Effects of Respiratory Disorders on Smoking Cessation and Re-Initiation in an Italian Cohort Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Assessment of Smoking Habits
2.3. Assessment of Respiratory Disorders
2.4. Statistical Analyses
3. Results
3.1. Response to Follow-Up
3.2. Changes in Smoking Habits
3.3. Possible Selection Bias in Participation to the Follow-Up
3.4. Determinants of Smoking Cessation
3.5. Determinants of Smoking Re-Initiation
4. Discussion
- The smoking intensity and cumulative smoke exposure were inversely related to smoking cessation, which represented its most important predictors in agreement with the current literature [12,17,18]. On the opposite side, the duration of smoking abstinence was inversely related to smoking re-initiation and was the most important predictor according to the current literature [19,20,21].
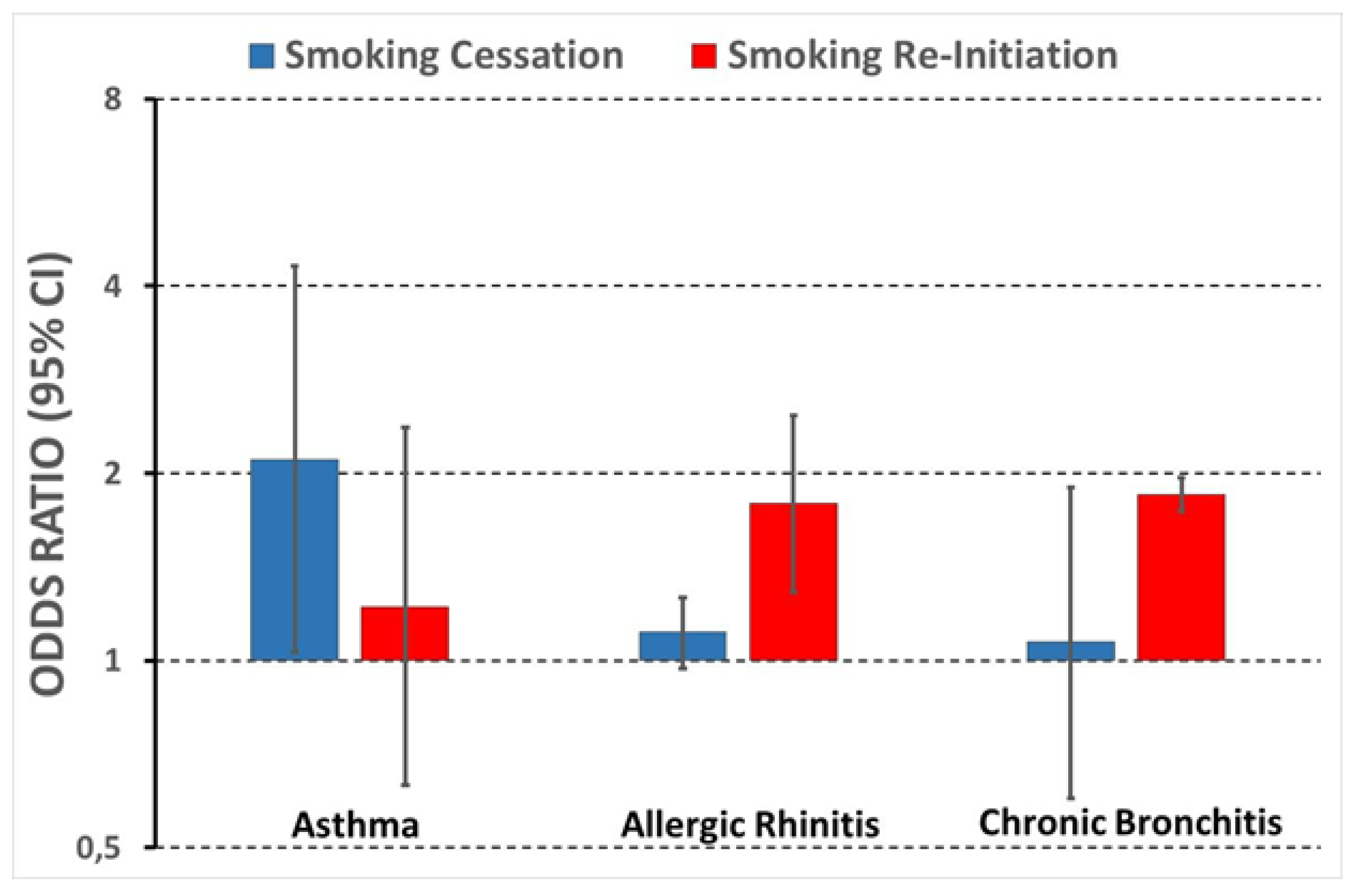
- As regards respiratory disorders, the probability to quit smoking was affected neither by allergic rhinitis nor chronic cough/phlegm, while being doubled by current asthma. Conversely, the risk to re-start smoking increased almost twice in people with allergic rhinitis or chronic cough/phlegm, while being unaffected by asthma. Chronic cough/phlegm seemed to blunt the decrease in smoking resumption associated with longer abstinence duration.
- People aged 20–31 years old had a higher probability to quit smoking than older people which, however, was partly counterbalanced by a much higher probability to resume smoking.
4.1. Determinants of Smoking Cessation
4.2. Determinants of Smoking Re-Initiation
4.3. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Availability of Data and Materials
Ethics Approval and Consent to Participate
Consent for Publication
Abbreviations
References
- WHO Report on the Global Tobacco Epidemic, 2017: Monitoring Tobacco Use and Prevention Policies; World Health Organization: Geneva, Switzerland, 2017.
- World Health Organization. Who Global Report on Trends in Prevalence of Tobacco Smoking 2000–2025, 2nd ed.; World Health Organization: Geneva, Switzerland, 2018; 121p. [Google Scholar]
- Sun, R.; Mendez, D. Finding the optimal mix of smoking initiation and cessation interventions to reduce smoking prevalence. PLoS ONE 2019, 14, e0212838. [Google Scholar] [CrossRef]
- Castro, Y.; Cano, M.A.; Businelle, M.S.; Correa-Fernandez, V.; Wetter, D.W. A cross-lagged analysis of five intrapersonal determinants of smoking abstinence. Drug Alcohol Depend. 2014, 140, e29. [Google Scholar] [CrossRef]
- Kong, G.; Camenga, D.; Krishnan-Sarin, S. Parental influence on adolescent smoking cessation: Is there a gender difference? Addict. Behav. 2012, 37, 211–216. [Google Scholar] [CrossRef][Green Version]
- Jackson, S.E.; Steptoe, A.; Wardle, J. The influence of Partner’s behavior on health behavior change: The English longitudinal study of Ageing. JAMA Intern. Med. 2015, 175, 385–392. [Google Scholar] [CrossRef]
- Filippidis, F.T.; Gerovasili, V.; Vardavas, C.I.; Agaku, I.T.; Tountas, Y. Determinants of use of smoking cessation aids in 27 European countries. Prev. Med. 2014, 65, 99–102. [Google Scholar] [CrossRef]
- Gallus, S.; Muttarak, R.; Franchi, M.; Pacifici, R.; Colombo, P.; Boffetta, P.; Leon, M.E.; La Vecchia, C. Why do smokers quit? Eur. J. Cancer Prev. 2013, 22, 96–101. [Google Scholar] [CrossRef]
- Smedberg, J.; Lupattelli, A.; Mårdby, A.C.; Nordeng, H. Characteristics of women who continue smoking during pregnancy: A cross-sectional study of pregnant women and new mothers in 15 European countries. BMC Pregnancy Childbirth 2014, 14, 213. [Google Scholar] [CrossRef]
- Stegberg, M.; Hasselgren, M.; Montgomery, S.; Lisspers, K.; Ställberg, B.; Janson, C.; Sundh, J. Changes in smoking prevalence and cessation support, and factors associated with successful smoking cessation in Swedish patients with asthma and COPD. Eur. Clin. Respir. J. 2018, 5, 1421389. [Google Scholar] [CrossRef]
- Holm, M.; Schiöler, L.; Andersson, E.; Forsberg, B.; Gislason, T.; Janson, C.; Jogi, R.; Schlünssen, V.; Svanes, C.; Torén, K. Predictors of smoking cessation: A longitudinal study in a large cohort of smokers. Respir. Med. 2017, 132, 164–169. [Google Scholar] [CrossRef]
- Bush, T.; Zbikowski, S.M.; Mahoney, L.; Deprey, M.; Mowery, P.; Cerutti, B. State quitlines and cessation patterns among adults with selected chronic diseases in 15 states, 2005–2008. Prev. Chronic Dis. 2012, 9, E163. [Google Scholar] [CrossRef]
- Hylkema, M.N.; Sterk, P.J.; De Boer, W.I.; Postma, D.S. Tobacco use in relation to COPD and asthma. Eur. Respir. J. 2007, 29, 438–445. [Google Scholar] [CrossRef]
- Jankowski, M.; Lawson, J.A.; Shpakou, A.; Poznański, M.; Zielonka, T.M.; Klimatckaia, L.; Loginovich, Y.; Rachel, M.; Gereová, J.; Minarowski, Ł.; et al. Smoking cessation and vaping cessation attempts among cigarette smokers and E-cigarette users in Central and Eastern Europe. Int. J. Environ. Res. Public Health 2020, 17, 28. [Google Scholar] [CrossRef]
- Hilberink, S.R.; Jacobs, J.E.; Schlösser, M.; Grol, R.P.T.M.; De Vries, H. Characteristics of patients with COPD in three motivational stages related to smoking cessation. Patient Educ. Couns. 2006, 61, 449–457. [Google Scholar] [CrossRef]
- Melzer, A.C.; Feemster, L.C.; Crothers, K.; Carson, S.S.; Gillespie, S.E.; Henderson, A.G.; Krishnan, J.A.; Lindenauer, P.K.; McBurnie, M.A.; Mularski, R.A.; et al. Respiratory and bronchitic symptoms predict intention to quit smoking among current smokers with, and at risk for, chronic obstructive pulmonary disease. Ann. Am. Thorac. Soc. 2016, 13, 1490–1496. [Google Scholar] [CrossRef]
- Masaoka, H.; Gallus, S.; Ito, H.; Watanabe, M.; Yokomizo, A.; Eto, M.; Matsuo, K. Aldehyde dehydrogenase 2 polymorphism is a predictor of smoking cessation. Nicotine Tob. Res. 2017, 19, 1087–1094. [Google Scholar] [CrossRef]
- Jeong Yang, J.; Song, M.; Yoon, H.S.; Lee, H.W.; Lee, Y.; Lee, S.A.; Choi, J.Y.; Lee, J.K.; Kang, D. What are the major determinants in the success of smoking cessation: Results from the health examinees study. PLoS ONE 2015, 10, e0143303. [Google Scholar]
- García-Rodríguez, O.; Secades-Villa, R.; Flórez-Salamanca, L.; Okuda, M.; Liu, S.M.; Blanco, C. Probability and predictors of relapse to smoking: Results of the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC). Drug Alcohol Depend. 2013, 132, 479–485. [Google Scholar] [CrossRef]
- Wetter, D.W.; Cofta-Gunn, L.; Fouladi, R.T.; Cinciripini, P.M.; Sui, D.; Gritz, E.R. Late relapse/sustained abstinence among former smokers: A longitudinal study. Prev. Med. 2004, 39, 1156–1163. [Google Scholar] [CrossRef]
- Herd, N.; Borland, R.; Hyland, A. Predictors of smoking relapse by duration of abstinence: Findings from the International Tobacco control (ITC) four country survey. Addiction 2009, 104, 2088–2099. [Google Scholar] [CrossRef]
- Gökbayrak, N.S.; Paiva, A.L.; Blissmer, B.J.; Prochaska, J.O. Predictors of relapse among smokers: Transtheoretical effort variables, demographics, and smoking severity. Addict. Behav. 2015, 42, 176–179. [Google Scholar] [CrossRef]
- Caraballo, R.S.; Kruger, J.; Asman, K.; Pederson, L.; Widome, R.; Kiefe, C.I.; Hitsman, B.; Jacobs, D.R. Relapse among Cigarette Smokers: The CARDIA longitudinal study—1985–2011. Addict. Behav. 2014, 39, 101–106. [Google Scholar] [CrossRef]
- Kukkamalla, M.A.; Pentapati, K.C.; Suresh, G.; Goyal, R.; Cornelio, S.M. Smoking re-initiation after cessation program: Comparison of associated factors between young and older adults. J. Nat. Sci. Biol. Med. 2013, 4, 440. [Google Scholar]
- Piñeiro, B.; López-Durán, A.; Martínez-Vispo, C.; Fernández del Río, E.; Martínez, Ú.; Rodríguez-Cano, R.; Míguez, M.C.; Becoña, E. Smoking relapse situations among a community-recruited sample of Spanish daily smokers. Addict. Behav. 2017, 75, 152–158. [Google Scholar] [CrossRef]
- Blok, D.J.; De Vlas, S.J.; Van Empelen, P.; Van Lenthe, F.J. The role of smoking in social networks on smoking cessation and relapse among adults: A longitudinal study. Prev. Med. 2017, 99, 105–110. [Google Scholar] [CrossRef]
- Moore, S.; Teixeira, A.; Stewart, S. Effect of network social capital on the chances of smoking relapse: A two-year follow-up study of urban-dwelling adults. Am. J. Public Health 2014, 104, e72–e76. [Google Scholar] [CrossRef]
- Hajek, P.; Stead, L.F.; West, R.; Jarvis, M.; Hartmann-Boyce, J.; Lancaster, T. Relapse prevention interventions for smoking cessation. Cochrane Database Syst. Rev. 2013. [Google Scholar] [CrossRef]
- Caponnetto, P.; Polosa, R. Are we addressing relevant determinants of smoking cessation? Eur. Respir. J. 2017, 50, 1701615. [Google Scholar] [CrossRef]
- Verlato, G.; Nguyen, G.; Marchetti, P.; Accordini, S.; Marcon, A.; Marconcini, R.; Bono, R.; Fois, A.; Pirina, P.; De Marco, R. Smoking and new-onset asthma in a prospective study on Italian adults. Int. Arch. Allergy Immunol. 2016, 170, 149–157. [Google Scholar] [CrossRef]
- Verlato, G.; Melotti, R.; Corsico, A.G.; Bugiani, M.; Carrozzi, L.; Marinoni, A.; Dallari, R.; Pirina, P.; Struzzo, P.; Olivieri, M.; et al. Time trends in smoking habits among Italian young adults. Respir. Med. 2006, 100, 2197–2206. [Google Scholar] [CrossRef][Green Version]
- Verlato, G.; Corsico, A.; Villani, S.; Cerveri, I.; Migliore, E.; Accordini, S.; Carolei, A.; Piccioni, P.; Bugiani, M.; Cascio, V.L. Is the prevalence of adult asthma and allergic rhinitis still increasing? Results of an Italian study. J. Allergy Clin. Immunol. 2003, 111, 1232–1238. [Google Scholar] [CrossRef]
- De Marco, R.; Zanolin, M.E.; Accordini, S.; Signorelli, D.; Marinoni, A.; Bugiani, M.; Cascio, V.; Woods, R.; Burn, P. A new questionnaire for the repeat of the first stage of the European Community Respiratory Health Survey: A pilot study. Eur. Respir. J. 1999, 14, 1044–1048. [Google Scholar] [CrossRef]
- De Marco, R.; Accordini, S.; Antonicelli, L.; Bellia, V.; Bettin, M.D.; Bombieri, C.; Bonifazi, F.; Bugiani, M.; Carosso, A.; Casali, L.; et al. The gene-environment interactions in respiratory diseases (GEIRD) project for the GEIRD study group. Int. Arch. Allergy Immunol. 2010, 152, 255–263. [Google Scholar] [CrossRef]
- Olivieri, M.; Poli, A.; Marco RDe Zuccaro, P.; Ferrari, M.; Lampronti, G.; De Marco, R.; Cascio, V.L.; Pacifici, R. Tobacco Smoke Exposure and Serum Cotinine in a Random Sample of Adults Living in Verona, Italy. Arch. Environ. Health 2002, 57, 355–359. [Google Scholar] [CrossRef]
- Compalati, E.; Ridolo, E.; Passalacqua, G.; Braido, F.; Villa, E.; Canonica, G.W. The link between allergic rhinitis and asthma: The united airways disease. Expert Rev. Clin. Immunol. 2010, 6, 413–423. [Google Scholar] [CrossRef]
- Hosmer, D.W.; Lemeshow, S.; Sturdivant, R.X. Applied Logistic Regression, 3rd ed.; John Wiley & Sons: Hoboken, NJ, USA, 2013. [Google Scholar]
- Coppo, A.; Baldissera, S.; Migliardi, A.; Minardi, V.; Quarchioni, E.; Ferrante, G.; Dal Molin, A.; Faggiano, F.; PASSI Working Group. Quit attempts and smoking cessation in Italian adults (25–64 years): Factors associated with attempts and successes. Eur. J. Public Health 2017, 27, 717–722. [Google Scholar] [CrossRef][Green Version]
- Samim, D.; Méan, M.; Clair, C.; Marques-Vidal, P. A 10-year observational study on the trends and determinants of smoking status. PLoS ONE 2018, 13, e0200010. [Google Scholar] [CrossRef]
- Pesce, G.; Marcon, A.; Calciano, L.; Perret, J.L.; Abramson, M.J.; Bono, R.; Bousquet, J.; Fois, A.G.; Janson, C.; Jarvis, D.; et al. Time and age trends in smoking cessation in Europe. PLoS ONE 2019, 14, e0211976. [Google Scholar] [CrossRef]
- Verlato, G.; Melotti, R.; Olivieri, M.; Corsico, A.; Bugiani, M.; Accordini, S.; Villani, S.; Migliore, E.; Marinoni, A.; Pirina, P.; et al. Asthmatics and ex-smokers respond early, heavy smokers respond late to mailed surveys in Italy. Respir. Med. 2010, 104, 172–179. [Google Scholar] [CrossRef]
- Johannessen, A.; Verlato, G.; Benediktsdottir, B.; Forsberg, B.; Franklin, K.; Gislason, T.; Villani, S.; Migliore, E.; Marinoni, A.; Pirina, P.; et al. Longterm follow-up in European respiratory health studies—patterns and implications. BMC Pulm. Med. 2014, 14, 63. [Google Scholar] [CrossRef]
- Everard, C.D.; Silveira, M.L.; Kimmel, H.L.; Marshall, D.; Blanco, C.; Compton, W.M. Association of Electronic Nicotine Delivery System Use With Cigarette Smoking Relapse Among Former Smokers in the United States. JAMA Netw. Open 2020, 3, e204813. [Google Scholar] [CrossRef]
| Baseline | Smokers | Baseline | Ex-Smokers | |||
|---|---|---|---|---|---|---|
| Responders 965 (51.5%) | Non-Responders 909 (48.5%) | p-Value | Responders 735 (63%) | Non-Responders 431 (37%) | p-Value | |
| Centre | <0.001 | <0.001 | ||||
| Verona–ISIA | 305 (66.3) | 155 (33.7) | 323 (77.8) | 92 (22.2) | ||
| Verona–ISAYA | 412 (59.2) | 284 (40.8) | 276 (64.6) | 151 (35.4) | ||
| Sassari–ISAYA | 248 (34.5) | 470 (65.5) | 136 (42.0) | 188 (58.0) | ||
| Sex | <0.001 | 0.058 | ||||
| Men | 519 (48.1) | 561 (51.9) | 379 (60.5) | 247 (39.5) | ||
| Women | 446 (56.2) | 348 (43.8) | 356 (65.9) | 184 (34.1) | ||
| Age class (years) | <0.001 | <0.001 | ||||
| 20–31.2 | 313 (47.9) | 340 (52.1) | 122 (49.4) | 125 (50.6) | ||
| 31.3–42.5 | 374 (50.1) | 373 (49.9) | 390 (63.6) | 223 (36.4) | ||
| 42.6–53.9 | 278 (58.6) | 196 (41.4) | 222 (72.8) | 83 (27.2) | ||
| Occupation | <0.001 | <0.001 | ||||
| Businessman | 142 (50.5) | 139 (49.5) | 116 (60.4) | 76 (39.6) | ||
| Clerk | 324 (56.2) | 253 (43.8) | 255 (65.1) | 137 (34.9) | ||
| Workman | 187 (52.4) | 170 (47.6) | 141 (71.6) | 56 (28.4) | ||
| Unemployed | 48 (33.6) | 95 (66.4) | 17 (34) | 33 (66) | ||
| Housewife | 88 (55.3) | 71 (44.7) | 90 (67.7) | 43 (32.3) | ||
| Student | 82 (48.0) | 89 (52.0) | 21 (42.9) | 28 (57.1) | ||
| Others | 89 (50.3) | 88 (49.7) | 93 (62.4) | 56 (37.6) | ||
| Nasal allergies | 0.625 | 0.884 | ||||
| No | 790 (51.8) | 734 (48.2) | 563 (62.7) | 335 (37.3) | ||
| Yes | 163 (50.3) | 161 (49.7) | 162 (63.3) | 94 (36.7) | ||
| Asthma | 0.092 | 0.236 | ||||
| No | 923 (51.8) | 858 (48.2) | 668 (62.3) | 405 (37.7) | ||
| Yes | 35 (42.2) | 48 (57.8) | 57 (69.5) | 25 (30.5) | ||
| Chronic bronchitis | 0.033 | 0.182 | ||||
| No | 772 (52.8) | 690 (47.2) | 634 (63.5) | 364 (36.5) | ||
| Yes | 178 (46.6) | 204 (53.4) | 82 (57.7) | 60 (42.3) | ||
| Cigarette smoked daily | 10 (7–20) | 15 (10–20) | <0.001 | 10 (6–20) | 10 (6–20) | 0.557 |
| Age at smoking initiation | 17 (15–19) | 17 (15–18) | 0.380 | ---- | ---- | ---- |
| Pack-years | 9.0 (4.1–18.1) | 9.4 (4.5–17.0) | 0.737 | 12.6 (6.3–21) | 15.1 (5.1–27.7) | 0.872 |
| Abstinence years | ----- | ----- | ----- | 8.4 (3.1–13.9) | 6.5 (2.3–11.3) | 0.002 |
| Current Smokers at Baseline | Smoking Quitters (per cent) | p-Value | |
|---|---|---|---|
| Centre | 0.008 | ||
| Verona-ISIA | 305 | 78 (25.6) | |
| Verona-ISAYA | 412 | 149 (36.2) | |
| Sassari-ISAYA | 248 | 85 (34.3) | |
| Sex | 0.129 | ||
| Male | 519 | 179 (34.5) | |
| Female | 446 | 133 (29.8) | |
| Age class (years old) | <0.001 | ||
| 20–31.2 | 361 | 144 (39.9) | |
| 31.3–42.5 | 412 | 118 (28.6) | |
| 42.6–53.9 | 192 | 50 (26.0) | |
| Occupation | 0.009 | ||
| Businessman | 142 | 46 (32.4) | |
| Clerk | 324 | 107 (33.0) | |
| Workman | 187 | 64 (34.2) | |
| Unemployed | 48 | 15 (31.2) | |
| Housewife | 88 | 22 (25) | |
| Student | 82 | 39 (47.6) | |
| Retired and others | 89 | 18 (20.2) | |
| Allergic rhinitis | 0.097 | ||
| No | 790 | 245 (31.0) | |
| Yes | 163 | 62 (38.0) | |
| Asthma | 0.043 | ||
| No | 923 | 293 (31.7) | |
| Yes | 35 | 17 (48.6) | |
| Chronic bronchitis | 0.510 | ||
| No | 772 | 254 (32.9) | |
| Yes | 178 | 54 (30.3) | |
| Cigarettes smoked daily | <0.001 | ||
| 1–5 | 195 | 71 (36.4) | |
| 6–10 | 295 | 114 (38.6) | |
| 11–15 | 182 | 48 (26.4) | |
| 16–40 | 263 | 56 (21.3) | |
| Age of smoking initiation | 0.860 | ||
| 8–15 years old | 252 | 73 (29.0) | |
| 16–17 years old | 262 | 73 (27.9) | |
| 18–19 years old | 207 | 58 (28.0) | |
| >20 years old | 185 | 58 (31.4) | |
| Pack-years | <0.001 | ||
| <5 | 272 | 99 (36.4) | |
| (5–10) | 211 | 69 (32.7) | |
| (10–15) | 141 | 42 (29.8) | |
| (15–80) | 274 | 50 (18.2) |
| OR (95% CI) | p-Value | |
|---|---|---|
| Centre | ||
| Verona-ISIA | 1 | |
| Verona-ISAYA | 1.56 (1.42–1.72) | <0.001 |
| Sassari-ISAYA | 1.24 (1.13–1.36) | <0.001 |
| Sex (women vs. men) | 0.70 (0.54–0.91) | 0.009 |
| Age class (years old) | ||
| 20–31.2 | 1 | |
| 31.3–42.5 | 0.83 (0.72–0.95) | 0.006 |
| 40.6–53.9 | 0.89 (0.65–1.21) | 0.444 |
| Asthma (Yes vs. No) | 2.10 (1.03–4.31) | 0.042 |
| Cigarettes smoked daily | ||
| 1–5 | 1 | |
| 6–10 | 1.24 (0.78–1.98) | 0.352 |
| 11–15 | 0.70 (0.44–1.11) | 0.130 |
| 16–40 | 0.55 (0.33–0.92) | 0.022 |
| Age of smoking initiation | ||
| 8–15 | 1 | |
| 16–17 | 0.87 (0.70–1.07) | 0.176 |
| 18–19 | 0.83 (0.53–1.30) | 0.408 |
| >20 | 1.05 (0.88–1.25) | 0.578 |
| Ex-Smokers at Baseline | People Who Resumed Smoking (per cent) | p-Value | |
|---|---|---|---|
| Centre | 0.087 | ||
| Verona-ISIA | 323 | 31 (9.6) | |
| Verona-ISAYA | 276 | 32 (11.6) | |
| Sassari-ISAYA | 136 | 23 (16.9) | |
| Sex | 0.819 | ||
| Male | 379 | 43 (11.3) | |
| Female | 356 | 43 (12.1) | |
| Age class (years old) | <0.001 | ||
| 20–31.2 | 122 | 22 (18) | |
| 31.3–42.5 | 390 | 52 (13.3) | |
| 42.6–53.9 | 222 | 12 (5.4) | |
| Occupation | 0.222 | ||
| Businessman | 116 | 17 (14.7) | |
| Clerk | 255 | 28 (11) | |
| Workman | 141 | 17 (12.1) | |
| Unemployed | 17 | 5 (29.4) | |
| Housewife | 90 | 9 (10) | |
| Student | 21 | 3 (14.3) | |
| Retired and others | 93 | 7 (7.53) | |
| Allergic rhinitis | 0.038 | ||
| No | 563 | 59 (10.5) | |
| Yes | 162 | 27 (16.7) | |
| Asthma | 0.528 | ||
| No | 688 | 78 (11.7) | |
| Yes | 57 | 8 (14) | |
| Chronic bronchitis | 0.006 | ||
| No | 634 | 66 (10.4) | |
| Yes | 82 | 17 (20.7) | |
| Cigarettes smoked daily | 0.902 | ||
| 1–5 | 148 | 11 (7.43) | |
| 6–10 | 216 | 39 (18.1) | |
| 11–15 | 117 | 10 (8.5) | |
| 16–40 | 187 | 23 (12.3) | |
| Age of smoking initiation | 0.477 | ||
| 1–15 years old | 225 | 28 (12.4) | |
| 16–17 years old | 195 | 19 (9.7) | |
| 18–19 years old | 156 | 23 (14.7) | |
| >20 years old | 105 | 15 (14.3) | |
| Pack-years | 0.087 | ||
| <5 | 170 | 27 (15.9) | |
| 5–9 | 87 | 25 (28.7) | |
| 10–14 | 58 | 15 (25.9) | |
| 15–80 | 56 | 12 (21.4) | |
| Abstinence duration (years) | <0.001 | ||
| <3 years | 153 | 42 (27.5) | |
| 3–7.4 years | 140 | 20 (14.3) | |
| 7.5–13.4 years | 167 | 13 (7.8) | |
| >13.5 years | 169 | 6 (3.6) |
| OR (95% CI) | p-Value | |
|---|---|---|
| Centre | ||
| Verona-ISIA | 1 | |
| Verona-ISAYA | 0.86 (0.80–0.91) | <0.001 |
| Sassari-ISAYA | 1.08 (0.97–1.20) | 0.170 |
| Sex (women vs. men) | 1.18 (0.77–1.79) | 0.448 |
| Age class (years old) | ||
| 20–31.2 | 1 | |
| 31.3–42.5 | 0.99 (0.57–1.71) | 0.961 |
| 42.6–53.9 | 0.34 (0.22–0.54) | <0.001 |
| Asthma (Yes vs. No) | 1.22 (0.63–2.37) | 0.559 |
| Cigarettes smoked daily | ||
| 1–5 | 1 | |
| 6–10 | 3.19 (2.01–5.07) | <0.001 |
| 11–15 | 1.26 (0.58–2.73) | 0.550 |
| 16–40 | 2.41 (1.41–4.14) | <0.001 |
| Abstinence duration (years) | ||
| <3 years | 1 | |
| 3–7.4 years | 0.46 (0.34–0.63) | <0.001 |
| 7.5–13.4 years | 0.23 (0.18–0.29) | <0.001 |
| >13.5 years | 0.15 (0.06–0.36) | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Finocchio, E.; Olivieri, M.; Nguyen, G.; Bortolami, O.; Marchetti, P.; Vesentini, R.; Torroni, L.; Spiteri, G.; Locatelli, F.; Moretti, F.; et al. Effects of Respiratory Disorders on Smoking Cessation and Re-Initiation in an Italian Cohort Study. Int. J. Environ. Res. Public Health 2021, 18, 903. https://doi.org/10.3390/ijerph18030903
Finocchio E, Olivieri M, Nguyen G, Bortolami O, Marchetti P, Vesentini R, Torroni L, Spiteri G, Locatelli F, Moretti F, et al. Effects of Respiratory Disorders on Smoking Cessation and Re-Initiation in an Italian Cohort Study. International Journal of Environmental Research and Public Health. 2021; 18(3):903. https://doi.org/10.3390/ijerph18030903
Chicago/Turabian StyleFinocchio, Eliana, Mario Olivieri, Giang Nguyen, Oscar Bortolami, Pierpaolo Marchetti, Roberta Vesentini, Lorena Torroni, Gianluca Spiteri, Francesca Locatelli, Francesca Moretti, and et al. 2021. "Effects of Respiratory Disorders on Smoking Cessation and Re-Initiation in an Italian Cohort Study" International Journal of Environmental Research and Public Health 18, no. 3: 903. https://doi.org/10.3390/ijerph18030903
APA StyleFinocchio, E., Olivieri, M., Nguyen, G., Bortolami, O., Marchetti, P., Vesentini, R., Torroni, L., Spiteri, G., Locatelli, F., Moretti, F., Fois, A., Pirina, P., Ferrari, M., & Verlato, G. (2021). Effects of Respiratory Disorders on Smoking Cessation and Re-Initiation in an Italian Cohort Study. International Journal of Environmental Research and Public Health, 18(3), 903. https://doi.org/10.3390/ijerph18030903








