Effect of Ambient Air Pollution on Hospital Readmissions among the Pediatric Asthma Patient Population in South Texas: A Case-Crossover Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Sources and Study Setting
2.2. Study Design and Measurement
2.3. Statistical Analysis
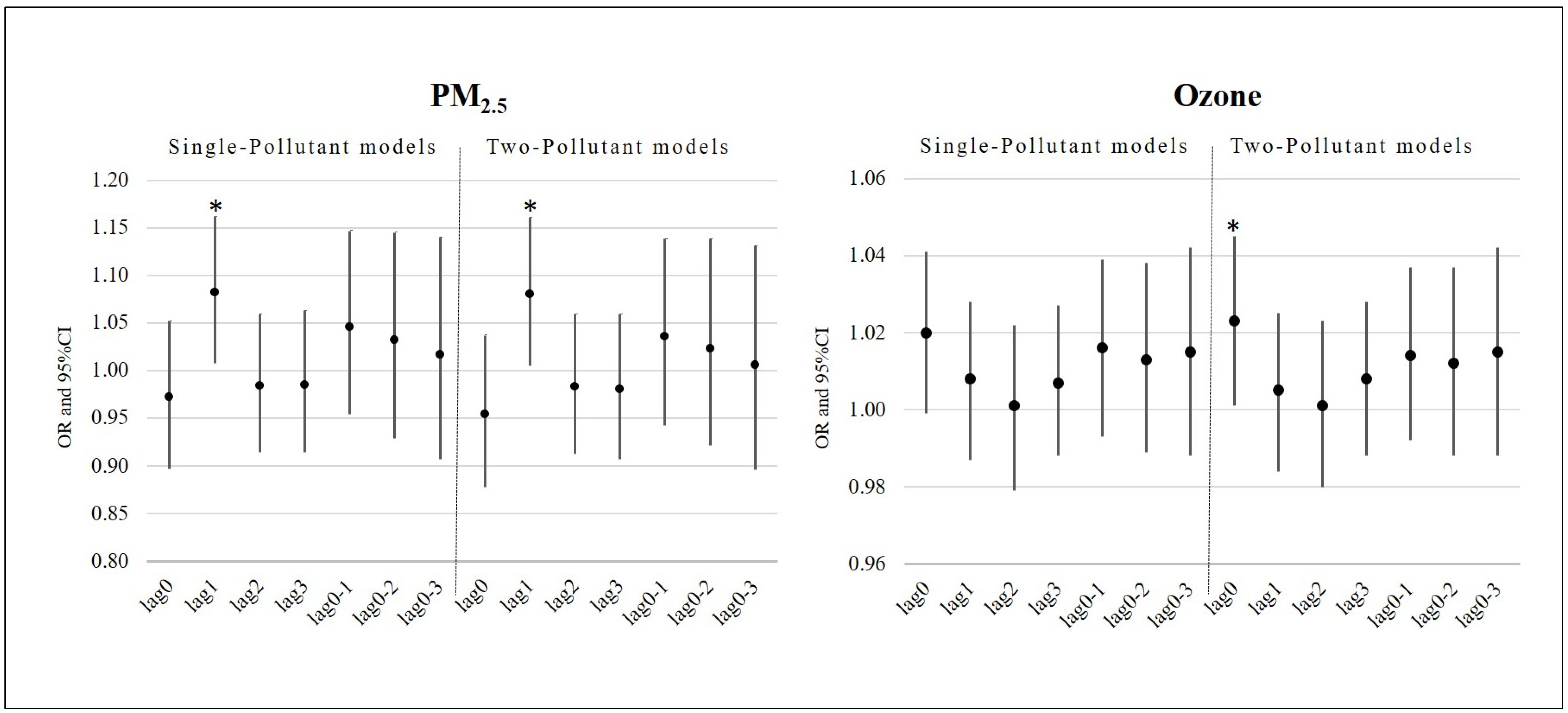
3. Results
4. Discussion
4.1. Limitations
4.2. Health Policy and Practice Implications
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Variable | PM2.5 | Ozone | Temperature |
|---|---|---|---|
| PM2.5 | 1.00 | ||
| Ozone | −0.214 * | 1.00 | |
| Temperature | −0.216 * | 0.077 | 1.00 |
References
- Watson, L.; Turk, F.; Rabe, K.F. Burden of asthma in the hospital setting: An Australian analysis. Int. J. Clin. Pract. 2007, 61, 1884–1888. [Google Scholar] [CrossRef] [Green Version]
- Berry, J.G.; Hall, D.E.; Kuo, D.Z.; Cohen, E.; Agrawal, R.; Feudtner, C.; Hall, M. Hospital utilization and characteristics of patients experiencing recurrent readmissions within children’s hospitals. JAMA 2011, 305, 682–690. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liu, S.Y.; Pearlman, D.N. Hospital readmissions for childhood asthma: The role of individual and neighborhood factors. Public Health Rep. 2009, 124, 65–78. [Google Scholar] [CrossRef] [PubMed]
- Regenstein, M.; Andres, E. Reducing hospital readmissions among medicaid patients: A review of the literature. Qual. Manag. Healthc. 2014, 23, 203–225. [Google Scholar] [CrossRef] [PubMed]
- Purdy, S.; Griffin, T.; Salisbury, C.; Sharp, D. Ambulatory care sensitive conditions: Terminology and disease coding need to be more specific to aid policy makers and clinicians. Public Health 2009, 123, 169–173. [Google Scholar] [CrossRef]
- Lu, S.; Kuo, D.Z. Hospital charges of potentially preventable pediatric hospitalizations. Acad. Pediatr. 2012, 12, 436–444. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kenyon, C.C.; Melvin, P.R.; Chiang, V.W.; Elliott, M.N.; Schuster, M.A.; Berry, J.G. Rehospitalization for childhood asthma: Timing, variation, and opportunities for intervention. J. Pediatr. 2014, 164, 300–305. [Google Scholar] [CrossRef]
- Krieger, J. Home is where the triggers are: Increasing asthma control by improving the home environment. Pediatr. Allergy Immunol. Pulmonol. 2010, 23, 139–145. [Google Scholar] [CrossRef] [Green Version]
- Takaro, T.K.; Krieger, J.; Song, L.; Sharify, D.; Beaudet, N. The breathe-easy home: The impact of asthma-friendly home construction on clinical outcomes and trigger exposure. Am. J. Public Health 2011, 101, 55–62. [Google Scholar] [CrossRef]
- Howrylak, J.A.; Spanier, A.J.; Huang, B.; Peake, R.W.A.; Kellogg, M.D.; Sauers, H.; Kahn, R.S. Cotinine in children admitted for asthma and readmission. Pediatrics 2014, 133, e355–e362. [Google Scholar] [CrossRef] [Green Version]
- Vicendese, D.; Dharmage, S.C.; Tang, M.L.K.; Olenko, A.; Allen, K.J.; Abramson, M.J.; Erbas, B. Bedroom air quality and vacuuming frequency are associated with repeat child asthma hospital admissions. J. Asthma 2015, 52, 727–731. [Google Scholar] [CrossRef]
- Kim, J.J. Ambient air pollution: Health hazards to children. Pediatrics 2004, 114, 1699–1707. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cook, A.G.; Annemarie, J.B.M.; Pereira, G.; Jardine, A.; Weinstein, P. Use of a total traffic count metric to investigate the impact of roadways on asthma severity: A case–control study. Environ. Health 2011, 10, 52. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brown, M.S.; Sarnat, S.E.; DeMuth, K.A.; Brown, L.A.S.; Whitlock, D.R.; Brown, S.W.; Tolbert, P.E.; Fitzpatrick, A.M. Residential proximity to a major roadway is associated with features of asthma control in children. PLoS ONE 2012, 7, e37044. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Newman, N.C.; Ryan, P.H.; Huang, B.; Beck, A.F.; Sauers, H.S.; Kahn, R.S. Traffic–related air pollution and asthma hospital readmission in children: A longitudinal cohort study. J. Pediatr. 2014, 164, 1396–1402.e1. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Delfino, R.J.; Chang, J.; Wu, J.; Ren, C.; Tjoa, T.; Nickerson, B.; Cooper, D.; Gillen, D.L. Repeated hospital encounters for asthma in children and exposure to traffic–related air pollution near the home. Ann. Allergy Asthma Immunol. 2009, 102, 138–144. [Google Scholar] [CrossRef] [Green Version]
- Chang, J.; Delfino, R.J.; Gillen, D.; Tjoa, T.; Nickerson, B.; Cooper, D. Repeated respiratory hospital encounters among children with asthma and residential proximity to traffic. Occup. Environ. Med. 2009, 66, 90–98. [Google Scholar] [CrossRef] [Green Version]
- Centers for Disease Control and Prevention. National Environmental Public Health Tracking Network. 2018. Available online: www.cdc.gov/ephtracking (accessed on 1 August 2019).
- Centers for Disease Control and Prevention. Downloadable Datasets. 2018. Available online: https://ephtracking.cdc.gov/download (accessed on 1 August 2019).
- Centers for Disease Control and Prevention. Outdoor Air. In: Monitor + Model Air Data. 2019. Available online: https://ephtracking.cdc.gov/showAirMonModData (accessed on 1 August 2019).
- Liu, H.; Tian, Y.; Cao, Y.; Song, J.; Huang, C.; Xiang, X.; Li, M.; Hu, Y. Fine particulate air pollution and hospital admissions and readmissions for acute myocardial infarction in 26 Chinese cities. Chemosphere 2018, 192, 282–288. [Google Scholar] [CrossRef]
- O’Lenick, C.R.; Winquist, A.; Mulholland, J.A.; Friberg, M.D.; Chang, H.H.; Kramer, M.R.; Darrow, L.A.; Sarnat, S.E. Assessment of neighbourhood-level socioeconomic status as a modifier of air pollution-asthma associations among children in Atlanta. J. Epidemiol. Community Health 2017, 71, 129–136. [Google Scholar] [CrossRef]
- Orellano, P.; Quaranta, N.; Reynoso, J.; Balbi, B.; Vasquez, J. Effect of outdoor air pollution on asthma exacerbations in children and adults: Systematic review and multilevel meta-analysis. PLoS ONE 2017, 12, e0174050. [Google Scholar] [CrossRef]
- Zhang, Y.; Ni, H.; Bai, L.; Cheng, Q.; Zhang, H.; Wang, S.; Xie, M.; Zhao, D.; Su, H. The short-term association between air pollution and childhood asthma hospital admissions in urban areas of Hefei City in China: A time-series study. Environ. Res. 2019, 169, 510–516. [Google Scholar] [CrossRef]
- Hua, J.; Yin, Y.; Peng, L.; Du, L.; Geng, F.; Zhu, L. Acute effects of black carbon and PM2.5 on children asthma admissions: A time–series study in a Chinese city. Sci. Total Environ. 2014, 481, 433–438. [Google Scholar] [CrossRef]
- Ding, L.; Zhu, D.; Peng, D.; Zhao, Y. Air pollution and asthma attacks in children: A case–crossover analysis in the city of Chongqing, China. Environ. Pollut. 2017, 220, 348–353. [Google Scholar] [CrossRef]
- Li, S.; Batterman, S.; Wasilevich, E.; Wahl, R.; Wirth, J.; Su, F.-C.; Mukherjee, B. Association of daily asthma emergency department visits and hospital admissions with ambient air pollutants among the pediatric Medicaid population in Detroit: Time-series and time-stratified case-crossover analyses with threshold effects. Environ. Res. 2011, 111, 1137–1147. [Google Scholar] [CrossRef] [PubMed]
- Zu, K.; Liu, X.; Shi, L.; Tao, G.; Loftus, C.T.; Lange, S.; Goodman, J.E. Concentration-response of short-term ozone exposure and hospital admissions for asthma in Texas. Environ. Int. 2017, 104, 139–145. [Google Scholar] [CrossRef] [PubMed]
- Silverman, R.A.; Ito, K. Age-related association of fine particles and ozone with severe acute asthma in New York City. J. Allergy Clin. Immunol. 2010, 125, 367–373.e5. [Google Scholar] [CrossRef] [PubMed]
- Gharibi, H.; Entwistle, M.R.; Ha, S.; Gonzalez, M.; Brown, P.; Schweizer, D.; Cisneros, R. Ozone pollution and asthma emergency department visits in the Central Valley, California, USA, during June to September of 2015: A time–stratified case–crossover analysis. J. Asthma 2019, 56, 1037–1048. [Google Scholar] [CrossRef]
- Ko, F.W.S.; Tam, W.; Wong, T.W.; Lai, C.K.W.; Wong, G.W.K.; Leung, T.F.; Ng, S.S.S.; Hui, D.S.C. Effects of air pollution on asthma hospitalization rates in different age groups in Hong Kong. Clin. Exp. Allergy 2007, 37, 1312–1319. [Google Scholar] [CrossRef]
- Son, J.-Y.; Lee, J.-T.; Park, Y.H.; Bell, M.L. Short–term effects of air pollution on hospital admissions in Korea. Epidemiology 2013, 24, 545–554. [Google Scholar] [CrossRef]
- Iskandar, A.; Andersen, Z.J.; Bønnelykke, K.; Ellermann, T.; Andersen, K.K.; Bisgaard, H. Coarse and fine particles but not ultrafine particles in urban air trigger hospital admission for asthma in children. Thorax 2012, 67, 252–257. [Google Scholar] [CrossRef] [Green Version]
- Villeneuve, P.J.; Chen, L.; Rowe, B.H.; Coates, F. Outdoor air pollution and emergency department visits for asthma among children and adults: A case–crossover study in northern Alberta, Canada. Environ. Health 2007, 6, 40. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Strickland, M.J.; Darrow, L.A.; Klein, M.; Flanders, W.D.; Sarnat, J.A.; Waller, L.A.; Sarnat, S.E.; Mulholland, J.A.; Tolbert, P.E. Short–term associations between ambient air pollutants and pediatric asthma emergency department visits. Am. J. Respir. Crit. Care Med. 2010, 182, 307–316. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gleason, J.A.; Bielory, L.; Fagliano, J.A. Associations between ozone, PM2.5, and four pollen types on emergency department pediatric asthma events during the warm season in New Jersey: A case–crossover study. Environ. Res. 2014, 132, 421–429. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Chen, Q.; Zheng, X.; Li, Y.; Han, M.; Liu, T.; Xiao, J.; Guo, L.; Zeng, W.; Zhang, J.; et al. Effects of ambient ozone concentrations with different averaging times on asthma exacerbations: A meta–analysis. Sci. Total Environ. 2019, 691, 549–561. [Google Scholar] [CrossRef] [PubMed]
- Jalaludin, B.; Khalaj, B.; Sheppeard, V.; Morgan, G. Air pollution and ED visits for asthma in Australian children: A case–crossover analysis. Int. Arch. Occup. Environ. Health 2008, 81, 967–974. [Google Scholar] [CrossRef]
- Bateson, T.F.; Schwartz, J. Children’s response to air pollutants. J. Toxicol Environ. Health A 2008, 71, 238–243. [Google Scholar] [CrossRef]
- Diffey, B.L. An overview analysis of the time people spend outdoors. Br. J. Dermatol. 2011, 164, 848–854. [Google Scholar] [CrossRef]
- Goldman, G.T.; Mulholland, J.A.; Russell, A.G.; Strickland, M.J.; Klein, M.; Waller, L.A.; Tolbert, P.E. Impact of exposure measurement error in air pollution epidemiology: Effect of error type in time–series studies. Environ. Health 2011, 10, 61. [Google Scholar] [CrossRef] [Green Version]
- Parikh, K.; Hall, M.; Kenyon, C.C.; Teufel, R.J.; Mussman, G.M.; Montalbano, A.; Gold, J.; Antoon, J.W.; Subramony, A.; Mittal, V.; et al. Impact of discharge components on readmission rates for children hospitalized with asthma. J. Pediatr. 2018, 195, 175–181.e2. [Google Scholar] [CrossRef]
- Kash, B.A.; Baek, J.; Cheon, O.; Coleman, N.E.; Jones, S.L. Successful hospital readmission reduction initiatives: Top five strategies to consider implementing today. Int. J. Hosp. Tour. Adm. 2018, 7, 16–23. [Google Scholar] [CrossRef] [Green Version]
- Baek, J.; Huang, K.; Conner, L.; Tapangan, N.; Xu, X.; Carrillo, G. Effects of the home-based educational intervention on health outcomes among primarily Hispanic children with asthma: A quasi-experimental study. BMC Public Health 2019, 19, 912. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carrillo, G.; Spence-Almaguer, E.; Lucio, R.L.; Chong-Menard, B.; Smith, K. Improving asthma in Hispanic families through a home-based educational intervention. Pediatr. Allergy Immunol. Pulmonol. 2015, 28, 165–171. [Google Scholar] [CrossRef]
- Fernandes, J.C.; Biskupiak, W.W.; Brokaw, S.M.; Carpenedo, D.; Loveland, K.M.; Tysk, S.; Volg, S. Outcomes of the Montana Asthma Home Visiting Program: A home–based asthma education program. J. Asthma 2019, 56, 104–110. [Google Scholar] [CrossRef] [PubMed]
- Kash, B.A.; Baek, J.; Davis, E.; Champagne-Langabeer, T.; Langabeer II, J.R. Review of successful hospital readmission reduction strategies and the role of health information exchange. Int. J. Med. Inform. 2017, 104, 97–104. [Google Scholar] [CrossRef]
| Variable | Mean ± SD [Min, Max] or N (%) |
|---|---|
| Age (years) | 9.54 ± 3.34 [5, 18] |
| Age | |
| 5–11 years old | 88 (79.3) |
| 12–18 years old | 23 (20.7) |
| Gender | |
| Female | 47 (42.3) |
| Male | 64 (57.6) |
| Ethnicity | |
| Hispanic | 88 (79.3) |
| Non-Hispanic | 23 (20.7) |
| Type of insurance | |
| Public (Medicaid) | 78 (70.3) |
| Private | 29 (26.1) |
| Self-pay | 4 (3.6) |
| Days to readmission (days) | 386.5 ± 364.24 [1, 1651] |
| 1–30 days | 9 (8.1) |
| 31–90 days | 12 (10.8) |
| 91–180 days | 19 (17.1) |
| 181–365 days | 30 (27.1) |
| 366 days or longer | 41 (36.9) |
| Season | |
| Warm (May–October) | 53 (47.7) |
| Cold (November–April) | 58 (52.3) |
| Year | |
| 2010 | 13 (11.7) |
| 2011 | 22 (19.8) |
| 2012 | 18 (16.2) |
| 2013 | 26 (23.4) |
| 2014 | 32 (28.8) |
| Variable | Mean | SD | Minimum | Percentile | Maximum | IQR | ||
|---|---|---|---|---|---|---|---|---|
| 25 | 50 | 75 | ||||||
| PM2.5 (μg/m3) | 8.30 | 1.49 | 4.66 | 7.19 | 8.25 | 9.19 | 12.37 | 2.0 |
| Ozone (ppb) | 37.37 | 6.81 | 20.53 | 31.47 | 37.24 | 42.11 | 52.84 | 10.64 |
| Temperature (°C) | 20.20 | 5.85 | 8.83 | 16.31 | 21.01 | 26.91 | 29.73 | 10.6 |
| Single- and Cumulative-Day Lags | Single-Pollutant Model | Two-Pollutant Model | ||||||
|---|---|---|---|---|---|---|---|---|
| PM2.5 | Ozone | PM2.5 | Ozone | |||||
| OR (95% CI) | p-Value | OR (95% CI) | p-Value | OR (95% CI) | p-Value | OR (95% CI) | p-Value | |
| Lag0 | 0.972 (0.897–1.052) | 0.479 | 1.020 (0.999–1.041) | 0.064 | 0.954 (0.878–1.037) | 0.272 | 1.023 (1.001–1.045) | 0.042 * |
| Lag1 | 1.082 (1.008–1.162) | 0.030 * | 1.008 (0.987–1.028) | 0.469 | 1.080 (1.005–1.161) | 0.036 * | 1.005 (0.984–1.025) | 0.665 |
| Lag2 | 0.984 (0.914–1.059) | 0.664 | 1.001 (0.979–1.022) | 0.955 | 0.983 (0.912–1.059) | 0.655 | 1.001 (0.980–1.023) | 0.904 |
| Lag3 | 0.985 (0.914–1.063) | 0.700 | 1.007 (0.988–1.027) | 0.472 | 0.980 (0.907–1.059) | 0.613 | 1.008 (0.988–1.028) | 0.429 |
| Lag0–1 | 1.046 (0.954–1.147) | 0.334 | 1.016 (0.993–1.039) | 0.168 | 1.036 (0.942–1.138) | 0.468 | 1.014 (0.992–1.037) | 0.222 |
| Lag0–2 | 1.032 (0.929–1.145) | 0.558 | 1.013 (0.989–1.038) | 0.292 | 1.023 (0.921–1.138) | 0.667 | 1.012 (0.988–1.037) | 0.667 |
| Lag0–3 | 1.017 (0.907–1.140) | 0.779 | 1.015 (0.988–1.042) | 0.275 | 1.006 (0.896–1.131) | 0.915 | 1.015 (0.988–1.042) | 0.290 |
| Single- and Cumulative-Day Lags | 5–11 Years Old | 12–18 Years Old | ||||||
|---|---|---|---|---|---|---|---|---|
| Single-Pollutant | Two-Pollutant | Single-Pollutant | Two-Pollutant | |||||
| PM2.5 | Ozone | PM2.5 | Ozone | PM2.5 | Ozone | PM2.5 | Ozone | |
| Lag0 | 0.934 (0.850–1.026) | 1.022 (0.999–1.047) | 0.908 (0.821–1.004) | 1.029* (1.004–1.055) | 1.123 (0.942–1.337) | 1.009 (0.964–1.057) | 1.122 (0.942–1.336) | 1.008 (0.965–1.054) |
| Lag1 | 1.075 (0.994–1.162) | 1.009 (0.986–1.033) | 1.071 (0.990–1.159) | 1.006 (0.982–1.030) | 1.112 (0.924–1.338) | 1.001 (0.959–1.046) | 1.113 (0.924–1.339) | 1.002 (0.960–1.045) |
| Lag2 | 0.962 (0.881–1.050) | 1.003 (0.980–1.027) | 0.959 (0.878–1.048) | 1.005 (0.981–1.029) | 1.045 (0.908–1.204) | 0.983 (0.933–1.034) | 1.062 (0.917–1.230) | 0.978 (0.927–1.031) |
| Lag3 | 0.983 (0.905–1.067) | 1.004 (0.982–1.026) | 0.980 (0.902–1.066) | 1.005 (0.983–1.027) | 0.969 (0.795–1.182) | 1.016 (0.968–1.067) | 0.953 (0.779–1.166) | 1.019 (0.969–1.071) |
| Lag0–1 | 1.017 (0.917–1.127) | 1.018 (0.993–1.044) | 1.000 (0.899–1.112) | 1.018 (0.992–1.045) | 1.174 (0.945–1.459) | 1.006 (0.958–1.056) | 1.176 (0.946–1.462) | 1.007 (0.960–1.055) |
| Lag0–2 | 0.994 (0.880–1.122) | 1.016 (0.989–1.044) | 0.982 (0.868–1.111) | 1.017 (0.989–1.045) | 1.152 (0.923–1.437) | 1.000 (0.948–1.056) | 1.153 (0.923–1.440) | 0.997 (0.946–1.051) |
| Lag0–3 | 0.983 (0.861–1.121) | 1.016 (0.987–1.047) | 0.970 (0.848–1.110) | 1.017 (0.987–1.048) | 1.123 (0.879–1.435) | 1.006 (0.948–1.067) | 1.122 (0.877–1.435) | 1.003 (0.946–1.063) |
| Single- and Cumulative-Day Lags | Girls | Boys | ||||||
|---|---|---|---|---|---|---|---|---|
| Single-Pollutant | Two-Pollutant | Single-Pollutant | Two-Pollutant | |||||
| PM2.5 | Ozone | PM2.5 | Ozone | PM2.5 | Ozone | PM2.5 | Ozone | |
| Lag0 | 0.936 (0.819–1.070) | 1.021 (0.989–1.054) | 0.902 (0.776–1.048) | 1.029 (0.993–1.066) | 0.994 (0.900–1.099) | 1.019 (0.991–1.047) | 0.983 (0.888–1.089) | 1.019 (0.991–1.048) |
| Lag1 | 1.113 (0.997–1.244) | 1.012 (0.984–1.042) | 1.108 (0.989–1.240) | 1.007 (0.977–1.037) | 1.061 (0.965–1.166) | 1.002 (0.973–1.032) | 1.061 (0.965–1.166) | 1.001 (0.972–1.031) |
| Lag2 | 0.972 (0.858–1.102) | 1.003 (0.973–1.035) | 0.967 (0.849–1.101) | 1.006 (0.974–1.038) | 0.986 (0.900–1.079) | 0.996 (0.967–1.027) | 0.986 (0.900–1.080) | 0.996 (0.967–1.027) |
| Lag3 | 0.984 (0.875–1.107) | 1.007 (0.979–1.037) | 0.972 (0.858–1.100) | 1.010 (0.980–1.041) | 0.985 (0.892–1.087) | 1.005 (0.979–1.033) | 0.984 (0.891–1.087) | 1.006 (0.979–1.033) |
| Lag0–1 | 1.053 (0.911–1.218) | 1.018 (0.986–1.052) | 1.032 (0.885–1.203) | 1.016 (0.983–1.051) | 1.044 (0.926–1.175) | 1.012 (0.982–1.044) | 1.038 (0.921–1.171) | 1.011 (0.980–1.043) |
| Lag0–2 | 1.038 (0.882–1.222) | 1.016 (0.981–1.052) | 1.019 (0.859–1.208) | 1.015 (0.979–1.052) | 1.026 (0.897–1.175) | 1.009 (0.974–1.044) | 1.025 (0.895–1.173) | 1.008 (0.974–1.044) |
| Lag0–3 | 1.015 (0.852–1.209) | 1.016 (0.979–1.054) | 0.989 (0.821–1.193) | 1.017 (0.978–1.057) | 1.013 (0.872–1.176) | 1.011 (0.973–1.050) | 1.012 (0.871–1.176) | 1.011 (0.973–1.050) |
| Single- and Cumulative-Day Lags | Warm Season (May–October) | Cold Season (November–April) | ||||||
|---|---|---|---|---|---|---|---|---|
| Single-Pollutant | Two-Pollutant | Single-Pollutant | Two-Pollutant | |||||
| PM2.5 | Ozone | PM2.5 | Ozone | PM2.5 | Ozone | PM2.5 | Ozone | |
| Lag0 | 1.056 (0.941–1.184) | 1.043 ** (1.012–1.075) | 0.993 (0.874–1.127) | 1.043 * (1.010–1.078) | 0.920 (0.818–1.034) | 1.023 (0.986–1.062) | 0.922 (0.818–1.038) | 1.022 (0.985–1.061) |
| Lag1 | 1.134 * (1.019–1.262) | 1.016 (0.989–1.043) | 1.125 * (1.009–1.254) | 1.009 (0.982–1.037) | 1.032 (0.933–1.141) | 1.013 (0.975–1.053) | 1.030 (0.931–1.138) | 1.013 (0.975–1.052) |
| Lag2 | 1.038 (0.933–1.155) | 1.003 (0.976–1.031) | 1.037 (0.930–1.158) | 1.001 (0.973–1.030) | 0.934 (0.837–1.042) | 1.008 (0.970–1.047) | 0.932 (0.835–1.041) | 1.009 (0.970–1.050) |
| Lag3 | 1.011 (0.915–1.116) | 1.013 (0.989–1.039) | 0.995 (0.895–1.106) | 1.014 (0.988–1.041) | 0.956 (0.853–1.071) | 1.011 (0.973–1.051) | 0.956 (0.853–1.071) | 1.011 (0.972–1.052) |
| Lag0–1 | 1.146 * (1.003–1.309) | 1.033 * (1.002–1.065) | 1.105 (0.961–1.271) | 1.025 (0.993–1.059) | 0.965 (0.844–1.104) | 1.023 (0.982–1.066) | 0.968 (0.846–1.108) | 1.022 (0.981–1.066) |
| Lag0–2 | 1.151 (0.989–1.340) | 1.026 (0.994–1.060) | 1.123 (0.960–1.314) | 1.020 (0.987–1.054) | 0.926 (0.793–1.081) | 1.023 (0.977–1.071) | 0.927 (0.795–1.082) | 1.023 (0.977–1.072) |
| Lag0–3 | 1.132 (0.965–1.329) | 1.031 (0.997–1.066) | 1.098 (0.929–1.296) | 1.025 (0.990–1.062) | 0.892 (0.744–1.070) | 1.029 (0.976–1.085) | 0.894 (0.747–1.070) | 1.029 (0.975–1.087) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baek, J.; Kash, B.A.; Xu, X.; Benden, M.; Roberts, J.; Carrillo, G. Effect of Ambient Air Pollution on Hospital Readmissions among the Pediatric Asthma Patient Population in South Texas: A Case-Crossover Study. Int. J. Environ. Res. Public Health 2020, 17, 4846. https://doi.org/10.3390/ijerph17134846
Baek J, Kash BA, Xu X, Benden M, Roberts J, Carrillo G. Effect of Ambient Air Pollution on Hospital Readmissions among the Pediatric Asthma Patient Population in South Texas: A Case-Crossover Study. International Journal of Environmental Research and Public Health. 2020; 17(13):4846. https://doi.org/10.3390/ijerph17134846
Chicago/Turabian StyleBaek, Juha, Bita A. Kash, Xiaohui Xu, Mark Benden, Jon Roberts, and Genny Carrillo. 2020. "Effect of Ambient Air Pollution on Hospital Readmissions among the Pediatric Asthma Patient Population in South Texas: A Case-Crossover Study" International Journal of Environmental Research and Public Health 17, no. 13: 4846. https://doi.org/10.3390/ijerph17134846








