Association between Changes in the Regularity of Working Hours and Cognitive Impairment in Middle-Aged and Older Korean Workers: The Korean Longitudinal Study of Aging, 2008–2018
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data and Study Population
2.2. Variables
2.3. Statistical Analysis
3. Results
3.1. Descriptive Statistics
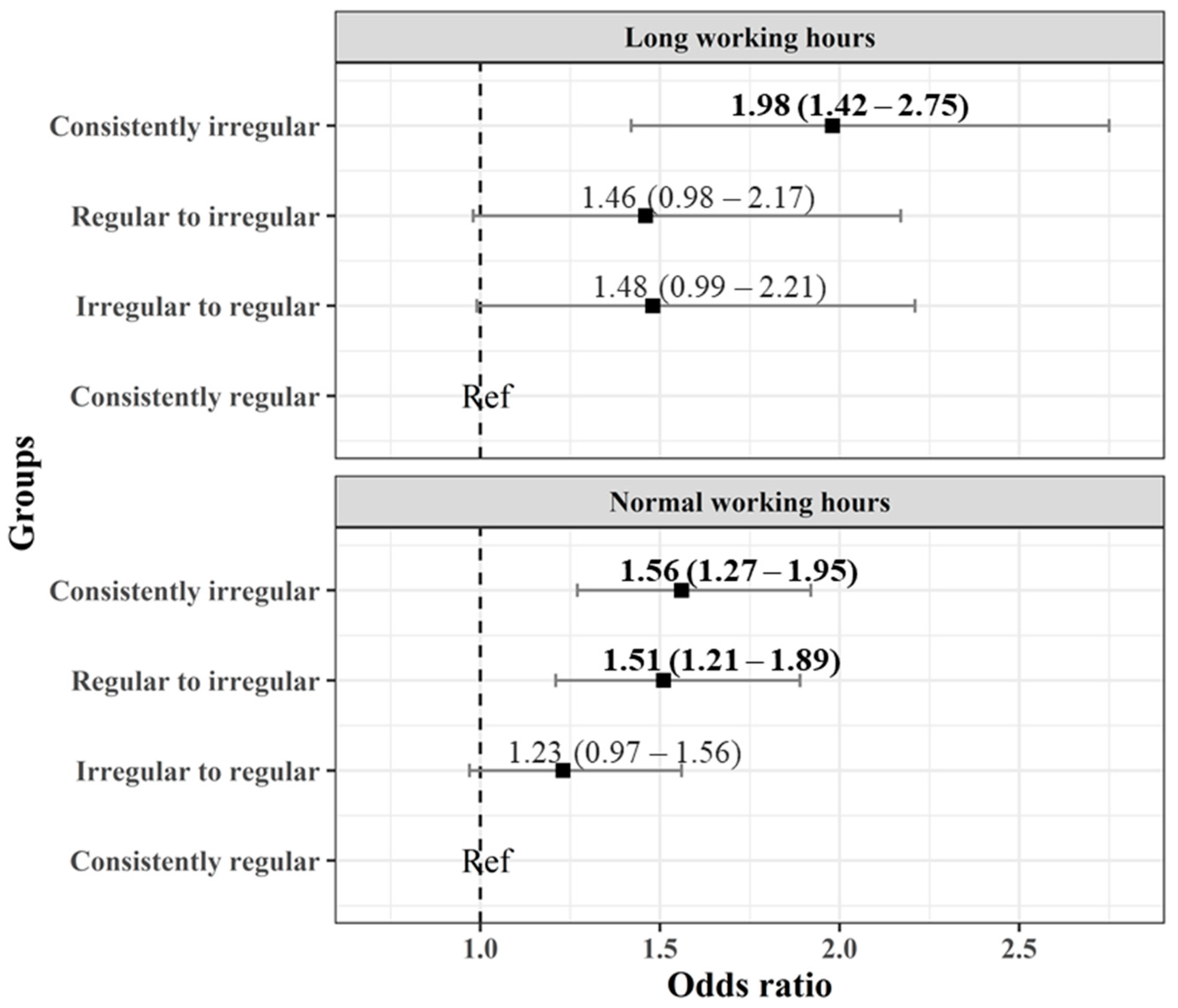
3.2. The GEE Model Analysis
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- George, E.; Chattopadhyay, P. Non-Standard Work and Workers: Organizational Implications; ILO: Geneva, Switzerland, 2015. [Google Scholar]
- Folkard, S.; Tucker, P. Shift work, safety and productivity. Occup. Med. 2003, 53, 95–101. [Google Scholar] [CrossRef] [Green Version]
- Ryu, J.; Jung-Choi, K.; Choi, K.-H.; Kwon, H.-J.; Kang, C.; Kim, H. Associations of Shift Work and Its Duration with Work-Related Injury among Electronics Factory Workers in South Korea. Int. J. Environ. Res. Public Health 2017, 14, 1429. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Boivin, D.B.; Tremblay, G.M.; James, F.O. Working on atypical schedules. Sleep Med. 2007, 8, 578–589. [Google Scholar] [CrossRef]
- Bardasi, E.; Francesconi, M. The Impact of Atypical Employment on Individual Wellbeing: Evidence from a Panel of British Workers. Soc. Sci. Med. 2004, 58, 1671–1688. [Google Scholar] [CrossRef] [Green Version]
- Lin, P.-C.; Chen, C.-H.; Pan, S.-M.; Pan, C.-H.; Chen, C.-J.; Chen, Y.-M.; Hung, H.-C.; Wu, M.-T. Atypical work schedules are associated with poor sleep quality and mental health in Taiwan female nurses. Int. Arch. Occup. Environ. Health 2012, 85, 877–884. [Google Scholar] [CrossRef] [PubMed]
- Wimo, A.; Guerchet, M.; Ali, G.C.; Wu, Y.T.; Prina, A.M.; Winblad, B.; Jönsson, L.; Liu, Z.; Prince, M. The worldwide costs of dementia 2015 and comparisons with 2010. Alzheimer’s Dement. 2017, 13, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Hampel, H.; Lista, S. The rising global tide of cognitive impairment. Nat. Rev. Neurol. 2016, 12, 131–132. [Google Scholar] [CrossRef]
- Ballard, C.; Gauthier, S.; Corbett, A.; Brayne, C.; Aarsland, D.; Jones, E. Alzheimer’s disease. Lancet 2011, 377, 1019–1031. [Google Scholar] [CrossRef]
- Hansen, E.C.; Hughes, C.; Routley, G.; Robinson, A.L. General practitioners’ experiences and understandings of diagnosing dementia: Factors impacting on early diagnosis. Soc. Sci. Med. 2008, 67, 1776–1783. [Google Scholar] [CrossRef]
- Korea, S. Korean Population and Housing Census. 2020. Available online: https://kostat.go.kr/portal/korea/kor_nw/1/2/2/index.board?bmode=read&bSeq=&aSeq=391020&pageNo=1&rowNum=10&navCount=10&currPg=&searchInfo=&sTarget=title&sTxt= (accessed on 30 July 2021).
- Virtanen, M.; Singh-Manoux, A.; Ferrie, J.E.; Gimeno, D.; Marmot, M.G.; Elovainio, M.; Jokela, M.; Vahtera, J.; Kivimäki, M. Long Working Hours and Cognitive Function: The Whitehall II Study. Am. J. Epidemiol. 2009, 169, 596–605. [Google Scholar] [CrossRef]
- Then, F.S.; Luck, T.; Luppa, M.; Thinschmidt, M.; Deckert, S.; Nieuwenhuijsen, K.; Seidler, A.; Riedel-Heller, S.G. Systematic review of the effect of the psychosocial working environment on cognition and dementia. Occup. Environ. Med. 2014, 71, 358–365. [Google Scholar] [CrossRef] [PubMed]
- Kang, Y.; Na, D.L.; Hahn, S. A validity study on the Korean Mini-Mental State Examination (K-MMSE) in dementia patients. J. Korean Neurol. Assoc. 1997, 15, 300–308. [Google Scholar]
- Kvitting, A.S.; Fällman, K.; Wressle, E.; Marcusson, J. Age-Normative MMSE Data for Older Persons Aged 85 to 93 in a Longitudinal Swedish Cohort. J. Am. Geriatr. Soc. 2019, 67, 534–538. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Han, C.; Jo, S.A.; Jo, I.; Kim, E.; Park, M.H.; Kang, Y. An adaptation of the Korean mini-mental state examination (K-MMSE) in elderly Koreans: Demographic influence and population-based norms (the AGE study). Arch. Gerontol. Geriatr. 2008, 47, 302–310. [Google Scholar] [CrossRef]
- Kang, Y. A Normative Study of the Korean-Mini Mental State Examination (K-MMSE) in the Elderly. Korean J. Psychol. 2006, 25, 1–12. [Google Scholar]
- Folstein, M.F.; Folstein, S.E.; McHugh, P.R. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 1975, 12, 189–198. [Google Scholar] [CrossRef]
- Iverson, G.L. Interpretation of Mini-Mental State Examination scores in community-dwelling elderly and geriatric neuropsychiatry patients. Int. J. Geriatr. Psychiatry 1998, 13, 661–666. [Google Scholar] [CrossRef]
- Freitas, S.; Simões, M.R.; Alves, L.; Santana, I. The Relevance of Sociodemographic and Health Variables on MMSE Normative Data. Appl. Neuropsychol. Adult 2015, 22, 311–319. [Google Scholar] [CrossRef]
- Aggarwal, H.K.; Jain, D.; Bhavikatti, A. Cognitive Dysfunction in Patients with Chronic Kidney Disease. Saudi J. Kidney Dis. Transpl. 2020, 31, 796–804. [Google Scholar] [CrossRef]
- Boo, Y.Y.; Jutila, O.E.; Cupp, M.A.; Manikam, L.; Cho, S.I. The identification of established modifiable mid-life risk factors for cardiovascular disease which contribute to cognitive decline: Korean Longitudinal Study of Aging (KLoSA). Aging Clin. Exp. Res. 2021, 33, 2573–2586. [Google Scholar] [CrossRef]
- Nicholson, P.J.; D’Auria, D.A.P. Shift work, health, the working time regulations and health assessments. Occup. Med. 1999, 49, 127–137. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rouch, I.; Wild, P.; Ansiau, D.; Marquié, J.C. Shiftwork experience, age and cognitive performance. Ergonomics 2005, 48, 1282–1293. [Google Scholar] [CrossRef] [PubMed]
- Marquié, J.-C.; Tucker, P.; Folkard, S.; Gentil, C.; Ansiau, D. Chronic effects of shift work on cognition: Findings from the VISAT longitudinal study. Occup. Environ. Med. 2015, 72, 258. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ansiau, D.; Wild, P.; Niezborala, M.; Rouch, I.; Marquié, J.C. Effects of working conditions and sleep of the previous day on cognitive performance. Appl. Ergon. 2008, 39, 99–106. [Google Scholar] [CrossRef]
- Bokenberger, K.; Ström, P.; Dahl Aslan, A.K.; Åkerstedt, T.; Pedersen, N.L. Shift work and cognitive aging: A longitudinal study. Scand. J. Work Environ. Health 2017, 43, 485–493. [Google Scholar] [CrossRef] [Green Version]
- Devore, E.E.; Grodstein, F.; Schernhammer, E.S. Shift work and cognition in the Nurses’ Health Study. Am. J. Epidemiol. 2013, 178, 1296–1300. [Google Scholar] [CrossRef] [Green Version]
- Marioni, R.E.; Proust-Lima, C.; Amieva, H.; Brayne, C.; Matthews, F.E.; Dartigues, J.-F.; Jacqmin-Gadda, H. Social activity, cognitive decline and dementia risk: A 20-year prospective cohort study. BMC Public Health 2015, 15, 1089. [Google Scholar] [CrossRef] [Green Version]
- Qiu, C.; Winblad, B.; Marengoni, A.; Klarin, I.; Fastbom, J.; Fratiglioni, L. Heart Failure and Risk of Dementia and Alzheimer Disease: A Population-Based Cohort Study. Arch. Intern. Med. 2006, 166, 1003–1008. [Google Scholar] [CrossRef] [Green Version]
- Faraco, G.; Iadecola, C. Hypertension: A harbinger of stroke and dementia. Hypertension 2013, 62, 810–817. [Google Scholar] [CrossRef] [Green Version]
- Kuo, S.-C.; Lai, S.-W.; Hung, H.-C.; Muo, C.-H.; Hung, S.-C.; Liu, L.-L.; Chang, C.-W.; Hwu, Y.-J.; Chen, S.-L.; Sung, F.-C. Association between comorbidities and dementia in diabetes mellitus patients: Population-based retrospective cohort study. J. Diabetes Its Complicat. 2015, 29, 1071–1076. [Google Scholar] [CrossRef]
- Nabe-Nielsen, K.; Garde, A.H.; Aust, B.; Diderichsen, F. Increasing work-time influence: Consequences for flexibility, variability, regularity and predictability. Ergonomics 2012, 55, 440–449. [Google Scholar] [CrossRef] [PubMed]
- Nabe-Nielsen, K.; Garde, A.H.; Ishtiak-Ahmed, K.; Gyntelberg, F.; Mortensen, E.L.; Phung, T.K.T.; Rod, N.H.; Waldemar, G.; Westendorp, R.G.; Hansen, Å.M. Shift work, long working hours, and later risk of dementia: A long-term follow-up of the Copenhagen Male Study. Scand. J. Work. Environ. Health 2017, 43, 569–577. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Scheer, F.A.J.L.; Hilton, M.F.; Mantzoros, C.S.; Shea, S.A. Adverse metabolic and cardiovascular consequences of circadian misalignment. Proc. Natl. Acad. Sci. USA 2009, 106, 4453–4458. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baron, K.G.; Reid, K.J. Circadian misalignment and health. Int. Rev. Psychiatry 2014, 26, 139–154. [Google Scholar] [CrossRef] [Green Version]
- Tranah, G.J.; Blackwell, T.; Ancoli-Israel, S.; Paudel, M.L.; Ensrud, K.E.; Cauley, J.A.; Redline, S.; Hillier, T.A.; Cummings, S.R.; Stone, K.L. Circadian activity rhythms and mortality: The study of osteoporotic fractures. J. Am. Geriatr. Soc. 2010, 58, 282–291. [Google Scholar] [CrossRef]
- Leng, Y.; Musiek, E.S.; Hu, K.; Cappuccio, F.P.; Yaffe, K. Association between circadian rhythms and neurodegenerative diseases. Lancet Neurol. 2019, 18, 307–318. [Google Scholar] [CrossRef]
- Musiek, E.S.; Lim, M.M.; Yang, G.; Bauer, A.Q.; Qi, L.; Lee, Y.; Roh, J.H.; Ortiz-Gonzalez, X.; Dearborn, J.T.; Culver, J.P.; et al. Circadian clock proteins regulate neuronal redox homeostasis and neurodegeneration. J. Clin. Investig. 2013, 123, 5389–5400. [Google Scholar] [CrossRef]
- Cronin, P.; McCarthy, M.J.; Lim, A.S.P.; Salmon, D.P.; Galasko, D.; Masliah, E.; De Jager, P.L.; Bennett, D.A.; Desplats, P. Circadian alterations during early stages of Alzheimer’s disease are associated with aberrant cycles of DNA methylation in BMAL1. Alzheimer’s Dement. 2017, 13, 689–700. [Google Scholar] [CrossRef]
- Kress, G.J.; Liao, F.; Dimitry, J.; Cedeno, M.R.; FitzGerald, G.A.; Holtzman, D.M.; Musiek, E.S. Regulation of amyloid-β dynamics and pathology by the circadian clock. J. Exp. Med. 2018, 215, 1059–1068. [Google Scholar] [CrossRef]
- Conrad, C.D. Chronic stress-induced hippocampal vulnerability: The glucocorticoid vulnerability hypothesis. Rev. Neurosci. 2008, 19, 395–412. [Google Scholar] [CrossRef] [Green Version]
- Naugle, R.I.; Kawczak, K. Limitations of the Mini-Mental State Examination. Cleve Clin. J. Med. 1989, 56, 277–281. [Google Scholar] [CrossRef] [PubMed]
- Stewart, S.; O’Riley, A.; Edelstein, B.; Gould, C. A Preliminary Comparison of Three Cognitive Screening Instruments in Long Term Care: The MMSE, SLUMS, and MoCA. Clin. Gerontol. 2012, 35, 57–75. [Google Scholar] [CrossRef]
- Nasreddine, Z.S.; Phillips, N.A.; Bédirian, V.; Charbonneau, S.; Whitehead, V.; Collin, I.; Cummings, J.L.; Chertkow, H. The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment. J. Am. Geriatr. Soc. 2005, 53, 695–699. [Google Scholar] [CrossRef] [PubMed]
- Doherty, R.W.; Orimoto, L.; Singelis, T.M.; Hatfield, E.; Hebb, J. Emotional Contagion: Gender and Occupational Differences. Psychol. Women Q. 1995, 19, 355–371. [Google Scholar] [CrossRef]

| Total | Noncognitive Impairment | Cognitive Impairment | p-Value | |
|---|---|---|---|---|
| (n = 3826) | (n = 3361) | (n = 465) | ||
| MMSE | ||||
| Mean (SD) | 27.2 (± 3.42) | 28.2 (± 1.83) | 19.9 (± 3.54) | <0.001 |
| Work regularity (baseline) | ||||
| Regular | 2029 (53.0%) | 1862 (55.4%) | 167 (35.9%) | <0.001 |
| Irregular | 1797 (47.0%) | 1499 (44.6%) | 298 (64.1%) | |
| Changes in work regularity | ||||
| Consistently irregular | 1215 (31.8%) | 979 (29.1%) | 236 (50.8%) | <0.001 |
| Regular to irregular | 531 (13.9%) | 462 (13.7%) | 69 (14.8%) | |
| Irregular to regular | 582 (15.2%) | 520 (15.5%) | 62 (13.3%) | |
| Consistently regular | 1498 (39.2%) | 1400 (41.7%) | 98 (21.1%) | |
| Sex | ||||
| Male | 2226 (58.2%) | 2031 (60.4%) | 195 (41.9%) | <0.001 |
| Female | 1600 (41.8%) | 1330 (39.6%) | 270 (58.1%) | |
| Age, years | ||||
| 45–54 | 1307 (34.2%) | 1246 (37.1%) | 61 (13.1%) | <0.001 |
| 55–64 | 1464 (38.3%) | 1341 (39.9%) | 123 (26.5%) | |
| 65–74 | 823 (21.5%) | 644 (19.2%) | 179 (38.5%) | |
| 75 or above | 232 (6.1%) | 130 (3.9%) | 102 (21.9%) | |
| Income | ||||
| 1Q | 918 (24.0%) | 662 (19.7%) | 256 (55.1%) | <0.001 |
| 2Q | 985 (25.7%) | 879 (26.2%) | 106 (22.8%) | |
| 3Q | 963 (25.2%) | 894 (26.6%) | 69 (14.8%) | |
| 4Q | 960 (25.1%) | 926 (27.6%) | 34 (7.3%) | |
| Education level | ||||
| Elementary school | 1257 (32.9%) | 925 (27.5%) | 332 (71.4%) | <0.001 |
| Middle school | 718 (18.8%) | 652 (19.4%) | 66 (14.2%) | |
| High school | 1359 (35.5%) | 1304 (38.8%) | 55 (11.8%) | |
| University | 492 (12.9%) | 480 (14.3%) | 12 (2.6%) | |
| Residential area | ||||
| Urban | 1501 (39.2%) | 1384 (41.2%) | 117 (25.2%) | <0.001 |
| Small city | 1223 (32.0%) | 1107 (32.9%) | 116 (24.9%) | |
| Rural | 1102 (28.8%) | 870 (25.9%) | 232 (49.9%) | |
| Marital status | ||||
| Married | 3319 (86.7%) | 2970 (88.4%) | 349 (75.1%) | <0.001 |
| Separated/Not married | 507 (13.3%) | 391 (11.6%) | 116 (24.9%) | |
| Smoking | ||||
| Current smoker | 960 (25.1%) | 882 (26.2%) | 78 (16.8%) | <0.001 |
| Ex-smoker | 619 (16.2%) | 561 (16.7%) | 58 (12.5%) | |
| Non-smoker | 2247 (58.7%) | 1918 (57.1%) | 329 (70.8%) | |
| Drinking | ||||
| Current drinker | 1964 (51.3%) | 1783 (53.0%) | 181 (38.9%) | <0.001 |
| Ex-drinker | 368 (9.6%) | 320 (9.5%) | 48 (10.3%) | |
| Non-smoker | 1494 (39.0%) | 1258 (37.4%) | 236 (50.8%) | |
| Working hours | ||||
| Long | 1153 (30.1%) | 1044 (31.1%) | 109 (23.4%) | <0.001 |
| Normal | 2673 (69.9%) | 2317 (68.9%) | 356 (76.6%) | |
| Chronic disease * | ||||
| Yes | 1409 (36.8%) | 1194 (35.5%) | 215 (46.2%) | <0.001 |
| No | 2417 (63.2%) | 2167 (64.5%) | 250 (53.8%) | |
| Social activity | ||||
| Active | 3155 (82.5%) | 2862 (85.2%) | 293 (63.0%) | <0.001 |
| Inactive | 671 (17.5%) | 499 (14.8%) | 172 (37.0%) | |
| Variable | ORs * | 95% CI |
|---|---|---|
| Regularity | ||
| Consistently regular | 1.00 | Ref |
| Consistently irregular | 1.56 | (1.30–1.88) |
| Regular to irregular | 1.46 | (1.20–1.77) |
| Irregular to regular | 1.24 | (1.01–1.53) |
| Sex | ||
| Male | 1.00 | Ref |
| Female | 1.39 | (1.11–1.74) |
| Age, years | ||
| 45–54 | 1.00 | Ref |
| 55–64 | 1.34 | (1.06–1.70) |
| 65–74 | 2.38 | (1.82–3.11) |
| 75 or above | 3.9 | (2.84–5.34) |
| Income | ||
| 1Q | 1.36 | (1.07–1.73) |
| 2Q | 0.95 | (0.75–1.21) |
| 3Q | 1.06 | (0.84–1.33) |
| 4Q | 1.00 | Ref |
| Education level | ||
| Elementary school | 4.17 | (2.96–5.88) |
| Middle school | 2.4 | (1.68–3.42) |
| High school | 1.51 | (1.08–2.12) |
| University | 1.00 | Ref |
| Residential area | ||
| Urban | 1.00 | Ref |
| Small city | 1.22 | (1.00–1.49) |
| Rural | 1.36 | (1.12–1.65) |
| Marital status | ||
| Married | 1.00 | Ref |
| Separated/Not married | 1.23 | (1.02–1.48) |
| Smoking | ||
| Current smoker | 0.96 | (0.75–1.22) |
| Ex-smoker | 1.00 | (0.78–1.28) |
| Non-smoker | 1.00 | Ref |
| Drinking | ||
| Current drinker | 1.18 | (0.94–1.47) |
| Ex-drinker | 0.99 | (0.83–1.18) |
| Non-smoker | 1.00 | Ref |
| Working hours | ||
| Long | 0.94 | (0.80–1.09) |
| Normal | 1.00 | Ref |
| Chronic disease | ||
| Yes | 1.11 | (0.96–1.28) |
| No | 1.00 | Ref |
| Social activity | ||
| Active | 1.00 | Ref |
| Inactive | 1.98 | (1.70–2.30) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, W.-T.; Lim, S.-S.; Yoon, J.-H.; Won, J.-U. Association between Changes in the Regularity of Working Hours and Cognitive Impairment in Middle-Aged and Older Korean Workers: The Korean Longitudinal Study of Aging, 2008–2018. Int. J. Environ. Res. Public Health 2022, 19, 4161. https://doi.org/10.3390/ijerph19074161
Lee W-T, Lim S-S, Yoon J-H, Won J-U. Association between Changes in the Regularity of Working Hours and Cognitive Impairment in Middle-Aged and Older Korean Workers: The Korean Longitudinal Study of Aging, 2008–2018. International Journal of Environmental Research and Public Health. 2022; 19(7):4161. https://doi.org/10.3390/ijerph19074161
Chicago/Turabian StyleLee, Won-Tae, Sung-Shil Lim, Jin-Ha Yoon, and Jong-Uk Won. 2022. "Association between Changes in the Regularity of Working Hours and Cognitive Impairment in Middle-Aged and Older Korean Workers: The Korean Longitudinal Study of Aging, 2008–2018" International Journal of Environmental Research and Public Health 19, no. 7: 4161. https://doi.org/10.3390/ijerph19074161






