Resilience Improves the Quality of Life and Subjective Happiness of Physiotherapists during the COVID-19 Pandemic
Abstract
:1. Introduction
2. Material and Methods
2.1. Study Design and Participants
2.2. Data Collection and Ethical Considerations
2.3. Demographic Data
2.4. 14-Item Resilience Scale (14-RS)
2.5. 36-item Short Form Health Survey (SF-36)
2.6. Subjective Happiness Scale (SHS)
2.7. Statistical Analysis
3. Results
3.1. Demographic Characteristics of Groups Categorized in Terms of Resilience and Working with COVID-19 Patients
3.2. Physiotherapists’ Perceptions of Health (Question 2/SF-36)
3.3. SF-36 and SHS for Groups Categorized in Terms of Resilience and Working with COVID-19 Patients
3.4. Regression Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Appendix A. 14-Item Resilience Scale (14-RS)

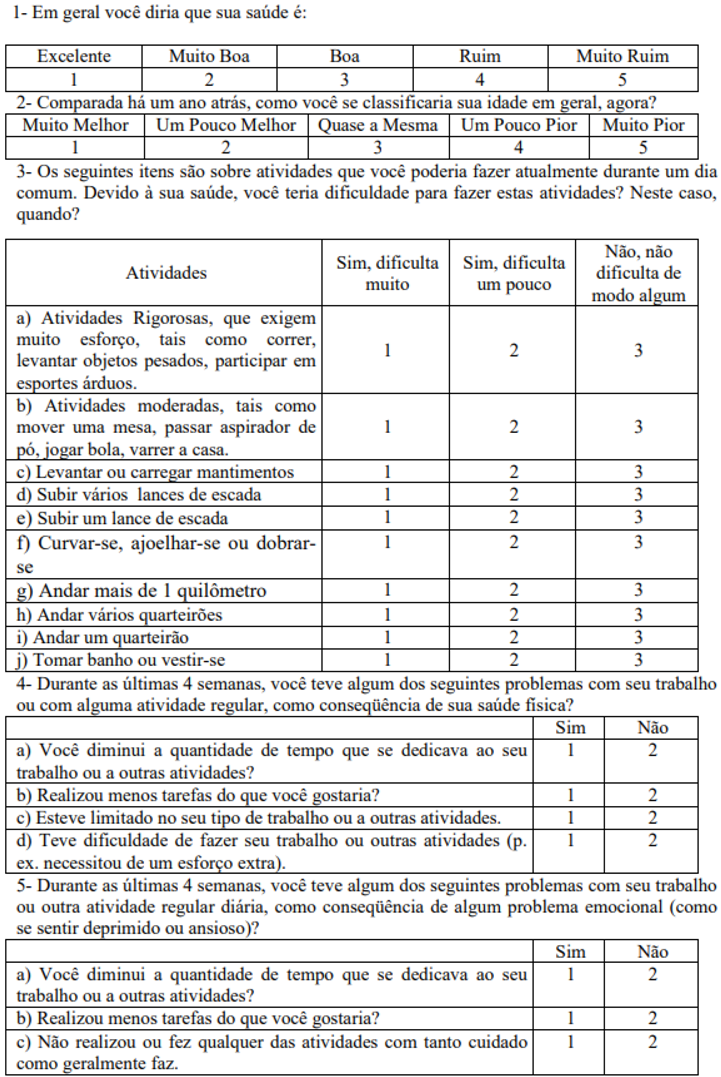
Appendix B. 36 Item Short Form Survey (SF-36)


Appendix C. Subjective Happiness Scale (SHS)

References
- World Health Organization. COVID-19 Cases and Deaths by Country. Available online: https://portal.who.int/report/eios-covid19-cunts/#display=Countries_and_Territories&nrow=2&ncol=3&arr=row&pg=1&labels=&sort=cur_case_who;desc&filter=&sidebar=0&fv= (accessed on 7 October 2021).
- Instituto Brasileiro de Geografia e Estatística (IBGE). Projeção da População do Brasil e Unidades de Federação. Available online: https://www.ibge.gov.br/apps/populacao/projecao/inex.html?utm_source=portal&utm_medium=poplock&utm_campaign=novo_poplock (accessed on 7 October 2021).
- Mallah, S.I.; Ghorab, O.K.; Al-Salmi, S.; Abdellatif, O.S.; Tharmaratnam, T.; Iskandar, M.A.; Sefen, J.; Sidhu, P.; Atallah, B.; El-Lababidi, R.; et al. COVID-19: Breaking down a global health crisis. Ann. Clin. Microbiol. Antimicrob. 2021, 20, 35. [Google Scholar] [CrossRef]
- World Health Organization. Brazil: WHO Coronavirus Disease (COVID-19) Dashboard with Vaccination Data. Available online: https://covid19.who.int/region/amro/country/br (accessed on 7 October 2021).
- Nakada, L.Y.K.; Urban, R.C. COVID-19 pandemic: Environmental and social factors influencing the spread of SARS-CoV-2 in São Paulo, Brazil. Environ. Sci. Pollut. Res. Int. 2021, 28, 40322–40328. [Google Scholar] [CrossRef] [PubMed]
- De Souza, W.M.; Buss, L.F.; Candido, D.D.S.; Carrera, J.P.; Li, S.; Zarebski, A.E.; Pereira, R.; Prete, C.A., Jr.; de Souza-Santos, A.A.; Parag, K.V.; et al. Epidemiological and clinical characteristics of the COVID-19 epidemic in Brazil. Nat. Hum. Behav. 2020, 4, 856–865. [Google Scholar] [CrossRef]
- Fortaleza, C.M.C.B.; Guimarães, R.B.; de Almeida, G.B.; Pronunciate, M.; Ferreira, C.P. Taking the inner route: Spatial and demographic factors affecting vulnerability to COVID-19 among 604 cities from inner São Paulo State, Brazil. Epidemiol. Infect. 2020, 148, e118. [Google Scholar] [CrossRef] [PubMed]
- Moreira, R.D.S. COVID-19: Intensive care units, mechanical ventilators, and latent mortality profiles associated with case-fatality in Brazil. Cad. Saude Publica 2020, 36, e00080020. [Google Scholar] [CrossRef] [PubMed]
- Palamim, C.V.C.; Marson, F.A.L. COVID-19—The Availability of ICU Beds in Brazil during the Onset of Pandemic. Ann. Glob. Health 2020, 86, 100. [Google Scholar] [CrossRef] [PubMed]
- Vincent, J.L.; Creteur, J. Ethical aspects of the COVID-19 crisis: How to deal with an overwhelming shortage of acute beds. Eur. Heart J. Acute Cardiovasc. Care 2020, 9, 248–252. [Google Scholar] [CrossRef]
- Tyrrell, C.S.B.; Mytton, O.T.; Gentry, S.V.; Thomas-Meyer, M.; Allen, J.; Narula, A.A.; McGrath, B.; Lupton, M.; Broadbent, J.; Ahmed, A.; et al. Managing intensive care admissions when there are not enough beds during the COVID-19 pandemic: A systematic review. Thorax 2021, 76, 302–312. [Google Scholar] [CrossRef] [PubMed]
- Noronha, K.V.M.S.; Guedes, G.R.; Turra, C.M.; Andrade, M.V.; Botega, L.; Nogueira, D.; Calazans, J.A.; Carvalho, L.; Servo, L.; Ferreira, M.F. The COVID-19 pandemic in Brazil: Analysis of supply and demand of hospital and ICU beds and mechanical ventilators under different scenarios. Pandemia por COVID-19 no Brasil: Análise da demanda e da oferta de leitos hospitalares e equipamentos de ventilação assistida segundo diferentes cenários. Cad. Saude Publica 2020, 36, e00115320. [Google Scholar] [PubMed]
- Martin-Delgado, J.; Viteri, E.; Mula, A.; Serpa, P.; Pacheco, G.; Prada, D.; Campos de Andrade Lourenção, D.; Campos Pavan Baptista, P.; Ramirez, G.; Mira, J.J. Availability of personal protective equipment and diagnostic and treatment facilities for healthcare workers involved in COVID-19 care: A cross-sectional study in Brazil, Colombia, and Ecuador. PLoS ONE 2020, 15, e0242185. [Google Scholar] [CrossRef]
- Griffin, K.M.; Karas, M.G.; Ivascu, N.S.; Lief, L. Hospital Preparedness for COVID-19: A Practical Guide from a Critical Care Perspective. Am. J. Respir. Crit. Care Med. 2020, 201, 1337–1344. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Arabi, Y.M.; Azoulay, E.; Al-Dorzi, H.M.; Phua, J.; Salluh, J.; Binnie, A.; Hodgson, C.; Angus, D.C.; Cecconi, M.; Du, B.; et al. How the COVID-19 pandemic will change the future of critical care. Intensive Care Med. 2021, 47, 282–291. [Google Scholar] [CrossRef] [PubMed]
- Firew, T.; Sano, E.D.; Lee, J.W.; Flores, S.; Lang, K.; Salman, K.; Greene, M.C.; Chang, B.P. Protecting the front line: A cross-sectional survey analysis of the occupational factors contributing to healthcare workers’ infection and psychological distress during the COVID-19 pandemic in the USA. BMJ Open 2020, 10, e042752. [Google Scholar] [CrossRef] [PubMed]
- Feingold, J.H.; Hurtado, A.; Feder, A.; Peccoralo, L.; Southwick, S.M.; Ripp, J.; Pietrzak, R.H. Posttraumatic growth among health care workers on the frontlines of the COVID-19 pandemic. J. Affect. Disord. 2022, 296, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Tran, T.V.; Nguyen, H.C.; Pham, L.V.; Nguyen, M.H.; Nguyen, H.C.; Ha, T.H.; Phan, D.T.; Dao, H.K.; Nguyen, P.B.; Trinh, M.V.; et al. Impacts and interactions of COVID-19 response involvement, health-related behaviours, health literacy on anxiety, depression and health-related quality of life among healthcare workers: A cross-sectional study. BMJ Open 2020, 10, e041394. [Google Scholar] [CrossRef]
- Martín, J.; Padierna, Á.; Villanueva, A.; Quintana, J.M. Evaluation of the mental health of health professionals in the COVID-19 era. What mental health conditions are our health care workers facing in the new wave of coronavirus? Int. J. Clin. Pract. 2021, 75, e14607. [Google Scholar] [CrossRef]
- Farì, G.; de Sire, A.; Giorgio, V.; Rizzo, L.; Bruni, A.; Bianchi, F.P.; Zonno, A.; Pierucci, P.; Ranieri, M.; Megna, M. Impact of COVID-19 on the mental health in a cohort of Italian rehabilitation healthcare workers. J. Med. Virol. 2022, 94, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Righetti, R.F.; Onoue, M.A.; Politi, F.V.A.; Teixeira, D.T.; Souza, P.N.; Kondo, C.S.; Moderno, E.V.; Moraes, I.G.; Maida, A.; Pastore Junior, L.; et al. Physiotherapy care of patients with Coronavirus disease 2019 (COVID-19)—A Brazilian experience. Clinics 2020, 75, e2017. [Google Scholar] [CrossRef] [PubMed]
- Simonelli, C.; Paneroni, M.; Fokom, A.G.; Saleri, M.; Speltoni, I.; Favero, I.; Garofali, F.; Scalvini, S.; Vitacca, M. How the COVID-19 infection tsunami revolutionized the work of respiratory physiotherapists: An experience from Northern Italy. Monaldi Arch. Chest Dis. 2020, 90, 292–298. [Google Scholar] [CrossRef]
- Conselho Federal de Fisioterapia Terapia Ocupacional (COFFITO). Available online: https://www.coffito.gov.br/nsite/?p=3208 (accessed on 9 April 2022).
- Fonseca, M.C.M.; Araújo, G.T.B.; Scorza, F.A.; Silva, P.; Andrade, T.; Farah, D.; Sansone, D. Who is going to turn on the ventilators? Einstein 2021, 19, eAO6211. [Google Scholar] [CrossRef]
- Crippa, J.A.S.; Zuardi, A.W.; Guimarães, F.S.; Campos, A.C.; de Lima Osório, F.; Loureiro, S.R.; Dos Santos, R.G.; Souza, J.; Ushirohira, J.M.; Pacheco, J.C.; et al. Efficacy and Safety of Cannabidiol Plus Standard Care vs Standard Care Alone for the Treatment of Emotional Exhaustion and Burnout Among Frontline Health Care Workers During the COVID-19 Pandemic: A Randomized Clinical Trial. JAMA Netw. Open 2021, 4, e2120603. [Google Scholar] [CrossRef]
- Duarte, H.; Daros Vieira, R.; Cardozo Rocon, P.; Andrade, A.; Wittmer, V.L.; Capellini, V.K.; Soares, S.; Paro, F.M. Factors associated with Brazilian physical therapists’ perception of stress during the COVID-19 pandemic: A cross-sectional survey. Psychol. Health Med. 2022, 27, 42–53. [Google Scholar] [CrossRef]
- Lino, J.A.; CG Frota, L.G.; VAbdon, A.P.; Cavalheri, V.; Mont’Alverne, D.G.B.; Mesquita, R. Sleep quality and associated factors amongst Brazilian physiotherapists during the COVID-19 pandemic. Physiother. Theory Pract. 2021, 1–9. [Google Scholar] [CrossRef]
- Cheng, S.K.; Sheng, B.; Lau, K.K.; Wong, C.W.; Ng, Y.K.; Li, H.L.; Chan, E.L.; Tso, E.Y.; Lam, K.; Chau, T.N.; et al. Adjustment outcomes in Chinese patients following one-month recovery from severe acute respiratory syndrome in Hong Kong. J. Nerv. Ment. Dis. 2004, 192, 868–871. [Google Scholar] [CrossRef]
- Lehmann, M.; Bruenahl, C.A.; Addo, M.M.; Becker, S.; Schmiedel, S.; Lohse, A.W.; Schramm, C.; Löwe, B. Acute Ebola virus disease patient treatment and health-related quality of life in health care professionals: A controlled study. J. Psychosom. Res. 2016, 83, 69–74. [Google Scholar] [CrossRef]
- Buselli, R.; Corsi, M.; Baldanzi, S.; Chiumiento, M.; Del Lupo, E.; Dell’Oste, V.; Bertelloni, C.A.; Massimetti, G.; Dell’Osso, L.; Cristaudo, A.; et al. Professional Quality of Life and Mental Health Outcomes among Health Care Workers Exposed to SARS-CoV-2 (COVID-19). Int. J. Environ. Res. Public Health 2020, 17, 6180. [Google Scholar] [CrossRef]
- Suryavanshi, N.; Kadam, A.; Dhumal, G.; Nimkar, S.; Mave, V.; Gupta, A.; Cox, S.R.; Gupte, N. Mental health and quality of life among healthcare professionals during the COVID-19 pandemic in India. Brain Behav. 2020, 10, e01837. [Google Scholar] [CrossRef]
- Kuykendall, L.; Tay, L.; Ng, V. Leisure engagement and subjective well-being: A meta-analysis. Psychol. Bull. 2015, 141, 364–403. [Google Scholar] [CrossRef]
- Feliu-Soler, A.; de Diego-Adeliño, J.; Luciano, J.V.; Iraurgi, I.; Alemany, C.; Puigdemont, D.; Pérez, V.; Portella, M.J.; Trujols, J. Unhappy While Depressed: Examining the Dimensionality, Reliability and Validity of the Subjective Happiness Scale in a Spanish Sample of Patients with Depressive Disorders. Int. J. Environ. Res. Public Health 2021, 18, 10964. [Google Scholar] [CrossRef]
- Diener, E.; Oishi, S.; Tay, L. Advances in subjective well-being research. Nat. Hum. Behav. 2018, 2, 253–260. [Google Scholar] [CrossRef]
- Oates, J. What keeps nurses happy? Implications for workforce well-being strategies. Nurs. Manag. 2018, 25, 34–41. [Google Scholar] [CrossRef] [PubMed]
- Gray, P.; Senabe, S.; Naicker, N.; Kgalamono, S.; Yassi, A.; Spiegel, J.M. Workplace-Based Organizational Interventions Promoting Mental Health and Happiness among Healthcare Workers: A Realist Review. Int. J. Environ. Res. Public Health 2019, 16, 4396. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dhingra, V.; Dhingra, M. Effect of perceived stress on psychological well-being of health care workers during COVID 19: Mediating role of subjective happiness. Eur. J. Mol. Clin. Med. 2020, 7, 3683–3701. [Google Scholar]
- Hardy, G.E.; Woods, D.; Wall, T.D. The impact of psychological distress on absence from work. J. Appl. Psychol. 2003, 88, 306–314. [Google Scholar] [CrossRef]
- Tawfik, D.S.; Profit, J.; Morgenthaler, T.I.; Satele, D.V.; Sinsky, C.A.; Dyrbye, L.N.; Tutty, M.A.; West, C.P.; Shanafelt, T.D. Physician Burnout, Well-being, and Work Unit Safety Grades in Relationship to Reported Medical Errors. Mayo Clin. Proc. 2018, 93, 1571–1580. [Google Scholar] [CrossRef]
- Russell, J.E.A. Promoting Subjective Well-Being at Work. J. Career Assess. 2008, 16, 117–131. [Google Scholar] [CrossRef]
- Medvedev, O.N.; Landhuis, C.E. Exploring constructs of well-being, happiness and quality of life. Peer J. 2018, 6, e4903. [Google Scholar] [CrossRef]
- Robertson, H.D.; Elliott, A.M.; Burton, C.; Iversen, L.; Murchie, P.; Porteous, T.; Matheson, C. Resilience of primary healthcare professionals: A systematic review. Br. J. Gen. Pract. 2016, 66, e423–e433. [Google Scholar] [CrossRef] [Green Version]
- Ristevska-Dimitrovska, G.; Filov, I.; Rajchanovska, D.; Stefanovski, P.; Dejanova, B. Resilience and Quality of Life in Breast Cancer Patients. Open Access Maced. J. Med. Sci. 2015, 3, 727–731. [Google Scholar] [CrossRef] [Green Version]
- Gerino, E.; Rollè, L.; Sechi, C.; Brustia, P. Loneliness, Resilience, Mental Health, and Quality of Life in Old Age: A Structural Equation Model. Front. Psychol. 2017, 8, 2003. [Google Scholar] [CrossRef]
- Tempski, P.; Santos, I.S.; Mayer, F.B.; Enns, S.C.; Perotta, B.; Paro, H.B.; Gannam, S.; Peleias, M.; Garcia, V.L.; Baldassin, S.; et al. Relationship among Medical Student Resilience, Educational Environment and Quality of Life. PLoS ONE 2015, 10, e0131535. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Elliott, T.R.; Hsiao, Y.Y.; Kimbrel, N.A.; Meyer, E.; DeBeer, B.B.; Gulliver, S.B.; Kwok, O.M.; Morissette, S.B. Resilience and Traumatic Brain Injury among Iraq/Afghanistan War Veterans: Differential Patterns of Adjustment and Quality of Life. J. Clin. Psychol. 2017, 73, 1160–1178. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.; Ou, L. Resilience and quality of life among Wenchuan earthquake survivors: The mediating role of social support. Public Health 2014, 128, 430–437. [Google Scholar] [CrossRef] [PubMed]
- Hegney, D.G.; Rees, C.S.; Eley, R.; Osseiran-Moisson, R.; Francis, K. The contribution of individual psychological resilience in determining the professional quality of life of Australian nurses. Front. Psychol. 2015, 6, 1613. [Google Scholar] [CrossRef] [Green Version]
- Ferreira, P.; Gomes, S. The Role of Resilience in Reducing Burnout: A Study with Healthcare Workers during the COVID-19 Pandemic. Soc. Sci. 2021, 10, 317. [Google Scholar] [CrossRef]
- Delgado, C.; Upton, D.; Ranse, K.; Furness, T.; Foster, K. Nurses’ resilience and the emotional labour of nursing work: An integrative review of empirical literature. Int. J. Nurs. Stud. 2017, 70, 71–88. [Google Scholar] [CrossRef]
- Son, H.S.; Kim, K.; Cho, I.K.; Lee, J.; Choi, J.M.; Kil, K.H.; Kim, J.; Hong, Y.; Ahn, M.H.; Chung, S. Healthcare Workers’ Resilience Mediates the Influence of Organizational Commitment and Anxiety Response to Viral Epidemic on Their Quality of Life in the COVID-19 Pandemic. Front. Psychiatry 2022, 12, 735016. [Google Scholar] [CrossRef]
- Choi, H.J.; Yang, C.M.; Lee, S.Y.; Lee, H.J.; Jang, S.H. Mental Health and Quality of Life for Healthcare Workers in a University Hospital Under COVID-19. Psychiatry Investig. 2022, 19, 85–91. [Google Scholar] [CrossRef]
- Bajaj, B.; Khoury, B.; Sengupta, S. Resilience and Stress as Mediators in the Relationship of Mindfulness and Happiness. Front. Psychol. 2022, 13, 771263. [Google Scholar] [CrossRef]
- Lü, W.; Wang, Z.; Liu, Y.; Zhang, H. Resilience as a mediator between extraversion, neuroticism and happiness, PA and NA. Personal. Individ. Differ. 2014, 63, 128–133. [Google Scholar] [CrossRef]
- Babić, R.; Babić, M.; Rastović, P.; Ćurlin, M.; Šimić, J.; Mandić, K.; Pavlović, K. Resilience in Health and Illness. Psychiatr. Danub. 2020, 32, 226–232. [Google Scholar] [PubMed]
- Jackson, D.; Firtko, A.; Edenborough, M. Personal resilience as a strategy for surviving and thriving in the face of workplace adversity: A literature review. J. Adv. Nurs. 2007, 60, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Haglund, M.E.; Nestadt, P.S.; Cooper, N.S.; Southwick, S.M.; Charney, D.S. Psychobiological mechanisms of resilience: Relevance to prevention and treatment of stress-related psychopathology. Dev. Psychopathol. 2007, 19, 889–920. [Google Scholar] [CrossRef] [PubMed]
- Young, K.P.; Kolcz, D.L.; O’Sullivan, D.M.; Ferrand, J.; Fried, J.; Robinson, K. Health Care Workers’ Mental Health and Quality of Life During COVID-19: Results From a Mid-Pandemic, National Survey. Psychiatr. Serv. 2021, 72, 122–128. [Google Scholar] [CrossRef] [PubMed]
- Morganstein, J.C.; Flynn, B.W. Enhancing Psychological Sustainment & Promoting Resilience in Healthcare Workers during COVID-19 & Beyond: Adapting Crisis Interventions from High-Risk Occupations. J. Occup. Environ. Med. 2021, 63, 482–489. [Google Scholar]
- Rose, S.; Hartnett, J.; Pillai, S. Healthcare worker’s emotions, perceived stressors and coping mechanisms during the COVID-19 pandemic. PLoS ONE 2021, 16, e0254252. [Google Scholar] [CrossRef]
- Davydov, D.M.; Stewart, R.; Ritchie, K.; Chaudieu, I. Resilience and mental health. Clin. Psychol. Rev. 2010, 30, 479–495. [Google Scholar] [CrossRef] [Green Version]
- Pesce, R.P.; Assis, S.G.; Avanci, J.Q.; Santos, N.C.; Malaquias, J.V.; Carvalhaes, R. Cross-cultural adaptation, reliability, and validity of the resilience scale. Cad. Saude Publica 2005, 21, 436–448. [Google Scholar] [CrossRef] [Green Version]
- Wagnild, G.M.; Young, H.M. Development and psychometric evaluation of the Resilience Scale. J. Nurs. Meas. 1993, 1, 165–178. [Google Scholar]
- Brazier, J.E.; Harper, R.; Jones, N.M.; O’Cathain, A.; Thomas, K.J.; Usherwood, T.; Westlake, L. Validating the SF-36 health survey questionnaire: New outcome measure for primary care. BMJ 1992, 305, 160–164. [Google Scholar] [CrossRef] [Green Version]
- Ware, J.E., Jr.; Snow, K.K.; Kosinski, M.; Gandek, B. SF-36 Health Survey Manual and Interpretation Guide; The Health Institute, New England Medical Center: Boston, MA, USA, 1993. [Google Scholar]
- Ciconelli, R.M.; Ferraz, M.B.; Santos, W.; Meinão, I. Brazilian-Portuguese version of the SF-36. A reliable and valid quality of life outcome measure. Rev. Bras. Reumatol. 1999, 39, 143–150. [Google Scholar]
- Lyubomirsky, S.; Lepper, H.S. A Measure of Subjective Happiness: Preliminary Reliability and Construct Validation. Soc. Indic. Res. 1999, 46, 137–155. [Google Scholar] [CrossRef]
- Pais-Ribeiro, J.L. Validação Transcultural da Escala de Felicidade Subjectiva de Lyubomirsky e Lepper. Psicol. Saúde Doenças 2012, 12, 157–168. [Google Scholar]
- Solis, A.C.; Lotufo-Neto, F. Predictors of quality of life in Brazilian medical students: A systematic review and meta-analysis. Braz. J. Psychiatry 2019, 41, 556–567. [Google Scholar] [CrossRef]
- Di Trani, M.; Mariani, R.; Ferri, R.; De Berardinis, D.; Frigo, M.G. From Resilience to Burnout in Healthcare Workers During the COVID-19 Emergency: The Role of the Ability to Tolerate Uncertainty. Front. Psychol. 2021, 12, 646435. [Google Scholar] [CrossRef]
- Di Tella, M.; Romeo, A.; Benfante, A.; Castelli, L. Mental health of healthcare workers during the COVID-19 pandemic in Italy. J. Eval. Clin. Pract. 2020, 26, 1583–1587. [Google Scholar] [CrossRef]
- Lai, J.; Ma, S.; Wang, Y.; Cai, Z.; Hu, J.; Wei, N.; Wu, J.; Du, H.; Chen, T.; Li, R.; et al. Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Netw. Open 2020, 3, e203976. [Google Scholar] [CrossRef]
- Stojanov, J.; Malobabic, M.; Stanojevic, G.; Stevic, M.; Milosevic, V.; Stojanov, A. Quality of sleep and health-related quality of life among health care professionals treating patients with coronavirus disease-19. Int. J. Soc. Psychiatry 2021, 67, 175–181. [Google Scholar] [CrossRef]
- Manh Than, H.; Minh Nong, V.; Trung Nguyen, C.; Dong, K.P.; Ngo, H.T.; Doan, T.T.; Do, N.T.; Nguyen, T.H.T.; Van Do, T.; Dao, C.X.; et al. Mental Health and Health-Related Quality-of-Life Outcomes among Frontline Health Workers during the Peak of COVID-19 Outbreak in Vietnam: A Cross-Sectional Study. Risk Manag. Healthc. Policy 2020, 13, 2927–2936. [Google Scholar] [CrossRef]
- An, Y.; Yang, Y.; Wang, A.; Li, Y.; Zhang, Q.; Cheung, T.; Ungvari, G.S.; Qin, M.Z.; An, F.R.; Xiang, Y.T. Prevalence of depression and its impact on quality of life among frontline nurses in emergency departments during the COVID-19 outbreak. J. Affect. Disord. 2020, 276, 312–315. [Google Scholar] [CrossRef]
- Li, W.Q.; Yuan, P.; Sun, J.; Xu, M.L.; Wang, Q.X.; Ge, D.D.; Jiang, M.M.; Xing, L.Q.; Du, W.J.; Li, Q. Resilience, coping style, and COVID-19 stress: Effects on the quality of life in frontline health care workers. Psychol. Health Med. 2022, 27, 312–324. [Google Scholar] [CrossRef] [PubMed]
- Korkmaz, S.; Kazgan, A.; Çekiç, S.; Tartar, A.S.; Balcı, H.N.; Atmaca, M. The anxiety levels, quality of sleep and life and problem-solving skills in healthcare workers employed in COVID-19 services. J. Clin. Neurosci. 2020, 80, 131–136. [Google Scholar] [CrossRef] [PubMed]
- Korkut, S. Research on the frequency of post-traumatic stress disorder in healthcare workers during the COVID-19 pandemic. Ir. J. Med. Sci. 2021, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Palacios-Ceña, D.; Fernández-de-Las-Peñas, C.; Florencio, L.L.; de-la-Llave-Rincón, A.I.; Palacios-Ceña, M. Emotional Experience and Feelings during First COVID-19 Outbreak Perceived by Physical Therapists: A Qualitative Study in Madrid, Spain. Int. J. Environ. Res. Public Health 2020, 18, 127. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.; Kwak, S.G.; Ko, E.J.; Chang, M.C. The Mental Health Burden of the COVID-19 Pandemic on Physical Therapists. Int. J. Environ. Res. Public Health 2020, 17, 3723. [Google Scholar] [CrossRef]
- Chigwedere, O.C.; Sadath, A.; Kabir, Z.; Arensman, E. The Impact of Epidemics and Pandemics on the Mental Health of Healthcare Workers: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 6695. [Google Scholar] [CrossRef]
- Woon, L.S.; Mansor, N.S.; Mohamad, M.A.; Teoh, S.H.; Leong Bin Abdullah, M.F.I. Quality of Life and Its Predictive Factors Among Healthcare Workers After the End of a Movement Lockdown: The Salient Roles of COVID-19 Stressors, Psychological Experience, and Social Support. Front. Psychol. 2021, 12, 652326. [Google Scholar] [CrossRef]
- World Health Organization. Constitution. Available online: https://www.who.int/about/governance/constitution (accessed on 12 October 2021).
- Notaras, M.; van den Buuse, M. Neurobiology of BDNF in fear memory, sensitivity to stress, and stress-related disorders. Mol. Psychiatry 2020, 25, 2251–2274. [Google Scholar] [CrossRef]
- Albott, C.S.; Wozniak, J.R.; McGlinch, B.P.; Wall, M.H.; Gold, B.S.; Vinogradov, S. Battle Buddies: Rapid Deployment of a Psychological Resilience Intervention for Health Care Workers During the COVID-19 Pandemic. Anesth. Analg. 2020, 131, 43–54. [Google Scholar] [CrossRef]
- Ding, J.; Jia, Y.; Zhao, J.; Yang, F.; Ma, R.; Yang, X. Optimizing quality of life among Chinese physicians: The positive effects of resilience and recovery experience. Qual. Life Res. 2020, 29, 1655–1663. [Google Scholar] [CrossRef]
- Hirten, R.P.; Danieletto, M.; Tomalin, L.; Choi, K.H.; Zweig, M.; Golden, E.; Kaur, S.; Helmus, D.; Biello, A.; Pyzik, R.; et al. Factors Associated With Longitudinal Psychological and Physiological Stress in Health Care Workers During the COVID-19 Pandemic: Observational Study Using Apple Watch Data. J. Med. Internet Res. 2021, 23, e31295. [Google Scholar] [CrossRef] [PubMed]
- Cohn, M.A.; Fredrickson, B.L.; Brown, S.L.; Mikels, J.A.; Conway, A.M. Happiness unpacked: Positive emotions increase life satisfaction by building resilience. Emotion 2009, 9, 361–368. [Google Scholar] [CrossRef] [PubMed]
- Kim, E.J.; Lim, J.Y.; Kim, G.M.; Kim, S.K. Nursing Students’ Subjective Happiness: A Social Network Analysis. Int. J. Environ. Res. Public Health 2021, 18, 11612. [Google Scholar] [CrossRef] [PubMed]
- Satici, S.A.; Kayis, A.R.; Satici, B.; Griffiths, M.D.; Can, G. Resilience, Hope, and Subjective Happiness among the Turkish Population: Fear of COVID-19 as a Mediator. Int. J. Ment. Health Addict. 2020, 18, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Satici, S.A. Psychological vulnerability, resilience, and subjective well-being: The mediating role of hope. Personal. Individ. Differ. 2016, 102, 68–73. [Google Scholar] [CrossRef]
- Magnavita, N.; Soave, P.M.; Antonelli, M. A One-Year Prospective Study of Work-Related Mental Health in the Intensivists of a COVID-19 Hub Hospital. Int. J. Environ. Res. Public Health 2021, 18, 9888. [Google Scholar] [CrossRef]
- Carmassi, C.; Foghi, C.; Dell’Oste, V.; Cordone, A.; Bertelloni, C.A.; Bui, E.; Dell’Osso, L. PTSD symptoms in healthcare workers facing the three coronavirus outbreaks: What can we expect after the COVID-19 pandemic. Psychiatry Res. 2020, 292, 113312. [Google Scholar] [CrossRef]
- Spilg, E.G.; Rushton, C.H.; Phillips, J.L.; Kendzerska, T.; Saad, M.; Gifford, W.; Gautam, M.; Bhatla, R.; Edwards, J.D.; Quilty, L.; et al. The new frontline: Exploring the links between moral distress, moral resilience and mental health in healthcare workers during the COVID-19 pandemic. BMC Psychiatry 2022, 22, 19. [Google Scholar] [CrossRef]
- Pollock, A.; Campbell, P.; Cheyne, J.; Cowie, J.; Davis, B.; McCallum, J.; McGill, K.; Elders, A.; Hagen, S.; McClurg, D.; et al. Interventions to support the resilience and mental health of frontline health and social care professionals during and after a disease outbreak, epidemic, or pandemic: A mixed methods systematic review. Cochrane Database Syst. Rev. 2020, 11, CD013779. [Google Scholar]
- Baskin, R.G.; Bartlett, R. Healthcare worker resilience during the COVID-19 pandemic: An integrative review. J. Nurs. Manag. 2021, 29, 2329–2342. [Google Scholar] [CrossRef]
- Abo-Ali, E.A.; Al-Rubaki, S.; Lubbad, S.; Nchoukati, M.; Alqahtani, R.; Albraim, S.; Ghareeb, W.A.; Al-Haffashi, B.; Alghamdi, F.; Zaytoun, S. Mental Well-Being and Self-Efficacy of Healthcare Workers in Saudi Arabia During the COVID-19 Pandemic. Risk Manag. Healthc. Policy 2021, 14, 3167–3177. [Google Scholar] [CrossRef] [PubMed]
- Rajkumar, R.P. Harnessing the Neurobiology of Resilience to Protect the Mental Well-Being of Healthcare Workers during the COVID-19 Pandemic. Front. Psychol. 2021, 12, 621853. [Google Scholar] [CrossRef]
- Franklin, P.; Gkiouleka, A. A Scoping Review of Psychosocial Risks to Health Workers during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 2453. [Google Scholar] [CrossRef] [PubMed]
- Rangachari, P.; LWoods, J. Preserving Organizational Resilience, Patient Safety, and Staff Retention during COVID-19 Requires a Holistic Consideration of the Psychological Safety of Healthcare Workers. Int. J. Environ. Res. Public Health 2020, 17, 4267. [Google Scholar] [CrossRef] [PubMed]
- Alhalaiqa, F.N.; Khalifeh, A.H.; Al Omari, O.; Yehia, D.B.; Khalil, M.M.H. Psychological Problems in a Sample of Jordanian Healthcare Workers Involved in Caring for Patients With COVID-19: A Cross-Sectional Study. Front. Psychol. 2021, 12, 679785. [Google Scholar] [CrossRef]
| Variables | Low Resilience (N = 145) | High Resilience (N = 374) | p Value |
|---|---|---|---|
| Age, n (%) | |||
| 20–30 years | 35 (28.9) | 115 (35.7) | 0.135 |
| 31–40 years | 63 (52.1) | 161 (50.0) | 0.933 |
| 41–50 years | 20 (16.5) | 39 (12.1) | 0.284 |
| 51–60 years | 3 (2.5) | 7 (2.2) | 0.857 |
| Female, n (%) | 127 (87.6) | 327 (87.4) | 0.975 |
| Pregnancy status, n (%) | 3 (2.1) | 10 (2.7) | 0.733 |
| Marital status, n (%) | |||
| Married | 41 (33.9) | 132 (41.0) | 0.128 |
| Divorced | 7 (5.8) | 13 (4.0) | 0.312 |
| Separated | 1 (0.8) | 1 (0.3) | 0.558 |
| Not married | 59 (48.8) | 150 (46.6) | 0.901 |
| Stable union | 11 (9.1) | 23 (7.1) | 0.867 |
| Others | 2 (1.7) | 3 (0.9) | 0.565 |
| Has children, n (%) | 43 (35.5) | 122 (37.7) | 0.519 |
| Family members living together, n % | |||
| Seniors | 25 (17.2) | 73 (19.5) | 0.560 |
| Children | 52 (35.9) | 135 (36.1) | 0.963 |
| Death in family or close friends due to COVID-19, n (%) | 48 (33.1) | 103 (27.5) | 0.214 |
| Graduation time, n (%) | |||
| ˂5 years | 34 (23.4) | 85 (22.7) | 0.854 |
| 5–10 years | 54 (37.2) | 119 (31.8) | 0.242 |
| 11–20 years | 48 (33.1) | 150 (40.1) | 0.141 |
| 21–30 years | 9 (6.2) | 20 (5.3) | 0.692 |
| Physical activity, n (%) | |||
| Practice of regular physical activity * | 64 (44.1) | 203 (54.3) | 0.038 |
| Physical activity during the pandemic period | 17 (13.3) | 63 (18.5) | 0.146 |
| Medical history, n (%) | |||
| Previous chronic disease | 28 (19.3) | 57 (15.2) | 0.266 |
| Absence from work due to other diseases | 19 (13.1) | 47 (12.6) | 0.858 |
| COVID-19 diagnosis | 33 (22.8) | 98 (26.2) | 0.422 |
| Needed hospitalization due to COVID-19 | 5 (3.4) | 5 (1.3) | 0.147 |
| Nature of the institution where they work, n (%) | |||
| Public | 53 (39.0) | 114 (35.7) | 0.187 |
| Private | 50 (36.8) | 108 (33.9) | 0.216 |
| Both | 33 (24.3) | 97 (30.4) | 0.458 |
| Removed from work due to, n (%) | |||
| Pregnancy | 2 (8.7) | 5 (11.9) | 0.932 |
| A chronic disease | 3 (13.0) | 2 (4.8) | 0.158 |
| Adapted to work at home office | 0 | 2 (4.8) | . a |
| Other reasons | 18 (78.3) | 33 (78.6) | 0.226 |
| The hospital sector where they work, n (%) | |||
| Critical care unit | 110 (75.9) | 264 (70.6) | 0.231 |
| Semi intensive unit | 4 (2.8) | 13 (3.5) | 0.714 |
| Ward | 25 (17.2) | 71 (19.0) | 0.655 |
| Emergency room | 2 (1.4) | 6 (1.6) | 0.900 |
| Supervisor occupations | 2 (1.4) | 11 (2.9) | 0.330 |
| Ambulatory medicine | 2 (1.4) | 9 (2.4) | 0.506 |
| Weekly workload, n (%) | |||
| ˂20 h | 2 (1.4) | 6 (1.6) | 0.900 |
| 20–30 h | 64 (44.8) | 155 (41.6) | 0.578 |
| 31–40 h | 32 (22.4) | 100 (26.8) | 0.210 |
| 41–50 h | 13 (9.1) | 32 (8.6) | 0.868 |
| 51–60 h | 24 (16.8) | 47 (12.6) | 0.242 |
| ˃60 h | 8 (5.6) | 33 (8.8) | 0.212 |
| Wage/income in R$, n (%) | |||
| ˂1.500,00 | 2 (1.4) | 6 (1.6) | 0.900 |
| 1.500,00–3.000,00 | 29 (20.1) | 70 (18.8) | 0.733 |
| 3.000,00–5.000,00 | 72 (50.0) | 184 (49.3) | 0.925 |
| 5.000,00–7.000,00 | 27 (18.8) | 79 (21.2) | 0.533 |
| ˃7.000,00 | 14 (9.7) | 34 (9.1) | 0.829 |
| Salary reduction during the pandemic, n (%) | 25 (17.2) | 84 (22.5) | 0.190 |
| Support for coping with the pandemic, n (%) | |||
| Received personal protective equipment | 136 (93.8) | 358 (95.7) | 0.366 |
| Received host leadership * | 83 (57.2) | 263 (70.3) | 0.005 |
| Received training * | 107 (73.8) | 307 (82.1) | 0.038 |
| Variables | NO COVID (N = 74) | COVID (N = 445) | p Value |
|---|---|---|---|
| Age, n (%) | |||
| 20–30 years | 22 (36.1) | 128 (33.5) | 0.856 |
| 31–40 years | 31 (50.8) | 193 (50.5) | 0.816 |
| 41–50 years | 6 (9.8) | 53 (13.9) | 0.351 |
| 51–60 years | 2 (3.3) | 8 (2.1) | 0.588 |
| Female, n (%) | 68 (91.9) | 386 (86.7) | 0.215 |
| Pregnancy status, n (%) ** | 7 (9.5) | 6 (1.3) | 0.000 |
| Marital status, n (%) | |||
| Married | 18 (29.5) | 155 (40.6) | 0.073 |
| Divorced | 2 (3.3) | 18 (4.7) | 0.632 |
| Separated | 1 (1.6) | 1 (0.3) | 0.285 |
| Not married | 33 (54.1) | 176 (46.1) | −0.415 |
| Stable union | 6 (9.8) | 28 (7.3) | 0.549 |
| Others | 1 (1.6) | 4 (1.0) | 0.688 |
| Has children, n (%) | 23 (37.1) | 142 (37.1) | 0.897 |
| Family members living together, n (%) | |||
| Seniors | 13 (17.6) | 85 (19.1) | 0.774 |
| Children ** | 40 (54.1) | 147 (33.0) | 0.000 |
| Death in family or close friends due to COVID-19, n (%) | 22 (29.7) | 129 (29) | 0.887 |
| Graduation time, n (%) | |||
| ˂5 years | 13 (17.6) | 106 (23.8) | 0.237 |
| 5–10 years * | 14 (18.9) | 159 (35.7) | 0.003 |
| 11–20 years * | 38 (51.4) | 160 (36.0) | 0.013 |
| 21–30 years * | 9 (12.2) | 20 (4.5) | 0.017 |
| Physical activity, n (%) | |||
| Practice of regular physical activity | 40 (54.1) | 227 (51) | 0.631 |
| Physical activity during the pandemic * | 19 (27.9) | 61 (15.3) | 0.013 |
| Medical history, n (%) | |||
| Previous chronic disease | 12 (16.2) | 73 (16.4) | 0.989 |
| Absence from work due to other diseases * | 2 (2.7) | 64 (14.4) | 0.001 |
| COVID-19 diagnosis | 15 (20.3) | 116 (26.1) | 0.291 |
| Needed hospitalization due to COVID-19 | 1 (1.4) | 9 (2) | 0.782 |
| Nature of the institution where they work, n (%) | |||
| Public | 15 (26.3) | 152 (38.2) | 0.142 |
| Private * | 28 (49.1) | 130 (32.7) | 0.015 |
| Both | 14 (24.6) | 116 (29.1) | 0.188 |
| Removed from work due to, n (%) | |||
| Pregnancy ** | 5 (35.7) | 2 (3.9) | 0.000 |
| A chronic disease | 2 (14.3) | 3 (5.9) | 0.173 |
| Adapted to work at home office | 1 (7.1) | 1 (2.0) | 0.285 |
| Other reasons | 6 (42.9) | 45 (88.2) | 0.620 |
| The hospital sector where they work, n (%) | |||
| Critical care unit ** | 26 (35.1) | 348 (78.2) | 0.000 |
| Semi intensive unit | 4 (5.4) | 13 (2.9) | 0.293 |
| Ward ** | 30 (40.5) | 66 (14.8) | 0.000 |
| Emergency room | 0 | 8 (1.8) | . a |
| Supervisor occupations * | 5 (6.8) | 8 (1.8) | 0.031 |
| Ambulatory medicine ** | 9 (12.2) | 2 (0.4) | 0.000 |
| Weekly workload, n (%) | |||
| ˂20 h | 2 (2.7) | 6 (1.4) | 0.410 |
| 20–30 h | 38 (52.1) | 181 (40.9) | 0.088 |
| 31–40 h | 19 (26.0) | 113 (25.5) | 0.946 |
| 41–50 h | 9 (12.3) | 36 (8.1) | 0.263 |
| 51–60 h * | 3 (4.1) | 68 (15.3) | 0.004 |
| ˃60 h | 2 (2.7) | 39 (8.8) | 0.060 |
| Wage/income in R$, n (%) | |||
| ˂1500,00 | 0 | 8 (1.8) | . a |
| 1.500,00–3.000,00 | 18 (24.7) | 81 (18.2) | 0.223 |
| 3.000,00–5.000,00 | 30 (41.1) | 226 (50.9) | 0.104 |
| 5.000,00–7.000,00 | 12 (16.4) | 94 (21.2) | 0.338 |
| ˃7.000,00 * | 13 (17.8) | 35 (7.9) | 0.014 |
| Salary reduction during the pandemic, n (%) * | 22 (29.7) | 87 (19.6) | 0.047 |
| Support for coping with the pandemic, n (%) | |||
| Received personal protective equipment | 74 (100) | 420 (94.4) | . a |
| Received host leadership ** | 62 (83.8) | 284 (63.8) | 0.000 |
| Received training | 61 (82.4) | 353 (79.3) | 0.522 |
| SF-36 (Question 2) | |||
|---|---|---|---|
| Resilience | Low | High | p Value |
| 3 (3–4) | 3 (2–4) | <0.001 | |
| Works with COVID-19 patients | No | Yes | |
| 3 (2–3) | 3 (3–4) | <0.001 | |
| Resilience | |||
|---|---|---|---|
| Low | High | p Value | |
| 36-item Short Form Health Survey (SF-36) % | |||
| Physical functioning | 80 (60–90) | 90 (75–100) | <0.001 |
| Role-physical | 50 (25–100) | 75 (25–100) | <0.001 |
| Bodily pain | 51 (41–62) | 62 (51–84) | <0.001 |
| General health | 60 (50–73) | 72 (60–82) | <0.001 |
| Vitality | 35 (20–45) | 50 (35–65) | <0.001 |
| Social functioning | 50 (37–50) | 50 (37–50) | 0.163 |
| Role-emotional | 33 (0–66) | 100 (91–100) | <0.001 |
| Mental health | 44 (36–52) | 66 (0–100) | <0.001 |
| Subjective Happiness Scale (SHS) | 4.25 (3.62–5.00) | 5.50 (5.00–6.25) | <0.001 |
| Resilience | 67 (60–71) | 86 (80–97) | <0.001 |
| Works in COVID-19 | |||
|---|---|---|---|
| No | Yes | p Value | |
| 36-item Short Form Health Survey (SF-36) % | |||
| Physical functioning | 95 (85–100) | 85 (70–95) | <0.001 |
| Role-physical | 100 (75–100) | 50 (25–100) | <0.001 |
| Bodily pain | 84 (62–100) | 51 (41–72) | <0.001 |
| General health | 80 (61–90) | 67 (55–77) | <0.001 |
| Vitality | 65 (55–80) | 40 (30–55) | <0.001 |
| Social functioning | 50 (37–50) | 50 (37–50) | 0.638 |
| Role-emotional | 100 (91–100) | 33 (0–100) | <0.001 |
| Mental health | 82 (68–92) | 52 (44–64) | <0.001 |
| Subjective Happiness Scale (SHS) | 6.12 (5.25–6.75) | 5.00 (4.25–5.75) | <0.001 |
| Resilience | 90 (84–95) | 80 (72–88) | <0.001 |
| Outcomes | Unadjusted B (SE) | Adjusted B (SE) # | ||||
|---|---|---|---|---|---|---|
| Resilience | COVID | ΔR2 (Resilience + COVID) | Resilience | COVID | Total R2 | |
| Physical functioning | 8.284 (2.112) ** | −6.354 (2.694) * | 0.058 | 7.300 (2.068) ** | −4.181 (2.664) | 0.140 |
| Role physical | 13.152 (4.128) * | −29,667 (5.226) ** | 0.110 | 12.350 (4.102) * | −25.289 (5.285) ** | 0.162 |
| Bodily pain | 7.748 (2.420) ** | −18.442 (3.088) ** | 0.119 | 6.934 (2.401) * | −15.553 (3.094) ** | 0.174 |
| General health | 8.850 (1.820) ** | −7.255 (2.322) * | 0.100 | 7.894 (1.771) ** | −4.983 (2.282) | 0.179 |
| Vitality | 13.879 (1.956) ** | −22.417 (2.495) ** | 0.282 | 12.544 (1.903) ** | −19.350 (2.452) ** | 0.352 |
| Social functioning | −2.475 (1.600) | 2.332 (2.041) | 0.011 | −2.358 (1.634) | 2.515 (2.105) | 0.017 |
| Role emotional | 19.102(4.487) ** | −39.314(5.724) ** | 0.162 | 17.994 (4.463) | −34.649 (5.750) | 0.210 |
| Mental health | 16.541 (1.159) ** | −21.619 (2.243) ** | 0.353 | 14.935 (1.664) ** | −18.260 (2.143) | 0.448 |
| Happiness | 0.056 (0.004) ** | −0.469 (0.129) ** | 0.403 | 0.053 (0.004) ** | −0.363 (0.129) * | 0.438 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pigati, P.A.d.S.; Righetti, R.F.; Dourado, V.Z.; Nisiaymamoto, B.T.C.; Saraiva-Romanholo, B.M.; Tibério, I.d.F.L.C. Resilience Improves the Quality of Life and Subjective Happiness of Physiotherapists during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2022, 19, 8720. https://doi.org/10.3390/ijerph19148720
Pigati PAdS, Righetti RF, Dourado VZ, Nisiaymamoto BTC, Saraiva-Romanholo BM, Tibério IdFLC. Resilience Improves the Quality of Life and Subjective Happiness of Physiotherapists during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2022; 19(14):8720. https://doi.org/10.3390/ijerph19148720
Chicago/Turabian StylePigati, Patricia Angeli da Silva, Renato Fraga Righetti, Victor Zuniga Dourado, Bruna Tiemi Cunha Nisiaymamoto, Beatriz Mangueira Saraiva-Romanholo, and Iolanda de Fátima Lopes Calvo Tibério. 2022. "Resilience Improves the Quality of Life and Subjective Happiness of Physiotherapists during the COVID-19 Pandemic" International Journal of Environmental Research and Public Health 19, no. 14: 8720. https://doi.org/10.3390/ijerph19148720
APA StylePigati, P. A. d. S., Righetti, R. F., Dourado, V. Z., Nisiaymamoto, B. T. C., Saraiva-Romanholo, B. M., & Tibério, I. d. F. L. C. (2022). Resilience Improves the Quality of Life and Subjective Happiness of Physiotherapists during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health, 19(14), 8720. https://doi.org/10.3390/ijerph19148720





