Urban Stress Indirectly Influences Psychological Symptoms through Its Association with Distress Tolerance and Perceived Social Support among Adults Experiencing Homelessness
Abstract
:1. Introduction
- Greater urban stress would be associated with increased likelihood of psychological symptoms (i.e., depression and PTSD).
- Greater urban stress would be associated with lower distress tolerance, and greater distress tolerance would be associated with decreased likelihood of psychological symptoms. Thus, the negative impact of urban stress on psychological symptoms would be associated through lower distress tolerance.
- Greater urban stress would be associated with lower perceived social support, and greater perceived social support would be associated with decreased likelihood of psychological symptoms. Thus, the negative impact of urban stress on psychological symptoms would be associated via lower social support.
- Lower perceived social support would be associated with lower distress tolerance. The negative impact of urban stress on psychological symptoms would be associated through the impact of social support on distress tolerance.
2. Materials and Methods
2.1. Study Participants and Data Collection
2.2. Measures
2.2.1. Major Depressive Disorder
2.2.2. PTSD Symptoms
2.2.3. Urban Life Stress
2.2.4. Distress Tolerance
2.2.5. Perceived Social Support
2.2.6. Covariates
2.3. Statistical Analysis
3. Results
3.1. Descriptive Analysis
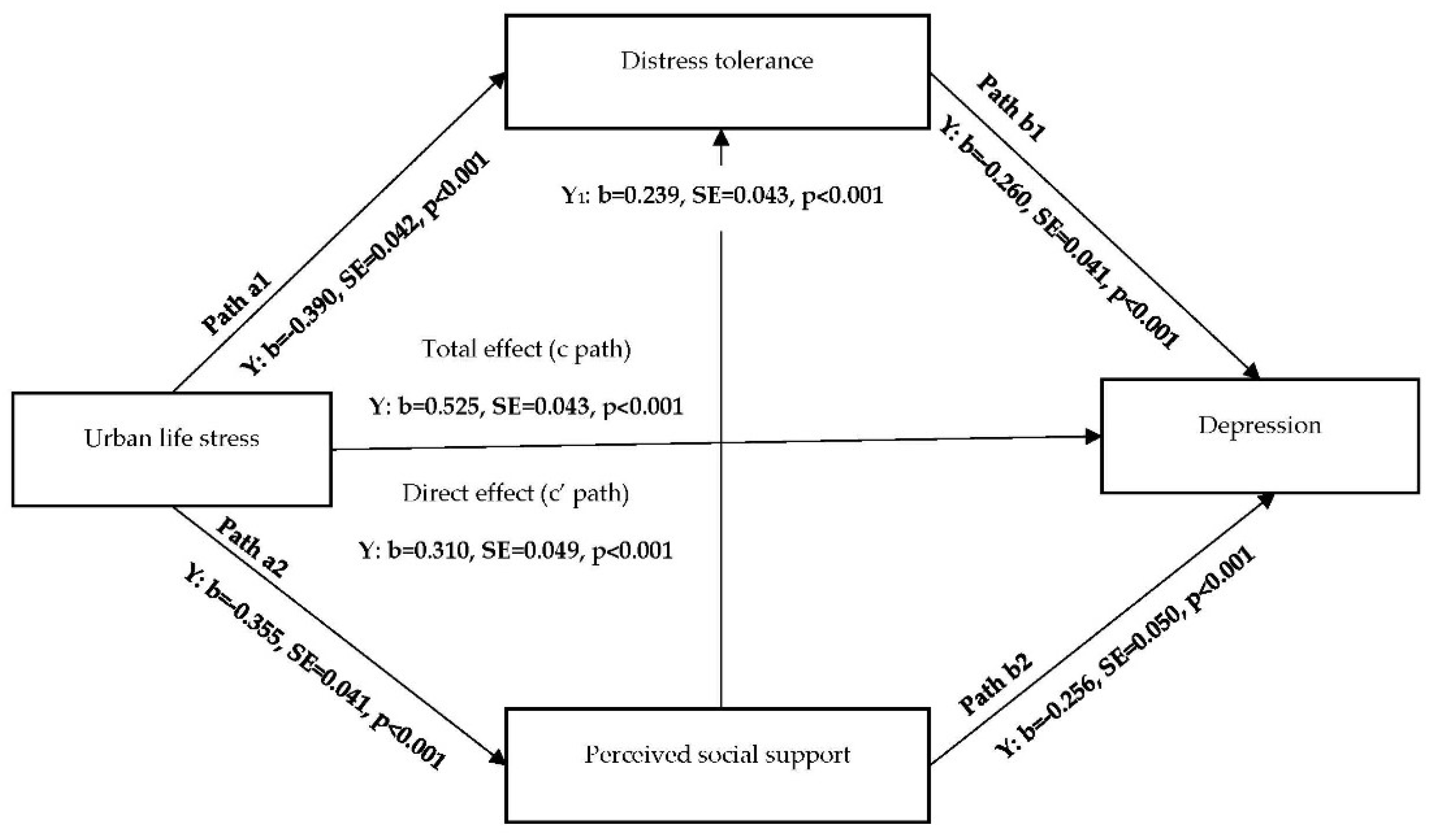
3.2. Indirect Effect Model for Major Depressive Disorder
3.3. Indirect Effect Model for PTSD Symptoms
4. Discussion
Implications for Practice
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Henry, M.; Mahathey, A.; Morrill, T.; Robinson, A.; Shivji, A.; Watt, R.; Associates, A. The 2018 Annual Homeless Assessment Report (AHAR) to Congress. Part. 1: Point-in-Time Estimates of Homelessness; The U.S. Department of Housing and Urban Development, Office of Community Planning and Developement: Washington, DC, USA, 2018.
- Chang, H.L.; Fisher, F.D.; Reitzel, L.R.; Kendzor, D.E.; Nguyen, M.A.; Businelle, M.S. Subjective sleep inadequacy and self-rated health among homeless adults. Am. J. Health Behav. 2015, 39, 14–21. [Google Scholar] [CrossRef] [PubMed]
- Childress, S.; Reitzel, L.R.; Maria, D.S.; Kendzor, D.E.; Moisiuc, A.; Businelle, M.S. Mental illness and substance use problems in relation to homelessness onset. Am. J. Health Behav. 2015, 39, 549–555. [Google Scholar] [CrossRef] [PubMed]
- Sun, S.; Irestig, R.; Burstrom, B.; Beijer, U.; Burstrom, K. Health-related quality of life (EQ-5D) among homeless persons compared to a general population sample in Stockholm County, 2006. Scand. J. Public Health 2012, 40, 115–125. [Google Scholar] [CrossRef] [PubMed]
- Strehlau, V.; Torchalla, I.; Kathy, L.; Schuetz, C.; Krausz, M. Mental health, concurrent disorders, and health care utilization in homeless women. J. Psychiatr. Pract. 2012, 18, 349–360. [Google Scholar] [CrossRef]
- Whitbeck, L.B.; Armenta, B.E.; Gentzler, K.C. Homelessness-related traumatic events and PTSD among women experiencing episodes of homelessness in three U.S. cities. J. Trauma. Stress 2015, 28, 355–360. [Google Scholar] [CrossRef]
- Coohey, C.; Easton, S.D. Distal stressors and depression among homeless men. Health Soc. Work 2016, 41, 111–119. [Google Scholar] [CrossRef]
- Lecic-Tosevski, D. Is urban living good for mental health? Curr. Opin. Psychiatry 2019, 32, 204–209. [Google Scholar] [CrossRef]
- Galea, S.; Ahern, J.; Rudenstine, S.; Wallace, Z.; Vlahov, D. Urban built environment and depression: A multilevel analysis. J. Epidemiol. Community Health 2005, 59, 822–827. [Google Scholar] [CrossRef] [Green Version]
- Nicolaidis, C.; Timmons, V.; Thomas, M.J.; Waters, A.S.; Wahab, S.; Mejia, A.; Mitchell, S.R. “You don’t go tell White people nothing”: African American women’s perspectives on the influence of violence and race on depression and depression care. Am. J. Public Health 2010, 100, 1470–1476. [Google Scholar] [CrossRef]
- Zerger, S.; Bacon, S.; Corneau, S.; Skosireva, A.; McKenzie, K.; Gapka, S.; O’Campo, P.; Sarang, A.; Stergiopoulos, V. Differential experiences of discrimination among ethnoracially diverse persons experiencing mental illness and homelessness. BMC Psychiatry 2014, 14, 353. [Google Scholar] [CrossRef] [Green Version]
- Agrawal, P.; Neisler, J.; Businelle, M.; Kendzor, D.; Hernandez, D.; Odoh, C.; Reitzel, L. Exposure to violence and sleep inadequacies among men and women living in a shelter setting. Health Behav. Res. 2019, 2. [Google Scholar] [CrossRef] [Green Version]
- Wrighting, Q.; Reitzel, L.R.; Chen, T.A.; Kendzor, D.E.; Hernandez, D.C.; Obasi, E.M.; Shree, S.; Businelle, M.S. Characterizing Discrimination Experiences by Race among Homeless Adults. Am. J. Health Behav. 2019, 43, 531–542. [Google Scholar] [CrossRef] [PubMed]
- Zvolensky, M.J.; Bernstein, A.; Vujanovic, A.A. Distress Tolerance: Theory, Research, and Clinical Applications; Guilford Press: New York, NY, USA, 2011. [Google Scholar]
- Leyro, T.M.; Zvolensky, M.J.; Bernstein, A. Distress tolerance and psychopathological symptoms and disorders: A review of the empirical literature among adults. Psychol. Bull. 2010, 136, 576–600. [Google Scholar] [CrossRef] [PubMed]
- Marshall-Berenz, E.C.; Vujanovic, A.A.; Bonn-Miller, M.O.; Bernstein, A.; Zvolensky, M.J. Multimethod study of distress tolerance and PTSD symptom severity in a trauma-exposed community sample. J. Trauma. Stress 2010, 23, 623–630. [Google Scholar] [CrossRef] [Green Version]
- Vujanovic, A.A.; Bonn-Miller, M.O.; Potter, C.M.; Marshall, E.C.; Zvolensky, M.J. An evaluation of the relation between distress tolerance and posttraumatic stress within a trauma-exposed sample. J. Psychopathol. Behav. Assess. 2011, 33, 129–135. [Google Scholar] [CrossRef] [Green Version]
- Vujanovic, A.A.; Hart, A.S.; Potter, C.M.; Berenz, E.C.; Niles, B.; Bernstein, A. Main and interactive effects of distress tolerance and negative affect intensity in relation to PTSD symptoms among trauma-exposed adults. J. Psychopathol. Behav. Assess. 2013, 35, 235–243. [Google Scholar] [CrossRef] [Green Version]
- Reitzel, L.R.; Short, N.A.; Schmidt, N.B.; Garey, L.; Zvolensky, M.J.; Moisiuc, A.; Reddick, C.; Kendzor, D.E.; Businelle, M.S. Distress tolerance links sleep problems with stress and health in homeless. Am. J. Health Behav. 2017, 41, 760–774. [Google Scholar] [CrossRef]
- Hernandez, D.C.; Daundasekara, S.S.; Arlinghaus, K.R.; Sharma, A.P.; Reitzel, L.R.; Kendzor, D.E.; Businelle, M.S. Fruit and vegetable consumption and emotional distress tolerance as potential links between food insecurity and poor physical and mental health among homeless adults. Prev. Med. Rep. 2019, 14, 100824. [Google Scholar] [CrossRef]
- Cohen, S.; Wills, T.A. Stress, social support, and the buffering hypothesis. Psychol. Bull. 1985, 98, 310–357. [Google Scholar] [CrossRef]
- Cohen, S.; Mermelstein, R.; Kamarck, T.; Hoberman, H.M. Measuring the functional components of social support. In Social Support: Theory, Research, and Applications; Sarason, I.G., Sarason, B.R., Eds.; Martinus Nijhoff: The Hague, The Netherlands, 1985; pp. 73–94. [Google Scholar]
- Lakey, B.; Cohen, S. Social support theory and measurement. In Social Support Measurement and Intervention: A Guide for Health and Social Scientists; Cohen, S., Underwood, L.G., Gottlieb, B.H., Eds.; Oxford University Press: Oxford, UK, 2000; pp. 29–52. [Google Scholar]
- Gallo, L.C.; Fortmann, A.L.; McCurley, J.L.; Isasi, C.R.; Penedo, F.J.; Daviglus, M.L.; Roesch, S.C.; Talavera, G.A.; Gouskova, N.; Gonzalez, F.; et al. Associations of structural and functional social support with diabetes prevalence in U.S. Hispanics/Latinos: Results from the HCHS/SOL Sociocultural Ancillary Study. J. Behav. Med. 2015, 38, 160–170. [Google Scholar] [CrossRef] [Green Version]
- Hernandez, D.C.; Reitzel, L.R.; Wetter, D.W.; McNeill, L.H. Social support and cardiovascular risk factors among black adults. Ethn. Dis 2014, 24, 444–450. [Google Scholar] [PubMed]
- White, A.M.; Philogene, G.S.; Fine, L.; Sinha, S. Social support and self-reported health status of older adults in the United States. Am. J. Public Health 2009, 99, 1872–1878. [Google Scholar] [CrossRef] [PubMed]
- La Gory, M.; Ferris, R.; Fitzpatrick, K. Homelessness and affiliation. Sociol. Q. 1991, 32, 201–218. [Google Scholar] [CrossRef]
- Fischer, P.J.; Shapiro, S.; Breakey, W.R.; Anthony, J.C.; Kramer, M. Mental health and social characteristics of the homeless: A survey of mission users. Am. J. Public Health 1986, 76, 519–524. [Google Scholar] [CrossRef] [PubMed]
- Durbin, A.; Nisenbaum, R.; Kopp, B.; O’Campo, P.; Hwang, S.W.; Stergiopoulos, V. Are resilience and perceived stress related to social support and housing stability among homeless adults with mental illness? Health Soc. Care Community 2019, 27, 1053–1062. [Google Scholar] [CrossRef]
- Hwang, S.W.; Kirst, M.J.; Chiu, S.; Tolomiczenko, G.; Kiss, A.; Cowan, L.; Levinson, W. Multidimensional social support and the health of homeless individuals. J. Urban Health 2009, 86, 791–803. [Google Scholar] [CrossRef] [Green Version]
- Baek, R.N.; Tanenbaum, M.L.; Gonzalez, J.S. Diabetes burden and diabetes distress: The buffering effect of social support. Ann. Behav. Med. 2014, 48, 145–155. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carpenter, K.M.; Fowler, J.M.; Maxwell, G.L.; Andersen, B.L. Direct and buffering effects of social support among gynecologic cancer survivors. Ann. Behav. Med. 2010, 39, 79–90. [Google Scholar] [CrossRef] [Green Version]
- Puterman, E.; Epel, E.S.; O’Donovan, A.; Prather, A.A.; Aschbacher, K.; Dhabhar, F.S. Anger is associated with increased IL-6 stress reactivity in women, but only among those low in social support. Int. J. Behav. Med. 2014, 21, 936–945. [Google Scholar] [CrossRef] [Green Version]
- Marroquin, B. Interpersonal emotion regulation as a mechanism of social support in depression. Clin. Psychol. Rev. 2011, 31, 1276–1290. [Google Scholar] [CrossRef]
- Cohen, J.R.; Danielson, C.K.; Adams, Z.W.; Ruggiero, K.J. Distress tolerance and social support in adolescence: Predicting risk for internalizing and externalizing symptoms following a natural disaster. J. Psychopathol. Behav. Assess. 2016, 38, 538–546. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mohammadzadeh Ebrahimi, A.; Rahimi Pordanjani, T.; Tad, H. Structural Model of Social Support and Distress Tolerance by Mental Health Mediation in Elderlies With Cardiovascular Disease. Health Res. J. 2019, 4, 189–196. [Google Scholar] [CrossRef] [Green Version]
- Nyamathi, A.; Leake, B.; Keenan, C.; Gelberg, L. Type of social support among homeless women: Its impact on psychosocial resources, health and health behaviors, and use of health services. Nurs. Res. 2000, 49, 318–326. [Google Scholar] [CrossRef] [PubMed]
- Davis, T.C.; Long, S.W.; Jackson, R.H.; Mayeaux, E.; George, R.B.; Murphy, P.W.; Crouch, M.A. Rapid estimate of adult literacy in medicine: A shortened screening instrument. Fam. Med. 1993, 25, 391–395. [Google Scholar] [PubMed]
- Murphy, P.W.; Davis, T.C.; Long, S.W.; Jackson, R.H.; Decker, B.C. Rapid estimate of adult literacy in medicine (REALM): A quick reading test for patients. J. Read. 1993, 37, 124–130. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Patient Health Questionnaire Primary Care Study Group. Validation and utility of a self-report version of PRIME-MD: The PHQ primary care study. JAMA 1999, 282, 1737–1744. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kroenke, K.; Strine, T.W.; Spitzer, R.L.; Williams, J.B.; Berry, J.T.; Mokdad, A.H. The PHQ-8 as a measure of current depression in the general population. J. Affect. Disord. 2009, 114, 163–173. [Google Scholar] [CrossRef]
- Prins, A.; Ouimette, P.; Kimerling, R.; Cameron, R.P.; Hugelshofer, D.S.; Shaw-Hegwer, J.; Thraikill, A.; Gusman, F.D.; Sheikh, J.I. The primary care PTSD screen (PC-PTSD): Development and operating characteristics. Prim. Care Psychiatry 2003, 9, 9–14. [Google Scholar] [CrossRef]
- Jaffee, K.D.; Liu, G.C.; Canty-Mitchell, J.; Qi, R.A.; Austin, J.; Swigonski, N. Race, urban community stressors, and behavioral and emotional problems of children with special health care needs. Psychiatr. Serv. 2005, 56, 63–69. [Google Scholar] [CrossRef] [Green Version]
- Simons, J.S.; Gaher, R.M. The distress tolerance scale: Development and validation of a self-report measure. Motiv. Emot. 2005, 29, 83–102. [Google Scholar] [CrossRef]
- Cohen, S.; Kamarck, T.; Mermelstein, R. A global measure of perceived stress. J. Health Soc. Behav. 1983, 24, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Burke, C.; Johnson, E.E.; Bourgault, C.; Borgia, M.; O’Toole, T.P. Losing work: Regional unemployment and its effect on homeless demographic characteristics, needs, and health care. J. Health Care Poor Underserved 2013, 24, 1391–1402. [Google Scholar] [CrossRef] [PubMed]
- Winetrobe, H.; Wenzel, S.; Rhoades, H.; Henwood, B.; Rice, E.; Harris, T. Differences in Health and Social Support between Homeless Men and Women Entering Permanent Supportive Housing. Women’s Health Issues 2017, 27, 286–293. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baggett, T.P.; Campbell, E.G.; Chang, Y.; Magid, L.M.; Rigotti, N.A. Posttraumatic Stress Symptoms and Their Association With Smoking Outcome Expectancies Among Homeless Smokers in Boston. Nicotine Tob. Res. 2016, 18, 1526–1532. [Google Scholar] [CrossRef] [Green Version]
- Zima, B.T.; Wells, K.B.; Benjamin, B.; Duan, N. Mental Health Problems Among Homeless Mothers: Relationship to Service Use and Child Mental Health Problems. Arch. Gen. Psychiatry 1996, 53, 332–338. [Google Scholar] [CrossRef]
- Wong, Y.-L.I.; Piliavin, I. Stressors, resources, and distress among homeless persons: A longitudinal analysis. Soc. Sci. Med. 2001, 52, 1029–1042. [Google Scholar] [CrossRef]
- IBM Corp. IBM SPSS Statistics for Windows; Version 26.0; IBM Corp: Armonk, NY, USA, 2019. [Google Scholar]
- Kelley, K. The effects of nonnormal distributions on confidence intervals around the standardized mean difference: Bootstrap and parametric confidence intervals. Educ. Psychol. Meas. 2005, 65, 51–69. [Google Scholar] [CrossRef]
- Muthén, L.K.; Muthén, B.O. Mplus User’s Guide, 8th ed.; Muthén & Muthén: Los Angeles, CA, USA, 2017. [Google Scholar]
- Preacher, K.J.; Hayes, A.F. Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behav. Res. Methods 2008, 40, 879–891. [Google Scholar] [CrossRef]
- VanGeest, J.B.; Johnson, T.P. Substance use patterns among homeless migrants and nonmigrants in Chicago. Subst. Use Misuse 1997, 32, 877–907. [Google Scholar] [CrossRef]
- Garey, L.; Reitzel, L.R.; Neisler, J.; Kendzor, D.E.; Zvolensky, M.J.; Neighbors, C.; Hernandez, D.C.; Businelle, M.S. Health-Related Quality of Life Among Homeless Smokers: Risk and Protective Factors of Latent Class Membership. Behav. Med. 2019, 45, 40–51. [Google Scholar] [CrossRef]
- Richards, R.; Smith, C. Shelter environment and placement in community affects lifestyle factors among homeless families in Minnesota. Am. J. Health Promot. AJHP 2006, 21, 36–44. [Google Scholar] [CrossRef] [PubMed]
- Bassuk, E.L.; Weinreb, L.F.; Buckner, J.C.; Browne, A.; Salomon, A.; Bassuk, S.S. The characteristics and needs of sheltered homeless and low-income housed mothers. JAMA 1996, 276, 640–646. [Google Scholar] [CrossRef] [PubMed]
- Solarz, A.; Bogat, G.A. When social support fails: The homeless. J. Community Psychol. 1990, 18, 79–96. [Google Scholar] [CrossRef]
- Segal, Z.V.; Williams, J.M.G.; Teasdale, J. Mindfulness-Based Cognitive Therapy for Depression; Guilford Publications: New York, NY, USA, 2012. [Google Scholar]
- Wong, S.-L. Flash Technique Group Protocol for Highly Dissociative Clients in a Homeless Shelter: A Clinical Report. J. EMDR Pract. Res. 2019, 13, 20–31. [Google Scholar] [CrossRef]
- Hansen, K.; Lloyd, J.; Stough, C. Emotional intelligence and clinical disorders. In Assessing Emotional Intelligence. The Springer Series on Human Exceptionality; Parker, J., Saklofske, D., Stough, C., Eds.; Springer: Boston, MA, USA, 2009. [Google Scholar]
- Casper, L.M.; Hogan, D.P. Family networks in prenatal and postnatal health. Soc. Biol. 1990, 37, 84–101. [Google Scholar] [CrossRef] [PubMed]
- Schilling, R.F.; el-Bassel, N.; Schinke, S.P.; Gordon, K.; Nichols, S. Building skills of recovering women drug users to reduce heterosexual AIDS transmission. Public Health Rep. 1991, 106, 297–304. [Google Scholar]
- Toro, P.A.; Tulloch, E.; Ouellette, N. Stress, social support, and outcomes in two probability samples of homeless adults. J. Community Psychol. 2008, 36, 483–498. [Google Scholar] [CrossRef]
- Nyamathi, A.; Flaskerud, J.; Leake, B. HIV-risk behaviors and mental health characteristics among homeless or drug-recovering women and their closest sources of social support. Nurs. Res. 1997, 46, 133–137. [Google Scholar] [CrossRef]
- O’Campo, P.; Kirst, M.; Schaefer-McDaniel, N.; Firestone, M.; Scott, A.; McShane, K. Community-Based Services for Homeless Adults Experiencing Concurrent Mental Health and Substance Use Disorders: A Realist Approach to Synthesizing Evidence. J. Urban Health 2009, 86, 965. [Google Scholar] [CrossRef] [Green Version]

| Characteristics | N (%) or Mean (SD) |
|---|---|
| Mental health outcomes | |
| Depression | 174 (30.7%) |
| PTSD symptoms | 184 (32.5%) |
| Predictor variable | |
| Urban life stress | 48.92 (14.86) |
| Mediator variables | |
| Distress tolerance | 3.10 (0.98) |
| Perceived social support | 32.95 (8.73) |
| Socio-demographic characteristics | |
| Age (years) | 43.56 (12.0) |
| Sex | |
| Male | 360 (63.5%) |
| Female | 207 (36.5%) |
| Race/ethnicity | |
| White/non-minority | 321 (56.6%) |
| Minority | 246 (43.4%) |
| Marital status | |
| Married | 70 (12.4%) |
| Not married | 497 (87.6%) |
| Education | |
| Less than high school diploma | 147 (25.9%) |
| High school diploma or higher | 420 (74.1%) |
| Employment status | |
| Employed | 66 (11.6%) |
| Unemployed/disability limiting employment | 501 (88.4%) |
| Sources of income | |
| No source of income | 305 (53.8%) |
| Have at least one source of income | 262 (46.2%) |
| Health insurance | |
| No health insurance | 399 (70.4%) |
| Insured to any extent | 168 (29.6%) |
| Health behaviors | |
| Alcohol abuse/dependence | 155 (27.3%) |
| Current smoker | 444 (78.3%) |
| Homelessness characteristics | |
| Total amount of time homeless (years) | 3.17 (4.31) |
| Shelter services utilization (number of services used) | 4.48 (2.52) |
| Variables | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|
| Main study variables | |||||
| Depression | 1.00 | ||||
| PTSD symptoms | 0.41 *** | 1.00 | |||
| Urban life stress | 0.42 *** | 0.38 *** | 1.00 | ||
| Distress tolerance | −0.40 *** | −0.30 *** | −0.49 *** | 1.00 | |
| Perceived social support | −0.37 *** | −0.24 *** | −0.35 *** | 0.36 *** | 1.00 |
| Covariates | |||||
| Age | 0.05 | 0.04 | 0.02 | 0.02 | −0.10 * |
| Sex (Female) | 0.11 * | 0.16 *** | 0.10 * | −0.10 * | 0.07 |
| Race/ethnicity (White/non-minority) | 0.09 * | 0.01 | 0.01 | −0.01 | −0.05 |
| Marital status (Married) | −0.04 | −0.08 | −0.001 | −0.02 | 0.13 ** |
| Education (Less than high school) | −0.01 | −0.06 | 0.06 | −0.12 ** | −0.07 |
| Employment (unemployed) | 0.06 | 0.03 | 0.08 * | −0.02 | −0.06 |
| Income (no source of income) | 0.04 | −0.02 | −0.01 | −0.06 | −0.01 |
| Health insurance (uninsured) | −0.05 | −0.06 | 0.02 | −0.04 | 0.07 |
| Alcohol abuse/dependence | 0.06 | 0.13 ** | 0.17 *** | −0.12 ** | −0.09 * |
| Current smoker | 0.04 | 0.06 | 0.03 | -0.06 | −0.04 |
| Total amount of time homeless | −0.02 | 0.06 | 0.02 | 0.001 | −0.08 |
| Shelter services utilization | 0.01 | 0.04 | 0.02 | −0.01 | 0.02 |
| Indirect Effect | b | SE | 95% Bootstrap CI |
|---|---|---|---|
| Urban life stress → Distress tolerance → Depression | 0.101 | 0.022 | 0.061, 0.147 |
| Urban life stress → Perceived social support → Depression | 0.091 | 0.020 | 0.053, 0.133 |
| Urban life stress → Perceived social support → Distress tolerance → Depression | 0.022 | 0.007 | 0.011, 0.037 |
| Indirect Effect | b | SE | 95% Bootstrap CI |
|---|---|---|---|
| Urban life stress → Distress tolerance → PTSD symptoms | 0.065 | 0.022 | 0.023, 0.112 |
| Urban life stress → Perceived social support → PTSD symptoms | 0.043 | 0.019 | 0.006, 0.082 |
| Urban life stress → Perceived social support → Distress tolerance → PTSD symptoms | 0.014 | 0.006 | 0.005, 0.026 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hernandez, D.C.; Daundasekara, S.S.; Zvolensky, M.J.; Reitzel, L.R.; Maria, D.S.; Alexander, A.C.; Kendzor, D.E.; Businelle, M.S. Urban Stress Indirectly Influences Psychological Symptoms through Its Association with Distress Tolerance and Perceived Social Support among Adults Experiencing Homelessness. Int. J. Environ. Res. Public Health 2020, 17, 5301. https://doi.org/10.3390/ijerph17155301
Hernandez DC, Daundasekara SS, Zvolensky MJ, Reitzel LR, Maria DS, Alexander AC, Kendzor DE, Businelle MS. Urban Stress Indirectly Influences Psychological Symptoms through Its Association with Distress Tolerance and Perceived Social Support among Adults Experiencing Homelessness. International Journal of Environmental Research and Public Health. 2020; 17(15):5301. https://doi.org/10.3390/ijerph17155301
Chicago/Turabian StyleHernandez, Daphne C., Sajeevika S. Daundasekara, Michael J. Zvolensky, Lorraine R. Reitzel, Diane Santa Maria, Adam C. Alexander, Darla E. Kendzor, and Michael S. Businelle. 2020. "Urban Stress Indirectly Influences Psychological Symptoms through Its Association with Distress Tolerance and Perceived Social Support among Adults Experiencing Homelessness" International Journal of Environmental Research and Public Health 17, no. 15: 5301. https://doi.org/10.3390/ijerph17155301







