Validation of the Korean Version of Nurses’ Moral Courage Scale
Abstract
:1. Introduction
2. Materials and Methods
2.1. Research Design
2.2. Participants and Data Collection
2.3. Instruments
2.3.1. General Characteristics
2.3.2. Nurses’ Moral Courage Scale
2.3.3. Korean Version of the Professional Moral Courage Scale
2.3.4. Korean Moral Sensitivity Questionnaire
2.3.5. Data Analysis
- Substantive Stage: Translation and Cross-cultural adaptation of NMCS
- Structural Stage: Internal Relations among subdomains of K-NMCS
- External stage: Relations among Constructs
2.3.6. Ethical Considerations
3. Results
3.1. Participants and Descriptive Statics
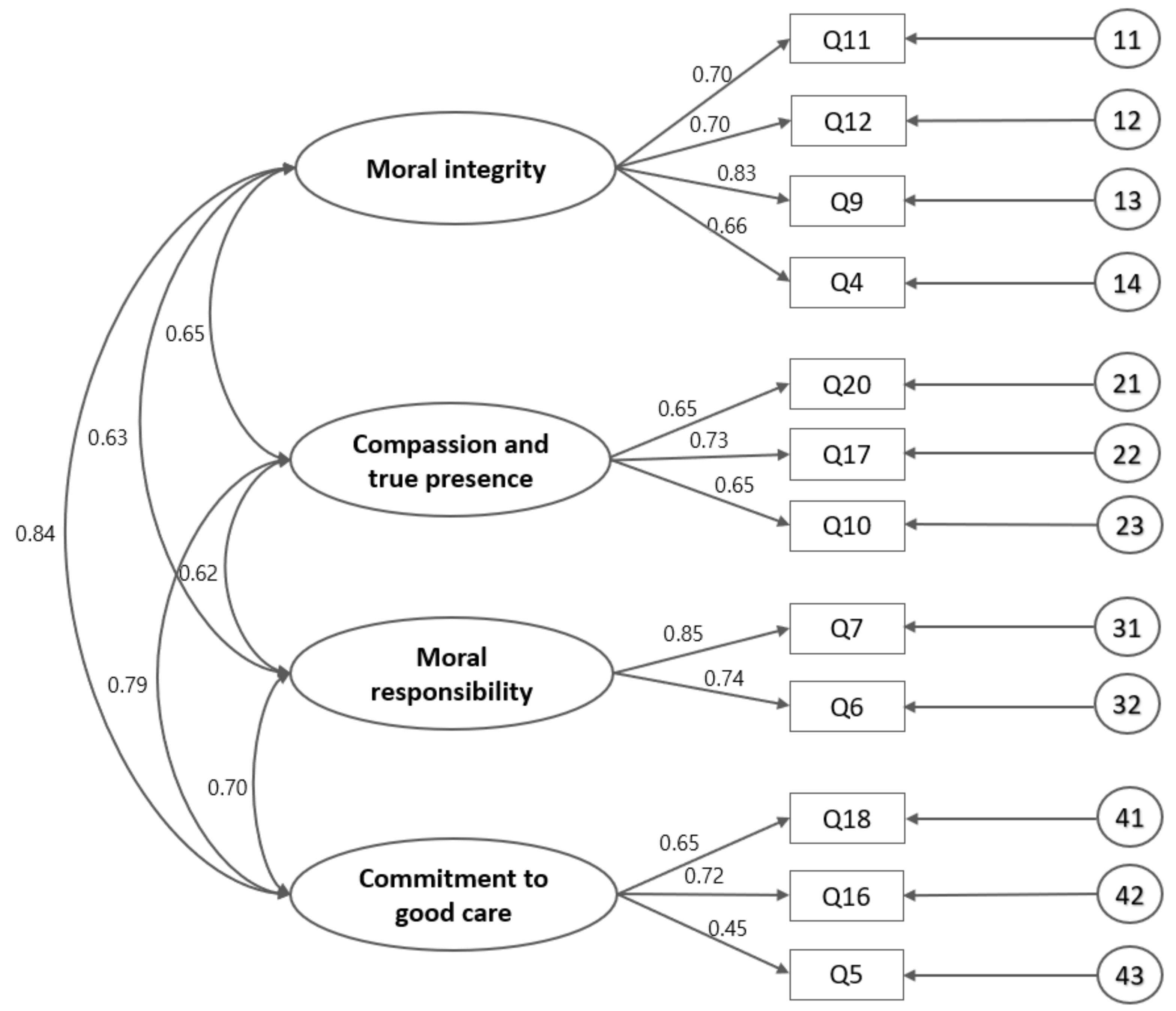
3.2. Structural Stage: Internal Relations among Subdomains of K-NMCS
- Construct validity of K-NMCS
- Reliability of K-NMCS
- Convergent and Discriminant Validity
3.3. External Stage: Relations among Constructs
4. Discussion
4.1. Implications
4.2. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Oh, Y.; Gastmans, C. Moral distress experienced by nurses: A quantitative literature review. Nurs. Ethics 2015, 22, 15–31. [Google Scholar] [CrossRef] [PubMed]
- Park, B.; Oh, Y. Impact of ethical climate, ethical leadership perceived by nurses on moral distress. JKDAS 2017, 19, 1099–1116. [Google Scholar] [CrossRef]
- Numminen, O.; Katajisto, J.; Leino-Kilpi, H. Development and validation of Nurses’ Moral Courage Scale. Nurs. Ethics 2019, 26, 2438–2455. [Google Scholar] [CrossRef] [PubMed]
- Kleemola, E.; Leino-Kilpi, H.; Numminen, O. Care situations demanding moral courage: Content analysis of nurses’ experiences. Nurs. Ethics 2020, 27, 714–725. [Google Scholar] [CrossRef] [PubMed]
- Gallagher, A. Slow Ethics and the Art of Care; Emerald Group Publishing: Bingley, UK, 2020; p. 30. [Google Scholar]
- Schröck, R.A. Conscience and courage—A critical examination of professional conduct. Nurse Educ. Today 1990, 10, 3–9. [Google Scholar] [CrossRef]
- Fokkema, M.; Greiff, S. How Performing PCA and CFA on the Same Data Equals Trouble. Eur. J. Psychol. Assess 2017, 33, 399–402. [Google Scholar] [CrossRef]
- Fitzpatrick, J.J. Teaching moral courage: Obligation and challenge. Nurs. Educ. Perspect. 2018, 39, 200. [Google Scholar] [CrossRef]
- Lachman, V.D. Moral courage: A virtue in need of development? Medsurg. Nurs. 2007, 16, 131–133. [Google Scholar]
- Oh, Y. Impact of moral courage, professional autonomy on moral distress. In Proceedings of the Nursing Ethics International Conference, London, UK, 2–4 September 2021; p. 2. [Google Scholar]
- Oh, Y. Nursing ethics in COVID-19 era: What is the ontological nursing? In Proceedings of the Korean Society for Medical Ethics Conference, Seoul, Korea, 29 May 2021; pp. 133–139. [Google Scholar]
- Thorup, C.B.; Rundqvist, E.; Roberts, C.; Delmar, C. Care as a matter of courage: Vulnerability, suffering and ethical formation in nursing care. Scand. J. Caring Sci. 2012, 26, 427–435. [Google Scholar] [CrossRef]
- LaSala, C.A.; Bjarnason, D. Creating workplace environments that support moral courage. J. Issues Nurs. 2010, 15, 4. [Google Scholar] [CrossRef]
- Black, S.; Curzio, J.; Terry, L. Failing a student nurse: A new horizon of moral courage. Nurs. Ethics 2014, 21, 224–238. [Google Scholar] [CrossRef] [PubMed]
- Numminen, O.; Konings, K.; Claerhout, R.; Gastmans, C.; Katajisto, J.; Leino-Kilpi, H.; Dierckx de Casterlé, B. Validation of the Dutch-language version of Nurses’ Moral Courage Scale. Nurs. Ethics 2021, 28, 809–822. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Oh, Y.; Lee, E.; Kim, S.-J. Impact of Nurse-Physician Collaboration, Moral Distress, and Professional Autonomy on Job Satisfaction among Nurses Acting as Physician Assistants. Int. J. Env. Res. Public Health 2022, 19, 661. [Google Scholar] [CrossRef] [PubMed]
- Bickhoff, L.; Sinclair, P.M.; Levett-Jones, T. Moral courage in undergraduate nursing students: A literature review. Collegian 2017, 24, 71–83. [Google Scholar] [CrossRef]
- Brown, G. Ethical and Moral Courage is Distress among Professional Nurses: A Workplace Issue. ABNF J. 2015, 26, 63–64. [Google Scholar]
- Escolar-Chua, R.L. Moral sensitivity, moral distress, and moral courage among baccalaureate Filipino nursing students. Nurs. Ethics 2018, 25, 458–469. [Google Scholar] [CrossRef]
- Taraz, Z.; Loghmani, L.; Abbaszadeh, A.; Ahmadi, F.; Safavibiat, Z.; Borhani, F. The relationship between ethical climate of hospital and moral courage of nursing staff. Electron. J. Gen. Med. 2019, 16, em109. [Google Scholar]
- Sekerka, L.E.; Bagozzi, R.P.; Charnigo, R. Facing ethical challenges in the workplace: Conceptualizing and measuring professional moral courage. J. Bus. Ethics 2009, 89, 565. [Google Scholar] [CrossRef]
- Benson, J. Developing a Strong Program of Construct Validation: A Test Anxiety Example. Educ. Meas. Issues Pract. 1998, 17, 10–17. [Google Scholar] [CrossRef]
- Moon, S.J.; Kim, D.S. Convergence Study of Reliability and Validity testing for Professional Moral Courage Scale Translated in Korean. JKCS 2017, 8, 151–161. [Google Scholar] [CrossRef]
- Han, S.; Ahn, S.; Kim, Y.; Kim, J. Validation of a Korean version of the Moral Sensitivity Questionnaire. Nurs. Ethics 2010, 17, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Lutzen, K.; Evertzon, M.; Nordin, C. Moral sensitivity in psychiatric practice. Nurs. Ethics 1997, 4, 472–482. [Google Scholar] [CrossRef] [PubMed]
- Ohrbach, R.; Bjorner, J.; Jezewski, M.; John, M.; Lobbezoo, F. Guidelines for Establishing Cultural Equivalency of Instruments; University at Buffalo: New York, NY, USA, 2009; pp. 1–59. [Google Scholar]
- Sousa, V.D.; Rojjanasrirat, W. Translation, adaptation and validation of instruments or scales for use in cross-cultural health care research: A clear and user-friendly guideline. J. Eval. Clin. Pract. 2011, 17, 268–274. [Google Scholar] [CrossRef] [PubMed]
- Polit, D.F.; Beck, C.T. The content validity index: Are you sure you know what’s being reported? critique and recommendations. Res. Nurs. Health 2006, 29, 489–497. [Google Scholar] [CrossRef]
- Henson, R.K.; Roberts, J.K. Use of Exploratory Factor Analysis in Published Research:Common Errors and Some Comment on Improved Practice. Educ. Psychol. Meas. 2006, 66, 393–416. [Google Scholar] [CrossRef]
- Hair, J.F.; Black, W.C.; Babin, B.J.; Anderson, R.E.; Tatham, R.L. Multivariate Data Analysis (Vol. 6); Pearson Prentice Hall: Upper Saddle River, NJ, USA, 2006; pp. 35–37. [Google Scholar]
- Cheung, G.W.; Wang, C. Current Approaches for Assessing Convergent and Discriminant Validity with SEM: Issues and Solutions. Acad. Manag. Proc. 2017, 1, 12706. [Google Scholar] [CrossRef]
- Anderson, J.C.; Gerbing, D.W. Structural equation modeling in practice: A review and recommended two-step approach. PsyB 1988, 103, 411. [Google Scholar] [CrossRef]
- Xia, Y.; Yang, Y. RMSEA, CFI, and TLI in structural equation modeling with ordered categorical data: The story they tell depends on the estimation methods. Behav. Res. Methods 2019, 51, 409–428. [Google Scholar] [CrossRef]
- Knekta, E.; Runyon, C.; Eddy, S. One Size Doesn’t Fit All: Using Factor Analysis to Gather Validity Evidence When Using Surveys in Your Research. CBE Life Sci. Educ. 2019, 18, rm1–rm17. [Google Scholar] [CrossRef]
- Samuels, P. Advice on Exploratory Factor Analysis; Centre for Academic Success, Birmingham City University: Birmingham, UK, 2017; pp. 1–7. Available online: https://www.open-access.bcu.ac.uk/id/eprint/6076 (accessed on 4 June 2022).
- Hu, L.t.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Ursachi, G.; Horodnic, I.A.; Zait, A. How reliable are measurement scales? External factors with indirect influence on reliability estimators. Procedia Econ. Financ. 2015, 20, 679–686. [Google Scholar] [CrossRef]
- Van Griethuijsen, R.A.; van Eijck, M.W.; Haste, H.; den Brok, P.J.; Skinner, N.C.; Mansour, N.; Gencer, A.S.; BouJaoude, S. Global patterns in students’ views of science and interest in science. Res. Sci. Educ. 2015, 45, 581–603. [Google Scholar] [CrossRef]
- Taber, K.S. The use of Cronbach’s alpha when developing and reporting research instruments in science education. Res. Sci. Educ. 2018, 48, 1273–1296. [Google Scholar] [CrossRef] [Green Version]
- Taherdoost, H. Validity and reliability of the research instrument; how to test the validation of a questionnaire/survey in a research. Int. J. Acad. Res. 2016, 5, 23–36. [Google Scholar] [CrossRef]
- Kim, M.; Oh, Y.; Kong, B. Ethical conflicts experienced by nurses in geriatric hospitals in South Korea: “If You Can’t Stand the Heat, Get Out of the Kitchen”. Int. J. Env. Res. Public Health 2020, 17, 4442. [Google Scholar] [CrossRef]
- Gallagher, A. Moral distress and moral courage in everyday nursing practice. J. Issues Nurs. 2011, 16, 8. [Google Scholar] [CrossRef]
- Jang, Y.; Oh, Y. Impact of ethical factors on job satisfaction among Korean nurses. Nurs. Ethics 2019, 26, 1186–1198. [Google Scholar] [CrossRef]
- Park, B.; Oh, Y. Moral distress experienced by nurses in South Korea; an integrated review. Korean J. Med. Ethics. 2016, 19, 312–327. [Google Scholar]
- Majima, T.; Yamamoto, T.; Sakai, I.; Ikezaki, S.; Nagasaka, I. Job satisfaction and related factors of nurses in university hospitals: Focusing on collaborative competency factors. J. Nurs. Manag. 2019, 27, 1409–1415. [Google Scholar] [CrossRef]
- Hospital Nurses Association. A survey on hospital nursing staffing. 2019. Available online: https://khna.or.kr/home/pds/utilities.php (accessed on 19 May 2022).
- Ziegler, M. Stop and state your intentions! Eur. J. Psychol. Assess 2014, 30, 239–242. [Google Scholar] [CrossRef]
- Choi, Y. Impact of Moral Courage and Professional Autonomy on Moral Distress among Nurses; Graduate School of Hally University: Seoul, Korea, 2021. [Google Scholar]
- Hyun, J.; Kim, D.; Park, J.; Choi, Y.; Choi, Y.; Kim, S. Factors that Influence Clinical Nurses’ Moral Courage. Korean J. Med. Ethics 2021, 24, 45–58. [Google Scholar]
- Spector, P.E. Method variance in organizational research truth or urban legend? Organ. Res. Methods 2006, 9, 221–232. [Google Scholar] [CrossRef] [Green Version]
| K-NMCS Sub-Scale and Items | Factors | ||||
|---|---|---|---|---|---|
| Factor Loading | Communalities | ||||
| 1 | 2 | 3 | 4 | ||
| III. Moral integrity | |||||
| If someone else* acts professionally dishonestly (e.g., steals medication from the ward), I bring it up for discussion | 0.780 | 0.675 | |||
| If someone else* tries to cover up an evident care mistake he/she has made, I bring it up for discussion | 0.748 | 0.667 | |||
| I bring up for discussion an ethical problem situation that arises in nursing care even if someone else* wants to remain silent about it | 0.693 | 0.693 | |||
| If someone else* acts unethically, I bring it up for discussion, even if I were to get negative feedback for it in my work community | 0.684 | 0.590 | |||
| I. Compassion and true presence | |||||
| Regardless of the care situation, I seek to create a genuine human encounter with the patient, even though a more superficial relationship would be easier for me | 0.837 | 0.725 | |||
| I support a suffering patient by being truly present for him/her, even if it were to lead me to encounter my own inner fears | 0.740 | 0.676 | |||
| Regardless of the care situation, I try to encounter each patient as a dignified human being, even if someone else were to disagree with my doing so | 0.535 | 0.669 | |||
| II. Moral responsibility | |||||
| I participate in the care team’s ethical decision-making regardless of someone else* disagreeing with the answer that I consider right | 0.828 | 0.800 | |||
| I participate in the care team’s ethical decision making despite the fact that ethical problem situations often involve uncertainty as to the right answer | 0.810 | 0.785 | |||
| IV. Commitment to good care | |||||
| I do not compromise on my patient’s right to good care even though someone else* were to bully me into doing so | 0.635 | 0.658 | |||
| I bring up for discussion the patient’s right to good care if someone else* compromises on adherence to the ethical principles of health care (human dignity, autonomy, justice, and justified care) | 0.599 | 0.684 | |||
| If I observe evident shortcomings in someone else’s professional competence, I bring it up for discussion | 0.581 | 0.616 | |||
| χ2 | df | p | CFI | TLI | RMSEA | |
|---|---|---|---|---|---|---|
| RMSEA | 95% CI | |||||
| 120.589 | 48 | <0.001 | 0.931 | 0.905 | 0.079 | 0.062–0.097 |
| Subscale | SMC | AVE | CR | |||
|---|---|---|---|---|---|---|
| F1 | F2 | F3 | F4 | |||
| Moral integrity (F1) | 1 | 0.702 | 0.904 | |||
| Compassion and true presence (F2) | 0.4212 | 1 | 0.592 | 0.813 | ||
| Moral responsibility (F3) | 0.3956 | 0.3881 | 1 | 0.769 | 0.869 | |
| Commitment to good care (F4) | 0.7006 | 0.6273 | 0.4844 | 1 | 0.715 | 0.879 |
| Mean | SD | K-NMCS | K-PMCS | K-MSQ | Cronbach’s α | |
|---|---|---|---|---|---|---|
| K-NMCS | 3.26 | 0.52 | 1 | 0.872 | ||
| K-PMCS | 4.75 | 0.73 | 0.679 *** | 1 | 0.916 | |
| K-MSQ | 4.74 | 0.60 | 0.348 *** | 0.449 *** | 1 | 0.855 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, B.; Oh, Y.; Lee, E.; Nam, K.A. Validation of the Korean Version of Nurses’ Moral Courage Scale. Int. J. Environ. Res. Public Health 2022, 19, 11642. https://doi.org/10.3390/ijerph191811642
Lee B, Oh Y, Lee E, Nam KA. Validation of the Korean Version of Nurses’ Moral Courage Scale. International Journal of Environmental Research and Public Health. 2022; 19(18):11642. https://doi.org/10.3390/ijerph191811642
Chicago/Turabian StyleLee, Boram, Younjae Oh, Eunhee Lee, and Kyoung A Nam. 2022. "Validation of the Korean Version of Nurses’ Moral Courage Scale" International Journal of Environmental Research and Public Health 19, no. 18: 11642. https://doi.org/10.3390/ijerph191811642








