Identifying Patterns of Symptom Distress in Pregnant Women: A Pilot Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Design
2.2. Participants and Setting
2.3. Data Collection
2.4. Measurements
2.5. Data Analyses
2.6. Ethical Considerations
3. Results
3.1. Participant Characteristics
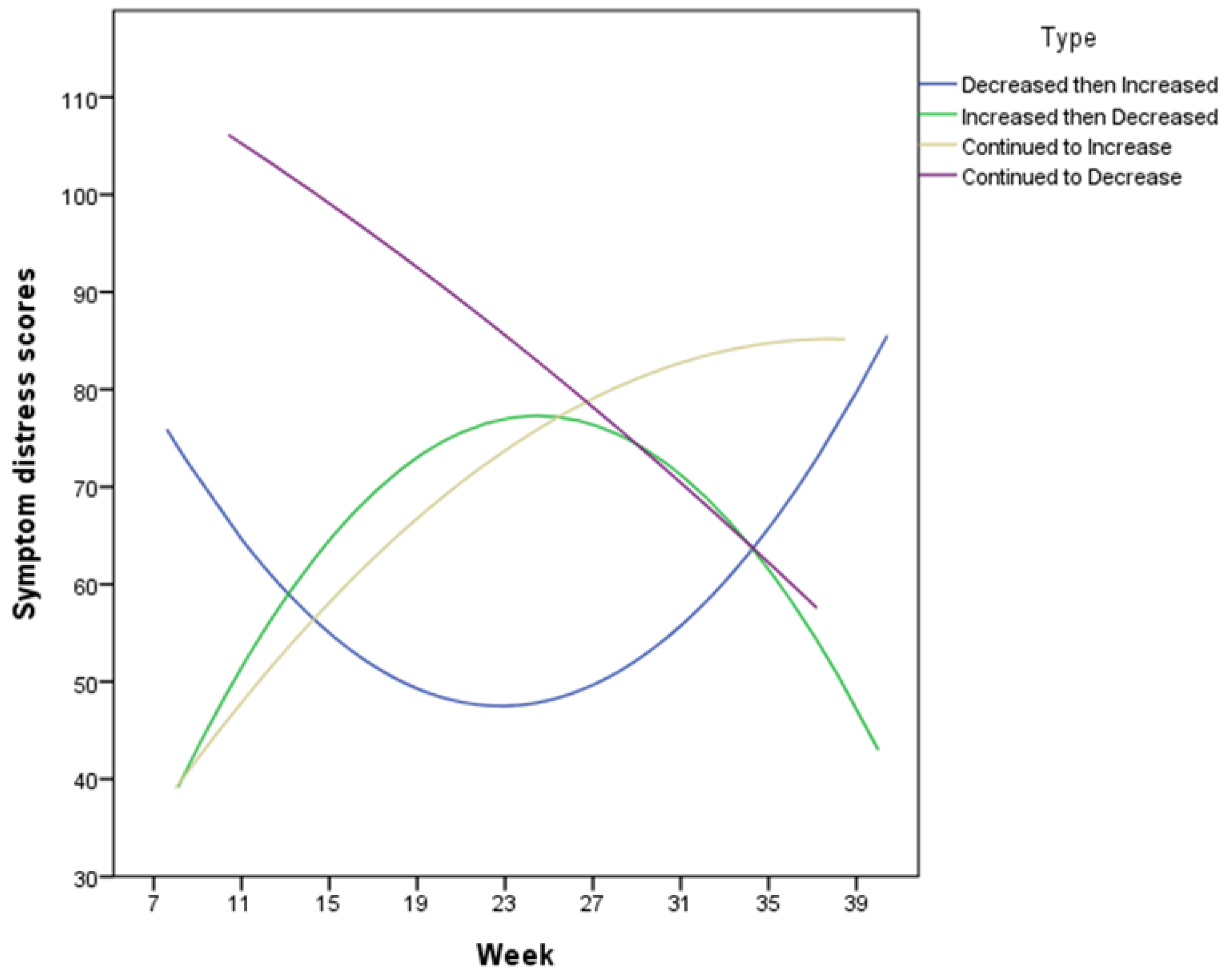
3.2. Patterns and Trends in Pregnancy-Induced Symptom Distress
3.3. The Distribution of Pregnancy-Related Symptom Distress Scores
3.4. Levels of Distress for Individual Symptoms Across the Patterns
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Beebe, K.R.; Gay, C.L.; Richoux, S.E.; Lee, K.A. Symptom experience in late pregnancy. J. Obstet. Gynecol. Neonatal Nurs. 2017, 46, 508–520. [Google Scholar] [CrossRef]
- Lutterodt, M.C.; Kähler, P.; Kragstrup, J.; Nicolaisdottir, D.R.; Siersma, V.; Ertmann, R.K. Examining to what extent pregnancy-related physical symptoms worry women in the first trimester of pregnancy: A cross-sectional study in general practice. BJGP Open 2019, 3, bjgpopen19X101674. [Google Scholar] [CrossRef]
- Jonsdottir, S.S.; Swahnberg, K.; Thome, M.; Oskarsson, G.K.; Bara Lydsdottir, L.; Olafsdottir, H.; Sigurdsson, J.F.; Steingrimsdottir, T. Pregnancy complications, sick leave and service needs of women who experience perinatal distress, weak social support and dissatisfaction in their partner relationships. Scand. J. Caring Sci. 2020, 34, 167–180. [Google Scholar] [CrossRef]
- Pearson, R.M.; Carnegie, R.E.; Cree, C.; Rollings, C.; Rena-Jones, L.; Evans, J.; Stein, A.; Tilling, K.; Lewcock, M.; Lawlor, D.A. Prevalence of prenatal depression symptoms among 2 Generations of pregnant mothers: The Avon longitudinal study of parents and children. JAMA Netw. Open 2018, 1, e180725. [Google Scholar] [CrossRef]
- Korhonen, L.S.; Karlsson, L.; Scheinin, N.M.; Korja, R.; Tolvanen, M.; Mertsola, J.; Peltola, V.; Karlsson, H. Prenatal maternal psychological distress and offspring risk for recurrent respiratory infections. J. Pediatr. 2019, 208, 229–235.e1. [Google Scholar] [CrossRef] [PubMed]
- Vollrath, M.E.; Sengpiel, V.; Landolt, M.A.; Jacobsson, B.; Latal, B. Is maternal trait anxiety a risk factor for late preterm and early term deliveries? BMC Pregnancy Childbirth 2016, 16, 286. [Google Scholar] [CrossRef]
- Rasouli, M.; Pourheidari, M.; Hamzeh Gardesh, Z. Effect of self-care before and during pregnancy to prevention and control preeclampsia in high-risk women. Int. J. Prev. Med. 2019, 10, 21. [Google Scholar] [CrossRef]
- Zheng, H.; Li, N.; Hao, Y.; Jin, C.; Meng, Y.; Yao, S.; Wei, J.; Pan, Y.; Gao, S.; Li, Z.; et al. Maternal severe stressful life events and risk of abnormal vaginal bleeding among urban Chinese pregnant women. J. Matern. Fetal Neonatal Med. 2020, 33, 2027–2031. [Google Scholar] [CrossRef]
- Pietikäinen, J.T.; Polo-Kantola, P.; Pölkki, P.; Saarenpää-Heikkilä, O.; Paunio, T.; Paavonen, E.J. Sleeping problems during pregnancy-a risk factor for postnatal depressiveness. Arch. Womens Ment. Health 2019, 22, 327–337. [Google Scholar] [CrossRef] [PubMed]
- Nakić Radoš, S.; Tadinac, M.; Herman, R. Anxiety during pregnancy and postpartum: Course, predictors and comorbidity with postpartum depression. Acta Clin. Croat. 2018, 57, 39–51. [Google Scholar] [CrossRef] [PubMed]
- Paul, S.; Corwin, E.J. Identifying clusters from multidimensional symptom trajectories in postpartum women. Res. Nurs. Health 2019, 42, 119–127. [Google Scholar] [CrossRef] [PubMed]
- Bai, G.; Korfage, I.J.; Groen, E.H.; Jaddoe, V.W.; Mautner, E.; Raat, H. Associations between Nausea, Vomiting, Fatigue and Health-Related Quality of Life of Women in Early Pregnancy: The Generation R Study. PLoS ONE 2016, 11, e0166133. [Google Scholar] [CrossRef] [PubMed]
- Starkweather, A.R.; Colloca, L.; Dorsey, S.G.; Griffioen, M.; Lyon, D.; Renn, C. Strengthening inter- and intraprofessional collaborations to advance biobehavioral symptom science. J. Nurs. Scholarsh. 2019, 51, 9–16. [Google Scholar] [CrossRef]
- Liu, M.C.; Kuo, S.H.; Lin, C.P.; Yang, Y.M.; Chou, F.H.; Yang, Y.H. Effects of professional support on nausea, vomiting, and quality of life during early pregnancy. Biol. Res. Nurs. 2014, 16, 378–386. [Google Scholar] [CrossRef]
- Jallo, N.; Ruiz, R.J.; Elswick, R.K., Jr.; French, E. Guided imagery for stress and symptom management in pregnant African American women. Evid. Based Complement. Alternat. Med. 2014, 2014, 840923. [Google Scholar] [CrossRef]
- Health Promotion Administration. Maternal Health Booklet. c2021. 29 January 2021. Available online: https://www.gender.ey.gov.tw/gecdb/Stat_Statistics_DetailData.aspx?sn=UNgbUqD746EaB%2fcBxzuqGw%3d%3d&d=194q2o4%2botzoYO%2b8OAMYew%3d%3d”https://www.hpa.gov.tw/File/Attach/7667/File_7162.pdf (accessed on 6 April 2021).
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Hedeker, D.; Gibbons, R.D.; Waternaux, C. Sample size estimation for longitudinal designs with attrition. J. Educ. Behav. Stat. 1999, 24, 70–93. [Google Scholar] [CrossRef]
- Lee, C.F.; Lin, H.M.; Sun, J.S.; Gu, Y.X. Symptom distress for women in different trimesters. J. Orient. Inst. Tech. 2009, 29, 206–217. [Google Scholar]
- Chien, S.Y. Comparison of Prenatal Stress, Symptom Distress, Social Support and Quality of Life Between Advanced-Age and Appropriate Reproductive Age Pregnant Women during Third Trimester. Master’s Thesis, Taipei University of Nursing and Health, Taipei, Taiwan, 2013. [Google Scholar]
- Harrison, X.A.; Donaldson, L.; Correa-Cano, M.E.; Evans, J.; Fisher, D.N.; Goodwin, C.E.D.; Robinson, B.S.; Hodgson, D.J.; Inger, R. A brief introduction to mixed effects modelling and multi-model inference in ecology. PeerJ 2018, 6, e4794. [Google Scholar] [CrossRef]
- Candel, M.J. Optimal designs for empirical bayes estimators of individual linear and quadratic growth curves in linear mixed models. Stat. Methods Med. Res. 2009, 18, 397–419. [Google Scholar] [CrossRef]
- Candel, M.J.J.M.; Winkens, B. Performance of empirical bayes estimators of level-2 random parameters in multilevel analysis: A Monte Carlo study for longitudinal designs. J. Educ. Behav. Stat. 2003, 28, 169–194. [Google Scholar] [CrossRef]
- Callahan, L. Fetal and placental Development and Functioning. In Core Curriculum for Maternal-Newborn Nursing, 5th ed.; Mattson, S., Smith, J.E., Eds.; Mosby: St Louis, MI, USA, 2018; pp. 37–62. [Google Scholar]
- Cunningham, F.G.; Leveno, K.J.; Bloom, S.L.; Dashe, J.S.; Hoffman, B.L.; Casey, B.M.; Spong, C.Y. Maternal physiology. In Williams Obstetrics, 25th ed.; Cunningham, F.G., Ed.; McGraw-Hill Education/Medical: New York, NY, USA, 2018; Chapter4. [Google Scholar]
- Bermas, B.L. Maternal Adaptations to Pregnancy: Musculoskeletal Changes and Pain; Lockwood, C.J., Ed.; 2021; Available online: https://www.uptodate.com/contents/maternal-adaptations-to-pregnancy-musculoskeletal-changes-and-pain (accessed on 13 February 2021).
- Lee, C.F.; Huang, Y.C.; Chi, L.K.; Lin, H.M.; Lin, C.J.; Hsiao, S.M. Constructing and applying an exercise counseling model for pregnant women: A preliminary study. Nurse Educ. Pract. 2018, 33, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.F.; Huang, Y.C.; Wen, F.H.; Lin, C.J.; Chi, L.K.; Chang, C.W. Effectiveness of individual face-to-face exercise counselling in changing exercise behaviours to relieve symptom distress in pregnant women. Int. J. Nurs. Pract. 2020, 26, e12837. [Google Scholar] [CrossRef] [PubMed]
- Ertmann, R.K.; Nicolaisdottir, D.R.; Kragstrup, J.; Siersma, V.; Lutterodt, M.C.; Bech, P. Physical discomfort in early pregnancy and postpartum depressive symptoms. Nord. J. Psychiatry 2019, 73, 200–206. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, S.M.; Nicoloro-SantaBarbara, J.; Auerbach, M.V.; Rosenthal, L.; Kocis, C.; Busso, C.E.; Lobel, M. Pregnancy-specific coping and changes in emotional distress from mid- to late pregnancy. J. Reprod. Infant. Psychol. 2019, 37, 397–412. [Google Scholar] [CrossRef]
- Aukia, L.; Paavonen, E.J.; Jänkälä, T.; Tolvanen, M.; Korja, R.; Karlsson, L.; Karlsson, H.; Polo-Kantola, P. Insomnia symptoms increase during pregnancy, but no increase in sleepiness—Associations with symptoms of depression and anxiety. Sleep Med. 2020, 72, 150–156. [Google Scholar] [CrossRef]
- Dryer, R.; Graefin von der Schulenburg, I.; Brunton, R. Body dissatisfaction and Fat Talk during pregnancy: Predictors of distress. J. Affect. Disord. 2020, 267, 289–296. [Google Scholar] [CrossRef] [PubMed]
- Obrochta, C.A.; Chambers, C.; Bandoli, G. Psychological distress in pregnancy and postpartum. Women Birth 2020, 33, 583–591. [Google Scholar] [CrossRef]
- Westerneng, M.; Witteveen, A.B.; Warmelink, J.C.; Spelten, E.; Honig, A.; de Cock, P. Pregnancy-specific anxiety and its association with background characteristics and health-related behaviors in a low-risk population. Compr. Psychiatry 2017, 75, 6–13. [Google Scholar] [CrossRef]
- Nakahara, K.; Michikawa, T.; Morokuma, S.; Ogawa, M.; Kato, K.; Sanefuji, M.; Shibata, E.; Tsuji, M.; Shimono, M.; Kawamoto, T.; et al. Association of maternal sleep before and during pregnancy with preterm birth and early infant sleep and temperament. Sci. Rep. 2020, 10, 11084. [Google Scholar] [CrossRef]
- Li, R.; Zhang, J.; Zhou, R.; Liu, J.; Dai, Z.; Liu, D.; Wang, Y.; Zhang, H.; Li, Y.; Zeng, G. Sleep disturbances during pregnancy are associated with cesarean delivery and preterm birth. J. Matern. Fetal Neonatal Med. 2017, 30, 733–738. [Google Scholar] [CrossRef]
- Tan, A.; Lowe, S.; Henry, A. Nausea and vomiting of pregnancy: Effects on quality of life and day-to-day function. Aust. N. Z. J. Obstet. Gynaecol. 2018, 58, 278–290. [Google Scholar] [CrossRef] [PubMed]
- Zielinski, R.; Searing, K.; Deibel, M. Gastrointestinal distress in pregnancy: Prevalence, assessment, and treatment of 5 common minor discomforts. J. Perinat. Neonatal Nurs. 2015, 29, 23–31. [Google Scholar] [CrossRef] [PubMed]
- Hu, X.; Ma, M.; Zhao, X.; Sun, W.; Liu, Y.; Zheng, Z.; Xu, L. Effects of exercise therapy for pregnancy-related low back pain and pelvic pain: A protocol for systematic review and meta-analysis. Medicine 2020, 99, e17318. [Google Scholar] [CrossRef]
- Cheng, C.Y.; Chou, Y.H.; Wang, P.; Tsai, J.M.; Liou, S.R. Survey of trend and factors in perinatal maternal fatigue. Nurs. Health Sci. 2015, 17, 64–70. [Google Scholar] [CrossRef]
- Winkel, S.; Einsle, F.; Wittchen, H.U.; Martini, J. Premenstrual symptoms are associated with psychological and physical symptoms in early pregnancy. Arch. Womens Ment. Health 2013, 16, 109–115. [Google Scholar] [CrossRef]
- Bender, M.S.; Janson, S.L.; Franck, L.S.; Lee, K.A. Theory of symptom management. In Middle Range Theory for Nursing, 4th ed.; Smith, M.J., Liehr, P.R., Eds.; Springer Publishing Co: New York, NY, USA, 2018; pp. 147–178. [Google Scholar]
- Chen, C.-N.; Yu, H.-C.; Chou, A.-K. Association between Maternal Pre-pregnancy Body Mass Index and Breastfeeding Duration in Taiwan: A Population-Based Cohort Study. Nutrients 2020, 12, 2361. [Google Scholar] [CrossRef] [PubMed]
- Ni, Y.L.; Chang, J.H.; Chen, L.H. Investigating the relationship between district-level socioeconomic status and individual obesity in Taiwanese adolescents: A large-scale cross-sectional analysis. Sci. Rep. 2019, 9, 2928. [Google Scholar] [CrossRef]
- Patabendige, M.; Athulathmudali, S.R.; Chandrasinghe, S.K. Mental Health Problems during Pregnancy and the Postpartum Period: A Multicenter Knowledge Assessment Survey among Healthcare Providers. J. Pregnancy 2020, 2020, 4926702. [Google Scholar] [CrossRef]
- Spedding, M.F.; Sorsdahl, K.; Parry, C.D.H.; Mathews, C.; Stein, D.J.; Williams, P.P. Psychological distress during pregnancy: Cross-sectional prevalence and associated risk factors in a South African sample. J. Nerv. Ment. Dis. 2020, 208, 755–763. [Google Scholar] [CrossRef] [PubMed]
| Variables | n | % |
| Education level | ||
| Junior high school or below | 8 | 8.4 |
| College or university or above | 87 | 91.6 |
| Family income | ||
| NT < 60,000 | 25 | 26.3 |
| NT 60,000–100,000 | 54 | 56.9 |
| NT > 100,000 | 16 | 16.8 |
| Occupation | ||
| Unemployed | 13 | 13.7 |
| Employed | 82 | 86.3 |
| Parity | ||
| Nulliparous | 52 | 54.7 |
| Multiparous | 43 | 45.3 |
| Abortion history | ||
| Yes | 11 | 11.6 |
| No | 84 | 88.4 |
| Prepregnancy BMI | ||
| Underweight (<18.5) | 9 | 9.5 |
| Normal (18.5–24.9) | 82 | 86.3 |
| Overweight or obese (>25) | 4 | 4.2 |
| Variables | Mean | SD |
| Age | 32.24 | 3.99 |
| Gestational weight gain (kg) | 9.11 | 4.22 |
| Decreased then Increased (n = 54) a | Increased then Decreased (n = 10) b | Continuously Increased (n = 27) c | Continuously Decreased (n = 4) d | F | p | Post Hoc Test | |
|---|---|---|---|---|---|---|---|
| Mean (SE) | Mean (SE) | Mean (SE) | Mean (SE) | ||||
| Total | 51.03(3.52) | 63.35(7.63) | 66.20(4.92) | 79.41(12.83) | 3.33 * | 0.023 | a < c a < d |
| Physical | 41.42(2.65) | 48.67(5.72) | 53.37(3.69) | 61.10(9.64) | 3.20 * | 0.027 | a < c |
| Psychological | 9.56(1.06) | 14.68(2.29) | 12.85(1.48) | 18.22(2.85) | 3.039 * | 0.033 | a < b a < d |
| Total average 1 | 2.32(0.16) | 2.88(0.35) | 3.02(0.22) | 3.61(0.58) | 3.313 * | 0.024 | a < c a < d |
| Turning point (weeks) | – | – | – | – | – | ||
| Total | 22.02 | 26.77 | |||||
| Physical | 21.01 | 26.69 | |||||
| Psychological | 22.34 | 23.99 |
| Decreased then Increased (n = 54) a | Increased then Decreased (n = 10) b | Continuously Increased (n = 27) c | Continuously Decreased (n = 4) d | F | p | Post Hoc Test | |
|---|---|---|---|---|---|---|---|
| Mean (SE) | Mean (SE) | Mean (SE) | Mean (SE) | ||||
| 4.06 (0.24) | 4.59 (0.50) | 5.22 (0.33) | 6.23 (0.86) | 4.14 ** | 0.008 | a < c; a < d |
| 3.84 (0.21) | 4.26 (0.44) | 4.76 (0.29) | 4.32 (0.75) | 2.26 | 0.086 | |
| 3.45 (0.26) | 4.39 (0.56) | 4.24 (0.37) | 5.51 (0.96) | 2.44 | 0.07 | |
| 3.38 (0.25) | 2.87 (0.54) | 4.04 (0.35) | 4.63 (0.93) | 1.78 | 0.16 | |
| 3.19 (0.32) | 3.04 (0.68) | 4.3 (0.44) | 2.97 (1.15) | 1.63 | 0.19 | |
| 2.70 (0.16) | 3.13 (0.56) | 3.67 (0.37) | 4.07 (0.95) | 1.91 | 0.13 | |
| 2.54 (0.26) | 3.58 (0.55) | 3.99 (0.36) | 5.42 (0.94) | 5.78 ** | 0.001 | a < c; a < d |
| 2.47 (0.24) | 3.57 (0.51) | 2.82 (0.33) | 3.49 (0.87) | 1.58 | 0.20 | |
| 2.28 (0.24) | 1.70 (0.50) | 2.38 (0.33) | 3.06 (0.87) | 0.74 | 0.53 | |
| 2.10 (0.22) | 2.34 (0.48) | 2.57 (0.31) | 2.41 (0.81) | 0.53 | 0.67 | |
| 1.85 (0.22) | 2.86 (0.46) | 2.76 (0.30) | 3.45 (0.79) | 3.45 * | 0.02 | a < b; a < c |
| 1.84 (0.20) | 2.78 (0.43) | 2.40 (0.28) | 3.15 (0.74) | 2.36 | 0.077 | |
| 1.66 (0.22) | 3.16 (0.47) | 2.17 (0.31) | 2.88 (0.81) | 3.29 * | 0.025 | a < b |
| 1.66 (0.21) | 1.47 (0.44) | 1.67 (0.29) | 2.50 (0.75) | 0.48 | 0.70 | |
| 1.64(0.24) | 2.39(0.50) | 2.72(0.33) | 2.53(0.86) | 2.61 | 0.06 | |
| 1.46(0.24) | .98(0.51) | 2.06(0.33) | 1.63(0.87) | 1.23 | 0.30 | |
| 1.14(0.18) | 1.67(0.39) | 1.83(0.26) | 2.57(0.67) | 2.73 * | 0.049 | a < c; a < d |
| 2.36(0.26) | 3.07(0.56) | 3.20(0.36) | 4.65(0.94) | 2.71 | 0.05 | |
| 1.91(0.23) | 3.14(0.49) | 2.55(0.32) | 3.97(0.82) | 3.56 * | 0.017 | a < b; a < d |
| 2.14(0.23) | 3.09(0.50) | 2.92(0.32) | 4.33(0.85) | 3.34 * | 0.023 | a < d |
| 1.64(0.20) | 2.78(0.44) | 2.24(0.29) | 3.01(0.74) | 3.03 * | 0.034 | a < b |
| 1.49(0.20) | 2.58(0.42) | 1.95(0.27) | 2.16(0.72) | 2.12 | 0.10 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, C.-F.; Wen, F.-H.; Hsiung, Y.; Huang, J.-P.; Chang, C.-W.; Chen, H.-H. Identifying Patterns of Symptom Distress in Pregnant Women: A Pilot Study. Int. J. Environ. Res. Public Health 2021, 18, 6333. https://doi.org/10.3390/ijerph18126333
Lee C-F, Wen F-H, Hsiung Y, Huang J-P, Chang C-W, Chen H-H. Identifying Patterns of Symptom Distress in Pregnant Women: A Pilot Study. International Journal of Environmental Research and Public Health. 2021; 18(12):6333. https://doi.org/10.3390/ijerph18126333
Chicago/Turabian StyleLee, Ching-Fang, Fur-Hsing Wen, Yvonne Hsiung, Jian-Pei Huang, Chun-Wei Chang, and Hung-Hui Chen. 2021. "Identifying Patterns of Symptom Distress in Pregnant Women: A Pilot Study" International Journal of Environmental Research and Public Health 18, no. 12: 6333. https://doi.org/10.3390/ijerph18126333
APA StyleLee, C.-F., Wen, F.-H., Hsiung, Y., Huang, J.-P., Chang, C.-W., & Chen, H.-H. (2021). Identifying Patterns of Symptom Distress in Pregnant Women: A Pilot Study. International Journal of Environmental Research and Public Health, 18(12), 6333. https://doi.org/10.3390/ijerph18126333






