Context-Aware Medical Systems within Healthcare Environments: A Systematic Scoping Review to Identify Subdomains and Significant Medical Contexts
Abstract
:1. Introduction
“any information that can be used to characterise the situation of an entity. An entity is a person, place, or object that is considered relevant to the interaction between a user and an application, including the user and applications themselves.”[1]
“A system is context-aware if it uses context to provide relevant information and/or services to the user, where relevance depends on the user’s task.”[1]
2. Methods
2.1. Objectives
2.2. Design
2.3. Study Eligibility
2.4. Search Design and Data Extraction
3. Results
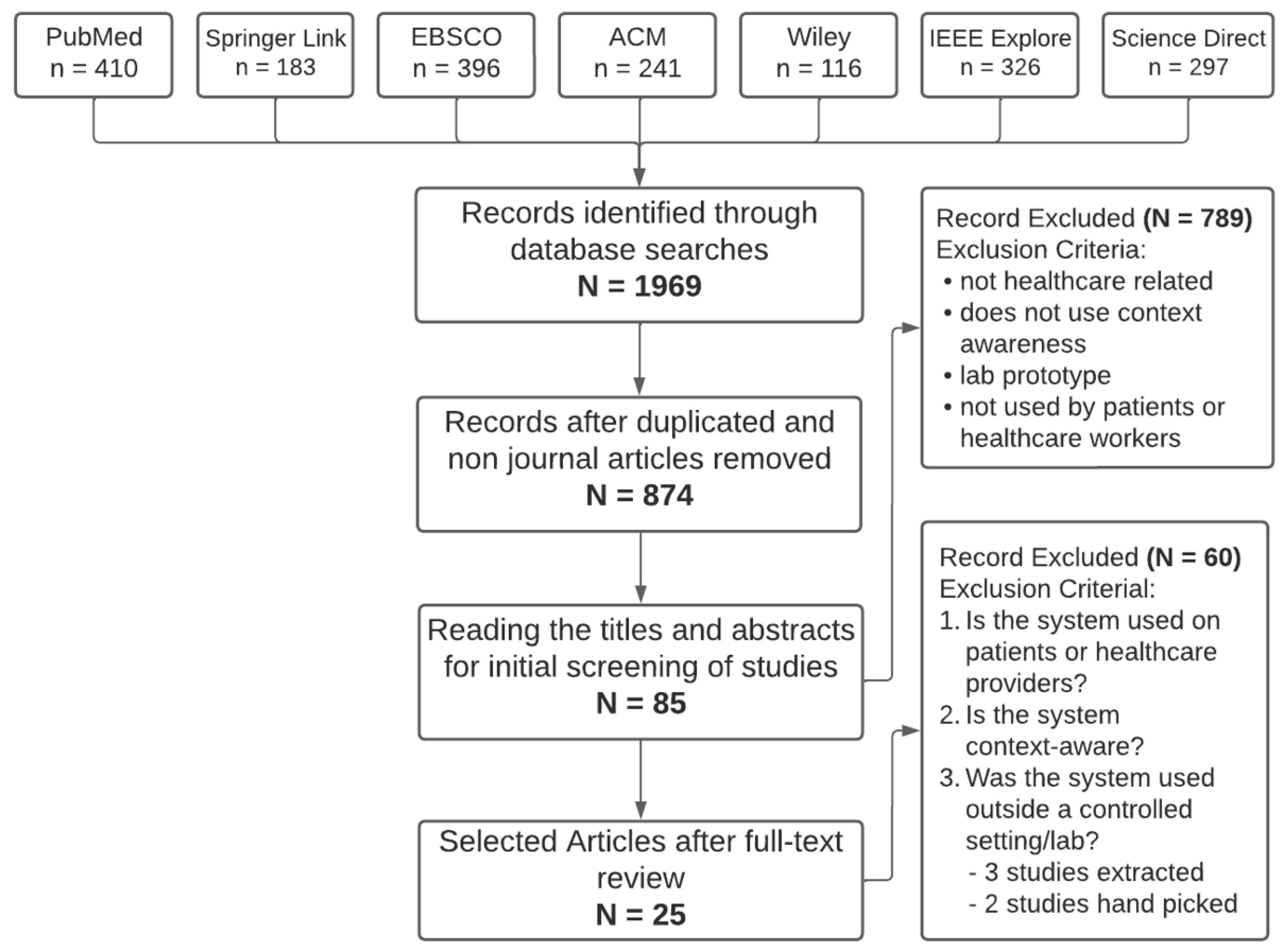
3.1. Study Selection
3.2. Study Characteristics
3.3. Technology and Contexts
4. Discussion
4.1. Smart Inpatient/Outpatient Software and Medical Device
4.2. Assisted-Living
4.3. Smart Diagnostic and Disease Systems
4.4. Therapy and Rehabilitation
4.5. Continuous Heath Monitoring and Persuasive and Emotional Well-Being
4.6. Important Contexts and Technology within the Domains
5. Limitations and Future Research
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Abowd, G.D.; Dey, A.K.; Brown, P.J.; Davies, N.; Smith, M.; Steggles, P. Towards a Better Understanding of Context and Context-Awareness. In Proceedings of the International Symposium on Handheld and Ubiquitous Computing, Karlsruhe, Germany, 27–29 September 1999; Volume 1707, pp. 304–307. [Google Scholar]
- Schilit, B.; Theimer, M. Disseminating active map information to mobile hosts. IEEE Netw. 1994, 8, 22–32. [Google Scholar] [CrossRef]
- Abowd, G.D.; Mynatt, E.D. Charting past, present, and future research in ubiquitous computing. ACM Trans. Comput. Interact. 2000, 7, 29–58. [Google Scholar] [CrossRef] [Green Version]
- Majumder, S.; Mondal, T.; Deen, M.J. Wearable Sensors for Remote Health Monitoring. Sensors 2017, 17, 130. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Majumder, B.S.; Chen, L.; Marinov, O.; Chen, C.H.; Mondal, T.; Deen, M.J. Non-Contact Wearable Wireless ECG Systems for Long Term Monitoring. IEEE Rev. Biomed. Eng. 2018, 11, 306–321. [Google Scholar] [CrossRef]
- Majumder, S.; Aghayi, E.; Noferesti, M.; Memarzadeh-Tehran, H.; Mondal, T.; Pang, Z.; Deen, M.J. Smart Homes for Elderly Healthcare—Recent Advances and Research Challenges. Sensors 2017, 17, 2496. [Google Scholar] [CrossRef] [Green Version]
- Deen, D.M.J. Information and Communications Technologies for Elderly Ubiquitous Healthcare in a Smart Home. Pers. Ubiquitous Comput. 2015, 19, 573–599. [Google Scholar] [CrossRef]
- Bricon-Souf, N.; Newman, C.R. Context awareness in health care: A review. Int. J. Med. Inform. 2007, 76, 2–12. [Google Scholar] [CrossRef]
- Quinde, M.; Khan, N.; Augusto, J.C.; van Wyk, A.; Stewart, J. Context-aware solutions for asthma condition management: A survey. Univers. Access Inf. Soc. 2020, 19, 571–593. [Google Scholar] [CrossRef]
- Tobón, D.P.; Falk, T.H.; Maier, M. Context awareness in WBANs: A survey on medical and non-medical applications. IEEE Wirel. Commun. 2013, 20, 30–37. [Google Scholar] [CrossRef]
- Gubert, L.C.; da Costa, C.A.; Righi, R.D.R. Context awareness in healthcare: A systematic literature review. Univers. Access Inf. Soc. 2020, 19, 245–259. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.J.; Horsley, T.; Weeks, L.; et al. PRISMA extension for Scoping Reviews (PRISMA-ScR): Checklist and explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef] [Green Version]
- Peters, M.D.J.; Godfrey, C.; McInerney, P.; Munn, Z.; Tricco, A.C.; Khalil, H. Chapter 11: Scoping reviews (2020 version). In JBI Manual for Evidence Synthesis; Aromataris, E., Munn, Z., Eds.; JBI: St. Miami, FL, USA, 2020; pp. 406–451. [Google Scholar]
- Wagner, S.; Buus, N.H.; Jespersen, B.; Ahrendt, P.; Bertelsen, O.W.; Toftegaard, T.S. Measurement Adherence in the Blood Pressure Self-Measurement Room. Telemed. e-Health 2013, 19, 826–833. [Google Scholar] [CrossRef] [Green Version]
- Lindahl, C.; Wagner, S.; Uldbjerg, N.; Schlütter, J.M.; Bertelsen, O.; Sandager, P. Effects of context-aware patient guidance on blood pressure self-measurement adherence levels. Health Inform. J. 2019, 25, 417–428. [Google Scholar] [CrossRef]
- Kim, E.; Yoo, S.; Hee, H.; Park, H.; Kim, G.; Ha, S. Patient satisfaction in a context-aware hospital guidance system. Stud. Health Technol. Inform. 2012, 180, 1177–1179. [Google Scholar]
- Grübler, M.D.S.; da Costa, C.A.; Righi, R.D.R.; Rigo, S.J.; Chiwiacowsky, L.D. A Hospital Bed Allocation Hybrid Model Based on Situation Awareness. CIN Comput. Inform. Nurs. 2018, 36, 249–255. [Google Scholar] [CrossRef]
- Coronato, A.; De Pietro, G.; Paragliola, G. A situation-aware system for the detection of motion disorders of patients with Autism Spectrum Disorders. Expert Syst. Appl. 2014, 41, 7868–7877. [Google Scholar] [CrossRef]
- Kaffash-Charandabi, N.; Alesheikh, A.A.; Sharif, M. A ubiquitous asthma monitoring framework based on ambient air pollutants and individuals’ contexts. Environ. Sci. Pollut. Res. 2019, 26, 7525–7539. [Google Scholar] [CrossRef]
- Kuo, Y.-M.; Lee, J.-S.; Chung, P.-C. A Visual Context-Awareness-Based Sleeping-Respiration Measurement System. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 255–265. [Google Scholar]
- Bächlin, M.; Plotnik, M.; Roggen, D.; Giladi, N.; Hausdorff, J.M.; Tröster, G. A Wearable System to Assist Walking of Parkinson’s Disease Patients. Methods Inf. Med. 2010, 49, 88–95. [Google Scholar]
- Klakegg, S.; Asare, K.O.; Van Berkel, N.; Visuri, A.; Ferreira, E.; Hosio, S.; Goncalves, J.; Huttunen, H.-L.; Ferreira, D. CARE: Context-awareness for elderly care. Health Technol. 2021, 11, 211–226. [Google Scholar] [CrossRef]
- de la Iglesia, D.H.; Mendes, A.S.; González, G.V.; Jiménez-Bravo, D.M.; Santana, J.F.d.P. Connected Elbow Exoskeleton System for Rehabilitation Training Based on Virtual Reality and Context-Aware. Sensors 2020, 20, 858. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Muylle, K.M.; Gentens, K.; Dupont, A.G.; Cornu, P. Evaluation of an optimized context-aware clinical decision support system for drug-drug interaction screening. Int. J. Med. Inform. 2021, 148, 104393. [Google Scholar] [CrossRef] [PubMed]
- Burns, M.N.; Begale, M.; Duffecy, J.; Gergle, D.; Karr, C.J.; Giangrande, E.; Mohr, D.C. Harnessing Context Sensing to Develop a Mobile Intervention for Depression. J. Med. Internet Res. 2011, 13, e55. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Borbolla, D.; Del Fiol, G.; Taliercio, V.; Otero, C.; Campos, F.; Martinez, M.; Luna, D.; Quiros, F. Integrating personalized health information from MedlinePlus in a patient portal. Stud. Health Technol. Inform. 2014, 205, 348–352. [Google Scholar] [PubMed]
- Tang, L.; Zhou, X.; Yu, Z.; Liang, Y.; Zhang, D.; Ni, H. MHS: A Multimedia System for Improving Medication Adherence in Elderly Care. IEEE Syst. J. 2011, 5, 506–517. [Google Scholar] [CrossRef]
- Hayes, T.L.; Cobbinah, K.; Dishongh, T.; Kaye, J.A.; Kimel, J.; Labhard, M.; Leen, T.; Lundell, J.; Ozertem, U.; Pavel, M.; et al. A study of medication-taking and unobtrusive, intelligent reminding. Telemed. J. e-Health 2009, 15, 770–776. [Google Scholar] [CrossRef] [Green Version]
- Wahle, F.; Kowatsch, T.; Fleisch, E.; Rufer, M.; Weidt, S. Mobile Sensing and Support for People with Depression: A Pilot Trial in the Wild. JMIR Mhealth Uhealth 2016, 4, e111. [Google Scholar] [CrossRef] [Green Version]
- Dai, X.; Gao, Y.; Shen, D. Online updating of context-aware landmark detectors for prostate localization in daily treatment CT images. Med. Phys. 2015, 42, 2594–2606. [Google Scholar] [CrossRef] [Green Version]
- Cornu, P.; Steurbaut, S.; Gentens, K.; Van de Velde, R.; Dupont, A.G. Pilot evaluation of an optimized context-specific drug–drug interaction alerting system: A controlled pre-post study. Int. J. Med. Inform. 2015, 84, 617–629. [Google Scholar] [CrossRef]
- Chan, S.W.T.; Sapkota, S.; Mathews, R.; Zhang, H.; Nanayakkara, S. Prompto: Investigating Receptivity to Prompts Based on Cognitive Load from Memory Training Conversational Agent. Proc. ACM Interact. Mob. Wearable Ubiquitous Technol. 2020, 4, 1–23. [Google Scholar] [CrossRef]
- Niazkhani, Z.; Fereidoni, M.; Khazaee, P.R.; Shiva, A.; Makhdoomi, K.; Georgiou, A.; Pirnejad, H. Translation of evidence into kidney transplant clinical practice: Managing drug-lab interactions by a context-aware clinical decision support system. BMC Med. Inform. Decis. Mak. 2020, 20, 196. [Google Scholar] [CrossRef]
- Ong, S.W.; Jassal, S.V.; Miller, J.A.; Porter, E.C.; Cafazzo, J.A.; Seto, E.; Thorpe, K.E.; Logan, A.G. Integrating a Smartphone–Based Self–Management System into Usual Care of Advanced CKD. Clin. J. Am. Soc. Nephrol. 2016, 11, 1054–1062. [Google Scholar] [CrossRef] [Green Version]
- Abdullah, S.; Matthews, M.; Frank, E.; Doherty, G.; Gay, G.; Choudhury, T. Automatic detection of social rhythms in bipolar disorder. J. Am. Med. Inform. Assoc. 2016, 23, 538–543. [Google Scholar] [CrossRef]
- Solvoll, T.; Arntsen, H.; Hartvigsen, G. Alarm Fatigue vs User Expectations Regarding Context-Aware Alarm Handling in Hospital Environments Using CallMeSmart. Stud. Health Technol. Inform. 2017, 241, 159–164. [Google Scholar]
- Stratou, G.; Morency, L. MultiSense—Context-Aware Nonverbal Behavior Analysis Framework: A Psychological Distress Use Case. IEEE Trans. Affect. Comput. 2017, 8, 190–203. [Google Scholar] [CrossRef]
- Devender, K.; Maharjan, R.; Maxhuni, A.; Dominguez, H.; Frølich, A.; Bardram, J.E. mCardia: A context-aware ECG col-lection system for ambulatory arrhythmia screening. ACM Trans. Comput. Healthc. (HEALTH) 2022, 3, 1–28. [Google Scholar]
- Luigi, B.; Sigcha, L.; Olmo, G. Context Recognition Algorithms for Energy-Efficient Freezing-of-Gait Detection in Parkin-son’s Disease. Sensors 2023, 23, 4426. [Google Scholar]
- Acampora, G.; Cook, D.J.; Rashidi, P.; Vasilakos, A.V. A Survey on Ambient Intelligence in Healthcare. Proc. IEEE 2013, 101, 2470–2494. [Google Scholar] [CrossRef]
- Franke, S.; Rockstroh, M.; Hofer, M.; Neumuth, T. The intelligent OR: Design and validation of a context-aware surgical working environment. Int. J. Comput. Assist. Radiol. Surg. 2018, 13, 1301–1308. [Google Scholar] [CrossRef]
- Lagrange, F.; Bennaga, C.; Taloub, F.; Keddi, M.; Dumoulin, B. A context-aware decision-support system in clinical pharmacy: Drug monitoring in the elderly. Pharm. Hosp. Clin. 2017, 52, 100–110. [Google Scholar] [CrossRef]
- Yin, K.; Laranjo, L.; Tong, H.L.; Lau, A.Y.; Kocaballi, A.B.; Martin, P.; Vagholkar, S.; Coiera, E. Context-Aware Systems for Chronic Disease Patients: Scoping Review. J. Med. Internet Res. 2019, 21, e10896. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wu, F.; Zhao, H.; Zhao, Y.; Zhong, H. Development of a Wearable-Sensor-Based Fall Detection System. Int. J. Telemed. Appl. 2015, 2015, 576364. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Abbate, S.; Avvenuti, M.; Bonatesta, F.; Cola, G.; Corsini, P.; Vecchio, A. A smartphone-based fall detection system. Pervasive Mob. Comput. 2012, 8, 883–899. [Google Scholar] [CrossRef]
- Alti, A.; Laborie, S.; Roose, P. Cloud semantic-based dynamic multimodal platform for building mHealth context-aware services. In Proceedings of the 2015 IEEE 11th international conference on wireless and mobile computing, networking and communications (WiMob), Abu Dhabi, United Arab Emirates, 19–21 October 2015; pp. 357–364. [Google Scholar]
- Perera, C.; Zaslavsky, A.; Christen, P.; Georgakopoulos, D. Context Aware Computing for The Internet of Things: A Survey. IEEE Commun. Surv. Tutor. 2013, 16, 414–454. [Google Scholar] [CrossRef] [Green Version]
- Awad, A.A.; Mohamed, A.; Chiasserini, C.F.; Tlili, M.; Erbad, A. Edge computing for smart health: Context-aware ap-proaches, opportunities, and challenges. IEEE Netw. 2019, 33, 196–203. [Google Scholar]
- Edgar, B.; Moncusi, M.A.; López-Aguilar, P.; Martínez-Ballesté, A.; Solanas, A. Sensors for context-aware smart healthcare: A security perspective. Sensors 2021, 21, 6886. [Google Scholar]
- Aromataris, E.; Munn, Z. JBI Manual for Evidence Synthesis. 2020. Available online: https://synthesismanual.jbi.global (accessed on 23 June 2023).
- Hoffmann, T.C.; Glasziou, P.P.; Milne, R.; Perera, R.; Moher, D.; Altman, D.G.; Barbour, V.; Macdonald, H.; Johnston, M.; Lamb, S.E.; et al. Better reporting of interventions template for intervention description and replication (TIDieR) checklist and guide. BMJ 2014, 348, 1687. [Google Scholar] [CrossRef] [Green Version]
| Article | Year | General Description | Sample Size | Mean Age | Test Length | Measured Signal | Assessment Method | Contexts Used | Context Awareness (How Did the App Change) |
|---|---|---|---|---|---|---|---|---|---|
| Patient Satisfaction in a Context-Aware Hospital Guidance System [16] | 2012 | 7.1-inch Galaxy Tablet with the hospital guidance system app [16] | 13 | 44 | Hospital visit | Patients’ location within the hospital | Patient satisfaction survey | Patient location within hospital, appointments, and procedures the patient needs to complete | The application changed based on the patients’ specific next task in the hospital; guidance changed based on their current location |
| A Hospital Bed Allocation Hybrid Model Based on Situation Awareness [17] | 2018 | Web app for hospital bed allocation [17] | 50 | N/A | 5 days | Rate of successful placement | Verify whether the bed selected was correct | Room type based on patients’ health plan, physician specialty, sex, type of treatment, risk (e.g., infectious), degree of dependency, age, time of hospitalization | Bed displayed to bed manager varied based on patient-specific context |
| A situation-aware system for the detection of motion disorders of patients with autism spectrum disorders [18] | 2014 | Wristwatch with an accelerometer worn by patients [18] | 5 | N/A | N/A | Detection of movement disorders | Compared with ground truth | Hand gesture type, time of day, gesture duration | The clinical reports varied based on contexts such as the duration of each gesture, time of day of the gesture, and type of movement disorder |
| A ubiquitous asthma monitoring framework based on ambient air pollutants and individuals’ contexts [19] | 2019 | Smartphone with a context-aware asthma management app [19] | 3 | 36.33 (32F, 35M, 42M) | N/A | Predicted peak expiratory flow (PEF) | Compared predicted PEF to actual PEF from devices that patients used | Environment/pollutant variables, user location, user’s age, gender, height | App warns patients of potential asthma attacks via predicted PEF which changed based on various contexts (e.g., environment/pollutant variables, user location, user’s age, gender, height, and PEF) |
| A Visual Context-Awareness-Based Sleeping-Respiration Measurement System [20] | 2010 | Near-infrared camera that monitored users as they slept to determine respiratory rate [20] | 18 | N/A | N/A | Respiratory rate | Compared RR results to those of the CO2SMO PLUS respiratory monitoring machine | Body motion of users | The system determining respiratory rate changes its action based on the body motion context (proceeds to RR calculation if still) |
| A wearable system to assist walking of Parkinson’s disease patients [21] | 2010 | Accelerometers used to detect freezing of gait (FOG) context in Parkinson’s in real time [21] | 10 | 66.4 | 237 FOG events | Freezing of gait | Physiotherapists observed video to determine FOG events and detection by the system was compared to ground truth | Gait state (i.e moving vs. frozen) | Auditory stimuli delivered if FOG context detected |
| CARE: Context awareness for elderly care [22] | 2020 | Android mobile app that shows activities of older adults determined by sensors in retirement homes [22] | 15 patients, 17 nurses | N/A | 2 months | Long-term trends in resident activity level, time in bed, proximity to nurses, proximity to other residents | Questionnaire was used to determine if nurses found the application useful | User location, nurse location, time in bed, level of activity | Different data displayed to nurses via android app depending on user contexts (e.g., how often resident is near nurses or other residents, their level of activity, etc.) |
| Connected Elbow Exoskeleton System for Rehabilitation Training Based on Virtual Reality and Context-Aware [23] | 2020 | VR-based physiotherapy application paired with an elbow exoskeleton device [23] | 5 | N/A | 1 month | Performance of patient over time in VR rehab exercises where patient moves ring along cable, but the ring should not touch the cable | Position, angle, and time deviation during the exercise relative to a perfect performance (e.g., wire kept in the center of the ring for position performance) | Performance on exercise | Patients’ performance on current exercise is used to inform how difficult the app makes the next exercise |
| Effects of context-aware patient guidance on blood pressure self measurement adherence levels [15] | 2019 | Smart chair and tablet paired with a blood pressure (BP) monitor to ensure proper contexts for BP measurement [15] | 100 | 29.9 | One time | Adherence to the requirements for proper blood pressure measurements when recommended by the system versus not recommended | Percent adherence to the different requirements | User rest time, legs crossed, back-supported, ambient noise/talking, participant compliance | App recommended rest time and not talking if motion/talking contexts were detected; other contexts not recommended |
| Evaluation of an optimized context-aware clinical decision support system for drug-drug interaction screening [24] | 2021 | Drug–drug interaction intervention application in hospitals [24] | 2630 alarms | N/A | 8 months | Drug–drug interactions and the acceptance rate of alerts | Tracked numbers of alerts that result in a change to a prescription | Patients’ current medications, age, sex, last potassium levels, and renal function | Application utilized patient-specific data to determine if it flags the current prescription as dangerous |
| Harnessing Context Sensing to Develop a Mobile Intervention for Depression [25] | 2011 | Mobile application to improve and predict major depressive order [25] | 8 | 37.4 | 8 weeks | Mood, location, activity, who the users were with or near | Compared predictions to those entered manually by participants | Location, time of day, who users were with, conversing or not, mood, contexts from phone apps such as recent calls, active applications | Moods predicted and thus tracked/displayed to users changed based on machine learning models that predicted mood from context data derived from phone sensors |
| Integrating Personalized Health Information from MedlinePlus in a Patient Portal [26] | 2014 | Patient portal in hospital that provides medical info specific to the patient’s context [26] | 80,000 | N/A | 1 year | Use of the lab test info and MedlinePlus explanatory info buttons | Number of clicks and percent of sessions the buttons were used in | Patients’ lab test results and condition/disease | The information offered to patients viz the patient portal varied based on what disease they had, or lab tests they received |
| MHS: A Multimedia System for Improving Medication Adherence in Elderly Care [27] | 2011 | Pill station equipped with a webcam that registers new medications and devices that prompt users to take meds [27] | 5 | Over 60 | 3 weeks | Adherence to taking medication | Unclear how ground truth medication taking is established, but likely assumed they take the medication when a pill box is opened | Users’ current activities such as watching TV, talking on the phone, eating, sitting, moving; exact list of used contexts not clear | The application prompts users to take medication based on their current contexts; i.e., if a pill is required with a meal, then they are prompted based on the eating context |
| A Study of Medication-Taking and Unobtrusive, Intelligent Reminding [28] | 2009 | Medication reminders of auditory/visual cues at user’s location in their home [28] | 10 | 82.7 | 10.7 weeks | Adherence rate for taking medication | Pill recorded as taken when the smart pill box container is opened | Location in home, when they are leaving home, a phone call in progress, in bed, using laptop, preferred time for medication | Audio and visual prompts around the home were triggered based on contexts, such as the user’s location, if they are not on the phone, the normal time they take the pill, if they have not taken the pill, if they are about to leave home |
| Mobile Sensing and Support for People With Depression: A Pilot Trial in the Wild [29] | 2016 | Mobile app for depression intervention and depression scores [29] | 126 | 20–57 | Over 9 months | PHQ-9 depression score | Compared PHQ-9 scores obtained from patients through questionnaire over time | Time of day, location, smartphone usage, activity level, walking time, time at home, geographic movement, number of unique Wi-Fi fingerprints, number of calls, calendar events | Interventions recommended varied based on users’ context (e.g., low activity level, walk recommended) and users’ feedback on interventions |
| Online updating of context-aware landmark detectors for prostate localization in daily treatment CT images [30] | 2015 | Prior treatment images used to improve landmark detection and prostate segmentation [30] | 24 | N/A | Length of treatment | Accuracy in segmenting prostate volume for algorithm relative to segmentation by physicians | Dice ratio and average surface distance | Patients’ inter-landmark distance, intra-landmark distance, and prostate segmentation from their prior images | The algorithm that identified landmarks and performs prostate segmentation varied based on patients’ prior treatment images and any adjustments from the physicians on the landmark/segmentation |
| Pilot evaluation of an optimized context-specific drug–drug interaction alerting system: A controlled pre-post study [31] | 2015 | Rule-based software applications to prevent dangerous prescriptions [31] | 1116 | N/A | 14 months | Acceptance rate of alerts when a new system that included context data was implemented | Tracked number of alerts that results in a change to a prescription | Patients’ current medications, age, sex, last potassium levels, and renal function | Application utilized patient-specific data to determine if it flags the current prescription as dangerous |
| Prompto: Investigating Receptivity to Prompts Based on Cognitive Load from Memory Training Conversational Agent [32] | 2020 | E4 wristband determines users’ availability for memory training [32] | 7 | 67.4 | 1 week | Responses to prompts and appropriateness of prompt timing according to user feedback | Percent of prompts that were accepted for memory training to commence | Cognitive load of users determined via heart rate variability and electrodermal activity | Application prompted users for memory training when cognitive load measured by E4 wristband was low |
| Translation of evidence into kidney transplant clinical practice: managing drug-lab interactions by a context-aware clinical decision support system [33] | 2020 | Smartphone application that prompts CKD patients to take BP measurements and symptoms [33] | 100 | 47.44 | N/A | Clinician satisfaction with the system | The “Questionnaire for user interface satisfaction” | Renal function via creatine clearance, lean body weight, pregnancy status | The system generated drug–lab interaction alerts based on the patient’s specific lab values (creatine clearance), lean body mass, and pregnancy status |
| Integrating a Smartphone–Based Self–Management System into Usual Care of Advanced CKD [34] | 2016 | Mobile app focused on predicting stability of bipolar disorder patients [34] | 47 | 59.4 | 6 months | User satisfaction with the app, change in blood pressure, change in CKD-relevant lab values | Exit interviews to assess satisfaction, BP measured by home monitoring device, and results compared between baseline and end of study | Patients’ adherence to BP measurements, their symptoms, and their medications | Frequency of messaging patients for BP changes based on their compliance, alerts sent to healthcare providers if symptoms warrant it, and medication discrepancies checked by the system throughout |
| Automatic detection of social rhythms in bipolar disorder [35] | 2016 | Social and activity contexts inferred from smartphone sensor data are used to predict social rhythm metrics [35] | 7 | 4 users 25–34; 3 were 34–64 | 4 weeks | Social rhythm metric | Compared SRM from models to that determined by manual inputs from patients | Phone usage patterns, location, distance traveled, number of conversations per day, duration of conversations, time speaking to others, speaking rate, speech pitch, time active vs. sedentary, SMS/call activity | Inferred behavioural rhythmicity and SRM changes based on contexts measured |
| Alarm Fatigue vs. User Expectations Regarding Context-Aware Alarm Handling in Hospital Environments Using CallMeSmart [36] | 2017 | Handheld communication system considers healthcare providers’ current context/activity to understand whether to page the user [36] | N/A | N/A | 2014–2017 | Satisfaction of healthcare workers with the new system relative to the old system | Interviews with users | Users’ calendar events (e.g., no calling while in patient consult), location (e.g., operating room) | Messages are relayed to healthcare workers based on urgency and their current availability as determined by their context (e.g., unavailable during patient consult) |
| MultiSense—Context-Aware Nonverbal Behavior Analysis Framework: A Psychological Distress Use Case [37] | 2017 | Topic of the discussion and what a normal, positive, or negative response looks like is used as context to determine distress levels [37] | 100 | N/A | One interview session | Distress levels of the person being interviewed | Root mean square error in systems predicted distress levels relative to ground truth levels | Users’ eye contact, smile level, and other behaviour indicators along with what the users affect should be based on the topic of conversation (e.g., smile while describing a trauma atypical) | Applications use patients’ non-verbal behavioural contexts to predict their distress levels and generate a patient-specific report |
| mCardia: A Context-Aware ECG Collection System for Ambulatory Arrhythmia Screening [38] | 2022 | Mobile electrocardiogram system uses contextual data in free-living conditions to provide a better understanding of what happens before, during, and after an arrhythmia [38] | 24 | 58.79 | 2 weeks | Electrical activity of the heart by the ECG | Participants were explained what was considered an event and taught how to report these events through the app | Gender, age, height, weight, sensor location, body position, step count, metabolic level, activity level | Would not consider high heart rates dangerous if the context warranted a higher heart rate (e.g., running) |
| Design and usability evaluation of COOK, an assistive technology for meal preparation for persons with severe TBI [39] | 2021 | A stove and kitchen are equipped with various sensors to assist those with past traumatic brain injuries in cooking [39] | 3 | Between 39–57 | 6 months | Heat surrounding the stove and whether human activity is present | User satisfaction according to questionnaires and evidence of increased stove use when cooking meals | Stove on or off, apartment vacant, apartment occupied, cooking, absent from the kitchen | The system warns the user if a dangerous situation/context is detected, such as the stove is left on after cooking; it may also turn the stove off itself |
| Application Category | Description | Subcategories | Reference Number | Contexts Found | Important Contexts | Technology Descriptions |
|---|---|---|---|---|---|---|
| Smart Inpatient and Outpatient Software and Medical Devices | Software systems to improve communication between healthcare staff and patients within the hospital | (A) Hospital/Inpatient systems (B) Outpatient systems | (A) [16,17,24,26,31,33,36] (B) [15,22] | healthcare provider location *, Patient location *, appointment time *, procedure type *, age *, sex *, physician specialty, medication list, lab test results, renal function *, weight, user taking or not *, activity level, time in bed * | location, calendar, medical history, medication list, demographic info, | Software applications using expert systems or machine learning and known contexts to make decisions; smart equipment using context to improve medical devices |
| Smart Diagnostic and Disease Management Systems | Diagnose patients’ using algorithms and identify ideal treatment plans | (A) Diagnostic systems (B) Disease management | (A) [18] (B) [19,21,25,30,35] | Movement type/status *, time of day *, age *, sex *, height, medical history, location *, who user is with *, phone use *, conversing or not *, medical images, disease-specific contexts (e.g., pollutant levels asthma) | Lab results, medical history, demographic data, time of day | Wearable sensors, machine learning, and user input used to make diagnoses and manage the disease |
| Continuous Health Monitoring | Wearable and ambient sensors for continuous healthcare monitoring | (A) Longitudinal physiological data monitoring (B) Emergency detection | (A) [20,38] (B) | Motion of the user’s body | Location, time of day, vitals, medical history, lab results | wearable sensors/medical devices to understand patients’ health and contexts like past medical history used to determine what normal is physiologically |
| Assisted Living | Developing smart environments to assist patients in their daily living activities | (A) Disease tracking (B) Physical Support (C) Social Support | (A) [27,28,34] (B) (C) [39] | User current activity (e.g., eating, tv), location *, conversing or not *. time in bed *, medication list *, symptoms, adherence to taking measurements (BP) | IADLs, location, time of day, symptoms, medication list | Mobile, web apps, and IoT devices used around the house to understand daily activities to help users perform tasks (e.g., taking medication) and manage disease |
| Therapy and Rehabilitation | Providing psychology-based therapy to improve or heal a disorder | (A) Smart rehabilitation (B) Psychology-based therapy | (A) [23,37] (B) [32] | Current performance in rehab tasks, cognitive load | Body position, mood | Wearable devices or software used to guide therapy or provide outputs that can be used in therapy |
| Persuasive and Emotional Well-Being | Systems aimed at improving physical and mental well-being | (A) Emotional analysis/state systems | (A) (B) [29] | Location, time of day, who users are with (alone, friends, family), conversing or not, mood, contexts from phone apps such as recent calls, active applications | Mood, activities, users’ specific goals | Mobile and web app software leverages smartphone sensors and IoT devices to understand the users’ state and lead them to better lifestyle choices |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zon, M.; Ganesh, G.; Deen, M.J.; Fang, Q. Context-Aware Medical Systems within Healthcare Environments: A Systematic Scoping Review to Identify Subdomains and Significant Medical Contexts. Int. J. Environ. Res. Public Health 2023, 20, 6399. https://doi.org/10.3390/ijerph20146399
Zon M, Ganesh G, Deen MJ, Fang Q. Context-Aware Medical Systems within Healthcare Environments: A Systematic Scoping Review to Identify Subdomains and Significant Medical Contexts. International Journal of Environmental Research and Public Health. 2023; 20(14):6399. https://doi.org/10.3390/ijerph20146399
Chicago/Turabian StyleZon, Michael, Guha Ganesh, M. Jamal Deen, and Qiyin Fang. 2023. "Context-Aware Medical Systems within Healthcare Environments: A Systematic Scoping Review to Identify Subdomains and Significant Medical Contexts" International Journal of Environmental Research and Public Health 20, no. 14: 6399. https://doi.org/10.3390/ijerph20146399







