The Variables of the Readiness for Discharge from Hospital in Patients after Myocardial Infarction
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Settings, and Participants
2.3. Instruments
2.4. Statistical Analyses
2.5. Ethical Procedure
3. Results
3.1. Characteristics of the Study Group
3.2. Readiness for Hospital Discharge (RHD-MIS)
3.2.1. RHD-MIS Subscale 1: The Assessment of Subjective Knowledge
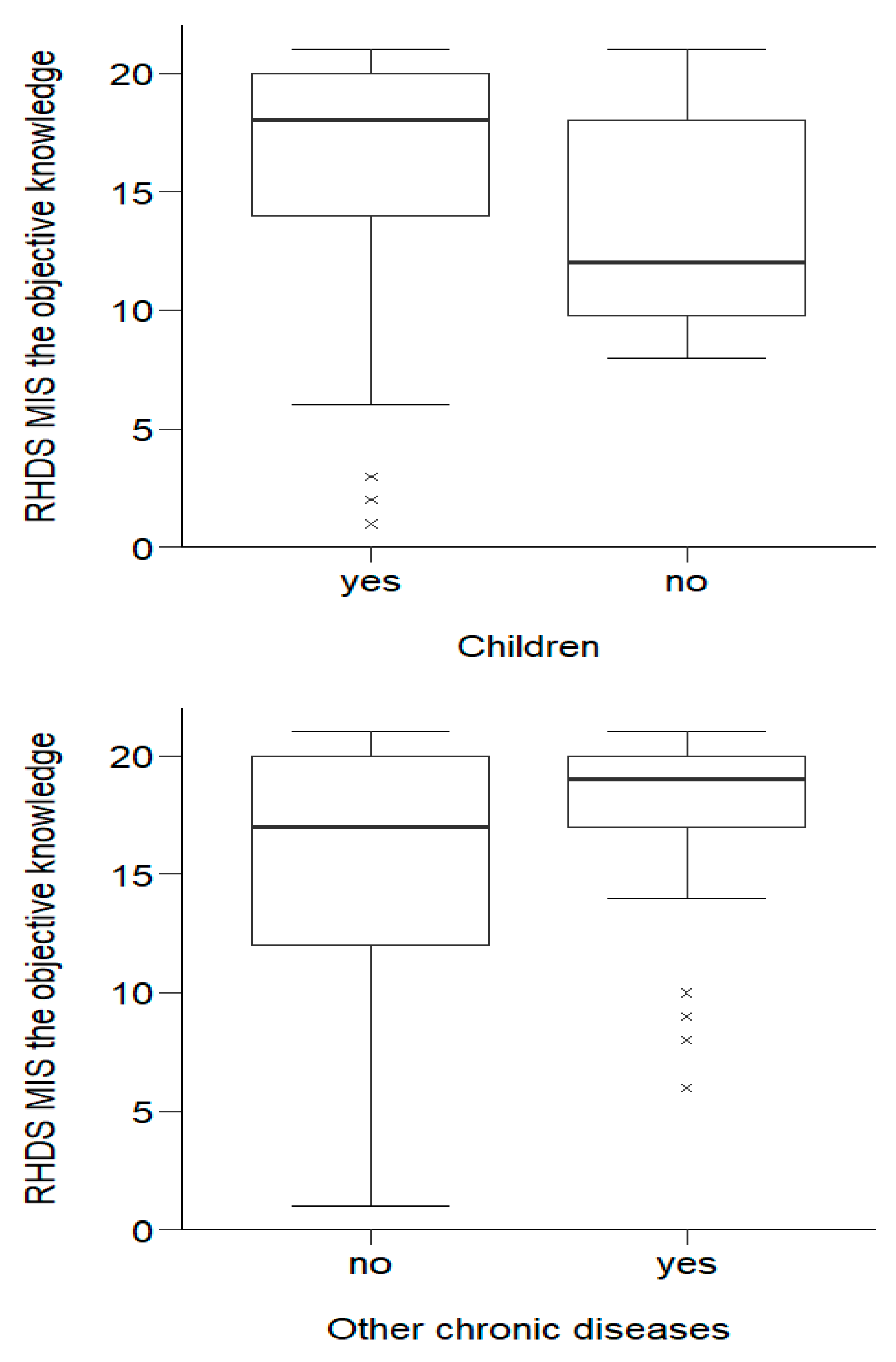
3.2.2. RHD-MIS Subscale 3: The Assessment of Objective Knowledge
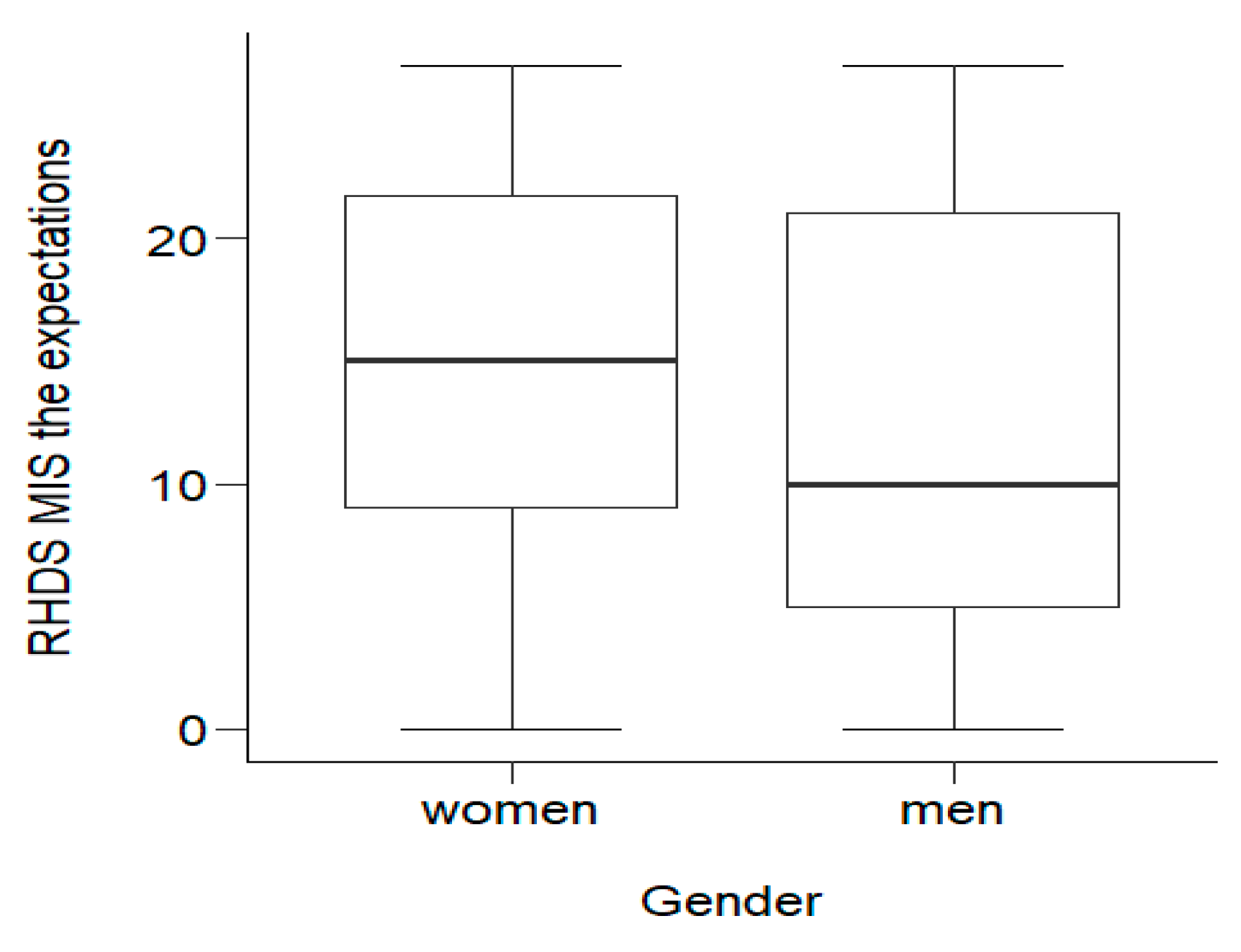
3.2.3. RHD-MIS Subscale 3: The Assessment of Expectations
3.3. The Functioning in Chronic Illness Scale (FCIS)
3.3.1. Part 1 of FCIS Scale: The Impact of Illness on Patient
3.3.2. Part 2 of FCIS Scale: The Patient’s Impact on the Illness
3.3.3. Part 3 of FCIS Scale: The Impact of Illness on Patient’s Attitude
3.4. Correlation between Readiness for Discharge from Hospital after MI and Functioning with Chronic Illness
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Carroll, A.; Dowling, M. Discharge planning: Communication, education and patient participation. Br. J. Nurs. 2007, 16, 882–886. [Google Scholar] [CrossRef]
- Galvin, E.C.; Wills, T.; Coffey, A. Readiness for hospital discharge: A concept analysis. J. Adv. Nurs. 2017, 73, 2547–2557. [Google Scholar] [CrossRef]
- Mabire, C.; Bachnick, S.; Ausserhofer, D.; Simon, M.; Match RN Study Group. Patient readiness for hospital discharge and its relationship to discharge preparation and structural factors: A cross-sectional study. Int. J. Nurs. Stud. 2019, 90, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Niedolaz, K.; Hałas, K.; Kaźmierczak-Dziuk, A. Treatment of patient after myocardial infarction. Pediatr. Med. Rodz. 2011, 7, 186–198. [Google Scholar]
- Xiong, L.; Liu, Y.; Chen, Q.; Tian, Y.; Yang, M. Readiness for Hospital Discharge of Adult Patients with Major Depressive Disorder in China: A Cross-Sectional Study. Patient Prefer. Adherence 2021, 15, 1681–1692. [Google Scholar] [CrossRef]
- Balaban, R.B.; Weissman, J.S.; Samuel, P.A.; Woolhandler, S. Redefining and Redesigning Hospital Discharge to Enhance Patient Care: A Randomized Controlled Study. J. Gen. Intern. Med. 2008, 23, 1228–1233. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, M.; Wang, Y.; Meng, N.; Li, X. The factors of patient-reported readiness for hospital discharge in patients with depression: A cross-sectional study. J. Psychiatr. Ment. HealthNurs. 2021, 28, 409–421. [Google Scholar] [CrossRef]
- Kosobucka, A.; Michalski, P.; Pietrzykowski, Ł.; Kasprzak, M.; Fabiszak, T.; Felsmann, M.; Kubica, A. The impact of readiness to discharge from hospital on adherence to treatment in patients after myocardial infarction. Cardiol. J. 2022, 29, 582–590. [Google Scholar] [CrossRef] [Green Version]
- Hydzik, P.; Kolarczyk, E.; Kustrzycki, W.; Kubielas, G.; Kałużna-Oleksy, M.; Szczepanowski, R.; Uchmanowicz, B. Readiness for Discharge from Hospital after Myocardial Infarction: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2021, 18, 6937. [Google Scholar] [CrossRef]
- Pietrzykowski, Ł.; Kasprzak, M.; Michalski, P.; Kosobucka, A.; Fabiszak, T.; Kubica, A. The influence of patient expectations on adherence to treatment regimen after myocardial infarction. Patient Educ. Couns. 2021, 105, 426–431. [Google Scholar] [CrossRef] [PubMed]
- von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P. STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for reporting observational studies. Int. J. Surg. 2014, 12, 1495–7499. [Google Scholar] [CrossRef]
- Statistics Poland, Demographic Surveys Department. Demographic Situation in Poland up to 2020.Death and Mortality. Available online: https://stat.gov.pl (accessed on 15 December 2022).
- Buszko, K.; Ksobucka, A.; Michalski, P.; Pietrzykowski, Ł.; Jurek, A.; Wawrzyniak, M.; Obońska, K.; Felsmann, M.; Kubica, A. The readiness for hospital discharge of patients after acute myocardial infarction: A new self-reported questionnaire. Med. Res. J. 2017, 2, 20–28. [Google Scholar] [CrossRef] [Green Version]
- Buszko, K.; Pietrzykowski, Ł.; Michalski, P.; Kosobucka, A.; Stolarek, W.; Fabiszak, T.; Kubica, A. Validation of the Functioning in Chronic Illness Scale (FCIS). Med. Res. J. 2018, 3, 63–69. [Google Scholar] [CrossRef] [Green Version]
- World Medical Association. World Medical Association Declaration of Helsinki: Ethical principles for medical research involving human subjects. JAMA 2013, 310, 2191–2194. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vijayananthan, A.; Nawawi, O. The importance of Good Clinical Practice guidelines and its role in clinical trials. Biomed. Imaging Interv. J. 2008, 4, e5. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, M.; Moriarty, H.; Schneider, A.; Dowdell, E.B.; Bowles, K.H. Patients’ and caregivers’ perspectives in determining discharge readiness from home health. Geriatr. Nurs. 2021, 42, 151–158. [Google Scholar] [CrossRef]
- Sobieszek, A.; Milewski, K. Specjalized managed care –heart attack. Kardiol. Inwazyjna 2017, 12, 4–6. [Google Scholar]
- Wallace, A.S.; Perkhounkova, Y.; Bohr, N.L.; Chung, S.J. Readiness for Hospital Discharge, Health Literacy, and Social Living Status. Clin. Nurs. Res. 2016, 25, 494–511. [Google Scholar] [CrossRef]
- Andruszkiewicz, A.; Kubica, A.; Nowik, M.; Michalski., P.; Idczak, H. Assessment of readiness for discharge of patients with chronic diseases. Zdr. Publicznei Zarządzanie 2016, 14, 44–52. [Google Scholar]
- Bahr, S.J.; Bang, J.; Yakusheva, O.; Bobay, K.L.; Krejci, J.; Costa, L.; Hughes, R.G.; Hamilton, M.; Siclovan, D.M.; Weiss, M.E. Nurse Continuity at Discharge and Return to Hospital. Nurs. Res. 2020, 69, 186–196. [Google Scholar] [CrossRef]
- Luther, B.; Wilson, R.D.; Kranz, C.; Krahulec, M. Discharge Processes: What Evidence Tells Us Is Most Effective. Orthop. Nurs. 2019, 38, 328–333. [Google Scholar] [CrossRef] [PubMed]
- Olano-Lizarraga, M.; Oroviogoicoechea, C.; Errasti-Ibarrondo, B.; Saracíbar-Razquin, M. The personal experience of living with chronic heart failure: A qualitative meta-synthesis of the literature. J. Clin. Nurs. 2016, 25, 2413–2429. [Google Scholar] [CrossRef] [PubMed]

| Variable | n | M ± SD | Me | Q1–Q3 | p | |
|---|---|---|---|---|---|---|
| Gender | women | 70 | 48.16 ± 8.97 | 49.00 | 43.00–54.00 | 0.057 2 |
| men | 149 | 45.94 ± 11.37 | 45.00 | 39.00–53.00 | ||
| Age range | ≤60 years | 78 | 47.83 ± 12,06 | 47.50 | 39.00–57.00 | 0.392 4 |
| 61–70 years | 73 | 47.47 ± 11.78 | 45.00 | 40.00–55.00 | ||
| ≥70 years | 66 | 44.44 ± 7.05 | 45.50 | 39.00–50.00 | ||
| BMI range | normal | 54 | 47.72 ± 10.19 | 48.00 | 40.00–54.00 | 0.959 3 |
| overweight | 93 | 46.65 ± 10.76 | 45.00 | 40.00–54.00 | ||
| obesity | 71 | 46.00 ± 11.05 | 45.00 | 39.00–53.00 | ||
| Marital status | in relationship | 148 | 46.82 ± 11.26 | 46.00 | 39.00–54.00 | 0.917 1 |
| single | 57 | 46.65 ± 9.19 | 46.00 | 40.00–52.00 | ||
| Place of residence | city | 107 | 47.17 ± 10.05 | 47.00 | 41.00–54.00 | 0.482 1 |
| village | 77 | 46.04 ± 11.59 | 45.00 | 39.00–54.00 | ||
| Education | primary | 35 | 45.37 ± 9.78 | 45.00 | 40.00–53.00 | 0.681 3 |
| vocational | 88 | 46.11 ± 11.42 | 45.50 | 39.00–53.50 | ||
| secondary | 68 | 47.79 ± 9.82 | 48.00 | 41.50–54.00 | ||
| higher | 23 | 47.43 ± 12.10 | 45.00 | 39.00–57.00 | ||
| Professional activity | active | 67 | 48.75 ± 11.74 | 48.00 | 39.00–58.00 | 0.176 2 |
| inactive | 100 | 45.70 ± 11.01 | 44.50 | 39.00–53.00 | ||
| Children | yes | 184 | 46.87 ± 10.93 | 46.00 | 39.50–54.00 | 0.861 1 |
| no | 16 | 46.38 ± 9.07 | 44.50 | 41.00–49.50 | ||
| Arterial hypertension | no | 71 | 47.63 ± 11.51 | 47.00 | 40.00–55.00 | 0.346 1 |
| yes | 148 | 46.18 ± 10.29 | 46.00 | 39.00–53.00 | ||
| Diabetes | no | 152 | 47.19 ± 10.78 | 46.50 | 40.00–54.00 | 0.259 1 |
| yes | 67 | 45.42 ± 10.49 | 46.00 | 39.00–52.00 | ||
| Lipid disorders | no | 164 | 46.48 ± 11.18 | 45.50 | 39.00–54.00 | 0.681 1 |
| yes | 55 | 47.16 ± 9.16 | 47.00 | 40.00–52.00 | ||
| Other chronic diseases | no | 149 | 46.79 ± 11.10 | 47.00 | 39.00–54.00 | 0.783 1 |
| yes | 70 | 46.36 ± 9.84 | 45.00 | 40.00–53.00 | ||
| Smoking | currently | 60 | 48.10 ± 10.30 | 47.50 | 42.50–54.50 | 0.307 3 |
| never | 105 | 47.19 ± 11.50 | 47.00 | 40.00–54.00 | ||
| in the past | 54 | 43.98 ± 9.09 | 42.00 | 37.00–48.00 | ||
| Myocardial infarction | first | 178 | 46.80 ± 10.44 | 46.00 | 40.00–54.00 | 0.689 1 |
| next | 40 | 46.05 ± 12.00 | 44.50 | 37.00–53.50 | ||
| Total | 219 | 46.65 ± 10.70 | 46.00 | 39.50–54.00 | - | |
| Readiness for hospital discharge | Number of points | Interpretation | n | % | ||
| 0–43 | Low level | 89 | 40.6% | |||
| 44–57 | Intermediate level | 94 | 42.9% | |||
| 58–69 | High level | 36 | 16.5% | |||
| Variable | n | M ± SD | Me | Q1–Q3 | p | |
|---|---|---|---|---|---|---|
| Gender | women | 70 | 17.03 ± 4.19 | 18.00 | 15.00–20.00 | 0.783 2 |
| men | 149 | 17.24 ± 4.61 | 18.00 | 14.00–21.00 | ||
| Age range | ≤60 years | 78 | 17.88 ± 4.79 | 19.00 | 15.00–21.00 | 0.232 4 |
| 61–70 years | 73 | 16.88 ± 4.57 | 18.00 | 14.00–21.00 | ||
| ≥70 years | 66 | 16.58 ± 3.93 | 17.00 | 15.00–20.00 | ||
| BMI range | normal | 54 | 16.81 ± 4.22 | 17.00 | 15.00–21.00 | 0.786 4 |
| overweight | 93 | 17.54 ± 4.86 | 19.00 | 15.00–21.00 | ||
| obesity | 71 | 17.03 ± 4.15 | 18.00 | 14.00–21.00 | ||
| Marital status | in relationship | 148 | 17.21 ± 4.59 | 18.00 | 15.00–21.00 | 0.376 2 |
| single | 57 | 17.61 ± 3.79 | 19.00 | 15.00–21.00 | ||
| Place of residence | City | 107 | 17.36 ± 3.66 | 19.00 | 14.00–21.00 | 0.603 2 |
| village | 77 | 17.57 ± 3.72 | 18.00 | 15.00–21.00 | ||
| Education | primary | 35 | 16.80 ± 4.34 | 17.00 | 15.00–20.00 | 0.403 4 |
| vocational | 88 | 16.93 ± 5.15 | 18.00 | 14.00–21.00 | ||
| secondary | 68 | 17.71 ± 3.56 | 18.50 | 15.00–21.00 | ||
| higher | 23 | 17.57 ± 3.89 | 19.00 | 16.00–21.00 | ||
| Professional activity | active | 67 | 18.61 ± 4.55 | 19.00 | 17.00–21.00 | 0.293 2 |
| inactive | 100 | 17.41 ± 4.28 | 19.00 | 15.00–21.00 | ||
| Children | yes | 184 | 17.36 ± 4.51 | 18.50 | 15.00–21.00 | 0.221 2 |
| no | 16 | 16.44 ± 3.16 | 15.00 | 14.50–20.00 | ||
| Arterial hypertension | no | 71 | 17.82 ± 5.22 | 19.00 | 16.00–21.00 | 0.192 2 |
| yes | 148 | 16.86 ± 4.05 | 18.00 | 14.00–21.00 | ||
| Diabetes | no | 152 | 17.39 ± 4.54 | 18.00 | 15.00–21.00 | 0.388 2 |
| yes | 67 | 16.69 ± 4.31 | 17.00 | 14.00–21.00 | ||
| Lipid disorders | no | 164 | 17.24 ± 4.22 | 19.00 | 15.00–21.00 | 0.159 2 |
| yes | 55 | 16.98 ± 5.20 | 17.00 | 15.00–20.00 | ||
| Other chronic diseases | no | 149 | 17.51 ± 4.30 | 18.00 | 15.00–21.00 | 0.311 2 |
| yes | 70 | 16.46 ± 4.78 | 18.00 | 14.00–21.00 | ||
| Smoking | currently | 60 | 17.32 ± 5.50 | 18.00 | 15.00–21.00 | 0.182 4 |
| never | 105 | 17.35 ± 4.30 | 19.00 | 15.00–21.00 | ||
| in the past | 54 | 16.67 ± 3.45 | 17.00 | 14.00–20.00 | ||
| Myocardial infarction | first | 178 | 17.35 ± 4.44 | 18.50 | 15.00–21.00 | 0.480 2 |
| next | 40 | 16.40 ± 4.62 | 17.00 | 14.00–21.00 | ||
| Total | 219 | 17.17 ± 4.47 | 18.00 | 15.00–21.00 | - | |
| Subjective knowledge | Number of points | Interpretation | n | % | ||
| 0–15 | Low level | 73 | 33.3% | |||
| 16–18 | Intermediate level | 41 | 18.8% | |||
| 19–21 | High level | 105 | 47.9% | |||
| Variable | n | M ± SD | Me | Q1–Q3 | p | |
|---|---|---|---|---|---|---|
| Gender | women | 80 | 81.99 ± 11.73 | 82.00 | 73.50–88.50 | 0.347 1 |
| men | 162 | 83.52 ± 12.05 | 85.00 | 76.00–92.00 | ||
| Age range | ≤60 years | 85 | 85.04 ± 11.81 | 87.00 | 76.00–93.00 | 0.444 3 |
| 61–70 years | 83 | 83.60 ± 11.48 | 85.00 | 77.00–90.00 | ||
| ≥70 years | 72 | 79.93 ± 12.30 | 81.00 | 72.50–87.00 | ||
| BMI range | normal | 57 | 83.09 ± 13.95 | 84.00 | 74.00–92.00 | 0.902 3 |
| overweight | 99 | 84.63 ± 11.22 | 85.00 | 79.00–93.00 | ||
| obesity | 84 | 81.06 ± 11.25 | 82.00 | 72.00–88.50 | ||
| Marital status | In relationship | 162 | 83.41 ± 11.21 | 84.00 | 77.00–91.00 | 0.538 1 |
| single | 66 | 82.35 ± 13.24 | 84.00 | 74.00–91.00 | ||
| Place of residence | city | 123 | 82.65 ± 11.14 | 84.00 | 76.00–89.00 | 0.383 1 |
| village | 83 | 84.08 ± 12.16 | 84.00 | 76.00–94.00 | ||
| Education | primary | 40 | 82.63 ± 11.72 | 85.00 | 74.50–90.50 | 0.500 4 |
| vocational | 98 | 82.68 ± 11.90 | 82.50 | 76.00–90.00 | ||
| secondary | 74 | 82.43 ± 11.99 | 84.00 | 75.00–89.00 | ||
| higher | 25 | 87.04 ± 12.27 | 86.00 | 79.00–97.00 | ||
| Professional activity | active B | 74 | 86.04 ± 11.63 | 87.50 | 80.00–93.00 | 0.026 1 |
| inactive | 116 | 82.03 ± 12.18 | 82.00 | 74.00–90.00 | ||
| Children | yes | 205 | 83.42 ± 11.42 | 85.00 | 76.00–91.00 | 0.065 1 |
| no | 17 | 77.94 ± 14.84 | 79.00 | 71.00–82.00 | ||
| Arterial hypertension | noB | 83 | 85.37 ± 11.65 | 86.00 | 77.00–93.00 | 0.034 2 |
| yes | 159 | 81.79 ± 11.94 | 82.00 | 75.00–89.00 | ||
| Diabetes | noB | 169 | 84.99 ± 11.41 | 86.00 | 80.00–92.00 | <0.001 2 |
| yes | 73 | 78.45 ± 11.96 | 78.00 | 70.00–86.00 | ||
| Lipid disorders | no | 184 | 83.76 ± 11.73 | 85.00 | 77.00–91.50 | 0.084 1 |
| yes | 58 | 80.66 ± 12.38 | 81.50 | 73.00–87.00 | ||
| Other chronic diseases | no B | 168 | 84.15 ± 10.99 | 85.00 | 78.00–91.00 | 0.040 1 |
| yes | 74 | 80.43 ± 13.60 | 81.00 | 71.00–89.00 | ||
| Smoking | currently | 64 | 85.31 ± 11.56 | 87.00 | 78.00–93.00 | 0.191 3 |
| never | 114 | 82.21 ± 12.80 | 82.00 | 74.00–90.00 | ||
| In the past | 64 | 82.16 ± 10.52 | 84.00 | 76.50–88.00 | ||
| Myocardial infarction | first | 199 | 83.64 ± 11.88 | 84.00 | 76.00–92.00 | 0.094 1 |
| next | 42 | 80.24 ± 12.06 | 85.00 | 72.00–89.00 | ||
| Total | 242 | 83.02 ± 11.94 | 84.00 | 76.00–90.75 | - | |
| General functioning in the illness | Number of points | Interpretation | n | % | ||
| 24–78 | Low level | 76 | 31.4% | |||
| 79–93 | Intermediate level | 118 | 48.8% | |||
| 94–120 | High level | 48 | 19.8% | |||
| Variable | n | M ± SD | Me | Q1–Q3 | p | |
|---|---|---|---|---|---|---|
| Gender | women | 80 | 26.18 ± 4.88 | 25.50 | 23.00–29.00 | 0.005 2 |
| men A | 162 | 27.60 ± 4.42 | 28.00 | 25.00–31.00 | ||
| Age range | ≤60 years C | 85 | 28.21 ± 3.86 | 28.00 | 25.00–32.00 | <0.001 4 |
| 61–70 years C | 83 | 27.39 ± 4.53 | 28.00 | 25.00–30.00 | ||
| ≤70 years | 72 | 25.40 ± 5.06 | 25.50 | 23.00–28.00 | ||
| BMI range | normal | 57 | 26.63 ± 5.18 | 26.00 | 24.00–30.00 | 0.676 4 |
| overweight | 99 | 27.34 ± 4.57 | 28.00 | 25.00–30.00 | ||
| obesity | 84 | 27.17 ± 4.32 | 27.00 | 24.00–30.50 | ||
| Marital status | in relationship | 162 | 27.35 ± 4.20 | 28.00 | 25.00–30.00 | 0.483 2 |
| single | 66 | 27.05 ± 5.35 | 27.00 | 24.00–31.00 | ||
| Place of residence | city | 123 | 27.37 ± 4.44 | 28.00 | 25.00–30.00 | 0.525 2 |
| village | 83 | 27.07 ± 4.85 | 27.00 | 24.00–30.00 | ||
| Education | primary | 40 | 26.98 ± 4.05 | 26.00 | 24.00–30.00 | 0.123 4 |
| vocational | 98 | 26.70 ± 5.20 | 27.00 | 24.00–29.00 | ||
| secondary | 74 | 27.09 ± 3.73 | 28.00 | 25.00–29.00 | ||
| higher | 25 | 29.20 ± 4.84 | 31.00 | 25.00–33.00 | ||
| Professional activity | active B | 74 | 28.70 ± 3.75 | 29.00 | 26.00–32.00 | 0.020 1 |
| inactive | 116 | 27.30 ± 4.19 | 28.00 | 24.00–30.00 | ||
| Children | yes | 205 | 27.42 ± 4.27 | 28.00 | 25.00–30.00 | 0.052 2 |
| no | 17 | 24.76 ± 6.76 | 25.00 | 23.00–29.00 | ||
| Arterial hypertension | noB | 83 | 28.06 ± 3.72 | 28.00 | 25.00–31.00 | 0.034 2 |
| yes | 159 | 26.64 ± 4.96 | 27.00 | 24.00–29.00 | ||
| Diabetes | noB | 169 | 27.55 ± 4.36 | 28.00 | 25.00–31.00 | 0.035 2 |
| yes | 73 | 26.15 ± 5.04 | 26.00 | 24.00–29.00 | ||
| Lipid disorders | no | 184 | 27.48 ± 4.03 | 28.00 | 25.00–30.00 | 0.070 2 |
| yes | 58 | 26.00 ± 6.01 | 25.00 | 24.00–29.00 | ||
| Other chronic diseases | no | 168 | 27.35 ± 4.64 | 28.00 | 25.00–31.00 | 0.167 2 |
| yes | 74 | 26.64 ± 4.56 | 27.00 | 24.00–30.00 | ||
| Smoking | currently | 64 | 28.33 ± 3.82 | 28.00 | 25.00–32.00 | 0.060 4 |
| never | 114 | 26.65 ± 4.69 | 27.00 | 24.00–29.00 | ||
| in the past | 64 | 26.78 ± 5.04 | 27.00 | 24.50–30.00 | ||
| Myocardial infarction | first | 199 | 27.32 ± 4.66 | 27.00 | 25.00–30.00 | 0.184 2 |
| next | 42 | 26.24 ± 4.41 | 26.50 | 24.00–29.00 | ||
| Total | 242 | 27.13 ± 4.61 | 27.00 | 25.00–30.00 | - | |
| The patient’s impact on the illness | Number of points | Interpretation | n | % | ||
| 8–24 | Low level | 59 | 24.4% | |||
| 25–29 | Intermediate level | 115 | 47.5% | |||
| 30–40 | High level | 68 | 28.1% | |||
| Variable | n | M ± SD | Me | Q1–Q3 | p | |
|---|---|---|---|---|---|---|
| Gender | women | 80 | 28.69 ± 4.90 | 28.00 | 26.00–31.50 | 0.079 2 |
| men | 162 | 29.60 ± 5.37 | 30.00 | 26.00–34.00 | ||
| Age range | ≤60 years | 85 | 29.96 ± 5.47 | 30.00 | 27.00–34.00 | 0.802 3 |
| 61–70 years | 83 | 29.53 ± 5.37 | 30.00 | 27.00–34.00 | ||
| ≥70 years | 72 | 28.29 ± 4.71 | 28.00 | 25.00–32.00 | ||
| BMI range | normal | 57 | 29.32 ± 5.99 | 29.00 | 25.00–34.00 | 0.736 3 |
| overweight | 99 | 29.94 ± 4.62 | 30.00 | 28.00–33.00 | ||
| obesity | 84 | 28.60 ± 5.35 | 28.00 | 25.00–33.00 | ||
| Marital status | in relationship | 162 | 29.44 ± 4.95 | 30.00 | 27.00–33.00 | 0.301 2 |
| single | 66 | 28.77 ± 5.86 | 28.50 | 25.00–33.00 | ||
| Place of residence | city | 123 | 28.83 ± 4.96 | 29.00 | 25.00–32.00 | 0.162 2 |
| village | 83 | 29.72 ± 5.31 | 30.00 | 27.00–33.00 | ||
| Education | primary | 40 | 28.48 ± 5.06 | 29.00 | 25.00–32.00 | 0.821 4 |
| vocational | 98 | 29.31 ± 5.26 | 30.00 | 26.00–34.00 | ||
| secondary | 74 | 29.55 ± 5.38 | 29.00 | 27.00–32.00 | ||
| higher | 25 | 29.84 ± 5.00 | 30.00 | 27.00–33.00 | ||
| Professional activity | active B | 74 | 30.51 ± 5.37 | 31.00 | 28.00–35.00 | 0.017 2 |
| inactive | 116 | 28.73 ± 5.22 | 29.00 | 25.00–32.00 | ||
| Children | yes B | 205 | 29.40 ± 5.20 | 30.00 | 26.00–33.00 | 0.046 2 |
| no | 17 | 26.88 ± 5.60 | 27.00 | 23.00–30.00 | ||
| Arterial hypertension | no | 83 | 30.07 ± 5.25 | 30.00 | 28.00–34.00 | 0.068 2 |
| yes | 159 | 28.89 ± 5.18 | 29.00 | 25.00–33.00 | ||
| Diabetes | noB | 169 | 30.21 ± 4.98 | 30.00 | 28.00–34.00 | <0.001 2 |
| yes | 73 | 27.18 ± 5.21 | 27.00 | 24.00–30.00 | ||
| Lipid disorders | no | 184 | 29.43 ± 5.42 | 30.00 | 26.50–33.00 | 0.313 2 |
| yes | 58 | 28.88 ± 4.58 | 29.00 | 26.00–32.00 | ||
| Other chronic diseases | no | 168 | 29.68 ± 5.00 | 30.00 | 27.00–33.00 | 0.147 2 |
| yes | 74 | 28.42 ± 5.65 | 29.00 | 25.00–33.00 | ||
| Smoking | currently | 64 | 30.20 ± 5.23 | 30.50 | 27.00–34.00 | 0.397 3 |
| never | 114 | 28.99 ± 5.18 | 29.00 | 26.00–32.00 | ||
| in the past | 64 | 28.94 ± 5.29 | 29.50 | 25.00–32.50 | ||
| Myocardial infarction | first | 199 | 29.48 ± 5.16 | 30.00 | 27.00–33.00 | 0.344 2 |
| next | 42 | 28.45 ± 5.59 | 29.00 | 25.00–32.00 | ||
| Total | 242 | 29.30 ± 5.23 | 29.00 | 26.00–33.00 | - | |
| The impact of illness on patient’s attitude | Number of points | Interpretation | n | % | ||
| 8–27 | Low level | 78 | 32.2% | |||
| 28–33 | Intermediate level | 111 | 45.9% | |||
| 34–40 | High level | 53 | 21.9% | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kolarczyk, E.; Witkowska, A.; Szymiczek, M.; Młynarska, A. The Variables of the Readiness for Discharge from Hospital in Patients after Myocardial Infarction. Int. J. Environ. Res. Public Health 2023, 20, 1582. https://doi.org/10.3390/ijerph20021582
Kolarczyk E, Witkowska A, Szymiczek M, Młynarska A. The Variables of the Readiness for Discharge from Hospital in Patients after Myocardial Infarction. International Journal of Environmental Research and Public Health. 2023; 20(2):1582. https://doi.org/10.3390/ijerph20021582
Chicago/Turabian StyleKolarczyk, Ewelina, Agnieszka Witkowska, Marek Szymiczek, and Agnieszka Młynarska. 2023. "The Variables of the Readiness for Discharge from Hospital in Patients after Myocardial Infarction" International Journal of Environmental Research and Public Health 20, no. 2: 1582. https://doi.org/10.3390/ijerph20021582




