Healthcare Service Use for Mood and Anxiety Disorders Following Acute Myocardial Infarction: A Cohort Study of the Role of Neighbourhood Socioenvironmental Characteristics in a Largely Rural Population
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Setting
2.2. Data Sources
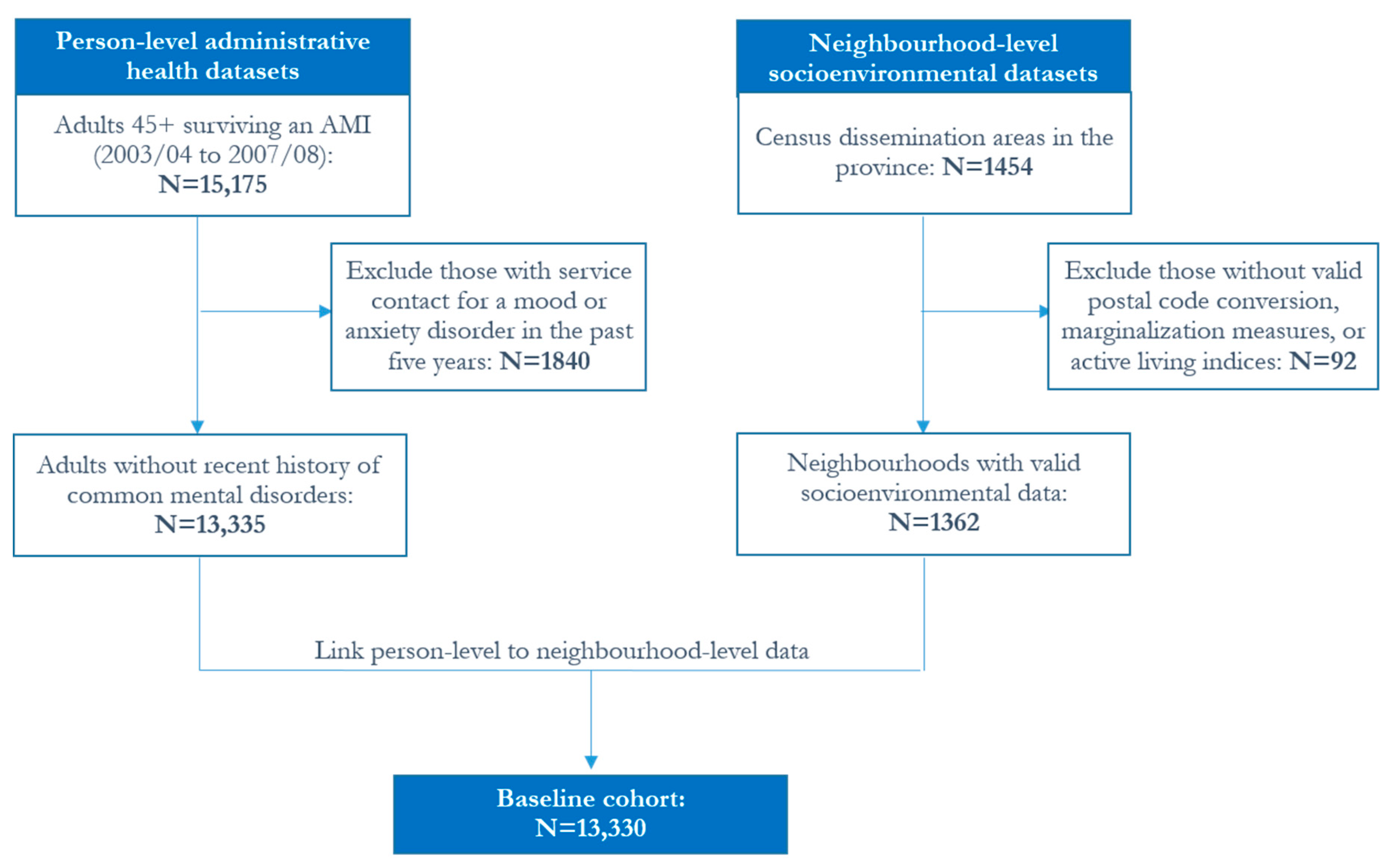
2.3. Study Population
2.4. Health Service Contacts for Mood and Anxiety Disorders
2.5. Neighbourhood Socioenvironmental Characteristics
2.6. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Public Health Agency of Canada. Report from the Canadian Chronic Disease Surveillance System: Heart Disease in Canada, 2018; Public Health Agency of Canada: Ottawa, ON, Canada, 2018. [Google Scholar]
- Lemstra, M.E.; Alsabbagh, W.; Rajakumar, R.J.; Rogers, M.; Blackburn, D. Neighbourhood income and cardiac rehabilitation access as determinants of nonattendance and noncompletion. Can. J. Cardiol. 2013, 29, 1599–1603. [Google Scholar] [CrossRef]
- Blais, C.; Hamel, D.; Rinfret, S. Impact of socioeconomic deprivation and area of residence on access to coronary revascularization and mortality after a first acute myocardial infarction in Québec. Can. J. Cardiol. 2012, 28, 169–177. [Google Scholar] [CrossRef]
- Trajanovska, A.S.; Kostov, J.; Perevska, Z. Depression in survivors of acute myocardial infarction. Mater. Socio Medica 2019, 31, 110–114. [Google Scholar] [CrossRef] [PubMed]
- Larsen, K.K. Depression following myocardial infarction--an overseen complication with prognostic importance. Dan. Med. J. 2013, 60, B4689. [Google Scholar] [PubMed]
- Echols, M.R.; O’Connor, C.M. Depression after myocardial infarction. Curr. Hear. Fail. Rep. 2010, 7, 185–193. [Google Scholar] [CrossRef] [PubMed]
- Frasure-Smith, N. Depression following myocardial infarction. Impact on 6-month survival. JAMA 1993, 270, 1819–1825. [Google Scholar] [CrossRef]
- Lesperance, F.; Frasure-Smith, N.; Talajic, M.; Bourassa, M.G. Five-year risk of cardiac mortality in relation to initial severity and one-year changes in depression symptoms after myocardial infarction. Circulation 2002, 105, 1049–1053. [Google Scholar] [CrossRef] [Green Version]
- Carney, R.M.; Blumenthal, J.A.; Catellier, D.; E Freedland, K.; Berkman, L.F.; Watkins, L.L.; Czajkowski, S.M.; Hayano, J.; Jaffe, A.S. Depression as a risk factor for mortality after acute myocardial infarction. Am. J. Cardiol. 2003, 92, 1277–1281. [Google Scholar] [CrossRef]
- Serpytis, P.; Navickas, P.; Lukaviciute, L.; Navickas, A.; Aranauskas, R.; Serpytis, R.; Deksnyte, A.; Glaveckaite, S.; Petrulioniene, Z.; Samalavicius, R. Gender-based differences in anxiety and depression following acute myocardial infarction. Arq. Bras. de Cardiol. 2018, 111, 676–683. [Google Scholar] [CrossRef]
- Janzon, E.; Abidi, T.; Bahtsevani, C. Can physical activity be used as a tool to reduce depression in patients after a cardiac event? What is the evidence? A systematic literature study. Scand. J. Psychol. 2015, 56, 175–181. [Google Scholar] [CrossRef]
- Hajna, S.; Kestens, Y.; Daskalopoulou, S.S.; Joseph, L.; Thierry, B.; Sherman, M.; Trudeau, L.; Rabasa-Lhoret, R.; Meissner, L.; Bacon, S.L.; et al. Neighbourhood walkability and home neighbourhood-based physical activity: An observational study of adults with type 2 diabetes. BMC Public Health 2016, 16, 957. [Google Scholar] [CrossRef] [Green Version]
- Creatore, M.I.; Glazier, R.H.; Moineddin, R.; Fazli, G.S.; Johns, A.; Gozdyra, P.; I Matheson, F.; Kaufman-Shriqui, V.; Rosella, L.C.; Manuel, D.G.; et al. Association of neighborhood walkability with change in overweight, obesity, and diabetes. JAMA 2016, 315, 2211. [Google Scholar] [CrossRef] [Green Version]
- Collins, P.; Tait, J.; Fein, A.; Dunn, J.R. Residential moves, neighbourhood walkability, and physical activity: A longitudinal pilot study in Ontario Canada. BMC Public Health 2018, 18, 933. [Google Scholar] [CrossRef] [PubMed]
- Crouse, D.L.; Foroughi, I.; Gupta, N. Neighbourhood environments and the risk of hospital admission for cardiometabolic and mental health comorbidities in multiple sclerosis. Mult. Scler. J. 2020. [Google Scholar] [CrossRef]
- Statistics Canada. Census Profile. 2016 Census. Statistics Canada Catalogue No. 98-316-X2016001; Statistics Canada: Ottawa, ON, Canada, 2017. [Google Scholar]
- Public Health Agency of Canada. Public Health Infobase: Canadian Chronic Disease Surveillance System [Online Database]; Public Health Agency of Canada: Ottawa, ON, Canada, 2019. [Google Scholar]
- Ayles, J.; McDonald, T. Key factors in the establishment of an academia-government center of public sector administrative data and policy research. Int. J. Popul. Data Sci. 2018, 3. [Google Scholar] [CrossRef] [Green Version]
- Doiron, D.; Setton, E.; Seed, E.; Shooshtari, M.; Brook, J. The Canadian Urban Environmental Health Research Consortium (CANUE): A national data linkage initiative. Int. J. Popul. Data Sci. 2018, 3. [Google Scholar] [CrossRef]
- Statistics Canada. Postal Code Conversion File Plus (PCCF+) Version 6D, Reference Guide. Catalogue No. 82-F0086-XDB; Statistics Canada: Ottawa, ON, Canada, 2016. [Google Scholar]
- Khan, S.; Pinault, L.; Tjepkema, M.; Wilkins, R. Positional accuracy of geocoding from residential postal codes versus full street addresses. Public Health Rep. 2018, 29, 3–9. [Google Scholar]
- Hamm, N.C.; Pelletier, L.; Ellison, J.; Tennenhouse, L.; Reimer, K.; Paterson, J.M.; Puchtinger, R.; Bartholomew, S.; Phillips, K.A.M.; Lix, L.M.; et al. Trends in chronic disease incidence rates from the Canadian Chronic Disease Surveillance System. Health Promot. Chronic Dis. Prev. Can. 2019, 39, 216–224. [Google Scholar] [CrossRef] [Green Version]
- Canadian Institute for Health Information. International Statistical Classification of Diseases and Related Health Problems, 10th Revision, Canada (ICD-10-CA); Canadian Institute for Health Information: Ottawa, ON, Canada, 2009. [Google Scholar]
- McCormick, N.; Lacaille, D.; Bhole, V.; Avina-Zubieta, J.A. Validity of myocardial infarction diagnoses in administrative databases: A systematic review. PLoS ONE 2014, 9, e92286. [Google Scholar] [CrossRef] [PubMed]
- Public Health Agency of Canada. Report from the Canadian Chronic Disease Surveillance System: Mood and Anxiety Disorders in Canada, 2016; Public Health Agency of Canada: Ottawa, ON, Canada, 2016. [Google Scholar]
- O’Donnell, S.; Vanderloo, S.; McRae, L.; Onysko, J.; Patten, S.; Pelletier, L. Comparison of the estimated prevalence of mood and/or anxiety disorders in Canada between self-report and administrative data. Epidemiol. Psychiatr. Sci. 2016, 25, 360–369. [Google Scholar] [CrossRef]
- I Matheson, F.; Dunn, J.R.; Smith, K.L.W.; Moineddin, R.; Glazier, R.H. Development of the Canadian Marginalization Index: A new tool for the study of inequality. Can. J. Public Health 2012, 103, S12–S16. [Google Scholar]
- Christidis, T.; Erickson, A.C.; Pappin, A.J.; Crouse, D.L.; Pinault, L.; Weichenthal, S.; Brook, J.R.; Van Donkelaar, A.; Hystad, P.; Martin, R.V.; et al. Low concentrations of fine particle air pollution and mortality in the Canadian Community Health Survey cohort. Environ. Heal. 2019, 18, 84–86. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Scott, G.M.; Best, C.; Fung, K.; Gupta, M.; Sommer, D.D.; Szeto, C.; Micomonaco, D.C. Impact of marginalization on tobacco use in individuals diagnosed with head and neck Cancer. J. Otolaryngol.-Head Neck Surg. 2019, 48, 54. [Google Scholar] [CrossRef] [PubMed]
- Hermann, T.; Gleckner, W.; A Wasfi, R.; Thierry, B.; Kestens, Y.; A Ross, N. A pan-Canadian measure of active living environments using open data. Public Health Rep. 2019, 30, 16–25. [Google Scholar]
- Ching, J.; Mills, G.; Bechtel, B.; See, L.; Feddema, J.; Wang, X.; Ren, C.; Brousse, O.; Martilli, A.; Neophytou, M.; et al. WUDAPT: An urban weather, climate, and environmental modeling infrastructure for the anthropocene. Bull. Am. Meteorol. Soc. 2018, 99, 1907–1924. [Google Scholar] [CrossRef] [Green Version]
- Stewart, I.D.; Oke, T.R. Local climate zones for urban temperature studies. Bull. Am. Meteorol. Soc. 2012, 93, 1879–1900. [Google Scholar] [CrossRef]
- Qiu, C.; Mou, L.; Schmitt, M.; Zhu, X.X. Local climate zone-based urban land cover classification from multi-seasonal Sentinel-2 images with a recurrent residual network. ISPRS J. Photogramm. Remote. Sens. 2019, 154, 151–162. [Google Scholar] [CrossRef] [PubMed]
- Cohen-Cline, H.; A A Beresford, S.; Barrington, W.E.; Matsueda, R.L.; Wakefield, J.; E Duncan, G. Associations between neighbourhood characteristics and depression: A twin study. J. Epidemiol. Community Health 2018, 72, 202–207. [Google Scholar] [CrossRef]
- Yen, I.H.; Michael, Y.L.; Perdue, L. Neighborhood environment in studies of health of older adults. Am. J. Prev. Med. 2009, 37, 455–463. [Google Scholar] [CrossRef] [Green Version]
- Petkovic, J.; Trawin, J.; Dewidar, O.; Yoganathan, M.; Tugwell, P.; Welch, V. Sex/gender reporting and analysis in Campbell and Cochrane systematic reviews: A cross-sectional methods study. Syst. Rev. 2018, 7, 113. [Google Scholar] [CrossRef] [Green Version]
- Gupta, N.; Crouse, D.L.; Balram, A. Individual and community-level income and the risk of diabetes rehospitalization among women and men: A Canadian population-based cohort study. BMC Public Health 2020, 20, 60. [Google Scholar] [CrossRef] [PubMed]

| Characteristic | (1) All Patients (n = 13,330) | (2) Females (n = 4755) | (3) Males (n = 8580) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| HR | Lower CI | Upper CI | HR | Lower CI | Upper CI | HR | Lower CI | Upper CI | ||
| Sex | ||||||||||
| Female (ref: Male) | 1.58 * | 1.48 | 1.68 | -- | -- | -- | -- | -- | -- | |
| Age group | ||||||||||
| 65–74 years (ref: 45–64 years) | 0.95 | 0.88 | 1.03 | 0.91 | 0.80 | 1.03 | 0.97 | 0.88 | 1.07 | |
| 75+ years | 0.94 * | 0.87 | 1.00 | 0.81 * | 0.72 | 0.91 | 1.05 | 0.96 | 1.16 | |
| Community size | ||||||||||
| Urban (ref: Rural) | 0.91 * | 0.85 | 0.97 | 0.95 | 0.85 | 1.06 | 0.88 * | 0.80 | 0.96 | |
| Neighbourhood material deprivation | ||||||||||
| High (ref: Low) | 1.03 | 0.95 | 1.12 | 1.16 * | 1.01 | 1.33 | 0.95 | 0.85 | 1.06 | |
| Neighbourhood population dependency | ||||||||||
| High (ref: Low) | 1.03 | 0.94 | 1.14 | 0.95 | 0.82 | 1.11 | 1.09 | 0.96 | 1.23 | |
| Neighbourhood residential instability | ||||||||||
| High (ref: Low) | 1.04 | 0.97 | 1.11 | 1.03 | 0.92 | 1.15 | 1.04 | 0.95 | 1.13 | |
| Neighbourhood ethnic concentration | ||||||||||
| High (ref: Low) | 1.11 * | 1.03 | 1.19 | 1.07 | 0.95 | 1.20 | 1.14 * | 1.03 | 1.25 | |
| Neighbourhood active living friendliness | ||||||||||
| High (ref: Low) | 1.01 | 0.92 | 1.10 | 1.01 | 0.88 | 1.15 | 1.00 | 0.89 | 1.12 | |
| Local climate zone | ||||||||||
| Compact high-rise (ref: Lightweight low-rise) | 1.01 | 0.94 | 1.08 | 1.07 | 0.96 | 1.19 | 0.97 | 0.89 | 1.05 | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Foroughi, I.; Gupta, N.; Crouse, D.L. Healthcare Service Use for Mood and Anxiety Disorders Following Acute Myocardial Infarction: A Cohort Study of the Role of Neighbourhood Socioenvironmental Characteristics in a Largely Rural Population. Int. J. Environ. Res. Public Health 2020, 17, 4939. https://doi.org/10.3390/ijerph17144939
Foroughi I, Gupta N, Crouse DL. Healthcare Service Use for Mood and Anxiety Disorders Following Acute Myocardial Infarction: A Cohort Study of the Role of Neighbourhood Socioenvironmental Characteristics in a Largely Rural Population. International Journal of Environmental Research and Public Health. 2020; 17(14):4939. https://doi.org/10.3390/ijerph17144939
Chicago/Turabian StyleForoughi, Ismael, Neeru Gupta, and Dan Lawson Crouse. 2020. "Healthcare Service Use for Mood and Anxiety Disorders Following Acute Myocardial Infarction: A Cohort Study of the Role of Neighbourhood Socioenvironmental Characteristics in a Largely Rural Population" International Journal of Environmental Research and Public Health 17, no. 14: 4939. https://doi.org/10.3390/ijerph17144939






