Accessibility to Digital Mental Health Services among the General Public throughout COVID-19: Trajectories, Influencing Factors and Association with Long-Term Mental Health Symptoms
Abstract
:1. Introduction
2. Methods
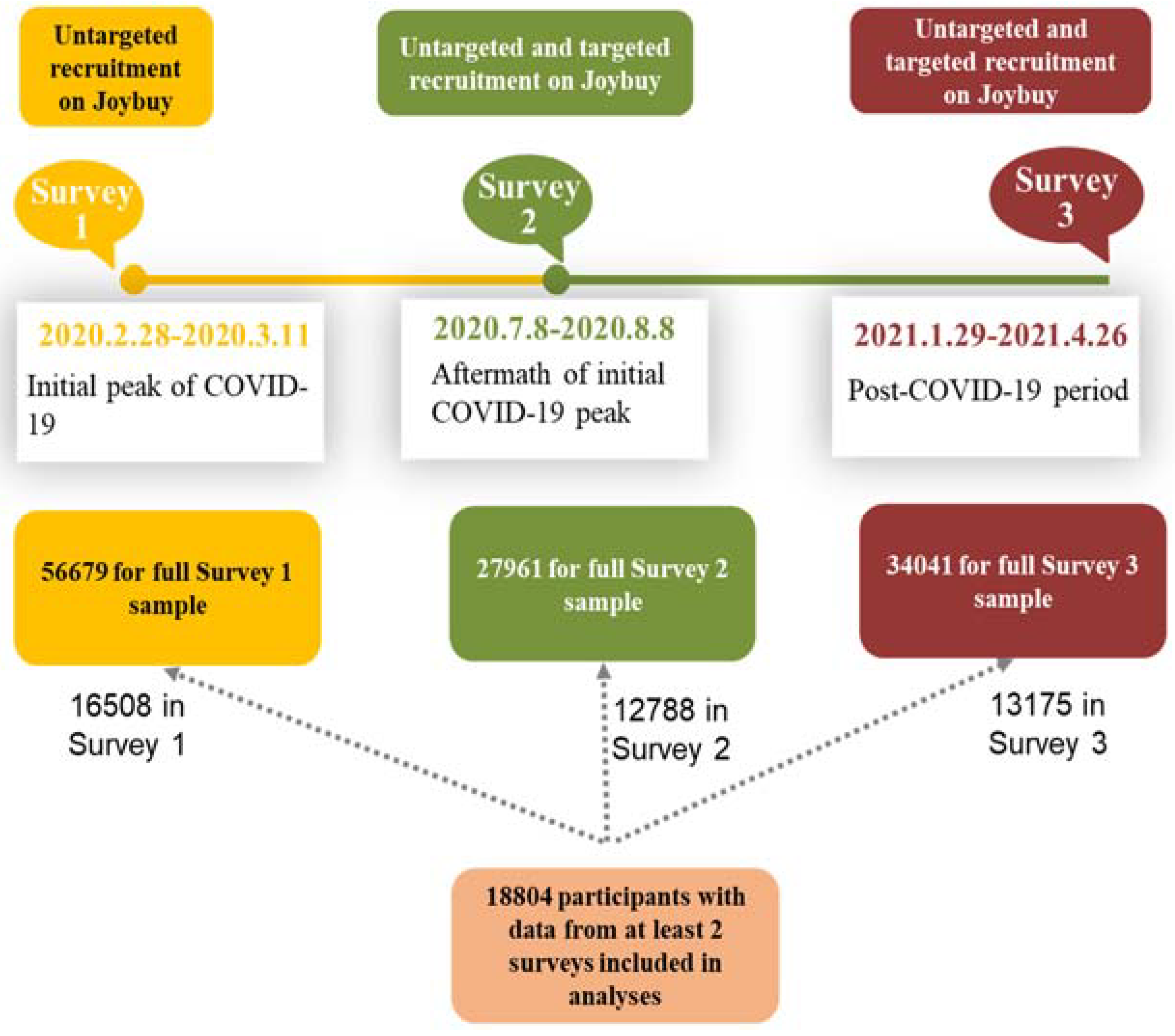
2.1. Procedures and Participants
2.2. Measures
2.3. Statistical Analyses
3. Results
3.1. Demographic Characteristics of the Longitudinal Sample
3.2. Trajectory of Accessibility to DMHSs from Before to One Year after COVID-19 Outbreak
3.3. Influencing Factors of Accessibility to DMHSs throughout COVID-19
3.4. Latent Trajectory Classes of Accessibility to DMHSs from Before to One Year after COVID-19 Outbreak
3.5. Association between Trajectory Class Membership of Accessibility to DMHSs and Long-Term Mental Health Symptoms
3.6. Supplementary Analyses of DMHS Usage throuhout COVID-19
4. Discussion
4.1. Trajectory of Accessibility to DMHSs during COVID-19
4.2. Latent Trajectory Classes of Accessibility to DMHSs during COVID-19
4.3. Influencing Factors of Accessibility to DMHSs throughout COVID-19
4.4. Association between Trajectory Class of Accessibility to DMHSs and Long-Term Mental Health Symptoms during COVID-19
5. Strengths and Limitations
6. Conclusions and Implications
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Luo, M.; Guo, L.; Yu, M.; Jiang, W.; Wang, H. The psychological and mental impact of coronavirus disease 2019 (COVID-19) on medical staff and general public—A systematic review and meta-analysis. Psychiatry Res. 2020, 291, 113190. [Google Scholar] [CrossRef]
- Wu, T.; Jia, X.; Shi, H.; Niu, J.; Yin, X.; Xie, J.; Wang, X. Prevalence of mental health problems during the COVID-19 pandemic: A systematic review and meta-analysis. J. Affect. Disord. 2021, 281, 91–98. [Google Scholar] [CrossRef]
- Shi, L.; Lu, Z.A.; Que, J.Y.; Huang, X.L.; Liu, L.; Ran, M.S.; Gong, Y.M.; Yuan, K.; Yan, W.; Sun, Y.K.; et al. Prevalence of and Risk Factors Associated with Mental Health Symptoms among the General Population in China during the Coronavirus Disease 2019 Pandemic. JAMA Netw. Open. 2020, 3, e2014053. [Google Scholar] [CrossRef]
- Shi, L.; Lu, Z.-A.; Que, J.-Y.; Huang, X.-L.; Lu, Q.-D.; Liu, L.; Zheng, Y.B.; Liu, W.-J.; Ran, M.-S.; Yuan, K.; et al. Long-Term Impact of COVID-19 on Mental Health among the General Public: A Nationwide Longitudinal Study in China. Int J. Environ. Res. Public Health 2021, 18, 8790. [Google Scholar] [CrossRef]
- Liu, S.; Yang, L.; Zhang, C.; Xiang, Y.T.; Liu, Z.; Hu, S.; Zhang, B. Online mental health services in China during the COVID-19 outbreak. Lancet Psychiatry 2020, 7, e17–e18. [Google Scholar] [CrossRef]
- Yao, H.; Chen, J.H.; Xu, Y.F. Rethinking online mental health services in China during the COVID-19 epidemic. Asian J. Psychiatry 2020, 50, 102015. [Google Scholar] [CrossRef]
- Li, W.; Yang, Y.; Liu, Z.H.; Zhao, Y.J.; Zhang, Q.; Zhang, L.; Cheung, T.; Xiang, Y.T. Progression of Mental Health Services during the COVID-19 Outbreak in China. Int. J. Biol. Sci. 2020, 16, 1732–1738. [Google Scholar] [CrossRef] [Green Version]
- Ifdil, I.; Fadli, R.P.; Suranata, K.; Zola, N.; Ardi, Z. Online mental health services in Indonesia during the COVID-19 outbreak. Asian J. Psychiatry 2020, 51, 102153. [Google Scholar] [CrossRef]
- Thummapol, O.; Park, T.; Barton, S. Exploring health services accessibility by indigenous women in Asia and identifying actions to improve it: A scoping review. Ethn. Health 2020, 25, 940–959. [Google Scholar] [CrossRef]
- Lee, J.E.; Kim, H.R.; Shin, H.I. Accessibility of medical services for persons with disabilities: Comparison with the general population in Korea. Disabil. Rehabil. 2014, 36, 1728–1734. [Google Scholar] [CrossRef]
- Lamontagne, M.E.; Djossa Adoun, M.; Blanchette, A.K.; Champagne, C.; Johnson, M.P.; Vincent, C.; Routhier, F. Facilitators and barriers to the use of service dogs: An exploratory study using the Theoretical Domains Framework. Disabil. Rehabil. Assist. Technol. 2020, 15, 537–544. [Google Scholar] [CrossRef] [PubMed]
- Kaihlanen, A.M.; Virtanen, L.; Buchert, U.; Safarov, N.; Valkonen, P.; Hietapakka, L.; Hörhammer, I.; Kujala, S.; Kouvonen, A.; Heponiemi, T. Towards digital health equity—A qualitative study of the challenges experienced by vulnerable groups in using digital health services in the COVID-19 era. BMC Health Serv. Res. 2022, 22, 188. [Google Scholar] [CrossRef] [PubMed]
- Lä ttman, K.; Olsson, L.E.; Friman, M. Development and test of the Perceived Accessibility Scale (PAC) in public transport. J. Transport. Geogr. 2016, 54, 257–263. [Google Scholar] [CrossRef]
- Scheepers, C.E.; Wendel-Vos, G.; Kempen, E.; Hollander, E.; Schuit, A.J. Perceived accessibility is an important factor in transport choice—Results from the AVENUE project. J. Transport. Health 2016, 3, 96–106. [Google Scholar] [CrossRef]
- Bao, Y.; Sun, Y.; Meng, S.; Shi, J.; Lu, L. 2019-nCoV epidemic: Address mental health care to empower society. Lancet 2020, 395, e37–e38. [Google Scholar] [CrossRef] [Green Version]
- Fancourt, D.; Steptoe, A.; Bu, F. Trajectories of anxiety and depressive symptoms during enforced isolation due to COVID-19 in England: A longitudinal observational study. Lancet Psychiatry 2021, 8, 141–149. [Google Scholar] [CrossRef]
- Mcginty, E.E.; Presskreischer, R.; Anderson, K.E.; Han, H.; Barry, C.L. Psychological Distress and COVID-19-Related Stressors Reported in a Longitudinal Cohort of US Adults in April and July 2020. JAMA 2020, 324, 2555–2557. [Google Scholar] [CrossRef]
- Nguena Nguefack, H.L.; Pagé, M.G.; Katz, J.; Choinière, M.; Vanasse, A.; Dorais, M.; Samb, O.M.; Lacasse, A. Trajectory Modelling Techniques Useful to Epidemiological Research: A Comparative Narrative Review of Approaches. Clin. Epidemiol. 2020, 12, 1205–1222. [Google Scholar] [CrossRef]
- Felt, J.M.; Depaoli, S.; Tiemensma, J. Latent Growth Curve Models for Biomarkers of the Stress Response. Front. Neurosci. 2017, 11, 315. [Google Scholar] [CrossRef] [Green Version]
- Mazza, G.L.; Enders, C.K.; Ruehlman, L.S. Addressing Item-Level Missing Data: A Comparison of Proration and Full Information Maximum Likelihood Estimation. Multivar. Behav. Res. 2015, 50, 504–519. [Google Scholar] [CrossRef] [Green Version]
- Lee, T.; Shi, D. A comparison of full information maximum likelihood and multiple imputation in structural equation modeling with missing data. Psychol. Methods 2021, 26, 466–485. [Google Scholar] [CrossRef] [PubMed]
- Burant, C.J. Latent Growth Curve Models: Tracking Changes over Time. Int. J. Aging Hum. Dev. 2016, 82, 336–350. [Google Scholar] [CrossRef] [PubMed]
- Van De Schoot, R. Latent Growth Mixture Models to estimate PTSD trajectories. Eur J. Psychotraumatol. 2015, 6, 27503. [Google Scholar] [CrossRef] [PubMed]
- Jones, J.W.; Ledermann, T.; Fauth, E.B. Self-rated health and depressive symptoms in older adults: A growth mixture modeling approach. Arch. Gerontol. Geriatr. 2018, 79, 137–144. [Google Scholar] [CrossRef]
- Taylor, C.B.; Fitzsimmons-Craft, E.E.; Graham, A.K. Digital technology can revolutionize mental health services delivery: The COVID-19 crisis as a catalyst for change. Int. J. Eat. Disord. 2020, 53, 1155–1157. [Google Scholar] [CrossRef] [PubMed]
- Ćosić, K.; Popović, S.; Šarlija, M.; Kesedžić, I. Impact of Human Disasters and COVID-19 Pandemic on Mental Health: Potential of Digital Psychiatry. Psychiatr. Danub. 2020, 32, 25–31. [Google Scholar] [CrossRef]
- Doubeni, C.A.; Li, W.; Fouayzi, H.; Difranza, J.R. Perceived accessibility as a predictor of youth smoking. Ann. Fam. Med. 2008, 6, 323–330. [Google Scholar] [CrossRef]
- Pratiwi, A.R.; Zhao, S.; Mi, X. Quantifying the relationship between visitor satisfaction and perceived accessibility to pedestrian spaces on festival days. Front. Archit. Res. 2015, 4, 285–295. [Google Scholar] [CrossRef] [Green Version]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Löwe, B.; Decker, O.; Müller, S.; Brähler, E.; Schellberg, D.; Herzog, W.; Herzberg, P.Y. Validation and standardization of the Generalized Anxiety Disorder Screener (GAD-7) in the general population. Med. Care 2008, 46, 266–274. [Google Scholar] [CrossRef]
- Gagnon, C.; Bélanger, L.; Ivers, H.; Morin, C.M. Validation of the Insomnia Severity Index in primary care. J. Am. Board Fam. Med. 2013, 26, 701–710. [Google Scholar] [CrossRef] [PubMed]
- Hu, L.T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Modeling A Multidiscip. J. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Akaike, H. Likelihood of a model and information criteria. J. Econom. 1981, 16, 3–14. [Google Scholar] [CrossRef]
- Schwartz, G. Estimating the dimension of a model. Ann. Stat. 1978, 6, 31–38. [Google Scholar] [CrossRef]
- Sclove, S.L. Application of model-selection criteria to some problems in multivariate analysis. Psychometrika 1987, 52, 333–343. [Google Scholar] [CrossRef]
- Lo, Y.T.; Mendell, N.R.; Rubin, D.B. Testing the number of components in a normal mixture. Biometrika 2001, 88, 767–778. [Google Scholar] [CrossRef]
- Bauer, D.J.; Curran, P.J. Distributional Assumptions of Growth Mixture Models: Implications for Overextraction of Latent Trajectory Classes. Psychol. Methods 2003, 8, 338–363. [Google Scholar] [CrossRef] [Green Version]
- Cham, H.; Reshetnyak, E.; Rosenfeld, B.; Breitbart, W. Full Information Maximum Likelihood Estimation for Latent Variable Interactions with Incomplete Indicators. Multivar. Behav. Res. 2017, 52, 12–30. [Google Scholar] [CrossRef] [Green Version]
- Levin-Zamir, D.; Bertschi, I. Media Health Literacy, eHealth Literacy, and the Role of the Social Environment in Context. Int. J. Environ. Res. Public Health 2018, 15, 1643. [Google Scholar] [CrossRef] [Green Version]
- Alam, K.; Mahumud, R.A.; Alam, F.; Keramat, S.A.; Erdiaw-Kwasie, M.O.; Sarker, A.R. Determinants of access to eHealth services in regional Australia. Int. J. Med. Inform. 2019, 131, 103960. [Google Scholar] [CrossRef]
- Ross, J.; Stevenson, F.; Lau, R.; Murray, E. Factors that influence the implementation of e-health: A systematic review of systematic reviews (an update). Implement. Sci. 2016, 11, 146. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cellini, N.; Canale, N.; Mioni, G.; Costa, S. Changes in sleep pattern, sense of time and digital media use during COVID-19 lockdown in Italy. J. Sleep Res. 2020, 29, e13074. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Li, Y.; Bao, Y.; Meng, S.; Sun, Y.; Schumann, G.; Kosten, T.; Strang, J.; Lu, L.; Shi, J. Brief Report: Increased Addictive Internet and Substance Use Behavior during the COVID-19 Pandemic in China. Am. J. Addict. 2020, 29, 268–270. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.X.; Wang, Y.; Rauch, A.; Wei, F. Unprecedented disruption of lives and work: Health, distress and life satisfaction of working adults in China one month into the COVID-19 outbreak. Psychiatry Res. 2020, 288, 112958. [Google Scholar] [CrossRef] [PubMed]
- Daly, M.; Sutin, A.R.; Robinson, E. Longitudinal changes in mental health and the COVID-19 pandemic: Evidence from the UK Household Longitudinal Study. Psychol. Med. 2020, 1–10. [Google Scholar] [CrossRef]
- Fiorillo, A.; Sampogna, G.; Giallonardo, V.; Del Vecchio, V.; Luciano, M.; Albert, U.; Carmassi, C.; Carrà, G.; Cirulli, F.; Dell’osso, B.; et al. Effects of the lockdown on the mental health of the general population during the COVID-19 pandemic in Italy: Results from the COMET collaborative network. Eur. Psychiatry 2020, 63, e87. [Google Scholar] [CrossRef]
- Greer, B.; Robotham, D.; Simblett, S.; Curtis, H.; Griffiths, H.; Wykes, T. Digital Exclusion among Mental Health Service Users: Qualitative Investigation. J. Med. Internet Res. 2019, 21, e11696. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baumann, E.; Czerwinski, F.; Reifegerste, D. Gender-Specific Determinants and Patterns of Online Health Information Seeking: Results from a Representative German Health Survey. J. Med. Internet Res. 2017, 19, e92. [Google Scholar] [CrossRef] [Green Version]
- Wellstead, P. Information behaviour of Australian men experiencing stressful life events: The role of social networks and confidants. Inf. Res. 2011, 16, 474. [Google Scholar]
- Torrent-Sellens, J.; Díaz-Chao, Á.; Soler-Ramos, I.; Saigí-Rubió, F. Modelling and Predicting eHealth Usage in Europe: A Multidimensional Approach from an Online Survey of 13,000 European Union Internet Users. J. Med. Internet Res. 2016, 18, e188. [Google Scholar] [CrossRef] [Green Version]
- Hamama-Raz, Y.; Palgi, Y.; Shrira, A.; Goodwin, R.; Kaniasty, K.; Ben-Ezra, M. Gender differences in psychological reactions to Hurricane Sandy among New York Metropolitan Area residents. Psychiatr. Q. 2015, 86, 285–296. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Shi, L.; Que, J.; Lu, Q.; Liu, L.; Lu, Z.; Xu, Y.; Liu, J.; Sun, Y.; Meng, S.; et al. The impact of quarantine on mental health status among general population in China during the COVID-19 pandemic. Mol. Psychiatry 2021, 26, 4813–4822. [Google Scholar] [CrossRef] [PubMed]
- Evanoff, B.A.; Strickland, J.R.; Dale, A.M.; Hayibor, L.; Page, E.; Duncan, J.G.; Kannampallil, T.; Gray, D.L. Work-Related and Personal Factors Associated with Mental Well-Being during the COVID-19 Response: Survey of Health Care and Other Workers. J. Med. Internet Res. 2020, 22, e21366. [Google Scholar] [CrossRef] [PubMed]
- Shao, R.; Shi, Z.; Zhang, D. Social Media and Emotional Burnout Regulation during the COVID-19 Pandemic: Multilevel Approach. J. Med. Internet Res. 2021, 23, e27015. [Google Scholar] [CrossRef] [PubMed]
- Dyrbye, L.N.; Leep Hunderfund, A.N.; Winters, R.C.; Moeschler, S.M.; Vaa Stelling, B.E.; Dozois, E.J.; Satele, D.V.; West, C.P. The Relationship between Burnout and Help-Seeking Behaviors, Concerns, and Attitudes of Residents. Acad. Med. 2020, 96, 701–708. [Google Scholar] [CrossRef]
- Hong, Y.A.; Zhou, Z.; Fang, Y.; Shi, L. The Digital Divide and Health Disparities in China: Evidence from a National Survey and Policy Implications. J. Med. Internet Res. 2017, 19, e317. [Google Scholar] [CrossRef]
- Helsper, E.J. A Corresponding Fields Model for the Links between Social and Digital Exclusion. Commun. Theory 2012, 22, 403–426. [Google Scholar] [CrossRef] [Green Version]
- Philip, L.; Cottrill, C.; Farrington, J.; Williams, F.; Ashmore, F. The digital divide: Patterns, policy and scenarios for connecting the ‘final few’ in rural communities across Great Britain. J. Rural. Stud. 2017, 54, 386–398. [Google Scholar] [CrossRef] [Green Version]
- Neter, E.; Brainin, E. eHealth literacy: Extending the digital divide to the realm of health information. J. Med. Internet Res. 2012, 14, e19. [Google Scholar] [CrossRef]
- Too, L.S.; Leach, L.; Butterworth, P. Mental Health Problems and Internet Access: Results from an Australian National Household Survey. JMIR Ment. Health 2020, 7, e14825. [Google Scholar] [CrossRef]
- Spanakis, P.; Peckham, E.; Mathers, A.; Shiers, D.; Gilbody, S. The digital divide: Amplifying health inequalities for people with severe mental illness in the time of COVID-19. Br. J. Psychiatry 2021, 219, 529–531. [Google Scholar] [CrossRef] [PubMed]



| Factors | No. (%)/Mean (SD) |
|---|---|
| Overall | 18,804 (100.0) |
| Gender | |
| Male | 8558 (45.5) |
| Female | 10,246 (54.5) |
| Mean for age (SD) | 36.6 (8.2) |
| Age group (years) | |
| 18–39 | 12,364 (65.8) |
| ≥40 | 6440 (34.2) |
| Living area | |
| Urban | 17,599 (93.6) |
| Rural | 1205 (6.4) |
| Educational level | |
| College school or higher | 15,489 (82.4) |
| Lower than college school | 3315 (17.6) |
| Marital status | |
| Married | 14,783 (78.6) |
| Unmarried | 4021 (21.4) |
| Income level (CNY) | |
| 0–4999 | 4186 (22.3) |
| ≥5000 | 14,618 (77.7) |
| History of chronic diseases | |
| Yes | 1201 (6.4) |
| Unknown/no | 17,603 (93.6) |
| History of mental disorders | |
| Yes | 122 (0.6) |
| Unknown/no | 18,682 (99.4) |
| Family history of mental disorders | |
| Yes | 235 (1.2) |
| Unknown/no | 18,569 (98.8) |
| Influencing Factors of the Intercept | B (SE) | p Value |
|---|---|---|
| Gender: male (vs. female) | 0.11 (0.04) | 0.008 |
| Age group: 18–39 (vs. ≥40) | 0.34 (0.04) | <0.001 |
| Living area: urban (vs. rural) | −0.13 (0.08) | 0.12 |
| Educational level: college school or higher (vs. lower than college school) | 0.07 (0.06) | 0.24 |
| Marital status: married (vs. unmarried) | −0.01 (0.05) | 0.87 |
| Family monthly income: 0–4999 (vs. ≥5000) | 0.09 (0.05) | 0.06 |
| COVID-19 patients or close contacts: yes (vs. no) | 0.06 (0.17) | 0.72 |
| Engaging in COVID-19-related work: yes (vs. no) | 0.12 (0.04) | 0.005 |
| Living in places severely affected by COVID-19: yes (vs. no) | 0.19 (0.05) | <0.001 |
| Quarantine: yes (vs. no) | 0.39 (0.04) | <0.001 |
| Increases in workload due to COVID-19: yes (vs. no) | 0.49 (0.04) | <0.001 |
| Unemployment due to COVID-19: yes (vs. no) | 0.43 (0.06) | <0.001 |
| Seeking psychological intervention: yes (vs. no) | 0.74 (0.06) | <0.001 |
| Influencing Factors of the Slope | B (SE) | p Value |
| Gender: male (vs. female) | 0.05 (0.01) | <0.001 |
| Age group: 18–39 (vs. ≥40) | 0.004 (0.014) | 0.77 |
| Living area: urban (vs. rural) | −0.02 (0.03) | 0.42 |
| Educational level: college school or higher (vs. lower than college school) | −0.02 (0.02) | 0.40 |
| Marital status: married (vs. unmarried) | −0.04 (0.02) | 0.004 |
| Family monthly income: 0–4999 (vs. ≥5000) | 0.03 (0.02) | 0.05 |
| COVID-19 patients or close contacts: yes (vs. no) | 0.20 (0.05) | <0.001 |
| Engaging in COVID-19-related work: yes (vs. no) | 0.08 (0.01) | <0.001 |
| Living in places severely affected by COVID-19: yes (vs. no) | 0.02 (0.02) | 0.13 |
| Quarantine: yes (vs. no) | −0.002 (0.014) | 0.90 |
| Increases in workload due to COVID-19: yes (vs. no) | 0.05 (0.01) | <0.001 |
| Unemployment due to COVID-19: yes (vs. no) | 0.05 (0.02) | 0.03 |
| Seeking psychological intervention: yes (vs. no) | 0.18 (0.02) | <0.001 |
| Number of Classes | AIC | BIC | aBIC | p Value for LMR-LRT | Entropy | Proportion for Latent Classes (%) |
|---|---|---|---|---|---|---|
| 1 class | 263,472.560 | 263,558.820 | 263,523.863 | / | / | / |
| 2 classes | 262,405.602 | 262,515.388 | 262,470.896 | <0.001 | 0.601 | 52.0/48.0 |
| 3 classes | 260,174.652 | 260,307.963 | 260,253.938 | <0.001 | 0.774 | 55.4/38.3/6.3 |
| 4 classes | 258,529.998 | 258,686.835 | 258,623.276 | <0.001 | 0.783 | 44.4/31.2/18.1/6.3 |
| 5 classes | 256,087.821 | 256,268.183 | 256,195.091 | <0.001 | 0.850 | 41.5/31.1/18.0/6.8/2.7 |
| 6 classes | 255,050.510 | 255,254.397 | 255,171.771 | <0.001 | 0.849 | 32.3/31.9/18.9/7.5/6.8/2.7 |
| 7 classes | 254,905.117 | 255,132.530 | 255,040.370 | <0.001 | 0.803 | 35.2/26.3/18.0/6.9/6.8/4.2/2.7 |
| Factors | Lowest–Great Increase (N = 1191) | Moderate Low–Slight Increase (N = 8347) | Moderate High–Slight Decrease (N = 3405) | Highest–Great Decrease (N = 5861) |
|---|---|---|---|---|
| Gender | ||||
| Male | 570 (47.9) b,c | 3899 (46.7) b,c | 1492 (43.8) | 2597 (44.3) |
| Female | 621 (52.1) | 4448 (53.3) | 1913 (56.2) | 3264 (55.7) |
| Age group (years) | ||||
| 18–39 | 804 (67.5) c | 5703 (68.3) c | 2269 (66.6) c | 3588 (61.2) |
| ≥40 | 387 (32.5) | 2644 (31.7) | 1136 (33.4) | 2273 (38.8) |
| Living area | ||||
| Urban | 1105 (92.8) | 7787 (93.3) c | 3191 (93.7) | 5516 (94.1) |
| Rural | 86 (7.2) | 560 (6.7) | 214 (6.3) | 345 (5.9) |
| Educational level | ||||
| College school or higher | 929 (78.0) a,b,c | 6961 (83.4) c | 2874 (84.4) c | 4725 (80.6) |
| Lower than college school | 262 (22.0) | 1386 (16.6) | 531 (15.6) | 1136 (19.4) |
| Marital status | ||||
| Married | 956 (80.3) | 6531 (78.2) | 2642 (77.6) c | 4654 (79.4) |
| Unmarried | 235 (19.7) | 1816 (21.8) | 763 (22.4) | 1207 (20.6) |
| Family income level (CNY) | ||||
| 0–4999 | 295 (24.8) b | 1896 (22.7) b | 695 (20.4) c | 1300 (22.2) |
| ≥5000 | 896 (75.2) | 6451 (77.3) | 2710 (79.6) | 4561 (77.8) |
| COVID-19 patients or close contacts | ||||
| Yes | 15 (1.3) | 139 (1.7) b | 39 (1.1) | 81 (1.4) |
| No | 1176 (98.7) | 8208 (98.3) | 3366 (98.9) | 5780 (98.6) |
| Engaged in work related to COVID-19 | ||||
| Yes | 474 (39.8) b,c | 3122 (37.4) | 1231 (36.2) | 2104 (35.9) |
| No | 717 (60.2) | 5225 (62.6) | 2174 (63.8) | 3757 (64.1) |
| Quarantine | ||||
| Yes | 492 (41.3) a,b,c | 2947 (35.3) c | 1190 (34.9) c | 1751 (29.9) |
| No | 699 (58.7) | 5400 (64.7) | 2215 (65.1) | 4110 (70.1) |
| Living in places severely affected by COVID-19 | ||||
| Yes | 347 (29.1) | 2578 (30.9) b,c | 933 (27.4) | 1598 (27.3) |
| No | 844 (70.9) | 5769 (69.1) | 2472 (72.6) | 4263 (72.7) |
| Increases in workload due to COVID-19 | ||||
| Yes | 613 (51.5) b,c | 4295 (51.5) b,c | 1527 (44.8) c | 2364 (40.3) |
| No | 578 (48.5) | 4052 (48.5) | 1878 (55.2) | 3497 (59.7) |
| Unemployment due to COVID-19 | ||||
| Yes | 215 (18.1) a,b,c | 1266 (15.2) b,c | 379 (11.1) | 698 (11.9) |
| No | 976 (81.9) | 7081 (84.8) | 3026 (88.9) | 5163 (88.1) |
| Seeking psychological consultation | ||||
| Yes | 272 (22.8) a,b,c | 1363 (16.3) b,c | 424 (12.5) c | 561 (9.6) |
| No | 919 (77.2) | 6984 (83.7) | 2981 (87.5) | 5300 (90.4) |
| Trajectory Class of Perceived Accessibility to DMHSs during COVID-19 | n/N (%) of Mental Health Symptoms from Survey 1 (N = 16,508) | n/N (%) of Mental Health Symptoms from Survey 2 (N = 12,788) | n/N (%) of Mental Health Symptoms from Survey 3 (N = 13,175) | AOR (95% CI) * | p Value | Rate Decrease from Survey 1 to Survey 3 (% (95% CI)) |
|---|---|---|---|---|---|---|
| Any mental health symptoms | ||||||
| Lowest– great increase | 733/1186 (61.8) | 463/828 (55.9) | 342/736 (46.5) | 2.75 (2.47–3.05) | <0.001 | 15.3 (10.7–19.9) |
| Moderate low–slight increase | 3890/6907 (56.3) | 3070/5778 (53.1) | 2746/6024 (45.6) | 2.56 (2.41–2.72) | <0.001 | 10.7 (9.0–12.5) |
| Moderate high–slight decrease | 1479/3389 (43.6) | 946/2141 (44.2) | 830/2281 (36.4) | 1.79 (1.66–1.93) | <0.001 | 7.3 (4.6–9.9) |
| Highest–great decrease | 1414/5026 (28.1) | 1207/4041 (29.9) | 993/4134 (24.0) | Reference | Reference | 4.1 (2.3–5.9) |
| Depression | ||||||
| Lowest– great increase | 536/1186 (45.2) | 379/828 (45.8) | 251/736 (34.1) | 2.92 (2.61–3.27) | <0.001 | 11.1 (6.5–15.6) |
| Moderate low–slight increase | 2609/6907 (37.8) | 2275/5778 (39.4) | 1999/6024 (33.2) | 2.52 (2.36–2.70) | <0.001 | 4.6 (3.0–6.3) |
| Moderate high–slight decrease | 902/3389 (26.6) | 670/2141 (31.3) | 562/2281 (24.6) | 1.77 (1.62–1.92) | <0.001 | 2.0 (−0.4–4.3) |
| Highest–great decrease | 786/5026 (15.6) | 792/4041 (19.6) | 632/4134 (15.3) | Reference | Reference | 0.4 (−1.2–1.9) |
| Anxiety | ||||||
| Lowest– great increase | 603/1186 (50.8) | 363/828 (43.8) | 230/736 (31.3) | 3.01 (2.70–3.36) | <0.001 | 19.6 (15.1–24.0) |
| Moderate low–slight increase | 2996/6907 (43.4) | 2224/5778 (38.5) | 1847/6024 (30.7) | 2.64 (2.47–2.83) | <0.001 | 12.7 (11.1–14.4) |
| Moderate high–slight decrease | 1037/3389 (30.6) | 645/2141 (30.1) | 501/2281 (22.0) | 1.78 (1.64–1.94) | <0.001 | 8.6 (6.3–10.9) |
| Highest–great decrease | 937/5026 (18.6) | 758/4041 (18.8) | 551/4134 (13.3) | Reference | Reference | 5.3 (3.8–6.8) |
| Insomnia | ||||||
| Lowest– great increase | 521/1186 (43.9) | 379/828 (45.8) | 272/736 (37.0) | 2.58 (2.31–2.88) | <0.001 | 7.0 (2.4–11.5) |
| Moderate low–slight increase | 2589/6907 (37.5) | 2408/5778 (41.7) | 2123/6024 (35.2) | 2.29 (2.14–2.45) | <0.001 | 2.2 (0.6–3.9) |
| Moderate high–slight decrease | 924/3389 (27.3) | 704/2141 (32.9) | 624/2281 (27.4) | 1.63 (1.50–1.78) | <0.001 | −0.1 (−2.5–2.3) |
| Highest–great decrease | 843/5026 (16.8) | 874/4041 (21.6) | 763/4134 (18.5) | Reference | Reference | −1.7 (−3.3–0.1) |
| Trajectory Class of Perceived Accessibility to DMHSs during COVID-19 | Median (IQR) of Mental Health Scores from Survey 1 | Median (IQR) of Mental Health Scores from Survey 2 | Median (IQR) of Mental Health Scores from Survey 3 | B (SE) for Main Effect * | p Value | B (SE) for Interaction with Time * | p Value |
|---|---|---|---|---|---|---|---|
| Depression | |||||||
| Lowest–great increase | 3.00 (0.00–9.00) | 3.00 (0.00–10.00) | 0.00 (0.00–9.00) | 2.67 (0.12) | <0.001 | −0.05 (0.01) | <0.001 |
| Moderate low–slight increase | 2.00 (0.00–9.00) | 1.00 (0.00–9.00) | 0.00 (0.00–8.00) | 1.71 (0.06) | <0.001 | −0.03 (0.00) | <0.001 |
| Moderate high–slight decrease | 0.00 (0.00–5.00) | 0.00 (0.00–7.00) | 0.00 (0.00–4.00) | 0.84 (0.08) | <0.001 | −0.01 (0.00) | 0.10 |
| Highest–great decrease | 0.00 (0.00–1.00) | 0.00 (0.00–2.00) | 0.00 (0.00–1.00) | Reference | Reference | Reference | Reference |
| Anxiety | |||||||
| Lowest–great increase | 5.00 (0.00–9.00) | 2.00 (0.00–8.00) | 0.00 (0.00–7.00) | 2.61 (0.11) | <0.001 | −0.10 (0.01) | <0.001 |
| Moderate low–slight increase | 3.00 (0.00–7.00) | 1.00 (0.00–7.00) | 0.00 (0.00–7.00) | 1.71 (0.05) | <0.001 | −0.06 (0.00) | <0.001 |
| Moderate high–slight decrease | 1.00 (0.00–6.00) | 0.00 (0.00–6.00) | 0.00 (0.00–3.00) | 0.85 (0.07) | <0.001 | −0.03 (0.00) | <0.001 |
| Highest–great decrease | 0.00 (0.00–3.00) | 0.00 (0.00–2.00) | 0.00 (0.00–0.00) | Reference | Reference | Reference | Reference |
| Insomnia | |||||||
| Lowest–great increase | 6.00 (1.00–11.00) | 7.00 (2.00–12.00) | 4.00 (1.00–10.00) | 2.36 (0.12) | <0.001 | −0.05 (0.01) | <0.001 |
| Moderate low–slight increase | 5.00 (2.00–10.00) | 6.00 (2.00–11.00) | 5.00 (1.00–9.00) | 2.00 (0.07) | <0.001 | −0.04 (0.00) | <0.001 |
| Moderate high–slight decrease | 4.00 (1.00–8.00) | 4.00 (1.00–9.00) | 4.00 (1.00–8.00) | 1.09 (0.08) | <0.001 | −0.01 (0.01) | 0.23 |
| Highest–great decrease | 2.00 (0.00–6.00) | 2.00 (0.00–7.00) | 1.00 (0.00–6.00) | Reference | Reference | Reference | Reference |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lu, Z.-A.; Shi, L.; Que, J.-Y.; Zheng, Y.-B.; Wang, Q.-W.; Liu, W.-J.; Huang, Y.-T.; Liu, X.-X.; Yuan, K.; Yan, W.; et al. Accessibility to Digital Mental Health Services among the General Public throughout COVID-19: Trajectories, Influencing Factors and Association with Long-Term Mental Health Symptoms. Int. J. Environ. Res. Public Health 2022, 19, 3593. https://doi.org/10.3390/ijerph19063593
Lu Z-A, Shi L, Que J-Y, Zheng Y-B, Wang Q-W, Liu W-J, Huang Y-T, Liu X-X, Yuan K, Yan W, et al. Accessibility to Digital Mental Health Services among the General Public throughout COVID-19: Trajectories, Influencing Factors and Association with Long-Term Mental Health Symptoms. International Journal of Environmental Research and Public Health. 2022; 19(6):3593. https://doi.org/10.3390/ijerph19063593
Chicago/Turabian StyleLu, Zheng-An, Le Shi, Jian-Yu Que, Yong-Bo Zheng, Qian-Wen Wang, Wei-Jian Liu, Yue-Tong Huang, Xiao-Xing Liu, Kai Yuan, Wei Yan, and et al. 2022. "Accessibility to Digital Mental Health Services among the General Public throughout COVID-19: Trajectories, Influencing Factors and Association with Long-Term Mental Health Symptoms" International Journal of Environmental Research and Public Health 19, no. 6: 3593. https://doi.org/10.3390/ijerph19063593





