Insights Gained in the Aftermath of the COVID-19 Pandemic: A Follow-Up Survey of a Recreational Training Program, Focusing on Sense of Coherence and Sleep Quality
Abstract
:1. Introduction
2. Materials and Methods
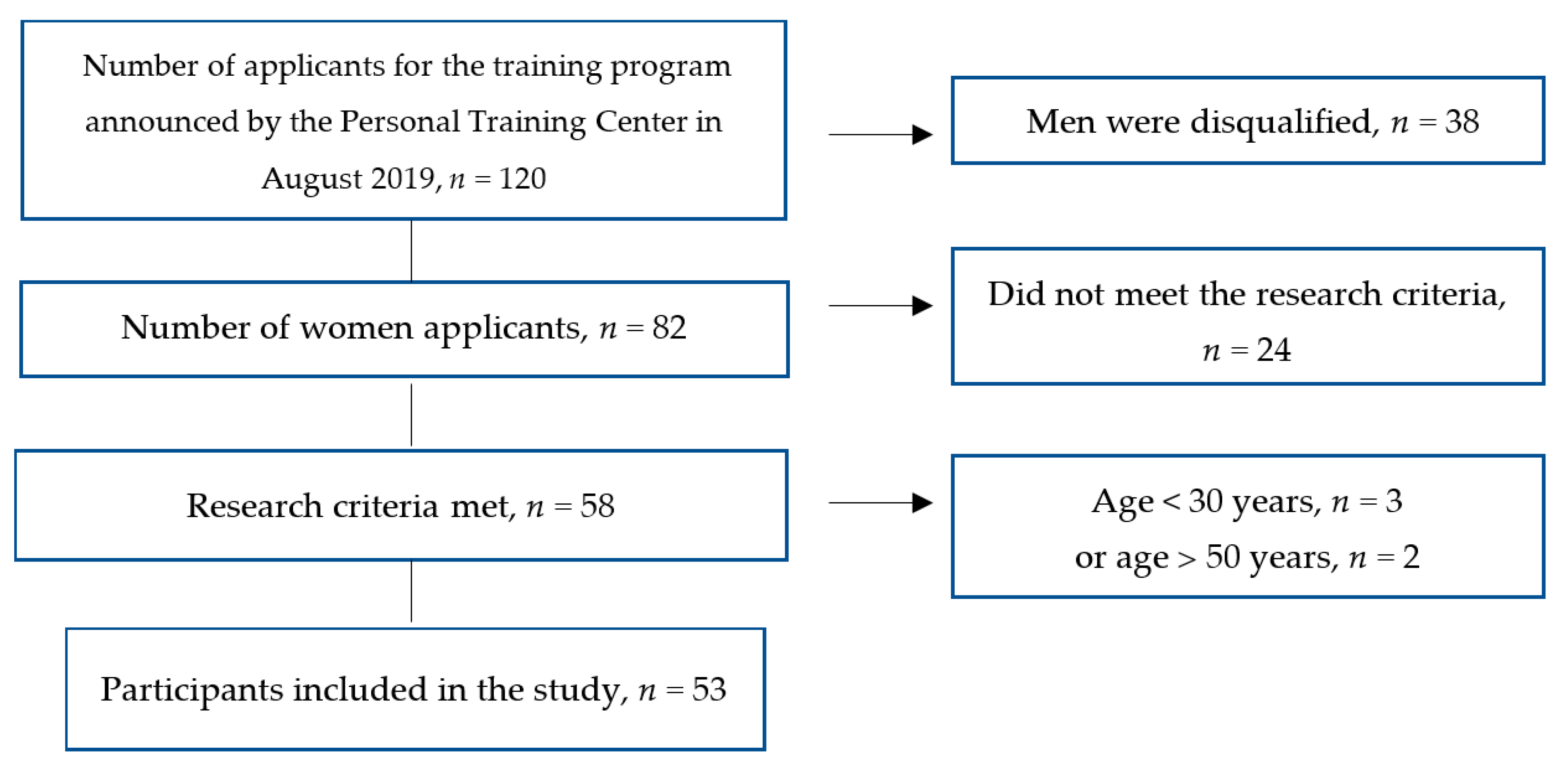
2.1. Participants and Procedure
2.2. Recreational Training
2.3. Measurements
2.3.1. Sense of Coherence
2.3.2. Regensburger Insomnia Scale
2.4. Statistical Analysis
2.5. Ethics
3. Results
3.1. Results of the Surveys Completed before the Pandemic, in the Course of the Recreational Training
3.1.1. Changes in Body Size
3.1.2. Change in Fitness Status
3.1.3. Eating Habits and Adherence to Diet-Related Advice
3.1.4. Changes in the Sense of Coherence as Well as Sleep Quality
3.2. Results of the Survey Related to the Lockdown Implemented Due to the Pandemic
3.2.1. Life Circumstances
3.2.2. Sleep Quality Deterioration
3.2.3. The Influence of Environmental Factors on Sleep Quality
3.2.4. The Effect of Physical Activity on Sleep Quality
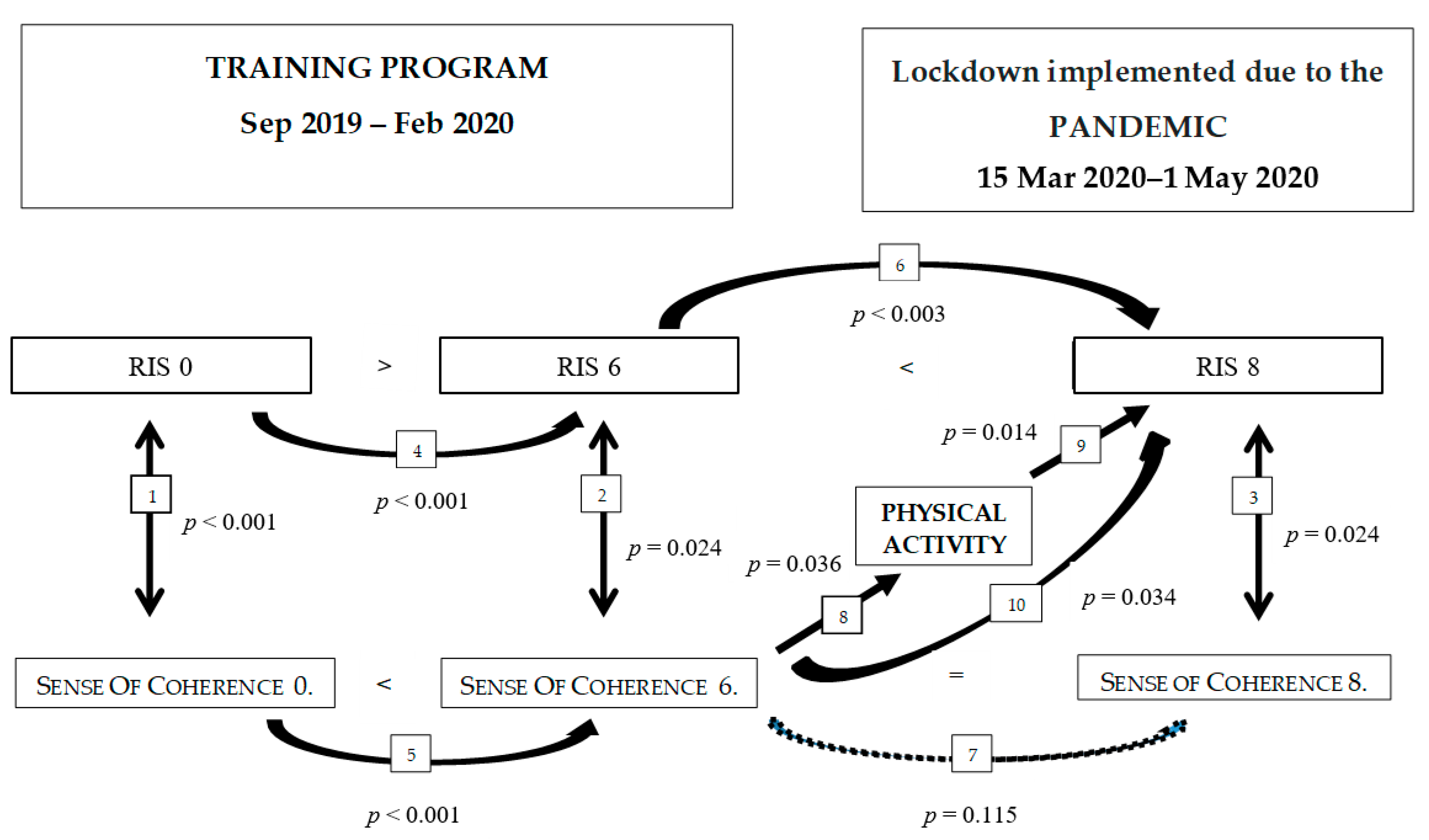
3.2.5. Connection between the Sense of Coherence and Physical Activity, and Their Effect on Sleep Quality
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Lee, I.-M.; Shiroma, E.J.; Lobelo, F.; Puska, P.; Blair, S.N.; Katzmarzyk, P.T. For the Lancet Physical Activity Series Working Group. Effect of physical inactivity on major non-communicabliseases worldwide: An analysis ourden oisease and lifxpectancy. Lancet 2012, 380, 219–229. [Google Scholar] [CrossRef] [Green Version]
- Booth, F.W.; Roberts, C.K.; Laye, M.J. Lack oxercise is a major cause of chronic diseases. Compr. Physiol. 2012, 2, 1143–1211. [Google Scholar] [PubMed] [Green Version]
- Bauman, A.E.; Reis, R.S.; Sallis, J.F.; Wells, J.C.; Loos, R.J.F.; Martin, B.W. For the Lancet Physical Activity Series Working Group. Correlates of physical activity: Why are some people physically active and others not? Lancet 2012, 380, 258–271. [Google Scholar] [CrossRef]
- Hassmén, P.; Koivula, N.; Uutela, A. Physical exercise and psychological well-being: A population study in Finland. Prev. Med. 2000, 30, 17–25. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mandolesi, L.; Polverino, A.; Montuori, S.; Foti, F.; Ferraioli, G.; Sorrentino, P.; Sorrentino, G. Effects of physical exercise on cognitive functioning and wellbeing: Biological and psychological benefits. Front. Psychol. 2018, 9, 509. [Google Scholar] [CrossRef] [PubMed]
- Penedo, F.J.; Dahn, J.R. Psychiatry exercise and well-being: A review of mental and physical health benefits associated with physical activity. Curr. Opin. Psychiatry 2005, 18, 189–193. [Google Scholar] [CrossRef]
- Peluso, M.; Andrade, L. Physical activity and mental health: The association between exercise and mood. Clinics 2005, 60, 61–70. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Papastergiou, D.; Kokaridas, D.; Bonotis, K.; Diggelidis, N.; Patsiaouras, A. Exercise, supportive group therapy, and mood profile of Greek cancerpatients: Intervention effect and related comparisons. Support Care Cancer 2018, 26, 3571–3578. [Google Scholar] [CrossRef]
- Windle, G.; Hughes, D.; Linck, P.; Russell, I.; Woods, B. Is Exercisffective in promoting mental well-being in older age? A Systematic Review. Aging Ment. Health 2010, 14, 652–669. [Google Scholar] [CrossRef]
- Zubala, A.; MacGillivray, S.; Frost, H.; Kroll, T.; Skelton, D.A.; Gavine, A.; Gray, N.M.; Toma, M.; Morris, J. Promotion of physical activity interventions for community dwelling older adults: A systematic review of reviews. PLoS ONE 2017, 12, e0180902. [Google Scholar] [CrossRef]
- Maugeri, G.; Castrogiovanni, P.; Battaglia, G.; Pippi, R.; D’Agata, V.; Palma, A.; Di Rosa, M.; Musumeci, G. The impact of physical activity on psychological health during Covid-19 pandemic in Italy. Heliyon 2020, 6, e04315. [Google Scholar] [CrossRef] [PubMed]
- Giustino, V.; Parroco, A.M.; Gennaro, A.; Musumeci, G.; Palma, A.; Battaglia, G. Physical activity levels and related energy expenditururing COVID-19 quarantine among the sicilian active population: A cross-sectional online survey study. Sustainability 2020, 12, 4356. [Google Scholar] [CrossRef]
- Antonovsky, A. Unraveling the Mystery of Health. How People Manage Stress and Stay Well, 1st ed.; Jossey-Bass: San Francisco, CA, USA; London, UK, 1987; pp. 190–194. [Google Scholar]
- Antonovsky, A. Health, Stress and Coping, 1st ed.; Jossey-Bass: San Francisco, CA, USA, 1979. [Google Scholar]
- Idan, O.; Eriksson, M.; Al-Yagon, M. The salutogenic model: The role of generalized resistance resources. In The Handbook of Salutogenesis; Mittelmark, M.B., Sagy, S., Eriksson, M., Bauer, G.F., Pelikan, J.M., Lindström, B., Espnes, G.A., Eds.; Springer: Cham, Switzerland, 2017; pp. 57–69. [Google Scholar]
- Eriksson, M.; Lindström, B. Antonovsky’s sense of coherence scale and its relation with quality of life: A systematic review. J. Epidemiol. Community Health 2007, 61, 938–944. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Super, S.; Wagemakers, M.A.E.; Picavet, H.S.J.; Verkooijen, K.T.; Koelen, M.A. Strengthening sense of coherence: Opportunities for theory building in health promotion. Health Promot. Int. 2016, 31, 869–878. [Google Scholar] [CrossRef] [PubMed]
- Kähönen, K.; Näätänen, P.; Tolvanen, A.; Salmela-Aro, K. Development of sense of coherencuring two group interventions. Scand. J. Psychol. 2012, 53, 523–527. [Google Scholar] [CrossRef]
- Feldt, T.; Leskinen, E.; Koskenvuo, M.; Suominen, S.; Vahtera, J.; Kivimäki, M. Development of sense of coherence in adulthood: A person-centered approach. The population-based HeSSup cohort study. Qual. Life Res. 2011, 20, 69–79. [Google Scholar] [CrossRef]
- Surtees, P.G.; Wainwright, N.W.J.; Khaw, K.-T. Resilience, misfortune, and mortality: Evidence that sense of coherence is a marker of social stress adaptive capacity. J. Psychosom. Res. 2006, 61, 221–227. [Google Scholar] [CrossRef]
- Surtees, P.G.; Wainwright, N.W.J.; Luben, R.L.; Wareham, N.J.; Bingham, S.A.; Khaw, K.-T. Adaptation to social adversity is associated with stroke incidence: Evidence from the EPIC-Norfolk prospective cohort study. Stroke 2007, 38, 1447–1453. [Google Scholar] [CrossRef] [Green Version]
- Krause, C. Developing sense of coherence in educational contexts: Making progress in promoting mental health in children. Int. Rev. Psychiatry 2011, 23, 525–532. [Google Scholar] [CrossRef] [Green Version]
- Idan, O.; Braun-Lewensohn, O.; Lindström, B.; Margalit, M. Salutogenesis: Sense of coherence in childhood and in families. In The Handbook of Salutogenesis; Mittelmark, M.B., Sagy, S., Eriksson, M., Bauer, G.F., Pelikan, J.M., Lindström, B., Espnes, G.A., Eds.; Springer: Cham, Switzerland, 2017; pp. 107–121. [Google Scholar]
- Chu, J.J.; Khan, M.H.; Jahn, H.J.; Kraemer, A. Sense of coherence and associated factors among university students in China: Cross-sectional evidence. BMublic Health 2016, 16, 336. [Google Scholar] [CrossRef] [Green Version]
- Endo, S.; Kanou, H.; Oishi, K. Sports activities and sense of coherence (SOC) among college students. Int. J. Sport Health Sci. 2012, 10, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Kuuppelomäki, M.; Utriainen, P. A 3 year follow-up study of health care students’ sense of coherence and related smoking, drinking and physical exercise factors. Int. J. Nurs. Stud. 2003, 40, 383–388. [Google Scholar] [CrossRef]
- Nilsson, B.; Holmgren, L.; Stegmayr, B.; Westman, G. Sense of coherence—Stability over time and relation to health, disease, and psychosocial changes in a general population: A longitudinal study. Scand. J. Public Health 2003, 31, 297–304. [Google Scholar] [CrossRef] [PubMed]
- Basta, M.; Chrousos, G.P.; Vela-Bueno, A.; Vgontzas, A.N. Chronic insomnia and the stress system. Sleep Med. Clin. 2007, 2, 279–291. [Google Scholar] [CrossRef] [Green Version]
- Irwin, M.R. Why sleep is important for health: A psychoneuroimmunology perspective. Annu. Rev. Psychol. 2015, 66, 143–172. [Google Scholar] [CrossRef] [Green Version]
- Medic, G.; Wille, M.; Hemels, M.E. Short- and long-term health consequences of sleep disruption. Nat. Sci. Sleep. 2017, 9, 151–161. [Google Scholar] [CrossRef] [Green Version]
- Harvey, A.G.; Stinson, K.; Whitaker, K.L.; Moskovitz, D.; Virk, H. The subjective meaning of sleep quality: A comparison of individuals with and without insomnia. Sleep 2008, 31, 383–393. [Google Scholar] [CrossRef] [Green Version]
- Szovák, E.; Tóth, Á.; Jeges, S. Mozgásos rekreációs tréningprogram hatásvizsgálata. [Impact assessment of sport-recreation training]. Rekreacio.eu 2012, 43, 42–47. [Google Scholar]
- Hennenhofer, G.; Heil, K.D. Angst Überwinden: Selbstbefreiung durch Verhaltenstraining; Deutsche Verlags-Anstalt DVA: Stuttgart, Germany, 1973. [Google Scholar]
- Van Woerkum, C.; Bouwman, L. ‘Getting thingone’: An everyday-life perspective towardridging the gap between intentions and practices in health-related behavior. Health Promot. Int. 2014, 29, 278–286. [Google Scholar] [CrossRef] [Green Version]
- Kovács, T.A.; Szollás, E. Edzéstani Alapok–Fitt-tan [Basics of Training]; Önkormányzati és Területfejlesztési Minisztérium Sport Szakállamtitkárság: Budapest, Hungary, 2008. [Google Scholar]
- Frenkl, R. Orvostudomány—Sport—Egészségnevelés. [Medicine—sports—health education]. In A sport Helye az Egészségnevelésben [The Role of Sport in Health Education]; Frenkl, R., Dobozy, L., Eőry, I., Eds.; Medicina Könykiadó: Budapest, Hungary, 1980; pp. 7–15. (In Hungarian) [Google Scholar]
- Body Fat Formula: US Navy. Available online: https://fitties.com/fat-caliper-plus/body-fat-calculation-methods/us-navy/ (accessed on 9 December 2020).
- Thompson, F.E.; Subar, A.F. Dietary assessment methodology. In Nutrition in Threvention and Treatment of Disease, 4th ed.; Coulston, A., Boushey, C., Ferruzzi, M., Delahanty, L., Eds.; Academic Press: San Diego, CA, USA, 2017; pp. 5–48. [Google Scholar]
- Magyar, É.E.; Tényi, D.; Gearhardt, A.; Jeges, S.; Abaligeti, G.; Tóth, Á.L.; Janszky, J.; Molnár, D.; Tényi, T.; Csábi, G. Adaptation and validation of the hungarian version of the Yale Food Addiction Scale for children. J. Behav. Addict. 2018, 7, 181–188. [Google Scholar] [CrossRef]
- Crönlein, T.; Langguth, B.; Popp, R.; Lukesch, H.; Pieh, C.; Hajak, G.; Geisler, P. Regensburger Insomnia Scale (RIS): A new short rating scale for the assessment of psychological symptoms and sleep in insomnia; Study design: Development and validation of a new short self-rating scale in a sample of 218 patients suffering from insomnia and 94 healthy controls. Health Qual. Life Outcome 2013, 11, 65. [Google Scholar]
- Forsberg, K.A.; Björkman, T.; Sandman, P.O.; Sandlund, M. Influence of a lifestyle intervention among persons with a psychiatric disability: A cluster randomised controlled trail on symptoms, quality of life and sense of coherence. J. Clin. Nurs. 2010, 19, 1519–1528. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, H.; Matsuzaki, I.; Sasahara, S.; Hatta, K.; Nagase, H.; Oshita, Y.; Ogawa, Y.; Nobukuni, Y.; Kambayashi, Y.; Ogino, K. Enhancement of a sense of coherence and natural killer cell activity which occurred in subjects who improved theixercise habits through health education in the workplace. J. Occup. Health 2003, 45, 278–285. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kohut, M.L.; McCann, D.A.; Russell, D.W.; Konopka, D.N.; Cunnick, J.E.; Franke, W.D.; Castillo, M.C.; Reighard, A.E.; Vanderah, E. Aerobic exercise, but not flexibility/resistancxercise, reduces serum IL-18, CRP, and IL-6 independent oeta-blockers, BMI, and psychosocial factors in older adults. Brain Behav. Immun. 2006, 20, 201–209. [Google Scholar] [CrossRef] [PubMed]
- Takafumi, M.; Takeda, F.; Tomohiro Okura, T. Physical activities impact sense of coherence among community-dwelling older adults. Geriatr. Gerontol. Int. 2017, 17, 2208–2215. [Google Scholar]
- Eriksson, M.; Lindström, B. Antonovsky’s sense of coherence scale and the relation with health: A systematic review. J. Epidemiol. Community Health 2006, 60, 376–381. [Google Scholar] [CrossRef] [PubMed]
- Wainwright, N.W.J.; Surtees, P.G.; Welch, A.A.; Luben, R.N.; Khaw, K.T.; Bingham, S.A. Healthy lifestyle choices: Could sense of coherence aid health promotion? J. Epidemiol. Community Health 2007, 61, 871–876. [Google Scholar] [CrossRef] [Green Version]
- Holmes, E.A.; O’Connor, R.C.; Perry, V.H.; Tracey, I.; Wessely, S.; Arseneault, L.; Ballard, C.; Christensen, H.; Cohen Silver, R.; Everall, I.; et al. Multidisciplinary research priorities for the COVID-19 pandemic: A call for action for mental health science. Lancet Psychiatry 2020, 7, 547–560. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of thvidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Gualano, M.R.; Loro, G.; Voglino, G.; Bert, F.; Siliquini, R. Effects of Covid-19 lockdown on mental health and sleep disturbances in Italy. Int. J. Environ. Res. Public Health 2020, 17, 4779. [Google Scholar] [CrossRef]
- Whitaker, C.; Stevelink, S.; Fear, N. Thse of facebook in recruiting participants for health research purposes: A systematic review. J. Med. Internet Res. 2017, 19, e290. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ali, S.H.; Foreman, J.; Capasso, A.; Jones, A.M.; Tozan, Y.; DiClemente, R.J. Social media as a recruitment platform for a nationwide online survey of COVID-19 knowledge, beliefs, and practices in the United States: Methodology and feasibility analysis. BMed Res. Methodol. 2020, 20, 116. [Google Scholar] [CrossRef] [PubMed]
- Fusz, K.; Tóth, Á.; Varga, B.; Rozmann, N.; Oláh, A. Different work schedules of nurses in Hungary and theiffects on health. Ideggyogy Sz 2017, 70, 136–139. [Google Scholar] [CrossRef] [PubMed]
- Ohayon, M.M. Epidemiology of insomnia: What we know and what we still need to learn. Sleep Med. Rev. 2002, 6, 97–111. [Google Scholar] [CrossRef]
- Cellini, N.; Natali, C.; Mioni, G.; Costa, S. Changes in sleep pattern, sense of time and digital media usuring COVID-19 lockdown in Italy. J. Sleep Res. 2020, 29, e13074. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Boros, S. Thffect of physical activity on sleep quality: A systematic review. Eur. J. Physiother. 2019. [Google Scholar] [CrossRef]
| Anthropometric Characteristics | Survey Date | Total | Friedman Test Pairwise Comparisons Adj. Sig. | |||
|---|---|---|---|---|---|---|
| N = 53 | ||||||
| Mean | Std. | 0–3 | 3–6 | 0–6 | ||
| Chest width (cm) | 0: Before starting the training | 94.5 | 8.9 | 0.808 | 0.001 | |
| After the 3rd month | 94.1 | 8.4 | 0.005 | |||
| After the 6th month | 93.3 | 8.0 | ||||
| Hip width (cm) | 0: Before starting the training | 98.3 | 9.9 | 0.308 | 0.001 | |
| After the 3rd month | 97.2 | 9.1 | <0.001 | |||
| After the 6th month | 96.0 | 8.5 | ||||
| Waist circumference (cm) | 0: Before starting the training | 88.0 | 10.8 | 0.734 | <0.001 | |
| After the 3rd month | 87.5 | 10.1 | <0.001 | |||
| After the 6th month | 85.9 | 10.1 | ||||
| Right thigh circumference (cm) | 0: Before starting the training | 55.3 | 4.7 | 0.884 | <0.001 | |
| After the 3rd month | 55.1 | 4.6 | <0.001 | |||
| After the 6th month | 54.0 | 4.4 | ||||
| Biceps circumference (cm) | 0: Before starting the training | 30.0 | 3.6 | 0.627 | 0.321 | |
| After the 3rd month | 29.8 | 3.3 | 0.887 | |||
| After the 6th month | 29.9 | 4.9 | ||||
| Body fat percentage | 0: Before starting the training | 28.5 | 5.9 | 0.285 | <0.001 | |
| After the 3rd month | 27.9 | 5.3 | <0.001 | |||
| After the 6th month | 26.9 | 3.3 | ||||
| Body Mass Index (kg/m2) | 0: Before starting the training | 23.3 | 4.3 | <0.001 | 0.627 | |
| After the 3rd month | 22.5 | 4.0 | <0.001 | |||
| After the 6th month | 23.1 | 4.0 | ||||
| Exercises | Survey Date | Total | Wilcoxon-Rank Test Sig. | |
|---|---|---|---|---|
| n = 53 | ||||
| Mean | Std. | 0 vs.6 | ||
| Squats | 0: Before starting the training | 24.9 | 7.4 | 0.022 |
| After 6 months | 26.5 | 6.9 | ||
| Pushups | 0: Before starting the training | 16.6 | 7.7 | 0.028 |
| After 6 months | 17.5 | 7.4 | ||
| Sit-ups | 0: Before starting the training | 18.2 | 7.3 | 0.033 |
| After 6 months | 19.9 | 6.0 | ||
| Stretches | 0: Before starting the training | 88.6 | 9.5 | 0.002 |
| After 6 months | 89.1 | 10.1 | ||
| Surveys | Healthy Diet | Unhealthy Diet | ||
|---|---|---|---|---|
| Spearman’s Rho | Sig. | Spearman’s Rho | Sig. | |
| Between months 0 and 3 | −0.296 | 0.142 | −0.201 | 0.315 |
| Between months 3 and 6 | −0.271 | 0.181 | −0.195 | 0.331 |
| Between months 0 and 6 | −0.690 | 0.001 | −0.202 | 0.312 |
| Variable | Survey Date | Total | Friedman Test Pairwise Comparisons Sig. | |||
|---|---|---|---|---|---|---|
| N = 53 | ||||||
| Mean | Std. | 0–3 | 3–6 | 0–6 | ||
| Comprehensibility | 0: Before starting the training | 9.3 | 3.1 | 0.143 | 0.048 | |
| After the 3rd month | 9.8 | 2.6 | 0.142 | |||
| After the 6th month | 10.5 | 3.0 | ||||
| Manageability | 0: Before starting the training | 8.7 | 2.5 | 0.174 | 0.003 | |
| After the 3rd month | 9.1 | 2.3 | 0.099 | |||
| After the 6th month | 10.1 | 3.1 | ||||
| Meaningfulness | 0: Before starting the training | 11.3 | 2.0 | 0.145 | 0.029 | |
| After the 3rd month | 11.8 | 2.2 | 0.466 | |||
| After the 6th month | 12.1 | 2.3 | ||||
| Sense of coherence | 0: Before starting the training | 29.3 | 5.8 | 0.356 | 0.005 | |
| After the 3rd month | 30.6 | 5.5 | 0.076 | |||
| After the 6th month | 32.7 | 7.6 | ||||
| Regensburger insomnia scale | 0: Before starting the training | 16.1 | 3.1 | <0.001 | <0.001 | |
| After the 3rd month | 13.8 | 2.9 | <0.001 | |||
| After the 6th month | 9.1 | 2.1 | ||||
| Variable | Sig. | Exp (B) | 95% CI for EXP (B) | |
|---|---|---|---|---|
| Lower | Upper | |||
| Do you live in a house with a garden? (yes = 1, no = 0) | 0.152 | 0.307 | 0.061 | 1.544 |
| Were you severely affected by the lockdown? | 0.449 | 1.252 | 0.700 | 2.239 |
| (yes = 1, no = 0) | ||||
| Did you spend less time outdoors? | 0.842 | 1.064 | 0.578 | 1.957 |
| (yes = 1, no = 0) | ||||
| Variable | Sig. | Exp(B) | 95% CI for EXP (B) | |
|---|---|---|---|---|
| Lower | Upper | |||
| SOC (stronger = 0, weaker = 1) | 0.091 | 2.101 | 2.101 | 0.887 |
| Physical activity (yes = 0, no = 1) | 0.036 | 0.383 | 0.383 | 0.156 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Szovák, E.; Varga, K.; Pelyva, I.Z.; Soós, R.; Jeges, S.; Kívés, Z.; Tóth, Á.L. Insights Gained in the Aftermath of the COVID-19 Pandemic: A Follow-Up Survey of a Recreational Training Program, Focusing on Sense of Coherence and Sleep Quality. Int. J. Environ. Res. Public Health 2020, 17, 9201. https://doi.org/10.3390/ijerph17249201
Szovák E, Varga K, Pelyva IZ, Soós R, Jeges S, Kívés Z, Tóth ÁL. Insights Gained in the Aftermath of the COVID-19 Pandemic: A Follow-Up Survey of a Recreational Training Program, Focusing on Sense of Coherence and Sleep Quality. International Journal of Environmental Research and Public Health. 2020; 17(24):9201. https://doi.org/10.3390/ijerph17249201
Chicago/Turabian StyleSzovák, Etelka, Károly Varga, Imre Zoltán Pelyva, Rita Soós, Sára Jeges, Zsuzsanna Kívés, and Ákos Levente Tóth. 2020. "Insights Gained in the Aftermath of the COVID-19 Pandemic: A Follow-Up Survey of a Recreational Training Program, Focusing on Sense of Coherence and Sleep Quality" International Journal of Environmental Research and Public Health 17, no. 24: 9201. https://doi.org/10.3390/ijerph17249201





