Self-Testing as a Hope to Reduce HIV in Transgender Women—Literature Review
Abstract
:1. Introduction
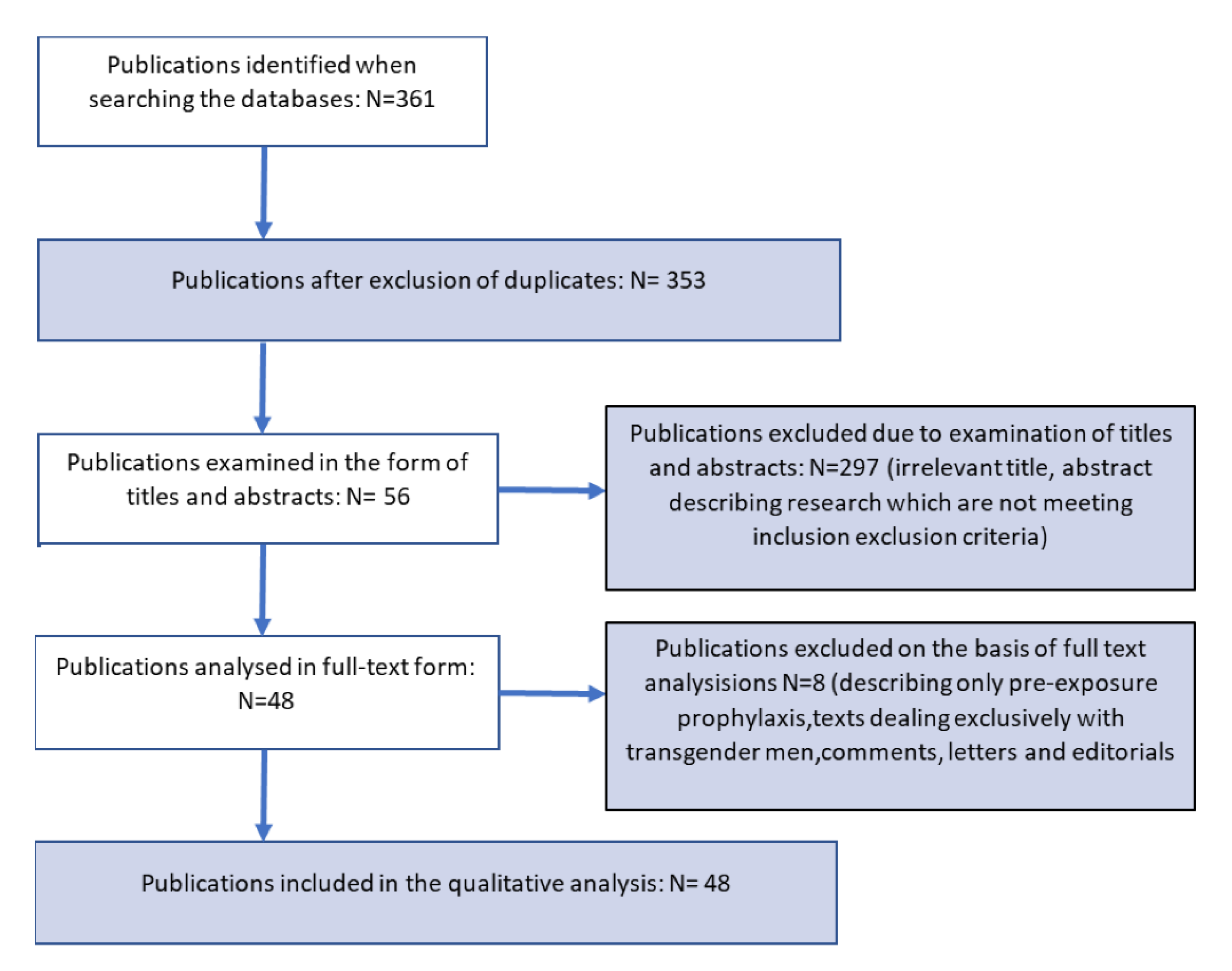
2. Material and Methods
3. Results
3.1. Details of the Studied Population
3.2. Definition and Types of Tests
3.3. Does TGW Know and Apply HIV Tests?
3.4. Motivating and Demotivating Factors for Self-Testing
3.5. Advantages of Self-Testing
3.6. Disadvantages of Self-Testing
3.7. Future Actions Concerning HIV Self-Testing
3.8. Combined HIV and Syphilis Testing
4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- 2020 Global AIDS Update—Seizing the Moment—Tackling Entrenched Inequalities to End Epidemics|UNAIDS. Available online: https://www.unaids.org/en/resources/documents/2020/global-aids-report (accessed on 9 June 2022).
- Baral, S.D.; Poteat, T.; Strömdahl, S.; Wirtz, A.L.; Guadamuz, T.E.; Beyrer, C. Worldwide burden of HIV in transgender women: A systematic review and meta-analysis. Lancet Infect Dis. 2013, 13, 214–222. [Google Scholar] [CrossRef]
- Lacombe-Duncan, A.; Logie, C.H.; Persad, Y.; Leblanc, G.; Nation, K.; Kia, H.; Scheim, A.I.; Lyons, T.; Horemans, C.; Olawale, R.; et al. Implementation and evaluation of the ‘Transgender Education for Affirmative and Competent HIV and Healthcare (TEACHH)’ provider education pilot. BMC Med. Educ. 2021, 21, 561. [Google Scholar] [CrossRef] [PubMed]
- Sandfort, T.G.; Hamilton, E.; Marais, A.; Guo, X.; Sugarman, J.; Chen, Y.Q.; Cummings, V.; Dadabhai, S.; Dominguez, K.; Panchia, R.; et al. The feasibility of recruiting and retaining men who have sex with men and transgender women in a multinational prospective HIV prevention research cohort study in sub-Saharan Africa (HPTN 075). J. Int. AIDS Soc. 2020, 23 (Suppl. S6), e25600. [Google Scholar] [CrossRef]
- Kaplan, R.L.; El Khoury, C.; Wehbe, S.; Lize, N.; Mokhbat, J. Pilot Results from the First HIV/AIDS Intervention AMONG Transgender Women in the Middle East: Gender Affirmation and Social Support from Within Trans Communities in Beirut, Lebanon. AIDS Res. Hum. Retrovir. 2020, 36, 501. [Google Scholar] [CrossRef] [PubMed]
- Kuhns, L.M.; Hereth, J.; Garofalo, R.; Hidalgo, M.; Johnson, A.K.; Schnall, R.; Reisner, S.L.; Belzer, M.; Mimiaga, M.J. A Uniquely Targeted, Mobile App-Based HIV Prevention Intervention for Young Transgender Women: Adaptation and Usability Study. J. Med. Internet Res. 2021, 23, e21839. [Google Scholar] [CrossRef] [PubMed]
- Calin, R.; Massari, V.; Pialoux, G.; Reydellet, N.; Plenel, E.; Chauvin, C.; Jauffret-Roustide, M.; Day, N.; Kreplak, G.; Maresca, A.F.; et al. Acceptability of on-site rapid HIV/HBV/HCV testing and HBV vaccination among three at-risk populations in distinct community-healthcare outreach centres: The ANRS-SHS 154 CUBE study. BMC Infect Dis. 2020, 20, 1–14. [Google Scholar] [CrossRef]
- Sok, S.; Hong, R.; Chhoun, P.; Chann, N.; Tuot, S.; Mun, P.; Brody, C.; Yi, S. HIV risks and recent HIV testing among transgender women in Cambodia: Findings from a national survey. PLoS ONE 2020, 15, e0238314. [Google Scholar] [CrossRef]
- Dijkstra, M.; Mohamed, K.; Kigoro, A.; Mumba, T.; Mahmoud, S.; Wesonga, A.; Mukuria, N.; Oduor, T.; Gichuru, E.; van der Loeff, M.F.S.; et al. Peer Mobilization and Human Immunodeficiency Virus (HIV) Partner Notification Services among Gay, Bisexual, and Other Men Who Have Sex With Men and Transgender Women in Coastal Kenya Identified a High Number of Undiagnosed HIV Infections. Open Forum Infect Dis. 2021, 8, ofab219. [Google Scholar] [CrossRef]
- Callander, D.; Schneider, J.A.; Radix, A.; Chaix, B.; Scheinmann, R.; Love, G.; Smith, J.; Regan, S.D.; Kawachi, I.; James, K.S.; et al. Longitudinal cohort of HIV-negative transgender women of colour in New York City: Protocol for the TURNNT (‘Trying to Understand Relationships, Networks and Neighbourhoods among Transgender women of colour’) study. BMJ Open 2020, 10, e032876. [Google Scholar] [CrossRef] [Green Version]
- Da Rocha, A.B.M.; Barros, C.; Generoso, I.P.; Bastos, F.I.; Veras, M.A. HIV continuum of care among trans women and travestis living in São Paulo, Brazil. Rev. Saude Publica 2020, 54, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Mujugira, A.; Nakyanzi, A.; Nabaggala, M.S.; Muwonge, T.R.; Ssebuliba, T.; Bagaya, M.; Nampewo, O.; Sapiri, O.; Nyanzi, K.R.; Bambia, F.; et al. Effect of HIV Self-Testing on PrEP Adherence among Gender-Diverse Sex Workers in Uganda: A Randomized Trial. J. Acquir. Immune Defic. Syndr. 2022, 89, 381. [Google Scholar] [CrossRef] [PubMed]
- Wood, O.R.; Garofalo, R.; Kuhns, L.M.; Scherr, T.F.; Zetina, A.P.M.; Rodriguez, R.G.; Nash, N.; Cervantes, M.; Schnall, R. A randomized controlled trial of an mHealth intervention for increasing access to HIV testing and care among young cisgender men and transgender women: The mLab App study protocol. BMC Public Health. 2021, 21, 1959. [Google Scholar] [CrossRef] [PubMed]
- Shrestha, R.K.; Sansom, S.L.; Schulden, J.D.; Song, B.; Smith, L.C.; Ramírez, R.; Mares-DelGrasso, A.; Heffelfinger, J.D. Costs and effectiveness of finding new HIV diagnoses by using rapid testing in transgender communities. AIDS Educ Prev. 2011, 23 (Suppl. S3), 49–57. [Google Scholar] [CrossRef]
- Garofalo, R.; Kuhns, L.M.; Reisner, S.L.; Mimiaga, M.J. Behavioral Interventions to Prevent HIV Transmission and Acquisition for Transgender Women: A Critical Review. J. Acquir. Immune Defic. Syndr. 2016, 72 (Suppl. S3). [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hall, H.I.; Song, R.; Rhodes, P.; Prejean, J.; An, Q.; Lee, L.M.; Karon, J.; Brookmeyer, R.; Kaplan, E.H.; McKenna, M.T.; et al. Estimation of HIV Incidence in the United States. JAMA 2008, 300, 520–529. [Google Scholar] [CrossRef] [Green Version]
- Mayer, K.H.; Grinsztejn, B.; El-Sadr, W.M. Transgender People and HIV Prevention: What We Know and What We Need to Know, a Call to Action. J. Acquir. Immune Defic. Syndr. 2016, 72 (Suppl. S3). [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pitasi, M.A.; Oraka, E.; Clark, H.; Town, M.; DiNenno, E.A. HIV Testing among Transgender Women and Men—27 States and Guam, 2014–2015. MMWR Morb. Mortal Wkly Rep. 2019, 66, 883–887. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Becasen, J.S.; Denard, C.L.; Mullins, M.M.; Higa, D.H.; Sipe, T.A. Estimating the prevalence of HIV and sexual behaviors among the US transgender population: A systematic review and meta-analysis, 2006–2017. Am. J. Public Health 2019, 109, E1–E8. [Google Scholar] [CrossRef]
- Town, K.; Tie, Y.; Dasgupta, S.; Kirkcaldy, R.D.; Crim, S.M.; Weiser, J.; Bernstein, K. Sexually Transmitted Infection Testing among Transgender Women Living with Human Immunodeficiency Virus in the United States: Medical Monitoring Project, 2015–2019. Clin. Infect Dis. 2021, 73, 899–902. [Google Scholar] [CrossRef]
- Rosenberg, E.S.; Grey, J.A.; Sanchez, T.H.; Sullivan, P.S. Rates of Prevalent HIV Infection, Prevalent Diagnoses, and New Diagnoses among Men Who Have Sex With Men in US States, Metropolitan Statistical Areas, and Counties, 2012–2013. JMIR Public Health Surveill. 2016, 2, e22. [Google Scholar] [CrossRef] [Green Version]
- Dolezal, C.; Rael, C.T.; Balán, I.C.; Giguere, R.; Lentz, C.; Lopez-Rios, J.; Sheinfil, A.Z.; Febo, I.; Carballo-Diéguez, A. Substance Use and Testing Sexual Partners Using HIV Self-tests. AIDS Behav. 2020, 24, 2856–2862. [Google Scholar] [CrossRef]
- Wirtz, A.L.; Clouse, E.; Veronese, V.; Thu, K.H.; Naing, S.; Baral, S.; Beyrer, C. New HIV testing technologies in the context of a concentrated epidemic and evolving HIV prevention: Qualitative research on HIV self-testing among men who have sex with men and transgender women in Yangon, Myanmar. J. Int. AIDS Soc. 2017, 20, 21796. [Google Scholar] [CrossRef]
- van Griensven, F.; Janamnuaysook, R.; Nampaisan, O.; Peelay, J.; Samitpol, K.; Mills, S.; Pankam, T.; Ramautarsing, R.; Teeratakulpisarn, N.; Phanuphak, P.; et al. Uptake of Primary Care Services and HIV and Syphilis Infection among Transgender Women attending the Tangerine Community Health Clinic, Bangkok, Thailand, 2016–2019. J. Int. AIDS Soc. 2021, 24, e25683. [Google Scholar] [CrossRef] [PubMed]
- Johnson, C.C.; Baggaley, R.; Forsythe, S.; Van Rooyen, H.; Ford, N.; Napierala Mavedzenge, S.; Corbett, E.; Natarajan, P.; Taegtmeyer, M. Realizing the Potential for HIV Self-Testing. AIDS Behav. 2014, 18, 391–395. [Google Scholar] [CrossRef] [PubMed]
- HIV Testing|HIV/AIDS|CDC. Available online: https://www.cdc.gov/hiv/testing/index.html (accessed on 9 June 2022).
- Frye, V.; Nandi, V.; Hirshfield, S.; Chiasson, M.A.; Wilton, L.; Usher, D.; Hoover, D.R.; Koblin, B.A. Randomized controlled trial of an intervention to match young Black men and transwomen who have sex with men or transwomen to HIV testing options in New York City (All About Me). J. Acquir. Immune Defic. Syndr. 2020, 83, 31. [Google Scholar] [CrossRef] [PubMed]
- Witzel, T.; Bourne, A.; Burns, F.; Rodger, A.; McCabe, L.; Gabriel, M.; Gafos, M.; Ward, D.; Collaco-Moraes, Y.; Dunn, D.; et al. HIV self-testing intervention experiences and kit usability: Results from a qualitative study among men who have sex with men in the SELPHI (Self-Testing Public Health Intervention) randomized controlled trial in England and Wales. HIV Med. 2020, 21, 189. [Google Scholar] [CrossRef] [PubMed]
- Witzel, T.C.; Wright, T.; McCabe, L.; Gabriel, M.M.; Wolton, A.; Gafos, M.; Ward, D.; Lampe, F.C.; Phillips, A.N.; Trevelion, R.; et al. Impact and acceptability of HIV self-testing for trans men and trans women: A mixed-methods subgroup analysis of the SELPHI randomised controlled trial and process evaluation in England and Wales. EClinicalMedicine 2021, 32, 100700. [Google Scholar] [CrossRef]
- Lentz, C.; Iribarren, S.; Giguere, R.; Conserve, D.F.; Dolezal, C.; Lopez-Rios, J.; Balán, I.C.; Sheinfil, A.Z.; Rael, C.T.; Brown, W.; et al. Broaching the Topic of HIV Self-testing with Potential Sexual Partners among Men and Transgender Women Who Have Sex with Men in New York and Puerto Rico. AIDS Behav. 2020, 24, 3033–3043. [Google Scholar] [CrossRef]
- Akinola, M.; Wirtz, A.L.; Chaudhry, A.; Cooney, E.; Reisner, S.L. American Cohort to Study HIV Acquisition among Transgender Women. Perceived acceptability and feasibility of HIV self-testing and app-based data collection for HIV prevention research with transgender women in the United States. AIDS Care 2021, 33, 1079–1087. [Google Scholar] [CrossRef]
- Bilardi, J.E.; Walker, S.; Read, T.; Prestage, G.; Chen, M.Y.; Guy, R.; Bradshaw, C.; Fairley, C.K. Gay and Bisexual Men’s Views on Rapid Self-Testing for HIV. AIDS Behav. 2013, 17, 2093–2099. [Google Scholar] [CrossRef]
- Carballo-Diéguez, A.; Frasca, T.; Balan, I.; Ibitoye, M.; Dolezal, C. Use of a rapid HIV home test prevents HIV exposure in a high risk sample of men who have sex with men. AIDS Behav. 2012, 16, 1753–1760. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Figueroa, C.; Johnson, C.; Verster, A.; Baggaley, R. Attitudes and Acceptability on HIV Self-testing among Key Populations: A Literature Review. AIDS Behav. 2015, 19, 1949. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lippman, S.; Lane, T.; Rabede, O.; Gilmore, H.; Chen, Y.-H.; Mlotshwa, N.; Maleke, K.; Marr, A.; McIntyre, J.A. High Acceptability and Increased HIV Testing Frequency Following Introduction of HIV Self-Testing and Network Distribution among South African MSM. J. Acquir. Immune Defic. Syndr. 2018, 77, 279. [Google Scholar] [CrossRef] [PubMed]
- Pal, K.; Ngin, C.; Tuot, S.; Chhoun, P.; Ly, C.; Chhim, S.; Luong, M.-A.; Tatomir, B.; Yi, S. Acceptability Study on HIV Self-Testing among Transgender Women, Men who Have Sex with Men, and Female Entertainment Workers in Cambodia: A Qualitative Analysis. PLoS ONE 2016, 11, e0166129. [Google Scholar] [CrossRef]
- Lina Rosengren, A.; Huang, E.; Daniels, J.; Young, S.D.; Marlin, R.W.; Klausner, J.D. Feasibility of using GrindrTM to distribute HIV self-test kits to men who have sex with men in Los Angeles, California. Sex. Health 2016, 13, 389–392. [Google Scholar] [CrossRef] [Green Version]
- Volk, J.E.; Lippman, S.; Grinsztejn, B.; Lama, J.R.; Fernandes, N.M.; Gonzales, P.; Hessol, N.A.; Buchbinder, S. Acceptability and feasibility of HIV self-testing among men who have sex with men in Peru and Brazil. Int. J. STD AIDS. 2016, 27, 531–536. [Google Scholar] [CrossRef] [Green Version]
- Yan, H.; Yang, H.; Raymond, H.F.; Li, J.; Shi, L.-E.; Huan, X.; Wei, C. Experiences and correlates of HIV self-testing among men who have sex with men in Jiangsu Province, China. AIDS Behav. 2015, 19, 485–491. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rael, C.T.; Giguere, R.; Lopez-Rios, J.; Lentz, C.; Balán, I.C.; Sheinfil, A.; Dolezal, C.; Brown, W.; Frasca, T.; Torres, C.C.; et al. Transgender Women’s Experiences Using a Home HIV-Testing Kit for Partner-Testing. AIDS Behav. 2020, 24, 2732–2741. [Google Scholar] [CrossRef]
- Girault, P.; Wong, C.M.; Jittjang, S.; Fongkaew, K.; Cassell, M.M.; Lertpiriyasuwat, C.; Vannakit, R.; Avery, M.; Linjongrat, D.; Sumalu, S.; et al. Uptake of oral fluid-based HIV self-testing among men who have sex with men and transgender women in Thailand. PLoS ONE 2021, 16, e0256094. [Google Scholar] [CrossRef]
- Stevens, D.R.; Vrana, C.J.; Dlin, R.E.; Korte, J.E. A Global Review of HIV Self-testing: Themes and Implications. AIDS Behav. 2018, 22, 497–512. [Google Scholar] [CrossRef]
- Muessig, K.E.; Golinkoff, J.M.; Hightow-Weidman, L.B.; Rochelle, A.E.; Mulawa, M.I.; Hirshfield, S.; Rosengren, A.L.; Aryal, S.; Buckner, N.; Wilson, M.S.; et al. Increasing HIV Testing and Viral Suppression via Stigma Reduction in a Social Networking Mobile Health Intervention among Black and Latinx Young Men and Transgender Women Who Have Sex With Men (HealthMpowerment): Protocol for a Randomized Controlled Trial. JMIR Res. Protoc. 2020, 9, e24043. [Google Scholar] [CrossRef] [PubMed]
- Hirshfield, S.; Teran, R.A.; Downing, M.J., Jr.; Chiasson, M.A.; Tieu, H.V.; Dize, L.; Gaydos, C.A. Quantification of HIV-1 RNA among Men Who Have Sex With Men Using an At-Home Self-Collected Dried Blood Spot Specimen: Feasibility Study. JMIR Public Health Surveill. 2018, 4, e10847. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Teran, R.A.; Sobieszczyk, M.E.; Chiasson, M.A.; Uhlemann, A.-C.; Weidler, J.; Shah, J.G.; Chang, J.Y.; Otto, C.; Hirshfield, S. Longitudinal Viral Load Monitoring Using Home-Collected Dried Blood Spot Specimens of MSM Living with HIV: Results from a Feasibility Pilot Study. AIDS Behav. 2021, 25, 661–666. [Google Scholar] [CrossRef]
- Gichangi, A.; Wambua, J.; Mutwiwa, S.; Njogu, R.; Bazant, E.; Wamicwe, J.; Wafula, R.; Vrana, C.J.; Stevens, D.R.; Mudany, M.; et al. Impact of HIV Self-Test Distribution to Male Partners of ANC Clients: Results of a Randomized Controlled Trial in Kenya. J. Acquir. Immune Defic. Syndr. 2018, 79, 467–473. [Google Scholar] [CrossRef] [PubMed]
- Masters, S.H.; Agot, K.; Obonyo, B.; Napierala Mavedzenge, S.; Maman, S.; Thirumurthy, H. Promoting Partner Testing and Couples Testing through Secondary Distribution of HIV Self-Tests: A Randomized Clinical Trial. PLOS Med. 2016, 13, e1002166. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Maman, S.; Murray, K.R.; Napierala Mavedzenge, S.; Oluoch, L.; Sijenje, F.; Agot, K.; Thirumurthy, H. A qualitative study of secondary distribution of HIV self-test kits by female sex workers in Kenya. PLoS ONE 2017, 12, e0174629. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Matovu, J.K.B.; Buregyeya, E.; Arinaitwe, J.; Wanyenze, R.K. ‘… if you bring the kit home, you [can] get time and test together with your partner’: Pregnant women and male partners’ perceptions regarding female partner-delivered HIV self-testing in Uganda—A qualitative study. Int. J. STD AIDS 2017, 28, 1341–1347. [Google Scholar] [CrossRef]
- Frola, C.E.; Zalazar, V.; Cardozo, N.; Vázquez, M.L.; Aristegui, I.; Lucas, M.; Gun, A.; Cahn, P.; Sued, O. Home-based HIV testing: Using different strategies among transgender women in Argentina. PLoS ONE 2020, 15, e0230429. [Google Scholar] [CrossRef] [Green Version]
- Parker, M.M.; Bennett, S.B.; Sullivan, T.J.; Fordan, S.; Wesolowski, L.G.; Wroblewski, K.; Gaynor, A.M. Performance of the Alere DetermineTM HIV-1/2 Ag/Ab Combo Rapid Test with algorithm-defined acute HIV-1 infection specimens. J. Clin. Virol. 2018, 104, 89–91. [Google Scholar] [CrossRef]
- Szeląg, H.; Wąż, K. Prevention and counseling for adults in the field of HIV / AIDS. Changing needs. Discourses Young -Dragogues 2015, 16, 115–127. [Google Scholar]
- Sevelius, J.M.; Poteat, T.; Luhur, W.E.; Reisner, S.L.; Meyer, I.H. HIV Testing and PrEP Use in a National Probability Sample of Sexually Active Transgender People in the United States. J. Acquir. Immune Defic. Syndr. 2020, 84, 437–442. [Google Scholar] [CrossRef] [PubMed]
- Bauer, G.R.; Travers, R.; Scanlon, K.; Coleman, T.A. High heterogeneity of HIV-related sexual risk among transgender people in Ontario, Canada: A province-wide respondent-driven sampling survey. BMC Public Health 2012, 12, 292. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reisner, S.L.; Mimiaga, M.J.; Skeer, M.; VanDerwarker, R.; Gaucher, M.J.; O’Connor, C.A.; Medeiros, M.S.; Safren, S.A. Differential HIV risk behavior among men who have sex with men seeking health-related mobile van services at diverse gay-specific venues. AIDS Behav. 2009, 13, 822–831. [Google Scholar] [CrossRef] [PubMed]
- Gyasi, R.M.; Abass, K. Sexual risk behavior and uptake of HIV counseling and testing among youth in Metropolitan Kumasi, Ghana. J. HIV/AIDS Soc. Serv. 2018, 17, 127–145. [Google Scholar] [CrossRef]
- Hibbert, M.P.; Wolton, A.; Weeks, H.; Ross, M.; Brett, C.E.; Porcellato, L.A.; Hope, V.D. Psychosocial and sexual factors associated with recent sexual health clinic attendance and HIV testing among trans people in the UK. BMJ Sex. Reprod. Health 2020, 46, 116–125. [Google Scholar] [CrossRef]
- Nemoto, T.; Iwamoto, M.; Perngparn, U.; Areesantichai, C.; Kamitani, E.; Sakata, M. HIV-Related Risk Behaviors among Kathoey (Male-to-Female Transgender) Sex Workers in Bangkok, Thailand. AIDS Care 2012, 24, 210–219. [Google Scholar] [CrossRef] [Green Version]
- Yi, S.; Sok, S.; Chhim, S.; Chhoun, P.; Chann, N.; Tuot, S.; Mun, P.; Pantelic, M. Access to community-based HIV services among transgender women in Cambodia: Findings from a national survey. Int. J. Equity Health 2019, 18, 1–13. [Google Scholar] [CrossRef] [Green Version]
- Yi, S.; Tuot, S.; Chhoun, P.; Brody, C.; Tith, K.; Oum, S. The impact of a community-based HIV and sexual reproductive health program on sexual and healthcare-seeking behaviors of female entertainment workers in Cambodia. BMC Infect Dis. 2015, 15, 221. [Google Scholar] [CrossRef] [Green Version]
- Yi, S.; Tuot, S.; Chhoun, P.; Pal, K.; Ngin, C.; Choub, S.C.; Brody, C. Improving prevention and care for HIV and sexually transmitted infections among men who have sex with men in Cambodia: The sustainable action against HIV and AIDS in communities (SAHACOM). BMC Health Serv. Res. 2016, 16, 599. [Google Scholar] [CrossRef] [Green Version]
- Shrestha, R.; Galka, J.M.; Azwa, I.; Lim, S.H.; Guadamuz, T.E.; Altice, F.L.; Wickersham, J.A. Willingness to Use HIV Self-Testing and Associated Factors among Transgender Women in Malaysia. Transgender Health 2020, 5, 182–190. [Google Scholar] [CrossRef]
- Balán, I.C.; Lopez-Rios, J.; Nayak, S.; Lentz, C.; Arumugam, S.; Kutner, B.; Dolezal, C.; Macar, O.U.; Pabari, T.; Ying, A.W.; et al. SMARTtest: A smartphone app to facilitate HIV and syphilis self- and partner-testing, interpretation of results, and linkage to care. AIDS Behav. 2020, 24, 1560. [Google Scholar] [CrossRef] [PubMed]
- Iribarren, S.; Lentz, C.; Sheinfil, A.Z.; Giguere, R.; Lopez-Rios, J.; Dolezal, C.; Frasca, T.; Balán, I.C.; Rael, C.T.; Brown, W.; et al. Using an HIV self-test kit to test a partner: Attitudes and preferences among high-risk populations. AIDS Behav. 2020, 24, 3232. [Google Scholar] [CrossRef] [PubMed]
- Eustaquio, P.C.; Figuracion, R.; Izumi, K.; Morin, M.J.; Samaco, K.; Flores, S.M.; Brink, A.; Diones, M.L. Outcomes of a community-led online-based HIV self-testing demonstration among cisgender men who have sex with men and transgender women in the Philippines during the COVID-19 pandemic: A retrospective cohort study. BMC Public Health 2022, 22, 366. [Google Scholar] [CrossRef] [PubMed]
- Witzel, T.C.; Eshun-Wilson, I.; Jamil, M.S.; Tilouche, N.; Figueroa, C.; Johnson, C.C.; Reid, D.; Baggaley, R.; Siegfried, N.; Burns, F.M.; et al. Comparing the effects of HIV self-testing to standard HIV testing for key populations: A systematic review and meta-analysis. BMC Med. 2020, 18, 381. [Google Scholar] [CrossRef] [PubMed]
- Pai, N.P.; Sharma, J.; Shivkumar, S.; Pillay, S.; Vadnais, C.; Joseph, L.; Dheda, K.; Peeling, R.W. Supervised and Unsupervised Self-Testing for HIV in High- and Low-Risk Populations: A Systematic Review. PLoS Med. 2013, 10, e1001414. [Google Scholar] [CrossRef] [Green Version]
- Choko, A.T.; Corbett, E.L.; Stallard, N.; Maheswaran, H.; Lepine, A.; Johnson, C.; Sakala, D.; Kalua, T.; Kumwenda, M.; Hayes, R.; et al. HIV self-testing alone or with additional interventions, including financial incentives, and linkage to care or prevention among male partners of antenatal care clinic attendees in Malawi: An adaptive multi-arm, multi-stage cluster randomised trial. PLoS Med. 2019, 16, e1002719. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gohil, J.; Baja, E.S.; Sy, T.R.; Guevara, E.G.; Hemingway, C.; Medina, P.M.B.; Coppens, L.; Dalmacion, G.V.; Taegtmeyer, M. Is the Philippines ready for HIV self-testing? BMC Public Health 2020, 20, 34. [Google Scholar] [CrossRef] [Green Version]
- Lippman, S.A.; Périssé, A.R.S.; Veloso, V.G.; Sullivan, P.S.; Buchbinder, S.; Sineath, R.C.; Grinsztejn, B. Acceptability of self-conducted home-based HIV testing among men who have sex with men in Brazil: Data from an on-line survey. Cad. Saude Publica. 2014, 30, 724. [Google Scholar] [CrossRef] [Green Version]
- Shi, Y.; Qiu, J.; Yang, Q.; Chen, T.; Lu, Y.; Chen, S.; Fan, X.; Lin, Z.; Han, Z.; Lu, J.; et al. Increasing the HIV testing among MSM through HIV test result exchange mechanism: Study protocol for a cluster randomized controlled trial. BMC Infect Dis. 2021, 21, 764. [Google Scholar] [CrossRef] [PubMed]
- Furegato, M.; Mitchell, H.; Ogaz, D.; Woodhall, S.; Connor, N.; Hughes, G.; Nardone, A.; Mohammed, H. The role of frequent HIV testing in diagnosing HIV in men who have sex with men. HIV Med. 2018, 19, 118–122. [Google Scholar] [CrossRef]
- Liu, Y.; Qian, H.-Z.; Ruan, Y.; Wu, P.; Osborn, C.Y.; Jia, Y.; Yin, L.; Lu, H.; He, X.; Shao, Y.; et al. Frequent HIV Testing: Impact on HIV Risk among Chinese Men Who Have Sex with Men. J. Acquir Immune Defic. Syndr. 2016, 72, 452. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Giguere, R.; Lopez-Rios, J.; Frasca, T.; Lentz, C.; Balán, I.C.; Dolezal, C.; Rael, C.T.; Brown, W.; Sheinfil, A.Z.; Torres, C.C.; et al. Use of HIV Self-testing Kits to Screen Clients among Transgender Female Sex Workers in New York and Puerto Rico. AIDS Behav. 2020, 24, 506. [Google Scholar] [CrossRef] [PubMed]
- Balán, I.C.; Lopez-Rios, J.; Giguere, R.; Lentz, C.; Dolezal, C.; Torres, C.C.; Brown, W.; Crespo, R.; Sheinfil, A.; Rael, C.T.; et al. Then We Looked at His Results: Men Who Have Sex with Men from New York City and Puerto Rico Report Their Sexual Partner’s Reactions to Receiving Reactive HIV Self-Test Results. AIDS Behav. 2020, 24, 2597–2605. [Google Scholar] [CrossRef] [PubMed]
- Lippman, S.A.; Moran, L.; Sevelius, J.; Castillo, L.S.; Ventura, A.; Treves-Kagan, S.; Buchbinder, S. Acceptability and Feasibility of HIV Self-Testing among Transgender Women in San Francisco: A Mixed Methods Pilot Study. AIDS Behav. 2016, 20, 928–938. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mavedzenge, S.N.; Baggaley, R.; Corbett, E.L. A Review of Self-Testing for HIV: Research and Policy Priorities in a New Era of HIV Prevention. Clin. Infect Dis. Off. Publ. Infect Dis. Soc. Am. 2013, 57, 126. [Google Scholar] [CrossRef]
- Wood, B.R.; Ballenger, C.; Stekler, J.D. Arguments for and against HIV self-testing. HIV AIDS 2014, 6, 117. [Google Scholar] [CrossRef] [Green Version]
- Martinez, O.; Carballo-Diéguez, A.; Ibitoye, M.; Frasca, T.; Brown, W.; Balan, I. Anticipated and Actual Reactions to Receiving HIV Positive Results Through Self-Testing among Gay and Bisexual Men. AIDS Behav. 2014, 18, 2485. [Google Scholar] [CrossRef] [Green Version]
- Carballo-Diéguez, A.; Giguere, R.; Balán, I.C.; Brown, W.; Dolezal, C.; Leu, C.-S.; Rios, J.L.; Sheinfil, A.Z.; Frasca, T.; Rael, C.T.; et al. Use of Rapid HIV Self-Test to Screen Potential Sexual Partners: Results of the ISUM Study. AIDS Behav. 2020, 24, 1929–1941. [Google Scholar] [CrossRef] [PubMed]
- Dinglasan, J.L.G.; Rosadiño, J.D.T.; Pagtakhan, R.G.; Cruz, D.P.; Briñes, M.T.; Regencia, Z.J.G.; Baja, E.S. ‘Bringing testing closer to you’: Barriers and facilitators in implementing HIV self-testing among Filipino men-having-sex-with-men and transgender women in National Capital Region (NCR), Philippines—A qualitative study. BMJ Open 2022, 12, e056697. [Google Scholar] [CrossRef]
- Bustamante, M.J.; Konda, K.A.; Davey, D.J.; Leon, S.; Calvo, G.M.; Salvatierra, J.; Brown, B.; Caceres, C.F.; Klausner, J.D. HIV self-testing in Peru: Questionable availability, high acceptability but potential low linkage to care among men who have sex with men and transgender women. Int. J. STD AIDS 2017, 28, 133–137. [Google Scholar] [CrossRef] [PubMed]
- Frye, V.; Wilton, L.; Hirshfield, S.; Chiasson, M.A.; Usher, D.; Lucy, D.; McCrossin, J.; Greene, E.; Koblin, B.; All About Me Study Team. “Just Because It’s Out There, People Aren’t Going to Use It.” HIV Self-Testing among Young, Black MSM, and Transgender Women. AIDS Patient Care STDs 2015, 29, 617–624. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pitasi, M.A.; Clark, H.A.; Chavez, P.R.; DiNenno, E.A.; Delaney, K.P. HIV Testing and Linkage to Care among Transgender Women Who Have Sex with Men: 23 U.S. Cities. AIDS Behav. 2020, 24, 2442. [Google Scholar] [CrossRef] [PubMed]
- Tiendrebeogo, T.; Plazy, M.; Darak, S.; Miric, M.; Perez-Then, E.; Butsashvili, M.; Tchendjou, P.; Dabis, F.; Orne-Gliemann, J. Couples HIV counselling and couple relationships in India, Georgia and the Dominican Republic. BMC Public Health 2017, 17, 901. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carballo-Diéguez, A.; Giguere, R.; Balán, I.C.; Dolezal, C.; Brown, W.; Lopez-Rios, J.; Sheinfil, A.; Frasca, T.; Rael, C.; Lentz, C.; et al. Few Aggressive or Violent Incidents are Associated with the Use of HIV Self-tests to Screen Sexual Partners among Key Populations. AIDS Behav. 2020, 24, 2220–2226. [Google Scholar] [CrossRef]
- Choko, A.T.; MacPherson, P.; Webb, E.L.; Willey, B.A.; Feasy, H.; Sambakunsi, R.; Mdolo, A.; Makombe, S.D.; Desmond, N.; Hayes, R.; et al. Uptake, Accuracy, Safety, and Linkage into Care over Two Years of Promoting Annual Self-Testing for HIV in Blantyre, Malawi: A Community-Based Prospective Study. PLoS Med. 2015, 12, e1001873. [Google Scholar] [CrossRef] [Green Version]
- Chanda, M.M.; Ortblad, K.F.; Mwale, M.; Chongo, S.; Kanchele, C.; Kamungoma, N.; Fullem, A.; Dunn, C.; Barresi, L.G.; Harling, G.; et al. HIV self-testing among female sex workers in Zambia: A cluster randomized controlled trial. PLoS Med. 2017, 14, e1002442. [Google Scholar] [CrossRef]
- Rael, C.T.; Kutner, B.A.; Lopez-Rios, J.; Lentz, C.; Dolezal, C.; Balán, I.C. Experiences of Transgender Women Who Used a Dual HIV/Syphilis Rapid Self-test to Screen Themselves and Potential Sexual Partners (the SMARTtest Study). AIDS Behav. 2022, 26, 1229–1237. [Google Scholar] [CrossRef]
- Kosenko, K.A. Meanings and dilemmas of sexual safety and communication for transgender individuals. Health Commun. 2010, 25, 131–141. [Google Scholar] [CrossRef]
- Vijay, A.; Earnshaw, V.A.; Tee, Y.C.; Pillai, V.; Hughto, J.M.W.; Clark, K.; Kamarulzaman, A.; Altice, F.L.; Wickersham, J.A. Factors Associated with Medical Doctors’ Intentions to Discriminate Against Transgender Patients in Kuala Lumpur, Malaysia. LGBT Health 2018, 5, 61–68. [Google Scholar] [CrossRef] [Green Version]
- Anderson, J.E.; Kanters, S. Lack of Sexual Minorities’ Rights as a Barrier to HIV Prevention among Men Who Have Sex with Men and Transgender Women in Asia: A Systematic Review. LGBT Health 2015, 2, 16–26. [Google Scholar] [CrossRef]
- Ahmed, S.I.; Syed Sulaiman, S.A.; Hassali, M.A.; Thiruchelvam, K.; Hasan, S.S.; Lee, C.K. Attitudes and barriers towards HIV screening: A qualitative study of people living with HIV/AIDS (PLWHA) in Malaysia. J. Infect Prev. 2017, 18, 242–247. [Google Scholar] [CrossRef] [PubMed]
- Estem, K.S.; Catania, J.; Klausner, J.D. HIV Self-Testing: A Review of Current Implementation and Fidelity. Curr. HIV/AIDS Rep. 2016, 13, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Kobrak, P.; Remien, R.H.; Myers, J.E.; Salcuni, P.; Edelstein, Z.; Tsoi, B.; Sandfort, T. Motivations and Barriers to Routine HIV Testing among Men Who Have Sex with Men in New York City. AIDS Behav. 2022, 1, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Takada, S.; Ettner, S.L.; Harawa, N.T.; Garland, W.H.; Shoptaw, S.J.; Cunningham, W.E. Life Chaos is Associated with Reduced HIV Testing, Engagement in Care, and ART Adherence among Cisgender Men and Transgender Women upon Entry into Jail. AIDS Behav. 2020, 24, 491–505. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jalil, E.M.; Wilson, E.C.; Luz, P.M.; Velasque, L.; Moreira, R.I.; Castro, C.V.; Monteiro, L.; Garcia, A.C.F.; Cardoso, S.W.; Coelho, L.E.; et al. HIV testing and the care continuum among transgender women: Population estimates from Rio de Janeiro, Brazil. J. Int. AIDS Soc. 2017, 20, 21873. [Google Scholar] [CrossRef] [Green Version]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Budzyńska, J.; Patryn, R.; Kozioł, I.; Leśniewska, M.; Kopystecka, A.; Skubel, T. Self-Testing as a Hope to Reduce HIV in Transgender Women—Literature Review. Int. J. Environ. Res. Public Health 2022, 19, 9331. https://doi.org/10.3390/ijerph19159331
Budzyńska J, Patryn R, Kozioł I, Leśniewska M, Kopystecka A, Skubel T. Self-Testing as a Hope to Reduce HIV in Transgender Women—Literature Review. International Journal of Environmental Research and Public Health. 2022; 19(15):9331. https://doi.org/10.3390/ijerph19159331
Chicago/Turabian StyleBudzyńska, Julia, Rafał Patryn, Ilona Kozioł, Magdalena Leśniewska, Agnieszka Kopystecka, and Tomasz Skubel. 2022. "Self-Testing as a Hope to Reduce HIV in Transgender Women—Literature Review" International Journal of Environmental Research and Public Health 19, no. 15: 9331. https://doi.org/10.3390/ijerph19159331





