.; McLellan, J.; Thorn, F. Astigmatism and the development of myopia in children. Vis. Res. 2000, 40, 1019–1026. [Google Scholar] [CrossRef] [Green Version]
- Abrahamsson, M.; Sjostrand, J. Astigmatic axis and amblyopia in childhood. Acta Ophthalmol. Scand. 2003, 81, 33–37. [Google Scholar] [CrossRef] [PubMed]
- Fulton, A.B.; Hansen, R.M.; Petersen, R.A. The relation of myopia and astigmatism in developing eyes. Ophthalmology 1982, 89, 298–302. [Google Scholar] [CrossRef]
- Tong, L.; Saw, S.M.; Carkeet, A.; Chan, W.Y.; Wu, H.M.; Tan, D. Prevalence rates and epidemiological risk factors for astigmatism in Singapore school children. Optom. Vis. Sci. 2002, 79, 606–613. [Google Scholar] [CrossRef]
- Wojciechowski, R. Nature and nurture: The complex genetics of myopia and refractive error. Clin. Genet. 2011, 79, 301–320. [Google Scholar] [CrossRef]
- Li, L.; Qi, Y.; Shi, W.; Wang, Y.; Liu, W.; Hu, M. A Meta-Analysis for Association of Maternal Smoking with Childhood Refractive Error and Amblyopia. J. Ophthalmol. 2016, 2016, 8263832. [Google Scholar] [CrossRef]
- Williams, C.; Northstone, K.; Howard, M.; Harvey, I.; Harrad, R.A.; Sparrow, J.M. Prevalence and risk factors for common vision problems in children: Data from the ALSPAC study. Br. J. Ophthalmol. 2008, 92, 959–964. [Google Scholar] [CrossRef]
- Chia, A.; Lin, X.; Dirani, M.; Gazzard, G.; Ramamurthy, D.; Quah, B.L.; Chang, B.; Ling, Y.; Leo, S.W.; Wong, T.Y.; et al. Risk factors for strabismus and amblyopia in young Singapore Chinese children. Ophthalmic Epidemiol. 2013, 20, 138–147. [Google Scholar] [CrossRef] [PubMed]
- Stone, R.A.; Wilson, L.B.; Ying, G.S.; Liu, C.; Criss, J.S.; Orlow, J.; Lindstrom, J.M.; Quinn, G.E. Associations between childhood refraction and parental smoking. Investig. Ophthalmol. Vis. Sci. 2006, 47, 4277–4287. [Google Scholar] [CrossRef] [PubMed]
- Stone, R.A.; Sugimoto, R.; Gill, A.S.; Liu, J.; Capehart, C.; Lindstrom, J.M. Effects of nicotinic antagonists on ocular growth and experimental myopia. Investig. Ophthalmol. Vis. Sci. 2001, 42, 557–565. [Google Scholar]
- Lindstrom, J. Nicotinic acetylcholine receptors in health and disease. Mol. Neurobiol. 1997, 15, 193–222. [Google Scholar] [CrossRef] [PubMed]
- Iyer, J.V.; Low, W.C.; Dirani, M.; Saw, S.M. Parental smoking and childhood refractive error: The STARS study. Eye 2012, 26, 1324–1328. [Google Scholar] [CrossRef] [PubMed]
- Fernandes, M.; Yang, X.; Li, J.Y.; Cheikh Ismail, L. Smoking during pregnancy and vision difficulties in children: A systematic review. Acta Ophthalmol. 2015, 93, 213–223. [Google Scholar] [CrossRef] [PubMed]
- Daw, N.W. Critical periods and amblyopia. Arch. Ophthalmol. 1998, 116, 502–505. [Google Scholar] [CrossRef]
- Bremond-Gignac, D.; Copin, H.; Lapillonne, A.; Milazzo, S. Visual development in infants: Physiological and pathological mechanisms. Curr. Opin. Ophthalmol. 2011, 22, S1–S8. [Google Scholar] [CrossRef] [PubMed]
- Lewis, T.L.; Maurer, D. Multiple sensitive periods in human visual development: Evidence from visually deprived children. Dev. Psychobiol. 2005, 46, 163–183. [Google Scholar] [CrossRef]
- Salmasi, G.; Grady, R.; Jones, J.; McDonald, S.D. Environmental tobacco smoke exposure and perinatal outcomes: A systematic review and meta-analyses. Acta Obstetricia et Gynecologica Scandinavica 2010, 89, 423–441. [Google Scholar] [CrossRef] [PubMed]
- Leonardi-Bee, J.; Smyth, A.; Britton, J.; Coleman, T. Environmental tobacco smoke and fetal health: Systematic review and meta-analysis. Arch. Dis. Child. Fetal Neonatal Ed. 2008, 93, F351–F361. [Google Scholar] [CrossRef] [PubMed]
- Lois, N.; Abdelkader, E.; Reglitz, K.; Garden, C.; Ayres, J.G. Environmental tobacco smoke exposure and eye disease. Br. J. Ophthalmol. 2008, 92, 1304–1310. [Google Scholar] [CrossRef] [PubMed]
- Schick, S.; Glantz, S. Philip Morris toxicological experiments with fresh sidestream smoke: More toxic than mainstream smoke. Tob. Control 2005, 14, 396–404. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Hsia, J.; Yang, G. Prevalence of smoking in China in 2010. N. Engl. J. Med. 2011, 364, 2469–2470. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.D.; Cao, J.; Dong, Z.; Li, J.X.; Li, G.; Ma, A.J.; Yang, X.L.; Liu, F.C.; Chen, J.C.; Huang, J.F.; et al. Prevalence of active and passive tobacco smoking among Beijing residents in 2011. Chronic Dis. Transl. Med. 2016, 2, 120–128. [Google Scholar] [CrossRef] [Green Version]
- Saxena, R.; Vashist, P.; Tandon, R.; Pandey, R.M.; Bhardawaj, A.; Gupta, V.; Menon, V. Incidence and progression of myopia and associated factors in urban school children in Delhi: The North India Myopia Study (NIM Study). PLoS ONE 2017, 12, e0189774. [Google Scholar] [CrossRef] [PubMed]
- Greenland, S.; Pearl, J.; Robins, J.M. Causal diagrams for epidemiologic research. Epidemiology 1999, 10, 37–48. [Google Scholar] [CrossRef]
- Borchert, M.; Tarczy-Hornoch, K.; Cotter, S.A.; Liu, N.; Azen, S.P.; Varma, R. Anisometropia in Hispanic and african american infants and young children the multi-ethnic pediatric eye disease study. Ophthalmology 2010, 117, 148–153. [Google Scholar] [CrossRef]
- Chua, S.Y.; Ikram, M.K.; Tan, C.S.; Stone, R.A.; Cai, S.; Gluckman, P.D.; Yap, S.C.; Yap, F.; Wong, T.Y.; Ngo, C.S.; et al. Is there a link between passive smoke exposure and early-onset myopia in preschool Asian children? Ophthalmic Physiol. Opt. J. Br. Coll. Ophthalmic Opt. 2016, 36, 370–380. [Google Scholar] [CrossRef]
- El-Shazly, A.A. Passive smoking exposure might be associated with hypermetropia. Ophthalmic Physiol. Opt. J. Br. Coll. Ophthalmic Opt. 2012, 32, 304–307. [Google Scholar] [CrossRef] [PubMed]
- Torp-Pedersen, T.; Boyd, H.A.; Poulsen, G.; Haargaard, B.; Wohlfahrt, J.; Holmes, J.M.; Melbye, M. In-utero exposure to smoking, alcohol, coffee, and tea and risk of strabismus. Am. J. Epidemiol. 2010, 171, 868–875. [Google Scholar] [CrossRef] [PubMed]
- Saw, S.M.; Chia, K.S.; Lindstrom, J.M.; Tan, D.T.; Stone, R.A. Childhood myopia and parental smoking. Br. J. Ophthalmol. 2004, 88, 934–937. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Duncan, J.R.; Garland, M.; Stark, R.I.; Myers, M.M.; Fifer, W.P.; Mokler, D.J.; Kinney, H.C. Prenatal nicotine exposure selectively affects nicotinic receptor expression in primary and associative visual cortices of the fetal baboon. Brain Pathol. 2015, 25, 171–181. [Google Scholar] [CrossRef] [PubMed]
- Oster, S.F.; Sretavan, D.W. Connecting the eye to the brain: The molecular basis of ganglion cell axon guidance. Br. J. Ophthalmol. 2003, 87, 639–645. [Google Scholar] [CrossRef] [PubMed]
- Wei, X.; Kumar, S.; Ding, J.; Khandelwal, N.; Agarwal, M.; Agrawal, R. Choroidal Structural Changes in Smokers Measured Using Choroidal Vascularity Index. Investig. Ophthalmol. Vis. Sci. 2019, 60, 1316–1320. [Google Scholar] [CrossRef] [PubMed]
- Xie, C.; Wen, X.; Ding, P.; Liu, T.; He, Y.; Niu, Z.; Lin, J.; Yuan, S.; Guo, X.; Jia, D.; et al. Influence of CYP2A6*4 genotypes on maternal serum cotinine among Chinese nonsmoking pregnant women. Nicotine Tob. Res. 2014, 16, 406–412. [Google Scholar] [CrossRef]

| Characteristics | Total n = 27,890 | Astigmatism (n, %) | χ2 | p |
|---|---|---|---|---|
| Gender | 1.16 | 0.28 | ||
| Male | 15,128 | 1120 (7.4%) | ||
| Female | 12,762 | 902 (7.1%) | ||
| Age | 19.87 | 0.000 | ||
| <3 years | 554 | 30 (5.4%) | ||
| 3 to <4 years | 7701 | 482 (6.3%) | ||
| 4 to <5 years | 9570 | 742 (7.8%) | ||
| 5 to <6 years | 9200 | 704 (7.7%) | ||
| ≥6 years | 865 | 64 (7.4%) | ||
| Maternal education | 0.25 | 0.88 | ||
| ≤High school | 11,923 | 875 (7.3%) | ||
| Junior college education | 10,064 | 724 (7.2%) | ||
| ≥Undergraduate college | 5903 | 423 (7.2%) | ||
| Paternal education | 2.80 | 0.25 | ||
| ≤High school | 10,830 | 789 (7.3%) | ||
| Junior college education | 8881 | 670 (7.5%) | ||
| ≥Undergraduate college | 8179 | 563 (6.9%) | ||
| Family monthly income a | 8.14 | 0.09 | ||
| ≤5000 yuan | 4098 | 301 (7.3%) | ||
| 5001–10,000 yuan | 7352 | 572 (7.8%) | ||
| 10,001–20,000 yuan | 9206 | 668 (7.3%) | ||
| 20,001–30,000 yuan | 3976 | 276 (6.9%) | ||
| >30,000 yuan | 3258 | 205 (6.3%) | ||
| Maternal age at childbirth | 2.50 | 0.48 | ||
| ≤22 years | 3271 | 242 (7.4%) | ||
| 22 to <30 years | 19,232 | 1408 (7.3%) | ||
| 30 to <40 years | 5236 | 358 (6.8%) | ||
| ≥40 years | 151 | 14 (9.3%) | ||
| Paternal age at childbirth | 4.22 | 0.24 | ||
| ≤22 years | 1143 | 82 (7.2%) | ||
| 22 to <30 years | 16,451 | 1221 (7.4%) | ||
| 30 to <40 years | 9506 | 653 (6.9%) | ||
| ≥40 years | 790 | 66 (8.4%) | ||
| Electronic screen exposure | 139.10 | 0.000 | ||
| No | 6870 | 278 (4.0%) | ||
| Yes | 21,020 | 1744 (8.3%) |
| TSETS-NECSPD | Total (n = 27,890) | Cases (n, %) | Crude OR (95% CI) | Adjusted OR a (95% CI) |
|---|---|---|---|---|
| 0 | 17,507 | 1141 (6.5%) | 1.00 | 1.00 |
| 1 | 1547 | 122 (7.9%) | 1.23 (1.01–1.49) * | 1.19 (0.98–1.45) |
| 2–3 | 4892 | 409 (8.4%) | 1.31 (1.16–1.47) *** | 1.25 (1.10–1.41) *** |
| 4–7 | 2472 | 217 (8.8%) | 1.38 (1.19–1.61) *** | 1.30 (1.11–1.52) *** |
| 8–11 | 952 | 90 (9.5%) | 1.50 (1.20–1.88) *** | 1.40 (1.12–1.76) ** |
| ≥12 | 520 | 43 (8.3%) | 1.29 (0.94–1.78) | 1.19 (0.86–1.64) |
| p for trend | <0.001 | <0.001 |
| TSETS-TECSPD | Total (n = 27,890) | Cases (n, %) | Crude OR (95% CI) | Adjusted OR a (95% CI) |
|---|---|---|---|---|
| 0 | 17,507 | 1141 (6.5%) | 1.00 | 1.00 |
| 1 | 2008 | 154 (7.7%) | 1.19 (1.00–1.42) * | 1.15 (0.97–1.38) |
| 2–3 | 6365 | 548 (8.6%) | 1.35 (1.22–1.50) *** | 1.28 (1.15–1.43) *** |
| 4–5 | 889 | 81 (9.1%) | 1.44 (1.14–1.82) ** | 1.35 (1.06–1.71) ** |
| 6–8 | 678 | 64 (9.4%) | 1.50 (1.15–1.95) ** | 1.40 (1.07–1.82) ** |
| ≥9 | 443 | 34 (7.7%) | 1.19 (0.84–1.70) | 1.12 (0.78–1.60) |
| p for trend | <0.001 | <0.001 |
| ETS Exposure | Subgroup 1 AOR a (95% CI) | Subgroup 2 AOR a (95% CI) | ||
|---|---|---|---|---|
| S1 | S2 | S3 | ||
| No | No | No | 1.00 | 1.00 |
| Yes | No | No | 1.01 (0.76–1.34) | 1.74 (0.56–5.45) |
| No | Yes | No | 1.18 (0.78–1.79) | 2.27 (0.60–8.58) |
| No | No | Yes | 1.08 (0.82–1.43) | 2.04 (0.72–5.80) |
| Yes | Yes | No | 1.32 (0.91–1.92) | 0.81 (0.10–6.76) |
| Yes | No | Yes | 1.28 (0.92–1.79) | 3.98 (1.16–13.60) * |
| No | Yes | Yes | 1.36 (1.09–1.69) * | 1.28 (0.54–3.02) |
| Yes | Yes | Yes | 1.29 (1.14–1.46) *** | 1.58 (0.93–2.66) |
| ETS Exposure | Subgroup 1 AOR a (95% CI) | Subgroup 2 AOR a (95% CI) | ||
|---|---|---|---|---|
| S1 | S2 | S3 | ||
| No | No | No | 1.00 | 1.00 |
| Yes | No | No | 1.03 (0.79–1.35) | 1.16 (0.51–2.65) |
| No | Yes | No | 1.27 (0.87–1.86) | 2.11 (0.78–5.72) |
| No | No | Yes | 1.10 (0.84–1.44) | 0.93 (0.39–2.21) |
| Yes | Yes | No | 1.22 (0.83–1.78) | 0.94 (0.28–3.20) |
| Yes | No | Yes | 1.35 (0.98–1.84) | 1.56 (0.63–3.83) |
| No | Yes | Yes | 1.35 (1.09–1.67) * | 1.37 (0.75–2.50) |
| Yes | Yes | Yes | 1.30 (1.15–1.46) *** | 1.20 (0.84–1.72) |
| Crude OR (95% CI) | Adjusted OR a (95% CI) | |
|---|---|---|
| ETS exposure | 1.49 (1.28–1.72) *** | 1.34 (1.16–1.56) *** |
| Parental history of visual problems | 2.62 (2.30–2.97) *** | 2.72 (2.39–3.10) *** |
| ETS exposure × Parental history of visual problems | 0.88 (0.73–1.06) | 0.88 (0.72–1.06) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, C.-G.; Yang, G.-Y.; Schmid, K.L.; Huang, L.-H.; He, G.-H.; Liu, L.; Ruan, Z.-L.; Chen, W.-Q. Associations between Environmental Tobacco Smoke Exposure in Early Life and Astigmatism among Chinese Preschool Children. Int. J. Environ. Res. Public Health 2019, 16, 3725. https://doi.org/10.3390/ijerph16193725
Li C-G, Yang G-Y, Schmid KL, Huang L-H, He G-H, Liu L, Ruan Z-L, Chen W-Q. Associations between Environmental Tobacco Smoke Exposure in Early Life and Astigmatism among Chinese Preschool Children. International Journal of Environmental Research and Public Health. 2019; 16(19):3725. https://doi.org/10.3390/ijerph16193725
Chicago/Turabian StyleLi, Chen-Guang, Gui-You Yang, Katrina L. Schmid, Li-Hua Huang, Guan-Hao He, Li Liu, Zeng-Liang Ruan, and Wei-Qing Chen. 2019. "Associations between Environmental Tobacco Smoke Exposure in Early Life and Astigmatism among Chinese Preschool Children" International Journal of Environmental Research and Public Health 16, no. 19: 3725. https://doi.org/10.3390/ijerph16193725





