Migrants and Service Providers’ Perspectives of Barriers to Accessing Mental Health Services in South Australia: A Case of African Migrants with a Refugee Background in South Australia
Abstract
1. Introduction
Theoretical Framework
2. Materials and Methods
2.1. Study Design and Sampling
2.2. Data Collection Procedure
2.3. Data Analysis
2.4. Ethical Consideration
3. Results
3.1. Sociodemographic Profile of the Participants
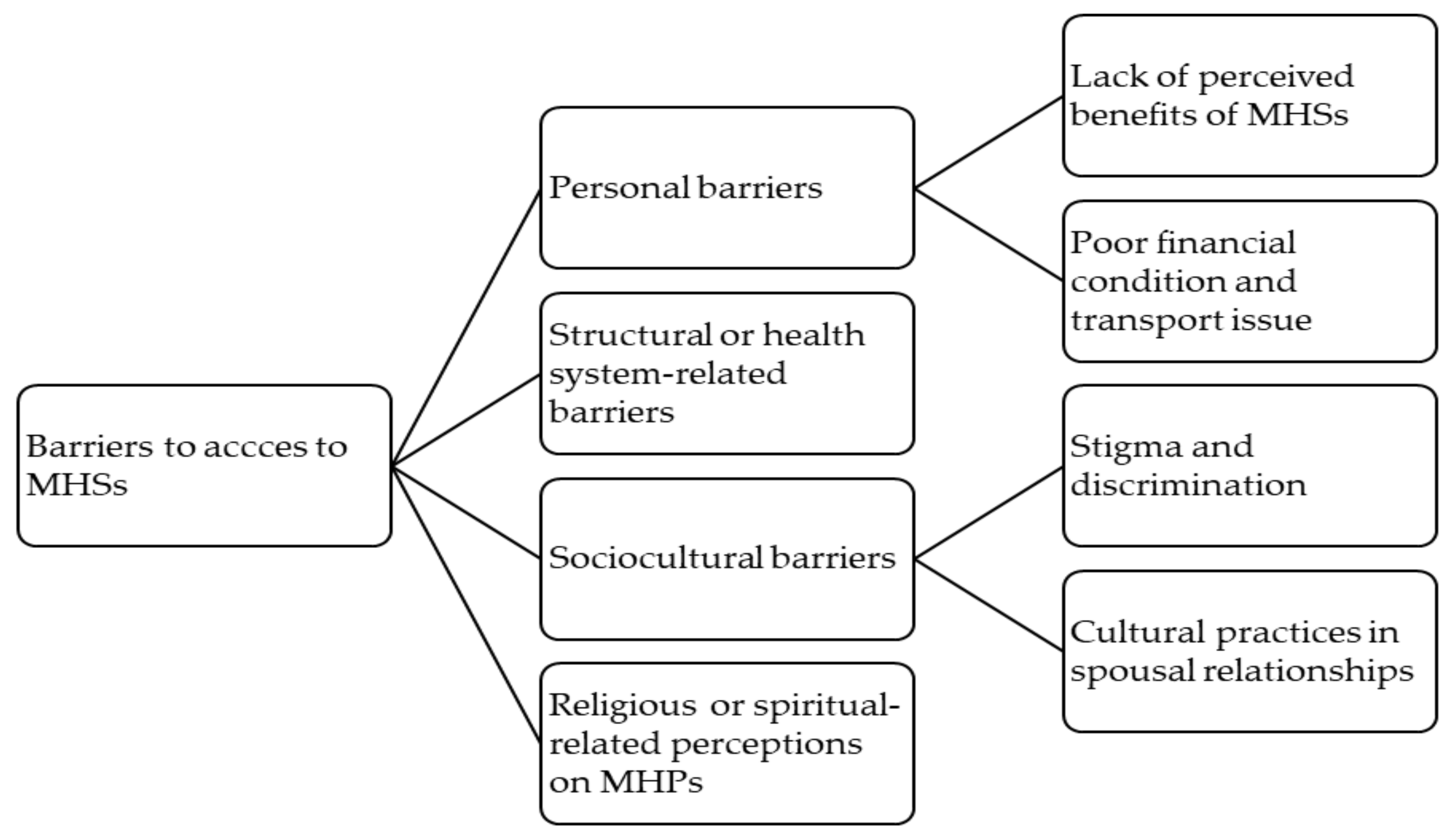
3.2. Personal Barriers
3.2.1. Lack of Knowledge of Mental Health Problems and Services
“I think it [barrier to access MHS] was also understanding what the services entailed, and really understanding what mental illness is. I mean, I didn’t properly understand mental health and mental illness until I came to university, and I actually started doing psychology as a course. I mean, high school, they talk about mental health and wellbeing a little bit, but they’re not really so focused on actually teaching you what it is and you know, there’s different levels and because you do have a mental illness, it’s impacting your life. I didn’t get much information about this at school or within the community where I live”(African migrant 8, female, Somalia)
“The main barrier [to access to MHSs] is that people don’t recognise that they are sick or they are suffering mental illness as such, then they are not prepared to access services, because they feel they fit”(African migrant 14, male, Burundi).
“I think the other barriers (to the access to MHSs) will be—it’s a lack of understanding around that mental health and well-being. …. The African community, I think they have limited understanding around mental illness, especially, based on the clients that I’ve been seeing, I do feel like they have no idea if we talk about mental health wellbeing. And also, I think there also is a lack of belief that mental health or mental illness is really there. …. I think lack of understanding around mental health and, I don’t know, mental illness, it’s I think the key. The key and the main barrier (to the access to MHSs)”(Service Provider 3, female)
“I think they really don’t even acknowledge there is a problem. One, because this person is not running on the street naked, because the traditional mental health that is known is for someone who is running on the street naked, that’s what we call that they have mental illness. Anything else doesn’t count. It doesn’t count as being a mental illness. …. I actually didn’t even think it was depression, I just thought it was just something that’s happening, getting emotional or something, but when I look back, I think I had depression. Now that I know, I know that it was depression”(African migrant 6, female, Burundi)
“Normally when people hear the word “mental health” in the community it is mainly for people that are considered—I guess, not normal, and everyone see you as being crazy”(Service Provider 5, Female)
3.2.2. Lack of Perceived Benefits of Mental Healthcare Services
“Also, another thing (that prevent her from accessing the services), I just feel like talking about it won’t really change, because they will just tell me to stay safe, to look after my children, and it’s always the same thing. …. So that’s also another thing that has made me not to speak to the health services”(African migrant 19, female, Kenya)
“.… You just go there and talk or sing, or they make fun of even relaxation technique and stuff like that. So, things like that, if I’m just coming and I’m just doing things to please you with no thought that it’s going to make a difference, then it’s not even going to have an effect”(African migrant 10, female, Democratic Republic of Congo)
“I can give a story of a guy that I was speaking to that told me he had been connected with a therapist doing trauma work. …he said, “Look, I’ve done it before. My clinician just asks me questions, questions, questions. And I came in, he asked the same questions in different ways. How is this helping me?”(Service Provider 8, Male)
3.2.3. Poor Financial Condition and Transport Issues
“If four of my kids have mental illnesses, then I have to pay for four of them to get (access the services)—you know. And with Medicare, I think you get seven—oh, no, ten sessions, and then it’s like okay, well, they’re only getting ten sessions (for free), I have to pay for the next few sessions. And then, that’s very costly. And then, I have private health insurance. …. Why am I putting $100, $200 for one session when my kid could use that for their new school uniform, you know?”(African migrant 8, female, Somalia)
“Financial issue is also a barrier for many of them (African migrants) to pay for transportation or healthcare services. …. Just lately—I have to share quickly something. I took a client to a service for financial issues and when I went there with him, he really was hopeless because he got sent an electricity bill. On hand, he got a letter saying like, okay, if you don’t pay by this time you get it cut off. Then I went with him to a service, he was really keen and when we went there the lady who was there said, ‘Oh no, I can’t help him’ ….”(Service Provider 6, male)
“The location is also another big barrier (to the access to MHSs). Because a lot of refugees now tend to stay in groups in certain areas. So, if I was to advise the government what is the best thing you want to—I’ll probably always try and put services in the place where these people are so that at least they can access them easily”(African migrant 1, male, South Sudan)
“The barriers are the locations of certain places that people need to travel, not understanding or not knowing how to catch public transport”(Service Provider 7, female)
“Another problem for some people, I think, is transport. Not every family has access to a vehicle and when it comes to such thinking: we’ll catch one bus and then we’ll go and catch another one and that becomes a bit of problem”(African migrant 13, male Democratic Republic of Congo)
3.3. Structural or Health System-Related Barriers
“You have to book and then maybe they give you appointment next week and by the time you reach on that day, maybe that feeling which you are having because you’ve lost somebody in your family or this and this and this, maybe it’s already covered. So that’s another barrier that is not actually immediate service which you can get straight away”(African migrant 14, male, Burundi)
“When I was working (role redacted to de-identify the participant) I got a report of the clients who (wanted an) appointment to see doctors, and every time they ring, “Oh, we are fully booked. Maybe call us in two weeks’ time,” and then two of the families go—told me that they went in ED—emergency department, and they were kept waiting for a long time before they come in”(African migrant 13, male, Democratic Republic of Congo)
- Q:
- “It’s really interesting that you’ve said you’d be happy to talk to someone (talk to a counsellor about your mental health issue), but you just don’t know who or where to go to find them. Is that right?
- A:
- Yeah.
- Q:
- Yeah. And your GP hasn’t helped with that, your GP hasn’t helped you connect to someone (e.g., a counsellor)?
- A:
- They gave me different GP. Since I’ve been here, I do not have particular one GP. The GP I used to see before, today when you book—you want to go see a GP, they will give you another GP. Then when you book, then they give you another GP. I keep telling I want to continue seeing one single GP. Not everyone you can go to talk to” (African migrant 12, female, Liberia).
“I have really discussed with people who refuse to go seeking for help because they are being disappointed. Because they are not being listened to, because they have been rejected, they were not satisfied with the services. …. I had another one who called me. He said to me, “Look can you change my GP?” And I said, “But why should I change your GP?” “Because I went there (to the GP) and I was not satisfied.” She told me, “You have to do quickly, I have a lot of clients waiting there.” …. that is a bit disappointing, so he wants to change that GP because he is not happy with the services”(Service Provider 6, male)
3.4. Sociocultural Factors
3.4.1. Stigma and Discrimination
“I have mental health issue, but I will not admit, or I will not accept that I actually have some mental illness. Because of that fear of the stigma (as crazy persons) from the community, that if I admit and say: I have some mental illness then I will be isolated from the community”(African migrant 1, male, South Sudan)
“I think the stigma and discrimination associated with mental health issue within the communities, it’s quite shunned upon. They’re quite—they don’t want the other community members to know, which—it’s really quite disheartening, but it is what it is. So, I think they’re denying themselves to actually have safe supports from within their community”(Service Provider 7, female)
“I don’t want to disclose this, I don’t want to disclose that I’ve been through this. I might be mocked or looked down at. It’s a very small community. My name will be there”(African migrant 3, male, Democratic Republic of Congo)
“It’s a bit shameful if you’ve got a mental illness. It’s not seen as similar to if you had a physical—if you had a physical break that’s okay, but if you have something going on inside your mind that you can’t see, it’s taken more as you’re not right in the head, rather than situational”(Service Provider 2, male)
“There have been a few cases recently where a few girls—who are actually just a few years older than me, they were admitted to mental health institutions because they had a reached a point where they were just keeping it in, keeping it in. They had just broken down completely. And then now there’s this negative connotation attached to them, their family, and then that sort of just shunned a lot of other girls from being able to speak out, because they’re afraid of it impacting the family and seeing how it went”(African migrant 9, female, Sierra Leone)
“You’re not a part of community anymore because you have mental health issue and have been visiting mental health clinic, you know? So, this why people may not like to disclose that. You are considered as an outcast (if you have a mental health issue). People will not listen to you if you have mental health illness. So, whatever good idea you may come up with, people will not consider it. That’s the problem”(African migrant 3, male, Democratic Republic of Congo)
“I got a clear picture when I came to Australia because back home, if there is a mental illness, it’s like, you’ve been written off. They use that to judge you, they label you. Anything you would talk or do, they will not take you seriously and say, ‘he is mad, he has got mental illness, you know?”(African migrant 15, male, Sierra Leone)
“I think in my country, especially the (tribe’s name redacted for confidentiality), they say if you are seeing a GP or a psychologist, they will think you are crazy. They will be like, you are crazy. And sometimes they say people who are seeing the counsellors and the GP and psychologists are crazy people. …. It (being crazy) means someone with the wrong mentality. Their brain does not have good thoughts, or the person does not act quite good, or has a problem in their brain, or has a mentality problem”(African migrant 17, female South Sudan)
“Even when they come there (mental healthcare facilities or services), they are not free to share much and sometimes they don’t want even to be known that they’ve gone there. They regard that—and this is for many—when they are being known that they are going to see someone to deal with their psychological or mental health, that they’re crazy”(African migrant 14, male, Burundi)
3.4.2. Cultural Practices in Spousal Relationships
“If they are women, women will never, never ever seek for assistance from our community. It’s a strong community that depends on husband’s permission”(African migrant 5, male, Democratic Republic of Congo)
“Another barrier is some of them (women), they are on this mental problem and they are still with their husband. And it’s hard for them to be with their husband and their husband does not want them to do this (access mental health services)”(African migrant 16, female, Liberia)
“Well, because I am finding that particular family that I’ve worked with, the husband is always the talker, and the wife is quite reserved. So, there has been times where I have noticed from a cultural perspective that it’s becoming quite clear that maybe the husband is quite dominant over the female”(Service Provider 7, female)
“Most of the Africans are brought up in a very cultural way where you are set up to be tough. You know, as a tough person. So, by saying words like I’m stressed and all this, then they regard, yeah, this man is not a tough guy”(African migrant 9, male, Sierra Leone)
“It’s something that, it’s cultural. When a guy reveals these things (mental health issues), they usually fear to be judged. They will be like this guy is very weak, and he doesn’t act like a man. So that’s why they usually keep their feelings inside because they are fearing to be judged. It’s a fear they have and also their cultural beliefs, so I think, yeah. They will feel like they’re weak. And they feel like they’re not macho, or they’re not men enough, because they usually say, you shouldn’t hurt a woman; that’s what is usually said. So, they say women heart is weak, and so if the men act, they will be like, don’t act like a woman. Be like ‘a man’. Stop revealing everything”(African migrant 17, female, South Sudan)
“They don’t want to talk about it, because they think they’ll look weak. …. Men, they don’t talk about it at all. Men don’t share emotions. So, it will be almost impossible to bring men to see counsellors. Women you can still try and try and try and you can go, and with their men, oh, my God”(Service Provider 1, female)
3.5. Religious or Spiritual-Related Perceptions on MHPs
“They will just say—because a lot of people believe in God and people who really don’t have education or so on, they think it’s a God’s punishment. So, if it is God’s punishment, no service can help you. So, I guess they don’t feel good when they think it’s something like this—they need to refer to faith”(Service Provider 6, male)
“Like, mental illnesses are considered in Ethiopia that they are like supernatural, come from the evil, come from God’s punishment. Like people believe in witchcraft and others. So, you know, those things are the things that will hinder or stop people from seeking mental health services here, and like people here, people will trust more to the Church and the priest around them”(African migrant 2, male, Ethiopia)
“They will go to the church; they will pray or to the mosque for the Imam to pray for them. So, they will just say; I have nightmares, I feel sad, or I cannot sleep, I cannot eat. Those are sign of depression”(Service Provider 6, male)
“Sometimes they would go with a faith leader. Because a lot of people have this idea that if you are experiencing mental illness, you are cursed, et cetera. And you do need some sort of healing through faith”(African migrant 8, female, Somalia)
“Even back home, even now, I don’t think that they (people in Africa) have many programs or types of services like what we have here. So, because of that, many people just rely on family or those who are Christian, maybe rely on churches and ministers for their support. Up to now, that’s still existing that maybe we don’t regard it is an issue”(African migrant 14, male, Burundi)
“They (religious leaders) come and counsel you, they teach you a lot of work in the Bible, that there are some people who struggle in the Bible and also sometime some people help you. And they can help you to come and do it, to work for you”(African migrant 11, female, South Sudan)
4. Discussion
4.1. Perceptions of MHPs, Health Literacy, Religiosity and Mental Health Stigma
4.2. Structural Factors including Health System and Patriarchal Beliefs as Barriers
4.3. Study Limitations and Strengths
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| No | Item | Guide Questions/Description | Page |
| Domain 1: Research team and reflexivity | |||
| Personal Characteristics | |||
| 1. | Interviewer/facilitator | Which author/s conducted the interview or focus group? | 4 |
| 2 | Credentials | What were the researcher’s credentials? E.g. PhD, MD | 4 |
| 3 | Occupation | What was their occupation at the time of the study? | 4 |
| 4 | Gender | Was the researcher male or female? | 4 |
| 5 | Experience and training | What experience or training did the researcher have? | 4 |
| Relationship with participants | |||
| 6 | Relationship established | Was a relationship established prior to study commencement? | 4 |
| 7 | Participant knowledge of the interviewer | What did the participants know about the researcher? e.g., personal goals, reasons for doing the research | 5 |
| 8 | Interviewer characteristics | What characteristics were reported about the interviewer/facilitator? e.g., Bias, assumptions, reasons and interests in the research topic | 5 |
| Domain 2: study design | |||
| Theoretical framework | |||
| 9 | Methodological orientation and Theory | What methodological orientation was stated to underpin the study? e.g., grounded theory, discourse analysis, ethnography, phenomenology, content analysis | 2–3 |
| Participant selection | |||
| 10 | Sampling | How were participants selected? e.g., purposive, convenience, consecutive, snowball | 4 |
| 11 | Method of approach | How were participants approached? e.g., face-to-face, telephone, mail, email | 4 |
| 12 | Sample size | How many participants were in the study? | 4 |
| 13 | Non-participation | How many people refused to participate or dropped out? Reasons? | 4 |
| Setting | |||
| 14 | Setting of data collection | Where was the data collected? e.g., home, clinic, workplace | 4 |
| 15 | Presence of non-participants | Was anyone else present besides the participants and researchers? | 4 |
| 16 | Description of sample | What are the important characteristics of the sample? e.g., demographic data, date | 5 |
| Data collection | |||
| 17 | Interview guide | Were questions, prompts, guides provided by the authors? Was it pilot tested? | 4 |
| 18 | Repeat interviews | Were repeat interviews carried out? If yes, how many? | 4 |
| 19 | Audio/visual recording | Did the research use audio or visual recording to collect the data? | 4 |
| 20 | Field notes | Were field notes made during and/or after the interview or focus group? | 4 |
| 21 | Duration | What was the duration of the interviews or focus group? | 4 |
| 22 | Data saturation | Was data saturation discussed? | 4 |
| 23 | Transcripts returned | Were transcripts returned to participants for comment and/or correction? | 4 |
| Domain 3: analysis and findings | |||
| Data analysis | |||
| 24 | Number of data coders | How many data coders coded the data? | 4–5 |
| 25 | Description of the coding tree | Did authors provide a description of the coding tree? | 13 |
| 26 | Derivation of themes | Were themes identified in advance or derived from the data? | 4–5 |
| 27 | Software | What software, if applicable, was used to manage the data? | 5 |
| 28 | Participant checking | Did participants provide feedback on the findings? | 4 |
| Reporting | |||
| 29 | Quotations presented | Were participant quotations presented to illustrate the themes/findings? Was each quotation identified? e.g., participant number | 6–12 |
| 30 | Data and findings consistent | Was there consistency between the data presented and the findings? | 6–12 |
| 31 | Clarity of major themes | Were major themes clearly presented in the findings? | 6–12 |
| 32 | Clarity of minor themes | Is there a description of diverse cases or discussion of minor themes? | 6–12 |
Appendix B. Interview Guide
- How mental health problems are perceived in your communities?
- What factors do you think influence your perceptions or perceptions in African communities about mental health problems?
- ◦
- Social, cultural and religious factors? Why? Please explain.
- ◦
- How they influence your perceptions about mental health problems?
- Do people talk about mental health problems in your communities? Why? Please explain.
- Where are the services available?
- ◦
- What kind of services have you accessed?
- ◦
- What are the procedures to access the services? Are they easy and helpful? Why?
- ◦
- How do feel about the services you have received? Comfortable or not and why?
- Do you think the services meet your expectations? Why? Please explain
- What do you think about benefits of the services to you? Please explain.
- What do you think about the influence of community perceptions about mental health problems on your access to mental healthcare services? Pleases explain.
- ◦
- Do you think such perceptions also influence the access of African migrants to mental healthcare service? Why? Please explain.
- Who makes the decision? Why?
- What factors do you think influence your or your family decision to access or not to access mental healthcare services? Why? Please explain.
- How and why? Please explain more about these.
- What are the costs for? Please explain.
- How do you reach healthcare facilities to access mental healthcare services?
- How far is it to reach mental healthcare services?
- They have good knowledge about mental health problems or not? Please explain more about it.
- What are the perceptions, if any, they have about mental health problems? Why?
- What influences their perceptions about the problem?
- ◦
- Culture, religion? Why?
- Do you think they understand the procedures to access the services or not? Are they easy and helpful? Why? Please explain more about these.
- What are the costs for? Please explain.
- Do you think transportation and location where they live have an influence on their access to mental healthcare services? Why? Please explain.
- What are they? Why? Please explain.
References
- Organization for Economic Cooperation and Development. International Migration Outlook 2013; OECD Publishing: Paris, France, 2013. [Google Scholar]
- Renzaho, A.; Polonsky, M.; Mellor, D.; Cyril, S. Addressing migration-related social and health inequalities in Australia: Call for research funding priorities to recognise the needs of migrant populations. Aust. Health Rev. 2016, 40, 3–10. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. Migration, Australia: Statistics on Australia’s International Migration, Internal Migration (Interstate and Intrastate), and the Population by Country of Birth; Australian Bureau of Statistics: Melbourne, Australia, 2020.
- Refugee Council of Australia. An analysis of UNHCR’s 2018 Global Refugee Statistics: How Generous Is Australia’s Refugee Program Compared to Other Countries? Refugee Council of Australia: Melbourne, Australia, 2019. [Google Scholar]
- Cooper, S.; Enticott, J.C.; Shawyer, F.; Meadows, G. Determinants of Mental Illness among Humanitarian Migrants: Longitudinal Analysis of Findings From the First Three Waves of a Large Cohort Study. Front. Psychiatry 2019, 10, 545. [Google Scholar] [CrossRef] [PubMed]
- Steel, Z.; Silove, D.; Brooks, R.; Momartin, S.; Alzuhairi, B.; Susljik, I. Impact of immigration detention and temporary protection on the mental health of refugees. Br. J. Psychiatry 2006, 188, 58–64. [Google Scholar] [CrossRef]
- Kirmayer, L.J.; Narasiah, L.; Munoz, M.; Rashid, M.; Ryder, A.G.; Guzder, J.; Hassan, G.; Rousseau, C.; Pottie, K. Common mental health problems in immigrants and refugees: General approach in primary care. CMAJ 2011, 183, E959–E967. [Google Scholar] [CrossRef] [PubMed]
- Porter, M.; Haslam, N. Predisplacement and postdisplacement factors associated with mental health of refugees and internally displaced persons: A meta-analysis. JAMA 2005, 294, 602–612. [Google Scholar] [CrossRef] [PubMed]
- Robjant, K.; Hassan, R.; Katona, C. Mental health implications of detaining asylum seekers: Systematic review. Br. J. Psychiatry 2009, 194, 306–312. [Google Scholar] [CrossRef] [PubMed]
- Hussain-Gambles, M.; Atkin, K.; Leese, B. Why ethnic minority groups are under-represented in clinical trials: A review of the literature. Health Soc. Care Community 2004, 12, 382–388. [Google Scholar] [CrossRef]
- Udah, H.; Singh, P.; Hiruy, K.; Mwanri, L. African Immigrants to Australia: Barriers and Challenges to Labor Market Success. JAAS 2019, 54, 1159–1174. [Google Scholar] [CrossRef]
- Wood, N.; Charlwood, G.; Zecchin, C.; Hansen, V.; Douglas, M.; Pit, S.W. Qualitative exploration of the impact of employment and volunteering upon the health and wellbeing of African refugees settled in regional Australia: A refugee perspective. BMC Public Health 2019, 19, 143. [Google Scholar] [CrossRef]
- Giallo, R.; Riggs, E.; Lynch, C.; Vanpraag, D.; Yelland, J.; Szwarc, J.; Duell-Piening, P.; Tyrell, L.; Casey, S.; Brown, S.J. The physical and mental health problems of refugee and migrant fathers: Findings from an Australian populationbased study of children and their families. BMJ Open 2017, 7, e015603. [Google Scholar] [CrossRef] [PubMed]
- O’Mahony, J.M.; Donnelly, T.T. The influence of culture on immigrant women’s mental health care experiences from the perspectives of health care providers. Issues Ment. Health Nurs. 2007, 28, 453–471. [Google Scholar] [CrossRef]
- Straiton, M.; Grant, J.F.; Winefield, H.R.; Taylor, A. Mental health in immigrant men and women in Australia: The North West Adelaide Health Study. BMC Public Health 2014, 14, 1111. [Google Scholar] [CrossRef]
- Blackmore, R.; Boyle, J.A.; Fazel, M.; Ranasinha, S.; Gray, K.M.; Fitzgerald, G.; Misso, M.; Gibson-Helm, M. The prevalence of mental illness in refugees and asylum seekers: A systematic review and meta-analysis. PLoS Med. 2020, 17, e1003337. [Google Scholar] [CrossRef] [PubMed]
- Shawyer, F.; Enticott, J.C.; Block, A.A.; Cheng, I.-H.; Meadows, G.N. The mental health status of refugees and asylum seekers attending a refugee health clinic including comparisons with a matched sample of Australian-born residents. BMC Psychiatry 2017, 17, 76. [Google Scholar] [CrossRef] [PubMed]
- Australian Institute of Health and Welfare. Australia’s Health 2020 Data Insights. Australia’s Health Series No. 17. Cat. No. AUS 231; AIHW: Canberra, Australia, 2020.
- Mares, S.; Jenkins, K.; Lutton, S.; Newman, L. Impact of COVID-19 on the mental health needs of asylum seekers in Australia. Australas. Psychiatry 2021, 29, 417–419. [Google Scholar] [CrossRef]
- O’Mara, B.; Monani, D.; Carey, G. Telehealth, COVID-19 and refugees and migrants in Australia: Policy and related barriers and opportunities for more inclusive health and technology systems. Int. J. Health Policy Manag. 2021, 1–5. [Google Scholar] [CrossRef]
- Tania Miletic. Mental Health and Wellbeing for Victoria’s Multicultural Communities under COVID-19; The Ethnic Communities’ Council of Victoria: Melbourne, Australia, 2020. [Google Scholar]
- Harmony Alliance. Migrant and Refugee Women in the COVID-19 Pandemic: Impact, Resilience and the Way Forward; National Consultation: Melbourne, Australia, 2021. [Google Scholar]
- Hunt, P.; Mesquita, J. Mental disabilities and the human right to the highest attainable standard of health. Hum. Rts. Q. 2006, 28, 332. [Google Scholar] [CrossRef]
- Baerenholdt, J.O.; Aarsaether, N. Coping strategies, social capital and space. Eur. Urban Reg. Stud. 2002, 9, 151–165. [Google Scholar] [CrossRef]
- Ball, W.; Beckford, J.A. Religion, education and city politics: A case study of community mobilisation. In Transforming Cities: Contested Governance and New Spatial Divisions; Jewson, N., MacGregor, S., Eds.; Routledge: London, UK, 1997; pp. 193–204. [Google Scholar]
- Byrow, Y.; Pajak, R.; McMahon, T.; Rajouria, A.; Nickerson, A. Barriers to Mental Health Help-Seeking amongst Refugee Men. Int. J. Environ. Res. Public Health 2019, 16, 2634. [Google Scholar] [CrossRef] [PubMed]
- Kiselev, N.; Pfaltz, M.; Haas, F.; Schick, M.; Kappen, M.; Sijbrandij, M.; De Graaff, A.M.; Bird, M.; Pernille Hansen, P.V. Structural and Socio-cultural Barriers to Accessing Mental Healthcare among Syrian Refugees and Asylum Seekers in Switzerland. Eur. J. Psychotraumatol. 2020, 11, 1717825. [Google Scholar] [CrossRef] [PubMed]
- Minas, H.; Kakuma, R.; Too, L.; Vayani, H.; Orapeleng, S.; Prasad-Ides, R.; Turner, G.; Procter, N.; Oehm, D. Mental health research and evaluation in multicultural Australia: Developing a culture of inclusion. Int. J. Ment. Health Syst. 2013, 7, 23. [Google Scholar] [CrossRef]
- Satinsky, E.; Fuhr, D.C.; Woodward, A.; Sondorp, E.; Roberts, B. Mental health care utilisation andaccess among refugees and asylum seekers in Europe: A systematic review. Health Policy 2019, 123, 851–863. [Google Scholar] [CrossRef]
- Slewa-Younan, S.; Mond, J.M.; Bussion, E.; Melkonian, M.; Mohammad, Y.; Dover, H.; Smith, M.; Milosevic, D.; Jorm, A.F. Psychological trauma and help seeking behaviour amongst resettled Iraqi refugees in attending English tuition classes in Australia. Int. J. Ment. Health Syst. 2015, 9, 5. [Google Scholar] [CrossRef]
- Maier, T.; Schmidt, M.; Mueller, J. Mental health and healthcare utilization in adult asylum seekers. Swiss Med. Wkly. 2010, 19, E1–E9. [Google Scholar] [CrossRef] [PubMed]
- Stuart, G.W.; Klimidis, S.; Minas, I.H. The treated prevalence of mental disorder amongst immigrants and the Australian-born: Community and primary-care rates. Int. J. Soc. Psychiatr. 1998, 44, 22–34. [Google Scholar] [CrossRef] [PubMed]
- Department of Health. Fourth National Mental Health Plan: An Agenda for Collaborative Government Action in Mental Health 2009–2014; Department of Health: Canberra, Australia, 2009.
- Henderson, S.; Kendall, E. Culturally and linguistically diverse peoples’ knowledge of accessibility and utilisation of health services: Exploring the need for improvement in health service delivery. Aust. J. Prim. Health 2011, 17, 195–201. [Google Scholar] [CrossRef]
- Slewa-Younan, S.; Mond, J.; Bussion, E.; Mohammad, Y.; Uribe Guajardo, M.G.; Smith, M.; Milosevic, D.; Lujic, S.; Jorm, A.F. Mental health literacy of resettled Iraqi refugees in Australia: Knowledge about posttraumatic stress disorder and beliefs about helpfulness of interventions. BMC Psychiatry 2014, 14, 320. [Google Scholar] [CrossRef]
- Wohler, Y.; Dantas, J.A. Barriers Accessing Mental Health Services among Culturally and Linguistically Diverse (CALD) Immigrant Women in Australia: Policy Implications. J. Immigr. Minority Health 2017, 19, 697–701. [Google Scholar] [CrossRef]
- Sullivan, C.; Vaughan, C.; Wright, J. Migrant and Refugee Women’s Mental Health in Australia: A Literature Review; School of Population and Global Health, University of Melbourne: Melbourne, Australia, 2020. [Google Scholar]
- United Nations Network on Migration. Enhancing Access to Services for Migrants in the Context of COVID-19 Preparedness, Prevention, and Response and Beyond; UNICEF: New York, NY, USA, 2021. [Google Scholar]
- Levesque, J.-F.; Harris, M.F.; Russell, G. Patient-centred access to health care: Conceptualising access at the interface of health systems and populations. Int. J. Equity Health 2013, 12, 18. [Google Scholar] [CrossRef] [PubMed]
- Rice, P.L.; Ezzy, D. Qualitative Research Method: A Health Focus; Oxford University Press: Melbourne, Australia, 2005. [Google Scholar]
- Allsop, J. Competing paradigms and health research: Design and process. In Researching Health, Qualitative, Quantitative and Mixed Methods; Saks, M., Allsop, J., Eds.; Sage: London, UK, 2013. [Google Scholar]
- Ritchie, J.; Spencer, L. Qualitative data analysis for applied policy research. In Analyzing Qualitative Data; Bryman, A., Burgess, R.G., Eds.; Routledge: London, UK, 1994; pp. 173–194. [Google Scholar]
- Moretti, F.; van Vliet, L.; Bensing, J.; Deledda, G.; Mazzi, M.; Rimondini, M.; Zimmermann, C.; Fletcher, I. A standardized approach to qualitative content analysis of focus group discussions from different countries. Patient Educ. Couns. 2011, 82, 420–428. [Google Scholar] [CrossRef]
- Mwanri, L.; Fauk, N.K.; Kustanti, C.Y.; Ambarwati, A.; Merry, M.S. HIV susceptibility among clients of female sex workers in Indonesia: A qualitative inquiry. Sex. Health 2018, 15, 246–253. [Google Scholar] [CrossRef]
- Basolo, V.; Strong, D. Understanding the neighbourhoods: From residents’ perceptions and needs to action. Hous. Policy Debate 2002, 13, 83–105. [Google Scholar] [CrossRef]
- Baum, F. (Ed.) The role of social capital in health promotion: Australian perspectives. In Proceedings of the 11th National Health Promotion Conference, Perth, WA, USA, 23–26 May 1999. [Google Scholar]
- Baum, F. The New Public Health: An Australian Perspective; Oxford University Press: Oxford, UK, 1998. [Google Scholar]
- Baum, F.; Palmer, C. ‘Opportunity structures’: Urban landscape, social capital and health promotion in Australia. Health Promot. Int. 2002, 17, 351–361. [Google Scholar] [CrossRef]
- Rintoul, A. Understanding the Mental Health and Wellbeing of Afghan Women in South East Melbourne; Monash University, Foundation House: Melbourne, Australia, 2010. [Google Scholar]
- Shafiei, T.; Flood, M.; Bee, J. Identifying the Perinatal Mental Health Needs of Immigrant and Refugee Women; Judith Lumley Centre, La Trobe University: Bendigo, Australia, 2018. [Google Scholar]
- Beaulieu, L.J.; Isreal, G.D. Strengthening social capital: The challenge for rural community sustainability. In Rural Sustainable Development in America; Audirac, I., Ed.; John Wiley and Sons, Inc.: New York, NY, USA, 1997; pp. 191–233. [Google Scholar]
- Baum, F. Social capital: Is it good for your health? Issues for a public health agenda. J. Epidemiol. Community Health 1999, 53, 195–196. [Google Scholar] [CrossRef][Green Version]
- Colucci, E.; Minas, H.; Szwarc, J.; Guerra, C.; Paxton, G. In or out? Barriers and facilitators to refugee background young people accessing mental health services. Transcult. Psychiatry 2015, 52, 766–790. [Google Scholar] [CrossRef]
- Goffman, E. Stigma: Notes on the management of spoiled identity. Simon and Schuster: New York, NY, USA, 2009. [Google Scholar]
- Russo, A.; Lewis, B.; Joyce, A.; Crockett, B.; Luchters, S. A qualitative exploration of the emotional wellbeing and support needs of new mothers from Afghanistan living in Melbourne, Australia. BMC Pregnancy Childb. 2015, 15, 197. [Google Scholar] [CrossRef] [PubMed]
- Valibhoy, M.C.; Kaplan, I.; Szwarc, J. “It comes down to just how human someone can be”: A qualitative study with young people from refugee backgrounds about their experiences of Australian mental health services. Transcult. Psychiatry 2017, 54, 23–45. [Google Scholar] [CrossRef] [PubMed]
- Yaser, A.; Slewa-Younan, S.; Smith, C.A.; Olson, R.E.; Guajardo, M.G.U.; Mond, J. Beliefs and knowledge about post-traumatic stress disorder amongst resettled afghan refugees in Australia. Int. J. Ment. Health Syst. 2016, 10, 31. [Google Scholar] [CrossRef] [PubMed]
| African Migrants | |
|---|---|
| Characteristics | N = 20 (%) |
| Age ≤30 31–40 41–50 51–60 | 4 (20) 4 (20) 6 (30) 6 (30) |
| Country of Origin The Democratic Republic of Congo South Sudan Liberia Sierra Leone Burundi Ethiopia Kenya Somalia | 5 (25) 4 (20) 3 (15) 3 (15) 2 (10) 1 (5) 1 (5) 1 (5) |
| Employment status Employed Unemployed Student | 11 (55) 7 (35) 2 (10) |
| Duration of Living in Australia (year) 1–5 6–10 11–15 16–20 | 5 (25) 2 (10) 8 (40) 5 (25) |
| Service providers | |
| Role | N = 10 (%) |
| Counsellor | 2 (10) |
| Clinical services manager | 1 (5) |
| Community development officer | 1 (5) |
| Refugee support program worker | 1 (5) |
| Mental health and well-being manager | 1 (5) |
| Mental health worker | 1 (5) |
| African family support worker | 1 (5) |
| Settlement engagement and support managers | 2 (10) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fauk, N.K.; Ziersch, A.; Gesesew, H.; Ward, P.; Green, E.; Oudih, E.; Tahir, R.; Mwanri, L. Migrants and Service Providers’ Perspectives of Barriers to Accessing Mental Health Services in South Australia: A Case of African Migrants with a Refugee Background in South Australia. Int. J. Environ. Res. Public Health 2021, 18, 8906. https://doi.org/10.3390/ijerph18178906
Fauk NK, Ziersch A, Gesesew H, Ward P, Green E, Oudih E, Tahir R, Mwanri L. Migrants and Service Providers’ Perspectives of Barriers to Accessing Mental Health Services in South Australia: A Case of African Migrants with a Refugee Background in South Australia. International Journal of Environmental Research and Public Health. 2021; 18(17):8906. https://doi.org/10.3390/ijerph18178906
Chicago/Turabian StyleFauk, Nelsensius Klau, Anna Ziersch, Hailay Gesesew, Paul Ward, Erin Green, Enaam Oudih, Roheena Tahir, and Lillian Mwanri. 2021. "Migrants and Service Providers’ Perspectives of Barriers to Accessing Mental Health Services in South Australia: A Case of African Migrants with a Refugee Background in South Australia" International Journal of Environmental Research and Public Health 18, no. 17: 8906. https://doi.org/10.3390/ijerph18178906
APA StyleFauk, N. K., Ziersch, A., Gesesew, H., Ward, P., Green, E., Oudih, E., Tahir, R., & Mwanri, L. (2021). Migrants and Service Providers’ Perspectives of Barriers to Accessing Mental Health Services in South Australia: A Case of African Migrants with a Refugee Background in South Australia. International Journal of Environmental Research and Public Health, 18(17), 8906. https://doi.org/10.3390/ijerph18178906







