Association of Allergic Diseases and Related Conditions with Dietary Fiber Intake in Korean Adults
Abstract
:1. Introduction
2. Materials and Methods
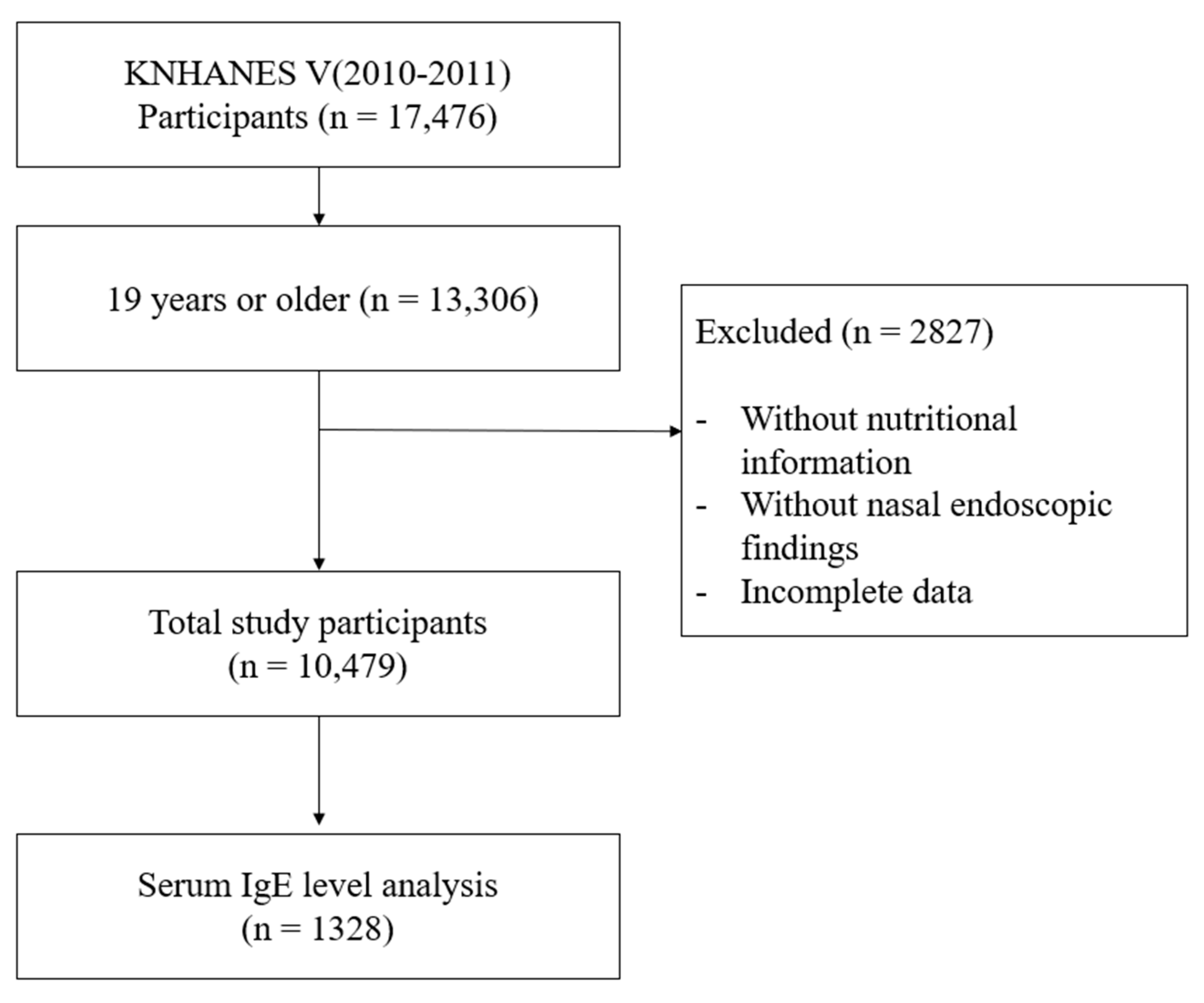
2.1. Study Population
2.2. Diagnosis of Allergic Diseases and Assessment of Related Conditions
2.3. Assessment of Daily Nutritional Intake
2.4. Assessment of Other Variables
2.5. Statistical Analysis
3. Results
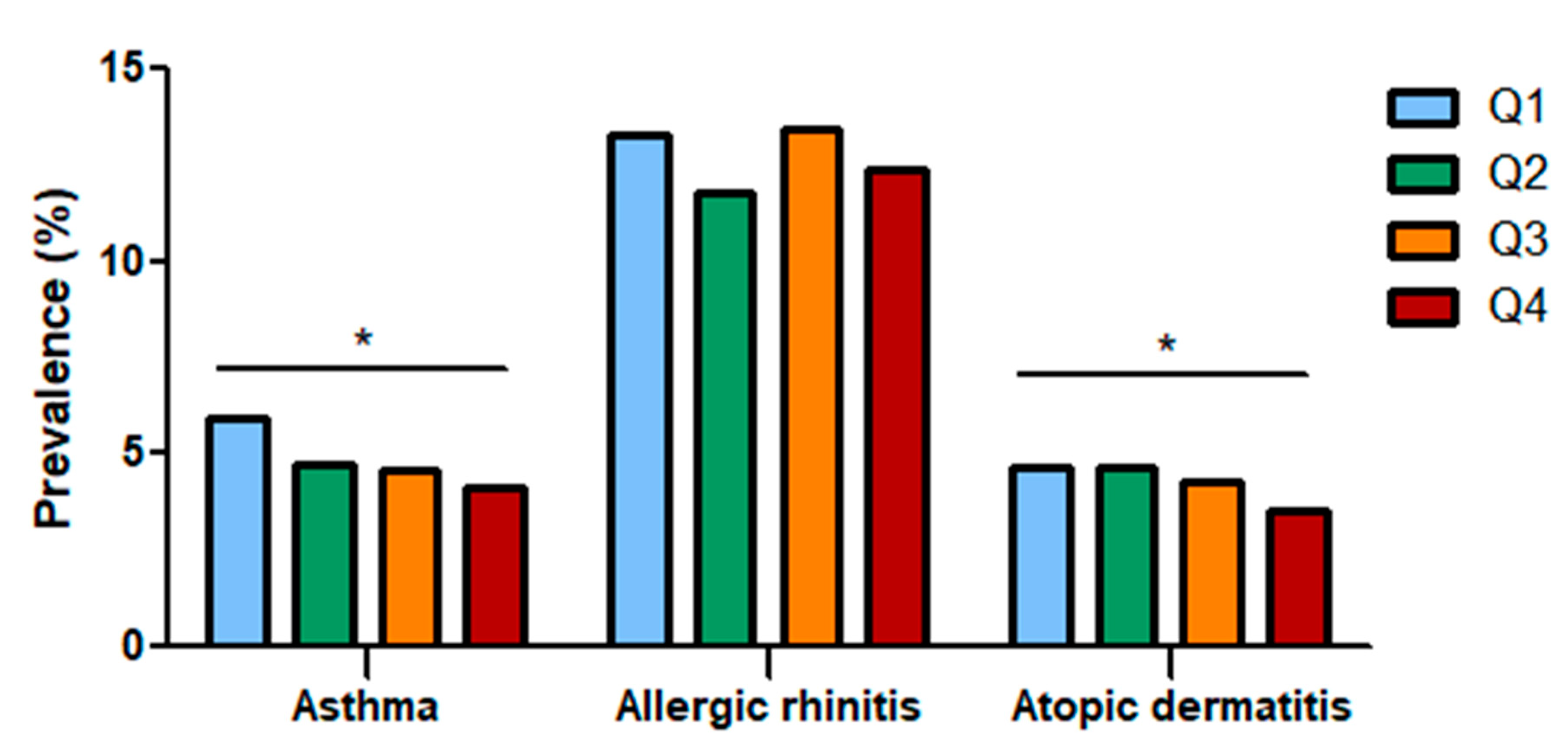
3.1. Association between Fiber Intake and Allergic Diseases
3.2. Association between Fiber Intake and Allergic Diseases with Respect to Sex
3.3. Association between Fiber Intake and Asthma-Related Conditions
3.4. Association between Fiber Intake and Allergic Rhinitis-Related Conditions
3.5. Association between Fiber Intake and Serum IgE Level
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Hipsley, E.H. Dietary “fibre” and pregnancy toxaemia. Br. Med. J. 1953, 2, 420–422. [Google Scholar] [CrossRef]
- Chutkan, R.; Fahey, G.; Wright, W.L.; McRorie, J. Viscous versus nonviscous soluble fiber supplements: Mechanisms and evidence for fiber-specific health benefits. J. Am. Acad. Nurse. Pract. 2012, 24, 476–487. [Google Scholar] [CrossRef]
- Soliman, G.A. Dietary fiber, atherosclerosis, and cardiovascular disease. Nutrients 2019, 11, 1155. [Google Scholar] [CrossRef] [Green Version]
- Dehghan, M.; Mente, A.; Rangarajan, S.; Sheridan, P.; Mohan, V.; Iqbal, R.; Gupta, R.; Lear, S.; Wentzl-Viljoen, E.; Avezum, A.; et al. Association of dairy intake with cardiovascular disease and mortality in 21 countries from five continents (PURE): A prospective cohort study. Lancet 2018, 392, 2288–2297. [Google Scholar] [CrossRef]
- Sun, J.; Buys, N. Effects of probiotics consumption on lowering lipids and CVD risk factors: A systematic review and meta-analysis of randomized controlled trials. Ann. Med. 2015, 47, 430–440. [Google Scholar] [CrossRef] [PubMed]
- Weickert, M.O.; Pfeiffer, A.F.H. Impact of dietary fiber consumption on insulin resistance and the prevention of type 2 diabetes. J. Nutr. 2018, 148, 7–12. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- El-Salhy, M.; Ystad, S.O.; Mazzawi, T.; Gundersen, D. Dietary fiber in irritable bowel syndrome (Review). Int. J. Mol. Med. 2017, 40, 607–613. [Google Scholar] [CrossRef] [Green Version]
- Ramkumar, D.; Rao, S.S. Efficacy and safety of traditional medical therapies for chronic constipation: Systematic review. Am. J. Gastroenterol. 2005, 100, 936–971. [Google Scholar] [CrossRef]
- Kaluza, J.; Harris, H.; Wallin, A.; Linden, A.; Wolk, A. Dietary fiber intake and risk of chronic obstructive pulmonary disease: A prospective cohort study of men. Epidemiology 2018, 29, 254–260. [Google Scholar] [CrossRef]
- Aune, D.; Chan, D.S.; Lau, R.; Vieira, R.; Greenwood, D.C.; Kampman, E.; Norat, T. Dietary fibre, whole grains, and risk of colorectal cancer: Systematic review and dose-response meta-analysis of prospective studies. BMJ 2011, 343, d6617. [Google Scholar] [CrossRef] [Green Version]
- Yang, J.J.; Yu, D.; Xiang, Y.B.; Blot, W.; White, E.; Robien, K.; Sinha, R.; Park, Y.; Takata, Y.; Lazovich, D.; et al. Association of dietary fiber and yogurt consumption with lung cancer risk: A pooled analysis. JAMA Oncol. 2020, 6, e194107. [Google Scholar] [CrossRef] [PubMed]
- Gibson, G.R.; Probert, H.M.; Loo, J.V.; Rastall, R.A.; Roberfroid, M.B. Dietary modulation of the human colonic microbiota: Updating the concept of prebiotics. Nutr. Res. Rev. 2004, 17, 259–275. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Buyken, A.E.; Goletzke, J.; Joslowski, G.; Felbick, A.; Cheng, G.; Herder, C.; Brand-Miller, J.C. Association between carbohydrate quality and inflammatory markers: Systematic review of observational and interventional studies. Am. J. Clin. Nutr. 2014, 99, 813–833. [Google Scholar] [CrossRef] [Green Version]
- Watzl, B.; Girrbach, S.; Roller, M. Inulin, oligofructose and immunomodulation. Br. J. Nutr. 2005, 93, S49–S55. [Google Scholar] [CrossRef] [PubMed]
- Fokkens, W.J.; Lund, V.J.; Mullol, J.; Bachert, C.; Alobid, I.; Baroody, F.; Cohen, N.; Cervin, A.; Douglas, R.; Gevaert, P.; et al. European position paper on rhinosinusitis and nasal polyps 2020. Rhinology 2020, 58, 1–464. [Google Scholar] [CrossRef] [PubMed]
- Long, A.; McFadden, C.; DeVine, D.; Chew, P.; Kupelnick, B.; Lau, J. Management of allergic and nonallergic rhinitis. Evid. Rep. Technol. Assess. 2002, 54, 1–6. [Google Scholar]
- Pretorius, R.A.; Bodinier, M.; Prescott, S.L.; Palmer, D.J. Maternal Fiber Dietary Intakes during Pregnancy and Infant Allergic Disease. Nutrients 2019, 11, 1767. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ismail, I.H.; Licciardi, P.V.; Tang, M.L. Probiotic effects in allergic disease. J. Paediatr. Child Health 2013, 49, 709–715. [Google Scholar] [CrossRef]
- Bisgaard, H.; Li, N.; Bonnelykke, K.; Chawes, B.L.; Skov, T.; Paludan-Müller, G.; Stokholm, J.; Smith, B.; Krogfelt, K.A. Reduced diversity of the intestinal microbiota during infancy is associated with increased risk of allergic disease at school age. J. Allergy Clin. Immunol. 2011, 128, 646–652. [Google Scholar] [CrossRef]
- Dotterud, C.K.; Storrø, O.; Johnsen, R.; Oien, T. Probiotics in pregnant women to prevent allergic disease: A randomized, double-blind trial. Br. J. Dermatol. 2010, 163, 616–623. [Google Scholar] [CrossRef]
- Thorburn, A.N.; McKenzie, C.I.; Shen, S.; Stanley, D.; Macia, L.; Mason, L.J.; Roberts, L.K.; Wong, C.H.; Shim, R.; Robert, R.; et al. Evidence that asthma is a developmental origin disease influenced by maternal diet and bacterial metabolites. Nat. Commun. 2015, 6, 7320. [Google Scholar] [CrossRef]
- Flinterman, A.E.; Knol, E.F.; Dijk, A.G.va.; Timmerman, H.M.; Knulst, A.C.; Bruijnzeel-Koomen, C.A.; Pasmans, S.G.; van Hoffen, E. Probiotics have a different immunomodulatory potential in vitro versus ex vivo upon oral administration in children with food allergy. Int. Arch. Allergy Immunol. 2007, 143, 237–244. [Google Scholar] [CrossRef] [PubMed]
- Brouwer, M.L.; Wolt-Plompen, S.A.; Dubois, A.E.; van der Heide, S.; Jansen, D.F.; Hoijer, M.A.; Kauffman, H.F.; Duiverman, E.J. No effects of probiotics on atopic dermatitis in infancy: A randomized placebo-controlled trial. Clin. Exp. Allergy. 2006, 36, 899–906. [Google Scholar] [CrossRef]
- Gerasimov, S.V.; Vasjuta, V.V.; Myhovych, O.O.; Bondarchuk, L.I. Probiotic supplement reduces atopic dermatitis in preschool children: A randomized, double-blind, placebo-controlled, clinical trial. Am. J. Clin. Dermatol. 2010, 11, 351–361. [Google Scholar] [CrossRef]
- Giovannini, M.; Agostoni, C.; Riva, E.; Salvini, F.; Ruscitto, A.; Zuccotti, G.V.; Radaelli, G. A randomized prospective double blind controlled trial on effects of long-term consumption of fermented milk containing Lactobacillus casei in pre-school children with allergic asthma and/or rhinitis. Pediatr. Res. 2007, 62, 215–220. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.S.; Jan, R.L.; Lin, Y.L.; Chen, H.H.; Wang, J.Y. Randomized placebo-controlled trial of lactobacillus on asthmatic children with allergic rhinitis. Pediatr. Pulmonol. 2010, 45, 1111–1120. [Google Scholar] [CrossRef] [PubMed]
- Devereux, G. The increase in the prevalence of asthma and allergy: Food for thought. Nat. Rev. Immunol. 2006, 6, 869–874. [Google Scholar] [CrossRef] [PubMed]
- Makki, K.; Deehan, E.C.; Walter, J.; Bäckhed, F. The impact of dietary fiber on gut microbiota in host health and disease. Cell Host Microbe. 2018, 23, 705–715. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Huffnagle, G.B. Increase in dietary fiber dampens allergic responses in the lung. Nat. Med. 2014, 20, 120–121. [Google Scholar] [CrossRef]
- Anand, S.; Mande, S.S. Diet, microbiota and gut-lung connection. Front. Microbiol. 2018, 9, 2147. [Google Scholar] [CrossRef]
- Zhang, Z.; Shi, L.; Pang, W.; Liu, W.; Li, J.; Wang, H.; Shi, G. Dietary fiber intake regulates intestinal microflora and inhibits ovalbumin-induced allergic airway inflammation in a mouse model. PLoS ONE 2016, 11, e0147778. [Google Scholar] [CrossRef] [Green Version]
- Peroni, D.G.; Bonomo, B.; Casarotto, S.; Boner, A.L.; Piacentini, G.L. How changes in nutrition have influenced the development of allergic diseases in childhood. Ital. J. Pediatr. 2012, 38, 22. [Google Scholar] [CrossRef] [Green Version]
- Andrianasolo, R.M.; Hercberg, S.; Kesse-Guyot, E.; Druesne-Pecollo, N.; Touvier, M.; Galan, P.; Varraso, R. Association between dietary fibre intake and asthma (symptoms and control): Results from the French national e-cohort NutriNet-Santé. Br. J. Nutr. 2019, 122, 1040–1051. [Google Scholar] [CrossRef]
- Folkerts, J.; Stadhouders, R.; Redegeld, F.A.; Tam, S.Y.; Hendriks, R.W.; Galli, S.J.; Maurer, M. Effect of dietary fiber and metabolites on mast cell activation and mast cell-associated diseases. Front. Immunol. 2018, 9, 1067. [Google Scholar] [CrossRef]
- Cildir, G.; Pant, H.; Lopez, A.F.; Tergaonkar, V. The transcriptional program, functional heterogeneity, and clinical targeting of mast cells. J. Exp. Med. 2017, 214, 2491–2506. [Google Scholar] [CrossRef]
- Chiu, C.Y.; Chan, Y.L.; Tsai, Y.S.; Chen, S.A.; Wang, C.J.; Chen, K.F.; Chung, I.F. Airway microbial diversity is inversely associated with mite-sensitized rhinitis and asthma in early childhood. Sci. Rep. 2017, 7, 1820. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fernstrand, A.M.; Bury, D.; Garssen, J.; Verster, J.C. Dietary intake of fibers: Differential effects in men and women on perceived general health and immune functioning. Food Nutr. Res. 2017, 61, 1297053. [Google Scholar] [CrossRef] [Green Version]
- Markle, J.G.; Frank, D.N.; Mortin-Toth, S.; Robertson, C.E.; Feazel, L.M.; Rolle-Kampczyk, U.; von Bergen, M.; McCoy, K.D.; Macpherson, A.J.; Danska, J.S. Sex differences in the gut microbiome drive hormone-dependent regulation of autoimmunity. Science 2013, 339, 1084–1088. [Google Scholar] [CrossRef] [Green Version]
- Koren, O.; Goodrich, J.K.; Cullender, T.C.; Spor, A.; Laitinen, K.; Bäckhed, H.K.; Gonzalez, A.; Werner, J.J.; Angenent, L.T.; Knight, R.; et al. Host remodeling of the gut microbiome and metabolic changes during pregnancy. Cell 2012, 150, 470–480. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hauner, H.; Bechthold, A.; Boeing, H.; Brönstrup, A.; Buyken, A.; Leschik-Bonnet, E.; Linseisen, J.; Schulze, M.; Strohm, D.; Wolfram, G. Evidence-based guideline of the German Nutrition Society: Carbohydrate intake and prevention of nutrition-related diseases. Ann. Nutr. Metab. 2012, 60, 1–58. [Google Scholar] [CrossRef] [PubMed]
| Allergic Rhinitis | Atopic Dermatitis | Asthma | |||||||
|---|---|---|---|---|---|---|---|---|---|
| No (N = 9147) | Yes (N = 1334) | p-Value | No (N = 10,034) | Yes (N = 447) | p-Value | No (N = 9974) | Yes (N = 507) | p-Value | |
| Energy (kcal, mean, SD) | 1973.80 ± 866.38 | 2034.46 ± 829.07 | 0.013 | 1977.79 ± 856.06 | 2065.29 ± 981.72 | 0.065 | 1986.63 ± 866.53 | 1881.07 ± 759.46 | 0.003 |
| Protein (g, mean, SD) | 69.98 ± 40.52 | 75.89 ± 40.20 | <0.0001 | 70.52 ± 40.10 | 75.34 ± 49.05 | 0.042 | 70.98 ± 40.65 | 65.78 ± 37.68 | 0.003 |
| Fat (g, mean, SD) | 38.05 ± 31.82 | 45.54 ± 31.96 | <0.0001 | 38.68 ± 31.77 | 46.28 ± 34.78 | <0.0001 | 39.29 ± 31.87 | 33.52 ± 32.67 | <0.0001 |
| Carbohydrates (g, mean, SD) | 322.92 ± 125.00 | 319.59 ± 122.66 | 0.363 | 322.65 ± 124.23 | 319.05 ± 135.08 | 0.581 | 322.54 ± 125.09 | 321.50 ± 117.02 | 0.846 |
| Water (g, mean, SD) | 990.78 ± 699.08 | 1057.04 ± 619.57 | <0.0001 | 995.23 ± 686.32 | 1088.57 ± 758.98 | 0.010 | 1005.41 ± 692.06 | 877.20 ± 632.04 | <0.0001 |
| Fiber (g, mean, SD) | 7.70 ± 8.13 | 7.38 ± 4.85 | 0.045 | 7.68 ± 7.88 | 7.01 ± 5.33 | 0.011 | 7.69 ± 7.90 | 7.07 ± 4.99 | 0.009 |
| Fiber Intake | Crude Odds Ratio (95% Confidence Interval) | Adjusted Odds Ratio a (95% Confidence Interval) | ||||
|---|---|---|---|---|---|---|
| Allergic Rhinitis | Asthma | Atopic Dermatitis | Allergic Rhinitis | Asthma | Atopic Dermatitis | |
| Q 1 | 1 (ref) | 1 (ref) | 1 (ref) | 1 (ref) | 1 (ref) | 1 (ref) |
| Q 2 | 0.877 (0.74–1.03) | 0.793 (0.62–1.01) | 1.004 (0.78–1.30) | 0.840 (0.70–1.00) | 0.797 (0.62–1.03) | 0.997 (0.76–1.31) |
| Q 3 | 1.019 (0.87–1.20) | 0.761 (0.60–0.97) | 0.911 (0.70–1.18) | 1.006 (0.84–1.21) | 0.777 (0.59–1.02) | 0.895 (0.67–1.20) |
| Q 4 | 0.925 (0.79–1.09) | 0.691 (0.54–0.89) | 0.746 (0.57–0.98) | 0.948 (0.77–1.17) | 0.656 (0.48–0.91) | 0.712 (0.50–1.01) |
| p for trend | 0.239 | 0.025 | 0.120 | <0.0001 | <0.0001 | <0.0001 |
| Fiber Intake | Adjusted Odds Ratio a (95% Confidence Interval) | |
|---|---|---|
| Male | Female | |
| Allergic rhinitis | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.704 (0.51–0.97) | 0.902 (0.73–1.11) |
| Q 3 | 0.862 (0.64–1.17) | 1.081 (0.87–1.34) |
| Q 4 | 0.898 (0.66–1.23) | 0.935 (0.73–1.20) |
| Asthma | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.734 (0.49–1.10) | 0.807 (0.58–1.12) |
| Q 3 | 0.589 (0.39–0.90) | 0.918 (0.66–1.29) |
| Q 4 | 0.523 (0.34–0.82) | 0.756 (0.51–1.12) |
| Atopic dermatitis | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.695 (0.45–1.09) | 1.200 (0.86–1.68) |
| Q 3 | 0.653 (0.42–1.02) | 1.067 (0.74–1.54) |
| Q 4 | 0.568 (0.35–0.91) | 0.778 (0.50–1.21) |
| Fiber Intake | Adjusted Odds Ratio a (95% CI) | |
|---|---|---|
| Male | Female | |
| Wheezing sound during breathing | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.806 (0.33–1.95) | 0.786 (0.40–1.56) |
| Q 3 | 0.641 (0.25–1.65) | 0.965 (0.48–1.93) |
| Q 4 | 1.341 (0.53–3.39) | 1.059 (0.48–2.33) |
| Exercise-induced exacerbation | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.779 (0.30–2.02) | 0.478 (0.21–1.07) |
| Q 3 | 0.906 (0.33–2.47) | 0.727 (0.33–1.59) |
| Q 4 | 0.516 (0.17–1.53) | 0.975 (0.41–2.33) |
| Fiber Intake | Adjusted Odds Ratio a (95% CI) | |
|---|---|---|
| Male | Female | |
| Rhinitis symptoms | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.806 (0.33–1.95) | 0.786 (0.40–1.56) |
| Q 3 | 0.641 (0.25–1.65) | 0.965 (0.48–1.93) |
| Q 4 | 1.341 (0.53–3.39) | 1.059 (0.48–2.33) |
| Endoscopic finding: Pale mucosa | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.779 (0.30–2.02) | 0.478 (0.21–1.07) |
| Q 3 | 0.906 (0.33–2.47) | 0.727 (0.33–1.59) |
| Q 4 | 0.516 (0.17–1.53) | 0.975 (0.41–2.33) |
| Endoscopic finding: Watery rhinorrhea | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.903 (0.68–1.19) | 0.786 (0.64–0.97) |
| Q 3 | 0.734 (0.55–0.97) | 0.913 (0.74–1.13) |
| Q 4 | 0.722 (0.54–0.97) | 0.957 (0.75–1.22) |
| Fiber Intake | Adjusted Odds Ratio a (95% CI) | |
|---|---|---|
| Male | Female | |
| Dog (≥0.35 kU/L) | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.600 (0.26–1.41) | 1.013 (0.37–2.80) |
| Q 3 | 0.319 (0.13–0.82) | 0.397 (0.10–1.56) |
| Q 4 | 0.338 (0.13–0.86) | 0.968 (0.31–3.05) |
| Cockroach (≥0.35 kU/L) | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 1.009 (0.59–1.73) | 1.056 (0.60–1.87) |
| Q 3 | 0.753 (0.44–1.29) | 0.670 (0.35–1.28) |
| Q 4 | 0.763 (0.44–1.32) | 1.033 (0.53–2.01) |
| House dust mite (≥0.35 kU/L) | ||
| 1 (ref) | 1 (ref) | |
| 1.092 (0.66–1.81) | 1.204 (0.81–1.79) | |
| 1.113 (0.68–1.82) | 0.939 (0.61–1.44) | |
| 1.157 (0.70–1.90) | 1.113 (0.68–1.82) | |
| Total IgE (≥100 kU/L) | ||
| Q 1 | 1 (ref) | 1 (ref) |
| Q 2 | 0.874 (0.53–1.45) | 1.078 (0.73–1.59) |
| Q 3 | 1.145 (0.70–1.88) | 0.788 (0.52–1.20) |
| Q 4 | 1.070 (0.65–1.77) | 1.064 (0.66–1.71) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, H.; Lee, K.; Son, S.; Kim, Y.-C.; Kwak, J.W.; Kim, H.G.; Lee, S.H.; Kim, T.H. Association of Allergic Diseases and Related Conditions with Dietary Fiber Intake in Korean Adults. Int. J. Environ. Res. Public Health 2021, 18, 2889. https://doi.org/10.3390/ijerph18062889
Lee H, Lee K, Son S, Kim Y-C, Kwak JW, Kim HG, Lee SH, Kim TH. Association of Allergic Diseases and Related Conditions with Dietary Fiber Intake in Korean Adults. International Journal of Environmental Research and Public Health. 2021; 18(6):2889. https://doi.org/10.3390/ijerph18062889
Chicago/Turabian StyleLee, Hoyoung, Kijeong Lee, Serhim Son, Young-Chan Kim, Ji Won Kwak, Hyeon Geun Kim, Sang Hag Lee, and Tae Hoon Kim. 2021. "Association of Allergic Diseases and Related Conditions with Dietary Fiber Intake in Korean Adults" International Journal of Environmental Research and Public Health 18, no. 6: 2889. https://doi.org/10.3390/ijerph18062889






