Late Diagnosis of Swyer Syndrome in a Patient with Bilateral Germ Cell Tumor Treated with a Contraceptive Due to Primary Amenorrhea
Abstract
:1. Introduction
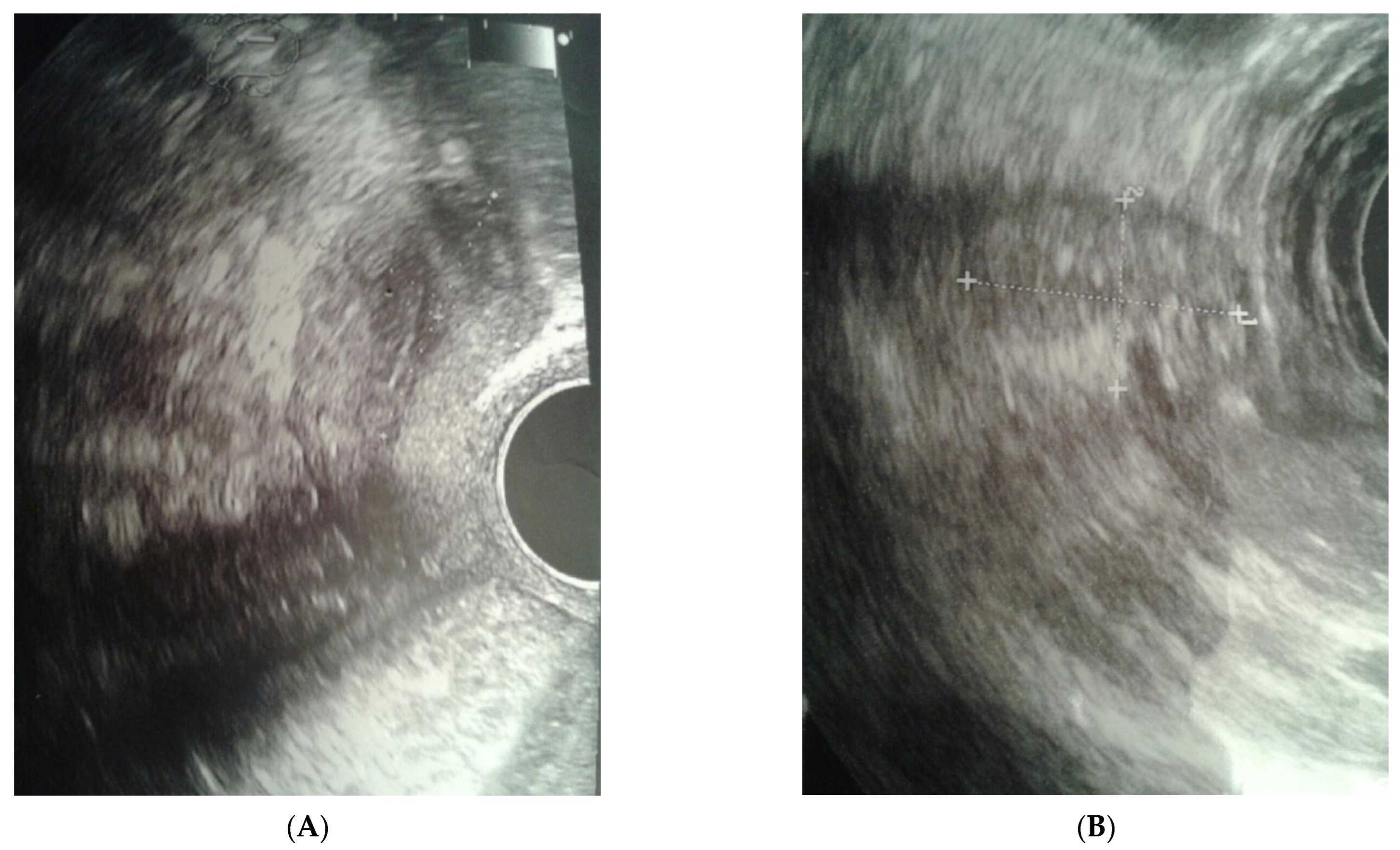
2. Case Report
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lee, P.A.; Houk, C.P.; Ahmed, S.F.; Hughes, I.A.; Achermann, J.; Baskin, L.; Berenbaum, S.; Bertelloni, S.; Brock, J.; Carmichael, P.; et al. Consensus statement on management of intersex disorders. Pediatrics 2006, 118, e488–e500. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ono, M.; Harley, V.R. Disorders of sex development: New genes, new concepts. Nat. Rev. Endocrinol. 2013, 9, 79–91. [Google Scholar] [CrossRef] [PubMed]
- King, T.F.J.; Conway, G.S. Swyer syndrome. Curr. Opin. Endocrinol. Diabetes Obes. 2014, 21, 504–510. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Loke, J.; Pearlman, A.; Radi, O.; Zuffardi, O.; Giussani, U.; Pallotta, R.; Camerino, G.; Ostrer, H. Mutations in MAP3K1 tilt the balance from SOX9/FGF9 to WNT/β-catenin signaling. Hum. Mol. Genet. 2014, 23, 1073–1083. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cools, M.; Drop, S.L.S.; Wolffenbuttel, K.P.; Oosterhuis, J.W.; Looijenga, L.H.J. Germ cell tumors in the intersex gonad: Old paths, new directions, moving frontiers. Endocr. Rev. 2006, 27, 468–484. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hughes, I.A.; Houk, C.; Ahmed, S.F.; Lee, P.A. Consensus statement on management of intersex disorders. J. Pediatr. Urol. 2006, 2, 148–162. [Google Scholar] [CrossRef] [PubMed]
- Michala, L.; Goswami, D.; Creighton, S.M.; Conway, G.S. Swyer syndrome: Presentation and outcomes. BJOG Int. J. Obstet. Gynaecol. 2008, 115, 737–741. [Google Scholar] [CrossRef] [PubMed]
- Seppä, S.; Kuiri, T.H.; Holopainen, E.; Voutilainen, R. Diagnosis and management of primary amenorrhea and female delayed puberty. Eur. J. Endocrinol. 2021, 184, R225–R242. [Google Scholar] [CrossRef] [PubMed]
- Klein, D.A.; Paradise, S.L.; Reeder, R.M. Amenorrhea: A systematic approach to diagnosis and management. Am. Fam. Physician 2019, 100, 39–48. [Google Scholar] [CrossRef] [PubMed]
- Reindollar, R.H.; Byrd, J.R.; McDonough, P.G. Delayed sexual development: A study of 252 patients. Am. J. Obstet. Gynecol. 1981, 140, 371–380. [Google Scholar] [CrossRef] [PubMed]
- Baxter, R.M.; Arboleda, V.A.; Lee, H.; Barseghyan, H.; Adam, M.P.; Fechner, P.Y.; Bargman, R.; Keegan, C.; Travers, S.; Schelley, S.; et al. Exome sequencing for the diagnosis of 46, XY disorders of sex development. J. Clin. Endocrinol. Metab. 2015, 100, E333–E344. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dong, Y.; Yi, Y.; Yao, H.; Yang, Z.; Hu, H.; Liu, J.; Gao, C.; Zhang, M.; Zhou, L.; Yi, X.; et al. Targeted next-generation sequencing identification of mutations in patients with disorders of sex development. BMC Med. Genet. 2016, 17, 23. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yoon, J.Y.; Cheon, C.K. Evaluation and management of amenorrhea related to congenital sex hormonal disorders. Ann. Pediatr. Endocrinol. Metab. 2019, 24, 149. [Google Scholar] [CrossRef] [PubMed]
- Marsh, C.A.; Grimstad, F.W. Primary amenorrhea: Diagnosis and management. Obstet. Gynecol. Surv. 2014, 69, 603–612. [Google Scholar] [CrossRef] [PubMed]
- Hughes, I.A.; Houk, C.; Ahmed, S.F.; Lee, P.A. Consensus statement on management of intersex disorders. Arch. Dis. Child. 2006, 91, 554–563. [Google Scholar] [CrossRef]
- Kersemaekers, A.M.; Honecker, F.; Stoop, H.; Cools, M.; Molier, M.; Wolffenbuttel, K.; Bokemeyer, C.; Li, Y.; Lau, Y.F.; Oosterhuis, J.W.; et al. Identification of germ cells at risk for neoplastic transformation in gonadoblastoma: An immunohistochemical study for OCT3/4 and TSPY. Hum. Pathol. 2005, 36, 512–521. [Google Scholar] [CrossRef] [PubMed]
- de Jong, J.; Stoop, H.; Dohle, G.R.; Bangma, C.H.; Kliffen, M.; van Esser, J.W.; van den Bent, M.; Kros, J.M.; Oosterhuis, J.W.; Looijenga, L.H. Diagnostic value of OCT3/4 for pre-invasive and invasive testicular germ cell tumours. J. Pathol. 2005, 262, 242–249. [Google Scholar] [CrossRef] [PubMed]
- Huang, H.; Wang, C.; Tian, Q. Gonadal tumour risk in 292 phenotypic female patients with disorders of sex development containing Y chromosome or Y-derived sequence. Clin. Endocrinol. 2017, 86, 621–627. [Google Scholar] [CrossRef] [PubMed]
- Bandala-Jacques, A.; Estrada-Rivera, F.; Cantu, D.; Prada, D.; Montalvo-Esquivel, G.; González-Enciso, A.; Barquet-Munoz, S.A. Role of optimal cytoreduction in patients with dysgerminoma. Int. J. Gynecol. Cancer 2019, 29, 1405–1410. [Google Scholar] [CrossRef] [PubMed]
- Wünsch, L.; Holterhus, P.M.; Wessel, L.; Hiort, O. Patients with disorders of sex development (DSD) at risk of gonadal tumour development: Management based on laparoscopic biopsy and molecular diagnosis. BJU Int. 2012, 110, E958–E965. [Google Scholar] [CrossRef] [PubMed]




| Group of Risk | Malignancy Risk [%] | Disorder | Procedure |
|---|---|---|---|
| High | 15–35 | gonadal dysgenesis (Y +, intraabdominal gonads) | gonadectomy (during the diagnosis period) |
| 50 | PAIS (testicles outside the scrotum) | ||
| 40–60 | Frasier, Denys Drash (Y+) | ||
| Middle | 12 | Turner (Y+) | gonadectomy (during the diagnosis period) |
| 28 | 17ß HSD deficiency | Monitoring | |
| ? | Gonadal dysgenesis (Y +, gonads in the scrotum) | Biopsy during puberty and irradiation ? | |
| ? | PAIS—partial insensitivity to androgens (gonads in the scrotum) | Biopsy during puberty and irradiation ? | |
| Low | 3 | CAIS—complete insensitivity to androgens | Biopsy during puberty and ? |
| 2 | Ovarian-nuclear DSD | Testis tissue removal ? | |
| 1 | Turner (Y-) | None |
| Parameter | Score | Sr |
|---|---|---|
| FSH | 56.7 mIU/mL | 2.8–11.3 |
| LH | 19.8 mIU/mL | 1.2–11.6 |
| Estradiol | <5 pg/mL | 10–160 |
| Testosteron | 0.348 ng/mL | 0.006–0.8 |
| ACTH | 28.6 pg/mL | 7.2–63.3 |
| Cortisol | 16.9 µg/dL | 6.2–19.4 |
| TSH | 3.7 mIU/mL | 0.2–4.0 |
| fT4 | 1.03 ng/dL | 0.9–1.7 |
| LDH | 118.0 U/L | 120–230 |
| beta-hCG | 0.753 IU/mL | <10 |
| AFP | 3.8 IU/mL | <6 |
| Ca-125 | 8.21 U/mL | <35 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sowińska-Przepiera, E.; Krzyścin, M.; Przepiera, A.; Brodowska, A.; Malanowska, E.; Kozłowski, M.; Cymbaluk-Płoska, A. Late Diagnosis of Swyer Syndrome in a Patient with Bilateral Germ Cell Tumor Treated with a Contraceptive Due to Primary Amenorrhea. Int. J. Environ. Res. Public Health 2023, 20, 2139. https://doi.org/10.3390/ijerph20032139
Sowińska-Przepiera E, Krzyścin M, Przepiera A, Brodowska A, Malanowska E, Kozłowski M, Cymbaluk-Płoska A. Late Diagnosis of Swyer Syndrome in a Patient with Bilateral Germ Cell Tumor Treated with a Contraceptive Due to Primary Amenorrhea. International Journal of Environmental Research and Public Health. 2023; 20(3):2139. https://doi.org/10.3390/ijerph20032139
Chicago/Turabian StyleSowińska-Przepiera, Elżbieta, Mariola Krzyścin, Adam Przepiera, Agnieszka Brodowska, Ewelina Malanowska, Mateusz Kozłowski, and Aneta Cymbaluk-Płoska. 2023. "Late Diagnosis of Swyer Syndrome in a Patient with Bilateral Germ Cell Tumor Treated with a Contraceptive Due to Primary Amenorrhea" International Journal of Environmental Research and Public Health 20, no. 3: 2139. https://doi.org/10.3390/ijerph20032139






