Renal Function in Patients with Cystic Fibrosis: A Single-Center Study
Abstract
1. Introduction
2. Materials and Methods
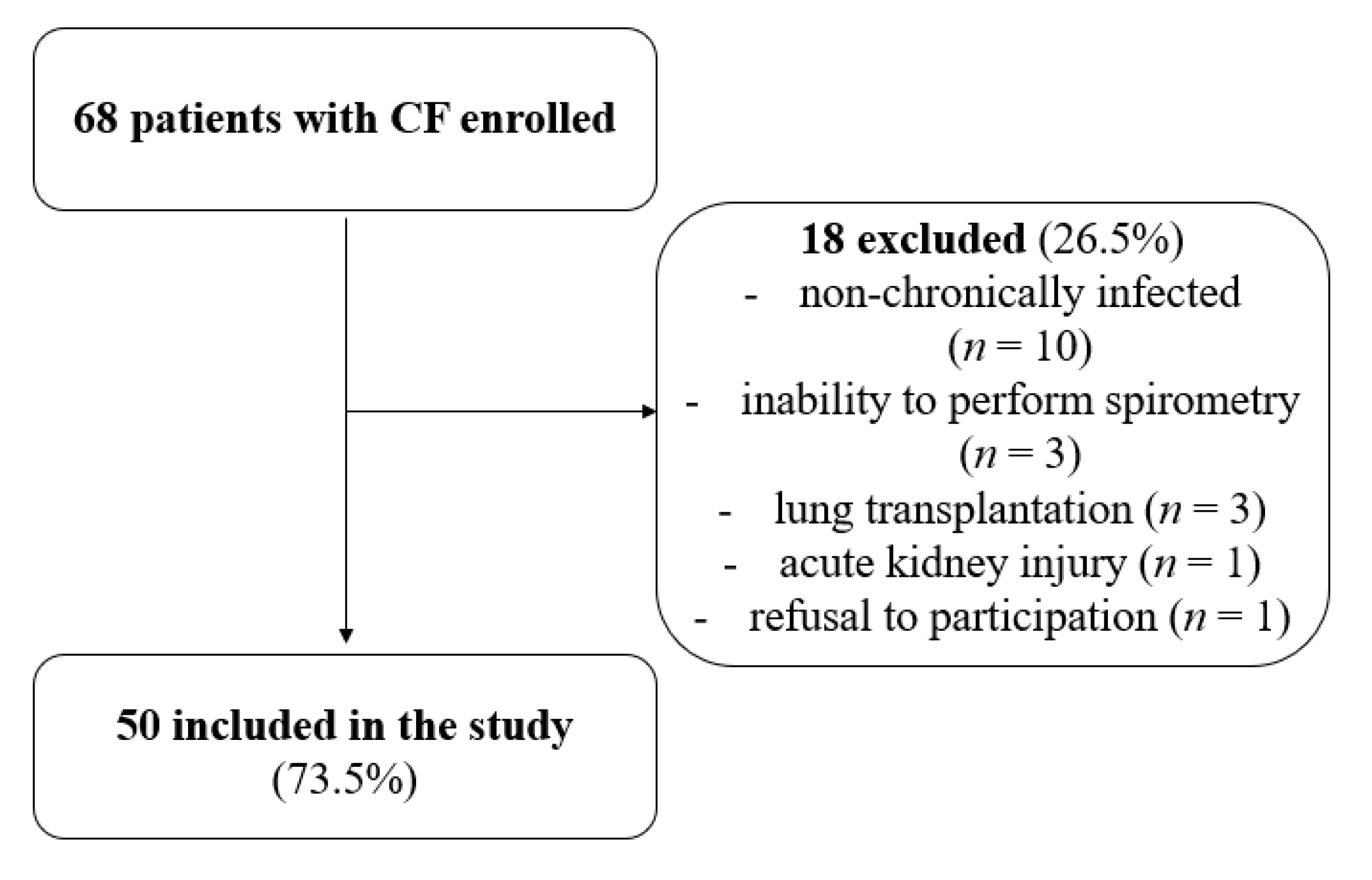
2.1. Study Population
2.2. Inclusion Criteria
2.3. Exclusion Criteria
2.4. Blood Collection
2.5. Urine Collection
2.6. Assessment of Renal Function
2.6.1. Cystatin C (CysC)
2.6.2. Estimating Glomerular Filtration Rate (eGFR)
2.6.3. Serum Creatinine (Cr)
2.6.4. Serum Urea
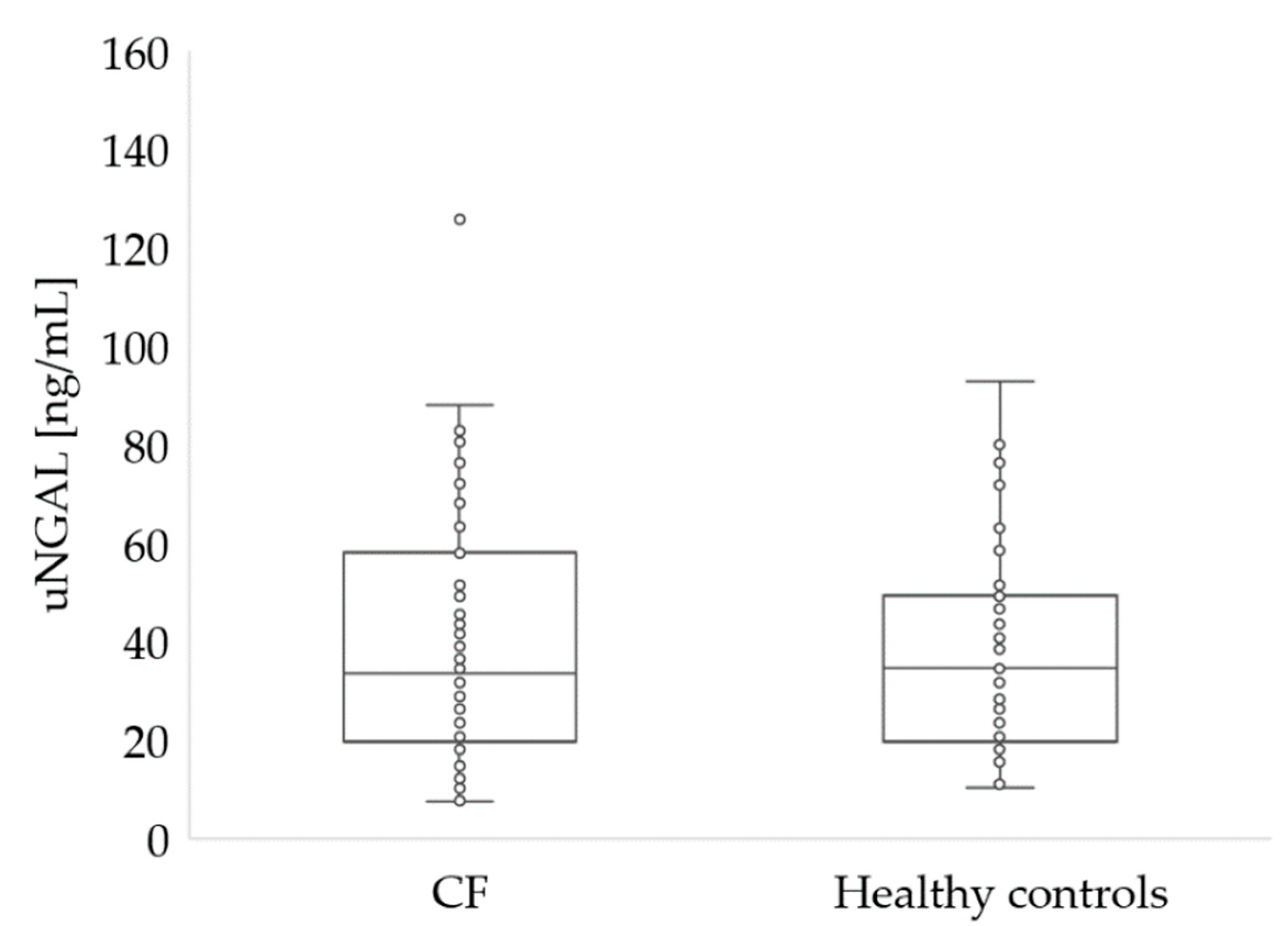
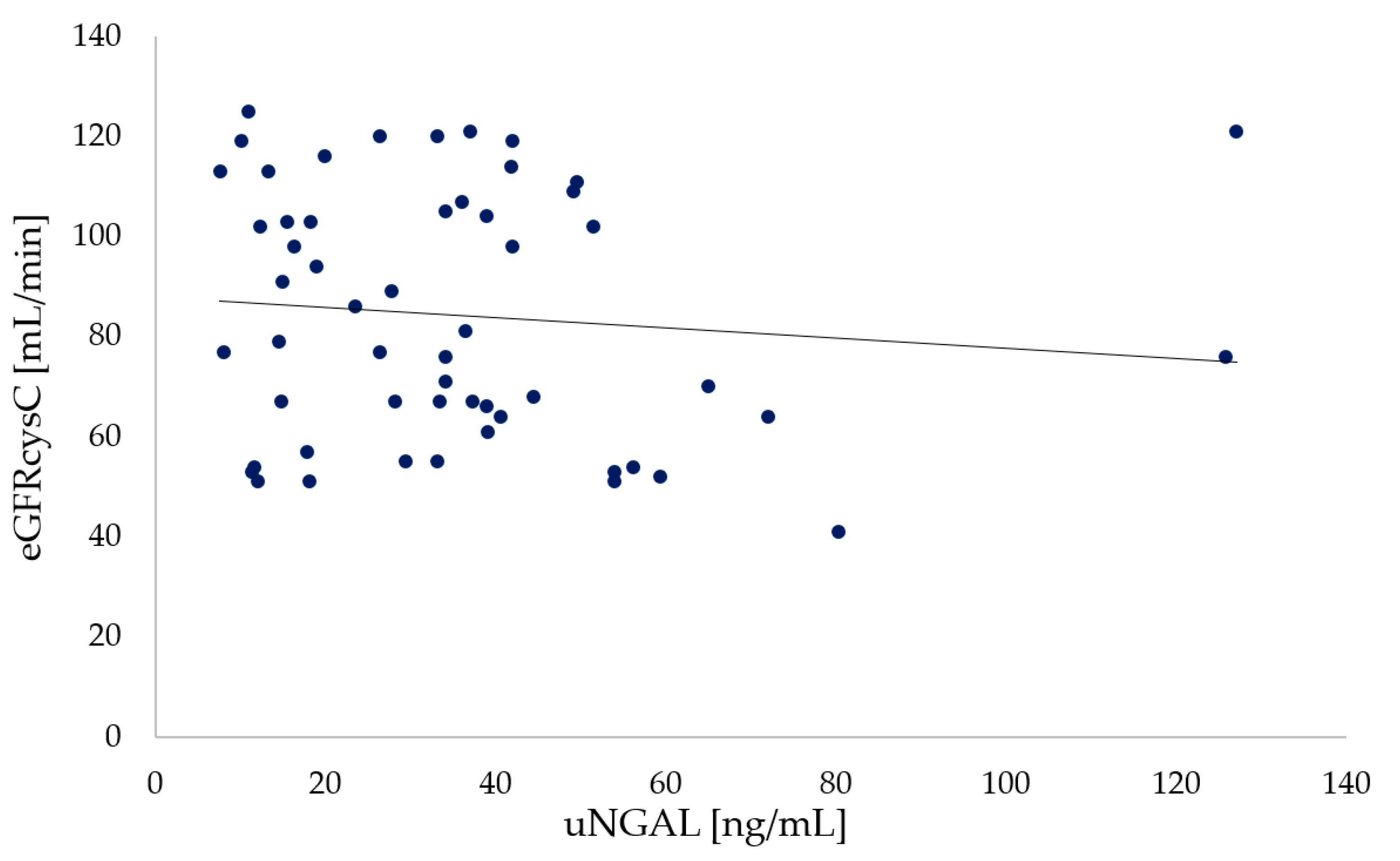
2.6.5. Urine Neutrophil Gelatinase-Associated Lipocalin (uNGAL)
2.7. Sputum Collection
2.8. Spirometry
2.9. Data Analysis
2.10. Ethics
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Rachel, M.; Topolewicz, S.; Śliwczyński, A.; Galiniak, S. Managing Cystic Fibrosis in Polish Healthcare. Int. J. Environ. Res. Public Health 2020, 17, 7630. [Google Scholar] [CrossRef] [PubMed]
- Scotet, V.; L’Hostis, C.; Férec, C. The Changing Epidemiology of Cystic Fibrosis: Incidence, Survival and Impact of the CFTR Gene Discovery. Genes 2020, 11, 589. [Google Scholar] [CrossRef]
- Sanders, D.B.; Fink, A.K. Background and Epidemiology. Pediatr. Clin. N. Am. 2016, 63, 567–584. [Google Scholar] [CrossRef] [PubMed]
- Nazareth, D.; Walshaw, M. A review of renal disease in cystic fibrosis. J. Cyst. Fibros. 2013, 12, 309–317. [Google Scholar] [CrossRef]
- Soulsby, N.; Greville, H.; Coulthard, K.; Doecke, C. Renal dysfunction in cystic fibrosis: Is there cause for concern? Pediatr. Pulmonol. 2009, 44, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Santoro, D.; Postorino, A.; Lucanto, C.; Costa, S.; Cristadoro, S.; Pellegrino, S.; Conti, G.; Buemi, M.; Magazzù, G.; Bellinghieri, G. Cystic Fibrosis: A Risk Condition for Renal Disease. J. Ren. Nutr. 2017, 27, 470–473. [Google Scholar] [CrossRef]
- Nickel, N.P.; O’Leary, J.M.; Brittain, E.L.; Fessel, J.P.; Zamanian, R.T.; West, J.D.; Austin, E.D. Kidney dysfunction in patients with pulmonary arterial hypertension. Pulm. Circ. 2017, 7, 38–54. [Google Scholar] [CrossRef] [PubMed]
- Husain-Syed, F.; McCullough, P.A.; Birk, H.W.; Renker, M.; Brocca, A.; Seeger, W.; Ronco, C. Cardio-Pulmonary-Renal Interactions: A Multidisciplinary Approach. J. Am. Coll. Cardio. 2015, 65, 2433–2448. [Google Scholar] [CrossRef]
- Wilcock, M.J.; Ruddick, A.; Gyi, K.M.; Hodson, M.E. Renal diseases in adults with cystic fibrosis: A 40 year single centre experience. J. Nephrol. 2015, 28, 585–591. [Google Scholar] [CrossRef]
- Lai, S.; Mazzaferro, S.; Mitterhofer, A.P.; Bonci, E.; Marotta, P.G.; Pelligra, F.; Murciano, M.; Celani, C.; Troiani, P.; Cimino, G.; et al. Renal involvement and metabolic alterations in adults patients affected by cystic fibrosis. J. Transl. Med. 2019, 17, 388. [Google Scholar] [CrossRef]
- Simpson, T.; Elston, C.; Macedo, P.; Perrin, F. Amyloidosis in cystic fibrosis. Paediatr. Respir. Rev. 2019, 31, 32–34. [Google Scholar] [CrossRef] [PubMed]
- Traynor, J.; Mactier, R.; Geddes, C.C.; Fox, J.G. How to measure renal function in clinical practice. BMJ 2006, 333, 733–737. [Google Scholar] [CrossRef] [PubMed]
- Wallace, A.; Price, A.; Fleischer, E.; Khoury, M.; Filler, G. Estimation of GFR in Patients With Cystic Fibrosis: A Cross-Sectional Study. Can. J. Kidney Health Dis. 2020, 7, 2054358119899312. [Google Scholar] [CrossRef] [PubMed]
- Shang, W.; Wang, Z. The Update of NGAL in Acute Kidney Injury. Curr. Protein Pept. Sci. 2017, 18, 1211–1217. [Google Scholar] [CrossRef]
- Munro, C.; Ranganathan, S.; Coulthard, K.; Quinlan, C. Use of neutrophil gelatinase-associated lipocalin (NGAL) in CF. J. Cyst. Fibros. 2015, 14, 154. [Google Scholar] [CrossRef][Green Version]
- Kellum, J.A.; Lameire, N.; Aspelin, P.; Barsoum, R.S.; Burdmann, E.A.; Goldstein, S.L.; Herzog, C.A.; Joannidis, M.; Kribben, A.; Levey, A.S.; et al. Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group KDIGO Clinical Practice Guideline for Acute Kidney Injury. Kidney Int. Suppl. 2012, 2, 1–138. [Google Scholar]
- Levey, A.S.; Stevens, L.A.; Schmid, C.H.; Zhang, Y.L.; Castro, A.F.; Feldman, H.I.; Kusek, J.W.; Eggers, P.; Van Lente, F.; Greene, T.; et al. CKD-EPI (Chronic Kidney Disease Epidemiology Collaboration). A new equation to estimate glomerular filtration rate. Ann. Intern. Med. 2009, 150, 604–612. [Google Scholar] [CrossRef]
- Lee, T.W.; Brownlee, K.G.; Conway, S.P.; Denton, M.; Littlewood, J.M. Evaluation of a new definition for chronic Pseudomonas aeruginosa infection in cystic fibrosis patients. J. Cyst. Fibros. 2003, 2, 29–34. [Google Scholar] [CrossRef]
- Souza-Menezes, J.; da Silva Feltran, G.; Morales, M.M. CFTR and TNR-CFTR expression and function in the kidney. Biophys. Rev. 2014, 6, 227–236. [Google Scholar] [CrossRef]
- Mody, H.; Ramakrishnan, V.; Chaar, M.; Lezeau, J.; Rump, A.; Taha, K.; Lesko, L.; Ait-Oudhia, S. A Review on Drug-Induced Nephrotoxicity: Pathophysiological Mechanisms, Drug Classes, Clinical Management, and Recent Advances in Mathematical Modeling and Simulation Approaches. Clin. Pharmacol. Drug Dev. 2020, 9, 896–909. [Google Scholar] [CrossRef]
- Kim, Y.W. Antimicrobial-induced Electrolyte and Acid-Base Disturbances. Electrolyte Blood Press. 2007, 5, 111–115. [Google Scholar] [CrossRef]
- Scoglio, M.; Bronz, G.; Rinoldi, P.O.; Faré, P.B.; Betti, C.; Bianchetti, M.G.; Simonetti, G.D.; Gennaro, V.; Renzi, S.; Lava, S.A.G.; et al. Electrolyte and Acid-Base Disorders Triggered by Aminoglycoside or Colistin Therapy: A Systematic Review. Antibiotics 2021, 10, 140. [Google Scholar] [CrossRef] [PubMed]
- Smyth, A.; Lewis, S.; Bertenshaw, C.; Choonara, I.; McGaw, J.; Watson, A. Case-control study of acute renal failure in patients with cystic fibrosis in the UK. Thorax 2008, 63, 532–535. [Google Scholar] [CrossRef] [PubMed]
- Berg, K.H.; Ryom, L.; Faurholt-Jepsen, D.; Pressler, T.; Katzenstein, T.L. Prevalence and characteristics of chronic kidney disease among Danish adults with cystic fibrosis. J. Cyst. Fibros. 2018, 17, 478–483. [Google Scholar] [CrossRef] [PubMed]
- Southern, K.W. Acute renal failure in people with cystic fibrosis. Thorax 2007, 62, 472–473. [Google Scholar] [CrossRef] [PubMed]
- Nowakowski, A.C.H. Cystic Fibrosis Kidney Disease: 10 Tips for Clinicians. Front. Med. 2018, 5, 242. [Google Scholar] [CrossRef] [PubMed]
- Yahiaoui, Y.; Jablonski, M.; Hubert, D.; Mosnier-Pudar, H.; Noël, L.H.; Stern, M.; Grenet, D.; Grünfeld, J.P.; Chauveau, D.; Fakhouri, F. Renal involvement in cystic fibrosis: Diseases spectrum and clinical relevance. Clin. J. Am. Soc. Nephrol. 2009, 4, 921–928. [Google Scholar] [CrossRef]
- Muirhead, C.; Lim, J.Y.; Lapidus, J.; MacDonald, K. Evaluation of the Risk for Acute Kidney Injury in Adult Cystic Fibrosis Patients Receiving Concomitant Vancomycin and Tobramycin. Cureus 2017, 9, e1912. [Google Scholar] [CrossRef]
- Askenazi, D.J. Risk factors for acute kidney injury during aminoglycoside therapy in patients with cystic fibrosis. Pediatr. Nephrol. 2015, 30, 1879–1888. [Google Scholar]
- Menon, S.; Kirkendall, E.S.; Nguyen, H.; Goldstein, S.L. Acute kidney injury associated with high nephrotoxic medication exposure leads to chronic kidney disease after 6 months. J. Pediatr. 2014, 165, 522–527.e2. [Google Scholar] [CrossRef]
- Quon, B.S.; Mayer-Hamblett, N.; Aitken, M.L.; Smyth, A.R.; Goss, C.H. Risk factors for chronic kidney disease in adults with cystic fibrosis. Am. J. Respir. Crit. Care Med. 2011, 184, 1147–1152. [Google Scholar] [CrossRef]
- Beringer, P.M.; Hidayat, L.; Heed, A.; Zheng, L.; Owens, H.; Benitez, D.; Rao, A.P. GFR estimates using cystatin C are superior to serum creatinine in adult patients with cystic fibrosis. J. Cyst. Fibros. 2009, 8, 19–25. [Google Scholar] [CrossRef] [PubMed]
- Hermida, J.; Tutor, J.C. Serum cystatin C for the prediction of glomerular filtration rate with regard to the dose adjustment of amikacin, gentamicin, tobramycin, and vancomycin. Ther. Drug Monit. 2006, 28, 326–331. [Google Scholar] [CrossRef] [PubMed]
- Zughaier, S.M.; Tangpricha, V.; Leong, T.; Stecenko, A.A.; McCarty, N.A. Peripheral monocytes derived from patients with cystic fibrosis and healthy donors secrete NGAL in response to Pseudomonas aeruginosa infection. J. Investig. Med. 2013, 61, 1018–1025. [Google Scholar] [CrossRef] [PubMed]
- Gala-Bładzińska, A.; Kuzniewski, M. Performance neutrophil gelatinase-associated lipocalin in clinical settings. Prz. Lek. 2013, 70, 400–403. [Google Scholar]
- Kashani, K.; Cheungpasitporn, W.; Ronco, C. Biomarkers of acute kidney injury: The pathway from discovery to clinical adoption. Clin. Chem. Lab. Med. 2017, 55, 1074–1089. [Google Scholar] [CrossRef]
- Mårtensson, J.; Bellomo, R. The rise and fall of NGAL in acute kidney injury. Blood Purif. 2014, 37, 304–310. [Google Scholar] [CrossRef]
- Hvidberg, V.; Jacobsen, C.; Strong, R.K.; Cowland, J.B.; Moestrup, S.K.; Borregaard, N. The endocytic receptor megalin binds the iron transporting neutrophil-gelatinase-associated lipocalin with high affinity and mediates its cellular uptake. FEBS Lett. 2005, 579, 773–777. [Google Scholar] [CrossRef]
- McWilliam, S.J.; Antoine, D.J.; Jorgensen, A.L.; Smyth, R.L.; Pirmohamed, M. Urinary Biomarkers of Aminoglycoside-Induced Nephrotoxicity in Cystic Fibrosis: Kidney Injury Molecule-1 and Neutrophil Gelatinase-Associated Lipocalin. Sci. Rep. 2017, 8, 5094. [Google Scholar] [CrossRef]

| CF | Healthy Controls | p | ||
|---|---|---|---|---|
| Age in years, median (Q1; Q3) | 18 (14; 22) | 17 (12.5; 20) | NS | |
| range | 7–44 | 8–43 | ||
| ≥18 years, n (%) | 29 (58%) | 24 (48%) | NS | |
| <18 years, n (%) | 21 (42%) | 26 (52%) | NS | |
| BMI, median (Q1; Q3) | 18.4 (17; 21) | 21.9 (20; 24) | <0.0001 | |
| range | 14–26 | 15–28 | ||
| Gender | ||||
| female, n (%) | 25 (50%) | 27 (54%) | NS | |
| male, n (%) | 25 (50%) | 23 (46%) | NS | |
| CF genotype | ||||
| homozygote ΔF508, n (%) | 33 (66%) | - | ||
| heterozygote ΔF508, n (%) | 11 (22%) | - | ||
| other, n (%) | 6 (12%) | - | ||
| Colonization | ||||
| Pseudomonas aeruginosa, n (%) | 20 (40%) | - | ||
| Staphylococcus aureus, n (%) | 25 (50%) | - | ||
| Burkholderia cepacia, n (%) | 2 (4%) | - | ||
| Stenotrophomonas maltophilia, n (%) | 3 (6%) | - | ||
| Candida albicans, n (%) | 18 (36%) | - | ||
| Average hospitalization time in days in the last year, median (Q1; Q3) | 52 (50, 54) | - | ||
| range | 42–62 | - | ||
| CF-related diabetes, n (%) | 9 (18%) | - | ||
| Acute exacerbation in last 6 months, n (%) | 30 (60%) | - | ||
| FEV1%, median (Q1; Q3) | 78 (67; 88) | 97.1 (90; 102) | <0.0001 | |
| range | 34–113 | 84–115 | ||
| WBC, * 103/μL, median (Q1; Q3) | 2.1 (0.5; 8.4) | 1.5 (0.6; 2.3) | <0.0001 | |
| range | 0.1–32.9 | 0.2–4.8 | ||
| CRP, mg/L, median (Q1; Q3) | 4.8 (3; 9.6) | 1.7 (1.5; 2.5) | 0.0234 | |
| range | 1.5–3.9 | |||
| IL-6, pg/mL, median (Q1; Q3) | 9 (7.7; 11.8) | 1.5 (0.6; 2.3) | <0.0001 | |
| range | 5–21.6 | 0.2–4.8 | ||
| Norm | CF (n = 50) | Healthy Controls (n = 50) | p | |||
|---|---|---|---|---|---|---|
| Median (Q1; Q3) | Range | Median (Q1; Q3) | Range | |||
| CysC [mg/L] | 0.64–1.23 | 0.91 (0.818; 1) | 0.7–1.16 | 0.78 (0.723; 0.868) | 0.64–1.02 | 0.00003 |
| sCr [mg/dL] < 18 years old | 0.4–0.72 | 0.68 (0.56; 0.77) | 0.43–0.99 | 0.65 (0.61; 0.7) | 0.58–0.72 | 0.576 |
| sCr [mg/dL] > 18 years old | 0.6–1.1 | 0.76 (0.66; 0.85) | 0.57–1 | 0.83 (0.74; 0.91) | 0.59–1.02 | 0.196 |
| sUrea [mg/dL] | 19–49 | 27 (23; 32) | 15–66 | 25 (22; 28) | 17–34 | 0.097 |
| eGFR [mL/min] | >90 | 106 (82.5; 117) | 56–152 | 118 (107.5; 130) | 89–130 | 0.002 |
| eGFRcysC [mL/min] | >90 | 81 (64; 107) | 41–125 | 99 (89; 108) | 68–148 | 0.007 |
| uNGAL [ng/mL] | 0–131.7 | 40.83 (20.9; 56.3) | 7.6–127 | 34.65 (20.1; 48.5) | 10.5–92.5 | 0.766 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rachel, M.; Galiniak, S.; Biesiadecki, M.; Gala-Błądzińska, A. Renal Function in Patients with Cystic Fibrosis: A Single-Center Study. Int. J. Environ. Res. Public Health 2022, 19, 5454. https://doi.org/10.3390/ijerph19095454
Rachel M, Galiniak S, Biesiadecki M, Gala-Błądzińska A. Renal Function in Patients with Cystic Fibrosis: A Single-Center Study. International Journal of Environmental Research and Public Health. 2022; 19(9):5454. https://doi.org/10.3390/ijerph19095454
Chicago/Turabian StyleRachel, Marta, Sabina Galiniak, Marek Biesiadecki, and Agnieszka Gala-Błądzińska. 2022. "Renal Function in Patients with Cystic Fibrosis: A Single-Center Study" International Journal of Environmental Research and Public Health 19, no. 9: 5454. https://doi.org/10.3390/ijerph19095454
APA StyleRachel, M., Galiniak, S., Biesiadecki, M., & Gala-Błądzińska, A. (2022). Renal Function in Patients with Cystic Fibrosis: A Single-Center Study. International Journal of Environmental Research and Public Health, 19(9), 5454. https://doi.org/10.3390/ijerph19095454









