Cryptosporidium and Cryptosporidiosis: The Perspective from the Gulf Countries
Abstract
:1. Introduction
2. Methods
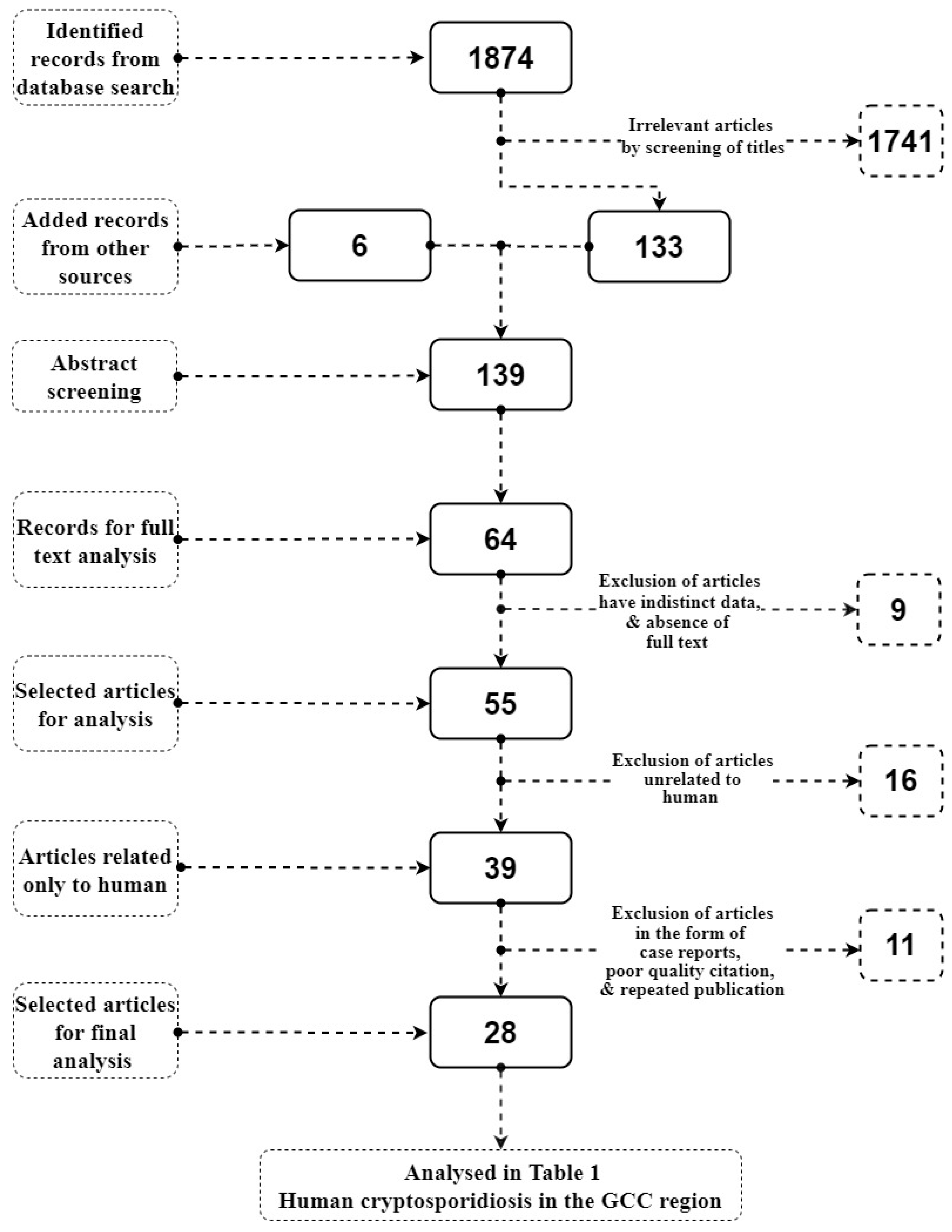
2.1. Search Strategy
2.2. Inclusion and Exclusion Criteria
3. Results and Discussion
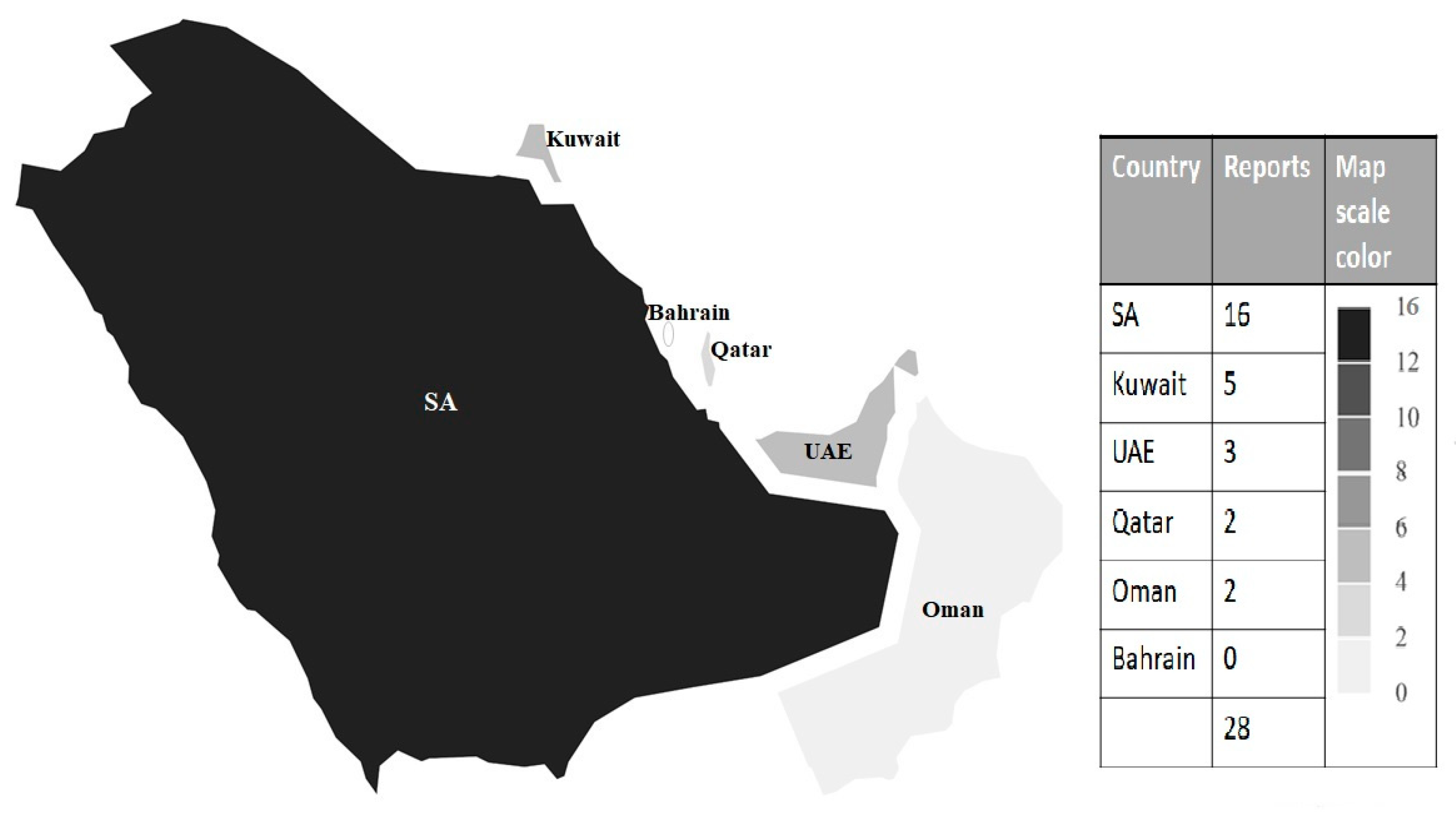
Burden of Cryptosporidium in the GCC Countries
4. Possible Risk Factors in the GCC Countries Associated with the Prevalence of Cryptosporidiosis
4.1. Cryptosporidium Contaminating Water Resources in the GCC Countries
4.2. Animals and Birds Invading Sports Events in the GCC Countries
4.3. Expatriate Labourers in the GCC Countries
4.4. Food as a Vehicle of Foodborne Cryptosporidiosis in the GCC Countries
4.5. Airborne Transmission of Cryptosporidium under Arid Climate Conditions
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Innes, E.A.; Chalmers, R.M.; Wells, B.; Pawlowic, M.C. A one health approach to tackle cryptosporidiosis. Trends Parasitol. 2020, 36, 290–303. [Google Scholar] [CrossRef] [Green Version]
- Efstratiou, A.; Ongerth, J.; Karanis, P. Evolution of monitoring for Giardia and Cryptosporidium in water. Water Res. 2017, 123, 96–112. [Google Scholar] [CrossRef]
- Plutzer, J.; Karanis, P. Genetic polymorphism in Cryptosporidium species: An update. Vet. Parasitol. 2009, 165, 187–199. [Google Scholar] [CrossRef]
- Messner, M.J.; Berger, P. Cryptosporidium infection risk: Results of new dose-response modeling. Risk Anal. 2016, 36, 1969–1982. [Google Scholar] [CrossRef] [PubMed]
- Holubová, N.; Zikmundová, V.; Limpouchová, Z.; Sak, B.; Konečný, R.; Hlásková, L.; Rajský, D.; Kopacz, Z.; McEvoy, J.; Kváč, M. Cryptosporidium proventriculi sp. n. (Apicomplexa: Cryptosporidiidae) in Psittaciformes birds. Eur. J. Protistol. 2019, 69, 70–87. [Google Scholar] [CrossRef] [PubMed]
- Koehler, A.V.; Whipp, M.J.; Haydon, S.R.; Gasser, R.B. Cryptosporidium cuniculus—New records in human and kangaroo in Australia. Parasites Vectors 2014, 7, 492. [Google Scholar] [CrossRef]
- Li, N.; Xiao, L.; Alderisio, K.; Elwin, K.; Cebelinski, E.; Chalmers, R.; Santin, M.; Fayer, R.; Kvac, M.; Ryan, U.; et al. Subtyping Cryptosporidium ubiquitum, a zoonotic pathogen emerging in humans. Emerg. Infect. Dis. 2014, 20, 217–224. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.N.; Sun, Y.; Zhou, H.H.; Lu, G.; Qi, M.; Liu, W.S.; Zhao, W. Prevalence and genotypic identification of Cryptosporidium spp. and Enterocytozoon bieneusi in captive Asiatic black bears (Ursus thibetanus) in Heilongjiang and Fujian provinces of China. BMC Vet. Res. 2020, 16, 84. [Google Scholar] [CrossRef]
- Kopacz, Z.; Kvá, M.; Karpinski, P.; Hendrich, A.B.; Sasiadek, M.M.; Leszczynski, P.; Sak, B.; McEvoy, J.; Kicia, M. The first evidence of Cryptosporidium meleagridis infection in a colon adenocarcinoma from an immunocompetent patient. Front. Cell. Infect. Microbiol. 2019, 9, 35. [Google Scholar] [CrossRef]
- Feng, Y.; Ryan, U.M.; Xiao, L. Genetic diversity and population structure of Cryptosporidium. Trends Parasitol. 2018, 34, 997–1011. [Google Scholar] [CrossRef]
- Khalil, I.A.; Troeger, C.; Rao, P.C.; Blacker, B.F.; Brown, A.; Brewer, T.G.; Colombara, D.V.; De Hostos, E.L.; Engmann, C.; Guerrant, R.L.; et al. Morbidity, mortality, and long-term consequences associated with diarrhoea from Cryptosporidium infection in children younger than 5 years: A meta-analyses study. Lancet Glob. Health 2018, 6, e758–e768. [Google Scholar] [CrossRef] [Green Version]
- Dadonaite, B.; Ritchie, H.; Roser, M. Diarrheal diseases. In Our World in Data. 2020. Available online: https://ourworldindata.org/diarrheal-diseases (accessed on 21 April 2020).
- Karanis, P.; Kourenti, C.; Smith, H. Waterborne transmission of protozoan parasites: A worldwide review of outbreaks and lessons learnt. J. Water Health 2007, 5, 1–38. [Google Scholar] [CrossRef] [PubMed]
- Baldursson, S.; Karanis, P. Waterborne transmission of protozoan parasites: Review of worldwide outbreaks—An update 2004–2010. Water Res. 2011, 45, 6603–6614. [Google Scholar] [CrossRef] [PubMed]
- Efstratiou, A.; Ongerth, J.E.; Karanis, P. Waterborne transmission of protozoan parasites: Review of worldwide outbreaks—An update 2011–2016. Water Res. 2017, 114, 14–22. [Google Scholar] [CrossRef]
- Rosado-García, F.M.; Guerrero-Flórez, M.; Karanis, G.; Hinojosa, M.D.C.; Karanis, P. Water-borne protozoa parasites: The Latin American perspective. Int. J. Hyg. Environ. Health 2017, 220, 783–798. [Google Scholar] [CrossRef]
- Ryan, U.; Hijjawi, N.; Xiao, L. Foodborne cryptosporidiosis. Int. J. Parasitol. 2018, 48, 1–12. [Google Scholar] [CrossRef] [Green Version]
- Ahmed, S.A.; Karanis, P. An overview of methods/techniques for the detection of Cryptosporidium in food samples. Parasitol. Res. 2018, 117, 629–653. [Google Scholar] [CrossRef]
- Ahmed, S.A.; Guerrero Flórez, M.; Karanis, P. The impact of water crises and climate changes on the transmission of protozoan parasites in Africa. Pathog. Glob. Health 2018, 112, 281–293. [Google Scholar] [CrossRef]
- Aldeyarbi, H.M.; Abu El-Ezz, N.M.T.; Karanis, P. Cryptosporidium and cryptosporidiosis: The African perspective. Environ. Sci. Pollut. Res. 2016, 23, 13811–13821. [Google Scholar] [CrossRef]
- GBD 2015 Eastern Mediterranean Region diarrhea collaborators. Burden of diarrhea in the Eastern Mediterranean region, 1990–2015: Findings from the global burden of disease 2015 study. Int. J. Public Health 2018, 63, 109–121. [Google Scholar] [CrossRef]
- Mahmoudi, M.R.; Ongerth, J.E.; Karanis, P. Cryptosporidium and cryptosporidiosis: The Asian perspective. Int. J. Hyg. Environ. Health 2017, 220, 1098–1109. [Google Scholar] [CrossRef] [PubMed]
- Kotloff, K.L.; Platts-Mills, J.A.; Nasrin, D.; Roose, A.; Blackwelder, W.C.; Levine, M.M. Global burden of diarrheal diseases among children in developing countries: Incidence, etiology, and insights from new molecular diagnostic techniques. Vaccine 2017, 35, 6783–6789. [Google Scholar] [CrossRef] [PubMed]
- Kotloff, K.L. The burden and etiology of diarrheal illness in developing countries. Pediatr. Clin. N. Am. 2017, 64, 799–814. [Google Scholar] [CrossRef] [PubMed]
- Kotloff, K.L.; Nataro, J.P.; Blackwelder, W.C.; Nasrin, D.; Farag, T.H.; Panchalingam, S.; Wu, Y.; Sow, S.O.; Sur, D.; Breiman, R.F.; et al. Burden and aetiology of diarrhoeal disease in infants and young children in developing countries (the Global Enteric Multicenter Study, GEMS): A prospective, case-control study. Lancet 2013, 382, 209–222. [Google Scholar] [CrossRef]
- Sow, S.O.; Muhsen, K.; Nasrin, D.; Blackwelder, W.C.; Wu, Y.; Farag, T.H.; Panchalingam, S.; Sur, D.; Zaidi, A.K.M.; Faruque, A.S.G.; et al. The burden of Cryptosporidium diarrheal disease among children < 24 months of age in moderate/high mortality regions of Sub-Saharan Africa and South Asia, utilizing data from the Global Enteric Multicenter Study (GEMS). PLoS Negl. Trop. Dis. 2016, 10, e0004729. [Google Scholar]
- Monge, S.; Pijnacker, R.; Van Pelt, W.; Franz, E.; Kortbeek, L.M.; Mangen, M.J.J. Accounting for long-term manifestations of Cryptosporidium spp infection in burden of disease and cost-of-illness estimations, the Netherlands (2013–2017). PLoS ONE 2019, 14, e0213752. [Google Scholar] [CrossRef] [Green Version]
- CDC. Crypto Outbreaks Linked to Swimming Have Doubled since 2014. 2017. Available online: https://www.cdc.gov/media/releases/2017/p0518-cryptosporidium-outbreaks.html (accessed on 18 March 2020).
- Bouzid, M.; Kintz, E.; Hunter, P.R. Risk factors for Cryptosporidium infection in low and middle income countries: A systematic review and meta-analysis. PLoS Negl. Trop. Dis. 2018, 12, e0006553. [Google Scholar] [CrossRef]
- Putignani, L.; Menichella, D. Global distribution, public health and clinical impact of the protozoan pathogen Cryptosporidium. Interdiscip. Perspect. Infect. Dis. 2010, 2010, 753512. [Google Scholar] [CrossRef] [Green Version]
- Fletcher, S.M.; Stark, D.; Harkness, J.; Ellis, J. Enteric protozoa in the developed world: A public health perspective. Clin. Microbiol. Rev. 2012, 25, 420–449. [Google Scholar] [CrossRef] [Green Version]
- Saif, O.; Mezher, T.; Arafat, H.A. Water security in the GCC countries: Challenges and opportunities. J. Environ. Stud. Sci. 2014, 4, 329–346. [Google Scholar] [CrossRef]
- Alrouh, H.; Ismail, A.; Cheema, S. Demographic and health indicators in Gulf Cooperation Council nations with an emphasis on Qatar. J. Local Glob. Health Perspect. 2013, 2013, 3. [Google Scholar] [CrossRef] [Green Version]
- Raof, M. Climate Change Threats, Opportunities, and the GCC Countries. Available online: https://www.mei.edu/publications/climate-change-threats-opportunities-and-gcc-countries (accessed on 18 March 2020).
- Ben Hassen, T.; El Bilali, H. Food security in the Gulf Cooperation Council countries: Challenges and prospects. J. Food Secur. 2019, 7, 159–169. [Google Scholar] [CrossRef]
- Sherif, M. Water availability and quality in the Gulf Cooperation Council countries: Implications for public health. Asia Pac. J. Public Health 2010, 22, 40S–47S. [Google Scholar] [CrossRef] [PubMed]
- Efron, S.; Fromm, C.; Gelfeld, B.; Nataraj, S.; Sova, C. Food Security in the Gulf Cooperation Council. Available online: https://www.rand.org/content/dam/rand/pubs/external_publications/EP60000/EP67748/RAND_EP67748.pdf (accessed on 14 April 2020).
- Lake, I.R.; Bentham, G.; Kovats, R.S.; Nichols, G.L. Effects of weather and river flow on cryptosporidiosis. J. Water Health 2005, 3, 469–474. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Iqbal, J.; Hira, P.R.; Al-Ali, F.; Philip, R. Cryptosporidiosis in Kuwaiti children: Seasonality and endemicity. Clin. Microbiol. Infect. 2001, 7, 261–266. [Google Scholar] [CrossRef] [Green Version]
- Hawash, Y.; Ghonaim, M.; Hussein, Y.; Alhazmi, A.; Alturkistani, A. Identification of Giardia lamblia and the human infectious-species of Cryptosporidium in drinking water resources in Western Saudi Arabia by nested-PCR assays. Trop. Biomed. 2015, 32, 216–224. [Google Scholar]
- Riddle, M.S.; Savarino, S.J.; Sanders, J.W. Review article: Gastrointestinal infections in deployed forces in the middle east theater: An historical 60 year perspective. Am. J. Trop. Med. Hyg. 2015, 93, 912–917. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sanders, J.W.; Putnam, S.D.; Riddle, M.S.; Tribble, D.R. Military importance of diarrhea: Lessons from the Middle East. Curr. Opin. Gastroenterol. 2005, 21, 9–14. [Google Scholar]
- IAMAT, International Association for Medical Assistance to Travellers. Saudi Arabia General Health Risks: Travellers’ Diarrhea. 2020. Available online: https://www.iamat.org/country/saudi-arabia/risk/traveller-s-diarrhea (accessed on 20 April 2020).
- Harb, A.; O’Dea, M.; Abraham, S.; Habib, I. Childhood diarrhoea in the Eastern Mediterranean region with special emphasis on non-typhoidal Salmonella at the human–food interface. Pathogens 2019, 8, 60. [Google Scholar] [CrossRef] [Green Version]
- Boughattas, S.; Behnke, J.M.; Al-Sadeq, D.; Ismail, A.; Abu-Madi, M. Cryptosporidium spp., prevalence, molecular characterisation and socio-demographic risk factors among immigrants in Qatar. PLoS Negl. Trop. Dis. 2019, 13, e0007750. [Google Scholar] [CrossRef]
- Boughattas, S.; Behnke, J.M.; Al-Ansari, K.; Sharma, A.; Abu-Alainin, W.; Al-Thani, A.; Abu-Madi, M.A. Molecular analysis of the enteric protozoa associated with acute diarrhea in hospitalized children. Front. Cell. Infect. Microbiol. 2017, 7, 343. [Google Scholar] [CrossRef] [PubMed]
- Al-Rifai, R.H.; Loney, T.; Sheek-Hussein, M.; Zoughbor, S.; Ajab, S.; Olanda, M.; Al-Rasbi, Z. Prevalence of, and factors associated with intestinal parasites in multinational expatriate workers in Al Ain City, United Arab Emirates: An occupational cross-sectional study. J. Immigr. Minor. Health 2019, 22, 359–374. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Elbakri, A.; Mogane, L.; Ezzedine, S.; Potgieter, N.; Bessong, P.; AbuOdeh, R.; Samie, A. Prevalence of Cryptosporidium spp. among asymptomatic healthy expatriate workers in Sharjah, United Arab Emirates. J. Infect. Dis. 2018, 12, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Iqbal, J.; Khalid, N.; Hira, P.R. Cryptosporidiosis in kuwaiti children: Association of clinical characteristics with cryptosporidium species and subtypes. J. Med. Microbiol. 2011, 60, 647–652. [Google Scholar] [CrossRef] [Green Version]
- Sulaiman, I.M.; Hira, P.R.; Zhou, L.; Al-Ali, F.M.; Al-Shelahi, F.A.; Shweiki, H.M.; Iqbal, J.; Khalid, N.; Xiao, L. Unique endemicity of cryptosporidiosis in children in Kuwait. J. Clin. Microbiol. 2005, 43, 2805–2809. [Google Scholar] [CrossRef] [Green Version]
- Al-Shammari, S.; Khoja, T.; El-Khwasky, F.; Gad, A. Intestinal parasitic diseases in Riyadh, Saudi Arabia: Prevalence, sociodemographic and environmental associates. Trop. Med. Int. Health 2001, 6, 184–189. [Google Scholar] [CrossRef] [Green Version]
- Cochrane, L.; Amery, H.A. Gulf Cooperation Council countries and the global land grab. Arab World Geogr. 2017, 20, 17–41. [Google Scholar]
- Abu-Madi, M.A.; Behnke, J.M.; Ismail, A. Patterns of infection with intestinal parasites in Qatar among food handlers and housemaids from different geographical regions of origin. Acta Trop. 2008, 106, 213–220. [Google Scholar] [CrossRef]
- Lalonde, L.F.; Gajadhar, A.A. Detection of Cyclospora cayetanensis, Cryptosporidium spp., and Toxoplasma gondii on imported leafy green vegetables in Canadian survey. Food Waterborne Parasitol. 2016, 2, 8–14. [Google Scholar] [CrossRef] [Green Version]
- Li, X.; Zhang, X.; Jian, Y.; Wang, G.; Ma, L.; Schou, C.; Karanis, P. Detection of Cryptosporidium oocysts and Giardia cysts in vegetables from street markets from the Qinghai Tibetan Plateau Area in China. Parasitol. Res. 2020, 119, 1847–1855. [Google Scholar] [CrossRef]
- Checkley, W.; White, A.C.; Jaganath, D.; Arrowood, M.J.; Chalmers, R.M.; Chen, X.-M.; Fayer, R.; Griffiths, J.K.; Guerrant, R.L.; Hedstrom, L.; et al. A review of the global burden, novel diagnostics, therapeutics, and vaccine targets for Cryptosporidium. Lancet Infect. Dis. 2015, 15, 85–94. [Google Scholar] [CrossRef] [Green Version]
- Varkey, P.; Jerath, A.U.; Bagniewski, S.; Lesnick, T. Intestinal parasitic infection among new refugees to Minnesota, 1996–2001. Travel Med. Infect. Dis. 2007, 5, 223–229. [Google Scholar] [CrossRef] [PubMed]
- Infection Prevention and Control Manual. Available online: https://www.moh.gov.sa/CCC/Documents/GCC%20Infection%20control%20manual%202013%20revisedOPT.pdf (accessed on 22 March 2020).
- Memish, Z.A.; Zumla, A.; Alhakeem, R.F.; Assiri, A.; Turkestani, A.; Al Harby, K.D.; Alyemni, M.; Dhafar, K.; Gautret, P.; Barbeschi, M.; et al. Hajj: Infectious disease surveillance and control. Lancet 2014, 383, 2073–2082. [Google Scholar] [CrossRef]
- Al-Harthi, S.A.; Jamjoom, M.B. Enteroparasitic occurrence in stools from residents in Southwestern region of Saudi Arabia before and during Umrah season. Saudi Med. J. 2007, 28, 386–389. [Google Scholar] [PubMed]
- Albert, M.J.; Rotimi, V.O.; Iqbal, J.; Chehadeh, W. Evaluation of the xTAG gastrointestinal pathogen panel assay for the detection of enteric pathogens in Kuwait. Med. Princ. Pract. 2016, 25, 472–476. [Google Scholar] [CrossRef]
- Daoud, A.S.; Zaki, M.; Pugh, R.N.; Al-Mutairi, G.; Al-Ali, F.; El-Saleh, Q. Cryptosporidium gastroenteritis in immunocompetent children from Kuwait. Trop. Geogr. Med. 1990, 42, 113–118. [Google Scholar]
- Idris, M.; Al-Jabri, A. Usefulness of Kato-Katz and trichrome staining as diagnostic methods for parasitic infections in clinical laboratories. J. Sci. Res. Med. Sci. 2001, 3, 65–68. [Google Scholar]
- Windsor, J.; El-Shafie, S.; Welch, S.; Al-Toqui, F. Cryptosporidiosis in Children from the Sultanate of Oman. Sultan Qaboos Univ. Med. J. 1999, 1, 59–62. [Google Scholar]
- Khan, Z.H.; Namnyak, S.S.; Al Jama, A.A.; Madan, I. Prevalence of cryptosporidiosis in Dammam and Alkhobar, Saudi Arabia. Ann. Trop. Paediatr. 1988, 8, 170–172. [Google Scholar] [CrossRef]
- Hawash, Y.; Dorgham, L.S.; Al-Hazmi, A.S.; Al-Ghamdi, M.S. Prevalence of Cryptosporidium-associated diarrhea in a high altitude–community of Saudi Arabia detected by conventional and molecular methods. Korean J. Parasitol. 2014, 52, 479–485. [Google Scholar] [CrossRef]
- Areeshi, M. Cryptosporidiosis in Two Regions of Saudi Arabia; British Library EThOS: Liverpool, UK, 2008. [Google Scholar]
- Hawash, Y.A.; Ismail, K.A.; Almehmadi, M. High frequency of enteric protozoan, viral, and bacterial potential pathogens in community-acquired acute diarrheal episodes: Evidence based on results of Luminex gastrointestinal pathogen panel assay. Korean J. Parasitol. 2017, 55, 513–521. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Elsafi, S.H.; Al-Sheban, S.S.; Al-Jubran, K.M.; Abu Hassan, M.M.; Al Zahrani, E.M. Comparison of Kinyoun’s acid-fast and immunofluorescent methods detected an unprecedented occurrence of Cryptosporidium in the Eastern region of Saudi Arabia. J. Taibah Univ. Med. Sci. 2014, 9, 263–267. [Google Scholar] [CrossRef] [Green Version]
- El-Malky, M.M.; Mowafy, N.M.; Zaghloul, D.A.; Al-Harthi, S.A.; El-Bali, M.A.; Mohamed, R.T.; Bakri, R.A.; Mohamed, A.A.; Elmedany, S. Prevalence of Cryptosporidium species isolated from diarrheic children in Makkah, Saudi Arabia. Trop. Biomed. 2018, 35, 76–81. [Google Scholar]
- Al Braiken, F.A.; Amin, A.; Beeching, N.J.; Hommel, M.; Hart, C.A. Detection of Cryptosporidium amongst diarrhoeic and asymptomatic children in Jeddah, Saudi Arabia. Ann. Trop. Med. Parasitol. 2003, 97, 505–510. [Google Scholar] [CrossRef]
- Al-Megrin, W.A.I. Intestinal parasites infection among immunocompromised patients in Riyadh, Saudi Arabia. Pak. J. Biol. Sci. 2010, 13, 390–394. [Google Scholar] [CrossRef] [Green Version]
- Bolbol, A.S. Cryptosporidiosis in young children suffering from diarrhoea in Riyadh, Saudi Arabia. J. Hyg. Epidemiol. Microbiol. Immunol. 1992, 36, 396–400. [Google Scholar]
- Fareid, M.A.; Alshankyty, I.M.; Omar, H.A. Prevalence of intestinal parasitic and bacterial pathogens in diarrhoeal and non-diarrhoeal school children’s at Hail, Saudi. N. Y. Sci. J. 2011, 4, 106–113. [Google Scholar]
- Sanad, M.M.; Al-Malki, J.S. Cryptosporidiosis among immunocompromised patients in Saudi Arabia. J. Egypt. Soc. Parasitol. 2007, 37, 765–774. [Google Scholar]
- Amer, O.S.O.; Al-Malki, E.S.; Waly, M.I.; AlAgeel, A.; Lubbad, M.Y. Prevalence of Intestinal parasitic infections among patients of King Fahd Medical City in Riyadh region, Saudi Arabia: A 5-year retrospective study. J. Parasitol. Res. 2018, 2018, 8076274. [Google Scholar] [CrossRef]
- Shalaby, I.; Gherbawy, Y.; Jamjoom, M. Prevalence and genotyping of Cryptosporidium in stool samples collected from children in Taif City (Saudi Arabia) Prevalence and genotyping of Cryptosporidium in stool samples collected from children in Taif City (Saudi Arabia). Trop. Biomed. 2014, 31, 215–224. [Google Scholar]
- Al-Brikan, F.A.; Salem, H.S.; Beeching, N.; Hilal, N. Multilocus genetic analysis of Cryptosporidium isolates from Saudi Arabia. J. Egypt. Soc. Parasitol. 2008, 38, 645–658. [Google Scholar] [PubMed]
- Amer, H.O.; Ashankyty, I.M.; Haouas, N.A.S. Prevalence of intestinal parasite infections among patients in local public hospitals of Hail, Northwestern Saudi Arabia. Asian Pac. J. Trop. Med. 2016, 9, 44–48. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Trad, O.; Jumaa, P.; Uduman, S.; Nawaz, A. Eradication of Cryptosporidium in four children with acute lymphoblastic leukemia. J. Trop. Pediatr. 2003, 49, 128–130. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Al-Bustan, M. Infectious and parasitic disease mortality in Kuwait and the role of health education. J. Public Health 1988, 10, 197–202. [Google Scholar] [CrossRef]
- World Bank National Accounts Data, and O.N.A. Data Files. GNI Per Capita, Atlas Method (Current US$). 2019. Data. Available online: https://data.worldbank.org/indicator/NY.GNP.PCAP.CD (accessed on 2 September 2020).
- Mukhtar, A. Intestinal parasites in the state of Bahrain. Indian J. Pathol. Microbiol. 1995, 38, 341–344. [Google Scholar]
- Wikipedia, the Free Encyclopedia. Economy of Bahrain. 2020. Available online: https://en.wikipedia.org/wiki/Economy_of_Bahrain (accessed on 23 April 2020).
- UNDP. United Nation Development Program. Kingdom of Bahrain. 2016. Available online: https://www.bh.undp.org/content/bahrain/en/home/ (accessed on 23 April 2020).
- Zaki, M.; Al-Ali, F.; Daoud, A.S.; Al-Saleh, Q.; Hira, P.R. Cryptosporidiosis in the Arabian Gulf: Report of two cases from Kuwait. Med. Princ. Pract. 1989, 1, 118–120. [Google Scholar] [CrossRef]
- Al-Ghamdi, M.A.; Bentham, G.; Hunter, P.R. Environmental risk factors for diarrhoea among male schoolchildren in Jeddah City, Saudi Arabia. J. Water Health 2009, 7, 380–391. [Google Scholar] [CrossRef] [Green Version]
- Howidi, M.; Al Kaabi, N.; El Khoury, A.C.; Brandtmüller, A.; Nagy, L.; Richer, E.; Haddadin, W.; Miqdady, M.S. Burden of acute gastroenteritis among children younger than 5 years of age–A survey among parents in the United Arab Emirates. BMC Pediatr. 2012, 12, 74. [Google Scholar] [CrossRef] [Green Version]
- Al Awaidy, S.A.; Bawikar, S.; Al Busaidy, S.; Baqiani, S.; Al Abedani, I.; Varghese, R.; Abdoan, H.S.; Al Abdoon, H.; Bhatnagar, S.; Al Hasini, K.S.; et al. Considerations for introduction of a Rotavirus vaccine in Oman: Rotavirus disease and economic burden. J. Infect. Dis. 2009, 200, S248–S253. [Google Scholar] [CrossRef] [Green Version]
- Ahmed, S.A.; Karanis, P. Comparison of current methods used to detect Cryptosporidium oocysts in stools. Int. J. Hyg. Environ. Health 2018, 221, 743–763. [Google Scholar] [CrossRef]
- Learmonth, J.J.; Ionas, G.; Ebbett, K.A.; Kwan, E.S. Genetic characterization and transmission cycles of Cryptosporidium species isolated from humans in New Zealand. Appl. Environ. Microbiol. 2004, 70, 3973–3978. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pumipuntu, N.; Piratae, S. Cryptosporidiosis: A zoonotic disease concern. Vet. World 2018, 11, 681–686. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, R.; Zhang, L.; Axén, C.; Bjorkman, C.; Jian, F.; Amer, S.; Liu, A.; Feng, Y.; Li, G.; Lv, C.; et al. Cryptosporidium parvum IId family: Clonal population and dispersal from Western Asia to other geographical regions. Sci. Rep. 2014, 4, 4208. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Papanikolopoulou, V.; Baroudi, D.; Guo, Y.; Wang, Y.; Papadopoulos, E.; Lafi, S.Q.; Abd El-Tawab, M.M.; Diakou, A.; Giadinis, N.D.; Feng, Y.; et al. Genotypes and subtypes of Cryptosporidium spp. in diarrheic lambs and goat kids in northern Greece. Parasitol. Int. 2018, 67, 472–475. [Google Scholar] [CrossRef] [PubMed]
- Majeed, Q.A.H.; El-Azazy, O.M.E.; Abdou, N.E.M.I.; Al-Aal, Z.A.; El-Kabbany, A.I.; Tahrani, L.M.A.; AlAzemi, M.S.; Wang, Y.; Feng, Y.; Xiao, L. Epidemiological observations on cryptosporidiosis and molecular characterization of Cryptosporidium spp. in sheep and goats in Kuwait. Parasitol. Res. 2018, 117, 1631–1636. [Google Scholar] [CrossRef]
- Wang, R.; Zhao, G.; Gong, Y.; Zhang, L. Advances and perspectives on the epidemiology of bovine Cryptosporidium in China in the past 30 years. Front. Microbiol. 2017, 8, 1823. [Google Scholar] [CrossRef] [Green Version]
- Amer, S.; Zidan, S.; Adamu, H.; Ye, J.; Roellig, D.; Xiao, L.; Feng, Y. Prevalence and characterization of Cryptosporidium spp. in dairy cattle in Nile River delta provinces, Egypt. Exp. Parasitol. 2013, 135, 518–523. [Google Scholar] [CrossRef]
- Yang, R.; Jacobson, C.; Gardner, G.; Carmichael, I.; Campbell, A.J.D.; Ng-Hublin, J.; Ryan, U. Longitudinal prevalence, oocyst shedding and molecular characterisation of Cryptosporidium species in sheep across four states in Australia. Vet. Parasitol. 2014, 200, 50–58. [Google Scholar] [CrossRef] [Green Version]
- Feng, Y.; Xiao, L. Molecular epidemiology of cryptosporidiosis in China. Front. Microbiol. 2017, 8, 1701. [Google Scholar] [CrossRef] [Green Version]
- AL-Megrin, W.A.I. Comparison of ELISA and microscopy for detection of Cryptosporidium oocysts in animals. Pak. J. Biol. Sci. 2015, 18, 341–345. [Google Scholar] [CrossRef]
- Razakandrainibe, R.; Diawara, E.H.I.; Costa, D.; Le Goff, L.; Lemeteil, D.; Ballet, J.J.; Gargala, G.; Favennec, L. Common occurrence of Cryptosporidium hominis in asymptomatic and symptomatic calves in France. PLoS Negl. Trop. Dis. 2018, 12, e0006355. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xiao, L. Molecular epidemiology of cryptosporidiosis: An update. Exp. Parasitol. 2010, 124, 80–89. [Google Scholar] [CrossRef] [PubMed]
- Abe, N. Genotype analysis of Cryptosporidium meleagridis isolates from humans in Japan. Jpn. J. Infect. Dis. 2010, 63, 214–215. [Google Scholar] [PubMed]
- Aleisa, E.; Al-Zubari, W. Wastewater reuse in the countries of the Gulf Cooperation Council (GCC): The lost opportunity. Environ. Monit. Assess. 2017, 189, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Dawoud, M.A. Environmental impacts of seawater desalination: Arabian Gulf case study. Int. J. Environ. Sustain. 2012, 1, 22–37. [Google Scholar] [CrossRef]
- Mohorjy, A.M. Importance weighting of impacts in environmental impact studies. J. Environ. Eng. 1997, 123, 1261–1267. [Google Scholar] [CrossRef]
- Mohorjy, A.M. Alternative solutions and mitigation measures of a sewerage system, Jeddah, Saudi Arabia. Int. J. Environ. Stud. 2001, 58, 683–700. [Google Scholar] [CrossRef]
- Sonbul, A.R.; Alyamani, M.S.; Sabtan, A.A.; Qadhi, T.M. Identification of the potential sources of nitrate in groundwater from shallow aquifer in Wadi Qudaid, western part of Saudi Arabia. J. King Abdulaziz Univ. Earth Sci. 2011, 22, 1–16. [Google Scholar] [CrossRef]
- Alyamani, M.S. Effects of cesspool systems on groundwater quality of shallow bedrock aquifers in the recharge area of Wadi Fatimah, Western Arabian Shield, Saudi Arabia. J. Environ. Hydrol. 2007, 15, 1–11. [Google Scholar]
- Omer, E.M.; Algamidi, A.; Algamidi, I.; Alsubaie, A.S.; Fadlelmula, A. The hygienic-related microbiological quality of drinking water sources Al-Baha Province, Kingdom of Saudi Arabia. J. Health Spec. 2014, 2, 68–74. [Google Scholar] [CrossRef]
- Aly, N.; Ali, R.; El badawy, H. Assessment of drinking water quality. Life Sci. J. 2013, 10, 1795–1803. [Google Scholar]
- Zaki, H.; Barnawi, H. Prevalence of Cryptosporidium and Giardia lamblia in water samples from Jeddah and Makkah cities—Neliti. J. Adv. Lab. Res. Biol. 2014, 5, 12–17. [Google Scholar]
- Aljanahi, A.A.A.; Khan, M.A. A Preliminary Assessment of the occurrence of Cryptosporidium and Giardia in the School swimming pool water in Dubai, United Arab Emirates. Int. J. Environ. Sci. Dev. 2014, 5, 303–308. [Google Scholar] [CrossRef] [Green Version]
- Khan, M.; Alkitbi, H.; Aljanahi, A.; Dghaim, R. Detection of Cryptosporidium and Giardia in irrigation water of public parks in Dubai, United Arab Emirates. In Proceedings of the Health and Environment. 2015. Available online: https://d1wqtxts1xzle7.cloudfront.net/37498828/IA8_Proceedings_OPen_Online_Surgical_Education_The_Experience_in_Hand_Surgery_March_2015_P132-147.pdf?1430738271=&response-content-disposition=inline%3B+filename%3DOpen_online_surgical_education_The_exper.pdf&Expires=1600423660&Signature=d6QUU7I35WiXG7IOHGn-lZgJjRAnE~~AyjWXQGfCx6KhAflLYW1JtY1g-hNnwRznncI-Ca1SG6TSK~uUVZVlWsEdqEhByZ5f5yXCB1TIUsBLL6Z9B36QhyhB~klRX2ywfBf0lF4IagONAT2aR3ZEdMiB~6cKpDYJFLjRkDW3hgzWxKl61k11ffSd4-sx5xmzz7PYWixuruCq3GU5pc6G3WLge5iz5suaboEAQkTM3FttumrHmQnYwcDjcsl1GsqqfR-7EeWLybLwsklJ~PMhaouTA1erc84ulrqXCPVcjEXAJ5BFp0QZtCi5JjyHyK9dwsNF9DwGKTT3IJvXIVdcng__&Key-Pair-Id=APKAJLOHF5GGSLRBV4ZA (accessed on 18 April 2020).
- Ayalew, D.; Boelee, E.; Endeshaw, T.; Petros, B. Cryptosporidium and Giardia infection and drinking water sources among children in Lege Dini, Ethiopia. Trop. Med. Int. Health 2008, 13, 472–475. [Google Scholar] [CrossRef] [PubMed]
- Al-Rashed, M.F.; Sherif, M.M. Water resources in the GCC countries: An overview. Water Resour. Manag. 2000, 14, 59–75. [Google Scholar] [CrossRef]
- Raouf, M. Water Issues in the Gulf: Time for Action. Available online: https://www.mei.edu/publications/water-issues-gulf-time-action (accessed on 31 March 2020).
- Karanis, P.; Sotiriadou, I.; Kartashev, V.; Kourenti, C.; Tsvetkova, N.; Stojanova, K. Occurrence of Giardia and Cryptosporidium in water supplies of Russia and Bulgaria. Environ. Res. 2006, 102, 260–271. [Google Scholar] [CrossRef]
- Nsanze, H.; Babarinde, Z.; Al Kohaly, H. Microbiological quality of bottled drinking water in the UAE and the effect of storage at different temperatures. In Proceedings of the Environment International; Elsevier Science Ltd.: Amsterdam, The Netherlands, 1999; Volume 25, pp. 53–57. [Google Scholar]
- Minnesota Department of Health. Cryptosporidium Fact Sheet. Minnesota 2014. Available online: https://www.health.state.mn.us/communities/environment/water/factsheet/cryptosporidium.html (accessed on 29 March 2020).
- New Jersey Department of Health and Senior Services Facts: Cryptosporidium in Drinking Water. New JERSY 1999. Available online: http://www.nesc.wvu.edu/ecommerce/products/DW_PublicEducation/DWBLPE212DL.pdf (accessed on 25 April 2020).
- CDC. Fecal Incident Response Recommendations for Aquatic Staff. U.S. 2018. Available online: https://www.cdc.gov/healthywater/swimming/pdf/fecal-incident-response-guidelines.pdf (accessed on 21 April 2020).
- CDC. Microbes in Pool Filter Backwash as Evidence of the Need for Improved Swimmer Hygiene—Metro-Atlanta, Georgia, 2012. MMWR. CDC. 2013. Available online: https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6219a3.htm (accessed on 21 April 2020).
- Korich, D.G.; Mead, J.R.; Madore, M.S.; Sinclair, N.A.; Sterling, C.R. Effects of ozone, chlorine dioxide, chlorine, and monochloramine on Cryptosporidium parvum oocyst viability. Appl. Environ. Microbiol. 1990, 56, 1423–1428. [Google Scholar] [CrossRef] [Green Version]
- Omarova, A.; Tussupova, K.; Berndtsson, R.; Kalishev, M.; Sharapatova, K. Protozoan parasites in drinking water: A system approach for improved water, sanitation and hygiene in developing countries. Int. J. Environ. Res. Public Health 2018, 15, 495. [Google Scholar] [CrossRef] [Green Version]
- Karanis, P. The truth about in vitro culture of Cryptosporidium species. Parasitology 2018, 145, 855–864. [Google Scholar] [CrossRef]
- Saati, A.; Faidah, H. Environmental prevalence of pathogens in different drinking water resources in Makkah City (Kingdom of Saudi Arabia). Curr. World Environ. J. 2013, 8, 37–53. [Google Scholar] [CrossRef] [Green Version]
- Lyons, B.P.; Devlin, M.J.; Abdul Hamid, S.A.; Al-Otiabi, A.F.; Al-Enezi, M.; Massoud, M.S.; Al-Zaidan, A.S.; Smith, A.J.; Morris, S.; Bersuder, P.; et al. Microbial water quality and sedimentary faecal sterols as markers of sewage contamination in Kuwait. Mar. Pollut. Bull. 2015, 100, 689–698. [Google Scholar] [CrossRef] [PubMed]
- Malek, C. Failure to Keep UAE Pools Clean May Endanger Children, Experts Warn—The National. UAE. 2012. Available online: https://www.thenational.ae/uae/failure-to-keep-uae-pools-clean-may-endanger-children-experts-warn-1.409939 (accessed on 2 April 2020).
- Al Amimi, A.S.H.; Khan, M.A.; Dghaim, R. Bacteriological quality of reclaimed wastewater used for irrigation of public parks in the United Arab Emirates. Int. J. Environ. Sci. Dev. 2014, 5, 309–312. [Google Scholar] [CrossRef] [Green Version]
- Alsharhan, A.S.; Rizk, Z.A.; Nairn, A.E.M.; Bakhit, D.W.; Alhajari, S.A. Hydrogeology of an Arid Region: The Arabian Gulf and Adjoining Areas—Google Books; Elsevier: Amsterdam, The Netherlands, 2001. [Google Scholar]
- Abdalla, O.; Kacimov, A.; Chen, M.; Al Maktoumi, A.; Al Hosni, T.; Clark, I. Water Resources in Arid Areas: The Way Forward; Springer International Publishing: Cham, Switzerland, 2017. [Google Scholar]
- Jumat, M.; Hasan, N.; Subramanian, P.; Heberling, C.; Colwell, R.; Hong, P.Y. Membrane bioreactor-based wastewater treatment plant in Saudi Arabia: Reduction of viral diversity, load, and infectious capacity. Water 2017, 9, 534. [Google Scholar] [CrossRef] [Green Version]
- Valipour, M.; Singh, V.P. Global experiences on wastewater irrigation: Challenges and prospects. In Balanced Urban Development: Options and Strategies for Liveable Cities; Water Science and Technology Library, Ed.; Springer: Cham, Switzerland, 2016; Volume 72, pp. 289–327. [Google Scholar]
- Majeed, Q.A.H.; Alazemi, M.S.H. Preliminary study on cryptosporidiosis in livestock from Kuwait. J. Egypt. Soc. Parasitol. 2014, 44, 389–392. [Google Scholar] [CrossRef] [PubMed]
- Majeed, Q.A.H.; Al-Batel, M.K.; Abdou, N.E.M.I.; El-Azazy, O.M.E.; Sami, A.M.; El-Said, H. Infectious causes of neonatal diarrhea in cattle in Kuwait with special reference to cryptosporidiosis. J. Anim. Vet. Adv. 2011, 10, 2282–2286. [Google Scholar]
- Johnson, E.H.; Muirhead, D.E.; Windsor, J.J.; King, G.J.; Al-Busaidy, R.; Cornelius, R. Atypical outbreak of caprine cryptosporidiosis in the Sultanate of Oman. Vet. Rec. 1999, 145, 521–524. [Google Scholar] [CrossRef]
- Elwathig, M.; Faye, B. Camel calf diarrhoea in Riyadh region, Saudi Arabia. In Proceedings of the Journal of Camel Practice and Research; Camel Publishing House: Bikaner, India, 2016; Volume 23, pp. 283–285. [Google Scholar]
- Mohammed, O.B.; Alagaili, A.N.; Omer, S.A.; Hussein, M.F. Parasites of the Arabian Oryx (Oryx leucoryx, Pallas, 1777) and their prevalence in the Kingdom of Saudi Arabia. Comp. Parasitol. 2012, 79, 288–292. [Google Scholar] [CrossRef]
- Azmanis, P.; di Somma, A.; Pappalardo, L.; Silvanose, C.D.; Bangoura, B. First detection of Cryptosporidium parvum in falcons (Falconiformes): Diagnosis, molecular sequencing, therapeutic trial and epidemiological assessment of a possible emerging disease in captive falcons. Vet. Parasitol. 2018, 252, 167–172. [Google Scholar] [CrossRef]
- Zylan, K.; Bailey, T.; Smith, H.V.; Silvanose, C.; Kinne, J.; Schuster, R.K.; Hyland, K. An outbreak of cryptosporidiosis in a collection of Stone curlews (Burhinus oedicnemus) in Dubai. Avian Pathol. 2008, 37, 521–526. [Google Scholar] [CrossRef]
- Brown, J.J.; Das, P.; Al-saidi, M. Sustainable agriculture in the Arabian/Persian Gulf region utilizing marginal water resources: Making the best of a bad situation. Sustainability 2018, 45, 1364. [Google Scholar] [CrossRef] [Green Version]
- Naciri, M.; Lefay, M.P.; Mancassola, R.; Poirier, P.; Chermette, R. Role of Cryptosporidium parvum as a pathogen in neonatal diarrhoea complex in suckling and dairy calves in France. Vet. Parasitol. 1999, 85, 245–257. [Google Scholar] [CrossRef]
- Al-Megrin, W.A.I. Prevalence rate of intestinal parasites in camels in Riyadh, Saudi Arabia. Int. J. Zool. Res. 2015, 11, 65–70. [Google Scholar] [CrossRef] [Green Version]
- Fayer, R.; Phillips, L.; Anderson, B.C.; Bush, M. Chronic cryptosporidiosis in a bactrian camel (Camelus bactrianus). J. Zoo Wildl. Med. 1991, 22, 228–232. [Google Scholar]
- Afzal, M.; Sakkir, M. Survey of antibodies against various infectious disease agents in racing camels in Abu Dhabi, United Arab Emirates. Rev. Sci. Tech. 1994, 13, 787–792. [Google Scholar] [CrossRef]
- Khalaf, S. Camel racing in the Gulf notes on the evolution of a traditional cultural sport. Anthropos 1999, 94, 85–106. [Google Scholar]
- Sazmand, A.; Joachim, A.; Otranto, D. Zoonotic parasites of dromedary camels: So important, so ignored. Parasites Vectors 2019, 12, 1–10. [Google Scholar] [CrossRef]
- Banaja, A.; Ghandour, A. A review of parasites of camels (Camelus dromedarius) in Saudi Arabia. J. King Abdulaziz Univ. Sci. 1994, 6, 75–86. [Google Scholar] [CrossRef]
- Zhu, S.; Zimmerman, D.; Deem, S.L. A review of zoonotic pathogens of dromedary camels. Ecohealth 2019, 16, 356–377. [Google Scholar] [CrossRef] [Green Version]
- CDC. Sources of Infection & Risk Factors/Prasites—Cryptosporidium. CDC, 2015. Available online: https://www.cdc.gov/parasites/crypto/infection-sources.html (accessed on 10 April 2020).
- Rules & Regulations for Medical Examination of Expatriates Coming to GCC States for Residence. Available online: http://ghc.sa/en-us/Documents/English%20Document.pdf (accessed on 13 April 2020).
- Zaglool, D.; Khodari, Y.; Othman, R.; Farooq, M. Prevalence of intestinal parasites and bacteria among food handlers in a tertiary care hospital. Niger. Med. J. 2011, 52, 266. [Google Scholar]
- Qureshy, F. Comparative study of intestinal parasitic infestation among food handlers in Abu Dhabi (U.A.E.) 1981–1982. J. Pak. Med. Assoc. 1988, 38, 163–166. [Google Scholar]
- Al-Awadhi, M.; Iqbal, J.; Ahmad, S. Cysticercosis/T. solium taeniasis, a potential public health concern in non-endemic country, Kuwait: A new diagnostic method to screen T. solium taeniasis carriers among the expatriate population. Med. Princ. Pract. 2019, 29, 347–353. [Google Scholar] [CrossRef] [PubMed]
- Taha, H.A.; Soliman, M.I.; Banjar, S.A.N. Intestinal parasitic infections among expatriate workers in Al-Madina Al-Munawarah, Kingdom of Saudi Arabia. Trop. Biomed. 2013, 30, 78–88. [Google Scholar] [PubMed]
- Imam, N.A.; Abdulbaqi, Z.; Fahad, R. The prevalence of intestinal parasitic infections among foreign workers in Madinah, Kingdom of Saudi Arabia. Saudi J. Med. Med. Sci. 2015, 3, 112–117. [Google Scholar] [CrossRef]
- Koshak, E.A.; Zakai, H.A. A spectrum of pathogenic and non-pathogenic intestinal parasites in pre-employment medical check-up for workers and their families. J. Fam. Community Med. 2003, 10, 47–53. [Google Scholar]
- Olsen, S.J.; MacKinnon, L.C.; Goulding, J.S.; Bean, N.H.; Slutsker, L. Surveillance for foodborne-disease outbreaks—United States, 1993–1997. MMWR CDC Surveill. Summ. 2000, 49, 1–62. [Google Scholar]
- Dafalla, A.I.A.; Almuhairi, S.A.S.O.; AlHosani, M.H.J.; Mohamed, M.Y.; Alkous, M.I.A.; AlAzzawi, M.A.; Abakar, A.D.; Nour, B.Y.M.; Hasan, H.; Abuodeh, R.O.; et al. Intestinal parasitic infections among expatriate workers in various occupations in Sharjah, United Arab Emirates. Rev. Inst. Med. Trop. Sao Paulo 2017, 59, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Spiess, A. Food Security in the Gulf Cooperation Council (GCC) Economies. GCC Network for Drylands Research and Development (NDRD). 2011. Available online: http://www.ndrd.org/Spiess_-_Working_Paper_on_Food_Security_in_the_GCC.pdf (accessed on 18 April 2020).
- Shahid, S.A.; Taha, F.K.; Abdelfattah, M.A. Developments in Soil Classification, Land Use Planning and Policy Implications: Innovative Thinking of Soil Inventory for Land Use Planning and Management of Land Resources; Springer: Berlin/Heidelberg, Germany, 2013; ISBN 9789400753327. [Google Scholar]
- OECD-FAO Agricultural Outlook 2018–2027. Chapter 2: Special Focus: Middle East and North. Available online: http://www.fao.org/3/I9166EN/I9166EN.pdf (accessed on 14 April 2020).
- Al-Busaidi, M.A.A. Effective Seafood Safety and Quality Management Systems:An Analysis of the Situation in the Sultanate of Oman; University of Reading: Reading, UK, 2017. [Google Scholar]
- Al-Busaidi, M.A.; Jukes, D.J. Assessment of the food control systems in the Sultanate of Oman. Food Control 2015, 51, 55–69. [Google Scholar] [CrossRef]
- Faour-Klingbeil, D.; Todd, E.C.D. Prevention and control of foodborne diseases in Middle-East North African countries: Review of national control systems. Int. J. Environ. Res. Public Health 2020, 17, 70. [Google Scholar] [CrossRef] [Green Version]
- WHO. Foodborne diseases burden epidemiology reference group 2007–2015. In WHO Estimates of the Global Burden of Foodborne Diseases; World Health Organization: Geneva, Switzerland, 2015; pp. 1–252. ISBN 9789241565165. [Google Scholar]
- Bakri, M.; Amin, F.A.L.; Fadil Saleh, A.; Taib Saeed, A.; Nabag, M.; Haroon, M.; Mohamed, K. Food hygiene in past ten years in Saudi Arabia. EC Microbiol. 2017, 7, 4–13. [Google Scholar]
- Refai, M. Incidence and control of brucellosis in the near East region. Vet. Microbiol. 2002, 90, 81–110. [Google Scholar] [CrossRef]
- Al-Mazrou, Y.Y. Food poisoning in Saudi Arabia. Potential for prevention? Saudi Med. J. 2004, 25, 11–14. [Google Scholar] [PubMed]
- Abdalla, A.S.; Omar, H.M. The prevalence of leafy vegetable-borne parasites in Al-Qassim region, Saudi Arabia. J. Agric. Vet. Med. 2013, 6, 29–40. [Google Scholar]
- Al-Goblan, A.; Jahan, S. Surveillance for foodborne illness outbreaks in Qassim, Saudi Arabia, 2006. Foodborne Pathog. Dis. 2010, 7, 1559–1562. [Google Scholar] [CrossRef] [PubMed]
- The Cooperation Council for The Arab States of The Gulf. GCC Guide for Control on Imported Foods. 2016. Available online: https://www.gcc-sg.org/en-us/CognitiveSources/DigitalLibrary/Lists/DigitalLibrary/Agriculture%20Livestock%20and%20Fisheries/1429075065.pdf (accessed on 14 April 2020).
- Balderrama-Carmona, A.P.; Gortáres-Moroyoqui, P.; Álvarez-Valencia, L.H.; Castro-Espinoza, L.; Mondaca-Fernández, I.; de Jesús Balderas-Cortés, J.; Chaidez-Quiroz, C.; Meza-Montenegro, M.M. Occurrence and quantitative microbial risk assessment of Cryptosporidium and Giardia in soil and air samples. Int. J. Infect. Dis. 2014, 26, 123–127. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mor, S.M.; Tumwine, J.K.; Ndeezi, G.; Srinivasan, M.G.; Kaddu-Mulindwa, D.H.; Tzipori, S.; Griffiths, J.K. Respiratory cryptosporidiosis in HIV-seronegative children in Uganda: Potential for respiratory transmission. Clin. Infect. Dis. 2010, 50, 1366–1372. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mor, S.M.; Ascolillo, L.R.; Nakato, R.; Ndeezi, G.; Tumwine, J.K.; Okwera, A.; Sponseller, J.K.; Tzipori, S.; Griffiths, J.K. Expectoration of Cryptosporidium parasites in sputum of human immunodeficiency virus-positive and -negative adults. Am. J. Trop. Med. Hyg. 2018, 98, 1086–1090. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sponseller, J.K.; Griffiths, J.K.; Tzipori, S. The evolution of respiratory cryptosporidiosis: Evidence for transmission by inhalation. Clin. Microbiol. Rev. 2014, 27, 575–586. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Patlakas, P.; Stathopoulos, C.; Flocas, H.; Kalogeri, C.; Kallos, G. Regional climatic features of the Arabian Peninsula. Atmosphere 2019, 10, 220. [Google Scholar] [CrossRef] [Green Version]
- Dbouk, T.; Drikakis, D. On coughing and airborne droplet transmission to humans. Phys. Fluids 2020, 32, 53310. [Google Scholar] [CrossRef]
- Heo, I.; Dutta, D.; Schaefer, D.A.; Iakobachvili, N.; Artegiani, B.; Sachs, N.; Boonekamp, K.E.; Bowden, G.; Hendrickx, A.P.A.; Willems, R.J.L.; et al. Modelling Cryptosporidium infection in human small intestinal and lung organoids. Nat. Microbiol. 2018, 3, 814–823. [Google Scholar] [CrossRef]
- Yan, J.; Grantham, M.; Pantelic, J.; De Mesquita, P.J.B.; Albert, B.; Liu, F.; Ehrman, S.; Milton, D.K. Infectious virus in exhaled breath of symptomatic seasonal influenza cases from a college community. Proc. Natl. Acad. Sci. USA 2018, 115, 1081–1086. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Country | Serial No. of Reports | City | Type of Residents | Patients Classification | Most Affected Age | Symptoms | Method of Detection | Prevalence No. of Infected/No. of Total (%) | Reference | |
|---|---|---|---|---|---|---|---|---|---|---|
| Bahrain | - | - | - | - | - | - | - | |||
| Kuwait | 1 | Safat | Inhabitants | Children | 4–8 Y | Diarrhoea | MZN, PCR-RFLP | 87/2548 | * (3.4%) | [49] |
| 2 | Farwanyia | Inhabitants | Children | >2 Y | Diarrhoea, nausea, vomiting | MSMB, DFA | 51/3549 | (10%) | [39] | |
| 3 | Jabryia | NM | Hospitalized patients | NM | Diarrhoea | xTAG GPPA | 1/109 | (0.9%) | [61] | |
| 4 | Safat | Inhabitants | Children | 2–3 Y | GIT symptoms mainly diarrhoea | MZN, PCR-RFLP | 58/62 | (94%) | [50] | |
| 5 | Farwanyia | NM | ICCT children | <3 Y | Diarrhoea, dehydration, fever, abdominal pain | NM | 35/2205 | (1.6%) | [62] | |
| Oman | 1 | Muscat | Expatriates | Food handlers | NM | Asymptomatic | KKT, TS, APFM | 2/100 | (0.2%) | [63] |
| 2 | Muscat | Inhabitants and expatriates | Children | <2 Y | Diarrhoea, fever, vomiting | MZN, APFM | 16/807 | (1.9%) | [64] | |
| Qatar | 1 | Doha | Inhabitants and expatriates | Hospitalized paediatrics | <2.5 Y | Chronic diarrhoea | q-PCR | 90/580 | (15.5%) | [46] |
| 2 | Doha | Expatriates | Immigrants | 23–29 Y | Asymptomatic | q-PCR | 38/839 | (4.5%) | [45] | |
| SA | 1 | Dammam and Alkhobar | Inhabitants | Children and adults | 2 Y | Diarrhoea | MZN, APFM | 2/321 | (0.6%) | [65] |
| 2 | Al-Taif | Inhabitants | Children and adults | <5 Y | Diarrhoea | MZN, LFIT, Con-PCR | 21/180 | (11.6%) | [66] | |
| 3 | Gizan and Madinna | NM | Children | <2 Y | Diarrhoea and asymptomatic | MZN, MSMB, EIA, PCR-RFLP, sequencing | 103/1641 | (6.3%) | [67] | |
| 4 | Al-Taif | NM | Children and adults | <5 Y | Acute diarrhoea | xTAG GPPA | 14/163 | (8.5%) | [68] | |
| 5 | Dhahran | NM | Various ages | NM | Abdominal symptoms mainly diarrhoea | MZN, DFA | 66/100 | (66%) | [69] | |
| 6 | Mekkah | Inhabitants | Children < 14 y | <5 Y | Diarrhoea | MZN, ICT, PCR-RFLP | 23/1380 | (1.7%) | [70] | |
| 7 | Jeddah | Inhabitants | Children | <5 Y | Asymptomatic and diarrhoea | MZN | 29/253 | (11.5%) | [71] | |
| 8 | Riyadh | NM | HIV patients | 2–10 Y | Diarrhoea and non-diarrhoea | MZN | 11/136 | (8.1%) | [72] | |
| 9 | Makkah | NM | People attending clinics around the Holy Masjid | <30 Y | Enteritis | MZN | 5/183 | (2.7%) | [60] | |
| 10 | Riyadh | NM | Children <10 y | NM | Diarrhoea | MSMB | 2/174 | (1.1%) | [73] | |
| 11 | Hail | NM | School children | NM | Diarrhoea and non-diarrhoea | MZN | 74/200 | (37%) | [74] | |
| 12 | Riyadh | Inhabitants | ICP | 16–40 Y | Chronic diarrhoea Malnutrition | MZN, ELISA | 285/408 | (69.9%) | [75] | |
| 13 | Riyadh | Inhabitants with few expatriates | In-and out-patients | 0–10 Y | NM | MZN | 6/5987 | (0.1%) | [76] | |
| 14 | Al-Taif | NM | Children | <10 Y | NM | MZN, AP-PCR, Sequencing | 11/100 | (11%) | [77] | |
| 15 | Jeddah | NM | Children | NM | NM | MZN, APFM, ELISA, Nested PCR, PCR-RFLP | 35/500 | (7%) | [78] | |
| UAE | 16 | Hail | Inhabitants and expatriates | Saudi and non-Saudi patients | NM | Asymptomatic | MZN | 25/130 | 19.2% | [79] |
| 1 | Sharjah | Expatriates | Adults | ≤25 Y | Asymptomatic | q-PCR | 26/134 | (19.4%) | [48] | |
| 2 | Al-Ain | Expatriates | Adults | 30–39 | Asymptomatic | MZN, Con-PCR | 16/86 | (18.6%) | [47] | |
| 3 | Al-Ain | NM | ICP and ICTT Children | <5 | Diarrhoea Fever Vomiting ALA | MZN | 7/140 | (5%) | [80] | |
| Country/City | Target Population | Methods Used | Gene Target | Reported Genotypes | No. of Cases within the Species (%) | Subtypes Allele Family | No. of Cases within Each Allele | Reference |
|---|---|---|---|---|---|---|---|---|
| Kuwait/Safat | Children with diarrhoea | PCR-RFLP |
18S rRNA Gp60 | C. parvum | 61/83 (73.5%) | C. parvum | [49] | |
| IIa | 29 | |||||||
| C. hominis | 22/83 (26.5%) | IId | 20 | |||||
| IIc | 12 | |||||||
| C. hominis | ||||||||
| Mixed “C. parvum and C. hominis” | 4/83 (4.8%) | Id | 12 | |||||
| Ia | 8 | |||||||
| Ie | 2 | |||||||
| Mixed infection | NI | |||||||
| Kuwait/Safat | Symptomatic children | PCR-RFLP Sequencing | 18S rRNA Gp60 | C. parvum | 58/62 (93.5%) | C. parvum | [50] | |
| IId | 29 | |||||||
| IIa | 28 | |||||||
| C. hominis | 3/62 (4.8%) | IIc | 1 | |||||
| Mixed “C. parvum and C. hominis” | 1/62 (1.6%) | IIf | 1 | |||||
| C. hominis | ||||||||
| Ib | 2 | |||||||
| Id | 1 | |||||||
| Ie | 1 | |||||||
| Qatar/Doha | Hospitalized paediatrics with diarrhoea | qPCR Sequencing | 18S rRNA Gp60 | C. parvum | 83/90 (92.2%) | C. parvum1 | [46] | |
| C. hominis | 4/90 (4.4%) | IId | 83 | |||||
| C. meleagridis | 1/90 (1.11) | C. hominis | ||||||
| Mixed “C. parvum and C. hominis” | 1/90 (1.11%) | Ib | 4 | |||||
| Mixed “C. parvum and C. meleagridis” | 1/90 (1.11%) | |||||||
| Qatar/Doha | Asymptomatic Immigrants | qPCR Sequencing | 18S rRNA Gp60 | C. parvum | 30/38 (80%) | C. parvum | [45] | |
| C. hominis | 1/38 (2.6%) | IId | 30 | |||||
| Mixed “C. parvum and C. hominis” | 4/38 (10.5%) | C. hominis | ||||||
| Mixed “C. parvum and C. meleagridis” | 3/38 (7.9%) | Ie | 1 | |||||
| SA/Makkah | Children with diarrhoea | PCR-RFLP | 18S rRNA | C. hominis | (81.1%) | NI | - | [70] |
| C. parvum | (16.7%) | NI | - | |||||
| SA/Gizan and Maddina | Children with diarrhoea and asymptomatic children | PCR-RFLP Sequencing |
18S rRNA Gp60 HSP70 | C. parvum | 79/101 (78.2%) | C. parvum | NM | [67] |
| IId | ||||||||
| C. hominis | 13/101 (12.9%) | IIa | ||||||
| IIc | ||||||||
| Mixed “C. parvum and C. hominis” | 8/101 (7.92%) | C. hominis | NM | |||||
| Ib | ||||||||
| Ie | ||||||||
| SA/Al-Taif | Children form different hospitals and laboratories |
AP-PCR Sequencing | 18S rRNA | C. parvum | 11/100 (11%) | NI | NI | [77] |
| SA/Jeddah | Asymptomatic Children | Nested PCR and PCR-RFLP |
18S rRNA COWP Gp60 | C. parvum | 15/35 (42.9%) | NI | NI | [78] |
| C. hominis | 13/35 (37%) | |||||||
| C. meleagridis | 1/35 (2.9%) | |||||||
| C. muris | 1/35 (2.9%) |
| Country/City | Type of Contaminated Water | Method Used | No. of Contaminated/No. of Total | Genotyping/Subtyping | References |
|---|---|---|---|---|---|
| Kuwait/Safat | Overhead water tanks | IFT PCR-RFLP of 18S rRNA | 1/5 | 2C. parvum subtype IIa | [49] |
| SA/Al-Taif | Underground water (UW) from wells | Nested PCR | UW 7/96 | NP | [52] |
| Desalinated water (DW) from tanks in private houses | DW 8/72 | ||||
| Bottled water (BW) | BW 0/60 | ||||
| 1 SA/Tabuk | Bottled water | Filtration MZN ELISA | 6/36 | NP | [111] |
| 1 SA/Mekka and Jeddah | Tap water | Double centrifugation MZN | Schools 13/44 | NP | [112] |
| Bottled water | Houses 33/122 | ||||
| Ablution water | Mosques 31/79 | ||||
| UAE/Dubai | School swimming pool | IFT | 5/5 | NP | [113] |
| UAE/Dubai | Irrigation water (IW) of public parks | IFT | IW 17/18 | NP | [114] |
| Chlorinated water (CW) samples from the sewage treatment plant | CW 5/5 |
| Country/City | Type of Animal | No. of Infected/No. of Total | Method Used | Genotyping of Cryptospori-Dium | Subtyping of Cryptosporidium | Reference |
|---|---|---|---|---|---|---|
| Kuwait/different areas | Sheep Goats | 38/334 16/222 | MZN EIA PCR-RFLP Sequencing | C. parvum | IIdA20G1 | [95] |
| C. ubiquitum | IIaA15G2R1 | |||||
| C. xiaoi | XIIa | |||||
| Kuwait/Kabd, Salmi, Abdelli and Wafra areas | Calves Goat kids Lambs | 15/40 12/57 16/128 | MZN ICT | NP | NP | [135] |
| Kuwait/Sulaibiya | Newborn calves | 31/80 | MZN | NP | NP | [136] |
| 1 Oman/Muscat | Goats | 238/238 | IFT MZN H&E histopathology TEM SEM | C. parvum | NP | [137] |
| SA/Riyadh | Goats | 24/72 | MZN ELISA | NP | NP | [100] |
| Sheep | 15/58 | |||||
| Camels | 20/49 | |||||
| 2 SA/Riyadh | Camels | 5/33 | NM | NP | NP | [138] |
| 2 SA/Riyadh | Arabian Oryx | NM | NM | NP | NP | [139] |
| UAE/Dubai | Falcons | 2/2 | MZN PCR Sequencing | C. parvum | NP | [140] |
| 1 UAE/Dubai | Stone curlew | 19/29 | MZN ICT H&E histopathology PCR-RFLP | C. parvum in two samples tested | NP | [141] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ahmed, S.A.; Karanis, P. Cryptosporidium and Cryptosporidiosis: The Perspective from the Gulf Countries. Int. J. Environ. Res. Public Health 2020, 17, 6824. https://doi.org/10.3390/ijerph17186824
Ahmed SA, Karanis P. Cryptosporidium and Cryptosporidiosis: The Perspective from the Gulf Countries. International Journal of Environmental Research and Public Health. 2020; 17(18):6824. https://doi.org/10.3390/ijerph17186824
Chicago/Turabian StyleAhmed, Shahira A., and Panagiotis Karanis. 2020. "Cryptosporidium and Cryptosporidiosis: The Perspective from the Gulf Countries" International Journal of Environmental Research and Public Health 17, no. 18: 6824. https://doi.org/10.3390/ijerph17186824






