Effects of Social Isolation Measures Caused by the COVID-19 Pandemic on Occupational Balance, Participation, and Activities’ Satisfaction in the Spanish Population
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design
2.2. Participants
2.3. Data Collection
2.3.1. Outcome Measures
Occupational Balance Questionnaire (OBQ)
Questions about Satisfaction and Performance of an Activities
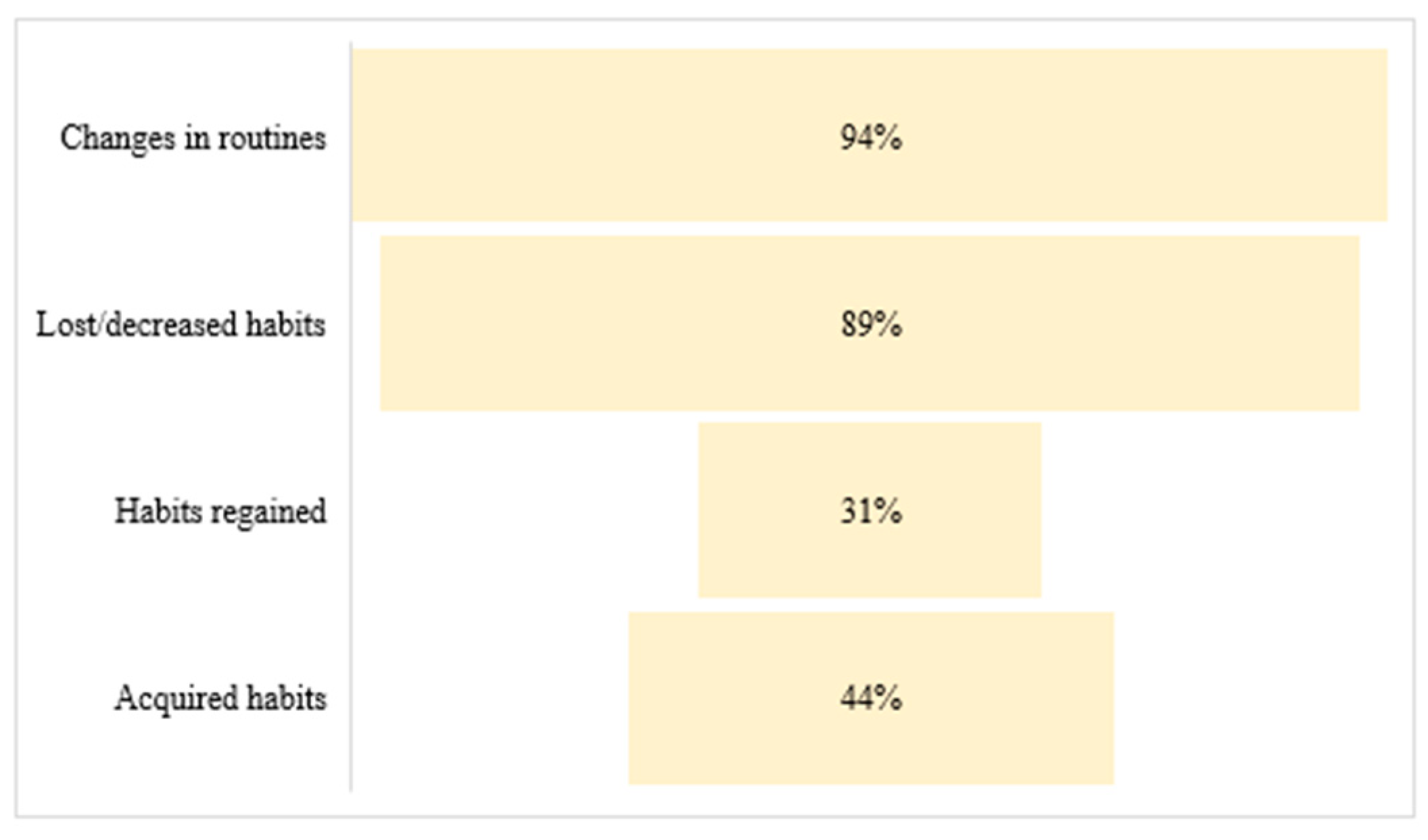
Questions on the Modification of Routine and Habits
2.4. Data Analysis
3. Results
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—11 March 2020. 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020 (accessed on 19 November 2020).
- Tobaiqy, M.; Qashqary, M.; Al-Dahery, S.; Mujallad, A.; Hershan, A.A.; Kamal, M.A.; Helmi, N. Therapeutic management of patients with COVID-19: A systematic review. Infect. Prev. Pract. 2020, 2, 100061. [Google Scholar] [CrossRef] [PubMed]
- Lai, C.C.; Shih, T.P.; Ko, W.C.; Tang, H.J.; Hsueh, P.R. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and coronavirus disease-2019 (COVID-19): The epidemic and the challenges. Int. J. Antimicrob. 2020, 55, 105924. [Google Scholar] [CrossRef]
- Vaira, L.A.; Salzano, G.; Deiana, G.; De Riu, G. Anosmia and Ageusia: Common Findings in COVID-19 Patients. Laryngoscope 2020, 130, 1787. [Google Scholar] [CrossRef] [Green Version]
- Rebholz, H.; Braun, R.J.; Ladage, D.; Knoll, W.; Kleber, C.; Hassel, A.W. Loss of Olfactory Function—Early Indicator for COVID-19, Other Viral Infections and Neurodegenerative Disorders. Front. Neurol. 2020, 11, 1264. [Google Scholar] [CrossRef] [PubMed]
- Lechien, J.R.; Hsieh, J.W.; Ayad, T.; Fakhry, N.; Hans, S.; Chiesa-Estomba, C.M.; Saussez, S. Gustatory dysfunctions in COVID-19. Eur. Arch. Oto-Rhino-Laryngol. 2020, 277, 2397–2398. [Google Scholar] [CrossRef] [PubMed]
- Scangas, G.A.; Bleier, B.S. Anosmia: Differential Diagnosis, Evaluation and Management. Am. J. Rhinol. Allergy 2017, 31, 3–7. [Google Scholar] [CrossRef] [PubMed]
- Kamalakannan, S.; Chakraborty, S. Occupational therapy: The key to unlocking locked-up occupations during the COVID-19 pandemic. Wellcome Open Res. 2020, 5, 153. [Google Scholar] [CrossRef]
- Gonzalez-Bernal, J.J.; Rodríguez-Fernández, P.; Santamaría-Peláez, M.; González-Santos, J.; León-Del-barco, B.; Minguez, L.A.; Soto-Cámara, R. Life satisfaction during forced social distancing and home confinement derived from the COVID-19 pandemic in Spain. Int. J. Environ. Res. Public Health 2021, 18, 1474. [Google Scholar] [CrossRef]
- Rodríguez-Rey, R.; Garrido-Hernansaiz, H.; Collado, S. Psychological Impact and Associated Factors During the Initial Stage of the Coronavirus (COVID-19) Pandemic Among the General Population in Spain. Front. Psychol. 2020, 11, 1540. [Google Scholar] [CrossRef]
- Qi, M.; Li, P.; Moyle, W.; Weeks, B.; Jones, C. Physical Activity, Health-Related Quality of Life, and Stress among the Chinese Adult Population during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2020, 17, 6494. [Google Scholar] [CrossRef]
- Epifanio, M.S.; Andrei, F.; Mancini, G.; Agostini, F.; Piombo, M.A.; Spicuzza, V.; Riolo, M.; Lavanco, G.; Trombini, E.; La Grutta, S. The Impact of COVID-19 Pandemic and Lockdown Measures on Quality of Life among Italian General Population. J. Clin. Med. 2021, 10, 289. [Google Scholar] [CrossRef] [PubMed]
- Teotônio, I.; Hecht, M.; Castro, L.C.; Gandolfi, L.; Pratesi, R.; Nakano, E.Y.; Zandonadi, R.P.; Pratesi, C.B. Repercussion of COVID-19 Pandemic on Brazilians’ Quality of Life: A Nationwide Cross-Sectional Study. Int. J. Environ. Res. Public Health 2020, 17, 8554. [Google Scholar] [CrossRef] [PubMed]
- Backman, C.L. Occupational balance: Exploring the relationships among daily occupations and their influence on well-being. Can. J. Occup. Ther. 2004, 71, 202–209. [Google Scholar] [CrossRef] [PubMed]
- González-Bernal, J.J.; Santamaría-Peláez, M.; González-Santos, J.; Rodríguez-Fernández, P.; León del Barco, B.; Soto-Cámara, R. Relationship of Forced Social Distancing and Home Confinement Derived from the COVID-19 Pandemic with the Occupational Balance of the Spanish Population. J. Clin. Med. 2020, 9, 3606. [Google Scholar] [CrossRef] [PubMed]
- Wagman, P.; Håkansson, C.; Björklund, A. Occupational balance as used in occupational therapy: A concept analysis. Scand. J. Occup. Ther. 2012, 19, 322–327. [Google Scholar] [CrossRef]
- Anaby, D.R.; Backman, C.L.; Jarus, T. Measuring occupational balance: A theoretical exploration of two approaches. Can. J. Occup. Ther. 2010, 77, 280–288. [Google Scholar] [CrossRef]
- Rodríguez-Fernández, P.; González-Santos, J.; Santamaría-Peláez, M.; Soto-Cámara, R.; González-Bernal, J.J. Exploring the Occupational Balance of Young Adults during Social Distancing Measures in the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 5809. [Google Scholar] [CrossRef]
- von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for reporting observational studies. Int. J. Surg. 2014, 12, 1495–1499. [Google Scholar] [CrossRef] [Green Version]
- World Medical Association. Declaration of Helsinki: Ethical Principles for Medical Research Involving Human Subjects. JAMA 2013, 310, 2191–2194. [Google Scholar] [CrossRef] [Green Version]
- Wagman, P.; Håkansson, C. Introducing the Occupational Balance Questionnaire (OBQ). Scand. J. Occup. Ther. 2014, 21, 227–231. [Google Scholar] [CrossRef]
- Peral-Gómez, P.; López-Roig, S.; Pastor-Mira, M.Á.; Abad-Navarro, E.; Valera-Gran, D.; Håkansson, C.; Wagman, P. Cultural Adaptation and Psychometric Properties of the Spanish Version of the Occupational Balance Questionnaire: An Instrument for Occupation-Based Research. Int. J. Environ. Res. Public Health 2021, 18, 7506. [Google Scholar] [CrossRef] [PubMed]
- Law, M.; Baptiste, S.; Mccoll, M.; Opzoomer, A.; Polatajko, H.; Pollock, N. The Canadian Occupational Performance Measure: An Outcome Measure for Occupational Therapy. Can. J. Occup. Ther. 1990, 57, 82–87. [Google Scholar] [CrossRef] [PubMed]
- Eklund, M.; Orban, K.; ArgentZell, E.; Bejerholm, U.; Tjörnstrand, C.; Erlandsson, L.K.; Håkansson, C. The linkage between patterns of daily occupations and occupational balance: Applications within occupational science and occupational therapy practice. Scand. J. Occup. Ther. 2017, 24, 41–56. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lipskaya-Velikovsky, L. COVID-19 isolation in healthy population in Israel: Challenges in daily life, mental health, resilience, and quality of life. Int. J. Environ. Res. Public Health 2021, 18, 999. [Google Scholar] [CrossRef]
- Savitsky, B.; Radomislensky, I.; Hendel, T. Nurses’ occupational satisfaction during COVID-19 pandemic. Appl. Nurs. Res. 2021, 59, 151416. [Google Scholar] [CrossRef]
- Yu, Y.; Manku, M.; Backman, C.L. Measuring occupational balance and its relationship to perceived stress and health: Mesurer l’équilibre occupationnel et sa relation avec le stress perçus et la santé. Can. J. Occup. Ther. 2018, 85, 117–127. [Google Scholar] [CrossRef]
- Håkansson, C.; Leo, U.; Oudin, A.; Arvidsson, I.; Nilsson, K.; Österberg, K.; Persson, R. Organizational and social work environment factors, occupational balance and no or negligible stress symptoms among Swedish principals–A cross-sectional study. BMC Public Health 2021, 21, 800. [Google Scholar] [CrossRef]
- Di Renzo, L.; Gualtieri, P.; Pivari, F.; Soldati, L.; Attinà, A.; Cinelli, G.; Leggeri, C.; Caparello, G.; Barrea, L.; Scerbo, F.; et al. Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J. Transl. Med. 2020, 18, 229. [Google Scholar] [CrossRef]
- Hay, J.W.; Gong, C.L.; Jiao, X.; Zawadzki, N.K.; Zawadzki, R.S.; Pickard, A.S.; Xie, F.; Crawford, S.A.; Gu, N.Y. A US Population Health Survey on the Impact of COVID-19 Using the EQ-5D-5L. J. Gen. Intern. Med. 2021, 36, 1292–1301. [Google Scholar] [CrossRef]
- Fridman, A.; Gershon, R.; Gneezy, A. COVID-19 and vaccine hesitancy: A longitudinal study. PLoS ONE 2021, 16, e0250123. [Google Scholar] [CrossRef]




| Variables | Descriptive Data |
|---|---|
| Sex | |
| Male | 134 (44.7%) |
| Female | 166 (55.3%) |
| Age (years) | |
| Median (IQR) | 39 (56–23) |
| Age range | |
| 18–30 years of age | 143 (47.7%) |
| 31–64 years of age | 118 (39.3%) |
| 65 years of age or more | 37 (12.3%) |
| Missing data | 2 (0.7%) |
| Region of residence | |
| North | 65 (21.7%) |
| Center | 213 (71%) |
| South | 19 (6.3%) |
| Missing data | 3 (1%) |
| OBQ-E | |||
|---|---|---|---|
| Median (IQR) | Statistic Value | p | |
| Whole sample | −10.789 | 0.001 | |
| before pandemic | 45 (51–39) | ||
| during pandemic | 35 (43.75–26) | ||
| Sex | |||
| before pandemic | |||
| Man | 44 (50–37) | 9272.000 a | 0.023 |
| Woman | 46 (52–40) | ||
| during pandemic | |||
| Man | 35 (43–24.75) | 8907.000 a | 0.33 |
| Woman | 36 (44.25–26.75) | ||
| Range of age | |||
| before pandemic | |||
| 18–30 years of age | 43 (50–37) | 28.396 b | 0 |
| 31–64 years of age | 46 (52–40) | ||
| 65 years of age or more | 50 (57–46) | ||
| during pandemic | |||
| 18–30 years of age | 32 (40–24) | 20.511 b | 0 |
| 31–64 years of age | 39 (47–26) | ||
| 65 years of age or more | 42 (49.5–36) | ||
| Region of residence | |||
| before pandemic | |||
| North | 48 (53–43) | 6.756 b | 0.034 |
| Center | 44 (51–38) | ||
| South | 45 (50–37) | ||
| during pandemic | |||
| North | 38.5 (47.75–26) | 2.047 b | 0.359 |
| Center | 35 (43–26) | ||
| South | 35 (39.5–24) | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rodríguez-Rivas, C.; Camacho-Montaño, L.R.; García-Bravo, C.; García-de-Miguel, M.; Pérez-de-Heredia-Torres, M.; Huertas-Hoyas, E. Effects of Social Isolation Measures Caused by the COVID-19 Pandemic on Occupational Balance, Participation, and Activities’ Satisfaction in the Spanish Population. Int. J. Environ. Res. Public Health 2022, 19, 6497. https://doi.org/10.3390/ijerph19116497
Rodríguez-Rivas C, Camacho-Montaño LR, García-Bravo C, García-de-Miguel M, Pérez-de-Heredia-Torres M, Huertas-Hoyas E. Effects of Social Isolation Measures Caused by the COVID-19 Pandemic on Occupational Balance, Participation, and Activities’ Satisfaction in the Spanish Population. International Journal of Environmental Research and Public Health. 2022; 19(11):6497. https://doi.org/10.3390/ijerph19116497
Chicago/Turabian StyleRodríguez-Rivas, Cristina, Lucia Rocío Camacho-Montaño, Cristina García-Bravo, María García-de-Miguel, Marta Pérez-de-Heredia-Torres, and Elisabet Huertas-Hoyas. 2022. "Effects of Social Isolation Measures Caused by the COVID-19 Pandemic on Occupational Balance, Participation, and Activities’ Satisfaction in the Spanish Population" International Journal of Environmental Research and Public Health 19, no. 11: 6497. https://doi.org/10.3390/ijerph19116497
APA StyleRodríguez-Rivas, C., Camacho-Montaño, L. R., García-Bravo, C., García-de-Miguel, M., Pérez-de-Heredia-Torres, M., & Huertas-Hoyas, E. (2022). Effects of Social Isolation Measures Caused by the COVID-19 Pandemic on Occupational Balance, Participation, and Activities’ Satisfaction in the Spanish Population. International Journal of Environmental Research and Public Health, 19(11), 6497. https://doi.org/10.3390/ijerph19116497





