Efficacy and Cost over 12 Hospitalization Weeks of Postacute Care for Stroke
Abstract
:1. Introduction
2. Materials and Methods
2.1. PAC-CVD Program
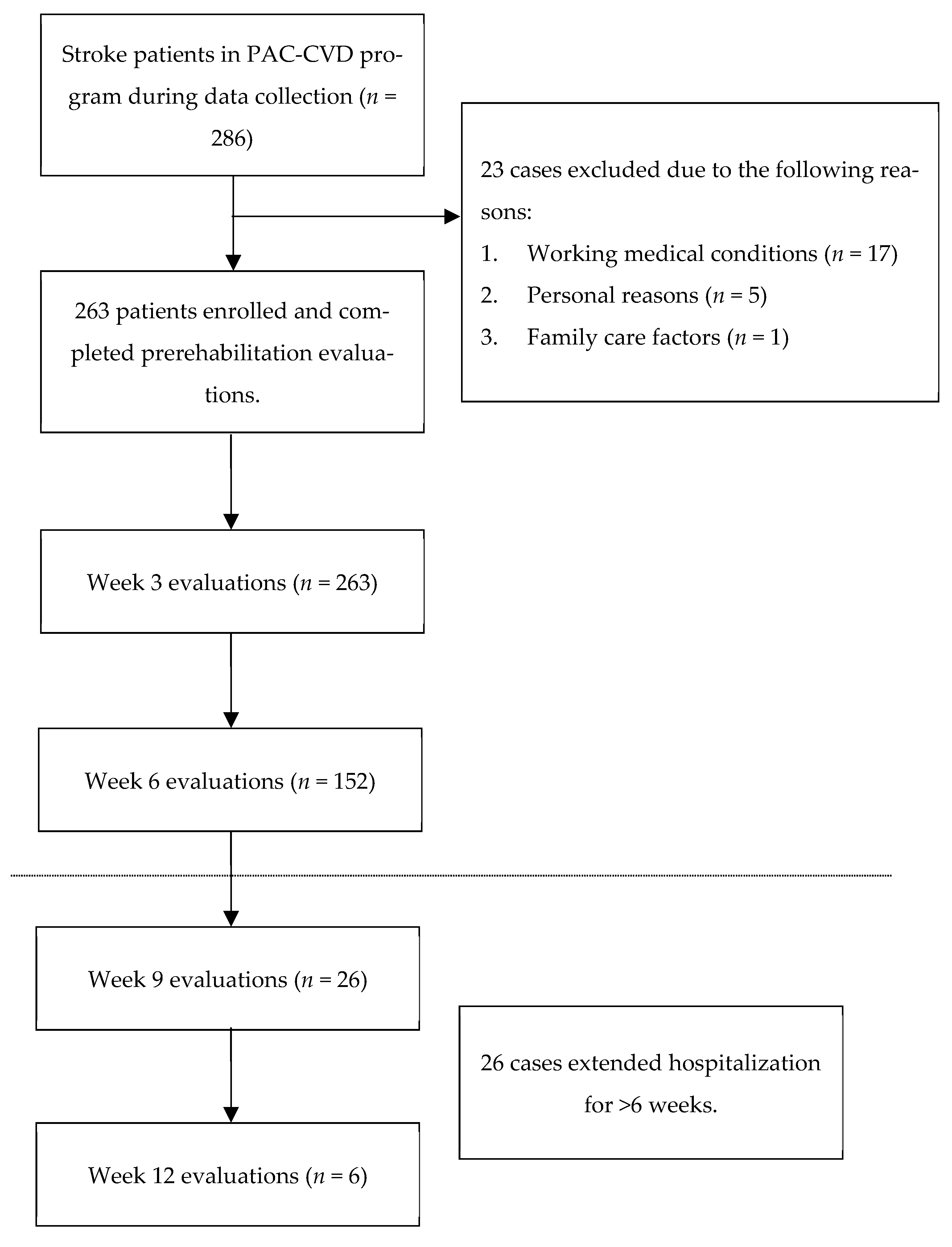
2.2. Study Design and Patients
2.3. Functional Performance Measures
2.4. Statistical Analysis
3. Results
3.1. Patient Characteristics
3.2. Functional Recovery and NHI Cost
3.2.1. Patients with PAC-CVD LOS of at Least 3 Weeks
3.2.2. Patients with a PAC-CVD LOS of at Least 6 Weeks
3.2.3. Patients with a PAC-CVD LOS of at Least 9 Weeks
3.2.4. Patients with a PAC-CVD LOS of 10–12 Weeks
3.2.5. Impact of Functional Performance on NHI Cost
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Feigin, V.L.; Forouzanfar, M.H.; Krishnamurthi, R.; Mensah, G.A.; Connor, M.; Bennett, D.A.; Moran, A.E.; Sacco, R.L.; Anderson, L.; Truelsen, T.; et al. Global and Regional Burden of Stroke During 1990-2010: Findings from the Global Burden of Disease Study 2010. Lancet 2014, 383, 245–254. [Google Scholar] [CrossRef] [PubMed]
- Patel, A.; Berdunov, V.; King, D.; Quayyum, Z.; Wittenberg, R.; Knapp, M. Executive Summary Part 2: Burden of Stroke in the Next 20 Years and Potential Returns from Increased Spending on Research; Stroke Association: London, UK, 2017. [Google Scholar]
- Hsieh, C.-Y.; Lee, T.-H.; Chang, K.-C.; Taiwan Stroke Society. A Nationwide Plan for Postacute Care of Stroke in Taiwan. Int. J. Stroke 2014, 9, E3. [Google Scholar] [CrossRef] [PubMed]
- Chien, S.H.; Sung, P.Y.; Liao, W.L.; Tsai, S.W. A Functional Recovery Profile for Patients with Stroke Following Post-Acute Rehabilitation Care in Taiwan. J. Formos. Med. Assoc. 2020, 119 Pt 2, 254–259. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, C.Y.; Tsao, W.C.; Lin, R.T.; Chao, A.C. Three Years of the Nationwide Post-Acute Stroke Care Program in Taiwan. J. Chin. Med. Assoc. 2018, 81, 87–88. [Google Scholar] [CrossRef] [PubMed]
- Lai, C.L.; Tsai, M.M.; Luo, J.Y.; Liao, W.C.; Hsu, P.S.; Chen, H.Y. Post-Acute Care for Stroke—A Retrospective Cohort Study in Taiwan. Patient Prefer. Adherence 2017, 11, 1309–1315. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Peng, L.-N.; Lu, W.-H.; Liang, C.-K.; Chou, M.-Y.; Chung, C.-P.; Tsai, S.-L.; Chen, Z.-J.; Hsiao, F.-Y.; Chen, L.-K.; Lin, C.-S.; et al. Functional Outcomes, Subsequent Healthcare Utilization, and Mortality of Stroke Postacute Care Patients in Taiwan: A Nationwide Propensity Score-Matched Study. J. Am. Med. Dir. Assoc. 2017, 18, 990.e7–990.e12. [Google Scholar] [CrossRef]
- Chou, H.Y.; Lo, Y.C.; Tsai, Y.W.; Shih, C.L.; Yeh, C.T. Increased Anxiety and Depression Symptoms in Post-Acute Care Patients with Stroke during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 19, 162. [Google Scholar] [CrossRef]
- Chu, C.L.; Lee, T.H.; Chen, Y.P.; Ro, L.S.; Hsu, J.L.; Chu, Y.C.; Chen, C.K.; Pei, Y.C. Recovery of Walking Ability in Stroke Patients through Postacute Care Rehabilitation. Biomed J. 2022. [Google Scholar] [CrossRef]
- Preston, E.; Ada, L.; Dean, C.; Stanton, R.; Waddington, G. What is the Probability of Patients who are Nonambulatory after Stroke Regaining Independent Walking? a Systematic Review. Int. J. Stroke 2011, 6, 531–540. [Google Scholar] [CrossRef]
- Rakesh, N.K.; Boiarsky, D.; Athar, A.; Hinds, S.; Stein, J. Post-Stroke Rehabilitation: Factors Predicting Discharge to Acute Versus Subacute Rehabilitation Facilities. Medicine 2019, 98, e15934. [Google Scholar] [CrossRef]
- Chiu, C.C.; Wang, J.J.; Hung, C.M.; Lin, H.F.; Hsien, H.H.; Hung, K.W.; Chiu, H.C.; Yeh, S.C.; Shi, H.Y. Impact of Multidisciplinary Stroke Post-Acute Care on Cost and Functional Status: A Prospective Study Based on Propensity Score Matching. Brain Sci. 2021, 11, 161. [Google Scholar] [CrossRef]
- Chen, Y.C.; Yeh, Y.J.; Wang, C.Y.; Lin, H.F.; Lin, C.H.; Hsien, H.H.; Hung, K.W.; Wang, J.D.; Shi, H.Y. Cost Utility Analysis of Multidisciplinary Postacute Care for Stroke: A Prospective Six-Hospital Cohort Study. Front. Cardiovasc. Med. 2022, 9, 826898. [Google Scholar] [CrossRef]
- Banks, J.L.; Marotta, C.A. Outcomes Validity and Reliability of the Modified Rankin Scale: Implications for Stroke Clinical Trials: A Literature Review and Synthesis. Stroke 2007, 38, 1091–1096. [Google Scholar] [CrossRef] [Green Version]
- Shah, S.; Vanclay, F.; Cooper, B. Improving the sensitivity of the Barthel Index for stroke rehabilitation. J. Clin. Epidemiol. 1989, 42, 703–709. [Google Scholar] [CrossRef]
- Mahoney, F.I.; Barthel, D.W. Functional evaluation: The Barthel Index. Md. State Med. J. 1965, 14, 61–65. [Google Scholar]
- Salbach, N.M.; Mayo, N.E.; Higgins, J.; Ahmed, S.; Finch, L.E.; Richards, C.L. Responsiveness and predictability of gait speed and other disability measures in acute stroke. Arch. Phys. Med. Rehabil. 2001, 82, 1204–1212. [Google Scholar] [CrossRef]
- Fulk, G.D.; He, Y.; Boyne, P.; Dunning, K. Predicting Home and Community Walking Activity Poststroke. Stroke 2017, 48, 406–411. [Google Scholar] [CrossRef]
- Kline, R.B. Principles and Practice of Structural Equation Modeling, 2nd ed.; Guilford Publications: New York, NY, USA, 2005. [Google Scholar]
- Hair, J.F., Jr.; Sarstedt, M.; Hopkins, L.; Kuppelwieser, V.G. Partial Least Squares Structural Equation Modeling (Pls-Sem): An Emerging Tool in Business Research. Eur. Bus. Rev. 2014, 26, 106–121. [Google Scholar] [CrossRef]
- Tung, Y.J.; Huang, C.T.; Lin, W.C.; Cheng, H.H.; Chow, J.C.; Ho, C.H.; Chou, W. Longer length of post-acute care stay causes greater functional improvements in poststroke patients. Medicine 2021, 100, e26564. [Google Scholar] [CrossRef]
- Wang, C.Y.; Chen, Y.R.; Hong, J.P.; Chan, C.C.; Chang, L.C.; Shi, H.Y. Rehabilitative post-acute care for stroke patients delivered by per-diem payment system in different hospitalization paths: A Taiwan pilot study. Int. J. Qual. Health Care 2017, 29, 779–784. [Google Scholar] [CrossRef] [Green Version]
- Wang, C.Y.; Miyoshi, S.; Chen, C.H.; Lee, K.C.; Chang, L.C.; Chung, J.H.; Shi, H.Y. Walking ability and functional status after post-acute care for stroke rehabilitation in different age groups: A prospective study based on propensity score matching. Aging 2020, 12, 10704–10714. [Google Scholar] [CrossRef] [PubMed]
- Quinn, T.; Harrison, J.K.; Arthur, M. Assessment scales in stroke: Clinimetric and clinical considerations. Clin. Interv. Aging 2013, 8, 201–211. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wolfe, C.D.; Taub, N.; Woodrow, E.; Burney, P.G. Assessment of Scales of Disability and Handicap for Stroke Patients. Stroke 1991, 22, 1242–1244. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liu, F.; Tsang, R.C.; Zhou, J.; Zhou, M.; Zha, F.; Long, J.; Wang, Y. Relationship of Barthel Index and its Short Form with the Modified Rankin Scale in acute stroke patients. J. Stroke Cerebrovasc. Dis. 2020, 29, 105033. [Google Scholar] [CrossRef] [PubMed]
- Schmid, A.; Duncan, P.; Studenski, S.; Lai, S.; Richards, L.; Perera, S.; Wu, S.S. Improvements in Speed-Based Gait Classifications Are Meaningful. Stroke 2007, 38, 2096–2100. [Google Scholar] [CrossRef] [Green Version]
- Brincks, J.; Nielsen, J.F. Increased power generation in impaired lower extremities correlated with changes in walking speeds in sub-acute stroke patients. Clin. Biomech. 2012, 27, 138–144. [Google Scholar] [CrossRef]
- In, T.S.; Jung, J.H.; Jung, K.S.; Cho, H.Y. Effect of Sit-to-Stand Training Combined with Taping on Spasticity, Strength, Gait Speed and Quality of Life in Patients with Stroke: A Randomized Controlled Trial. Life 2021, 11, 511. [Google Scholar] [CrossRef]
- Vistamehr, A.; Kautz, S.A.; Bowden, M.G.; Neptune, R.R. The influence of locomotor training on dynamic balance during steady-state walking post-stroke. J. Biomech. 2019, 89, 21–27. [Google Scholar] [CrossRef]
- Newell, A.M.; VanSwearingen, J.M.; Hile, E.; Brach, J.S. The Modified Gait Efficacy Scale: Establishing the Psychometric Properties in Older Adults. Phys. Ther. 2012, 92, 318–328. [Google Scholar] [CrossRef]
- Makizako, H.; Shimada, H.; Yoshida, D.; Anan, Y.; Ito, T.; Doi, T.; Tsutsumimoto, K.; Uemura, K.; Brach, J.S.; Suzuki, T. Reliability and Validity of the Japanese Version of the Modified Gait Efficacy Scale. J. Jpn. Phys. Ther. Assoc. 2014, 17, 45. [Google Scholar] [CrossRef] [Green Version]
- Chang, K.V.; Chen, K.; Chen, Y.; Lien, W.; Chang, W.; Lai, C.; Wu, C.; Chen, C.; Chen, Y.; Wu, W.; et al. A Multicenter Study to Compare the Effectiveness of the Inpatient Post Acute Care Program Versus Traditional Rehabilitation for Stroke Survivors. Sci. Rep. 2022, 12, 12811. [Google Scholar] [CrossRef]
- Longley, V.; Peters, S.; Swarbrick, C.; Bowen, A. What factors affect clinical decision-making about access to stroke rehabilitation? A systematic review. Clin. Rehabil. 2019, 33, 304–316. [Google Scholar] [CrossRef] [Green Version]
- Hung, C.Y.; Wu, W.T.; Chang, K.V.; Wang, T.G.; Han, D.S. Predicting the length of hospital stay of post-acute care patients in Taiwan using the Chinese version of the continuity assessment record and evaluation item set. PLoS ONE 2017, 12, e0183612. [Google Scholar] [CrossRef] [Green Version]
- Koton, S.; Telman, G.; Kimiagar, I.; Tanne, D. Gender differences in characteristics, management and outcome at discharge and three months after stroke in a national acute stroke registry. Int. J. Cardiol. 2013, 168, 4081–4084. [Google Scholar] [CrossRef]
- Mak, A.K.; Mackenzie, A.; Lui, M.H. Changing needs of Chinese family caregivers of stroke survivors. J. Clin. Nurs. 2007, 16, 971–979. [Google Scholar] [CrossRef]
- Qiu, X.; Sit, J.W.; Koo, F.K.; Qiu, O.X. The influence of Chinese culture on family caregivers of stroke survivors: A qualitative study. J. Clin. Nurs. 2017, 27, e309–e319. [Google Scholar] [CrossRef] [PubMed]
| Variables | Mean (SD) or n (%) | |
|---|---|---|
| Demographics | ||
| Age, years | 63.74 (13.08) | |
| Sex | Female | 91 (34.6%) |
| Male | 172 (65.4%) | |
| Clinical Attributes | ||
| Stroke Type | ||
| Ischemic | 188 (71.5%) | |
| Hemorrhagic | 75 (28.5%) | |
| Hypertension | 247 (93.9%) | |
| Coronary Artery Disease | 76 (28.9%) | |
| Diabetes Mellitus | 112 (42.6%) | |
| Hyperlipidemia | 121 (46.0%) | |
| Previous Stroke | 53 (20.2%) | |
| Common Risk Factors | ||
| Smoking | 59 (22.4%) | |
| Drinking | 29 (11.0%) | |
| Prerehabilitation Functional Status | ||
| mRS | 3.66 (0.47) | |
| BI | 44.56 (22.23) | |
| 5MWS | 0.1 (0.24) | |
| 6MWD | 25.67 (67.64) | |
| Medical Care of PAC-CVD Program | ||
| PAC-CVD LOS, days | 32.57 (15.28) | |
| Weeks of Hospitalization | ||
| 0–3 Weeks | 111 (42.2%) | |
| 4–6 Weeks | 126 (47.9%) | |
| 7–9 Weeks | 20 (7.6%) | |
| 10–12 Weeks | 6 (2.3%) | |
| Cost of NHI, USD | 3189.95 (1501.07) | |
| 0–3 Weeks Functional Status | |||
|---|---|---|---|
| Variables | W0 | W3 | p |
| mRS | 3.66 (0.47) | 3.02 (0.90) | <0.001 *** |
| BI | 44.56 (22.23) | 68.92 (24.40) | <0.001 *** |
| 5MWS | 0.1 (0.24) | 0.29 (0.45) | <0.001 *** |
| 6MWD | 25.67 (67.64) | 85.15 (126.87) | <0.001 *** |
| Cost of NHI | |||
| Admitted | 0–3 weeks | p | |
| Cost of NHI, USD | - | 1895.31 (251.47) | - |
| 0–6 Weeks Functional Status | ||||||
|---|---|---|---|---|---|---|
| Variables | W0 | W3 | W6 | F | p | Pairwise Comparison |
| mRS | 3.87 (0.33) | 3.51 (0.61) | 3.12 (0.73) | 131.88 *** | <0.001 | W0 > W3 a, W0 > W6 a, W3 > W6 a |
| BI | 34.38 (18.44) | 56.58 (21.73) | 67.89 (20.62) | 327.51 *** | <0.001 | W6 > W3 a, W6 > W0 a, W3 > W0 a |
| 5MWS | 0.02 (0.10) | 0.14 (0.42) | 0.23 (0.34) | 28.38 *** | <0.001 | W6 > W3 a, W6 > W0 a, W3 > W0 a |
| 6MWD | 6.59 (40.77) | 32.97 (81.13) | 65.54 (101.28) | 54.60 *** | <0.001 | W6 > W3 a, W6 > W0 a, W3 > W0 a |
| Cost of NHI | ||||||
| Admitted | W3 | W6 | F | p | Pairwise Comparison | |
| Cost of NHI, USD | - | 2014.74 (84.32) | 1843.27 (291.97) | 6344.74 *** | <0.001 | W3 > W6 a, W6 > W0 a, W3 > W0 a |
| 0–9 Weeks Functional Status | |||||||
|---|---|---|---|---|---|---|---|
| Variables | W0 | W3 | W6 | W9 | F | p | Pairwise Comparison |
| mRS | 3.88 (0.33) | 3.73 (0.45) | 3.54 (0.51) | 2.96 (0.77) | 21.16 *** | <0.001 | W0 > W3, W0 > W6 a, W0 > W9 a, W3 > W6, W3 > W9 a, W6 > W9 a |
| BI | 33.27 (16.55) | 51.35 (20.86) | 58.46 (19.17) | 74.62 (16.12) | 72.31 *** | <0.001 | W9 > W6 a, W9 > W3 a, W9 > W0 a, W6 > W3 a, W6 > W0 a, W3 > W0 a |
| 5MWS | <0.001 (<0.001) | 0.04 (0.14) | 0.07 (0.22) | 0.20 (0.28) | 9.86 *** | 0.001 | W9 > W6 a, W9 > W3 a, W9 > W0 a, W6 > W3, W6 > W0, W3 > W0 |
| 6MWD | <0.001 (<0.001) | 9.35 (37.59) | 21.98 (58.07) | 61.31 (104.13) | 7.66 ** | 0.004 | W9 > W6, W9 > W3 a, W9 > W0 a, W6 > W3, W6 > W0, W3 > W0 |
| Cost of NHI | |||||||
| Admitted | W3 | W6 | W9 | F | p | Pairwise Comparison | |
| Cost of NHI, USD | - | 1993.31 (92.54) | 2060.84 (44.57) | 1928.40 (178.61) | 2487.77 *** | <0.001 | W6 > W9 a, W3 > W9, W9 > W0 a, W6 > W3 a, W6 > W0 a, W3 > W0 a |
| 9–12 Weeks Functional Status | |||||
|---|---|---|---|---|---|
| Variables | W9 | W12 | |||
| Median (IQR) | Mean (SD) | Median (IQR) | Mean (SD) | p | |
| mRS | 3 (0.25) | 3.17 (0.41) | 3 (1) | 2.67 (0.52) | 0.08 |
| BI | 62.5 (13.75) | 63.33 (8.76) | 75 (16.25) | 77.50 (12.15) | 0.04 * |
| 5MWS | 0.05 (0.14) | 0.07 (0.08) | 0.17 (0.23) | 0.14 (0.12) | 0.07 |
| 6MWD | 0 (38.75) | 14.17 (22.45) | 59 (58.25) | 44.83 (30.92) | 0.04 * |
| Cost of NHI during 10 to 12 weeks | |||||
| Cost of NHI, USD | 1695.53 (264.65) | ||||
| Model Summary | |||||||
|---|---|---|---|---|---|---|---|
| Model | R | R2 | Adjusted R2 | R2 Change | F Change | Sig. F Change | Durbin-Watson |
| 1 | 0.208 | 0.043 | 0.036 | 0.043 | 5.858 | 0.003 | - |
| 2 | 0.263 | 0.069 | 0.032 | 0.026 | 0.879 | 0.535 | - |
| 3 | 0.407 | 0.166 | 0.119 | 0.097 | 7.175 | <0.001 | 1.552 |
| Predictive Factor Input | |||||||
| Model | Predictor | B | β | t | p | ||
| 1 | Constant | 59,524.25 | - | 24.14 | <0.001 | ||
| Age | −75.79 | −0.133 | −2.162 | 0.032 * | |||
| Sex | 2153.20 | 0.138 | 2.238 | 0.026 * | |||
| 2 | Constant | 56,156.05 | - | 15.95 | <0.001 | ||
| Age | −74.55 | −0.131 | −1.874 | 0.062 | |||
| Sex | 2576.49 | 0.165 | 2.487 | 0.014 * | |||
| Stroke Type | 31.11 | 0.002 | 0.025 | 0.980 | |||
| Previous Stroke | 1675.62 | 0.090 | 1.440 | 0.151 | |||
| Hypertension | 2474.72 | 0.080 | 1.271 | 0.205 | |||
| Coronary Artery Disease | 534.77 | 0.033 | 0.515 | 0.607 | |||
| Diabetes Mellitus | −770.90 | −0.051 | −0.806 | 0.421 | |||
| Hyperlipidemia | −687.58 | −0.046 | −0.669 | 0.504 | |||
| Smoking | 334.69 | 0.019 | 0.257 | 0.797 | |||
| Drinking | −2207.76 | −0.093 | −1.358 | 0.176 | |||
| 3 | Constant | 56,588.12 | - | 9.576 | <0.001 | ||
| Age | −110.62 | −0.194 | −2.836 | 0.005 ** | |||
| Sex | 2076.54 | 0.133 | 2.059 | 0.041 * | |||
| Stroke Type | −554.81 | −0.034 | −0.468 | 0.640 | |||
| Previous Stroke | 1849.77 | 0.100 | 1.660 | 0.098 | |||
| Hypertension | 2391.33 | 0.077 | 1.268 | 0.206 | |||
| Coronary Artery Disease | 496.01 | 0.030 | 0.494 | 0.622 | |||
| Diabetes Mellitus | −531.20 | −0.035 | −0.579 | 0.563 | |||
| Hyperlipidemia | −60.69 | −0.004 | −0.061 | 0.951 | |||
| Smoking | 637.66 | 0.036 | 0.510 | 0.611 | |||
| Drinking | −2144.91 | −0.090 | −1.379 | 0.169 | |||
| mRS | 1571.62 | 0.189 | 1.764 | 0.079 | |||
| BI | −40.13 | −0.132 | −1.352 | 0.178 | |||
| 5MWS | 124.40 | 0.008 | 0.073 | 0.942 | |||
| 6MWD | −2.06 | −0.035 | −0.328 | 0.743 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chou, H.-Y.; Tsai, Y.-W.; Ma, S.-C.; Ma, S.-M.; Shih, C.-L.; Yeh, C.-T. Efficacy and Cost over 12 Hospitalization Weeks of Postacute Care for Stroke. Int. J. Environ. Res. Public Health 2023, 20, 1419. https://doi.org/10.3390/ijerph20021419
Chou H-Y, Tsai Y-W, Ma S-C, Ma S-M, Shih C-L, Yeh C-T. Efficacy and Cost over 12 Hospitalization Weeks of Postacute Care for Stroke. International Journal of Environmental Research and Public Health. 2023; 20(2):1419. https://doi.org/10.3390/ijerph20021419
Chicago/Turabian StyleChou, Hsiang-Yun, Ya-Wen Tsai, Shang-Chun Ma, Shang-Min Ma, Chia-Li Shih, and Chieh-Ting Yeh. 2023. "Efficacy and Cost over 12 Hospitalization Weeks of Postacute Care for Stroke" International Journal of Environmental Research and Public Health 20, no. 2: 1419. https://doi.org/10.3390/ijerph20021419





